COPD Chronic Obstructive Pulmonary Disease Dr dr Tahan

COPD Chronic Obstructive Pulmonary Disease Dr. dr. Tahan P. H. , Sp. P. , DTCE. , MARS Penyakit Dalam FK-UWKS 15 -06 -12

Introduction Chronic Obstructive Pulmonary Disease (COPD) is one of the top five causes of global mortality COPD affects 210 million people worldwide and causes 3 million deaths annually (5% of all deaths worldwide)1 It is predicted to become third leading cause of global mortality by 20302 The economic burden of COPD is high, with costs increasing as the disease progresses - Costs associated with severe COPD are up to 17 times higher than those associated with mild COPD 3 High costs are associated with treatment of exacerbations, such as hospitalisation 3 Indirect costs include loss of productivity in the workplace owing to symptoms 3
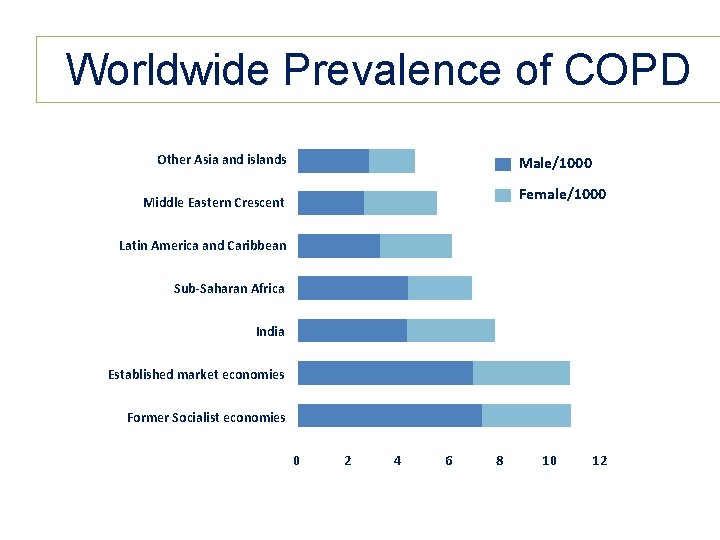
Worldwide Prevalence of COPD Other Asia and islands Male/1000 Female/1000 Middle Eastern Crescent Latin America and Caribbean Sub-Saharan Africa India Established market economies Former Socialist economies 0 2 4 6 8 10 12 Adapted from the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2005.

COPD Misdiagnosis Is Common in Women Hypothetical Male Patient With COPD Symptoms 65% Diagnosed as COPD by 65% of physicians 49% Hypothetical Female Patient With COPD Symptoms Diagnosed as COPD by 49% of physicians COPD symptoms in women were most commonly misdiagnosed as asthma Chapman KR, et al. Chest. 2001; 119: 1691 -1695.
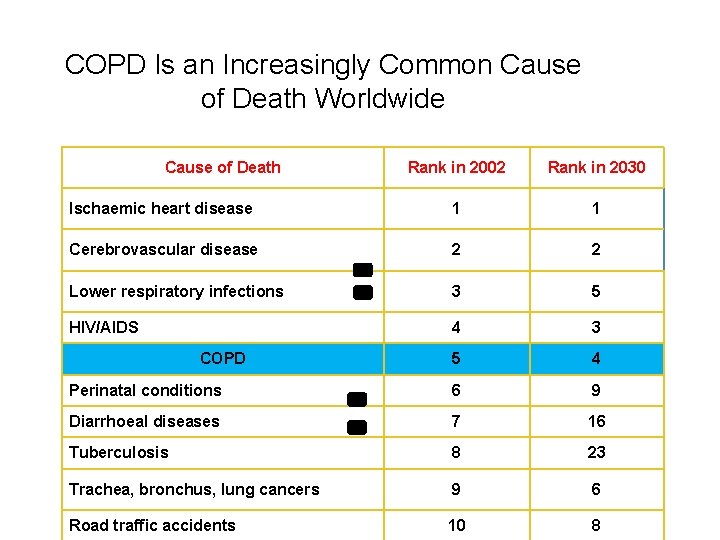
COPD Is an Increasingly Common Cause of Death Worldwide Cause of Death Rank in 2002 Rank in 2030 Ischaemic heart disease 1 1 Cerebrovascular disease 2 2 Lower respiratory infections 3 5 HIV/AIDS 4 3 5 4 Perinatal conditions 6 9 Diarrhoeal diseases 7 16 Tuberculosis 8 23 Trachea, bronchus, lung cancers 9 6 10 8 COPD Mathers CD, et al. PLo. S Med. 2006; 3: 2011 -2030. Road traffic accidents

What is COPD? Global Initiative for Chronic Obstructive Lung Disease (GOLD) defines COPD as (2009): “a preventable and treatable disease with some significant extrapulmonary effects that may contribute to the severity in individual patients. Its pulmonary component is characterised by airflow limitation that is not fully reversible. The airflow limitation is usually progressive and associated with abnormal inflammatory response of the lung to noxious particles or gases” Key points: - COPD is preventable and treatable - Airway limitation is not fully reversible and is usually progressive - Extrapulmonary (systemic) effects play a significant role - Associated with chronic inflammation in response to inhaled noxious irritants
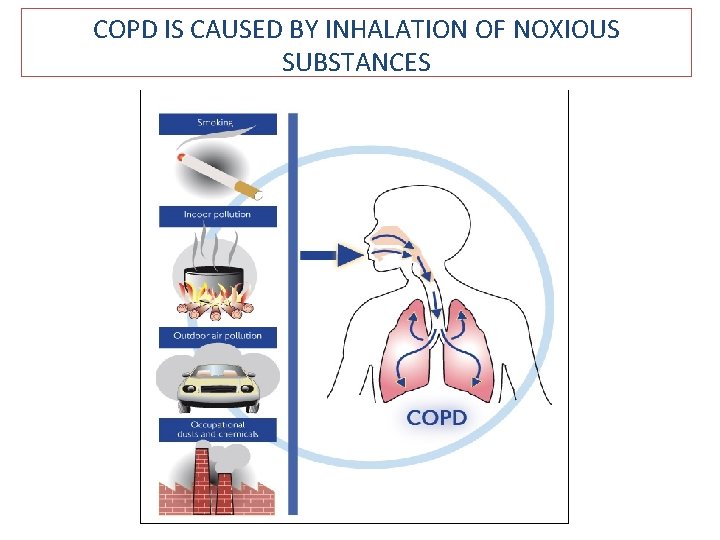
COPD IS CAUSED BY INHALATION OF NOXIOUS SUBSTANCES
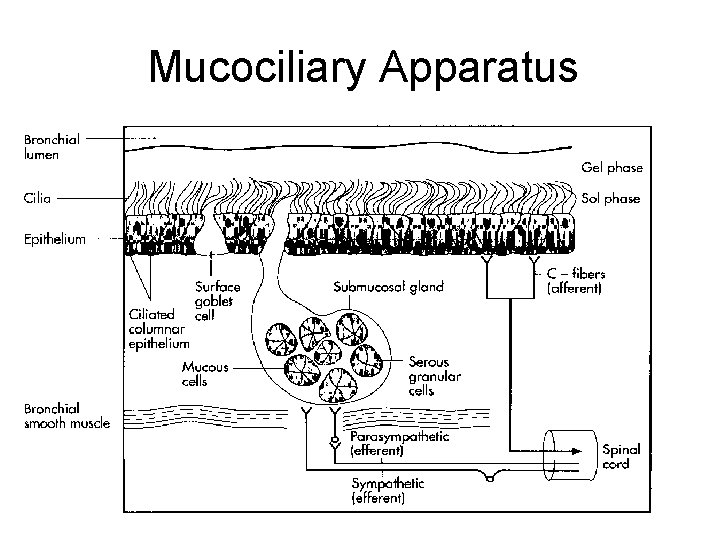
Mucociliary Apparatus
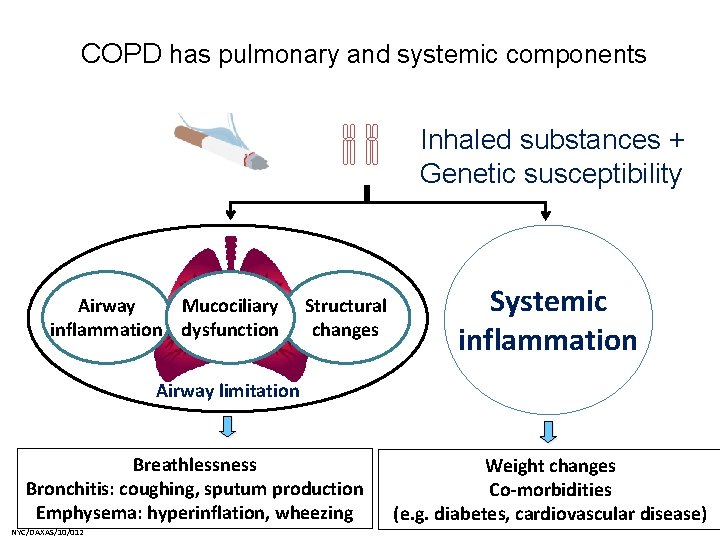
COPD has pulmonary and systemic components Inhaled substances + Genetic susceptibility Airway Mucociliary inflammation dysfunction Structural changes Systemic inflammation Airway limitation Breathlessness Bronchitis: coughing, sputum production Emphysema: hyperinflation, wheezing NYC/DAXAS/10/012 Weight changes Co-morbidities (e. g. diabetes, cardiovascular disease)

WHAT IS THE ROLE OF INFLAMMATION IN COPD?
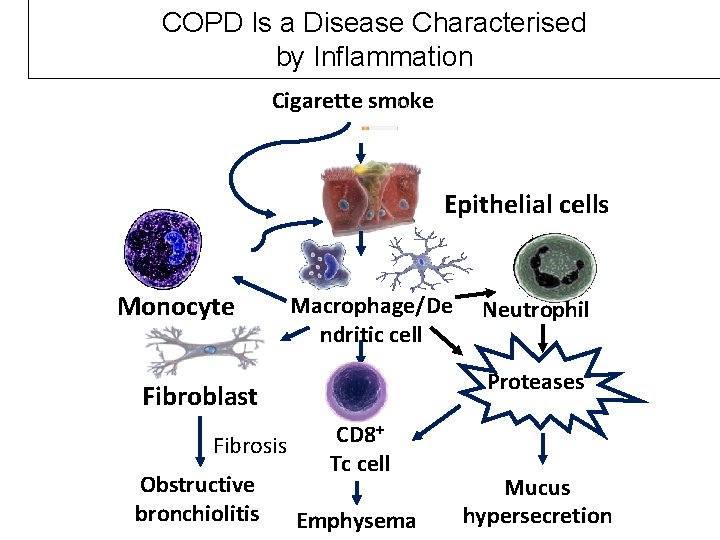
COPD Is a Disease Characterised by Inflammation Cigarette smoke Epithelial cells Monocyte Macrophage/De ndritic cell Proteases Fibroblast Fibrosis Obstructive bronchiolitis Neutrophil CD 8+ Tc cell Emphysema Mucus hypersecretion
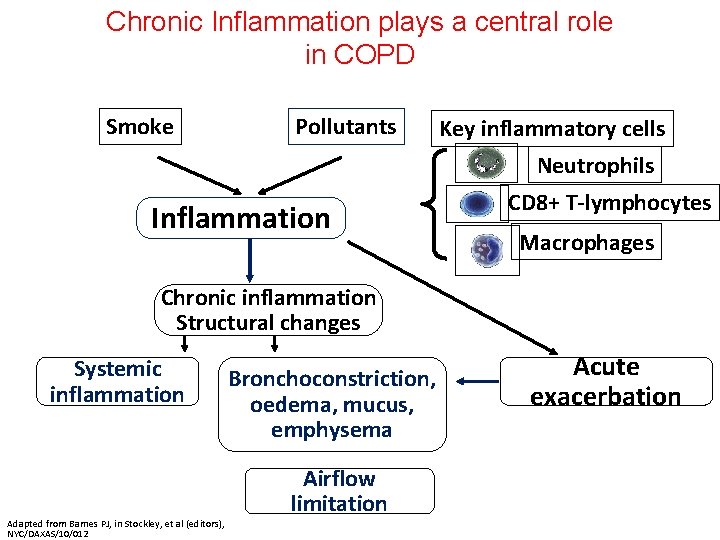
Chronic Inflammation plays a central role in COPD Smoke Pollutants Key inflammatory cells Neutrophils Inflammation CD 8+ T-lymphocytes Macrophages Chronic inflammation Structural changes Systemic inflammation Bronchoconstriction, oedema, mucus, emphysema Airflow limitation Acute exacerbation Adapted from Barnes PJ, in Stockley, et al (editors), Chronic Obstructive Pulmonary Disease. Oxford, England: Blackwell Publishing; 2007: 860. NYC/DAXAS/10/012

COPD inflammation is different from asthma inflammation COPD Noxious agent Asthma Onset Sensitising agent Neutrophils Inflammatory cells Eosinophils CD 4+ TCD 8+ Tlymphocytes Macrophages Mast cells Not fully reversible Airflow limitation From the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2009. Available from: http: //www. goldcopd. org. NYC/DAXAS/10/012 Reversible
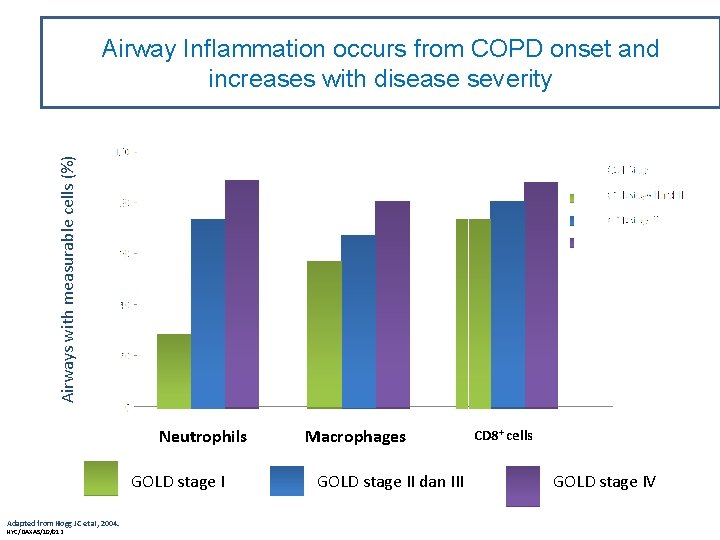
Airways with measurable cells (%) Airway Inflammation occurs from COPD onset and increases with disease severity Neutrophils GOLD stage I Adapted from Hogg JC et al, 2004. NYC/DAXAS/10/012 Macrophages GOLD stage II dan III CD 8+ cells GOLD stage IV

How is COPD diagnosed and managed? NYC/DAXAS/10/012
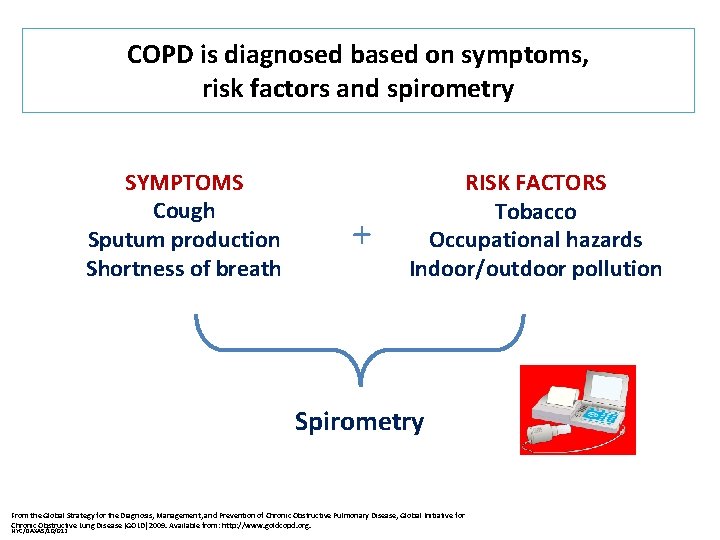
COPD is diagnosed based on symptoms, risk factors and spirometry SYMPTOMS Cough Sputum production Shortness of breath + RISK FACTORS Tobacco Occupational hazards Indoor/outdoor pollution Spirometry From the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2009. Available from: http: //www. goldcopd. org. NYC/DAXAS/10/012

Classification of cough • Cough is classified into acute and chronic and • Clinically subdivided into productive and dry cough. Productive cough is present at an expectoration rate of 30 ml/24 hours,

Classification of cough • Acute cough is defined as one lasting less than three weeks • Chronic cough is defined as one lasting greater than eight weeks

Acute Cough. . . < 3 weeks Differential Diagnosis • URTI : Sinusitis viral / bacterial • URTI triggering exacerbations of Chronic Lung Disease eg Asthma; COPD • Pneumonia • Left Ventricular Heart Failure • Foreign Body Aspiration
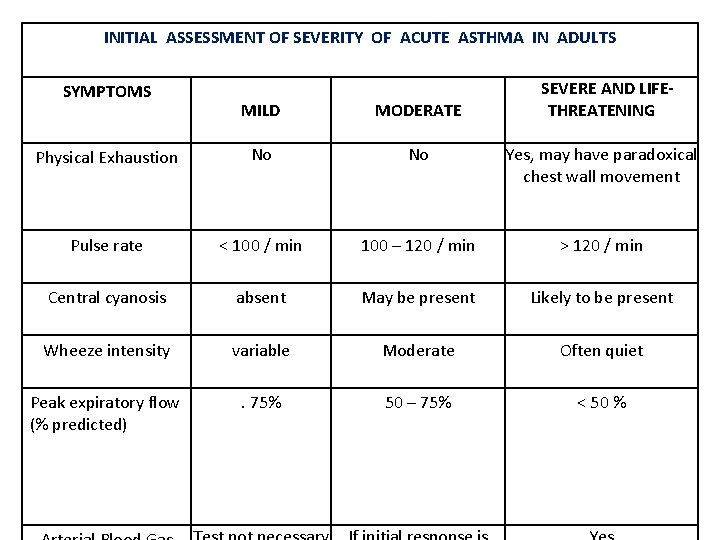
INITIAL ASSESSMENT OF SEVERITY OF ACUTE ASTHMA IN ADULTS SYMPTOMS SEVERE AND LIFETHREATENING MILD MODERATE Physical Exhaustion No No Yes, may have paradoxical chest wall movement Pulse rate < 100 / min 100 – 120 / min > 120 / min Central cyanosis absent May be present Likely to be present Wheeze intensity variable Moderate Often quiet Peak expiratory flow (% predicted) . 75% 50 – 75% < 50 %

GOALS OF COPD MANAGEMENT – Relieve symptoms – Improve exercise tolerance – Improve health status – Prevent and treat exacerbations – Prevent disease progression – Prevent and treat complications – Reduce mortality Adapted from the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2009. Available from: http: //www. goldcopd. org. NYC/DAXAS/10/012 Improve current control Reduce future risks
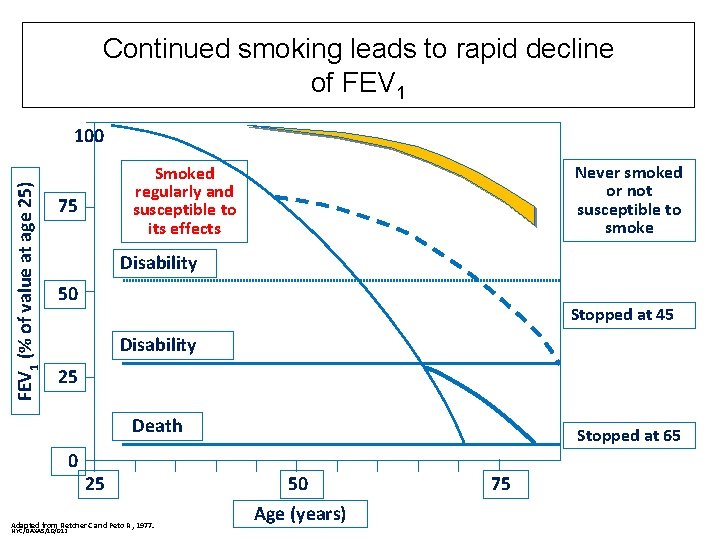
Continued smoking leads to rapid decline of FEV 1 (% of value at age 25) 100 Never smoked or not susceptible to smoke Smoked regularly and susceptible to its effects 75 Disability 50 Stopped at 45 Disability 25 Death 0 25 Adapted from Fletcher C and Peto R , 1977. NYC/DAXAS/10/012 Stopped at 65 50 Age (years) 75
What are exacerbations ? NYC/DAXAS/10/012

What are exacerbations? Global Initiative for Chronic Obstructive Lung Disease (GOLD) defines an exacerbation as: “an event in the natural course of the disease characterized by a change in the patient’s baseline dyspnea, cough, and/or sputum that is beyond normal day-to-day variations, is acute in onset and may warrant a change in regular medication” 1 – May be mild, moderate or severe in nature. More severe exacerbations can require hospitalisation and are associated with a prolonged recovery period 2 – Commonly caused by bacterial/viral infections of the lungs and airways 1 – Associated with increases in markers of inflammation 3, 4 – Distressing for patients and their loved ones
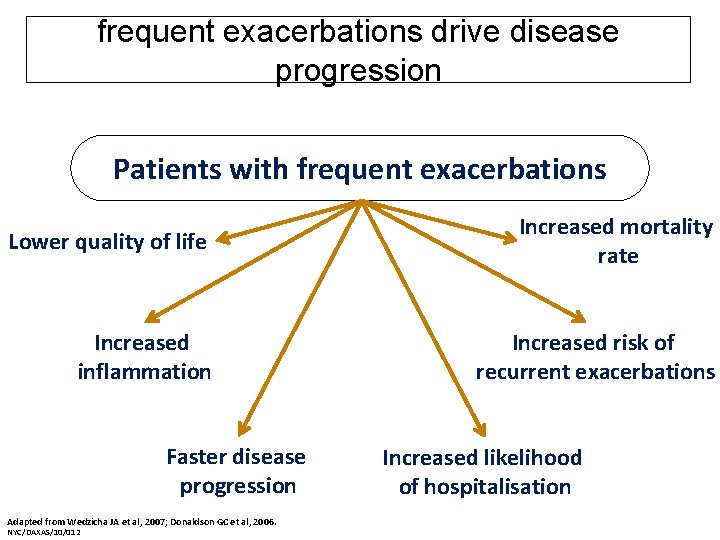
frequent exacerbations drive disease progression Patients with frequent exacerbations Lower quality of life Increased mortality rate Increased inflammation Increased risk of recurrent exacerbations Faster disease progression Adapted from Wedzicha JA et al, 2007; Donaldson GC et al, 2006. NYC/DAXAS/10/012 Increased likelihood of hospitalisation
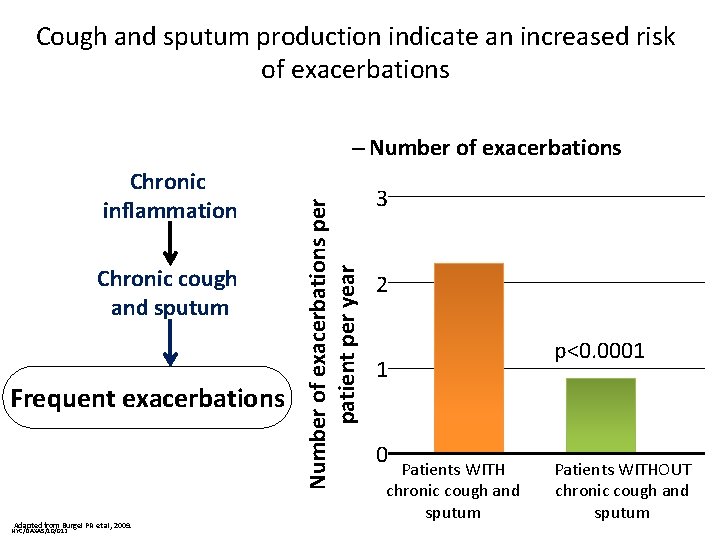
Cough and sputum production indicate an increased risk of exacerbations Chronic inflammation Chronic cough and sputum Frequent exacerbations Adapted from Burgel PR et al, 2009. NYC/DAXAS/10/012 Number of exacerbations per patient per year – Number of exacerbations 3 2 1 0 Patients WITH chronic cough and sputum p<0. 0001 Patients WITHOUT chronic cough and sputum

Definitions of Exacerbations COPD exacerbations were classified in clinical studies as follows: – ‘Severe’ COPD exacerbation – Requiring hospitalisation and/or leading to death – ‘Moderate’ COPD exacerbation – Initiation of oral or parenteral glucocorticosteroid therapy is required Calverley PMA et al, 2009. Fabbri L, et al, 2009. NYC/DAXAS/10/012
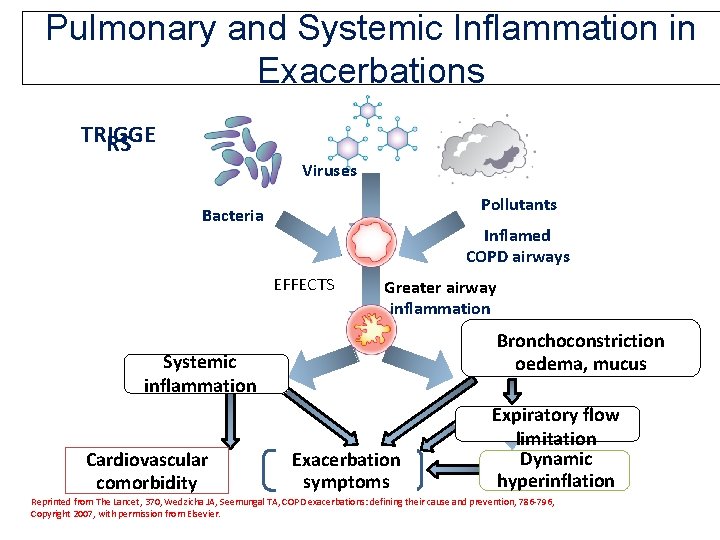
Pulmonary and Systemic Inflammation in Exacerbations TRIGGE RS Viruses Pollutants Bacteria Inflamed COPD airways EFFECTS Greater airway inflammation Bronchoconstriction oedema, mucus Systemic inflammation Cardiovascular comorbidity Exacerbation symptoms Expiratory flow limitation Dynamic hyperinflation Reprinted from The Lancet, 370, Wedzicha JA, Seemungal TA, COPD exacerbations: defining their cause and prevention, 786 -796, Copyright 2007, with permission from Elsevier. 28

FACTORS PRECIPITATING FAILURE • Sputum retention • Bronchospasm • Infection • Pneumothorax • Large bullae • Uncontrolled O 2 - administration • Pulmonary embolism • Left-ventricular failure • End-stage disease ACUTE

PATHO- PHYSIOLOGY…. FACTORS AFFECTING AIR-FLOW • • Mucosal edema Hypertrophy of mucosa Increased secretions Increased bronchospasm incr. Airway tortuosity More airway turbulance Loss of lung recoil

PATHO-PHYSIOLOGY…. contd AIR-FLOW OBSTRUCTION PROLONGED EXPIRATION PULMONARY HYPERINFLATION DUE TO AIR-TRAPPING INCREASED WORK OF BREATHING DYSPNOEA

PATH-PHYSIO…. . CONTD ALVEOLAR DISTORTION AND DESTRUCTION LOSS OF HYPOXIA CAUSING CAPILLARY BED PULMONARY VAS ON PULMONARY HYPERTENSION SECONDARY VASCULAR CHANGES
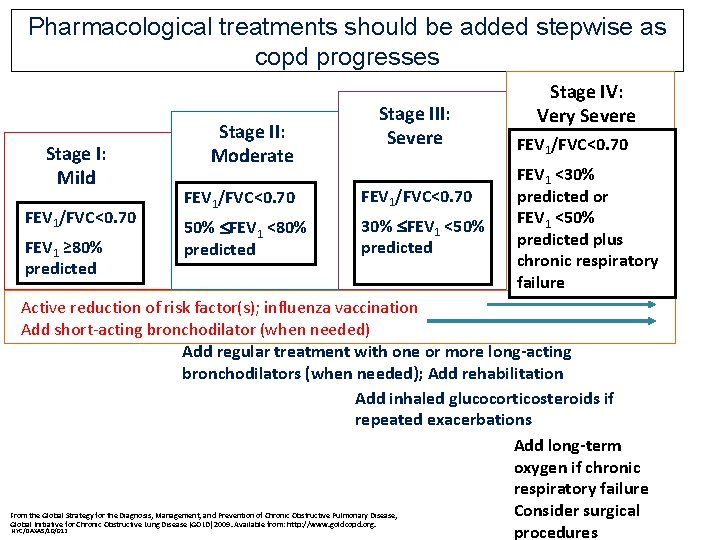
Pharmacological treatments should be added stepwise as copd progresses Stage I: Mild FEV 1/FVC<0. 70 FEV 1 ≥ 80% predicted Stage II: Moderate Stage III: Severe FEV 1/FVC<0. 70 50% FEV 1 <80% predicted 30% FEV 1 <50% predicted Stage IV: Very Severe FEV 1/FVC<0. 70 FEV 1 <30% predicted or FEV 1 <50% predicted plus chronic respiratory failure Active reduction of risk factor(s); influenza vaccination Add short-acting bronchodilator (when needed) Add regular treatment with one or more long-acting bronchodilators (when needed); Add rehabilitation Add inhaled glucocorticosteroids if repeated exacerbations Add long-term oxygen if chronic respiratory failure Consider surgical From the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2009. Available from: http: //www. goldcopd. org. procedures NYC/DAXAS/10/012

MANAGEMENT – NONINVASIVE # BRONCHODILATORS • ROUTINELY GIVEN • HELP RESIDUAL BRONCHODILATION AND MUCO-CILIARY CLEARANCE [ I. V. AMINOPHYLLINE / B 2 -AGONIST / IPRATROPIUM ] …CONTD

CONSERVATIVE MANAGEMENT …. contd # ANTIBIOTICS # STEROIDS … AVOID IN ARF DUE TO INFECTION # OTHER * STEAM / PHYSIOTHERAPY / ENCOURAGE COUGH * GENERAL HYDRATION * DIURETICS / LOW DIGOXIN IF LVF * HEPARIN S /C FOR D V T / PULM EMBOLISM * NUTRITION * RESPIRATORY STIMULANTS

MANAGEMENT - NON CONSERVATIVE…. CONSERVATIVE 1. INVASIVE TECHNIQUES FOR SPUTUM CLEARANCE • OROPHARYNGEAL / NASOPHARYNGEAL SUCTION • NASO-PHARYNGEAL AIR-WAY • THERAPEUTIC AND DIAGNOSTIC F O B • MINI TRACHEOSTOMY/ CRICOTHYROTOMY FOR SUCTION • ENDOTRACHEAL INTUBATION * FOR BETTER ACCESS * FOR VENTILATORY SUPPORT • TRACHEOSTOMY * IF VERY THICK SECRETIONS * INTUBATION > SEVEN DAYS
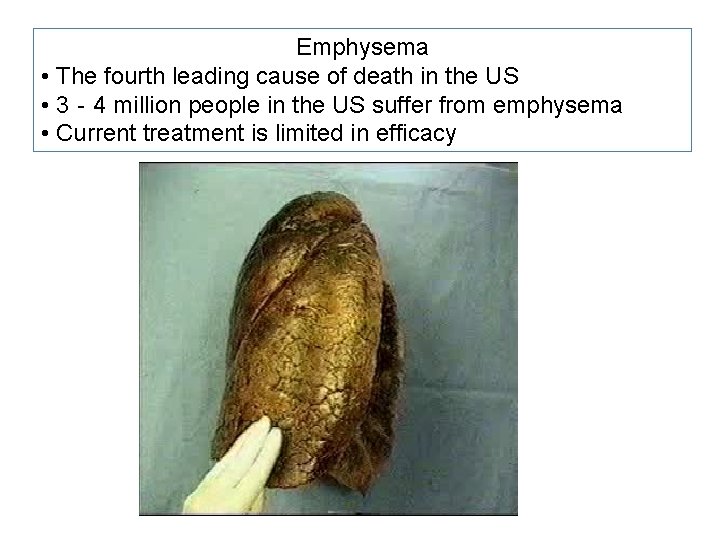
Emphysema • The fourth leading cause of death in the US • 3‐ 4 million people in the US suffer from emphysema • Current treatment is limited in efficacy

Bronchoscopic Lung Volume Reduction for Emphysema The Concept of lung Volume Reduction • Lung volume Reduction 1. – Removal of the most destroyed hyperinflated poorly perfused areas of the lung can enhance the function of the remaining “normal” lung and leads to func(onal and symptoma(c improvement 2. – Applicable in heterogeneous emphysema (upper lobe predominant) • Multiple retrospective and prospective studies reported success with surgical lung volume reduction

SUMMARY �COPD is a debilitating disease that presents a huge healthcare and economic burden around the world �The major risk factor for developing COPD is tobacco smoking �COPD encompasses damage to the airways, and chronic pulmonary and systemic inflammation �The symptoms of COPD include breathlessness, chronic cough and sputum production

�Chronic inflammation in the airways and systemic circulation contributes to the pathology of COPD �COPD-specific inflammation is characterised by increased neutrophils, CD 8+ T-lymphocytes and macrophages, as well as cytokines and other inflammatory mediators �Inflammatory processes activated in asthma are different from COPD-specific inflammation �Chronic inflammation is present from the onset of COPD and increases with disease progression. Airway inflammation increases during exacerbations �Effective COPD management should include agents that target the chronic inflammation underlying the

Exacerbations are attacks in which symptoms increase beyond daily variations Patients with frequent exacerbations have a poor prognosis and increased risk of mortality Inflammation is increased during exacerbations The symptoms of chronic cough and sputum production are associated with an increased risk of exacerbations Preventing exacerbations is a major goal of COPD management

COPD is diagnosed based on medical history, exposure to risk factors and assessment of lung function by spirometry GOLD guidelines recommend seven goals for COPD management, including reducing the frequency of exacerbations Non-pharmacological management of COPD includes smoking cessation GOLD guidelines recommend stepwise addition of pharmacological treatments based on the severity of

The Downward Spiral in COPD Lung inflammation Mucous hypersecretion Exacerbation Continued smoking Airway obstruction Impaired mucous clearance Exacerbation Alveolar destruction Submucousal gland hypertrophy Exacerbation Hypoxaemia DEATH From the Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease, Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2008. Available from: http: //www. goldcopd. org.

THANK-YOU
- Slides: 44