CONTRACEPTION MANAGEMENT Complexities in Contraceptive Care Theres an










































- Slides: 51

CONTRACEPTION MANAGEMENT: Complexities in Contraceptive Care

There’s an App for That!

Learning Objectives Apply evidenced-based guidelines to contraceptive provision using the CDC Medical Eligibility Criteria (MEC) resource 2. Explore contraception options in patients with a complex medical history 3. Accurately discuss the risks and benefits of medically complex contraception care with both patients and colleagues 1.

Complex Contraception In one study, only 40% of women aged 15 -34 and 32% of women aged 35 -44 with chronic medical conditions were using contraception.

Medical Eligibility Criteria Risk Level 1 Method can be used without restriction 2 Advantages generally outweigh theoretical or proven risk 3 Method usually not recommended unless other, more appropriate methods are not available or not acceptable 4 Method not to be used https: //www. cdc. gov/reproductivehealth/contraception

Amy 24 year old patient comes to the office with a UTI.

Amy You ask her the “One Key Question”

One Key Question “Can we help you today with birth control or pregnancy planning? ” • Offer preconception care vs birth control • Plus screen for DV (domestic violence), smoking, depression • Discuss exercise and diet

Amy – medical history • BMI = 34 • History of pregnancyrelated cholestasis

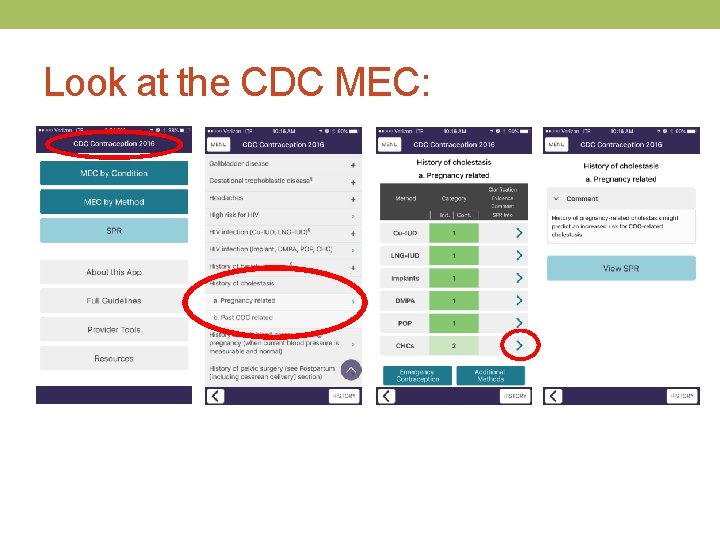
Look at the CDC MEC: BMI > 30 = 2

Look at the CDC MEC:

Medical Eligibility Criteria Risk Level 1 Method can be used without restriction 2 Advantages generally outweigh theoretical or proven risk 3 Method usually not recommended unless other, more appropriate methods are not available or not acceptable 4 Method not to be used https: //www. cdc. gov/reproductivehealth/contraception
Should Amy Restart her COCs? Does 2+2 = 2 or 3 or 4?

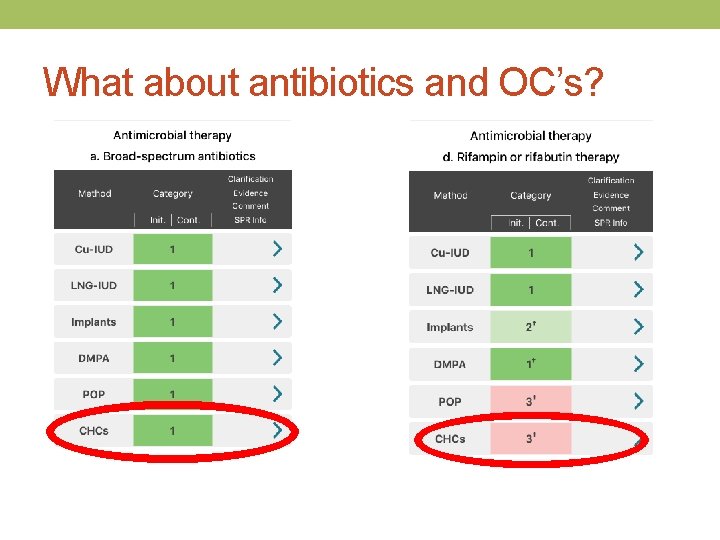
What about antibiotics and OC’s?

Learning points • Sometimes, 2 + 2 = 2 • Generally, antibiotics do not decrease efficacy of contraceptives

Doreen 46 year-old G 2 P 2. She would like to remove her copper IUD and try “the shot. ”

Medical Issues • Age (46) • Gallstones • Obesity (BMI > 30)

Can Doreen Safely Use the Depo? What does 2 + 1 equal?

How Should She Switch Methods?

Learning Points 2 + 1 can still = 2! Reference www. reproductiveaccess. org when switching birth control methods

Rosa 20 year old G 0 with sickle cell anemia wants to try the IUD “without hormones. ”

Category 4 Conditions for IUDs • Current PID, gonorrhea, chlamydia • Category 4 for initiation only • Certain anatomic abnormalities • May interfere with proper IUD placement • Endometrial cancer • Initiation only • Cervical cancer awaiting treatment • Initiation only • Active pregnancy • Options counseling • Unexplained vaginal bleeding • Suspicious for serious condition

Rosa • She can get a copper IUD, as it is a “ 2” for sickle cell disease. • History of PID also a “ 2”

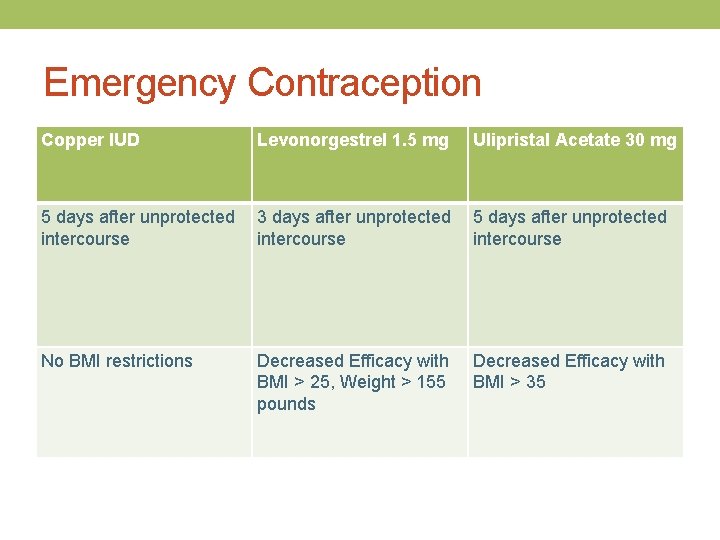
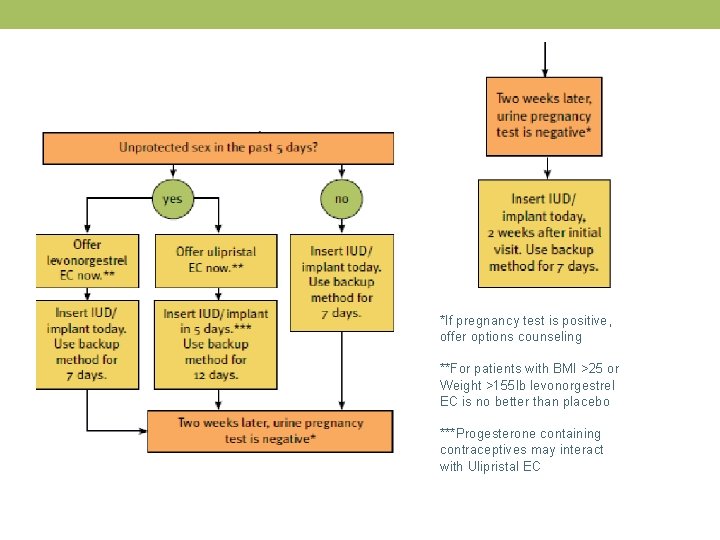
Emergency Contraception Copper IUD Levonorgestrel 1. 5 mg Ulipristal Acetate 30 mg 5 days after unprotected 3 days after unprotected 5 days after unprotected intercourse No BMI restrictions Decreased Efficacy with BMI > 25, Weight > 155 pounds Decreased Efficacy with BMI > 35

Learning Points • History of PID is a “ 2”, high risk of STI is a “ 2”

Audrey 38 year old G 3 P 3. She is happy with her Combined Oral Contraceptives & is here for a refill.

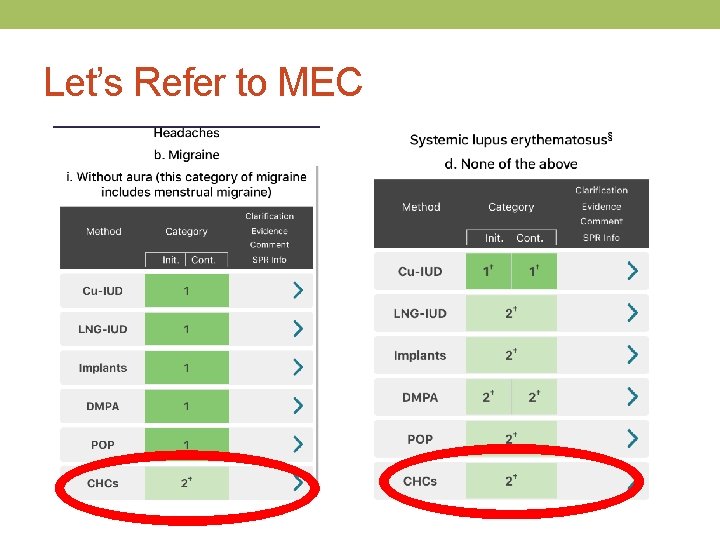
Let’s Refer to MEC

What about her age?
Should you refill Audrey’s COCs? What does 2 + 1 equal?

Learning Points Minor contraindications can be additive if they have the same pathway.

Julie 17 year old G 2 P 0. She is interested in learning more about the IUD.

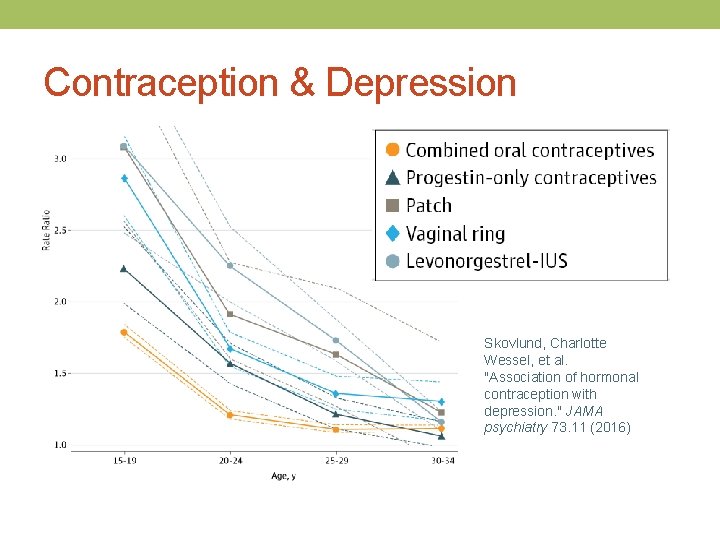
Contraception & Depression Skovlund, Charlotte Wessel, et al. "Association of hormonal contraception with depression. " JAMA psychiatry 73. 11 (2016)

Contraception & Depression Looking at Relative Risk Alone can be Misleading! When we consider Absolute Risk: • 2. 2 per 100 person years in Ever Users of Hormonal Contraception Vs • 1. 7 per 100 person years in Never Users or Hormonal Contraception

Different Types of IUDs Non-Hormonal Paragard Hormonal Skyla Kyleena Mirena/Liletta

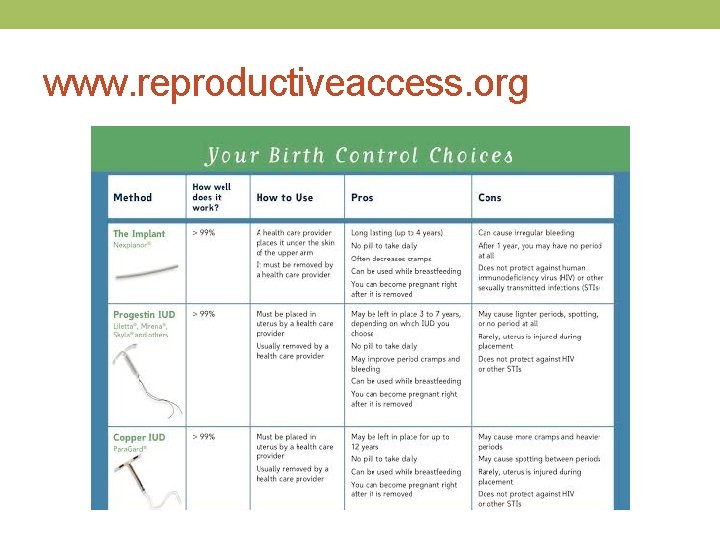
www. reproductiveaccess. org

Patient Centered Care Avoid pushing a method that teen “heard bad things about” • Reduces trust and adherence

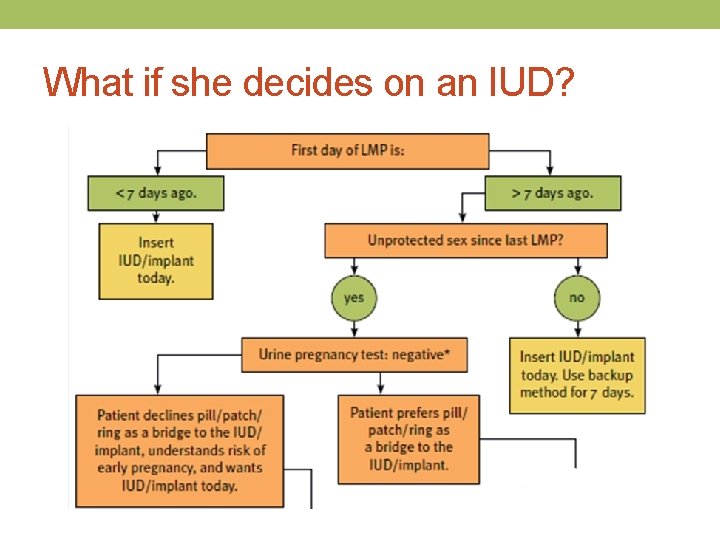
What if she decides on an IUD?

*If pregnancy test is positive, offer options counseling **For patients with BMI >25 or Weight >155 lb levonorgestrel EC is no better than placebo ***Progesterone containing contraceptives may interact with Ulipristal EC

Quick start method: history of STI • Same day insertion = gold standard • Do not insert an IUD with purulent cervicitis

IUDs Can be Inserted: a) Only during menses b) Only within 7 days of LMP c) Any time during the cycle if pregnancy has been reasonably ruled out

Katie 28 yo G 0 comes to your office for contraception she doesn’t have to think about - Likes the idea of the implant - History of a seizure d/o (stable on carbamazepine) - Type 1 DM diagnosed age 12

A different way to look at the CDC MEC

Should We Recommend the Implant for Katie? What does 2 + 2 equal? a) 2 b) 3 c) 4

Learning Points • The danger of anticonvulsants (except lamotrigine) is decreasing efficacy of contraceptives • Long term diabetes is a “ 2” for all progestin methods, a “ 3 -4” for estrogen containing products

Practice Recommendations • Particularly when patients have multiple medical problems, progestin methods are safer than estrogen + progestin • Copper IUD generally the safest method • Vasectomy is VERY safe! • Birth control and abortion are both safer than pregnancy

Questions?

Billing & Coding ICD 10 Codes to Know: • Z 30. 011 Initial, contraceptive pills • Z 30. 012 EC prescription • Z 30. 013 Initial, Injection • Z 30. 014 Initial, IUC • Z 30. 015 Initial, Ring • Z 30. 016 Initial, Patch • Z 30. 017 Initial, Implant • Z 30. 41 surveillance, contraceptive pills • Z 30. 42 Surveillance, Injection • Z 30. 43 Surveillance, IUC • Z 30. 44 Surveillance, Ring • Z 30. 45 Surveillance, Patch • Z 30. 46 Surveillance, Implant

Billing & Coding Procedure (CPT) Codes to Know: • 58300 Insertion of IUD • Z 30. 430 encounter for insertion of IUC • J 7298 Mirena, J 7297 Liletta, J 7300 Paragard, J 7301 Skyla, • 58301 IUD removal • Z 30. 432 encounter for removal of IUC • 58300 & 58301 for IUD removal & reinsertion • Z 30. 433 & relevant J code

Billing & Coding CPT Codes to Know Cont: • 11981 Insertion Implant • Z 30. 017 encounter for insertion of Implant • J 7307 Nexplanon • 11982 Removal Implant • Z 30. 46 encounter for surveillance of Implant • J 7307 • 11983 Removal & Reinsertion Implant • Z 30. 46

Billing & Coding Other helpful codes to know: • J 2000 Lidocaine • A 4550 Surgical Tray • 53 modifier can be used for attempted, but unsuccessful, IUD insertions

References & Resources • Hatcher et al, Contraceptive Technology 2007 • Centers for Disease Control and Prevention (CDC). U. S. Medical Eligibility Criteria for Contraceptive • • Use Managing Contraception – book online @ www. managingcontraception. org Association of Reproductive Health Professionals www. arhp. org Alan Guttmacher Institute www. agi-usa. org Planned Parenthood www. plannedparenthood. org The Cochrane Collaboration www. cochrane. org www. Not-2 -Late. com Reproductive Health Access Project www. reproductiveaccess. org www. bedsider. org