Contextual Factors SESSION 5 COLLABORATIVE LEARNING PROJECT Contextual

Contextual Factors SESSION 5: COLLABORATIVE LEARNING PROJECT

Contextual Factors in Presentation in Healthy Weight Program Barriers to Healthy Weight Program Attendance Sandra G Hassink, MD Medical Director, AAP Institute for Healthy Childhood Weight SESSION 5: COLLABORATIVE LEARNING PROJECT

Learning Objectives • Describe contextual factors that may moderate/influence HWP process evaluation and evaluation outcomes independent of the intervention and how to address them as a program is developed • Prioritize contextual factors to include in the core measures: Parent/child readiness to change Parent/child/staff expectations Parent/child socio-demographics Transportation/childcare Environmental factors (e. g. , opportunity for safe places to play; access to healthy affordable foods) Cost/finances SESSION 5: COLLABORATIVE LEARNING PROJECT

Learning Objectives Barriers to Healthy Weight Program Attendance • Transportation/childcare • Environmental factors (e. g. , opportunity for safe places to play, access to healthy affordable foods) • Cost/finances SESSION 5: COLLABORATIVE LEARNING PROJECT

Measures and Program Attendance • We typically measure and analyze our populations using demographic data • We measure BMI and comorbidities, but we are just beginning to stratify our populations with these disease- related measures • We are just beginning to measure patient contextual factors; much of the work is still in the qualitative phase SESSION 5: COLLABORATIVE LEARNING PROJECT
Barriers to Attendance • Focus group participants females aged 18 -57 years (71% black, 81% single parents) • Caretakers reported perceived barriers that would limit child’s future participation in a HWP Lack of time (parent, child) Frustration from prior unsuccessful weight loss attempts Perceived cost of healthy food and exercise options Transportation • Facilitators Convenient location Supportive program leader Rewards for child progress – – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 Sonneville KR, La Pelle N, Taveras EM, Gillman MW, Prosser LA. Economic and other barriers to adopting recommendations to prevent childhood obesity: results of a focus group study with parents. BMC Pediatr. 2009. December 21 9: 81 SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers: Transportation • Lack of public transportation – Brennan L, Walkley J, Wilks R. Parent- and adolescent-reported barriers to participation in an adolescent overweight and obesity intervention. Obesity (Silver Spring). 2012. June; 20 6: 13191324. • Need for reimbursement for transportation – Drury VB, Saw SM, Finkelstein E, Wong TY, Tay PK. A new community-based outdoor intervention to increase physical activity in Singapore children: findings from focus groups. Ann Acad Med Singapore. 2013. May; 42 5: 225 - 231. • Inadequate transportation to safe physical activity outlets for youth – Hannay J, Dudley R, Milan S, Leibovitz PK. Combining Photovoice and focus groups: engaging Latina teens in community assessment. Am J Prev Med. 2013. March; 44 3 Suppl 3: S 215 - S 224. inadequate transportation to safe physical activity outlets for youth SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers: Time • Long work hours and busy schedules Parents’ limited ability to engage in healthy behaviors with their child Parents’ limited ability to attend a weight-management program with their child • Children busy with school, homework, and extracurricular activities Little time for exercise or attending a lifestyle intervention – – – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 Berge JM, Arikian A, Doherty WJ, Neumark-Sztainer D. Healthful eating and physical activity in the home environment: results from multifamily focus groups. J Nutr Educ Behav. 2012. Mar-Apr; 44 2: 123 - 131. doi: 10. 1016/j. jneb. 2011. 06. 011. [PMC free article] [Pub. Med] [Google Scholar] Bentley GF, Goodred JK, Jago R, et al. Parents' views on child physical activity and their implications for physical activity parenting interventions: a qualitative study. BMC Pediatr. 2012. November 20; 12: 180 SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers: Time • Phone interviews of youths (11 -18 yrs. ) in weight management program 57% who did not complete the treatment • Lack of time • Conflicting school commitments as key barriers to sustained participation. – Brennan L, Walkley J, Wilks R. Parent- and adolescent-reported barriers to participation in an adolescent overweight and obesity intervention. Obesity (Silver Spring). 2012. June; 20 6: 13191324. SESSION 5: COLLABORATIVE LEARNING PROJECT

Facilitators: Time • Some parents/guardians stated that the time burden could be partially attenuated by: Scheduling program sessions far in advance Providing transportation assistance Mapping the frequency and duration of the program onto the academic school year. – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers: Access to Food • Barriers to purchasing fresh fruits and vegetables: Cost of fresh produce Expiration of fresh produce before use Child's dislike for vegetables – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers to Exercise • Cost of childcare The main exercise-related cost complaint was that parents/guardians would have to pay for childcare for younger siblings so that parents/guardians could take an older child to the gym or other organized activities – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 – Haerens L, De Bourdeaudhuij I, Eiben G, et al. Formative research to develop the IDEFICS physical activity intervention component: findings from focus groups with children and parents. J Phys Act Health. 2010. March; 7 2: 246 - 256. SESSION 5: COLLABORATIVE LEARNING PROJECT

Barriers: Community • Lack of safe places to exercise – Goh YY, Bogart LM, Sipple-Asher BK, et al. Using community-based participatory research to identify potential interventions to overcome barriers to adolescents' healthy eating and physical activity. J Behav Med. 2009. October; 32 5: 491 - 502. • Too few locations, not enough information about how to access these resources – Sonneville KR, Rifas-Shiman SL, Kleinman KP, Gortmaker SL, Gillman MW, Taveras EM. Associations of obesogenic behaviors in mothers and obese children participating in a randomized trial. Obesity (Silver Spring). 2012. July; 20 7: 1449 - 145418. SESSION 5: COLLABORATIVE LEARNING PROJECT

Facilitators: Transportation Best program location would be a local and convenient school, clinic or recreation facility Some parents/guardians suggested that the program should take place right after school to reduce transportation burden and parent/guardian time. – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 SESSION 5: COLLABORATIVE LEARNING PROJECT

Facilitators: Timing • Weekday evenings and Saturday afternoons would be the best program times • Open to attending program sessions from once per month to 2 -3 days per week • Most parents/guardians wanted the program to be year-round – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 • Interviews of 10 families enrolled in a pediatric weightmanagement program indicated that reducing the intervention length would improve program engagement – Holt NL, Neely KC, Newton AS, et al. Families' perceptions of and experiences related to a pediatric weight management intervention: a qualitative study. J Nutr Educ Behav. 2015. Sep-Oct; 47 5: 427431. e 1. SESSION 5: COLLABORATIVE LEARNING PROJECT

Facilitators: Incentives • Motivational program leader • Incentives to encourage attendance, goal achievement, reward healthy behaviors Gift cards or small prizes • Many parents/guardians used monetary incentives or food rewards to promote healthy behaviors in their children – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 SESSION 5: COLLABORATIVE LEARNING PROJECT

Facilitators: Program Structure • Group-based • Include the whole family • Must be fun to encourage child participation – Staiano AE, Marker AM, Comeaux J, Frelier JM, Hsia DS, Broyles ST. Family-Based Behavioral Treatment for Childhood Obesity: Caretaker-Reported Barriers and Facilitators. Ochsner J. 2017 Spring; 17(1): 83 -92 – Sonneville KR, Rifas-Shiman SL, Kleinman KP, Gortmaker SL, Gillman MW, Taveras EM. Associations of obesogenic behaviors in mothers and obese children participating in a randomized trial. Obesity (Silver Spring). 2012. July; 20 7: 1449 - 1454. SESSION 5: COLLABORATIVE LEARNING PROJECT

Characteristics of Participants Who Did Not Complete Program • The likelihood of not completing a program (<70 % attendance) opposed to completing the program (≥ 70 % attendance) was greater for those who Attended a larger group Attended a recent program year Started the program in April or September rather than January Higher Indices of Multiple Deprivation (IMD) Score (lower SES) and higher BMI Standard Deviation Score (SDS) • These associations were weaker than programmatic characteristics – Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT

Characteristics of Participants Who Only Initiated Program • Attended only the first third of sessions More white children than non white children were more likely to attend only the first third of the session Participants in larger group size were more likely to only initiate the program Likelihood of participants only initiating increased by 18% each program year (2009 -2014) • Unknown why this occurred Participants who started the program in April and September were also more likely to only initiate the program ‒ Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT
Characteristics of Participants Who Were Late Dropouts • Late dropouts attended in first and second third of the program, but did not attend in last third • Late dropouts had high BMI SDS, compared to children who completed the program • Participants who attended in more recent program years were more likely to be late dropouts Unknown why this occurred • Participants who began a program in April were more likely to be late dropouts ‒ Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT
Characteristics of Participants Who Were Sporadic Attenders • Attended between 50%-70% of time • Compared to completers Non-white ethnicity Higher IMD (Index of multiple deprivation) Lower Socioeconomic status (SES) • In participants who were sporadic attenders, higher IMD (lower SES) = decreased attendance ‒ Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT

Change in BMI SDS • BMI SDS reduction Completers: 0. 15 ± 0. 22 units during the program (p<0. 001) Initiators: 0. 02 ± 0. 20 units Late dropouts: 0. 07 ± 0. 21 Low sporadic attenders: 0. 07 ± 0. 18 units High sporadic attenders: 0. 09 ± 0. 18 units ‒ Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT

Measures of Program Characteristics • • • Program Year Group size (≥ 20 participants or <20 participants) Age groups (separated younger/older age or mixed ages) Program length (10 weeks or 12 weeks) Session delivery day (weekday or weekend) Delivery period (More. Life programs commence in either January, April, or September). – Nobles J, Griffiths C, Pringle A, Gately P. Design programmes to maximise participant engagement: a predictive study of programme and participant characteristics associated with engagement in paediatric weight management Int J Behav Nutr Phys Act. 2016 Jul 19; 13: 76. SESSION 5: COLLABORATIVE LEARNING PROJECT

Measures of Key Factors From Other Kinds of Programs • Adult cardiac rehab program Travel distance to program was the only statistically significant factor in determining uptake Easy access to transport (63%), family support (to a lesser extent) (49%), and work flexibility (43%) were the primary enablers to attendance – De Angelis C, Bunker S, Schoo A. Exploring the barriers and enablers to attendance at rural cardiac rehabilitation programs. Aust J Rural Health. 2008 Jun; 16(3): 137 -42. SESSION 5: COLLABORATIVE LEARNING PROJECT

Potential Measures That Might Impact Program Success • Childhood social determinants of health – Avelar Rodriguez D, Toro Monjaraz EM, Ignorosa Arellano KR, Ramirez Mayans J. Childhood obesity in Mexico: social determinants of health and other risk factors. BMJ Case Rep. 2018 Mar 30; 2018. pii: bcr 2017 -223862. • Neighborhood characteristics – Johnson Thornton RL, Greiner A, Fichtenberg CM, Feingold BJ, Ellen JM, Jennings JM. Achieving a healthy zoning policy in Baltimore: results of a health impact assessment of the Trans. Form Baltimore zoning code rewrite. Public Health Rep. 2013 Nov; 128 Suppl 3: 87 -103. Erratum in: Public Health Rep. 2014 Jan-Feb; 129(1): 7 SESSION 5: COLLABORATIVE LEARNING PROJECT

Measures: First Level Contextual Factors to Consider • Transportation Distance from program Means of transportation • Own car, public transportation, depending on friends/family for rides Cost of transportation • Childcare Availability during program time • Possibly on a scale of Always-Sometimes-Never • Time conflicts with program Parents’ work hours Other family commitments Child’s school Child’s extracurricular activities • Cost Can afford fresh fruits and vegetables • Possibly on a scale of Always-Sometimes-Never SESSION 5: COLLABORATIVE LEARNING PROJECT

Contextual Factors Barriers to Healthy Weight Program Attendance Kyung E. (Kay) Rhee, MD, MSc, MA UC San Diego School of Medicine Department of Pediatrics SESSION 5: COLLABORATIVE LEARNING PROJECT
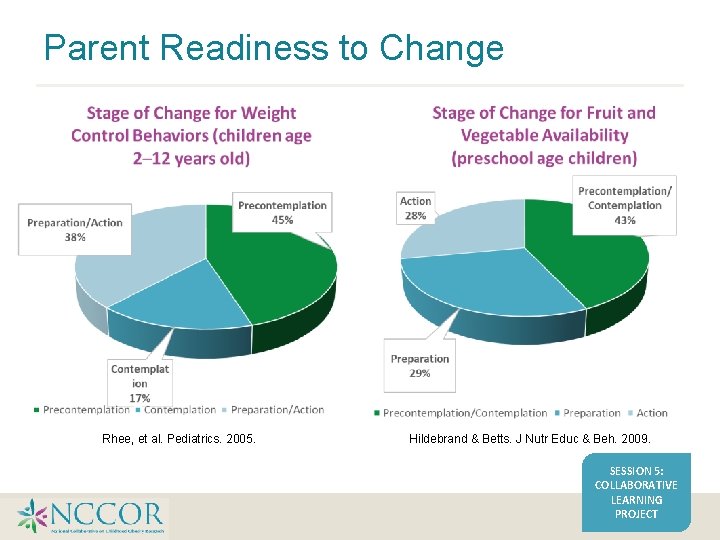
Parent Readiness to Change Rhee, et al. Pediatrics. 2005. Hildebrand & Betts. J Nutr Educ & Beh. 2009. SESSION 5: COLLABORATIVE LEARNING PROJECT
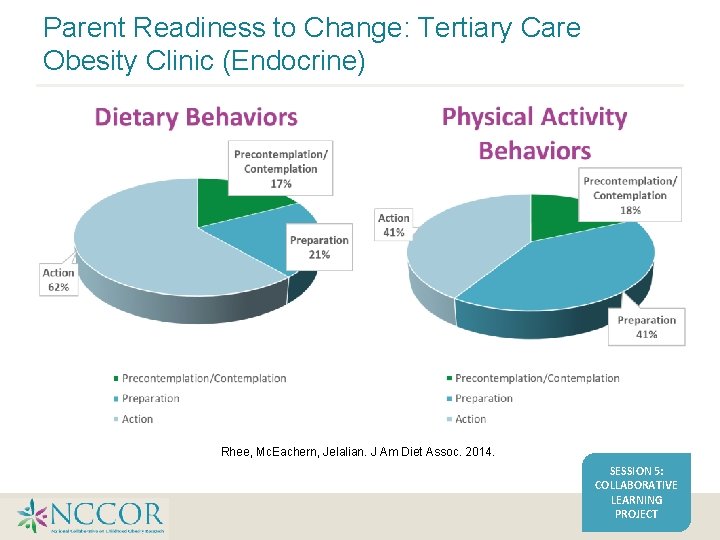
Parent Readiness to Change: Tertiary Care Obesity Clinic (Endocrine) Rhee, Mc. Eachern, Jelalian. J Am Diet Assoc. 2014. SESSION 5: COLLABORATIVE LEARNING PROJECT
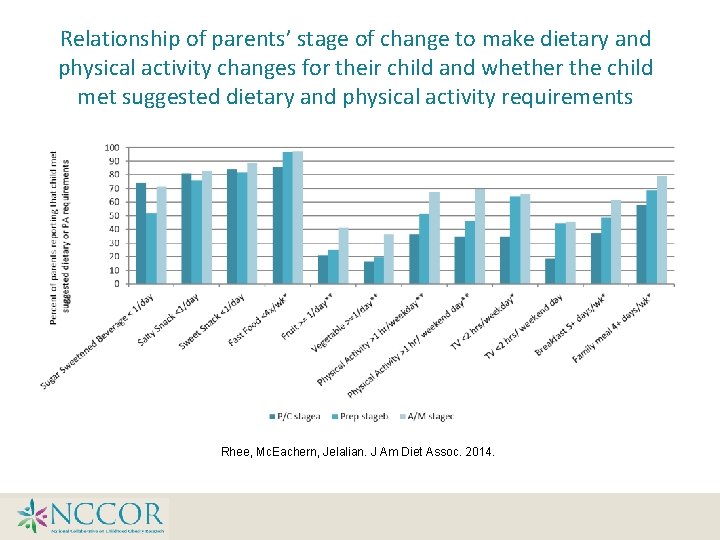
Relationship of parents’ stage of change to make dietary and physical activity changes for their child and whether the child met suggested dietary and physical activity requirements Rhee, Mc. Eachern, Jelalian. J Am Diet Assoc. 2014.

Assessing Readiness to Change How motivated are you to… ? (scale of 1– 10) Importance (scale of 1– 10) Confidence (scale of 1– 10) _________________________ 1 2 3 4 5 6 7 8 9 10 Not at all Confident/ Not Important Somewhat Confident/ Important Very Confident/ Important SESSION 5: COLLABORATIVE LEARNING PROJECT
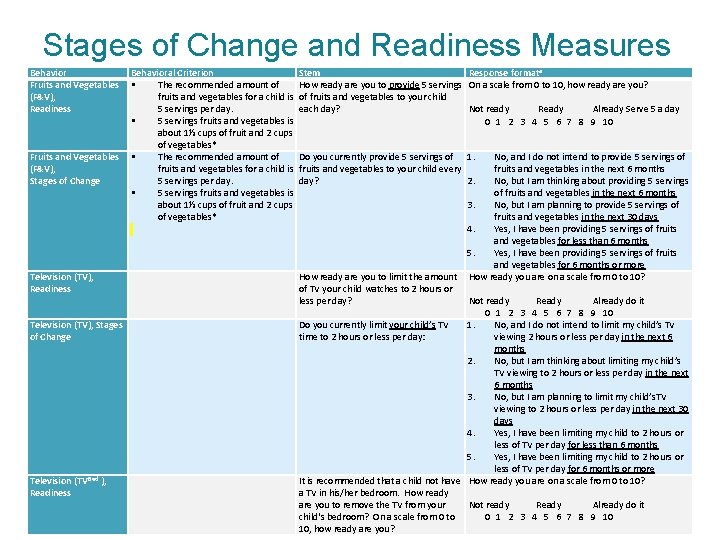
Stages of Change and Readiness Measures Behavioral Criterion Fruits and Vegetables The recommended amount of (F&V), fruits and vegetables for a child is Readiness 5 servings per day. 5 servings fruits and vegetables is about 1½ cups of fruit and 2 cups of vegetables* Fruits and Vegetables The recommended amount of (F&V), fruits and vegetables for a child is Stages of Change 5 servings per day. 5 servings fruits and vegetables is about 1½ cups of fruit and 2 cups of vegetables* Television (TV), Readiness Television (TV), Stages of Change Television (TVBed ), Readiness Stem How ready are you to provide 5 servings of fruits and vegetables to your child each day? Response formata On a scale from 0 to 10, how ready are you? Not ready Ready Already Serve 5 a day 0 1 2 3 4 5 6 7 8 9 10 Do you currently provide 5 servings of 1. fruits and vegetables to your child every day? 2. No, and I do not intend to provide 5 servings of fruits and vegetables in the next 6 months No, but I am thinking about providing 5 servings of fruits and vegetables in the next 6 months 3. No, but I am planning to provide 5 servings of fruits and vegetables in the next 30 days 4. Yes, I have been providing 5 servings of fruits and vegetables for less than 6 months 5. Yes, I have been providing 5 servings of fruits and vegetables for 6 months or more How ready are you to limit the amount How ready you are on a scale from 0 to 10? of TV your child watches to 2 hours or less per day? Not ready Ready Already do it 0 1 2 3 4 5 6 7 8 9 10 Do you currently limit your child’s TV 1. No, and I do not intend to limit my child’s TV time to 2 hours or less per day: viewing 2 hours or less per day in the next 6 months 2. No, but I am thinking about limiting my child’s TV viewing to 2 hours or less per day in the next 6 months 3. No, but I am planning to limit my child’s. TV viewing to 2 hours or less per day in the next 30 days 4. Yes, I have been limiting my child to 2 hours or less of TV per day for less than 6 months 5. Yes, I have been limiting my child to 2 hours or less of TV per day for 6 months or more It is recommended that a child not have How ready you are on a scale from 0 to 10? a TV in his/her bedroom. How ready are you to remove the TV from your Not ready Ready Already do it child's bedroom? On a scale from 0 to 0 1 2 3 4 5 6 7 8 9 10 10, how ready are you?
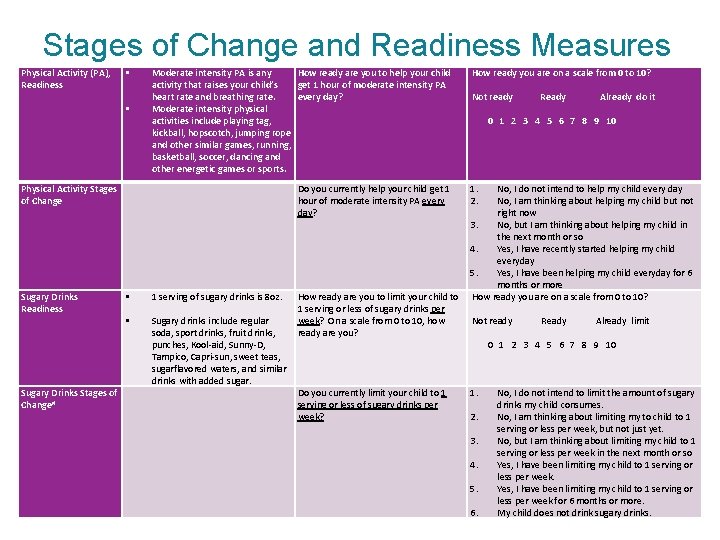
Stages of Change and Readiness Measures Physical Activity (PA), Readiness Physical Activity Stages of Change Sugary Drinks Readiness Sugary Drinks Stages of Change# Moderate intensity PA is any activity that raises your child’s heart rate and breathing rate. Moderate intensity physical activities include playing tag, kickball, hopscotch, jumping rope and other similar games, running, basketball, soccer, dancing and other energetic games or sports. How ready are you to help your child get 1 hour of moderate intensity PA every day? How ready you are on a scale from 0 to 10? Not ready Ready Already do it Do you currently help your child get 1 hour of moderate intensity PA every day? 1. 2. 0 1 2 3 4 5 6 7 8 9 10 No, I do not intend to help my child every day No, I am thinking about helping my child but not right now 3. No, but I am thinking about helping my child in the next month or so 4. Yes, I have recently started helping my child everyday 5. Yes, I have been helping my child everyday for 6 months or more 1 serving of sugary drinks is 8 oz. How ready are you to limit your child to How ready you are on a scale from 0 to 10? 1 serving or less of sugary drinks per Sugary drinks include regular week? On a scale from 0 to 10, how Not ready Ready Already limit soda, sport drinks, fruit drinks, ready are you? punches, Kool-aid, Sunny-D, 0 1 2 3 4 5 6 7 8 9 10 Tampico, Capri-sun, sweet teas, sugarflavored waters, and similar drinks with added sugar. Do you currently limit your child to 1 1. No, I do not intend to limit the amount of sugary serving or less of sugary drinks per drinks my child consumes. week? 2. No, I am thinking about limiting my to child to 1 serving or less per week, but not just yet. 3. No, but I am thinking about limiting my child to 1 serving or less per week in the next month or so 4. Yes, I have been limiting my child to 1 serving or less per week. 5. Yes, I have been limiting my child to 1 serving or less per week for 6 months or more. 6. My child does not drink sugary drinks.
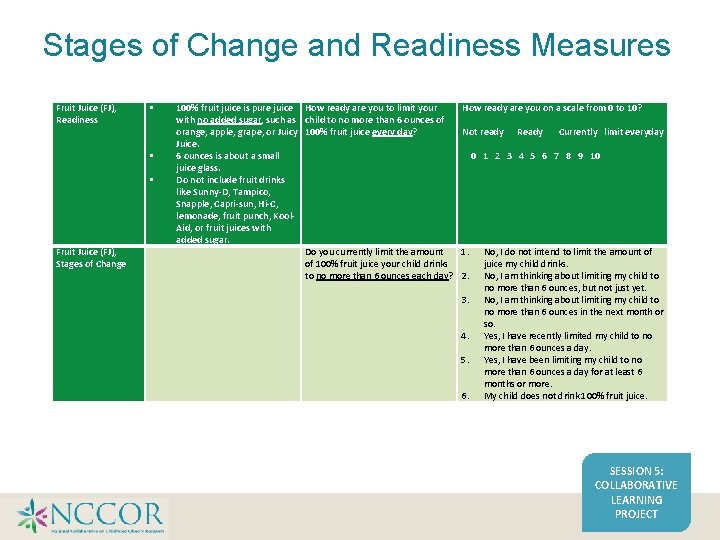

Stages of Change and Readiness Measures Fruit Juice (FJ), Readiness Fruit Juice (FJ), Stages of Change 100% fruit juice is pure juice How ready are you to limit your with no added sugar, such as child to no more than 6 ounces of orange, apple, grape, or Juicy 100% fruit juice every day? Juice. 6 ounces is about a small juice glass. Do not include fruit drinks like Sunny-D, Tampico, Snapple, Capri-sun, Hi-C, lemonade, fruit punch, Kool. Aid, or fruit juices with added sugar. Do you currently limit the amount of 100% fruit juice your child drinks to no more than 6 ounces each day? How ready are you on a scale from 0 to 10? Not ready Ready Currently limit everyday 0 1 2 3 4 5 6 7 8 9 10 1. 2. 3. 4. 5. 6. No, I do not intend to limit the amount of juice my child drinks. No, I am thinking about limiting my child to no more than 6 ounces, but not just yet. No, I am thinking about limiting my child to no more than 6 ounces in the next month or so. Yes, I have recently limited my child to no more than 6 ounces a day. Yes, I have been limiting my child to no more than 6 ounces a day for at least 6 months or more. My child does not drink 100% fruit juice. SESSION 5: COLLABORATIVE LEARNING PROJECT
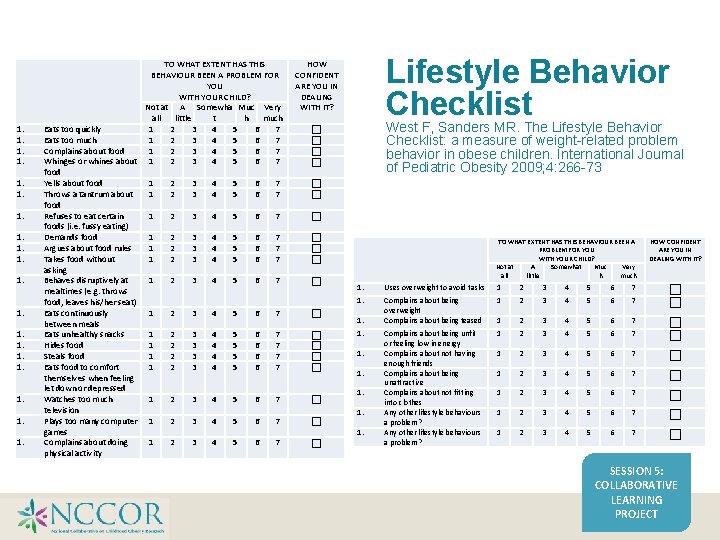
1. 1. 1. TO WHAT EXTENT HAS THIS BEHAVIOUR BEEN A PROBLEM FOR YOU WITH YOUR CHILD? Not at A Somewha Muc Very all little t h much Eats too quickly 1 2 3 4 5 6 7 Eats too much 1 2 3 4 5 6 7 Complains about food 1 2 3 4 5 6 7 Whinges or whines about 1 2 3 4 5 6 7 food Yells about food 1 2 3 4 5 6 7 Throws a tantrum about 1 2 3 4 5 6 7 food Refuses to eat certain 1 2 3 4 5 6 7 foods (i. e. fussy eating) Demands food 1 2 3 4 5 6 7 Argues about food rules 1 2 3 4 5 6 7 Takes food without 1 2 3 4 5 6 7 asking Behaves disruptively at 1 2 3 4 5 6 7 mealtimes (e. g. throws food, leaves his/her seat) Eats continuously 1 2 3 4 5 6 7 between meals Eats unhealthy snacks 1 2 3 4 5 6 7 Hides food 1 2 3 4 5 6 7 Steals food 1 2 3 4 5 6 7 Eats food to comfort 1 2 3 4 5 6 7 themselves when feeling let down or depressed Watches too much 1 2 3 4 5 6 7 television Plays too many computer 1 2 3 4 5 6 7 games Complains about doing 1 2 3 4 5 6 7 physical activity Lifestyle Behavior Checklist Lifestyle Behavior HOW CONFIDENT ARE YOU IN DEALING WITH IT? West F, Sanders MR. The Lifestyle Behavior Checklist: a measure of weight-related problem behavior in obese children. International Journal of Pediatric Obesity 2009; 4: 266 -73 Checklist West F, Sanders MR. The Lifestyle Behavior Checklist: a measure of weight-related problem behavior in obese children. International Journal of Pediatric Obesity 2009; 4: 266 -73 HOW CONFIDENT ARE YOU IN DEALING WITH IT? 1. Uses overweight to avoid tasks 1 2 3 4 5 6 7 1. Complains about being overweight Complains about being teased 1 2 3 4 5 6 7 Complains about being unfit or feeling low in energy Complains about not having enough friends Complains about being unattractive Complains about not fitting into clothes Any other lifestyle behaviours a problem? 1 2 3 4 5 6 7 1 2 3 4 5 6 7 1. 1. TO WHAT EXTENT HAS THIS BEHAVIOUR BEEN A PROBLEM FOR YOU WITH YOUR CHILD? Not at A Somewhat Muc Very all little h much SESSION 5: COLLABORATIVE LEARNING PROJECT
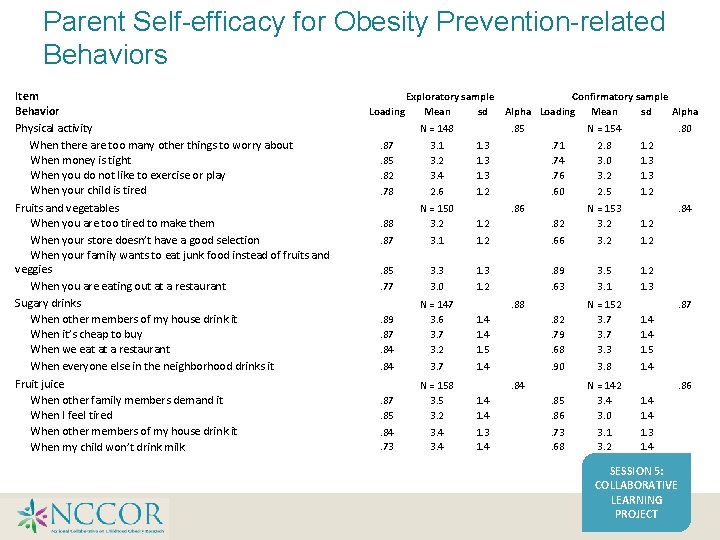
Parent Self-efficacy for Obesity Prevention-related Behaviors Parent Self-efficacy for obesity prevention related Exploratory sample Confirmatory sample Loading Mean sd Alpha behaviors N = 148 . 85 N = 154 . 80 Item Behavior Physical activity When there are too many other things to worry about When money is tight When you do not like to exercise or play When your child is tired Fruits and vegetables When you are too tired to make them When your store doesn’t have a good selection When your family wants to eat junk food instead of fruits and veggies When you are eating out at a restaurant Sugary drinks When other members of my house drink it When it’s cheap to buy When we eat at a restaurant When everyone else in the neighborhood drinks it Fruit juice When other family members demand it When I feel tired When other members of my house drink it When my child won’t drink milk . 87. 85. 82. 78 3. 1 3. 2 3. 4 2. 6 1. 3 1. 2 . 71. 74. 76. 60 2. 8 3. 0 3. 2 2. 5 1. 2 1. 3 1. 2 . 88 N = 150 3. 2 1. 2 . 86 . 82 N = 153 3. 2 1. 2 . 84 . 87 3. 1 1. 2 . 66 3. 2 1. 2 . 85 3. 3 1. 3 . 89 3. 5 1. 2 . 77 3. 0 1. 2 . 63 3. 1 1. 3 . 89. 87. 84 N = 147 3. 6 3. 7 3. 2 1. 4 1. 5 . 88 . 82. 79. 68 N = 152 3. 7 3. 3 1. 4 1. 5 . 87 . 84 3. 7 1. 4 . 90 3. 8 1. 4 . 87. 85 N = 158 3. 5 3. 2 1. 4 . 84 . 85. 86 N = 142 3. 4 3. 0 1. 4 . 86 . 84. 73 3. 4 1. 3 1. 4 . 73. 68 3. 1 3. 2 1. 3 1. 4 SESSION 5: COLLABORATIVE LEARNING PROJECT
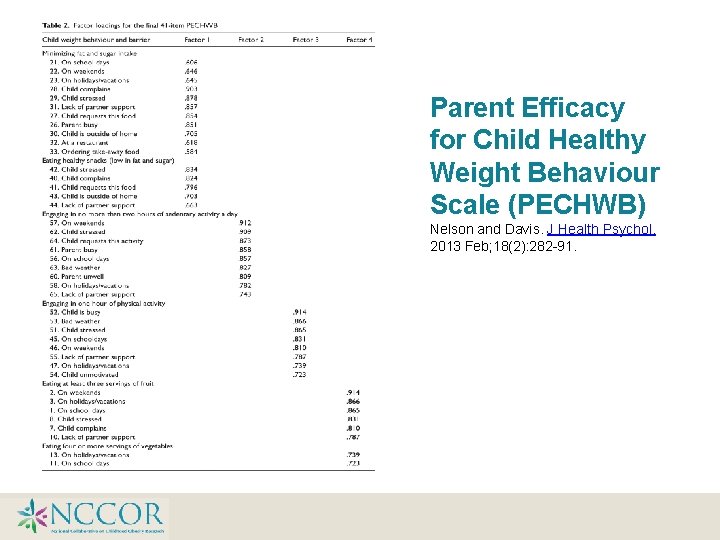
Parent Efficacy for Child Healthy Weight Behaviour Scale (PECHWB) Nelson and Davis. J Health Psychol. 2013 Feb; 18(2): 282 -91.
Weight Loss SELF-EFFICACY and MOTIVATION Factors influencing readiness, confidence, and self-efficacy

Physician Influence on Confidence and Readiness • Increased confidence if clinicians assessed: • Parent confidence in making overweight-related changes (β = 0. 73 [95% CI: 0. 04 to 1. 42]) • Parent readiness to change (β = 0. 80 [95% CI: 0. 10 to 1. 49]) (Arsenault, et al, 2014) • Increased readiness to make a change if child’s doctor commented that “child’s weight was a health problem” (OR 10. 80 (95% CI: 3. 78– 30. 86)) (Rhee, et al, 2005) • Increased odds of being in the Action/Maintenance SOC if providers discussed strategies for improved dietary behaviors (OR 2. 1 (1. 0 – 4. 0)) (Rhee, et al, 2014) SESSION 5: COLLABORATIVE LEARNING PROJECT
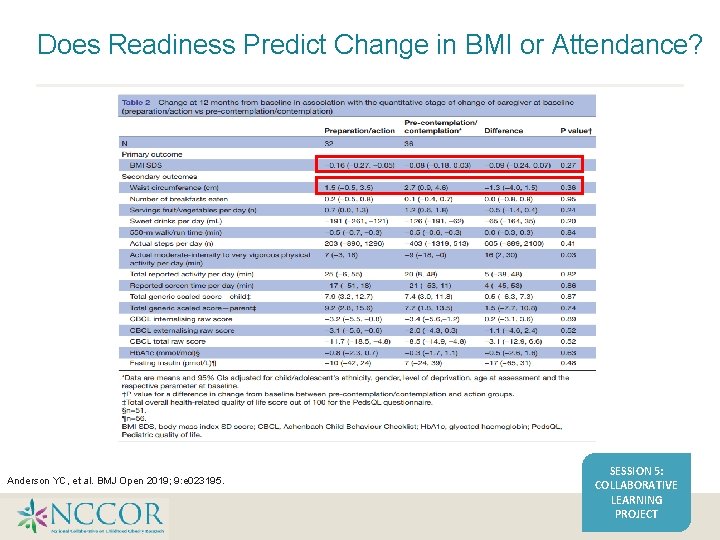

Does Readiness Predict Change in BMI or Attendance? Anderson YC, et al. BMJ Open 2019; 9: e 023195. SESSION 5: COLLABORATIVE LEARNING PROJECT
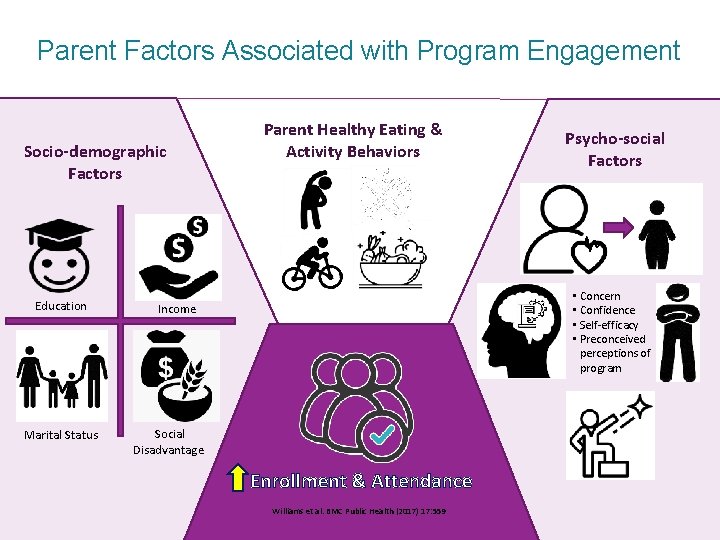
Parent Factors Associated with Program Engagement Socio-demographic Factors Education Marital Status Parent Healthy Eating & Activity Behaviors Psycho-social Factors • Concern • Confidence • Self-efficacy • Preconceived perceptions of program Income Social Disadvantage Enrollment & Attendance Williams et al. BMC Public Health (2017) 17: 559
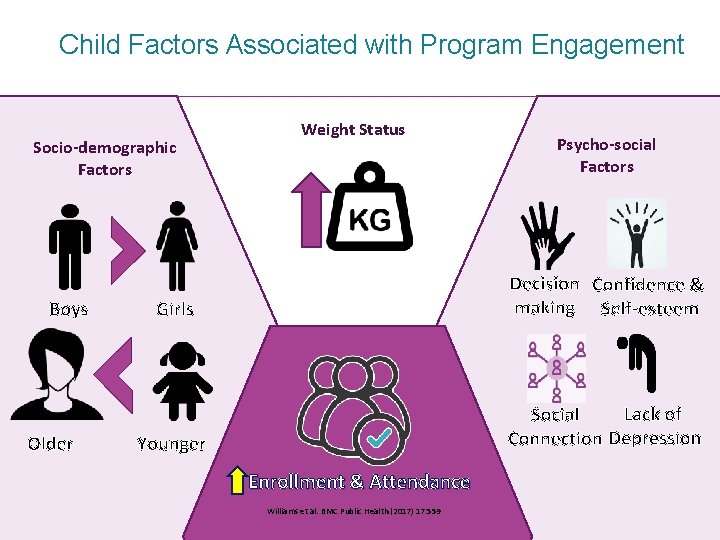
Child Factors Associated with Program Engagement Socio-demographic Factors Weight Status Psycho-social Factors Decision Confidence & making Self-esteem Boys Girls Lack of Social Connection Depression Older Younger Enrollment & Attendance Williams et al. BMC Public Health (2017) 17: 559
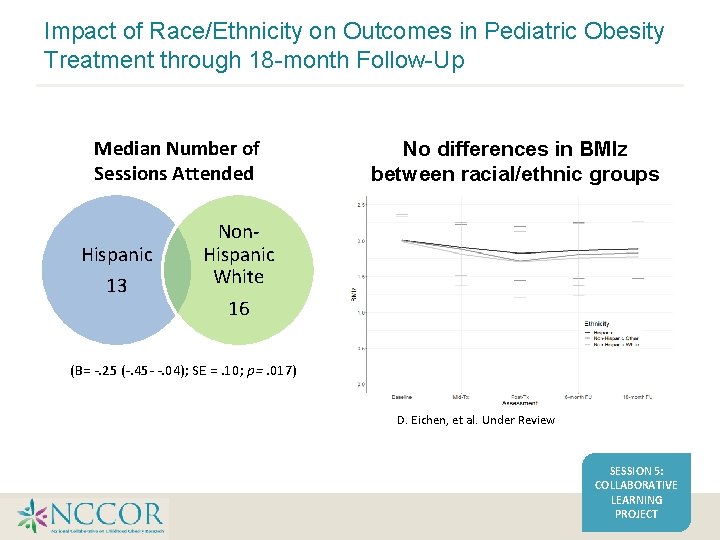
Impact of Race/Ethnicity on Outcomes in Pediatric Obesity Treatment through 18 -month Follow-Up Median Number of Sessions Attended Hispanic 13 No differences in BMIz between racial/ethnic groups Non. Hispanic White 16 (B= -. 25 (-. 45 - -. 04); SE =. 10; p=. 017) D. Eichen, et al. Under Review SESSION 5: COLLABORATIVE LEARNING PROJECT

Program Factors Associated with Program Engagement - Self-referred - Professional referral - Public ads Distance & transportation barriers Program factors Family support Facilitator familiarity with program materials Timing of program/ Scheduling conflicts Size of group & other unmet expectations Williams et al. BMC Public Health (2017) 17: 559
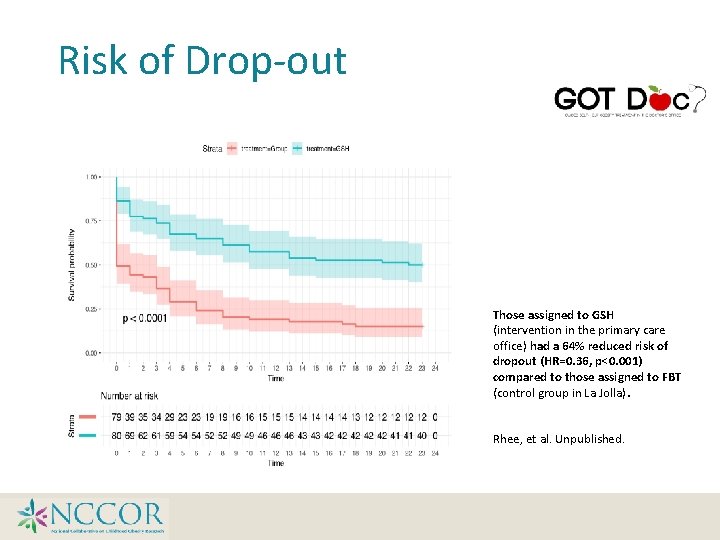
Risk of Drop-out Those assigned to GSH (intervention in the primary care office) had a 64% reduced risk of dropout (HR=0. 36, p<0. 001) compared to those assigned to FBT (control group in La Jolla). Rhee, et al. Unpublished.
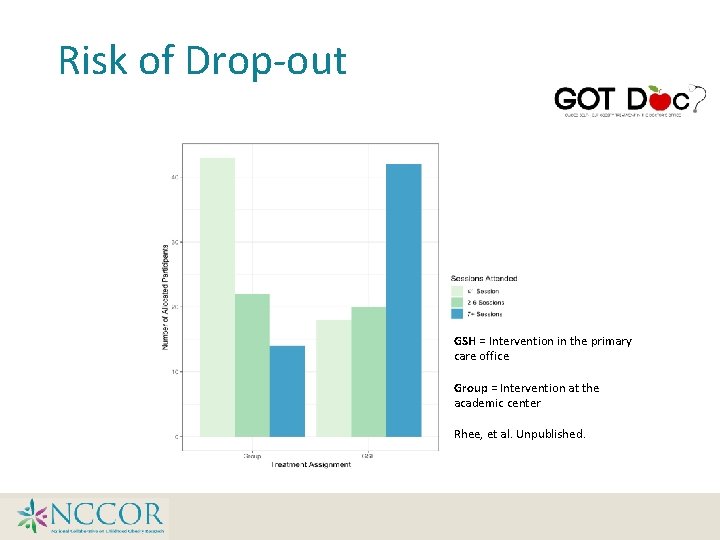
Risk of Drop-out GSH = Intervention in the primary care office Group = Intervention at the academic center Rhee, et al. Unpublished.
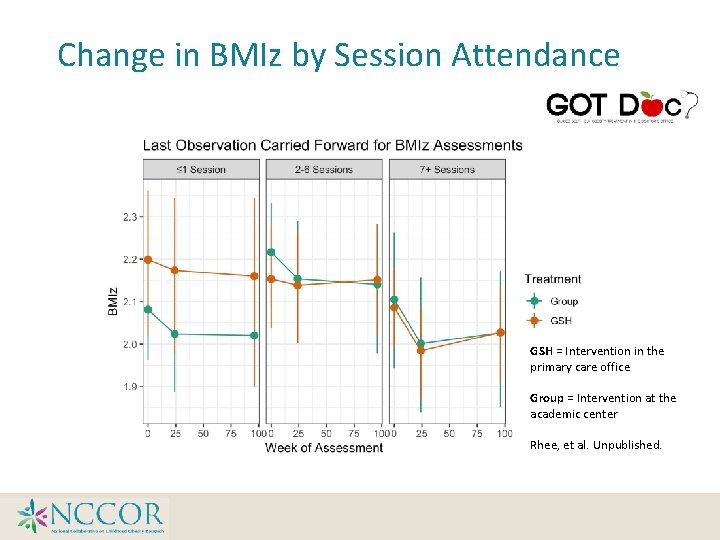
Change in BMIz by Session Attendance GSH = Intervention in the primary care office Group = Intervention at the academic center Rhee, et al. Unpublished.

Measures: First Level Contextual Factors to Consider • Readiness to change • Confidence • Self-efficacy • Importance or concern • Demographic characteristics • Sex/gender • Race/ethnicity • Income/education • Food insecurity • Family structure (single parent vs. two-parent household) • Immigration status (cultural factors) • Personal characteristics • Mental health (depression, anxiety) • Abuse history • Executive functioning or problem-solving ability • Social support (informational, emotional, functional) • Family functioning (connectedness, organization, chaos level) • Social connection with • Group leaders and behavioral/health coaches • Other group members • Alignment of program expectations Understand who your population is and what their barriers are! SESSION 5: COLLABORATIVE LEARNING PROJECT

Parent Readiness to Change References Pediatrics. 2005 Jul; 116(1): e 94 -101. Factors associated with parental readiness to make changes for overweight children. Rhee KE, De Lago CW, Arscott-Mills T, Mehta SD, Davis RK. J Acad Nutr Diet. 2014 Oct; 114(10): 1601 -10. doi: 10. 1016/j. jand. 2014. 029. Epub 2014 Jun 20. Parent readiness to change differs for overweight child dietary and physical activity behaviors. Rhee KE, Mc. Eachern R, Jelalian E. J Nutr Educ Behav. 2015 Mar-Apr; 47(2): 134 -42. e 1. doi: 10. 1016/j. jneb. 2014. 11. 003. Epub 2015 Jan 8. Validation of 5 stage-of-change measures for parental support of healthy eating and activity. Wright JA, Whiteley JA, Laforge RG, Adams WG 4 Berry D, Friedman RH. Int J Behav Nutr Phys Act. 2014 Apr 22; 11: 53. doi: 10. 1186/1479 -5868 -11 -53. Assessing parental self-efficacy for obesity prevention related behaviors. Wright JA, Adams WG, Laforge RG, Berry D, Friedman RH. J Nutr Educ Behav. 2009 Mar-Apr; 41(2): 110 -9. doi: 10. 1016/j. jneb. 2008. 09. 007. Assessment of stage of change, decisional balance, self-efficacy, and use of processes of change of low-income parents for increasing servings of fruits and vegetables to preschool-aged children. Hildebrand DA, Betts NM. Acad Pediatr. 2014 Sep-Oct; 14(5): 456 -62. doi: 10. 1016/j. acap. 2014. 03. 001. Epub 2014 May 6. Parents' obesity-related behavior and confidence to support behavioral change in their obese child: data from the STAR study. Arsenault LN, Xu K, Taveras EM, Hacker KA. SESSION 5: COLLABORATIVE LEARNING PROJECT
- Slides: 49