CONTEXT MATTERS Using home visits to explore social



















![Student perspectives …[The project] opened my eyes to what a patient goes through. I Student perspectives …[The project] opened my eyes to what a patient goes through. I](https://slidetodoc.com/presentation_image_h2/a18518c7fcc6b0b0eb5bddf9ad244d3b/image-22.jpg)








- Slides: 30

CONTEXT MATTERS Using home visits to explore social determinants of health Shipra Bansal, MD and Lisa Hardy, Ph. D January

AT Still University - SOMA Kirksville, MO campus is the first DO campus in the nation Sister campus in Mesa, AZ opened in 2007 with the mission of training primary care providers in underserved settings Students spend their first year in Mesa and then are sent to one of 11 community campuses nationwide for the remainder of their medical school training North Country in Flagstaff, AZ is a CHC-based site with 10 2 nd year students each year � Students live and study within the CHC community � Spend 8 hours a week in clinical activities

Background There is a nationwide awareness of the need for physicians to better address the social context our patients live in – often referred to as the Social Determinants of Health (SDH)

Background AAMC February 2012 decision to include social and behavioral sciences on the MCAT “In addition to medical knowledge, a wellrounded physician must understand the cultural, familial, economic, and demographic factors that affect health and disease…” AAMC President and CEO

Background Robert Wood Johnson Foundation survey December 2011 1000 primary care physicians across the nation 85% of physicians surveyed said unmet social needs directly lead to worse health 85% of physicians surveyed said patients’ social needs are as important to address as their medical needs 80% of physicians surveyed said they are not confident in their capacity to address their patients’ social needs

Home Visits The need for incorporating SDH in medical practice has been well documented How will medical schools implement adequate curriculum in this area? Used home visits as a way to help 2 nd year students develop skills in understanding and addressing SDH.

What are social determinants? Social and environmental factors that can impact a patients health Income Race Environmental surroundings Social Position Gender Access to care Support network Genetic Behavioral

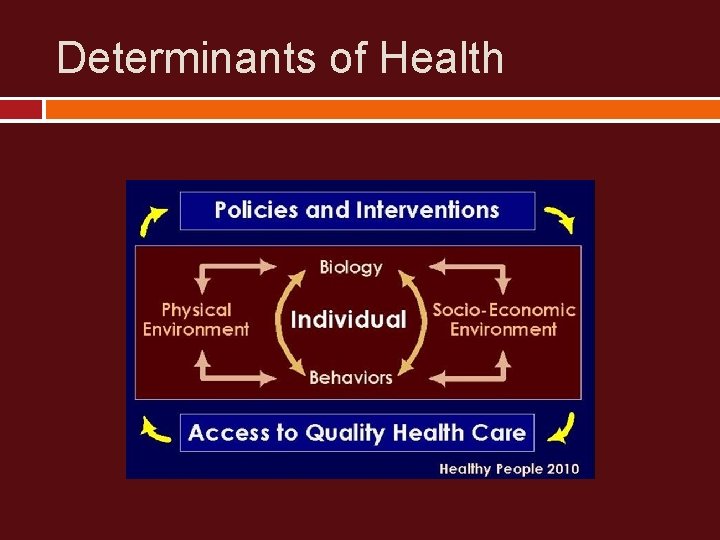
Determinants of Health

Project overview Different perspectives: � physician educator � public health professional � medical anthropologist Piloted with nine 2 nd year medical students who: � Enrolled a chronically ill patient � Conducted two home visits � Analyzed findings and searched for resources

Project objectives Allow students to: 1. View patients’ biological health within a social context. 2. Better understand be able to elicit core causes of what has traditionally been framed as “non-compliance. ” 3. Develop skills in addressing social context. 4. Increase their awareness of potential models that may address the rising costs of healthcare

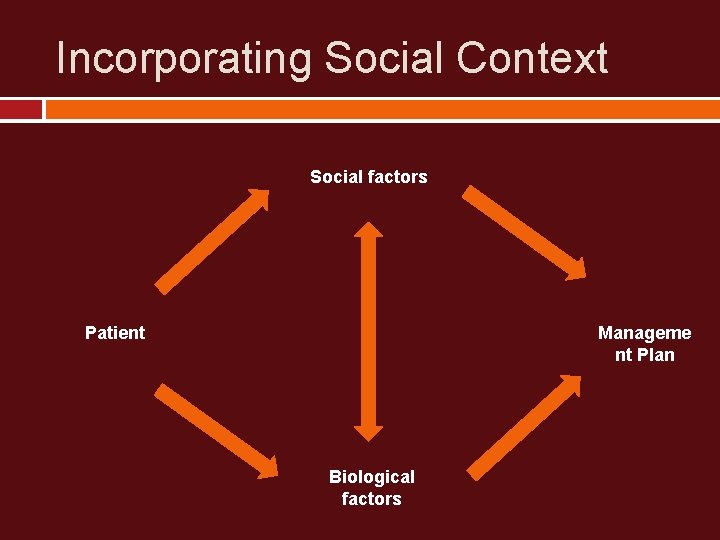
Incorporating Social Context Social factors Patient Manageme nt Plan Biological factors

Methods Each student chose a chronic diabetic or pain patient who had multiple visits to our CHC in the past 6 months but whose condition was still not well-controlled. � Students obtained consent from the patient and approval from PCP. � Patients agreed to filling out the WHO questionnaire on quality of life and two home visits � Patients were aware that any information presented to the student may be shared with the PCP

Methods Pre-visit training � What are Social determinants and how do they impact health � Ethics � Building rapport � What do you ask and how do you listen (semistructured interviewing techniques)

Methods First home visit � Students, accompanied by a medical anthropologist, conducted interviews to help understand the patient as a whole person. � How has the illness affected the person’s life and how has the person’s SDH affected the illness? � What are the patient’s own goals, strengths and obstacles?

Methods Post-visit discussion � Used student observations and notes from student and anthropologist. � A ‘web’ was drawn for several patients, that looked at the intertwining issues that have contributed to the patient’s current health status � Brainstorming on how some of these social determinants could be addressed

Web of Meaning

Methods Second home visit � Students, accompanied by a medical educator, presented some of the community resources or information they found to the patient � Worked collaboratively with the patient to develop a plan to address patient needs Pre- and post-visit surveys � Student’s used the WHO brief quality of life survey to assess the impact their visit had on patients � The pre-survey was done during the first visit and the post-survey was done at least 3 weeks after the 2 nd visit

Student Interventions “Joe” is a diabetic truck driver with intermittent Medicaid coverage who was very motivated to control his sugars without insulin so he could continue to drive Trucker x 20 years Intermittant access lead to poor sugar control and eventual amputation of big toe Amputation compromised ability to continue driving Off medicaid and without a job, gained weight Wanted to exercise to lose weight but felt limited Students found exercises that do not require weight bearing but would promote strengthening and aerobic exercise

Student Interventions “Marie” is a 38 year old female living in a trailer home who c/o constant unexplained respiratory problems including recurrent sinusitis and SOB. Despite a negative pulmonology work-up, she requires oxygen. Students obtained a referral for a free APS audit for home to help explore her very high heating bill and poor air quality inside the home

Student Interventions “Phil” is a very thin 62 year old male who has been suffering from coccygeal pain for 2 years after being on a snow blower for hours clearing snow. Steroid injections for the pain have not worked and the patient has been reluctant to take heavy pain medications His significant anxiety and pain has prevented him from holding a steady job. He now skips meals regularly so he will have enough money for firewood and other expenses. Students found information on community programs to provide firewood to the patient for free

Other Student Interventions…. Bringing in culturally appropriate recipes for a Latina diabetic and her son to try Finding websites that would allow a patient to obtain her insulin for free Finding alternative and reduced-fare transportation for a patient on oxygen without a car and who relied only on walking
![Student perspectives The project opened my eyes to what a patient goes through I Student perspectives …[The project] opened my eyes to what a patient goes through. I](https://slidetodoc.com/presentation_image_h2/a18518c7fcc6b0b0eb5bddf9ad244d3b/image-22.jpg)
Student perspectives …[The project] opened my eyes to what a patient goes through. I haven’t had to deal with anything major in my life. I don’t know what it’s like on a personal level. It opened my eyes to some of those things. Now I know options and directions to help. What I took away is an opportunity to delve and to explore things outside of the clinic. Psychosocial and biological factors will help one other thing…the traditional model of health visit isn’t making these people better. This approach can help these people in some ways you can’t effectively address or be aware of… in a 15 to 20 minute visit. [This project] helped me be aware of community programs for a patient with no insurance …calling pharmacies…becoming more aware.

Analysis Both qualitative and quantitative analysis is being done So far, three major themes have surfaced

Findings - Changes in Anticipated Practice 7 out of 9 students reported that this project “changed the way [they] would practice medicine. ”

Possible Ongoing Impact At least one student has been thoughtful about the teachings from the project in a deep and lasting way. Months after finishing the project, he wrote to project leads to discuss the impact of family relationships and social networks on patient health and wellbeing. He has already conducted similar home visits as part of his National Health Service Corp SEARCH project in his 3 rd year.

Findings – Incorporating SDH When given a scenario in a pre- and postquestionnaire asking how they would address health problems, 7 of 9 students increased the number of interventions they thought would be appropriate to take with patients.

Findings – “Floundering” Students had a difficult time shifting their perspective in a way that one student called “floundering. ” They were pulled toward asking the patients only medical questions even through the interview was designed to be inductive and broadly focused. Students reported this discomfort. The observation of floundering for students may be precisely the space where they shifted perspective and changed the way they understood patients. Instead of a negative aspect of the project, this discomfort may have been the most important part of their learning. They asked themselves to shift perspective into an area that made them uncomfortable.

Next steps � We plan to conduct follow-up assessment after one and possibly two years to assess the lasting impact the project had on medical student professional development and practice. � We hope to repeat the project with future 2 nd years

Discussion Is this project enough? � Can medical schools incorporate a learning module such as this to help students address SDH, or must there be a bigger paradigm shift in medical education?

References Mc Ginnis, Russo and Knickman. “The Case for More Active Policy Attention to Health Promotion” Health Affairs. 2002. Robert Wood Johnson Foundation. Health Care’s Blind Side: The Overlooked Connection between Social Needs and Good Health – A summary of findings from a survey of America’s physicians. Survey by Harris Interactive. December 2011. Gawande, Atul. “The Hot Spotters - Can we lower medical costs by giving the neediest patients better care? ” The New Yorker. January 24, 2001. Health Leads website: http: //healthleadsusa. org/what-we-do/our-model/ California Newsreel with Vital Pictures (producers). 2008. Unnatural Causes…Is Inequity Making Us Sick? Segment entitled, In Sickness and In Wealth [DVD]. United States.