Contents o o o Introduction History Tracheal Anomaly































- Slides: 46


Contents o o o Introduction History Tracheal Anomaly Bronchial Anomaly Lung Bud Anomaly

Introduction o o o o Arrested development, stillbirth, die after delivery Dyspnea and cyanosis at birth Feeding problem, respiratory infection Developmental delay, activity limitation Diagnosis : P/E, CXR, CT, MRI, echo, endoscopy Speed of diagnosis : critical Prenatal diagnosis : may opt for

History o o o Fontanus (1639) lung cyst Huber (1777) sequestration Mid -1800 s sequestration Gladstone (1917) sequestration Koontz (1925) disease Reinhoff (1933) correction An infant with a Intralobar Extralobar Theory of Congenital cystic lung First surgical

Tracheal Anomaly o o Tracheal Agenesis Tracheal Atresia Congenital Tracheal Stenosis Tracheomalacia

Tracheal Agenesis, Atresia § § § Partial or complete absence of trachea Survivor : rare Type I : Trachea originate from esophagus Type II : Carina originate from esophagus Type III : Main bronchus originate from esophagus

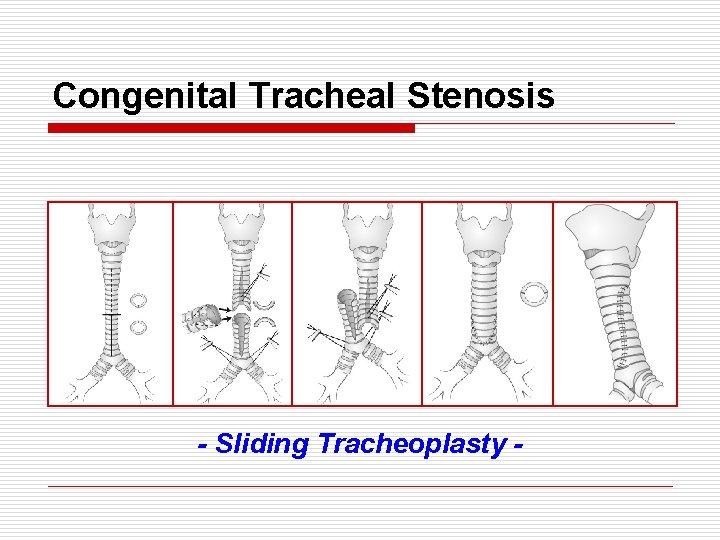
Congenital Tracheal Stenosis o o o o o Type I : full length stenosis Type II : funnel-shaped stenosis Type III : segmental stenosis of lower trachea Stenotic lesions : complete cartilaginous rings Pulmonary vascular sling or vascular ring : 50 % Sx : wheezing, stridor Dx : CT, bronchoscopy, echo Tx : partial tracheal resection and reconstruction Reconstruction : sliding tracheoplasty, pericardium, costal cartilage, aortic homograft, tracheal autograft Long-term outcome after resection : normal growth

Congenital Tracheal Stenosis - Sliding Tracheoplasty -

Tracheomalacia o o o o o Acquired (cartilage degeneration) > Congenital Acquired : vascular sling or ring, inflammation, tumor Expiration : collapse of weakened cartilage Inspiration : maintained patency Not usually manifest at birth Worsens as grows : several weeks of life Acute apnea (dying spell) : most severe presentation Improved with age in most cases Mild : observation Severe : stent, tracheostomy, aortopexy

Bronchial Anomaly o o o o o Bronchial Atresia Congenital Bronchiectasis Tracheobronchomegaly Laryngotracheoesophageal Cleft Tracheobronchial Esophageal Fistula Bronchobiliary fistula Bronchopulmonary Foregut Malformation Sequestration Azygos Lobe Bronchogenic Cyst

Bronchial Atresia o o o Lung tissue distal to the bronchial atresia expand Lung tissue become emphysematous through the ‘pore of Kohn’ Respiratory distress : 4 days ~ several weeks Segmental bronchus > lobar bronchus LUL > LLL > RUL Tx : lobectomy, segmentectomy (recurrent and serious infection, increasing size of translucent lung)

Congenital Bronchiectasis o o o Abnormal dilation of bronchus or bronchiole Ex : failure of mesenchyme to differentiate into cartilage and muscle Tx : Segmentectomy, lobectomy, pneumonectomy (localized symptomatic bronchiectasis)

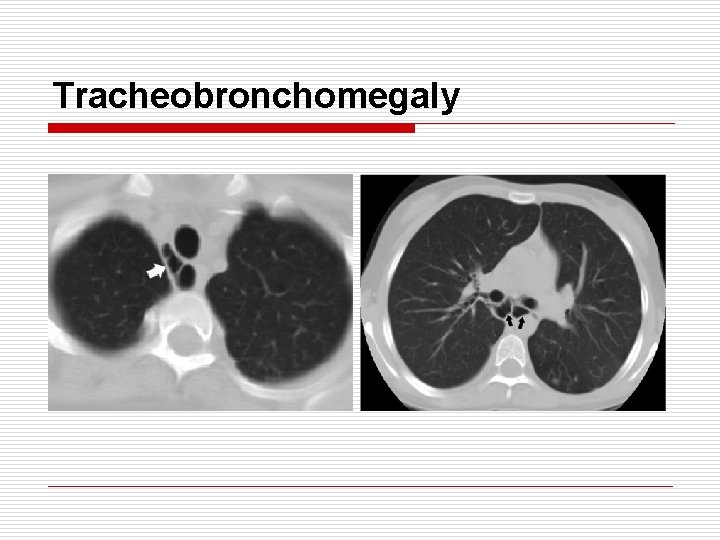
Tracheobronchomegaly o o o o Atrophy of elastic tissue and smooth muscle of trachea and bronchus Excessive dilatation of trachea and main bronchus Airway dilatation : continue to 3 rd-order subdivision Sx : mucus retention, recurrent infection, persistent cough Usually men : 3 rd ~ 4 th decade Surgical role : absent Tx : Stent, T-tube (provide significant palliation)

Tracheobronchomegaly

Laryngotracheoesophageal Cleft o o Failure of esophagus to separate from the laryngotrachea Sx : toneless cry, choke with feeding Dx : barium study, endoscopy Tx : gastrostomy, fistula division, repair of esophagus and larynx

Tracheobronchial Esophageal Fistula o o o o o Most common anomaly of the trachea : 2. 4/10, 000 Type A : esophageal atresia without TEF Type B : esophageal atresia with proximal TEF Type C : esophageal atresia with distal TEF : 87% Type D : esophageal atresia with proximal and distal TEF Type E : TEF without esophageal atresia Large air in stomach Sx : feeding difficulty, excessive slaivation, pneumonia Dx : failure of nasogastric tube passage

Bronchobiliary Fistula o o o Sx : productive green sptum, dyspnea, chronic cough RML, Rt. main bronchus : most frequently involved Drain : left hepatic ductal system Dx : bronchoscopy, bronchography, biliary scan Tx : division of fistula (as close to the airway as possible)

Bronchopulmonary Foregut Malformation o o o Abnormal communication between normal lung and esophagus RLL, LLL : most commonly affected Fistula almost always tracking to lower esophagus Dx : esophagogram Tx : lobectomy due to chronic infection resection of fistulous communication repair of esophageal defect

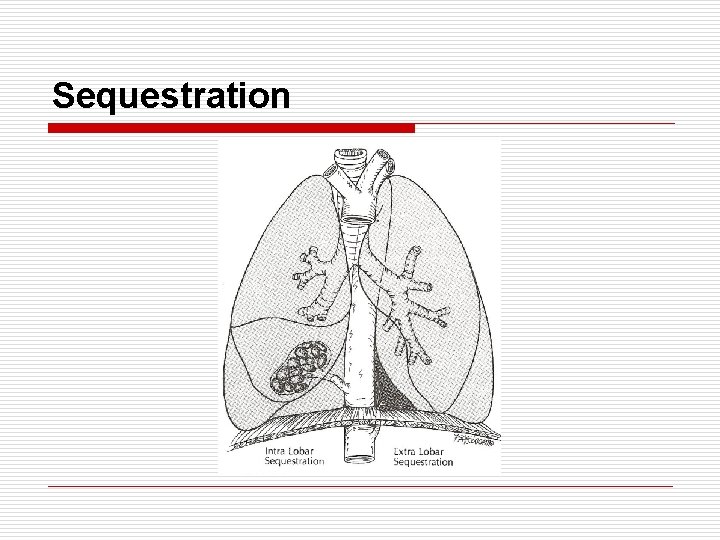
Sequestration o o o o o Nonfunctioning accessory tracheobronchial bud Lack of connection with normal bronchus Incidence : 1/1000 Arterial supply : systemic Venous drainage : systemic or pulmonary Arterial origin level : inferior pulmonary ligament Arterial size : < 1 mm (as large as 2. 5 mm) Location : base of lung ILS (75%) : share same pleural investment as normal parenchyma ELS (25%) : surrounded by their own pleura

Sequestration

Sequestration o o o Dx : prenatal US, postnatal CT, angiography, MRI Early complication : pulmonary hypoplasia and compression : associated anomalies - congenital diaphragmatic hernia - tracheoesophageal fistula - foregut duplication Late complication : high-output heart failure due to systemic blood supply : up to 50% or more of the total cardiac output in infant : hemoptysis and congestive heart failure in young adult

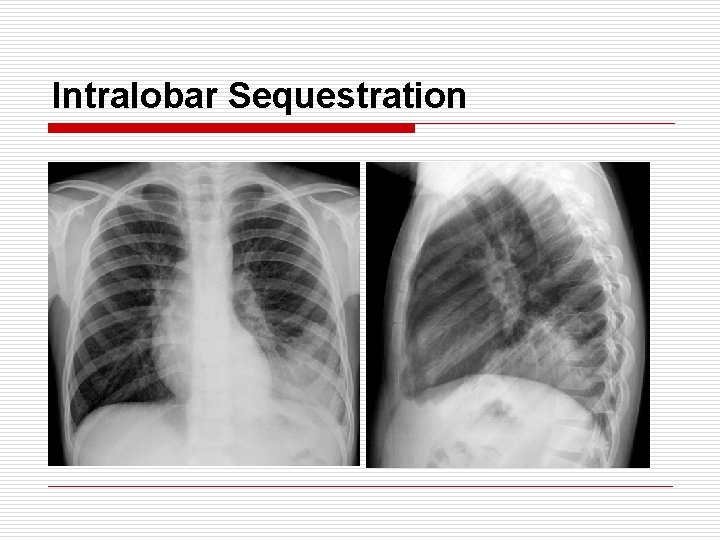
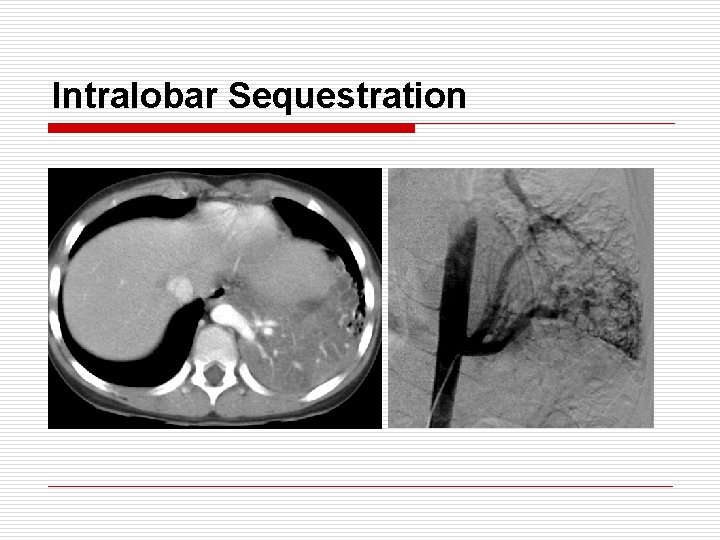
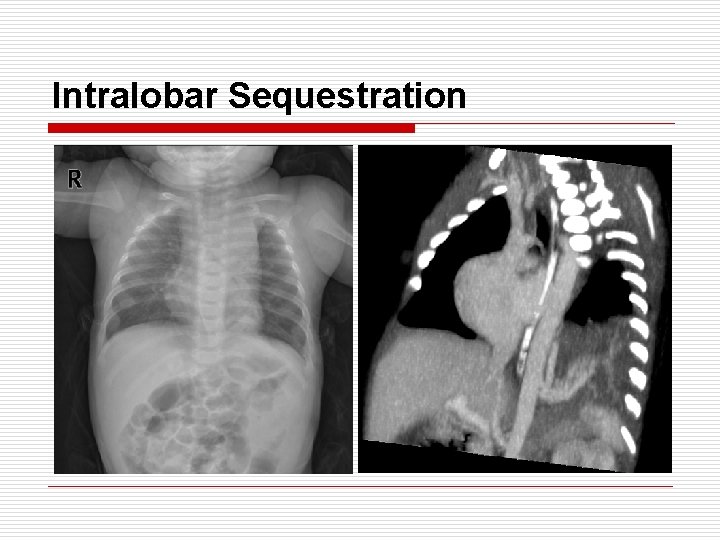
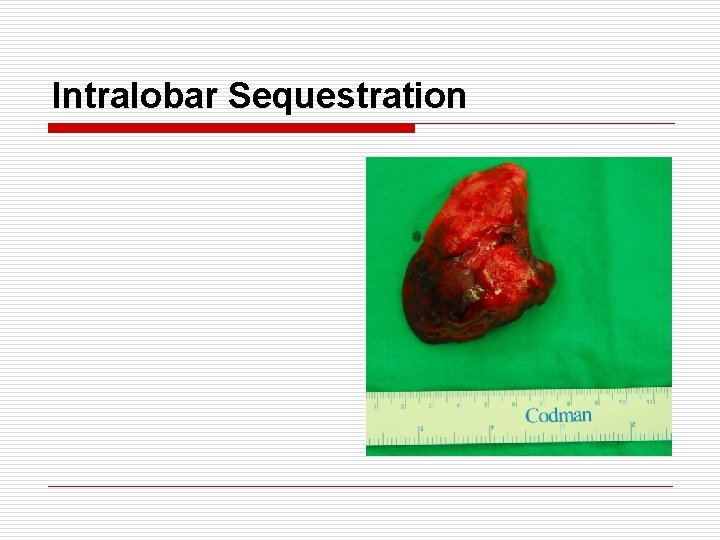
Intralobar Sequestration o o o o Arterial supply : thoracic aorta 70%, abdominal aorta 30% Venous drain : usually pulmonary vein Location : posterior basal region (usually LLL) Age : adolescent or young adult M: F = 1. 5: 1 / Associated anomaly : 10% Communication with normal lobe via ‘pore of Kohn’ Presentation : repeated infection, hemoptysis, cystic mass on CXR Tx : lobectomy (segmentectomy → incomplete resection, persistent air leak)

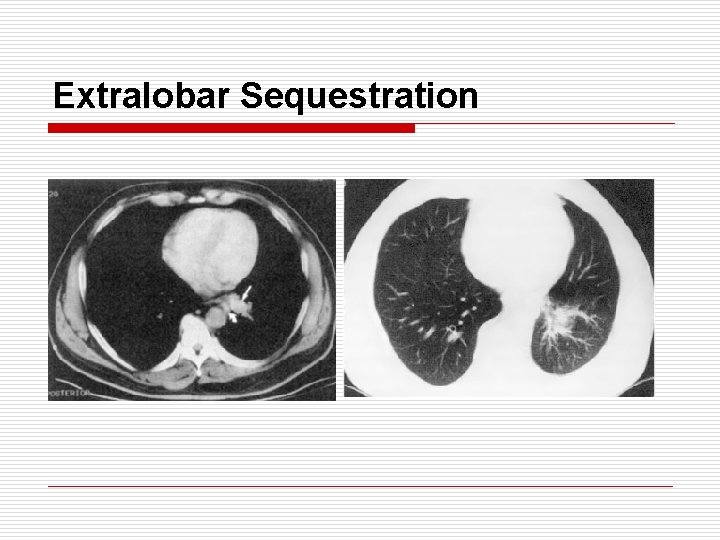
Extralobar Sequestration o o o o Arterial Supply : thoracic aorta 70%, abdominal aorta 30% Venous drain : usually systemic vein (azygos or portal vein) Location : posteromedial in lower chest Age : early childhood M: F = 3: 1 / Associated anomaly : 50% Presentation : dense triangular asymptomatic mass on CXR Infection : rare (may asymptomatic throughout life, may regress spontaneously) Tx : resection (wait until one year to decrease

Intralobar Sequestration

Intralobar Sequestration

Intralobar Sequestration

Intralobar Sequestration

Extralobar Sequestration

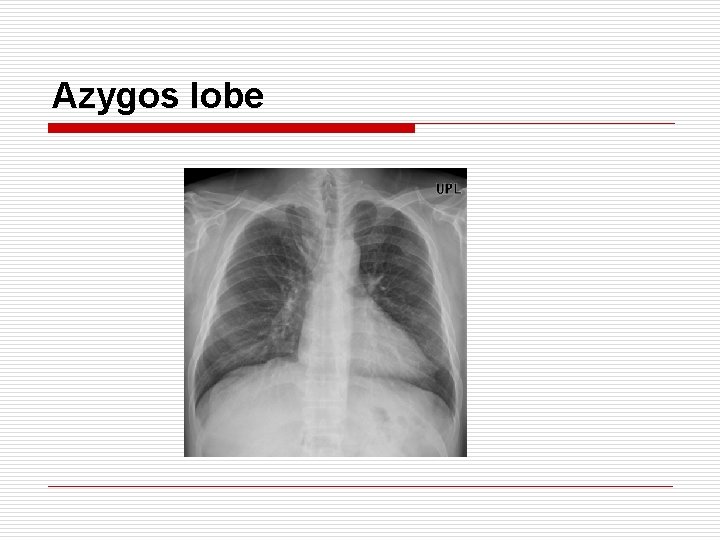
Azygos lobe

Bronchogenic Cyst o o o o o Abnormal budding from the perimeter of trachea Most frequent mediastinal cyst (60%) Usual location : right paratracheal area May located in carina, hilar, lobar bronchus, intrapulmonary Male > Female Bronchial communication : rare Unilocular (2~10 cm) May contain normal bronchial element (cartilage, smooth muscle) May contain mucus, blood, milky material

Bronchogenic Cyst o o o Incidental finding on CXR : air-filled cyst (with or without fluid) Intraparenchymal cyst : more frequent infectious symptom (90%) Sx : mass effect on trachea or bronchus, dysphagia, hemoptysis Dx : CT Tx : resection (even if asymptomatic) - achieve diagnosis - reduce complication (perforation, hemorrhage, enlargement,

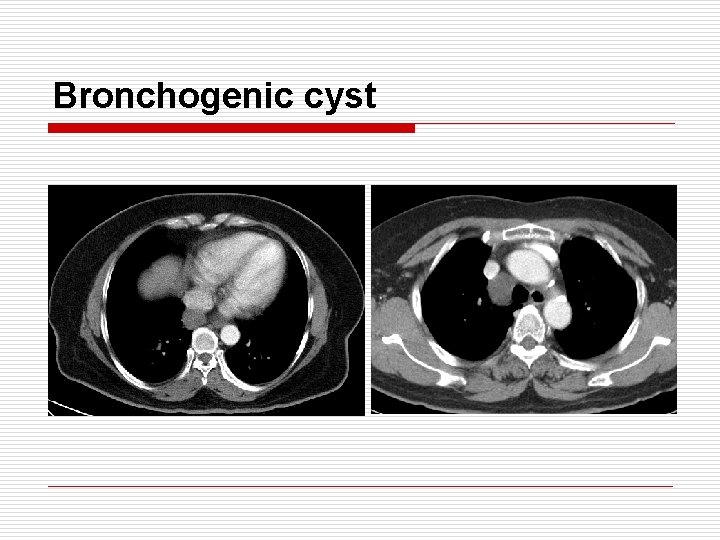
Bronchogenic cyst

Lung Bud Anomaly o o o o Pulmonary Agenesis, Aplasia, Hypoplasia Congenital Lobar Emphysema (CLE) Congenital Parenchymal Cyst Congenital Cystic Adenomatoid Malformation (CCAM) Infantile Pulmonary Emphysema Polyalveolar Lobe Pulmonary Lymphangiectasis

Pulmonary Agenesis, Aplasia, Hypoplasia o o o Pulmonary agenesis : complete absence of carina, bronchus, lung parenchyme Pulmonary aplasia : carina and bronchus are present (rudimentary stump) : vessles and parenchyma are absent Pulmonary hypoplasia : bronchus and bronchial tissue are poorly formed : reduced number of alveoli

Pulmonary Agenesis, Aplasia, Hypoplasia o o o Sx : tachypnea, dyspnea, cyanosis Unilateral agenesis : 30% die within 1 year : 50% die within 5 year Removal of rudimentary stump in recurrent infection Primary pulmonary hypoplasia : rare Most hypoplasia is the result of another defect : another defect prevents normal lung development : chest wall abnormality, diaphragmatic hernia, bone dysplasia

Congenital Lobar Emphysema o o o o o 50% of all congenital lung anomaly Ex : obstruction of a lobar bronchus Intrinsic obstruction : mucus plug, granulation Extrinsic obstruction : cardiac or vascular anomaly, adenopathy, mediastinal tumor, bronchogenic cyst > 50% : no identifiable etiologic factor Overexpansion of alveolar air space Lack of the parenchymal destruction Normal vasculature of the affected lobe Compressed adjacent lung by expanded lung Cartinaginous defect : 25%

Congenital Lobar Emphysema o o o o Asymptomatic at birth Sx : wheezing, dyspnea, cough after several days M: F = 3: 1 Most frequent affected lobe : LUL Tx : lobectomy in symptomatic (asymptomatic : lesion may resolve, should be observed) Symptomatic without treatment - 50% die within 1 st week, 30~40% die over the next Mo Greatest risk at the time of intubation - involved lobe does not collapse

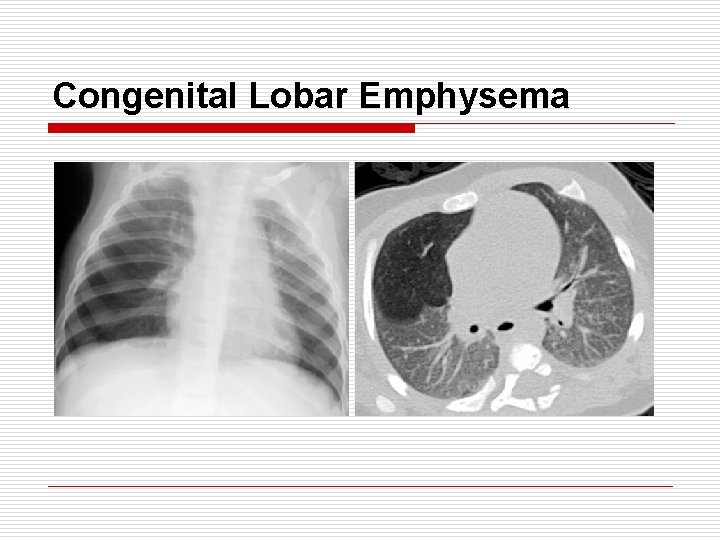
Congenital Lobar Emphysema

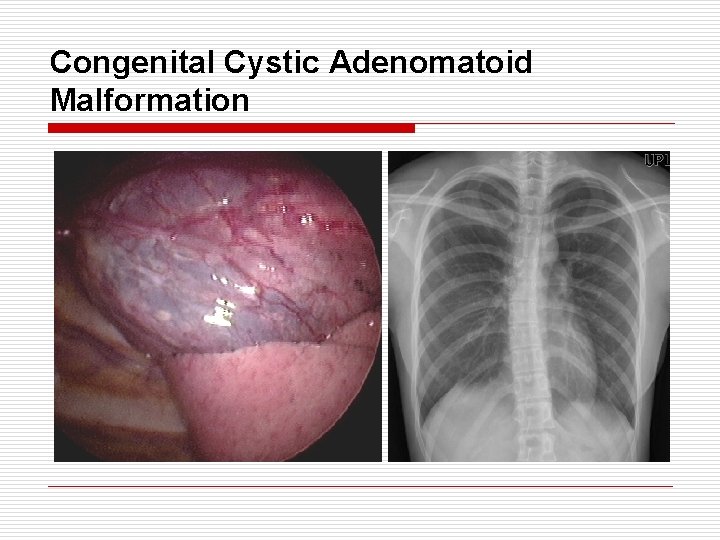
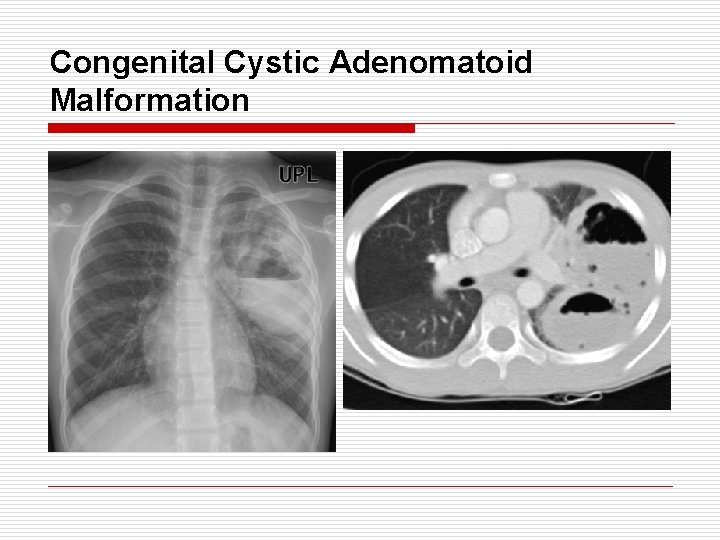
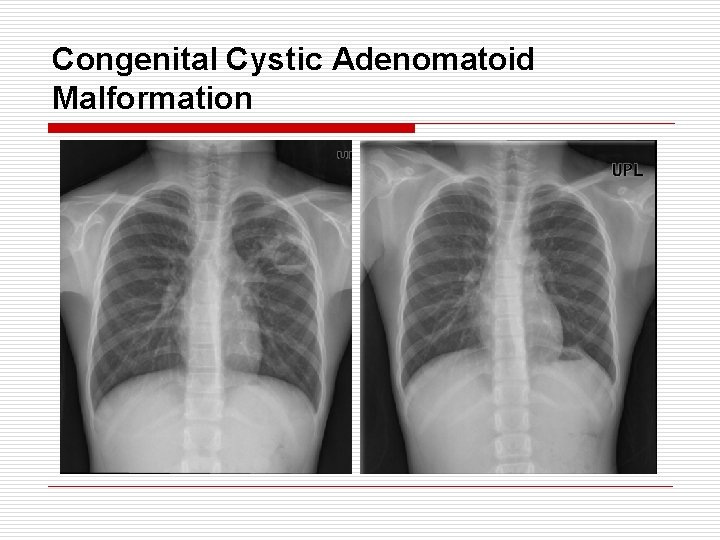
Congenital Cystic Adenomatoid Malformation o o o o o 25% of all congenital lung anomaly A mass of excessive proliferation of bronchus Without normal alveolar development Normal vascular development Affected area communicate with normal airway Usually affect one lobe Usually single lesion Type I : 50%, single or multiple cyst, > 2 cm → good prognosis Type II : 40%, multiple cyst, 1 cm → poor prognosis Type III : 10%, large mass, no or tiny cyst → poor prognosis (adenomatiod type)

Congenital Cystic Adenomatoid Malformation o o Sx Neonatal acute respiratory distress Recurrent infection, pneumothorax, hemoptysis, BAC Malignancy associated with CCAM Pleuropulmonary blastoma - infant, young children BAC - older children, adult DDx - Congenital diaphragmatic hernia Tx - lobectomy in symptomatic (asymptomatic - observation for the first 6 Mo, CT / 6 Mo)

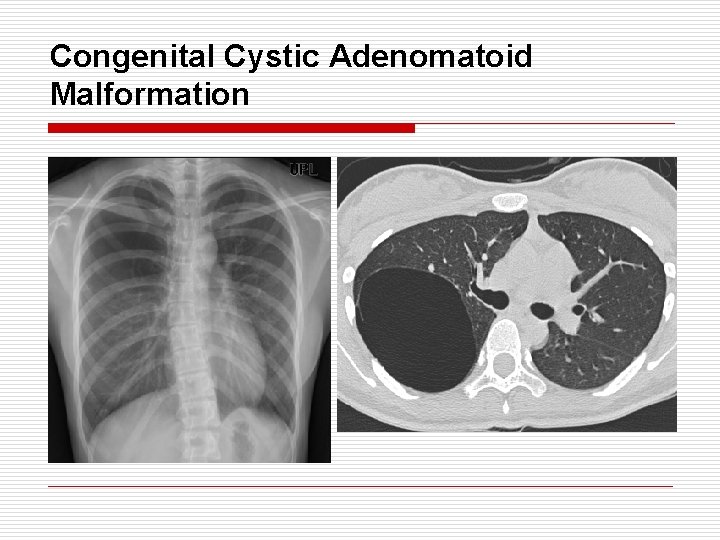
Congenital Cystic Adenomatoid Malformation

Congenital Cystic Adenomatoid Malformation

Congenital Cystic Adenomatoid Malformation

Congenital Cystic Adenomatoid Malformation

Management for Congenital Lung Disease Operation § All ILS § All bronchogenic cyst § All CCAM visible large cyst on CT § Symptomatic CLE Observation § Asymptomatic CLE § ELS without significant shunt

Timing of Surgery o o o Most patients will symptomatic sooner or later : Resection should be done in infancy Waiting for infection to occur : Complicate the surgery and prolong the time spent in hospital CT scan : Within 2 Mo of age Waiting until 4 weeks of age : Decrease anesthetic risk Operation : 3~6 months of age