Contents l l l Diabetes Mellitus 1 Type


Contents l l l 당뇨병(Diabetes Mellitus) 제 1형 당뇨병 (Type 1 diabetes) 제 2형 당뇨병 (Type 2 diabetes) 임신성 당뇨병(Gestational diabetes) 갑상선기능 저하증(Hypothyroidism) 갑상선기능 항진증(Hyperthyroidism) 뇌하수체질환(Pituitary disorders) 부신피질질환(Adrenal cortex disorders)

Brief History of Diabetes Mellitus
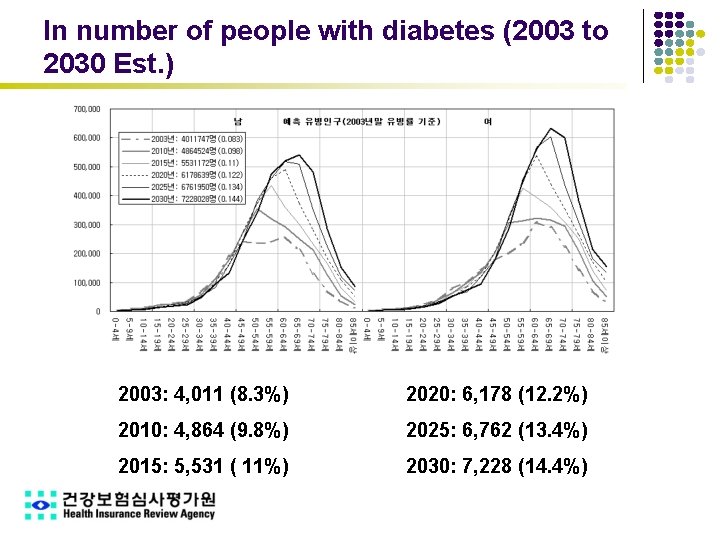
In number of people with diabetes (2003 to 2030 Est. ) 2003: 4, 011 (8. 3%) 2020: 6, 178 (12. 2%) 2010: 4, 864 (9. 8%) 2025: 6, 762 (13. 4%) 2015: 5, 531 ( 11%) 2030: 7, 228 (14. 4%)
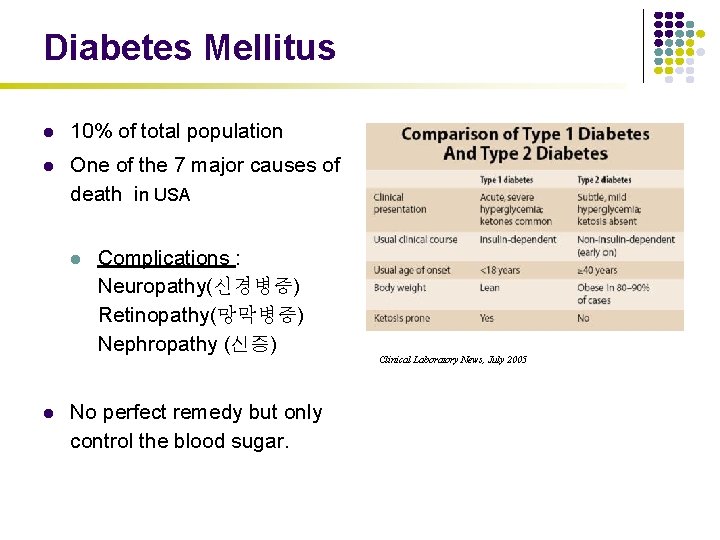

Diabetes Mellitus l 10% of total population l One of the 7 major causes of death in USA l l Complications : Neuropathy(신경병증) Retinopathy(망막병증) Nephropathy (신증) No perfect remedy but only control the blood sugar. Clinical Laboratory News, July 2005
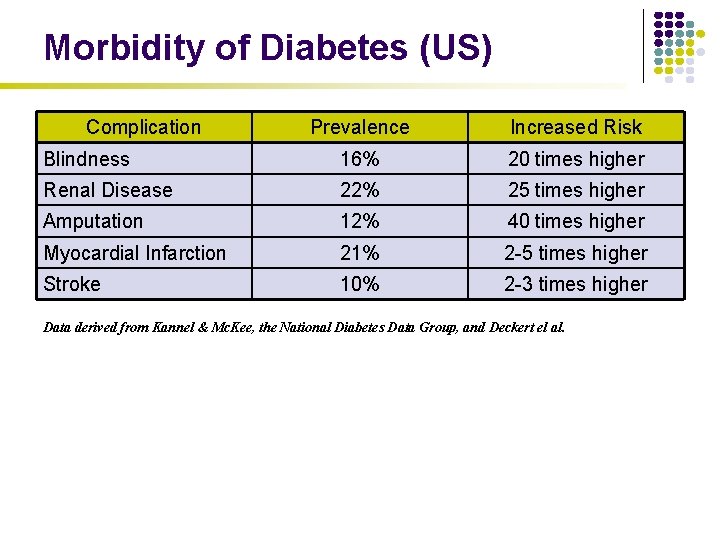
Morbidity of Diabetes (US) Complication Prevalence Increased Risk Blindness 16% 20 times higher Renal Disease 22% 25 times higher Amputation 12% 40 times higher Myocardial Infarction 21% 2 -5 times higher Stroke 10% 2 -3 times higher Data derived from Kannel & Mc. Kee, the National Diabetes Data Group, and Deckert el al.
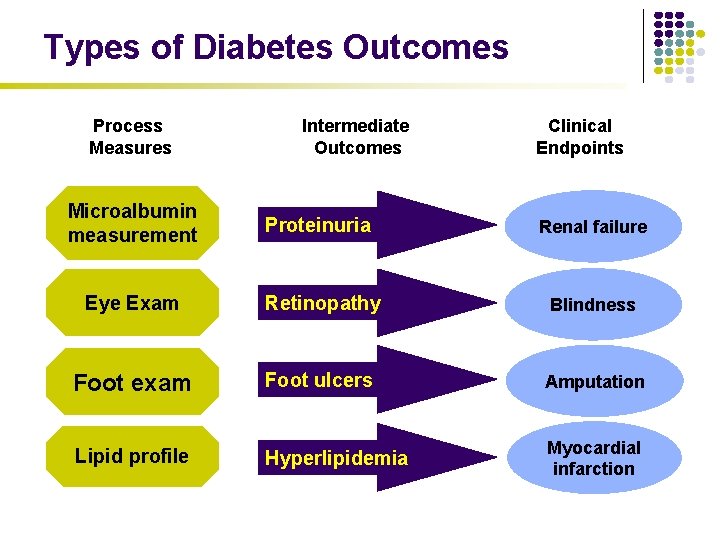
Types of Diabetes Outcomes Process Measures Intermediate Outcomes Clinical Endpoints Microalbumin measurement Proteinuria Renal failure Eye Exam Retinopathy Blindness Foot exam Foot ulcers Amputation Lipid profile Hyperlipidemia Myocardial infarction

The leading causes of death in the Korea Unit : 100, 000 Rank 1990 1999 2003 1 Cerebrovascular disease 75. 6 Cerebrovascular disease 72. 9 Cancer 131. 8 2 Heart disease 47. 4 Heart disease 39. 1 Cerebrovascular disease 75. 5 3 Traffic accident 39. 7 Traffic accident 26. 3 Heart disease 35. 6 4 Hypertension 35. 6 Stomach 24. 0 Diabetes Mellitus 25. 0 5 Liver disease 33. 8 Liver disease 23. 5 Suicide 24. 0 6 Stomach Cancer 31. 5 Lung Cancer 22. 1 Liver disease 20. 6 7 Liver Cancer 24. 1 Diabetes Mellitus 21. 8 Traffic accident 19. 1 8 Lung Cancer 14. 4 Liver cancer 20. 7 Chronic Lower Respiratory Infection 19. 1 9 Diabetes Mellitus 11. 8 Suicide 16. 1 Hypertension 10. 7 10 Tuberculosis 11. 0 Chronic Lower Respiratory Infection 13. 7 Death from a fall 7. 3 Source : 1999, 2003년 사망원인 통계연보

Definition of Diabetes Mellitus l Diabetes mellitus is a chronic disease caused by inherited and/or acquired deficiency in production of insulin by the pancreas, or by the ineffectiveness of the insulin produced. l Such a deficiency results in increased concentrations of glucose in the blood, which in turn damage many of the body’s systems, in particular the blood vessels and nerves. (World Health Organization, April 2002)


Endocrine pancreas l 내분비췌장: 4개의 주요 세포유형과 2개의 부가적 세포유형으로 구성되는 Langerhans섬 이라는 약 1백만개의 세포집단 1)ß-cells: insulin생산 2)α -cells: glucagon분비-간에서 글리코겐분해 활성화, 고혈당유발 3)δ-cells: somatostatin함유- insulin, glucagon분비 모두 억제 4)pp cells: pancreatic polypeptide 함유 5)D 1 cells: 혈관활성장폴리펩티드(VIP)분비-글리코겐분해, 고혈당유발 6)Enterochromaffin cell: serotonin합성 ( Robbins & Cotran 병리학 1118 -1135)

Type 1. (Juvenile-onset diabetes or IDDM) l Type 1 diabetes is usually diagnosed in children and young adults, and was previously known as juvenile diabetes. In type 1 diabetes, the body does not produce insulin. Insulin is a hormone that is needed to convert sugar (glucose), starches and other food into energy needed for daily life. l Metabolic condition in which the beta cells of pancreas no longer produce insulin; characterized by hyperglycemia, breakdown of body fats and protein and development of ketosis


Diagnostic tools § § § Blood Sugar(FBS, PP 2) (공복혈당, 식후 2시간 혈당) Oral glucose tolerance test (경구당부하검사) Glycohemoglobin(Hb. A 1 C) (당화혈색소) Insulin Urine glucose Others

Blood Sugar l Fasting glucose test a check of a person's blood glucose level after the person has not eaten for 8 to 12 hours (usually overnight). This test is used to diagnose pre-diabetes and diabetes. l Oral glucose tolerance test In the oral glucose tolerance test the patient, after fasting for 15 hours, drinks 75 g of glucose in 300 ml of water, over 5 minutes. Blood glucose is measured before the drink and after 30, 60, 90 and 120 minutes. Urine is collected before the drink, and after 60 and 120 minutes. Before the test, for a period of 6 hours, the patient should avoid smoking and drinking coffee l 2 h Postprandial method: Levels <140 mg/d. L are considered to reflect normal glucose metabolism. A result between 140 -199 mg/d. L indicates impaired glucose tolerance. A result of >=200 mg/d. L is provisional evidence of glucose intolerance.

Hemoglobin A 1 c Sub unit Glycosylation l Hb. A 2 a 2 b more than 90% l Hb. A 2 2 a 2 d less than 1. 5% l Hb. A 1 a 1 2 a 2(b-FDP) Fructose-1 -6 -Di-Pos. l Hb. A 1 a 2 2 a 2(b-G 6 P) Glucose-6 -phosphate l Hb. A 1 c 2 a 2(b-G) Glucose l Hb. F 2 a 2 r l Variants Hb. S, Hb. E, Hb. D less than 1% 4 -6% less than 0. 8%
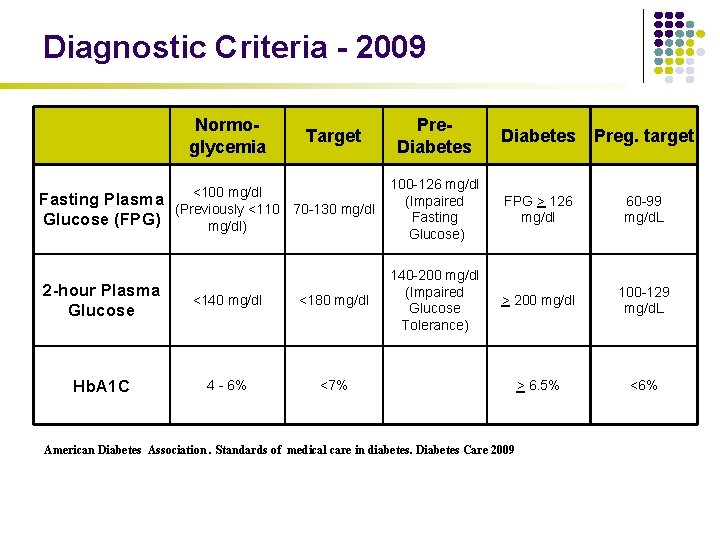
Diagnostic Criteria - 2009 Normoglycemia Fasting Plasma Glucose (FPG) Target <100 mg/dl (Previously <110 70 -130 mg/dl) 2 -hour Plasma Glucose <140 mg/dl <180 mg/dl Hb. A 1 C 4 - 6% <7% Pre. Diabetes Preg. target 100 -126 mg/dl (Impaired Fasting Glucose) FPG > 126 mg/dl 60 -99 mg/d. L 140 -200 mg/dl (Impaired Glucose Tolerance) > 200 mg/dl 100 -129 mg/d. L > 6. 5% <6% American Diabetes Association. Standards of medical care in diabetes. Diabetes Care 2009

Insulin 1. 2. 3. Insulin is a hormone released from the beta cells of the pancreas. Insulin's most important function is to facilitate glucose (blood sugar) uptake by a variety of tissues, especially adipose (fat) and skeletal muscle. Insulin also stimulates the synthesis and storage of triglycerides and proteins. Insulin is the most important regulator of blood glucose. High blood glucose (such as exists shortly after a meal) stimulates the release of insulin, whereas low blood glucose levels inhibit insulin release. Normal value: 5 -20 mc. U/m. L while fasting
Others C-peptide reactivity, CPR 1. § § § Is Proinsulin (A chain and B chain) linking connecting peptide Marker showing the function of beta cell of pancrase Normal Value: Plasma (0. 5~2. 0 ng/m. L), Urine (16~120 ug/day) Microalbumin (MA) 2. § § § Marker for early diagnosis of diabetic nephropathy Sample: 24 h urine Normal Value: 20~30 ug/min Examine for Complictions 3. § X-ray, electrocardiography, lipid profile, eye examine, Vibration sensory test etc



Types of Insulin l l Rapid-acting insulin, such as insulin Lispro (Eli Lilly), insulin Aspart (Novo Nordisk), or insulin Glulisine (sanofi-aventis), begins to work about 5 minutes after injection, peaks in about 1 hour, and continues to work for 2 to 4 hours. Regular or Short-acting insulin (human) usually reaches the bloodstream within 30 minutes after injection, peaks anywhere from 2 to 3 hours after injection, and is effective for approximately 3 to 6 hours. Intermediate-acting insulin (human) generally reaches the bloodstream about 2 to 4 hours after injection, peaks 4 to 12 hours later, and is effective for about 12 to 18 hours. Long-acting insulin (ultralente) reaches the bloodstream 6 to 10 hours after injection and is usually effective for 20 to 24 hours. There also two long-acting insulin analogues: glargine and detemir. They both tend to lower glucose levels fairly evenly over a 24 -hour period with less of a peak of action than ultralente.






Type 2. Diabetes mellitus (NIDDM) l l Type 2 diabetes is the most common form of diabetes. In type 2 diabetes, either the body does not produce enough insulin or the cells ignore the insulin. Insulin is necessary for the body to be able to use glucose for energy. When you eat food, the body breaks down all of the sugars and starches into glucose, which is the basic fuel for the cells in the body. Insulin takes the sugar from the blood into the cells. l When glucose builds up in the blood instead of going into cells, it can cause two problems: 1)Right away, your cells may be starved for energy. 2)Over time, high blood glucose levels may hurt your eyes, kidneys, nerves or heart. l Condition of fasting hyperglycemia occurring despite availability of body’s own insulin





- Slides: 33