CONTEMPORARY STANDARDS IN TREATMENT OF CHRONIC HEART FAILURE















































- Slides: 70

CONTEMPORARY STANDARDS IN TREATMENT OF CHRONIC HEART FAILURE JERZY JANKOWSKI MD DEPARTMENT OF CLINICAL PHARMACOLOGY

http: //www. zfk. ump. edu. pl/

Key issues in Chronic Heart Failure (CHF) is Common- 2% of the population n Dangerous- high mortality n Disabling- high morbidity n Costly- 2% of health care budget n Treatable- very successful pharmocological therapy developed n

Definition of CHF n Heart failure (HF) is the inability of the heart to maintain an output adequate to meet the metabolic demands of the body. n Definition of HF I. Symptoms and signs of heart failure (at rest or during exercise) and II. Objective evidence (preferably by echocardiography) of Cardiac dysfunction (systolicand/ordiastolic) (at rest) and (in cases where the diagnosis is in doubt) and III. Response to treatment directed towards heart failure *Criteria I and II should be fulfiled in all cases.






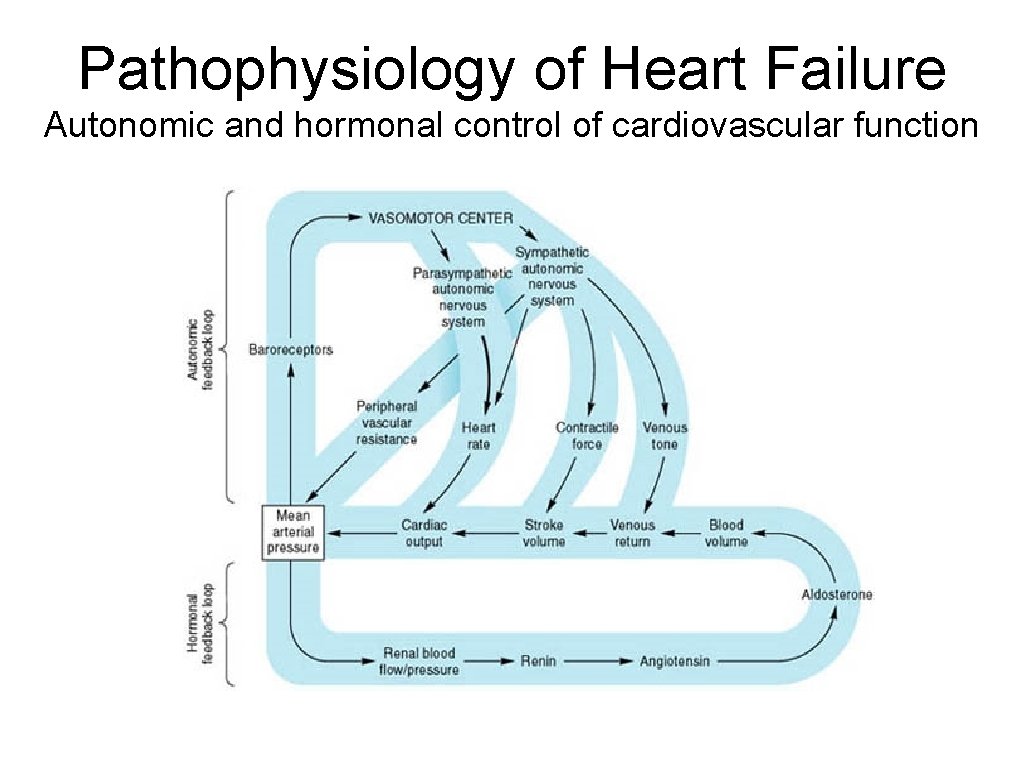
Pathophysiology of Heart Failure Autonomic and hormonal control of cardiovascular function

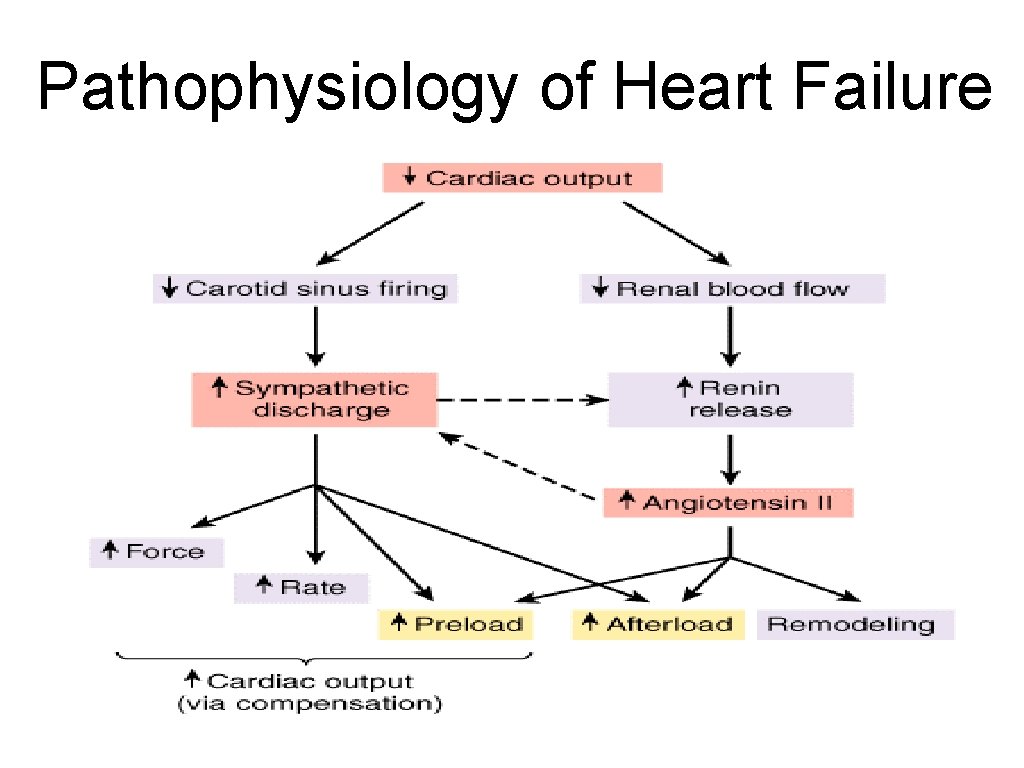
Pathophysiology of Heart Failure

Pathophysiology of Cardiac Performance Cardiac performance is a function of 4 factors PRELOAD AFTERLOAD CONTRACTILITY HEART RATE

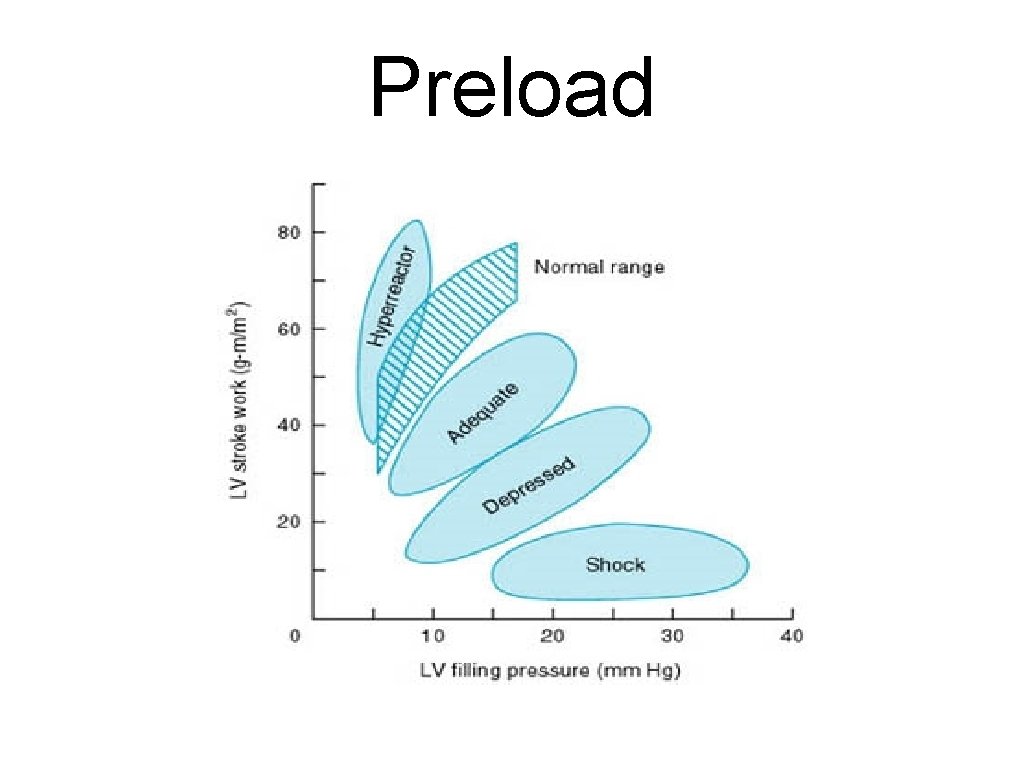
Preload























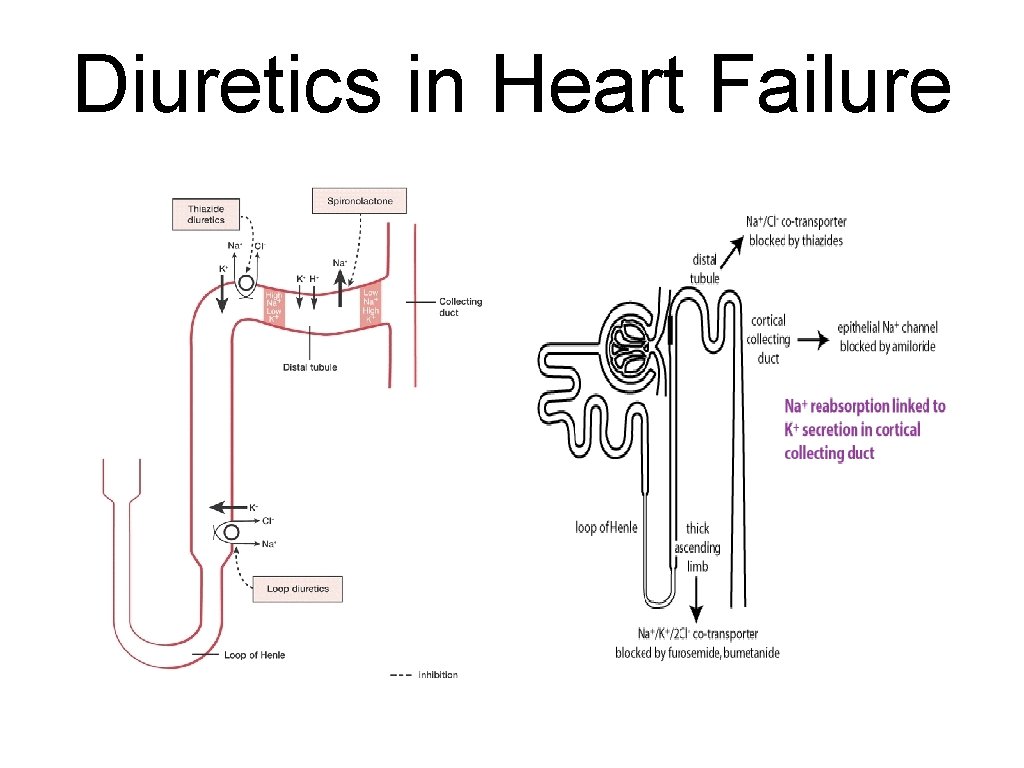
Diuretics in Heart Failure Loop diuretics: furosemide, torsemide Thiazide and thiazide-like diuretics: hydrochlorothiazide chlorthalidone + K sparing diuretics: + Na channel inhibitors: amiloride, triamterene Aldosteron antagonists: spironolactone, eplerenone

Diuretics in Heart Failure

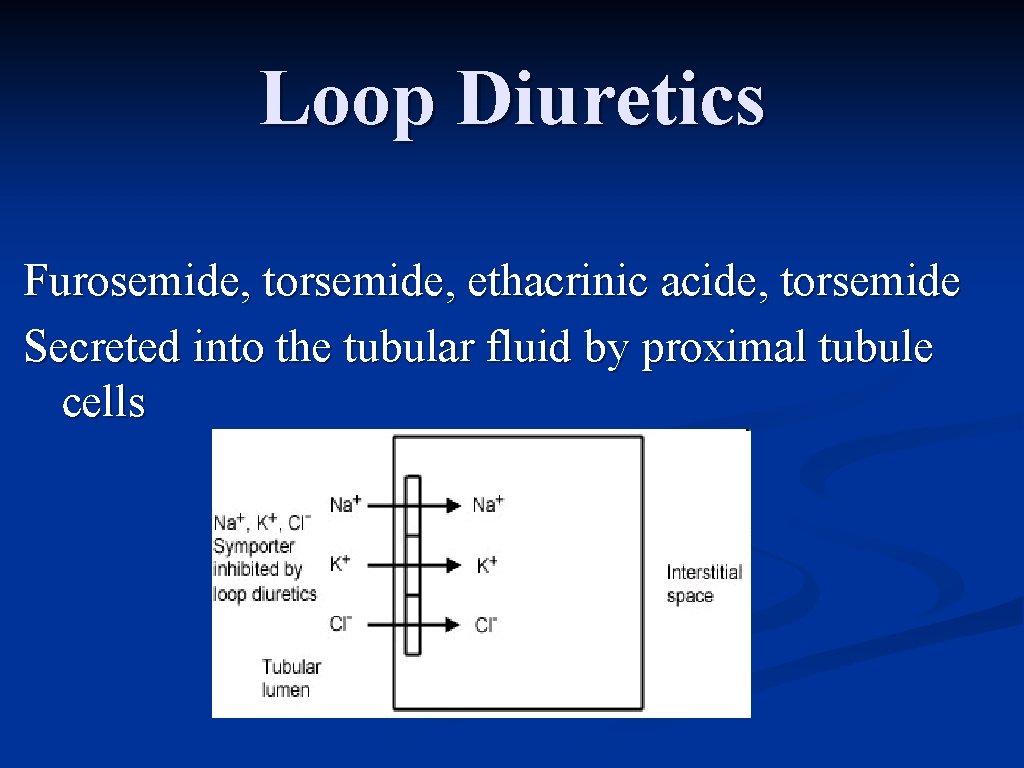
Loop Diuretics Furosemide, torsemide, ethacrinic acide, torsemide Secreted into the tubular fluid by proximal tubule cells

Loop Diuretics: Side Effects and Drug Interaction n n n Volume depletion, hyponatremia, hypokalemia Hypocalcemia, hypomagnesemia, hypochloremia Ototoxicity – especially with ethacrynic acid Hypotension Metabolic effects – hyperuricemia, hyperglycemia, hypercholesterolemia (↑LDL, ↓HDL, ↑TGL) Cardiac glycosides (risk of ventricular arrhythmias) Aminoglycoside antibiotics, cisplatin (risk of ototoxicity)

Loop Diuretics: Drug Interaction n NSAIDs – reduced effects n Probenecid – blocks secretion into the distal tubule and decreases the response to the LD

Thiazide Diuretics Hydrochlorothiazide – the prototype for this class of drugs n Thiazide-like – chlorthalidone, indapamide and metolazone (long acting diuretics) n The same mechanism of action n

Thiazide Diuretics – Side Effects Electrolyte abnormalities – hypokaliemia, hyponatremia, hypercalcemia, hypomagnesemia, hypochloremia, hypovolemia n Hyperuricemia, hyperglycemia (reduced effecacy of hypoglycemic drugs n Increased plasma levels of LDL and TGL n Sexual dysfunction n Cardiac arrhythmias n Drug interactions – as loop diuretics n




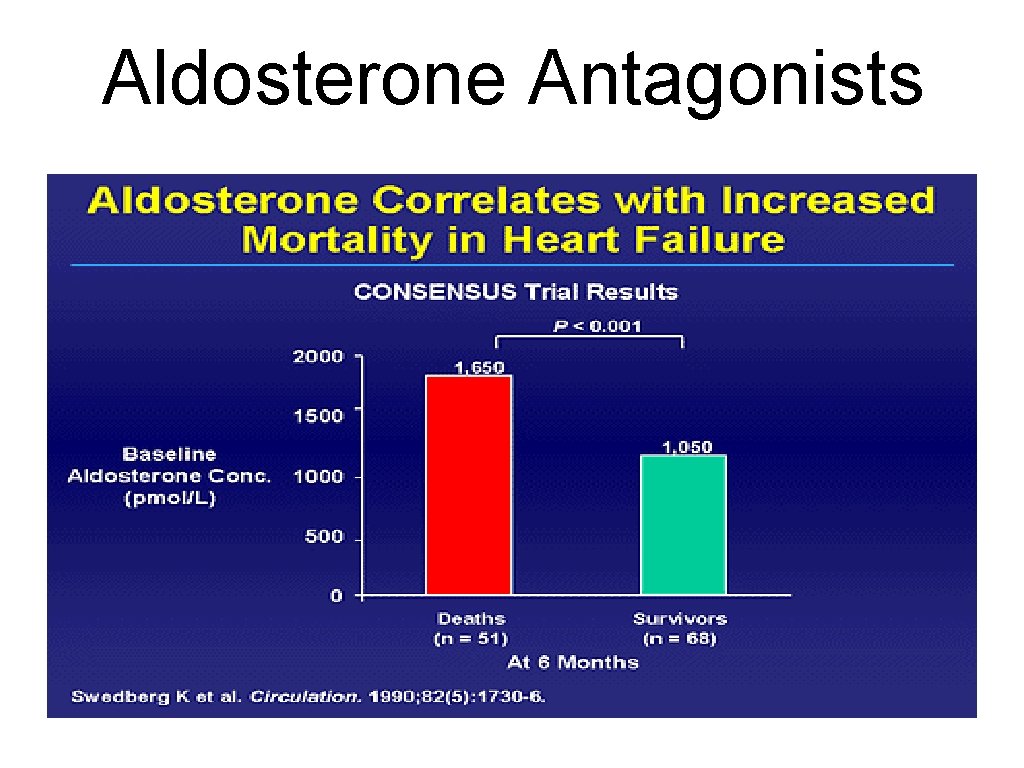
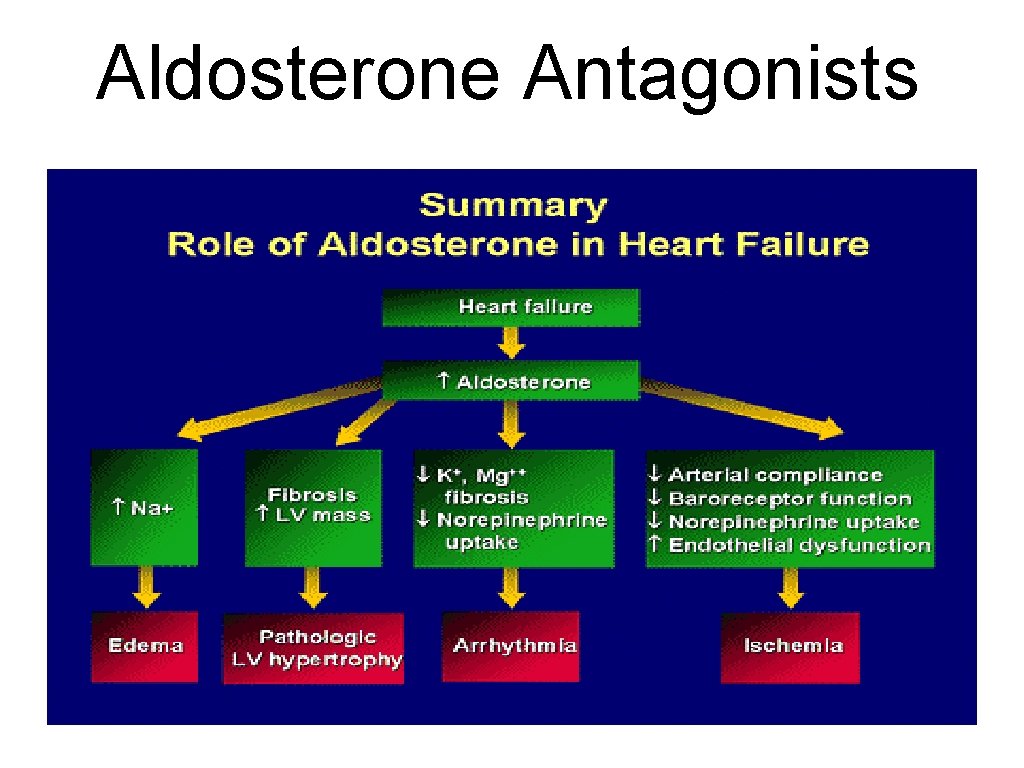
Aldosterone Antagonists

Aldosterone Antagonists

Aldosterone Antagonists

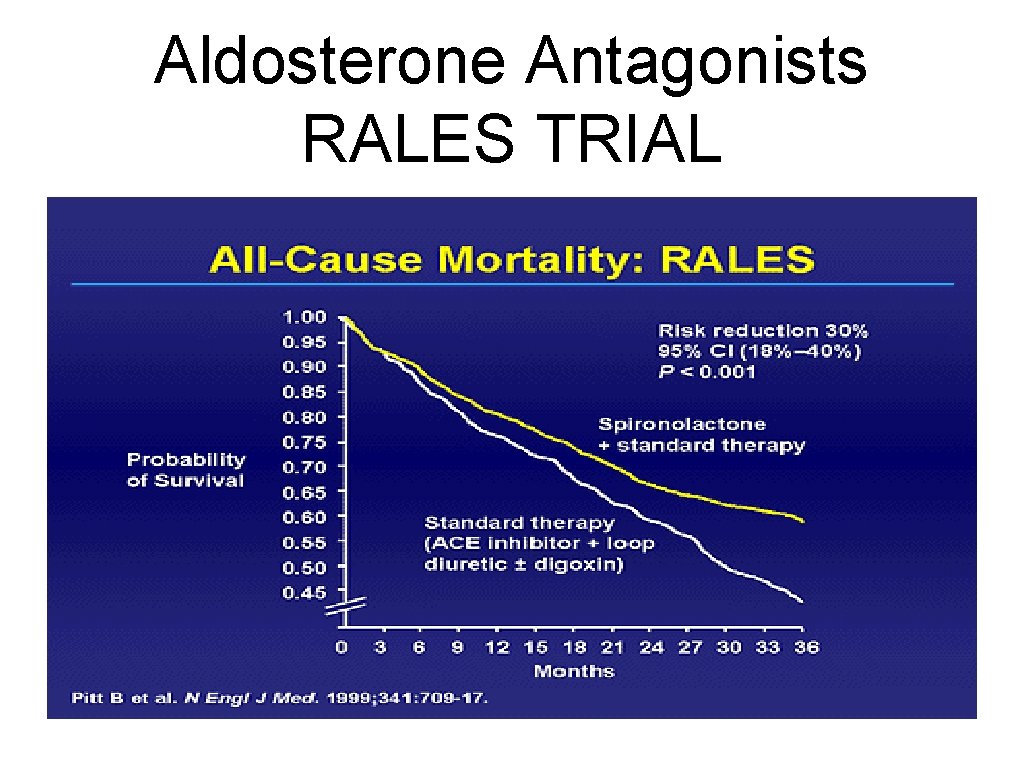
Aldosterone Antagonists RALES TRIAL

RALES TRIAL

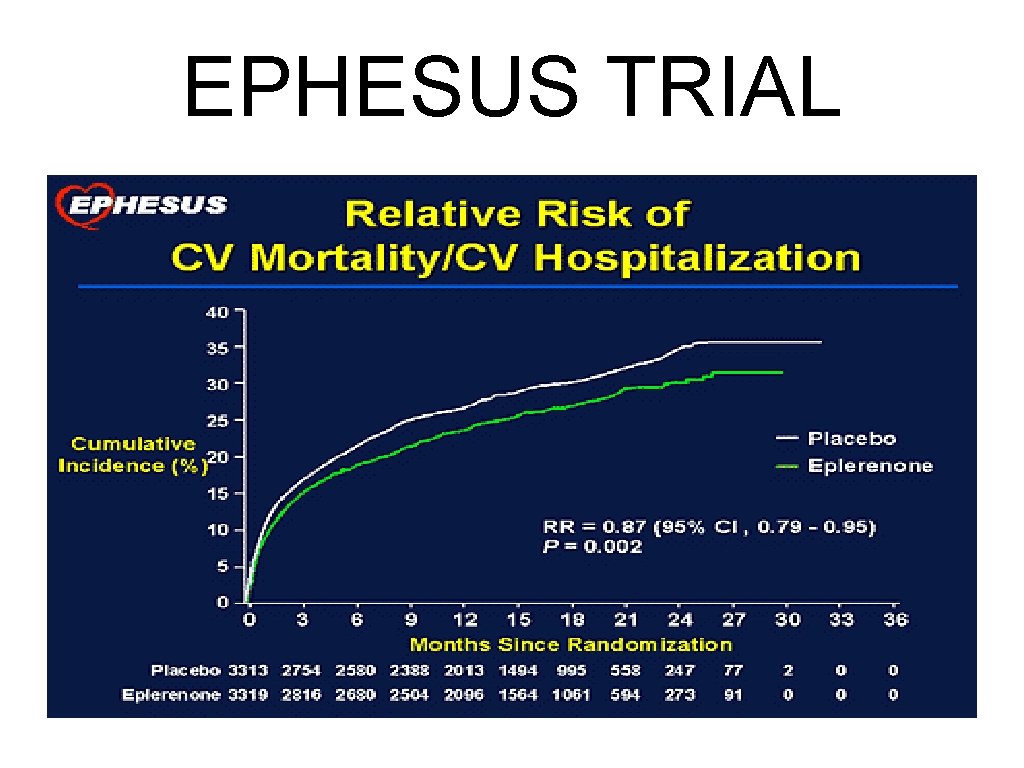
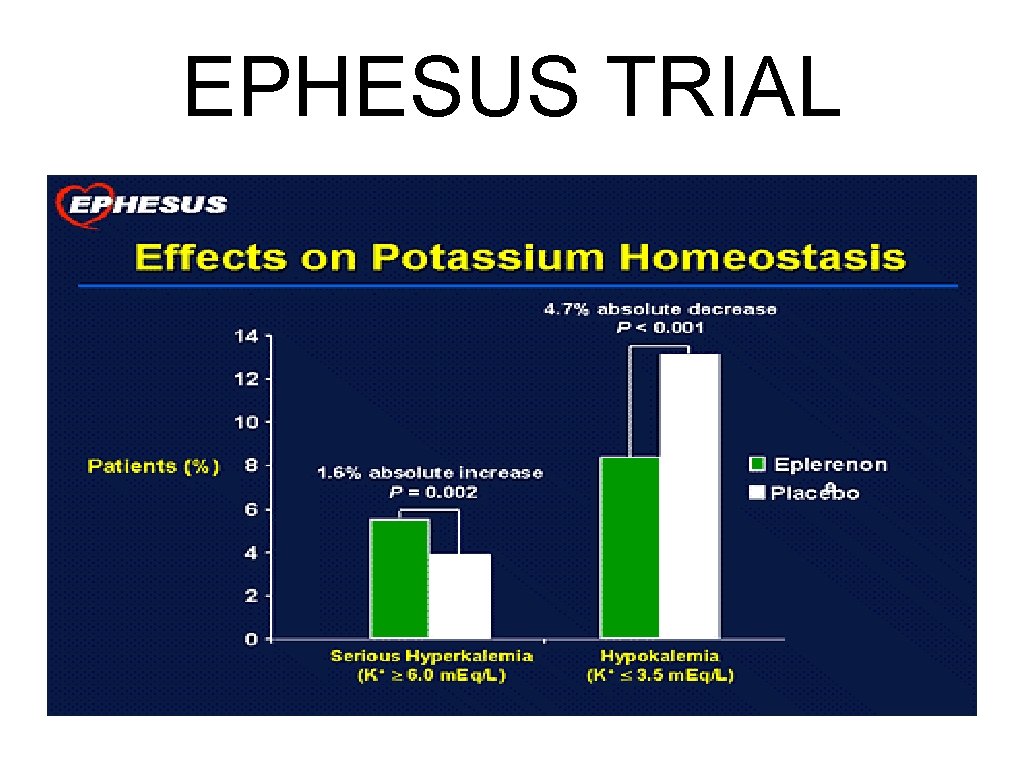
Aldosterone Antagonists EPHESUS TRIAL

EPHESUS TRIAL

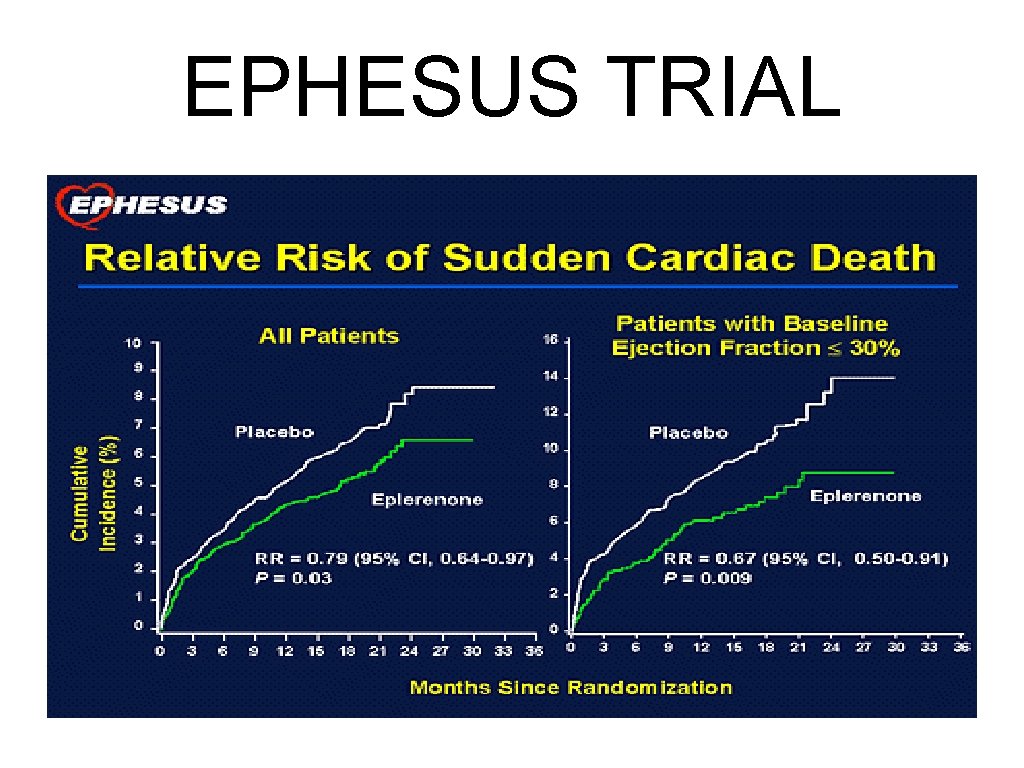
EPHESUS TRIAL

EPHESUS TRIAL

EPHESUS TRIAL

EPHESUS TRIAL


Cardiac glycosides

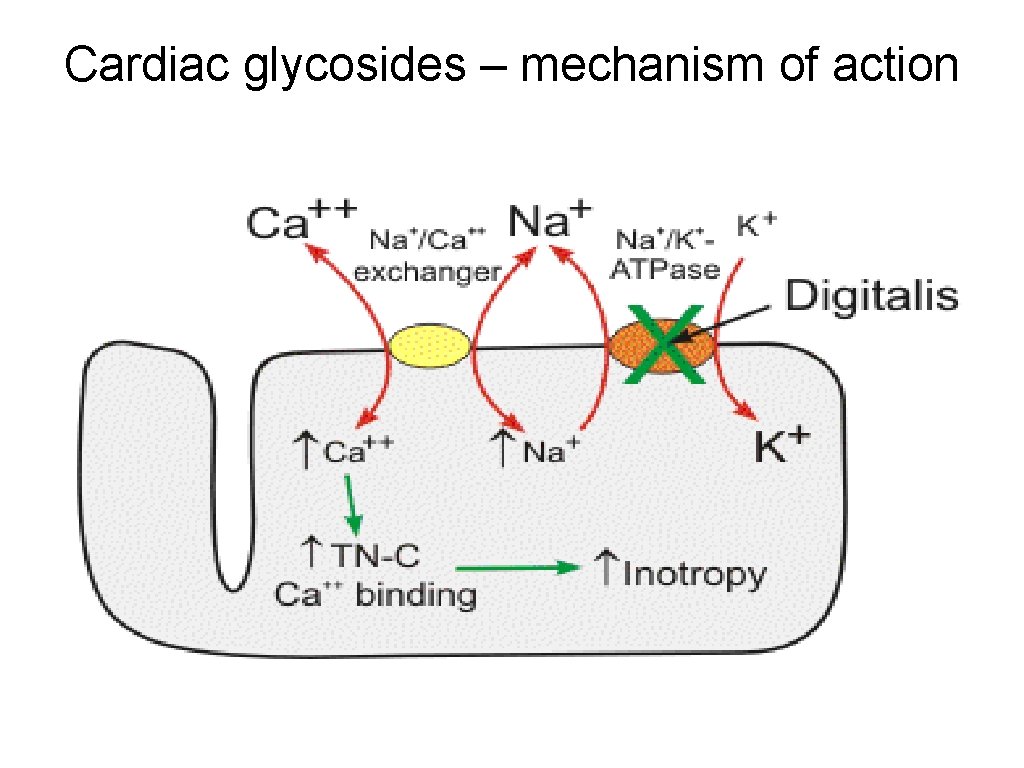
Cardiac glycosides – mechanism of action

Pharmacokinetics (Digoxin, Digitoxin) Highly variable kinetics + VERY narrow therapeutic index = need to individualize dose regiments Relatively long half-lives of elimination accumulation to stedy state loading doses employed delays following changes in therapy

Pharmacokinetics Plasma concentration determinations Effective range = 1. 0 – 2. 5 ng/ml Toxic range = 1. 5 – and up Rarely essential to a diagnosis of toxicity Estimate of degree of overdose Can be used to calculate dose adjustments

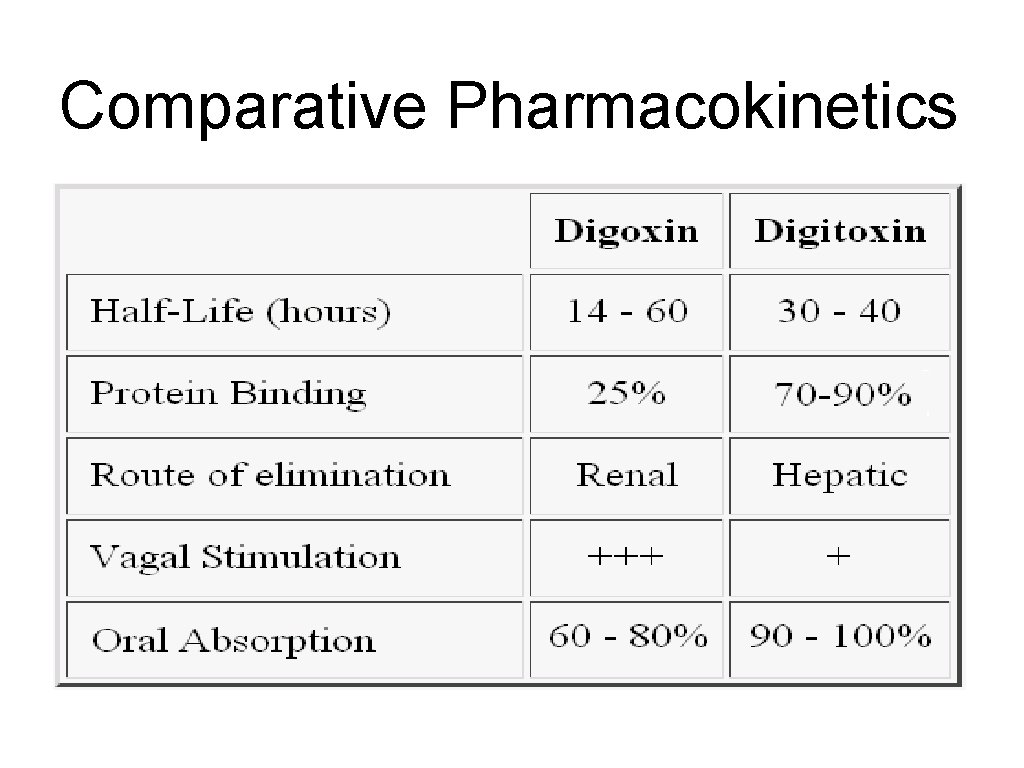
Comparative Pharmacokinetics

Toxicity Gastrointestinal (relate to vagal effects) anorexia abdominal discomfort vomiting diarrhea

Toxicity Cardiac disturbances premature ventricular depolarization nodal rhytms A – V dissociation

Treatment of Toxicity • Stop giving the drug (for a time) • Potassium (if hypokalemic) • Cholstyramine, activated charcoal (to bind digoxin in GI tract and shorten half-life ) • Digoxin Antibodies (Fab fragments) • Antiarrhythmics (very cautiously) • Electrotherapy (defibrillation only in the case of VF

Drug Interactions • Increased plasma concentration – verapamil, diltiazem, quinidine, amiodaron, spironolacton • Changes in plasma electrolyte – diuretics, salts (K+, Ca++), adrenocorticoids • Changes in digoxin absorption – antacids, cholestyramine, laxatives, antidiarrheal absorbents • Changes in cardiac cell activity sympathomimetics



