Contained antimicrobial resistance and the NDPHS Action Plan

Contained antimicrobial resistance and the NDPHS Action Plan on AMR (The NDPHS Strategy-objective-2) Martin Steinbakk Norwegian Institute of Public Health Domain for Infection Control and Environmental Health

Objective 2. Contained antimicrobial resistance – through inter-sectorial efforts supporting the implementation of regional and global strategies and/or action plans • Antibiotic resistance cost lives and money and threatens to undermine modern basic health care and advanced medicine • The scale of the challenge grows through globalisation and with increased mobility and worldwide food- and animal trade • National, regional and global initiatives are on-going. AMR surveillance systems, key indicators for antibiotic use and guidelines for rational use are in place in most of the NDPHS Partner Countries – CAESAR (Central Asian and Eastern European Surveillance of Antimicrobial Resistance) - coordinated by WHO – EARS-Net (European Antimicrobial Resistance Surveillance Network) – coordinated by ECDC – ESAC (European Surveillance of Antibiotic Consumption) – coordinated by ECDC – ESVAC (European Surveillance on Veterinary Antibiotic Consumption) – coordinated by EMA • However, the stored data have varying quality due to differences in the national participation and variations in sampling practices, as well as lack of individual data on bacterial strains and persons (in some cases only aggregated data are stored).

Europe: Extra number of deaths 25 000 USA: Extra number of deaths 23 000
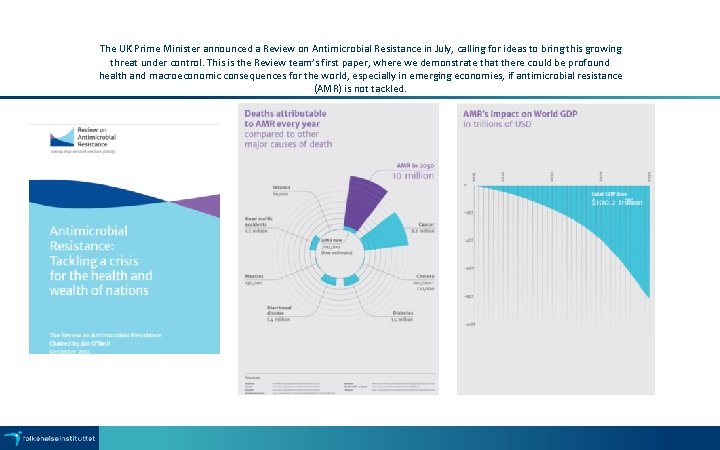
The UK Prime Minister announced a Review on Antimicrobial Resistance in July, calling for ideas to bring this growing threat under control. This is the Review team’s first paper, where we demonstrate that there could be profound health and macroeconomic consequences for the world, especially in emerging economies, if antimicrobial resistance (AMR) is not tackled.
Lord Kelvin 1883 World Health Organization 2015; ISBN 978 92 4 150976 3

Global Antimicrobial Surveillance System - GLASS

Objective 2. Footprint of the NDPHS work and expected results • Footprint – To contribute to the achievement of more rational use of antibiotics in all sectors in the Northern Dimension area based on a better assessment of the antibiotic resistance situation • Expected results – More representative and comparable AMR surveillance systems developed for implementation in the NDPHS Partner Countries – Improved measurement and monitoring of antibiotic use in the Northern Dimension area – Increased awareness of prescribers and policymakers on the antibiotic resistance situation in the Northern Dimension area and on specific measures to be taken

Objective 2. Planned activities towards the expected results • Improved measurement and monitoring of antibiotic use in the Northern Dimension area – Collect and evaluate the existing praxis of applying the key indicators for rational antibiotic use in the NDPHS Partner Countries Norway and Sweden and suggest improvements (if relevant) – Develop key indicators to accurately reflect rational antibiotic use in the remaining NDPHS Partner Countries – Arrange for dissemination activities to present the developed key indicators to policy makers, authorities and health care professionals – Implementation of activities to measure antibiotic use against the developed key indicators • Expected results – Key indicators – Data collected, analyzed and information disseminated on antibiotic use in the NDPHS Partner Countries

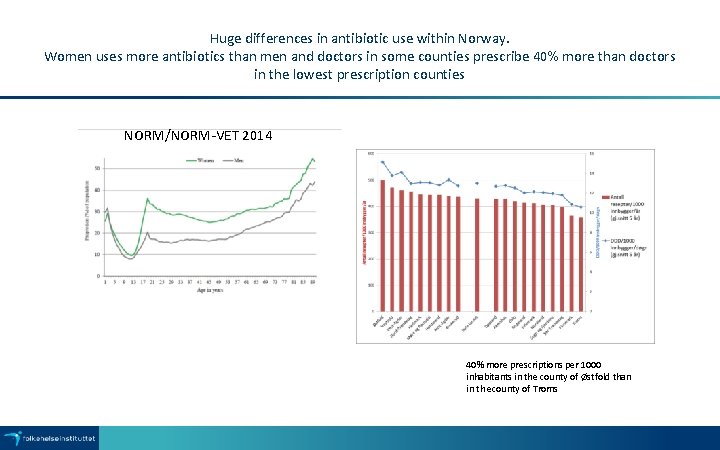
Huge differences in antibiotic use within Norway. Women uses more antibiotics than men and doctors in some counties prescribe 40% more than doctors in the lowest prescription counties NORM/NORM-VET 2014 40% more prescriptions per 1000 inhabitants in the county of Østfold than in th ecounty of Troms


National Strategy Against Antibiotic Resistance 2015 -2020

National Strategy Against Antibiotic Resistance 2015 -2020
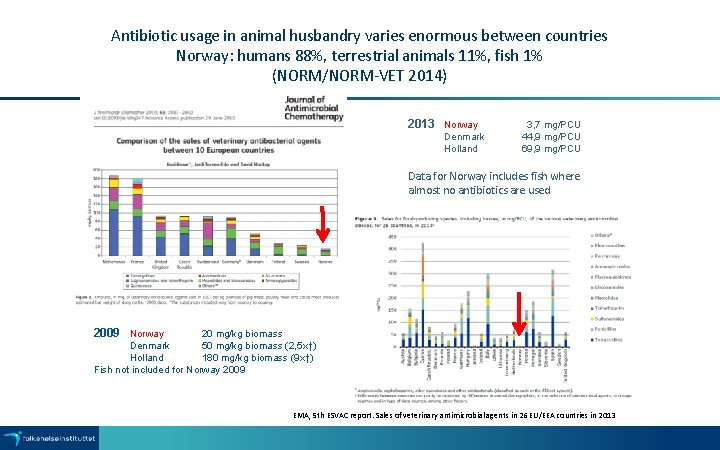
Antibiotic usage in animal husbandry varies enormous between countries Norway: humans 88%, terrestrial animals 11%, fish 1% (NORM/NORM-VET 2014) 2013 Norway Denmark Holland 3, 7 mg/PCU 44, 9 mg/PCU 69, 9 mg/PCU Data for Norway includes fish where almost no antibiotics are used 2009 Norway 20 mg/kg biomass Denmark 50 mg/kg biomass (2, 5 x↑) Holland 180 mg/kg biomass (9 x↑) Fish not included for Norway 2009 EMA, 5 th ESVAC report. Sales of veterinary antimicrobial agents in 26 EU/EEA countries in 2013


Annual report on: Usage of Antimicrobial Agents and Occurence of Antimicrobial resistance in Norway 2014 www. antibiotikaresistens. no All microbes (isolates) are stored with individual data NORM/NORM-VET 2014: Usage of Antimicrobial Agents and Occurrence of Antimicrobial Resistance in Norway. Tromsø / Oslo 2015. ISSN 1502 -2307 (print) / 1890 -2307 (electronic).
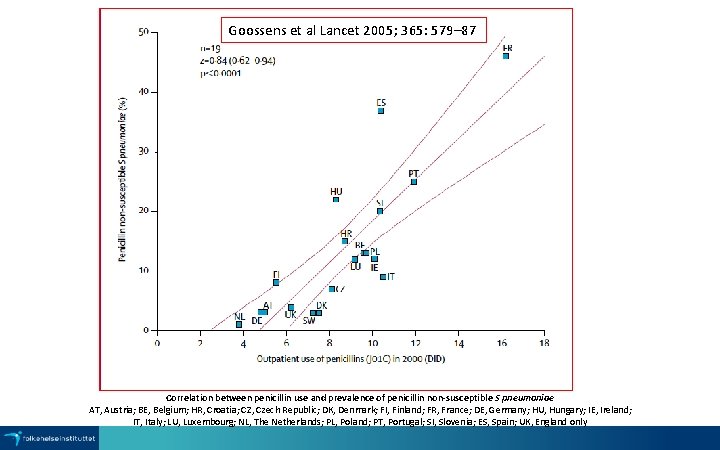
Goossens et al Lancet 2005; 365: 579– 87 Correlation between penicillin use and prevalence of penicillin non-susceptible S pneumoniae AT, Austria; BE, Belgium; HR, Croatia; CZ, Czech Republic; DK, Denmark; FI, Finland; FR, France; DE, Germany; HU, Hungary; IE, Ireland; IT, Italy; LU, Luxembourg; NL, The Netherlands; PL, Poland; PT, Portugal; SI, Slovenia; ES, Spain; UK, England only
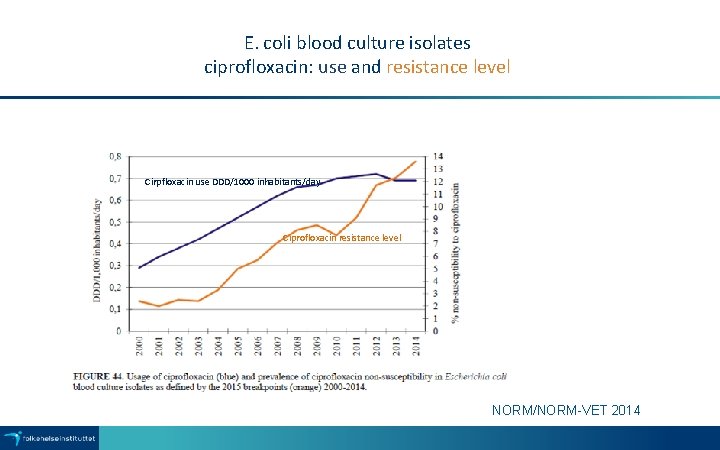
E. coli blood culture isolates ciprofloxacin: use and resistance level Cirpfloxacin use DDD/1000 inhabitants/day Ciprofloxacin resistance level NORM/NORM-VET 2014

Proportion of 3 rd generation cephalosporins (R+I) resistant Escherichia coli isolates in participating countries in 2005 - 2014 2012 2011 2013 2009 2014 2005 ECDC, EARS-Net http: //ecdc. europa. eu/en/healthtopics/antimicrobial_resistance/database/Pages/map_reports. aspx
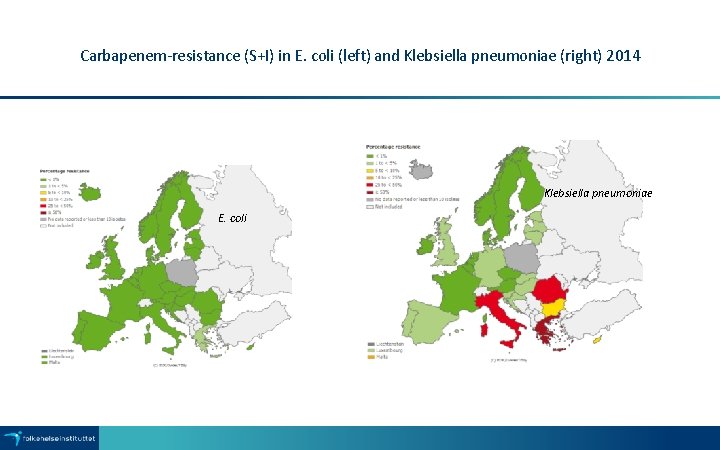
Carbapenem-resistance (S+I) in E. coli (left) and Klebsiella pneumoniae (right) 2014 Klebsiella pneumoniae E. coli

Objective 2. Policy and actions needed - Room for improvement • Generally a lack of comparable data on aspects other than invasive infections, leading to an incomplete understanding of the AMR in the Northern Dimension area, e. g. in urinary tract infections • Only a few NDPHS Partner Countries have key indicators for rational antibiotic use in place. The majority of the NDPHS Partner Countries have guidelines regarding rational use and infection prevention and control, but further collaboration and the evaluation of the use and impact of these guidelines would be useful. • Insufficient depth of knowledge and awareness in the general public on the impact of AMR on public health. Both due to inappropriate use of antibiotics in humans, animals and agriculture and inefficient prevention and control routines in health care settings.
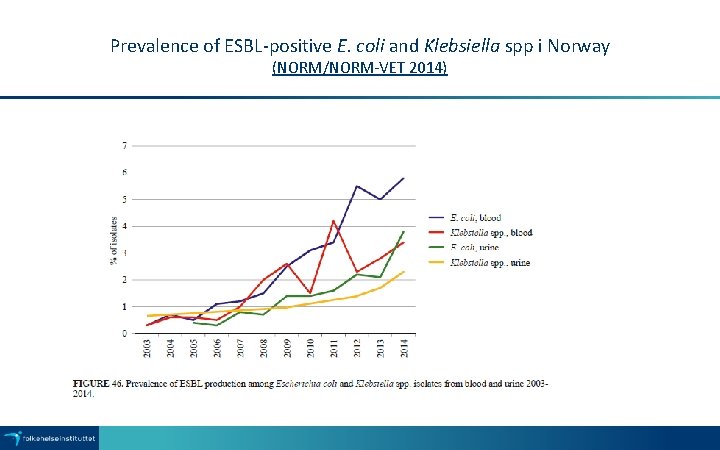
Prevalence of ESBL-positive E. coli and Klebsiella spp i Norway (NORM/NORM-VET 2014)

Objective 2. Planned activities towards the expected results • More representative and comparable AMR surveillance systems developed for implementation in the NDPHS Partner Countries – Establish AMR surveillance sites to investigate levels of specified antimicrobial resistance – Support the development of methodology for CAESAR/EARS-Net and other systems/network laboratories – Arrange workshop with participation from NDPHS Partner Countries with the aim to exchange experience and harmonize/improve data coverage • Deliverables – AMR data obtained through the AMR surveillance sites, shared internationally – Report from the workshop with recommendations and conclusions – Recommendations for harmonization and improvement of AMR surveillance systems in the NDPHS Partner Countries

Objective 2. Planned activities towards the expected results • Increased awareness of prescribers and policymakers on the antibiotic resistance situation in the Northern Dimension area and on specific measures to be taken – Assess the current national guidelines for the treatment of uncomplicated infections and antimicrobial resistance strategies – Arrange a workshop to present results of the work with the guidelines – Disseminate the results towards the target groups through relevant channels – Provide advice to relevant authorities and professional societies in order to facilitate revision of national treatment recommendations and antimicrobial resistance strategies • Deliverables – Assessment report of the national guidelines for the treatment of uncomplicated infections – Report from the workshop – Information campaigns towards the target groups
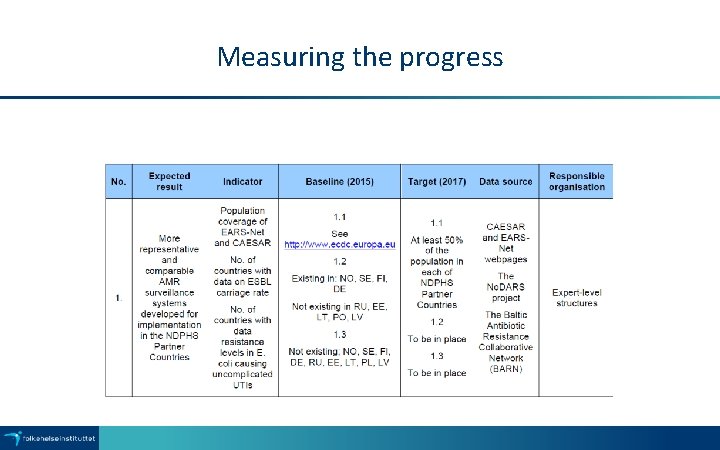
Measuring the progress

Measuring the progress

Measuring the progress
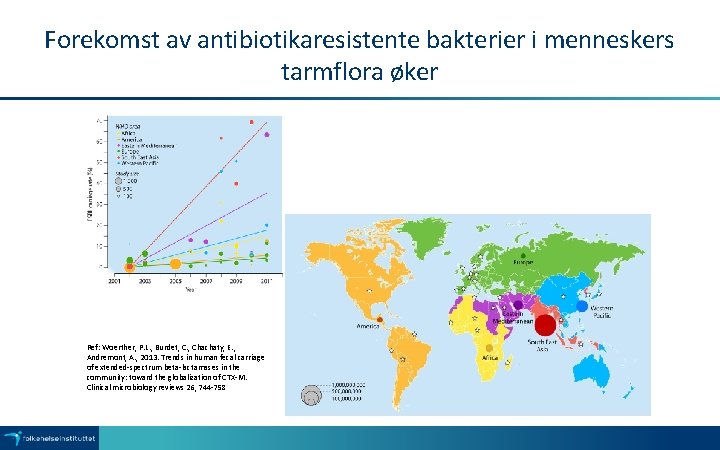
Forekomst av antibiotikaresistente bakterier i menneskers tarmflora øker Ref: Woerther, P. L. , Burdet, C. , Chachaty, E. , Andremont, A. , 2013. Trends in human fecal carriage of extended-spectrum beta-lactamases in the community: toward the globalization of CTX-M. Clinical microbiology reviews 26, 744 -758
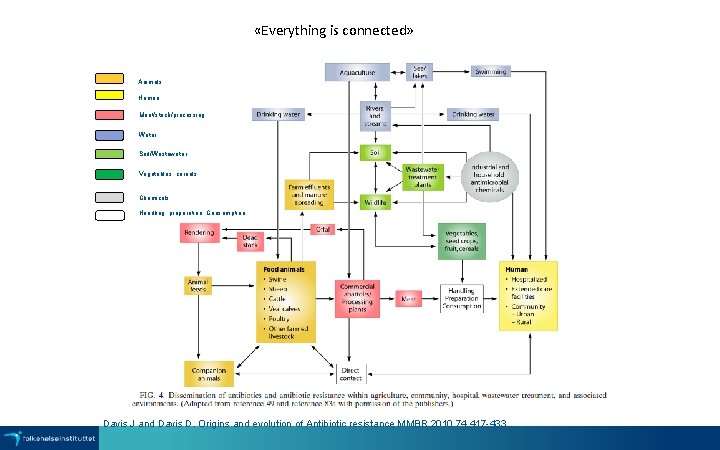
«Everything is connected» Animals Human Meat/stock/processing Water Soil/Wastewater Vegetables, cereals Chemicals Handling, preparation, Consumption Davis J and Davis D. Origins and evolution of Antibiotic resistance MMBR 2010 74 417 -433

• Thank you for your attention!
- Slides: 30