CONSTIPATION Dr Soad Jaber 2009 Constipation Physiology of

CONSTIPATION Dr. Soad Jaber 2009

Constipation Physiology of defecation u Understand the differences between u u Constipation u Encorporesis u Soiling Identify major causes of constipation u Differences between functional and organic causes u Understand the principle behind constipation management u

CONSTIPATION Physiology of defecation u In normal subjects : Distention of the rectum Reflex relaxation of internal sphincter Contraction of external sphincter *Lower rectum is normally empty *Entry of fecal material from above gives the sensation of the need to defecate. u If the rectum is chronically distended the sensation is lost retention of stool full rectum

Constipation: u u Delay or difficulty in defecation that has been present for two weeks or longer. is associated with anal and abdominal discomfort. u Full rectum

Functional Constipation: Is a voluntary withholding of stools Starts after the neonatal period Usually develop after passage of painful bowel movement.

Encopresis: u Day or night time passage of formed stool into inappropriate places beyond the age expected for toilet training (4 -5 year u Abnormal anal sphincter physiology.

Encopresis: A)RETENTIVE encopresis with constipation and overflow incontinence. 2/3 B)Non RETINTIVE encopresis: without n and overflow. 1/3 (A (A OR : 1 ry from infancy occur with global (B developmental delay and enuresis. 2 ry: after successful toilet training occur with (C psychosocial stress and mismanagement
Soiling: Involuntary escape of fluid or semi fluid stools into the under clothing usually due to overflow from a loaded cecum with feces which leads to stretch of internal sphincter

Neurogenic Soiling: Soiling which occur due to neurological abnormalities: Spinal bifida Paraplegia Myelomengiocel

Causes of Constipation: A. Infants and Children: 1. Non-organic Causes. Lack of dietary fibers. Inadequate fluid intake. Failure to develop regular bowel habits (neglect, stubborn child, MR). Follow illness. Change in environment or routine (Holidays… school entry)

Organic cause Anatomic(anaal u stenosis, imperforatecanus, anteriorly displaced anus. intestinal stricture) Abnormal musculature(prune-belly u syndrome, Gastroschisis, Down syndrome Intestinal nerve or muscle u abnormalities(Hirschprung diease) Spinal cord defects(spinal cord trauma or spina bifida) Drugs(Anticholinergics or u narcotics<Vincristine, vit D intoxication, Lead) u

Metabolic u disorders(Hypokalemia, hypercalcemia, hyp otghyroidism, D. M) Intestinal disorders: (celiac disease, cow u milk protein intolerance, meconium ileus, inflammatory bowel disease, tumour) Connective tissue u disorders SLE, sclerderma) Psychiatric diagnosis(Anorexia nervosa) u

2. Organic Causes • Hirschsprung’s disease *Clinical clues u Delayed muconium passage > 48 h or early onset of constipation u Empty rectum on examination Normal anal tone u Absence of ganglia in rectal sub mucosal biopsy u Barium enema transition zone u Manometery --- absence of internal sphincter relaxation

Conflict in training defecate Stool retention Pain in defecation withholding the stools distention of the rectum Rectal sensation necessitating a greater fecal mass to initiate the urge to

Complication of stool retention Impaction u Abdominal pain u Overflow diarrhea leakage around the fecal mass u Anal fissure u Rectal bleeding u Urinary tract infection u

Management: u History and clinical examination should reduce the number of investigation e. g. anal fissure u History of change in environment or diet u Presence of hard impacted stools u Barium study: ? XRAY. large rectum or recto -segmoid. impaction of stool

B. Elder Children He might present with recurrent abdominal pain u He might develop soiling u The elder child will eventually reach the stage where he is very quiet, withdrawn and isolated from his classmates u Parents and child should participate in a group discussion and plan the management to help the child u *If with soiling advise of Psychiatrist

1. 2. 3. 4. 5. Medical Hypertonic phosphate enemas daily or every other day for 1 week. Mineral oil 30 -60 mls twice daily between meals to minimize its effect in impairing the absorption of fat soluble vitamins -- with the response to stop within the period of about 6 months. Ensure that the child has sufficient fluid and fiber in the diet Bulk type of softness (Metamucil) maybe administered as the dose of mineral oil is tapered. Lactulose, senna, may have to be prescribed to break the vicious cycle of fecal retention and pain

Dietary Measures Intake of fluid High residual diet, bran – whole wheat Fruit and vegetable Prune Juice Anal Dilatation u Old method – local anesthesia u Well lubricated little finger inserted into the anus and kept for 1 minute

INFANTS *Treat the cause u Simple constipation … correct diet … add fiber… treat anal fissure. . Softening the stool to break the cycle u Daily stitz bath u Application of Vaseline ointment after the bath u Anesthetic ointment.

Managements: Hx Onset Associated findings FTT organic Ex Abdominal Rectal Signs of Hypothyroidism Explanation Common problem Will get better Physiology of defecation Long term managements up to 1 year

Goals: 1. Empty Rectum Clean out retained stool Enema Suppositories Senakot Bowel cleaning

2. Bulky stool High fiber diet (bran)

3. Improve habits Regular time of toilet after feed Stars chart Position- squatting De emotionalize home environment

Functional Constipation: WHY MAY THE TREATMENT FAIL ? ! u Inadequate clean out suppositories u Inadequate dosage of medication u On and off approach: Intermittent use of medication


Malabsorption Objectives: u Digestion u Definition u Identify major causes of malabsorption u Know to work up for malabsorption

Malabsorption Digestion u Stomach ------- u Small bowel---- breakdown ingested food by rhythmic contraction gastric acids. Intestinal secretion digestion. *Brush Border

Small bowel 2 halves Jejunum CHO maltose Fat F. A. mono glycerides Protien. . di , tri, tetra peptides + a. a. Minerals Vitamins Water Ileum Water B 12 Bile salts

Malabsorption Syndromes Malabsorptive disorders They are conditions that cause insufficient assimilation of ingested nutrients either as a result of mal digestion, or malabsorption. General presentation: Abdominal distention Pallor Foul smelling stools Bulky stools. . Normal… greasy…steatorrhea muscle wasting Poor weight gain … weight loss Growth retardation Clues: Acute diarrhea --- infection chronic diarrhea > 3 weeks ? Malabsorption Blood, FTT Overall appearance of the child

I. Malabsorption according to age of presentation 1. From birth up to two years of age: – – – – – Post infectious Protein intolerance Congenital microvillus inclusion disease. Glucose – galactose transport defects. Congenital chloride diarrhea Familial chronic villous atrophy Immune deficiency disease Cholestatic liver disease Gluten sensitive enteropathy Anatomical cause (short bowel syndrome) 2. Older children: – – Cystic fibrosis Crohn’s disease Gluten sensitive enteropathy Acquired lactose deficiency

II. Malabsorption according to substances: 1. Fat Celiac disease Cystic fibrosis OTHERS: Giardiasis Congenital intestinal malformation Crohn’s disease Biliary atrasia Liver cirrhosis

ydrate Glucose -galactose transport defect Genetic Lactose (Primary lactase deficiency) Sucrose (Congenital sucrase – isomaltase deficiency) Secondary celiac disease any chronic diarrhea

3. Protein Follow any chronic diarrhea Enzyme deficiency (trypsinogen) Allergy… Cow’s milk protein 4. Vitamins Fat soluble Vit. Secondary to steatorhea B 12 … Crohn’s

III. Malabsorption according to site of defects. 1. Mucosal Small intestinal injuries resulting in secondary deficiencies. - Celiac disease - Bacterial over growth - Cow’s milk enteropathy - Giardiasis - Rota virus infection - Chronic protracted diarrhea - Protein energy malnutrition - Crohn’s disease of small intestine - Short bowel syndrome - Drugs …neomycin … colchicines - Radiation enteritis
2. None mucosal Pancreatic disease Bile losses ------ cystic fibrosis ---- bacterial overgrowth deconjugation of bile acids Cholestasis Lymphatic obstruction-----lymphagiactasia A Beta–lipo proteinemia

How to approach: History: u u u Is he/she thriving Weight/height Appetite Other symptoms --- edema Repetition of symptoms with reintroduction of certain foods e. g. Gluten Lactose Cow’s milk u Stool Greasy Oil slik in the toilet Frothy – sugar intolerance Smell --- Rancid, CF -----foul, celiac
Examination Growth chart Pallor --- Iron, folate Clubbing CF, IBD, CD Chest problem CF Distended abdomen CD Muscle hypotonia + wasting Nappy rash Rectal examination (prolapsed)

Laboratory investigations: 1. Stool 1. microscopic examination – Fat droplet (stool + water + Sudan red stain) – 72 hours stool collection – Stool Giardia Cyst ELISA for Giardia antibodies. 2. Stool PH 5. 6 (CHO) 3. Spot antitrypsin level ( 2 days stool)

4. Stool reducing substance – Chromatography – Clintest tab 10 drops water + 5 drops stool+tab (-ve -- 4+) Color coding 2 + or suggest CHO malabsorption Sucrose is not reducing substance Should be hydrolyzed by HCl before analysis

5. Stool osmolarity (stool electrolyte content) 290 - 2(Na + K ) meq/L 100 mosm/L secretary as in cong chloride diarrhea u 100 mosm/L Osmotic diarrhea CHO intolerance u
2. Blood u CBC— u Serum albumin Serum immunoglobulins Trypsinogen (screening) Nutrients in blood u u u blood film------- A canthocyte hypochromic, microcytic anemia macrocytosis Iron. . Transferrin concentration folic acid –---- RBCs concentration , serum Ca, Mg, Vit D. , Vit A B 12 -- bile salt Vit E + Serum lipids Vit K ( PT , PTT) not

3. Others u Sweat chloride test u Hydrogen breath test u D-xylose test u Schilling test (Vit B 12)

4. Diagnostic Procedure: 1. Small bowel biopsy: 1. Duodenal mucosa Giardia trophozoite Colony count of bacteria Culture of proximal juice 2. For HIV parasitic bacteria or virus viral opportunistic entral pathogen 3. Gluten sensitive enteropathy Challenge test 4. Congenital microvillous inclusion disease 5. Eosinophillic gastroenteritis 6. Infectious disorders
2. Imaging procedure X-ray – site of colon - e. g. intestinal mal rotation Ultra sound (biliary tree. . Pancreas) Barium contrast meal and follow through Barium enema

Review of some disorders I. Disorders of CHO intolerance Symptoms Flatulence, Diarrhea, bloating, vomiting, abdominal cramping, barborygmi A. Congenital Disorders Lactose deficiency cong (rare) Acquired TX Lactose hydrolyzed milk. Lactid tab u u Sucrase deficiency: Recurrent watery diarrhea, u stool PH below 6 Glucose – Galactose malabsorption. Very rare neonates acidosis TX fructose formula severe hypoglycemia –

B. Acquired disorders: Secondary to acute viral OR bacterial gastro enteritis…. lactase def > sucrase u Generally children tolerate lactose withen (3 w-3 m) Stool PH 6 +ve clinitest tab u Secondary to celiac disease, Crohn’s disease, ulcerative colitis TX – lactose free diet u

II. Disorders of Proteins u Cow’s milk protein sensitivity A topic individuals Jejunal atrophy Colonic bleeding Iron deficiency anemia unresponsive to treatment with oral iron. TX D/C milk Repeat challenge with carefully increasing dose majority will tolerate milk by two years. 40% intolerant to Soya protein.

u Celiac disease u. Allergy to Gliaden portion of gluten (wheat, Rye, Oats or barley) – Screening antibodies Antigliadin Ig. A, Anti reticulin, Anti endomyseal EMA

Celiac Sprue: Gluten sensitive enteropathy C/P Abdominal distention Weight loss –FTT irritability Vomiting Steotorrhea mild cases, IDA, , , short stature , , , delayed puberty Investigation: Serum Iron folic acid albumin Flat Glucose tolerance test EMA +ve, , , +ve Antigliadin Small bowel biopsy 100% diagnostic - villous atrophy on a gluten free diet - Recurrence after a gluten challenge Treatment: Gluten free diet for life Prognosis: Strict diet - Normal growth – health - 1% lymphoma

Causes of flat small intestinal mucosa: 1. 2. 3. 4. 5. 6. 7. 8. Celiac disease Cow’s milk protein sensitivity Post enteritis syndrome Giardiasis Tropical sprue Soya protein intolerance Autoimmune enteropathy Protein energy malnutrition

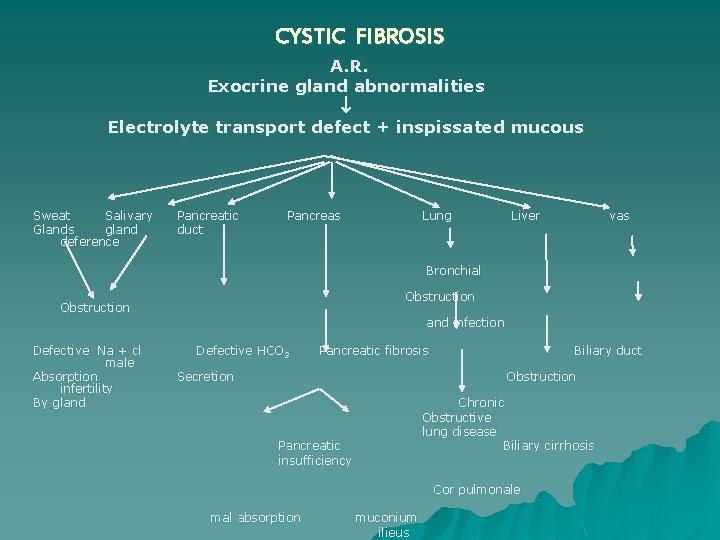
Mucoviscidosis Cystic fibrosis u u AR Defect: Mucus secreted by exocrine glands is abnormally thick and sticky due to defect in chloride permeability which lead to failure in maintaining the luminal hydration. It is an obstructive lesion in which a duct or airway passage is blocked by intra luminal mucous and other protein. 60% presents before 1 year. 85% before 5 years

C. P. Most presented with failure to thrive frequent foul smelling stocl Rectal prolapse 18. 5% by 1 -2 Yr. 10% muconium illeus - a plug of muconium in the terminal ileum which lead to ischemic ulceration and peritonitis - delayed passage of muconium in neonate 10% Pancreatic fibrosis Exocrine insufficiency malabsorption

80% Recurrent chest infection Atelactasis Bronchiactasis Emphysema Corpulmonal death Rare Boys Azospermia infertility Liver obstructive jaundice biliary cirrhosis Gallbladder Gall stones

Investigation: 1. 24 hour stool chymotripsin 2. True test for pancreatic function : by low enzyme output from Pancreas, follow stimulation by secretin and cholecytokinin 3. Sweat test. (Sweat chloride measurement) 60 meq/L ---- diagnostic If doubtful as is cases of edema , sweat test should be repeated once edema subside Treatment: Enteric coated – acid resistant oral pancreatic enzyme supplements Diet high in protein, low fat or MCT diet
CYSTIC FIBROSIS A. R. Exocrine gland abnormalities Electrolyte transport defect + inspissated mucous Sweat Salivary Glands gland deference Pancreatic duct Pancreas Lung Liver vas Bronchial Obstruction Defective Na + cl male Absorption infertility By gland infection Defective HCO 3 Pancreatic fibrosis Secretion Biliary duct Obstruction Chronic Obstructive lung disease Biliary cirrhosis Pancreatic insufficiency Cor pulmonale mal absorption muconium ilieus

Inflammatory bowel disease A. Croh’s disease: Regional enteritis Transmural inflammation with skip areas Genetic predisposition C/P Post prandial abdominal pain. ± diarrhea or constipation weight loss fever arthralgia /arthritis 2% Erythema nodosum Investigations: ESR Anemia albumin : Proctoscopy Double contrast colon X-ray Rectal biopsy Treatment: iron Enteral or parentral nutrition Medicine - Prednisone - Sulfasalazine (if colonic involvement) - Azathoprine - Cyclophosphamide -70% surgical treatment

B. Ulcerative colitis u u Mucosal inflammation ---rarely involve muscularis layer Toxic mega colon C/P bloody diarrhea + tenesmus Complication Hge Mega colon intractable symptoms Arthalgia / arthritis high risk of colonic cancer Treatment: Enteral and parentral nutrition medical: - Sulfasalazine oral - hydro cortison enema - systemic predisone - Cyclo sporins 25% surgical treatment colectomy if mega colon

Thank You
- Slides: 59