Consequences of thrombus consequences angina Myocardial infaction stroke
Consequences of thrombus consequences angina Myocardial infaction stroke Deep venous thrombosis
Anticoagulant Therapy Treatment of thrombus Prevent Thrombosis ØAnticoagulants ØAntiplatelets Removing the occlusion ØThrombolysis ØCoronary angioplasty Vasodilation ØNitrates ØCCB

Coagulation Cascade n Ø Ø Ø Anticoagulant therapy is aimed to: Prevent clot in patients at risk Prevent clot extension/ embolism Deep venous thrombosis (DVT) & pulmonary embolism (PE) Coagulation cascade Activated factor X (FXa) + FVa + Ca++ + phospholipids Prothrombin (FII) thrombin (FIIa) Fibrinogen fibrin blood clot Present on platelets’ surfaces. Act by accelerating thrombus formation.
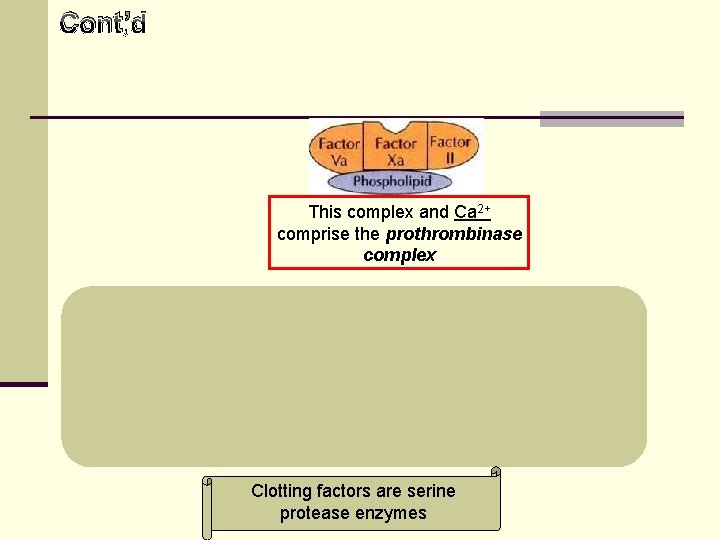
Cont’d This complex and Ca 2+ comprise the prothrombinase complex Thrombin stimulates platelet aggregation Coagulation ↑ platelet aggregation Phospholipids on platelets stimulate clot formation Clotting factors are serine protease enzymes

The Key Clotting Factor is: THROMBIN Because it acts on many aspects of the coagulation cascade
Scheme of anticoagulant drugs Anticoagulant drugs oral warfarin injected Direct acting: Lepirudin Antithrombin III dependent: heparin Low molecular weight heparin

THROMBIN INHIBITORS n Thrombin inhibitors can either inactivate thrombin directly or block thrombin formation n Thrombin can be inhibited irreversibly by glycosaminoglycans like heparin through an antithrombin III-dependent mechanism n The enzyme can be inhibited reversibly by hirudin and hirudin derivatives in an antithrombin III-independent manner (direct acting) n In addition to inhibiting thrombin, glycosaminoglycans also block thrombin generation

Antithrombin-III Dependent Thrombin Inhibitors q q q ü Standard Unfractionated Heparin (UFH) Heparin is a mixture of glycosaminoglycan molecules, which are heterogenous in molecular size The mean molecular weight of heparin is 15, 000 D Antithrombin III (ATIII) binding is necessary for its anticoagulant activity Antithrombin III (ATIII) is a slow endogenous progressive inhibitor of thrombin and other clotting enzymes (FXa)
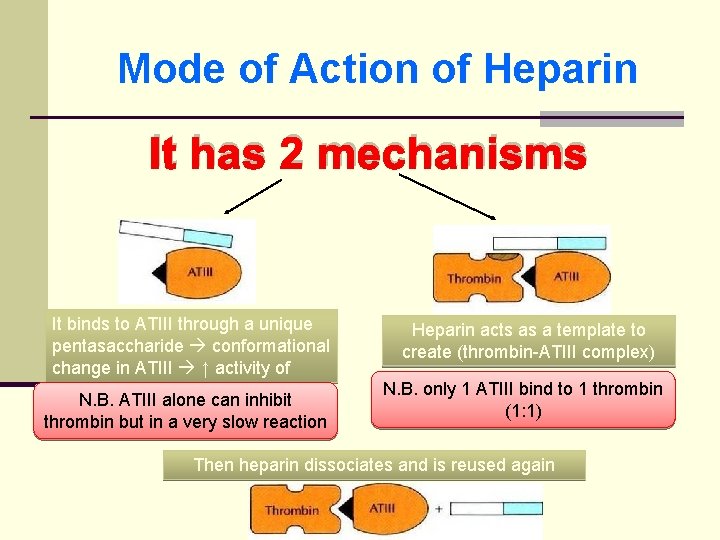
Mode of Action of Heparin It has 2 mechanisms It binds to ATIII through a unique pentasaccharide conformational change in ATIII ↑ activity of ATIII N. B. ATIII alone can inhibit thrombin but in a very slow reaction Heparin acts as a template to create (thrombin-ATIII complex) N. B. only 1 ATIII bind to 1 thrombin (1: 1) Then heparin dissociates and is reused again
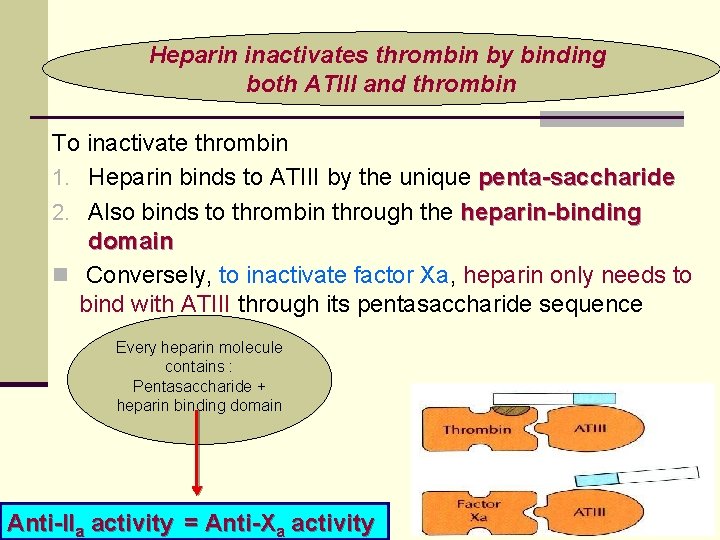
Heparin inactivates thrombin by binding both ATIII and thrombin To inactivate thrombin 1. Heparin binds to ATIII by the unique penta-saccharide 2. Also binds to thrombin through the heparin-binding domain n Conversely, to inactivate factor Xa, heparin only needs to bind with ATIII through its pentasaccharide sequence Every heparin molecule contains : Pentasaccharide + heparin binding domain Anti-IIa activity = Anti-Xa activity
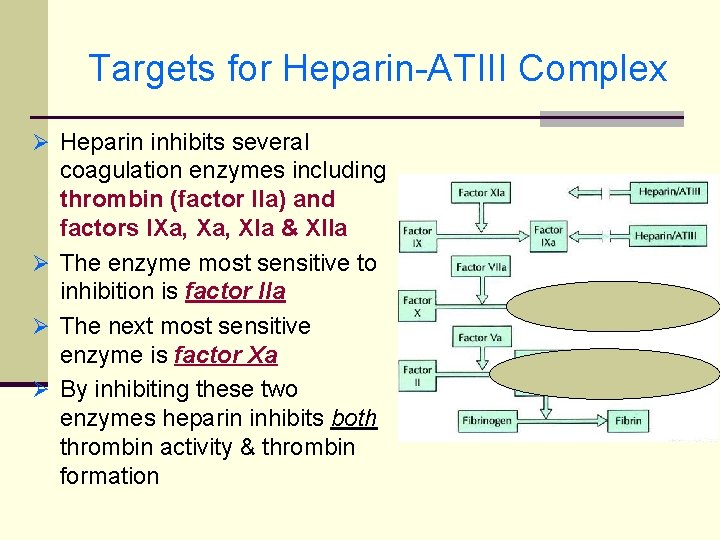
Targets for Heparin-ATIII Complex Ø Heparin inhibits several coagulation enzymes including thrombin (factor IIa) and factors IXa, XIa & XIIa Ø The enzyme most sensitive to inhibition is factor IIa Ø The next most sensitive enzyme is factor Xa Ø By inhibiting these two enzymes heparin inhibits both thrombin activity & thrombin formation

Limitations to Heparin’s use Need to be given in hospital and monitoring the patient

Low Molecular Weight Heparins (LMWHs) q Low molecular weight heparin have a mean molecular weight of 5000 D. q Prepared by controlled chemical or enzymatic depolymerization of standard unfractioned heparin are about ⅓ the size of starting material q 20% of LMWH molecules contain the pentasaccharide domain q Enoxaparin is the most used LMWH
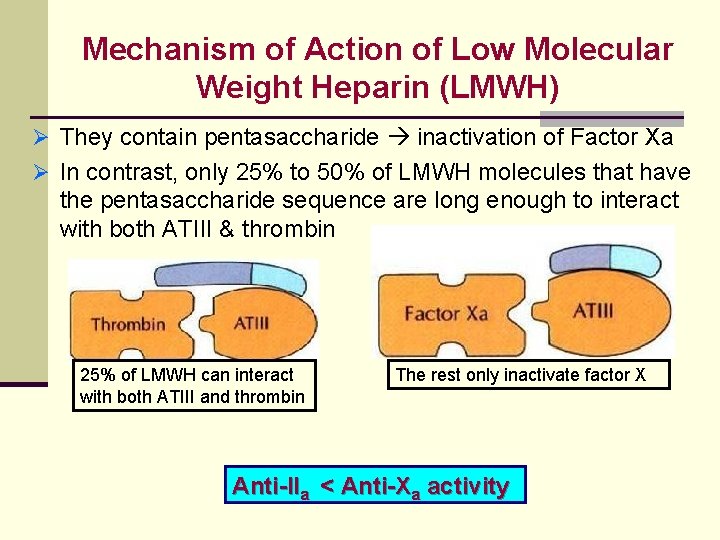
Mechanism of Action of Low Molecular Weight Heparin (LMWH) Ø They contain pentasaccharide inactivation of Factor Xa Ø In contrast, only 25% to 50% of LMWH molecules that have the pentasaccharide sequence are long enough to interact with both ATIII & thrombin 25% of LMWH can interact with both ATIII and thrombin The rest only inactivate factor X Anti-IIa < Anti-Xa activity

Pharmacokinetic Profile of LMWH Ø LMWH exhibit less binding to plasma proteins & cell Ø ü ü Ø Ø surfaces (better than heparin) The reduced binding to plasma proteins results in Better bioavailability (90% vs. 20% of heparin) more predictable anticoagulant response Laboratory monitoring of LMWH activity is not required LMWH has low resistance in comparison to heparin T 1/2 = 4 hours (more than heparin) Given at fixed doses once to twice daily by S. C. route, and is given for both inpatients as well as for outpatients.
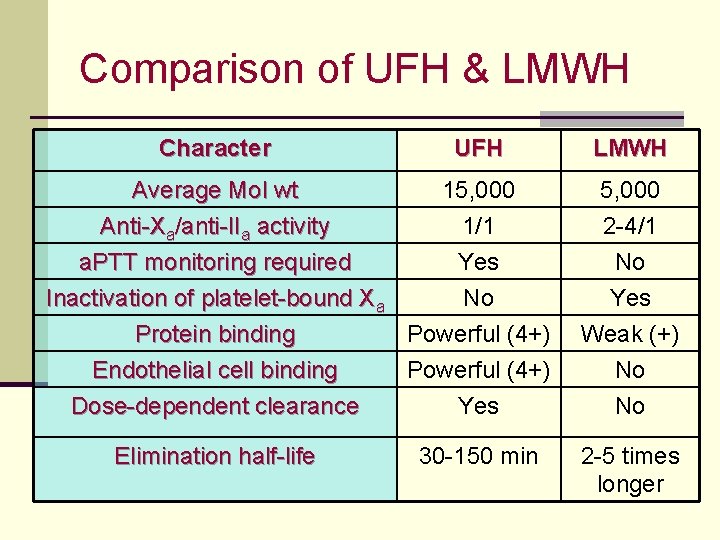
Comparison of UFH & LMWH Character UFH LMWH Average Mol wt Anti-Xa/anti-IIa activity a. PTT monitoring required 15, 000 1/1 Yes 5, 000 2 -4/1 No Inactivation of platelet-bound Xa No Protein binding Powerful (4+) Endothelial cell binding Powerful (4+) Dose-dependent clearance Yes Elimination half-life 30 -150 min Yes Weak (+) No No 2 -5 times longer
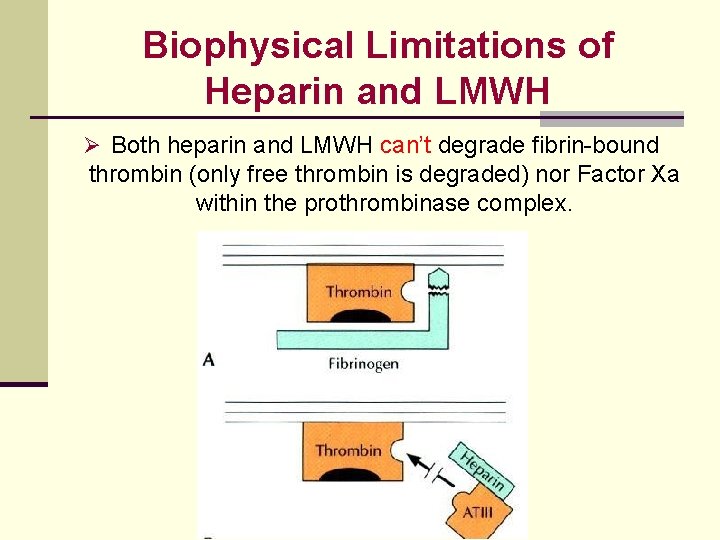
Biophysical Limitations of Heparin and LMWH Ø Both heparin and LMWH can’t degrade fibrin-bound thrombin (only free thrombin is degraded) nor Factor Xa within the prothrombinase complex.

Other Injectable Antithrombotic Agents n Fondaparinux, Fondaparinux a pentasaccharide, is an AT-III-dependent selective for factor Xa Ø Prevents venous thrombosis associated with orthopedic surgery Ø Administered > 6 hours postoperatively and the dose is adjusted for patients with renal impairment. To be revised …….

Therapeutic Uses o Heparin should be given either IV or S. C. injection. o onset of action: few minutes (IV) 1 -2 hours (S. C. ) o LMWHs are given by S. C. route o I. M. injection hematoma formation (thus is avoided) q Treatment of deep vein thrombosis q Treatment of pulmonary embolism q Prevention of postoperative venous thrombosis in patients with acute MI phase or one undergoing elective surgery(not emergency surgery) q Reduction of coronary artery thrombosis after thrombolytic treatment q Heparin is the anticoagulant of choice in pregnant women

Adverse Effects n Bleeding: they both lead to bleeding but the bleeding is less in LMWH Ø To treat bleeding: inject antidote protamine sulphate (1 mg IV for each 100 units of UFH) (reversal effect) n Thrombosis: heparin ↓ ATIII ↑ risk of thrombosis

Cont’d Thrombocytopenia: Heparin-induced thrombocytopenia (HIT) is a lifethreatening immune reaction ØOccurs in 3% of patients ØUsually occurs a week from starting heparin therapy ØHIT ↑ platelet activation platelet aggregation thrombosis. ØHIT endothelial damage ØHIT may occur in the early stages of treatmen (within 5 days) but it’s non-immune reaction (not life threatening) ØLMWHs, though of lower risk, are contraindicated with HIT. For patients with HIT we use lepirudin

How does HIT occur? n Heparin injection immune reaction with body produce antibody against heparin& also bind to platelet receptor activation of platelet thrombosis

Cont’d q Osteoporosis occurs with large doses of UFH >20, 000 U/day for 6 months or longer (chronic use) q Hyperkalemia rarely occurs with UFH Ø It is attributed to inhibition of aldosterone secretion Ø It occurs with both low- & high-dose UFH therapy Ø Onset is quick within a week after therapy initiation Ø It is reversible by therapy discontinuation Ø Diabetic & renal failure patients are at higher risk q Hypersensitivity: (Antigenicity due to animal source) ü rarely occurring reactions include urticaria, rash, rhinitis, angioedema & reversible alopecia(hair loss)
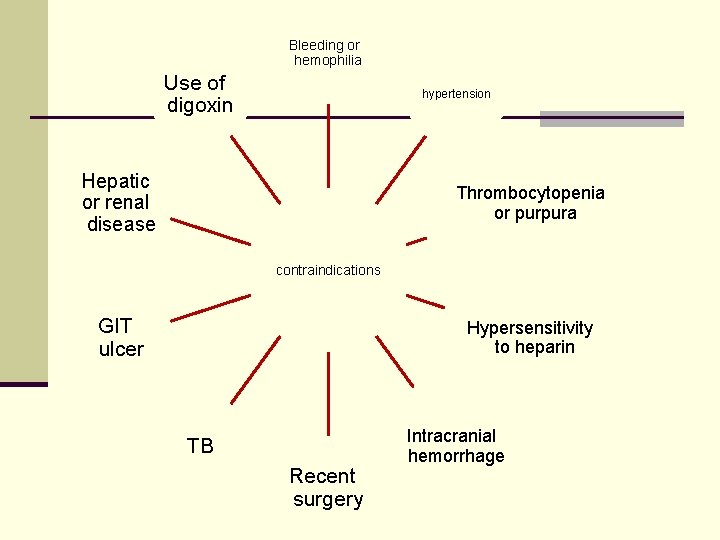
Bleeding or hemophilia Use of digoxin hypertension Hepatic or renal disease Thrombocytopenia or purpura contraindications GIT ulcer Hypersensitivity to heparin TB Recent surgery Intracranial hemorrhage

Clinically Approved Direct Thrombin Inhibitors n n n Ø Lepirudin, recombinant hirudin*-like peptide. Direct acting thrombin inhibitor Used in HIT patients (IV injection) Has renal clearance It acts on free thrombin and thrombin bound to fibrin It has potential use in unstable angina patients and after thrombolysis It binds to active site and substrate site of thrombin * hirudin: is a leech derived anticoagulant

DIRECT FACTOR Xa INHIBITORS FXa inhibitors Tick anticoagulant peptide (TAP) antistatin They are available by recombinant technology Differs from heparin Independent of AT III Inhibit FXa within prothrombinase complex

Oral Anticoagulants Vitamin K Antagonists (The Coumarins) n Vitamin K is co-factor for the hepatic synthesis of clotting factors II, VII, IX & X warfarin Vit. K By Vit. k reductase Vit. K epoxide (active form) Warfarin inhibits Vit. K reductase no active form of Vit. K no synthesis of clotting factors

Vitamin K Antagonists Warfarin Ø Onset: starts after 12 -16 hours Ø lasts for 4 -5 days Ø Clinical anticoagulant activity needs several days to develop (due to the already circulating clotting factors) o So the action of warfarin will appear after the elimination of prior clotting factors. o Elimination time (factor II needs: 60 hours factor X: 40 hours) q Overlap heparin & warfarin therapy taken together until the effect of warfarin appears (after 5 days) then stop taking heparin.

Vitamin K Antagonists Warfarin q Warfarin has 100% oral bioavailability, high plasma protein binding & long plasma t 1/2 of 36 hours q A high loading dose followed by an adjusted maintenance dose q Warfarin is contraindicated with pregnancy as it crosses the placental barrier and is teratogenic in the first trimester & and induce intracranial hemorrhage in the baby during delivery q Warfarin is metabolized by hepatic Cytochrome P 450 enzymes with half-life of 40 hrs

Warfarin Drug Pharmacokinetic & Pharmacodynamic Interactions Ø Ø Ø Potentiating warfarin Inhibitors of hepatic P 450 enzymes (cimetidine, cotrimoxazole, imipramine, amiodarone) Platelet aggregation inhibitors (NSAIDs e. g. aspirin) 3 rd generation cephalosporins* Drugs displacing warfarin from binding sites (NSAIDs) Drugs reducing the availability of vitamin K § § § Inhibiting Warfarin Vitamin K in some parenteral feed Inducers of hepatic P 450 enzymes (rifampicin, barbiturates, … etc) Reduction of GIT absorption (cholestyramine) Diuretics Hypothyroidism Ø Hepatic disease(↓ clotting factors)& hyperthyroidism (↑ basal metabolic rate) *Cephalosporins potentiate warfarin’s effect by killing vit. k producing normal flora

Warfarin Side-Effects n Drug-drug interactions n Bleeding disorder (thus should be monitored) Treatment for bleeding • Minor bleeding: stop therapy + oral Vitamin K • Severe Bleeding: stop therapy + I. V. Vitamin K fresh frozen plasma, recombinant factor VIIa or prothrombin complex may be used
- Slides: 31