CONNECTIVE TISSUE DISEASES Dr Rzan Objectives 1 define


CONNECTIVE TISSUE DISEASES Dr. Rzan

Objectives: � 1 - define CT. diseases. � 2 -Identify the common CT. diseases.

� The connective tissue diseases are a group of chronic inflammatory disorders that involve multiple body systems and exhibit a wide spectrum of clinical manifestations.

Aetiology �Their aetiology is multifactorial and involves: 1. Genetic, 2. Immunological (especially autoantibody production) 3. Environmental factors

SYSTEMIC LUPUS ERYTHEMATOSUS �SLE is the most common multisystem connective tissue disease. �It is characterised by a diverse spectrum of autoantibody production. � wide variety of clinical features.

�The prevalence varies according to geographical and racial background. �Around 90% of affected are women. �with peak onset in the second and third decades.

Aetiology and pathogenesis �Autoantibodies production. �At least 50 antigen targets for autoantibody production. �polyclonal B- and T-cell activation. �Many autoantigens in SLE are components of the intracellular and intranuclear machinery. �one mechanism may be exposure of intracellular antigens on the cell surface during apoptosis. .

Environmental factors that associate with flares of lupus: 1 -sunlight and artificial ultraviolet (UV) light. 2 -Pregnancy. 3 -Infection. -increase oxidative stress and subsequent apoptosis

REVISED AMERICAN RHEUMATISM ASSOCIATION CRITERIA FOR S L E Features 1. Malar rash 2. Discoid rash 3. Photosensitivity 4. Oral ulcers Characteristics �Fixed erythema, flat or raised, sparing the nasolabial folds �Erythematous plaques with adherent keratoticscales, scarring and follicular plugging �Rash as a result of unusual reaction to sunlight �Oral or nasopharyngeal ulceration, which may be painless

5 -Arthritis 6 -Serositis 7 --Renal disorder 8 --Neurological disorder �Non-erosive, two or more peripheral joints. �Pleuritis or Pericarditis �Persistent proteinuria > 0. 5 g/day or Cellular casts �Seizures or psychosis. 9 -Haematological disorder �Haemolytic anaemia or 11 -Antinuclear antibody (ANA) �Abnormal titre of ANA by Leucopenia 2 (< 4 ×× 109/l), or Lymphopenia 2 (< 1 ×× 109/l), or Thrombocytopenia 2 (< 100 ×× 109/l) in the 10 -Immunological �Anti-DNA antibodies or antibody to Sm disorder antigen or antiphospholipid antibodies. immunofluorescence

SLE is diagnosed by presence of 4 out of these 11 criteria �Mucocutaneous features �It is obvious that 4 of the 11 criteria were mucocutaneous. � 20% of all SLE cases present with initial skin manifestations. � 50– 70% of all SLE patients will eventually show skin symptoms during the course of their disease.

There are three main types OF LE 1. SLE. 2. Subacute cutaneous lupus erythematosus (SCLE). 3. Discoid lupus erythematosus (DLE).

The classic butterfly facial rash of SLE. �(20 -30% of patients) is painful or pruritic erythematous plaques and occurs in a photosensitive distribution that involves the cheecks , nasal bridge and spares the nasolabial folds.






Subacute cutaneous lupus erythematosus (SCLE): rashes are migratory nonscarring and either q (psoriasiform) q or annular with characteristic shawl distribution. .





Discoid lupus erythematosus (DLE) �lesions are long-lasting for up to decades. �discoid erythymatous scaly plaques with follicular plugging. �the scales are adherent and there removal may leave pits (carpet-tack sign). �healing in an area and continuing in another. �healing occurs with scarring and hypopigmentation.

�Scarring alopecia may result if DLE present on the scalp. �The external ear is a predilection sites of DLE. �When DLE lesions are present below the neck line it is concedered as generalised.



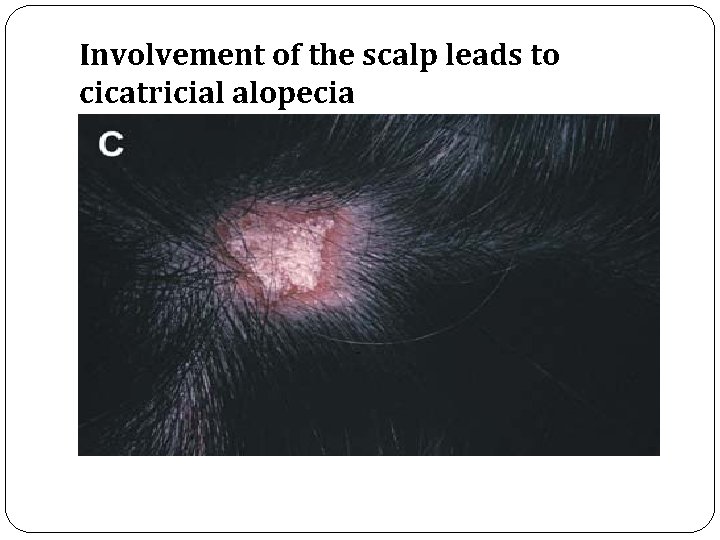
Involvement of the scalp leads to cicatricial alopecia


�Painful oral ulcers are common in SLE. � Diffuse, non-scarring, alopecia may occur with active disease � Raynaud's phenomenon. � Vasculitis. � livedo reticularis �periungual erythema. � Examination of nail-fold capillary loops using a dermtoscope may show loss of the normal loop pattern and capillary 'fallout' with haemorrhage and dots.



�Differential diagnosis of butterfly rash: 1 -SLE. 2 - rosacea. 3 -Polymorphic light eruption. PLE. 4 -Seborrhoic dermatitis. �Differential diagnosis of discoid lesion: 1 -DLE. 2 -DISCOID ECZEMA 3 -Tinea. 4 -psoriasis (silvery scale). 5 -lupus vulgaris (diascopy: apple jelly)
Histological findings 1. epidermal hyperkeratosis. 2. basal cell liquefaction degeneration. 3. thickening of the basement membrane. 4. mononuclear cell infiltrateat the dermo- epidermal junction , around blood vessels and adnexial structures. 5. Direct Immunofluorescence examination shows granular deposits of mostly Ig. G, Ig. M and complement C 3 in a continuous line along the dermo-epidermal junction (so-called lupus band ).

Management � General; avoiding sun and UV light exposure. � Topical: potent steroids for skin leasions. � Systemic: 1 - Intermittent NSAIDs. 2 -Hydroxychloroquine (200 -400 mg daily). 3 -Short courses of oral corticosteroids for mild to moderate disease activity. 4 -Acute or life-threatening disease requires highdose corticosteroids ( prednisolone 40 -60 mg daily or i. v. methylprednisolone 500 mg-1 g) in combination with pulse i. v. cyclophosphamide. 5 - immunosuppressive drugs (azathioprine, methotrexate, ciclosporin, , mycophenolate mofetil) are useful either alone or in combination with corticosteroids.

Prognosis �Overall 5 -year survival is greater than 90%. �Early mortality within 5 years of diagnosis is usually due to organ failure or sepsis. �the late mortality mainly results from premature cardiovascular disease to which chronic corticosteroid therapy contributes. �To reduce this, steroids should be used at the lowest effective dose and for the shortest period possible; combination therapy with immunosuppressive drugs may help to achieve this.
- Slides: 38