Connecting the Dots Improving Unit Safety Culture to






![Positive Correlation: HSOPS and Patient Satisfaction 6 “…. behaviors and attitudes [of hospital employees] Positive Correlation: HSOPS and Patient Satisfaction 6 “…. behaviors and attitudes [of hospital employees]](https://slidetodoc.com/presentation_image_h/f52f4a7a7d3f929fb2258d1796095b3c/image-8.jpg)































- Slides: 49

Connecting the Dots: Improving Unit Safety Culture to Stop HAI Katherine J. Jones, PT, Ph. D University of Nebraska Medical Center

Supported By • AHRQ Partnerships in Implementing Patient Safety Grants (1 U 18 HS 015822, 1 R 18 HS 021429) The content is solely the responsibility of the author and does not necessarily represent the official views of the Agency for Healthcare Research and Quality. • National Rural Health Association • Nebraska Department of Health and Human Services • AHRQ Office of Communications and Knowledge Transfer • Hospitals in Nebraska, Iowa, Louisiana, Washington, Oregon, Alaska 2

Learning Objectives • Define safety culture • Describe how to measure safety culture • Explain the relationship between prevention and healthcare-associated infections and safety culture 3

What is Safety Culture • • • 4 Definition Role of Organizational Culture Categories of Culture 3 Levels of Culture 4 Components of Culture

Definition of Safety Culture • Enduring, shared, LEARNED 1 beliefs and behaviors that reflect an organization’s willingness to learn from errors 2 • Four beliefs present in a safe, informed culture 3 – – 5 Our processes are designed to prevent failure We are committed to detect and learn from error We have a just culture that disciplines based on risk taking People who work in teams make fewer errors

The Role of Organizational Culture 1 Safety Culture 4 • Allows us to make sense of environment • Reflects common language… is heard and observed • Leaders create/teach culture • A cross cutting contextual factor • Moderates effectiveness of patient safety interventions • Associated with adverse events and patient satisfaction 6 – Share information – Reward, provide feedback – Hold people accountable

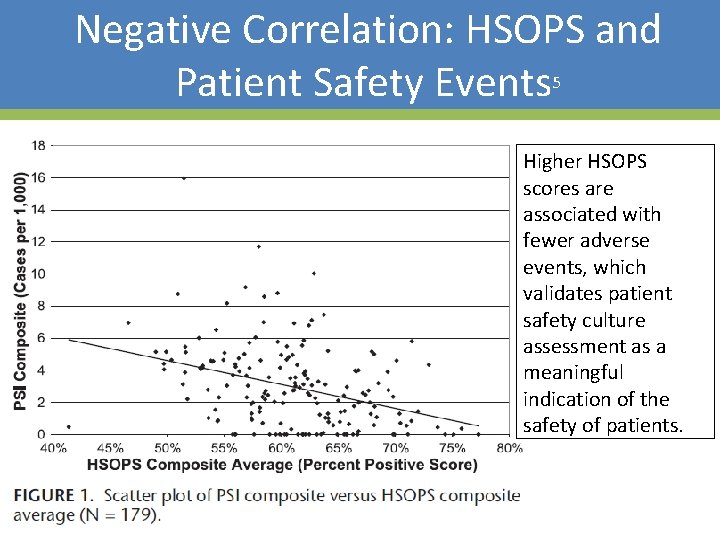
Negative Correlation: HSOPS and Patient Safety Events 5 Higher HSOPS scores are associated with fewer adverse events, which validates patient safety culture assessment as a meaningful indication of the safety of patients.
![Positive Correlation HSOPS and Patient Satisfaction 6 behaviors and attitudes of hospital employees Positive Correlation: HSOPS and Patient Satisfaction 6 “…. behaviors and attitudes [of hospital employees]](https://slidetodoc.com/presentation_image_h/f52f4a7a7d3f929fb2258d1796095b3c/image-8.jpg)
Positive Correlation: HSOPS and Patient Satisfaction 6 “…. behaviors and attitudes [of hospital employees] can directly affect the pain, discomfort, health, and recovery of patients. ”

Categories of Culture 1 • Macroculture • Subculture • Microculture • Organizational Culture 9

Three Levels of Organizational Culture 1 “…values reflect desired behavior but are not reflected in observed behavior. ” (Schein, 2010, pp. 24, 27) Behaviors Beliefs & Values 10 Underlying Assumptions Desired Behavior: Observed Behavior: Round to assess catheter Do not participate in appropriateness rounds Value: Teamwork Value: Autonomy Assumption: Safety is a system property Assumption: Safety is a result of individual competency

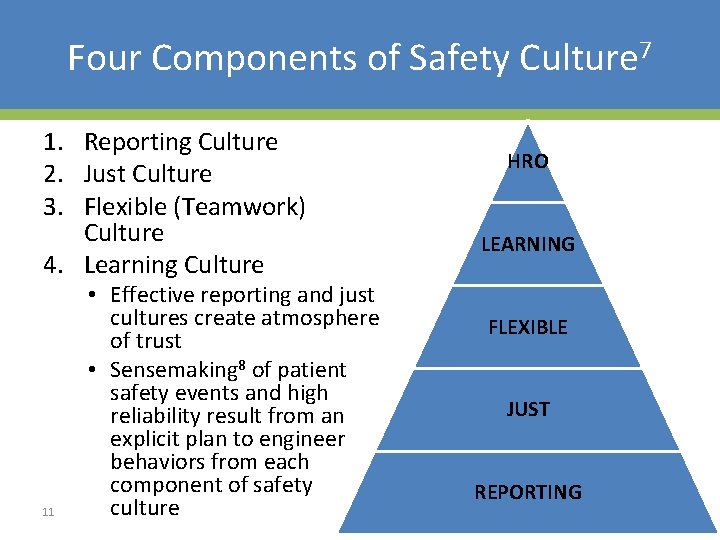
Four Components of Safety Culture 7 1. Reporting Culture 2. Just Culture 3. Flexible (Teamwork) Culture 4. Learning Culture 11 • Effective reporting and just cultures create atmosphere of trust • Sensemaking 8 of patient safety events and high reliability result from an explicit plan to engineer behaviors from each component of safety culture HRO LEARNING FLEXIBLE JUST REPORTING

Continuous Quality Improvement HROs Engage in Continuous Improvement Measure Beliefs and Behaviors Action Plan Implement Practices We can not change what we do not measure! 12

How Do you Measure Safety Culture? 1 • Qualitative – Focus Groups – Structured Interviews – Observation • Quantitative Survey Tools…use best tool for your setting – Goals of assessment 13

1, 9, 10 Goals of Culture Assessment • Identify areas of culture in need of improvement – Identify impairments in organizational learning • Increase awareness of patient safety concepts • Evaluate effectiveness of patient safety interventions over time • Conduct internal and external benchmarking, • Meet regulatory requirements • Identify gaps between beliefs and observed behaviors within subcultures and microcultures 14

When Should you Measure Safety Culture? 11 • Baseline prior to patient safety intervention • 12 – 24 month intervals to monitor change over time 15

Hospital Survey on Patient Safety 12 Culture • Survey tool kit available http: //www. ahrq. gov/qual/patientsafetyculture/hospsurvindex. htm • Comparative Database for Benchmarking http: //www. ahrq. gov/qual/hospsurvey 12/ – 1, 128 hospitals; 567, 703 respondents in 2012 database • 42 items categorized in 12 composites/dimensions – 9 dimensions measure culture at dept/unit level – 3 dimensions measure culture at hospital level • 2 additional outcome measures at dept/unit level (Patient Safety Grade, Number of Events Reported) • Comments 16

How Do you Interpret HSOPS Results? 1. Reason’s Components of Safety Culture 7 2. Identify unit-wide areas in need of improvement 3. Conduct external benchmarking 9 o State Averages o National Database ICU 4. Conduct internal benchmarking 9 o Nurse vs. Non-nurse (professional subcultures) 5. Understand Reverse-worded Items 6. Identify beliefs & behaviors in composites 1 17

Crosswalk Reason’s Components 7 Reason’s Components 4 HSOPS Dimension or Outcome Measure Reporting Culture – a safe organization is dependent on the willingness of front-line workers to report their errors and near-misses • Frequency of Events Reported (U) • Number of Events Reported (O) Just Culture – management will support and reward reporting; discipline occurs based on risktaking • Nonpunitive Response to Error (U) O=Outcome Measure, U=Unit, H=Hospital 18

Crosswalk Reason’s Components 7 Reason’s Components 4 HSOPS Dimension or Outcome Measure Flexible Culture - authority patterns relax when safety information is exchanged because those with authority respect the knowledge of front-line workers • • • Teamwork w/in Units (U) Staffing (U) Communication Openness (U) Teamwork ax Units (H) Hospital Handoffs (H) Learning Culture - organization will analyze reported information and then implement appropriate change • • • Hospital Mgt. Support (H) Manager Actions (U) Feedback & Communication (U) Organizational Learning (U) Overall Perceptions (U) Patient Safety Grade (O, U) 19

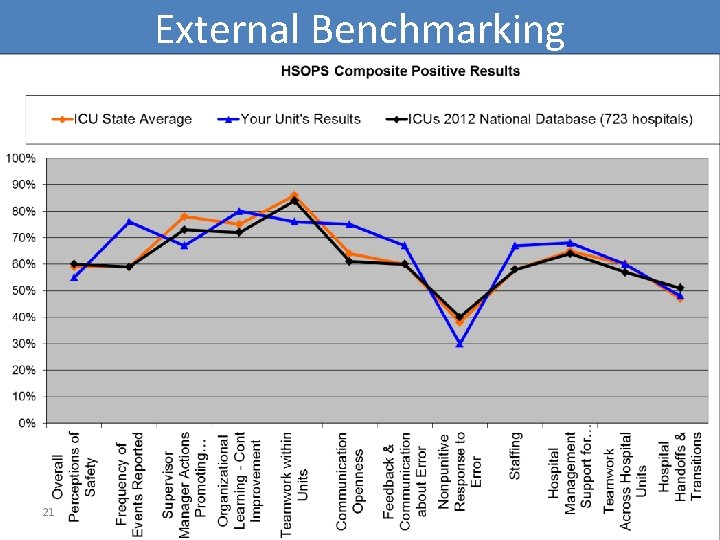
Unit-Wide Areas in Need of Improvement • Below State or National average • Less than 75% positive • Large “gap” between beliefs and behaviors within the composites 20

External Benchmarking 21

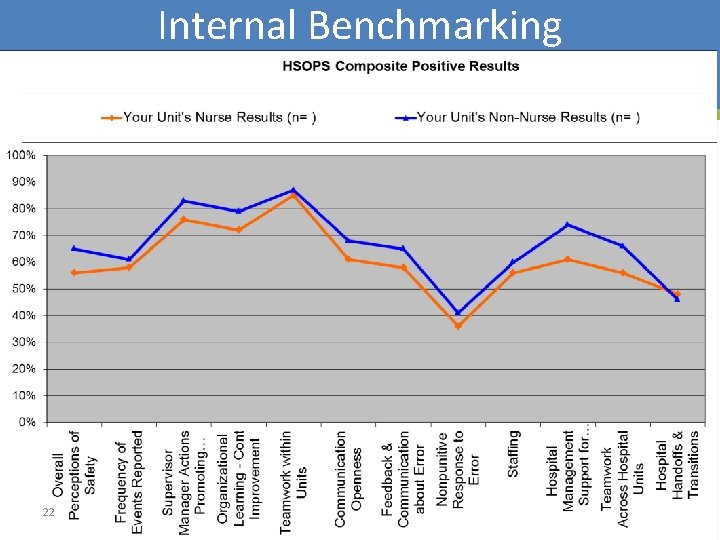
Internal Benchmarking 22

Reverse-Worded Items • Score reported is “percent positive” – Percentage of responses rated 4 or 5 (Agree/Strongly agree or Most of the Time/Always) for positively-worded items, or 1 or 2 (Disagree/Strongly Disagree or Rarely/Never) for reverseworded items • Positive is positive for patient safety, higher score better – We work in “crisis mode” trying to do too much, too quickly. (A 14 R) • 8 of 12 composites have at least 1 reverse-worded item • 2 Composites all items reverse-worded – Handoffs & Transitions – Nonpunitive Response to Error 23

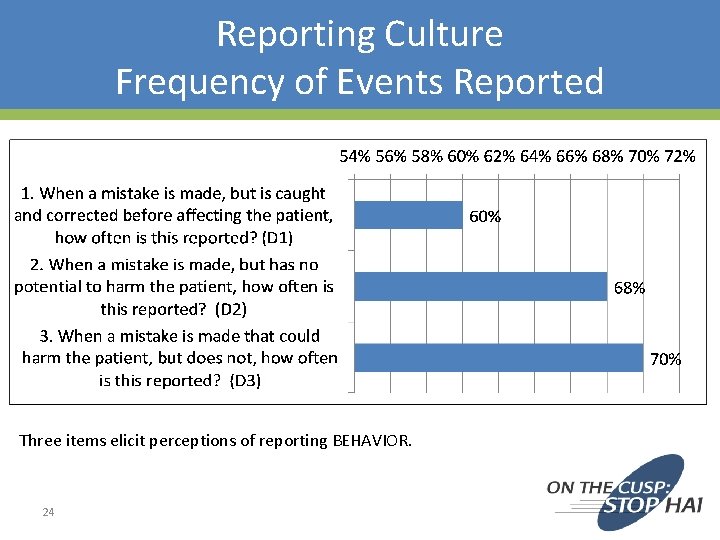
Reporting Culture Frequency of Events Reported Three items elicit perceptions of reporting BEHAVIOR. 24

Action Planning: Interventions Support Reporting Successful reporting systems 13 • Formal Reporting of adverse events with standardized taxonomies (e. g. National • Nonpunitive Coordinating Council for Medication Error • Confidential Reporting and Prevention A – I Error Severity • Independent Taxonomy) • Expert analysis • Near misses are frequently reported, valued, • Timely and learned from using anonymous log • Systems-oriented • Responsive • Non-harmful errors that reach the patient are frequently reported, valued, and learned from • Informal Reporting – Safety Briefings 14 • Informal Reporting – Leadership Walk. Rounds, 15 Leveraging Frontline Expertise 16

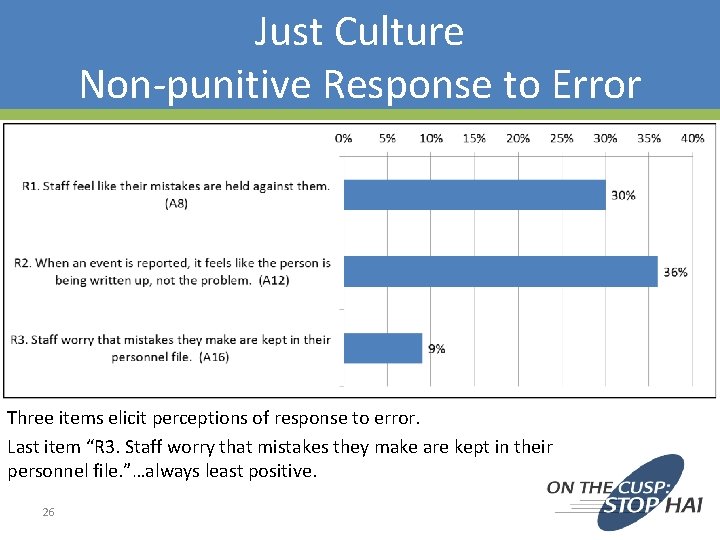
Just Culture Non-punitive Response to Error Three items elicit perceptions of response to error. Last item “R 3. Staff worry that mistakes they make are kept in their personnel file. ”…always least positive. 26

Action Planning: Interventions to Support Just Culture • Understand human error, 7 human factors – Active errors (sharp end) – Latent errors • Just Culture and behavior 17 -19 – Conduct: human error, negligence, reckless, intentional rule violation – Disciplinary decision-making: outcome-based, rule -based, risk-based • Unsafe Acts Algorithm 7 • Disruptive Behavior Policy/Standards 20 27

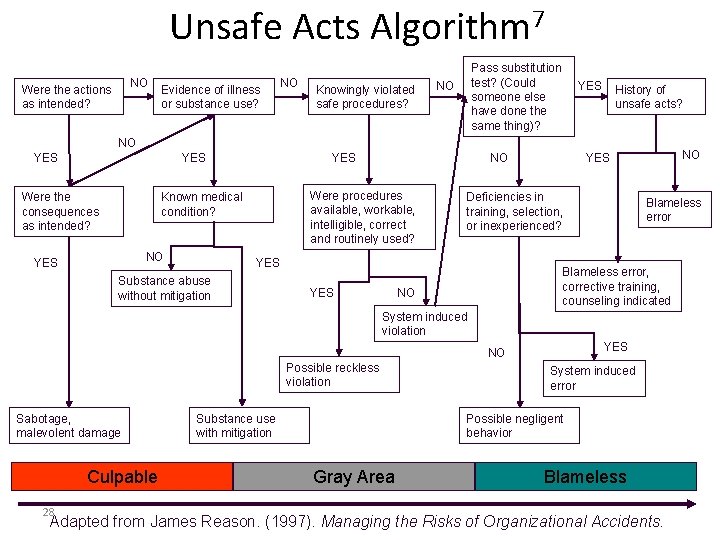
Unsafe Acts Algorithm 7 NO Were the actions as intended? Evidence of illness or substance use? NO Knowingly violated safe procedures? Pass substitution test? (Could someone else have done the same thing)? NO YES History of unsafe acts? NO YES YES Were procedures available, workable, intelligible, correct and routinely used? Known medical condition? Were the consequences as intended? NO YES NO Deficiencies in training, selection, or inexperienced? YES Substance abuse without mitigation Blameless error, corrective training, counseling indicated NO YES System induced violation YES NO Possible reckless violation Sabotage, malevolent damage Culpable 28 Substance use with mitigation System induced error Possible negligent behavior Gray Area Blameless Adapted from James Reason. (1997). Managing the Risks of Organizational Accidents.

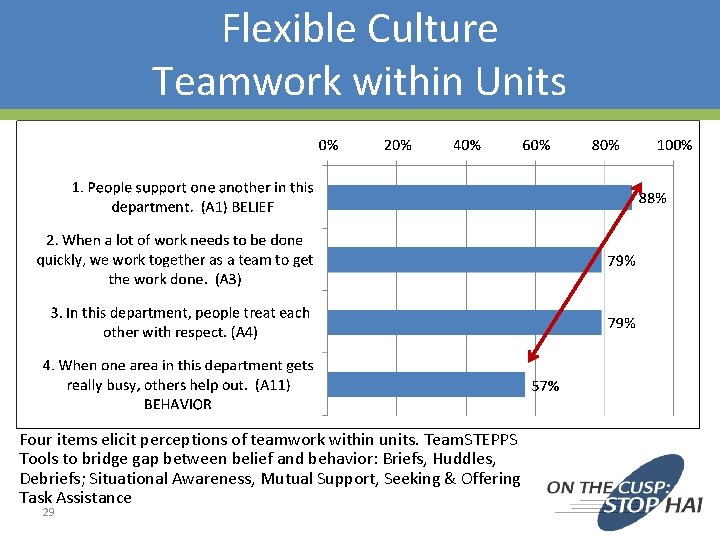
Flexible Culture Teamwork within Units Four items elicit perceptions of teamwork within units. Team. STEPPS Tools to bridge gap between belief and behavior: Briefs, Huddles, Debriefs; Situational Awareness, Mutual Support, Seeking & Offering Task Assistance 29

Flexible Culture Communication Openness Three items elicit perceptions of communication openness. Team. STEPPS Tools to Bridge the Gap between belief and behavior : Advocacy and Assertion, Two Challenge Rule, CUS 30

Flexible Culture Handoffs & Transitions Four items elicit perceptions of handoffs & transitions. Team. STEPPS Tools to Structure Communication: SBAR, Check Back, Call Out, I PASS the BATON 31

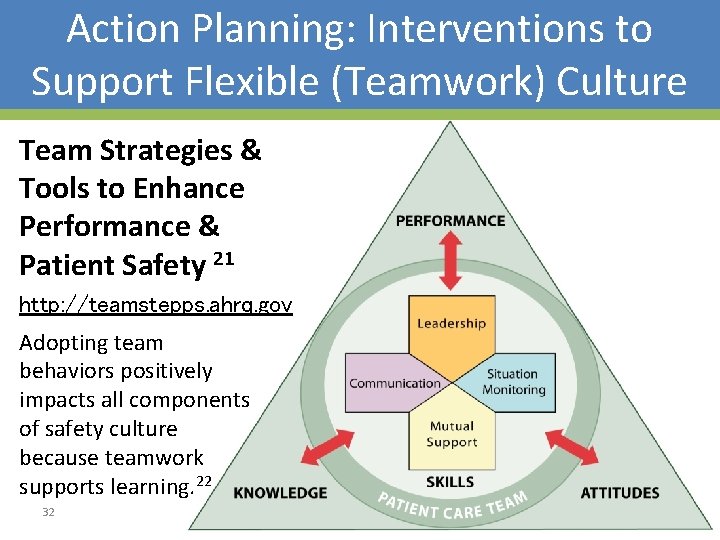
Action Planning: Interventions to Support Flexible (Teamwork) Culture Team Strategies & Tools to Enhance Performance & Patient Safety 21 http: //teamstepps. ahrq. gov A dopting team behaviors positively impacts all components of safety culture because teamwork supports learning. 22 32

Mutual Support Tool: CUS…Graded Assertiveness • I’m CONCERNED that Mr. Johnson has a urinary catheter. It was put in in the ICU without an order. • No response… • I’m UNCOMFORTABLE leaving it in because he does not currently have any evidence-based indications for a catheter. • No response… • This is a SAFTEY issue. Mr. Johnson is at risk for a CAUTI if we do not remove the catheter. 33

Communication Tool: SBAR…Brief, Clear, Timely, Complete Communication • At shift change: • S: Mr. Johnson still has a urinary catheter. • B: It was put in in the ED without an order. I have a call in to Dr. Smith, the hospitalist, to remove it. • A: Mr. Johnson does not currently have any indications for a catheter. • R: Call Dr. Smith again, if he does not return the call within an hour. 34

Learning Culture Supervisor Manager Expectations Four Items elicit perceptions of leadership behavior. Interventions: Team. STEPPS Leadership Tools (Briefs, Huddles, Debriefs; Feedback; Resource Management; Conflict Resolution); Frontline 15, 16 engagement 35

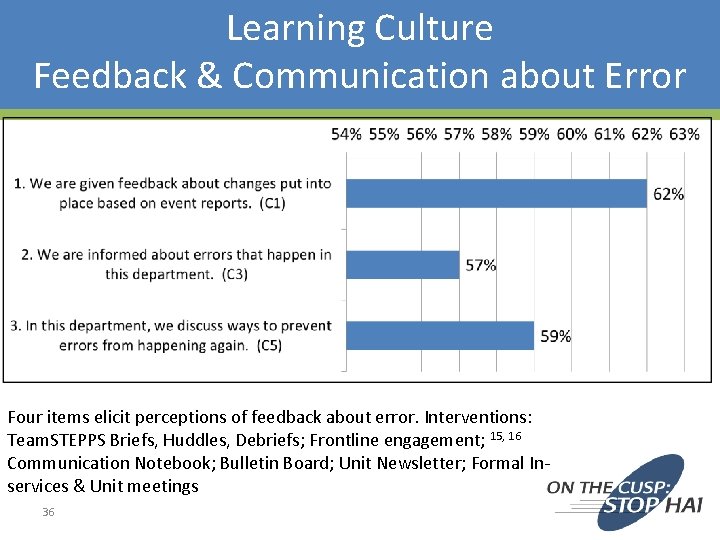
Learning Culture Feedback & Communication about Error Four items elicit perceptions of feedback about error. Interventions: Team. STEPPS Briefs, Huddles, Debriefs; Frontline engagement; 15, 16 Communication Notebook; Bulletin Board; Unit Newsletter; Formal Inservices & Unit meetings 36

Learning Culture Organizational Learning—Continuous Improvement Learning Tools : Briefs, Huddles, Debriefs; Leadership Walk. Rounds, 15 Leveraging Frontline Expertise; 16 Individual and Aggregate RCA; Failure Mode and Effects Analysis 37

Action Planning: Reporting, Just, and Flexible Practices Support Learning • Ultimately, the willingness of workers to report depends on their belief that the organization will analyze reported information and then implement appropriate change—organizational practices support a learning culture. 7 38 Practices/Tools • Individual RCA 23 • Aggregate RCA 24 • FMEA 25 • Safety Briefings 14 • Leadership Walk. Rounds, 15 Leveraging Frontline Expertise 16 • Close the loop with reporting…feedback

What is the Relationship between Patient Safety Interventions and Safety Culture? Safety culture, patient safety interventions and leadership influence each other. Patient Safety Intervention Safety Culture Leadership 39

Role of Leaders in Transformational Change 1 • Create a compelling positive vision • Concretely define the goal as a performance problem…not “changing culture” • Ensure new behaviors are formally taught • Ensure new behaviors are reinforced – Provide opportunities for practice, coaching, feedback – Be a positive role model • Create structures consistent with new way of thinking/working/behaving…policy/procedure, job descriptions, performance appraisals 40

Summary • What is safety culture? – Beliefs, behaviors reflect organizational ability to learn – Associated with adverse events, patient satisfaction • How do you interpret results? – Reason’s Components (12 composites – 4 components) – Gaps between beliefs/behaviors within composites – Variation by subculture (profession), microculture (unit) – Leadership must drive culture

Summary • Action Planning – Identify areas in need of improvement within 4 components…reporting, just culture, teamwork, learning • What is the relationship between STOP HAI and Safety Culture? STOP HAI Safety Culture Leadership

Leaders Engineer Culture “…it is the unique function of leadership to perceive the functional and dysfunctional elements and to manage cultural evolution and change. ” Schein, E. H. Organizational Leadership and Culture 4 th ed. San Francisco: John Wiley & Sons; 2010. 43

Thank you! Questions? 44

References 1. 2. 3. 4. 5. 6. 7. Schein, E. H. Organizational Leadership and Culture 4 th ed. San Francisco: John Wiley & Sons; 2010. Wiegmann. A synthesis of safety culture and safety climate research; 2002. http: //www. humanfactors. uiuc. edu/Reports&Papers. PDFs/Tech. Report/02 -03. pdf Institute of Medicine. Patient safety: Achieving a new standard of care. Washington, DC: The National Academies Press; 2004. Weaver SJ, Lubomski LH, Wilson RF, Pfoh ER, Martinez KA, Dy SM. Promoting a culture of safety as a patient safety strategy: A systematic review. Ann Int Med. 2013; 158: 369 -374. Mardon RE, Khanna K, Sorra J, Dyer N, Famolaro T. Exploring relationships between hospital patient safety culture and adverse events. J Patient Saf 2010; 6: 226 -232. Sorra J, Khanna K, Dyer N, Mardon R, Famolaro T. Exploring relationships between patient safety culture and patients’ assessments of hospital care. J Patient Saf 2012; 8: 131 -139. Reason, J. (1997). Managing the Risks of Organizational Accidents. Hampshire, England: Ashgate Publishing Limited. 45

References 8. 9. 10. 11. 12. 13. 46 Battles et al. (2006). Sensemaking of patient safety risks and hazards. HSR, 41(4 Pt 2), 1555 -1575. Nieva VF, Sorra J. Safety culture assessment: A tool for improving patient safety in healthcare organizations. Qual Saf Health Care 2003; 12(Suppl II): ii 17 -ii 23. Jones, Skinner, Xu, Sun, Mueller. (2008). The AHRQ Hospital Survey on Patient Safety Culture: a tool to plan and evaluate patient safety programs. Advances in Patient Safety: New Directions and Alternative Approaches http: //www. ncbi. nlm. nih. gov/books/NBK 43699/ National Quality Forum (NQF). Safe practices for better healthcare--2010 update: A consensus report. Washington, DC: NQF; 2010. Available at: http: //www. qualityforum. org/Publications/2010/04/Safe_Practices_for_Better_Healthcare_– _2010_Update. aspx AHRQ. Hospital Survey on Patient Safety Culture. Available at: http: //www. ahrq. gov/professionals/quality-patientsafety/patientsafetyculture/hospital/resources/index. html Leape, L. L. (2002) Reporting adverse events. The New England Journal of Medicine, 347, 16331638 Institute for Healthcare Improvement.

References 14. Conduct Safety Briefings. Available at: http: //www. ihi. org/knowledge/Pages/Changes/Conduct. Safety. Briefings. aspx Institute for Healthcare Improvement. Patient Safety Leadership Walk. Rounds. Available at: http: //www. ihi. org/knowledge/pages/tools/patientsafetyleadershipwalkrounds. aspx Singer SJ, Rivard PE, Hayes JE, Shokeen P, Gaba D, Rosen A. Improving patient care through leadership engagement with frontline staff: A Department of Veterans Affairs case study. The Joint Commission Journal on Quality and Patient Safety. 2013; 39: 349 -360. Marx D. Patient Safety and the “Just Culture”: A Primer for Health Care Executives. New York, NY: Columbia University; 2001. Available at: http: //psnet. ahrq. gov/resource. aspx? resource. ID=1582 Frankel AS, Leonard MW, Denham CR. Fair and just culture, team behavior, and leadership engagement: the tools to achieve high reliability. HSR. 2006; 41(4), Part. II: 1690 -1709. Wachter RM, Pronovost PJ. Balancing "no blame" with accountability in patient safety. N Engl J Med. 2009; 361: 1401 -1406. AHRQ. Patient Safety Primers. Disruptive and Unprofessional Behavior. Available at: http: //psnet. ahrq. gov/primer. aspx? primer. ID=15 15. 16. 17. 18. 19. 20. 47

References 21. Agency for Healthcare Research and Quality. Team. STEPPS: Strategies and tools to enhance performance and patient safety. Available at: http: //teamstepps. ahrq. gov/. 22. Jones KJ, Skinner AM, High R, Reiter-Palmon R. A theory-driven longitudinal evaluation of the impact of team training on safety culture in 24 hospitals. BMJ Qual Saf. 2013; 22: 394 -404. 23. US Department of Veterans Affairs. National Center for Patient Safety. Root Cause Analysis Tools. Available at: http: //www. patientsafety. gov/Cog. Aids/RCA/index. html#page=page-1 24. Neily et al. Using aggregate root cause analysis to improve patient safety. Jt Comm J Qual Saf 29(8): 434 -439, 2003. 25. US Department of Veterans Affairs. National Center for Patient Safety. Using Healthcare Failure Modes and Effects Analysis. Available at: http: //www. patientsafety. gov/Safety. Topics/HFMEA_JQI. html 48

Funding Prepared by the Health Research & Educational Trust of the American Hospital Association with contract funding provided by the Agency for Healthcare Research and Quality through the contract, “National Implementation of Comprehensive Unitbased Safety Program (CUSP) to Reduce Catheter-Associated Urinary Tract Infection (CAUTI), project number HHSA 290201000025 I/HHSA 29032001 T, Task Order #1. ”