Congestive Heart Failure Valvular Disease Keith Rischer RN






















- Slides: 25

Congestive Heart Failure & Valvular Disease Keith Rischer RN, MA, CEN 1

Todays Objectives… Ø Ø Ø Ø Review essential cardiac patho concepts Compare and contrast left-sided heart failure to right Describe special considerations for older adults with heart failure Discuss the prevention of complications for patients with heart failure Prioritize nursing care for clients with heart failure Identify common nursing diagnoses and collaborative problems for patients with heart failure Evaluate the effects of interventions for reducing preload and afterload through pharmacological management Compare and contrast common valvular disorders 2

Introduction Ø Definition of CHF q Etiology ü ü Ø Left sided vs. Right sided q Rt sided ü Ø Ø HTN MI COPD Systolic vs. Diastolic Ejection Fraction q 50 -70% normal 3

Cardiac Output v. CO = Stroke volume x heart rate v. SV (80 cc) x HR (80)= 6400 cc (6. 4 lpm) • • • Daily pumps 1800 gallons 657, 000 gallons every year Over 80 year lifetime: • 52, 560, 000 gallons 4

Definitions Ø Pre-load q q q Ø Stroke volume q Ø primarily venous blood return to RA Right and left side of heart filling pressure (atria>ventricles) Pressure/Stretch in ventricles end diastole Amount of blood ejected from the ventricle with each contraction Systole q Contraction; myocardium are tightening and shortening 5

Definitions Ø Ø Inotropic state/contractility Afterload: q q Ø Force of resistance that the LV must generate to open aortic valve Correlates w/SBP Diastole q Muscle fibers lengthen, the heart dilates, and cavities fill with blood 6

Patho: Starling’s Law of the Heart Ø Ø Ø Maximum efficency of CO achieved when myocardium stretched appx 2 ½ times length Think rubber band CO decreased with lower preload/filling pressures or too high 7

Compensatory Mechanisms in CHF Ø Ø Increased Sympathetic Nervous System Stimulation Renin-angiotensin system activation Natriuretic peptides q BNP Ventricular hypertrophy 8

Acute Pulmonary Edema: Ø Elevated capillary pressure within the lungs fluid pushed from circulating blood to interstitial tissues then to the alveoli, bronchioles, and bronchi 9

Nursing Assessment: Left Failure Ø Ø Ø Dyspnea Cough Bilateral crackles Orthopnea PND Pulmonary Edema S 3 (ken-tuck-ee) confusion fatigue and muscular weakness nocturia increase retention of sodium and water due to lowered glomerular filtration edema 10

Nursing Assessment: Right Failure Ø Ø Ø Dependent edema – q early sign q symmetric pitting edema q Bedrest-sacral edema q anasarca- late sign of CHF Ascites Anorexia, nausea and bloating Cyanosis of nail beds Anxious, frightened, depressed Weight gain >2# daily 11

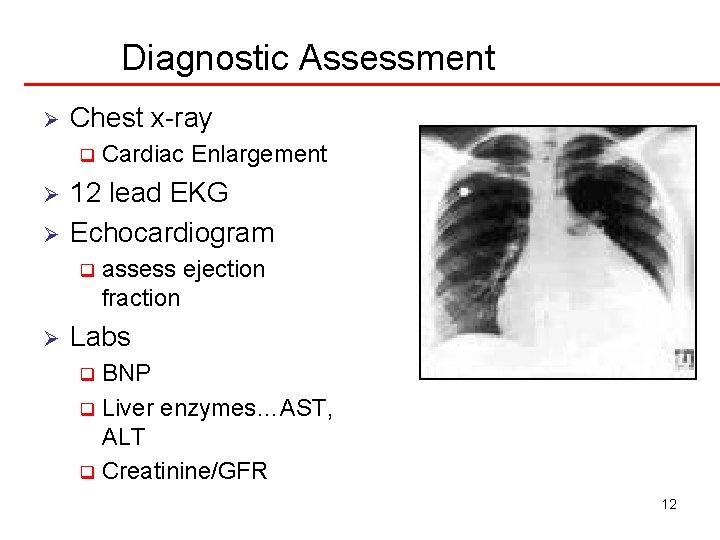
Diagnostic Assessment Ø Chest x-ray q Ø Ø 12 lead EKG Echocardiogram q Ø Cardiac Enlargement assess ejection fraction Labs BNP q Liver enzymes…AST, ALT q Creatinine/GFR q 12

Acute Left Failure/Pulmonary Edema: Collaborative Management: Ø Ø O 2 treatment Drug Treatment q q Ø Ø Ø Diuretics Vasodilators-NTG MS Digitalis Semi- Fowler’s position Frequent Heart and Lung Assessment Dietary Restrictions Planned rest periods Weigh daily Report to MD immediately: q persisting productive cough; dyspnea; pedal edema; restlessness 13

Drug therapy: Ø Ø Ø Diuretics ACE Inhibitors Beta Blockers Calcium Channel Blockers n. Nitroglycerine Positive Inotropic agents q Ø Digitalis Beta Adrenergic Stimulator q Dopamine, Dobutamine 14

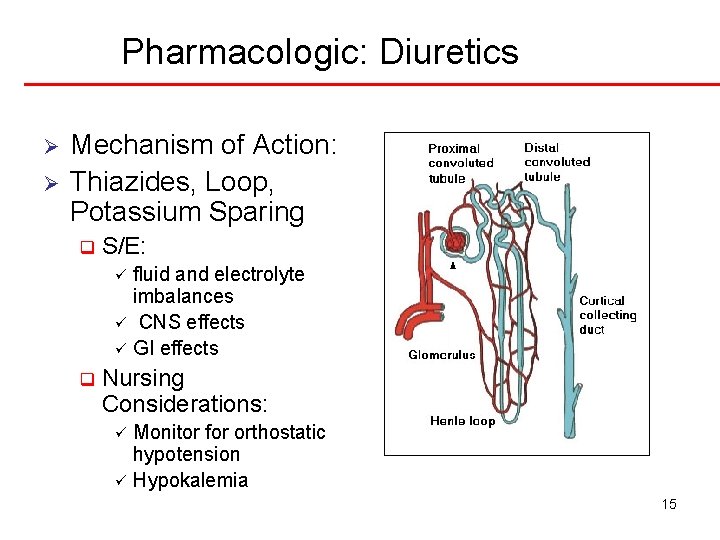
Pharmacologic: Diuretics Ø Ø Mechanism of Action: Thiazides, Loop, Potassium Sparing q S/E: fluid and electrolyte imbalances ü CNS effects ü GI effects ü q Nursing Considerations: Monitor for orthostatic hypotension ü Hypokalemia ü 15

Angiotensin Converting Enzyme (ACE) Inhibitors Mechanism of Action Ø S/E: Hypotension q cough q Hyperkalemia…esp w/CHF, CKD, DM q Angioedema q ü Ø Facial/laryngeal swelling Nursing considerations: Do not use with potassium sparing diuretic q Metabolized by liver-excreted by kidneys q 16

Adrenergic Inhibitors: Beta Blockers Mechanism of Action Ø Recommended for initial drug therapy of uncomplicated HTN (along with diuretic) q S/E: Orthostatic hypotension ü bradycardia ü bronchospasm ü q Nursing considerations: ü monitor pulse regularly 17

Calcium Channel Blockers Amlodipine, Diltiazem, Nifedipine Mechanism of Action: S/E: q Nausea q H/A q Peripheral edema Nursing considerations: q use with caution in patients with heart failure q Orthostatic changes q contraindicated in patients with 2 nd or 3 rd degree heart block q Concurrent use w/b-blockers incr risk of CHF 18

Vasodilators Mechanism of Action-NTG • Vasodilater-predominant on venous system by relaxing smooth muscles of vessels • Dilates coronary arteries/improves collateral flow • Up to 20% normal coronaries… 30 -40% pre/post stenosis • Decreases LVEDP…why? • Decreases O 2 needs myocardium Side effects • HA, hypotension, tachycardia Hydralazine • arterial vasodilator 19

Priority Nursing Diagnosis Ø Ø Impaired Gas exchange r/t ventilation perfusion imbalance Decreased Cardiac Output r/t altered contractility, preload and afterload Activity Intolerance r/t imbalance between O 2 supply and demand Knowledge Deficit Activity schedule q Recognizing worsening heart failure q Medications q Diet therapy q 20

Valvular Heart Disease: Mitral Valve Ø Mitral Stenosis q Ø Mitral Regurgitation q Ø Patho Mitral Valve Prolapse q Patho 21

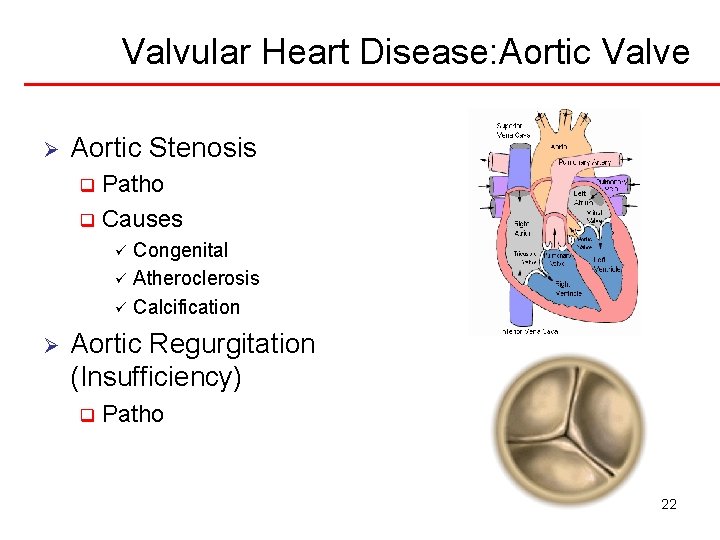
Valvular Heart Disease: Aortic Valve Ø Aortic Stenosis Patho q Causes q Congenital ü Atheroclerosis ü Calcification ü Ø Aortic Regurgitation (Insufficiency) q Patho 22

Treatment Valvular Disease Ø Non-surgical Management q q Diuretics Beta blockers Digoxin Antibiotics ü q Ø Before any invasives Coumadin-if artificial valve Surgical Management q q Balloon Valvuloplasty Open heart 23

Pericarditis Ø Patho q q Ø Assessment findings q q Ø Open heart AMI Friction rub CP w/insp CP relieves sitting up Global ST elevation Complications q q Pericardial effusion Cardiac tamponade ü pericardiocentesis 24

Endocarditis Ø Ø Patho Etiology q q q Ø Clinical Manifestations q q q Ø New murmur Heart failure Embolic Diagnosis q q Ø Valve replacement Structural cardiac defects Invasive procedures Transesophageal Echo + blood cultures Interventions q q IV abx Surgical 25