Congenital Larynx Lesions Stridor Evaluation Dr Vishal Sharma

































- Slides: 77

Congenital Larynx Lesions & Stridor Evaluation Dr. Vishal Sharma

Epidemiology • 80 – 85 % children < 3 yrs with stridor have congenital etiology for stridor • 60 % of these anomalies are in larynx • 20 -25 % are anomalies of trachea + bronchi • 45% patients have more than 1 anomalies

Etiology Supraglottis: Laryngomalacia, Supraglottic web, Saccular cyst, Congenital laryngocoele, Supraglottic cleft Glottis: Vocal cord paralysis, Glottic web, Glottic stenosis, Cri-du-chat syndrome Subglottis: Subglottic stenosis, Subglottic web, Subglottic hemangioma

Common congenital lesions • Laryngomalacia (60%) • Congenital vocal cord paralysis (20%) • Congenital subglottic stenosis (15%) • Subglottic hemangioma (1. 5%)

Supra-glottic abnormalities

Laryngomalacia • Most common congenital laryngeal anomaly Etiology: • Exact cause is not known 1. Mal-development of cartilaginous structures 2. Gastro-esophageal reflux disease 3. Immaturity of neuromuscular control

Clinical presentation • Symptoms begin few weeks after birth, progress over 9 -12 months & resolve by 2 years • Inspiratory stridor: 1. increased by: supine position, feeding, resp. infection & exertion (crying). 2. relieved by: neck extension & prone position. • Phonation & cry are normal. Feeding difficulties, failure to thrive, dyspnoea & cyanosis are rare.

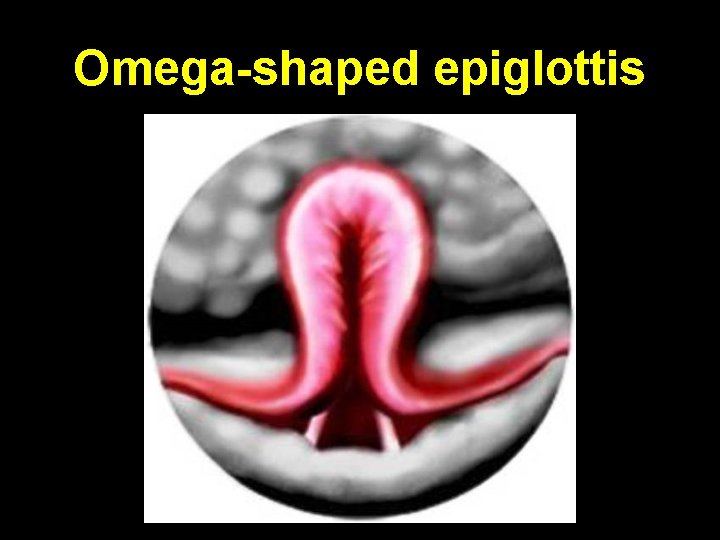
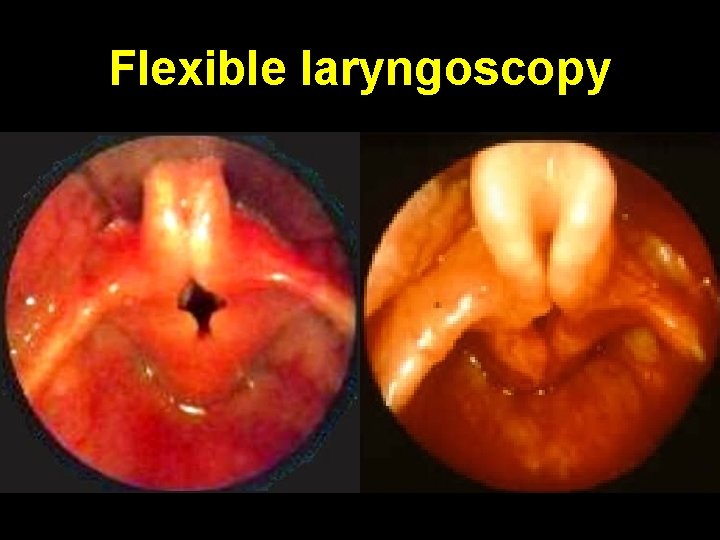
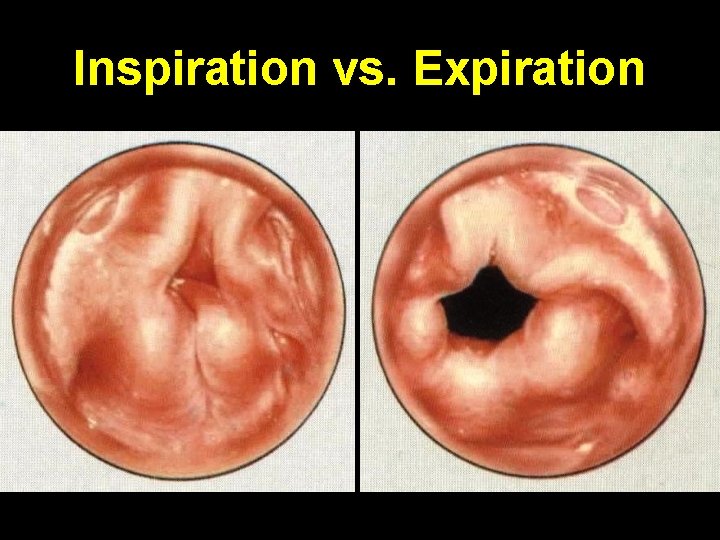
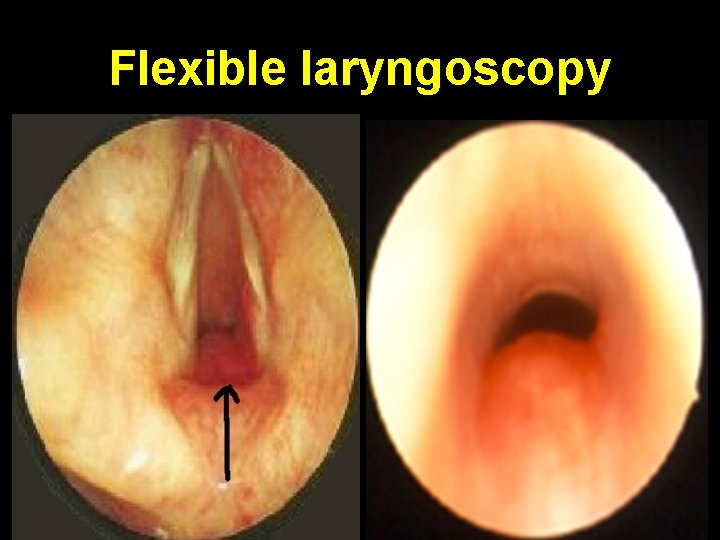
Flexible laryngoscopy • Elongation + longitudinal folding of epiglottis (omega shaped, ), falls postero-inferiorly on inspiration • Redundant bulky arytenoids prolapse anteriorly & medially on inspiration. Shortening + medial collapse of aryepiglottic folds. Expiration results in expulsion of these structures with free flow of air • Rigid bronchoscopy GA: exclude other anomaly

Omega-shaped epiglottis

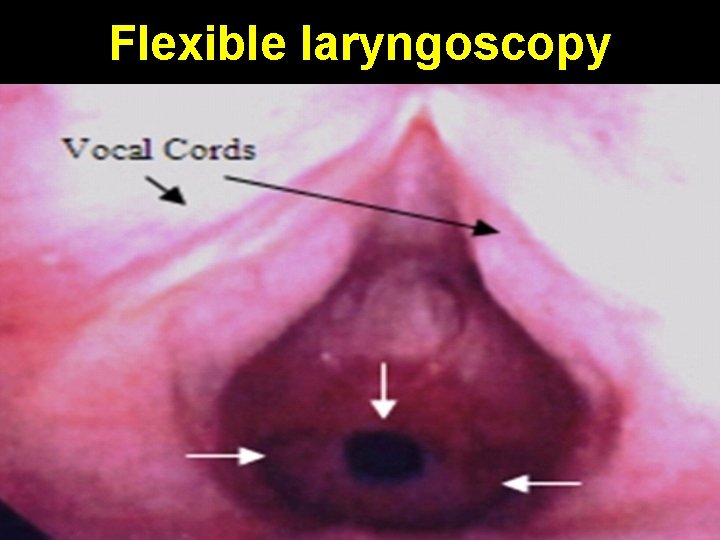
Flexible laryngoscopy

Inspiration vs. Expiration

Treatment 1. 99% cases: reassurance, sleep in prone position 2. Treatment of gastro-esophageal reflux disease 3. Surgical management (for 1% cases): a. Emergency Tracheostomy: kept till 2 yrs age b. Epiglottoplasty: cautery or laser assisted

Epiglottoplasty for laryngomalacia

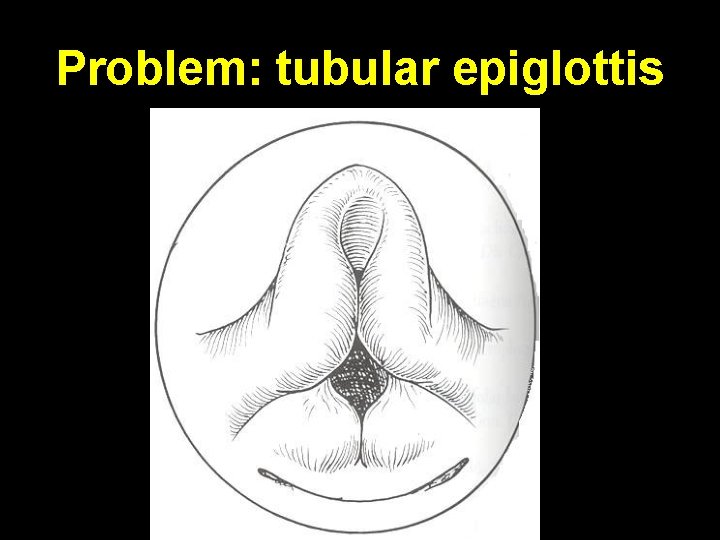
Problem: tubular epiglottis

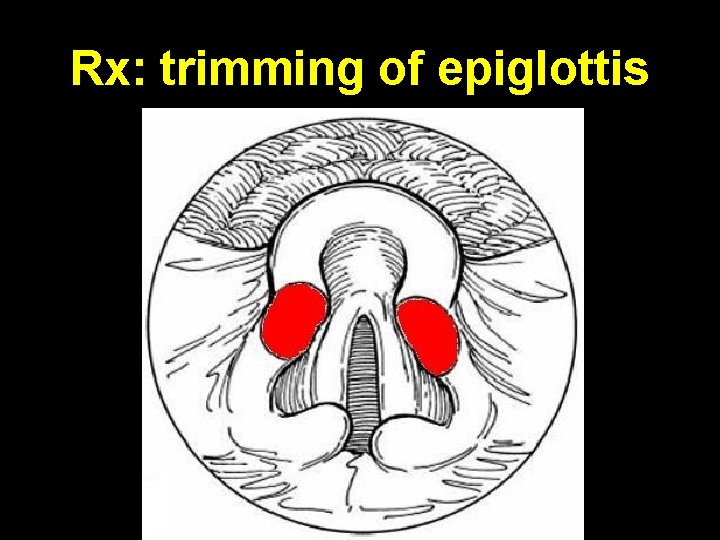
Rx: trimming of epiglottis

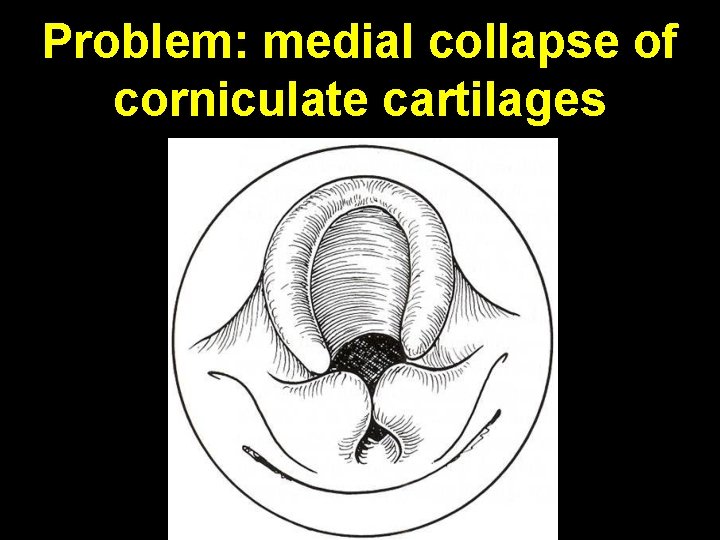
Problem: medial collapse of corniculate cartilages

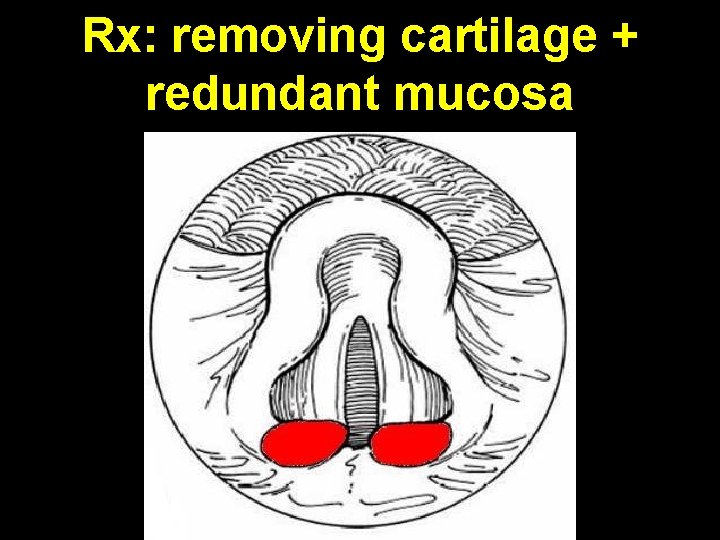
Rx: removing cartilage + redundant mucosa

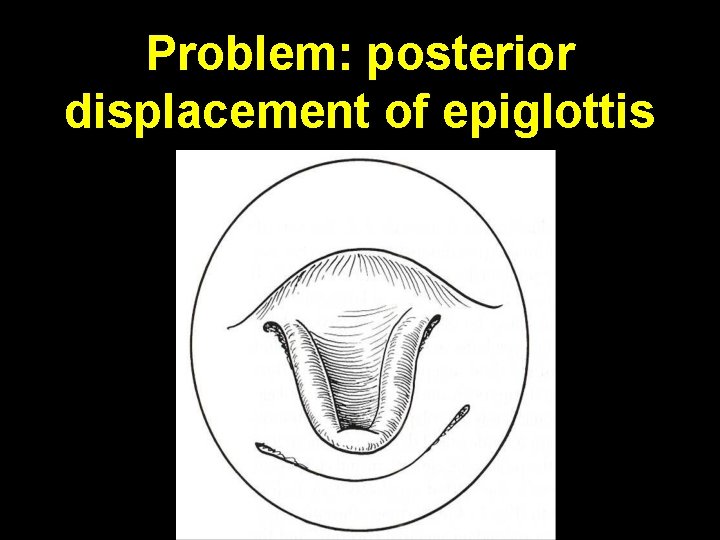
Problem: posterior displacement of epiglottis

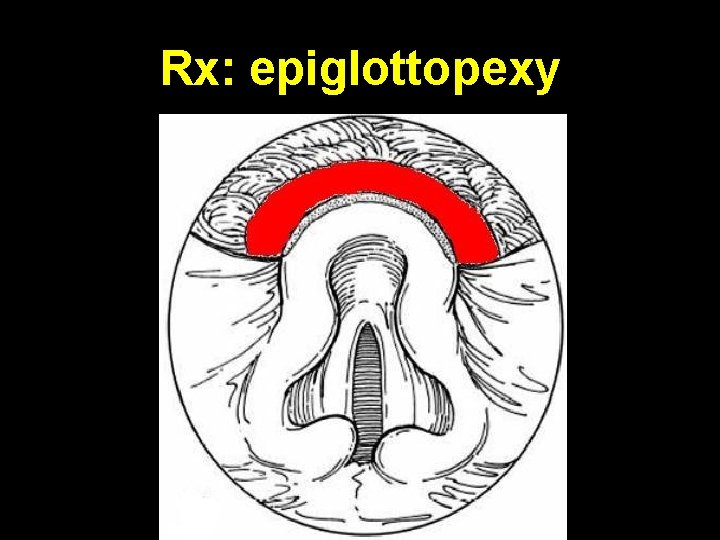
Rx: epiglottopexy

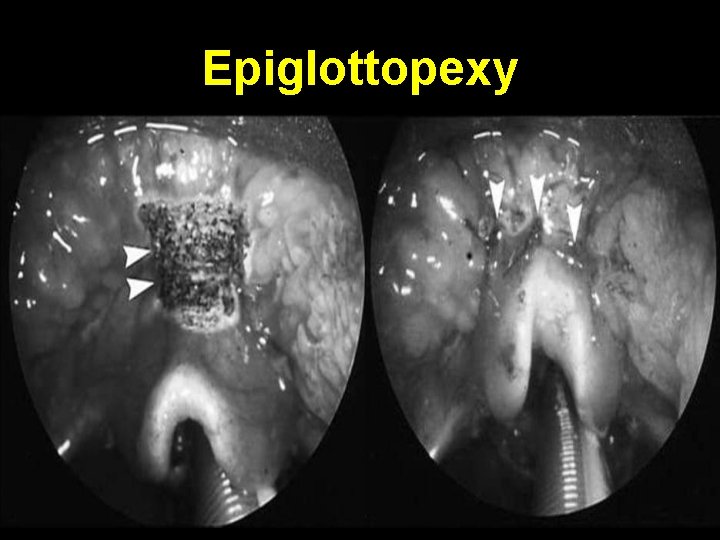
Epiglottopexy

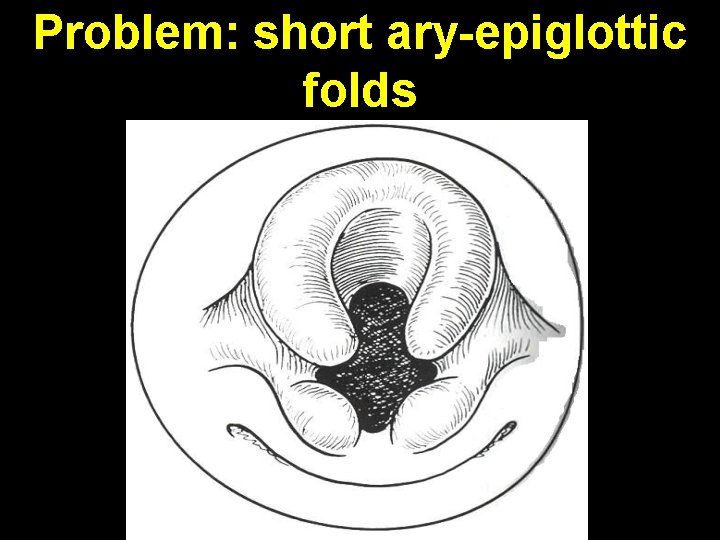
Problem: short ary-epiglottic folds

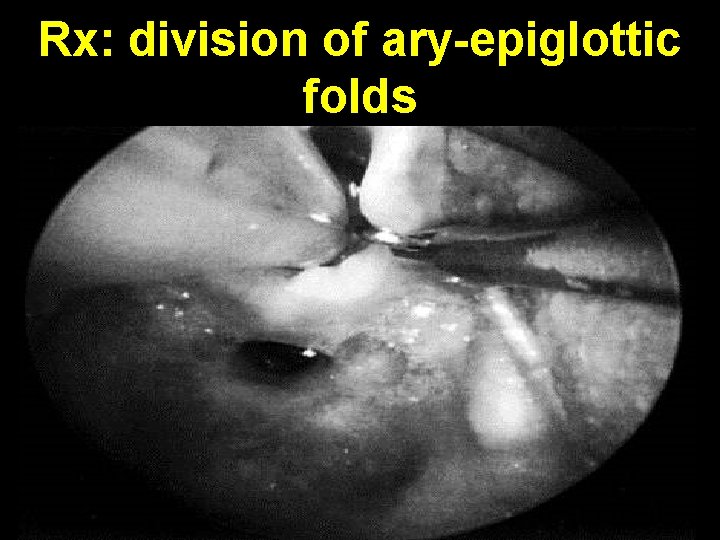
Rx: division of ary-epiglottic folds

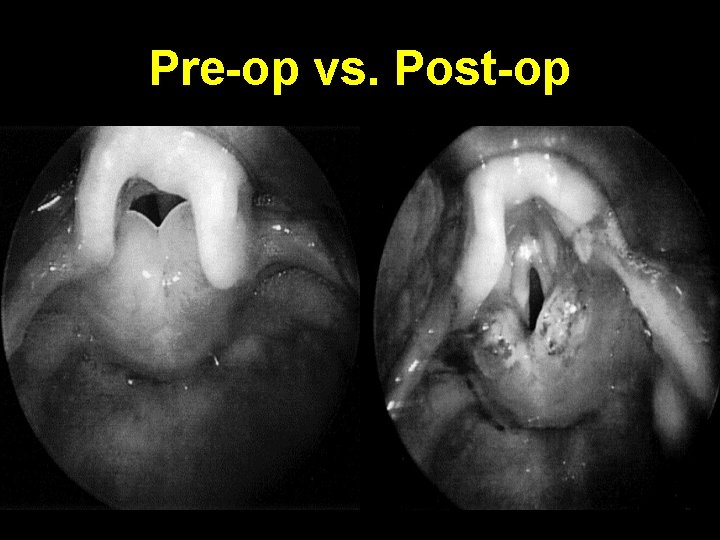
Pre-op vs. Post-op

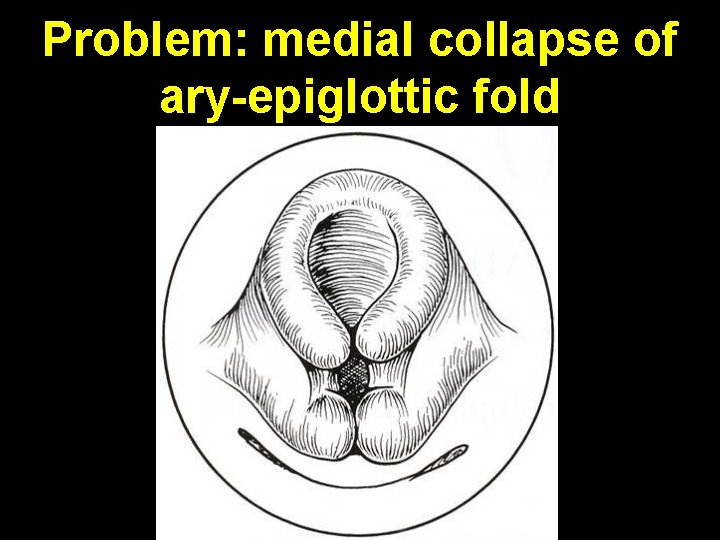
Problem: medial collapse of ary-epiglottic fold

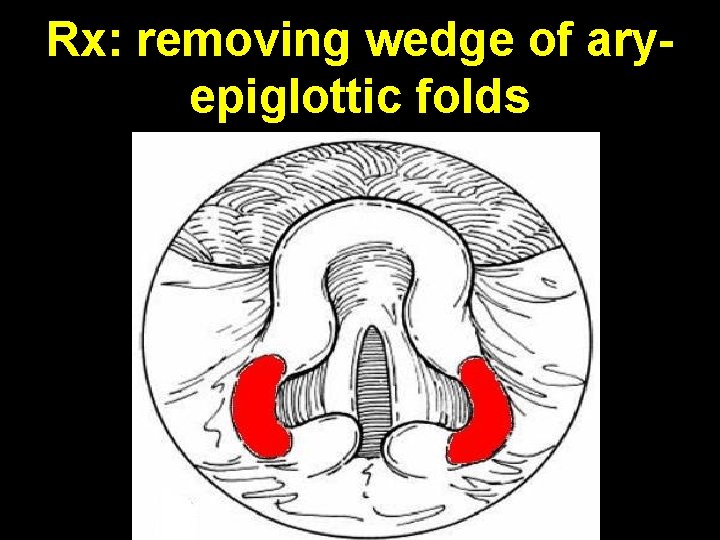
Rx: removing wedge of aryepiglottic folds

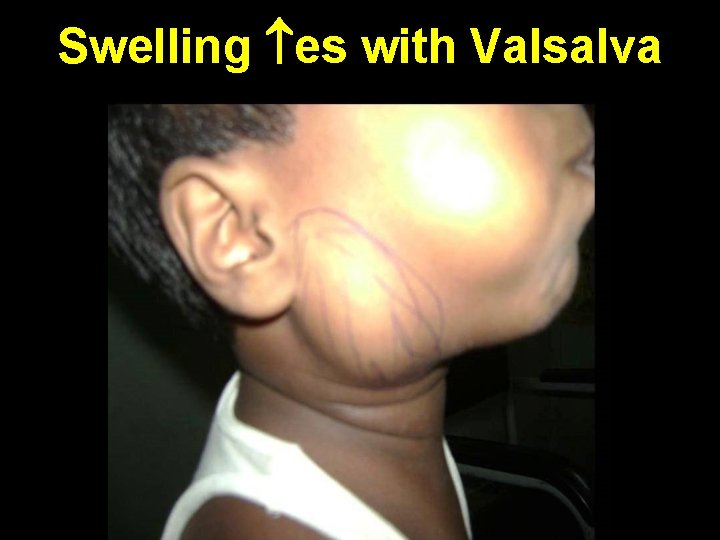
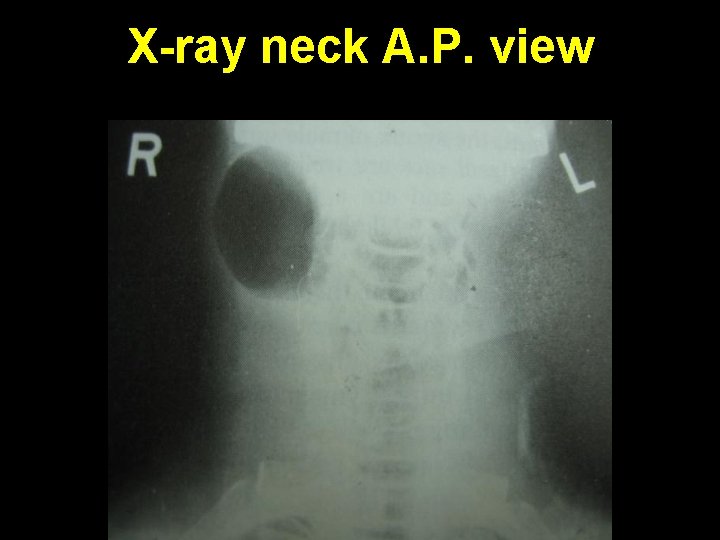
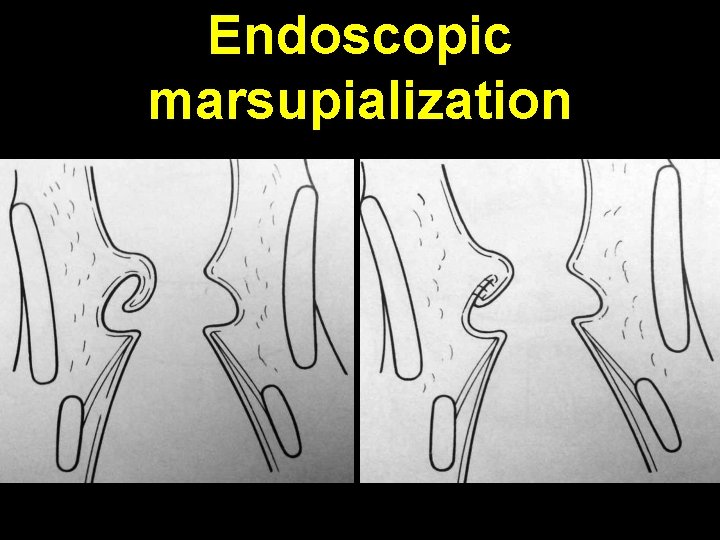
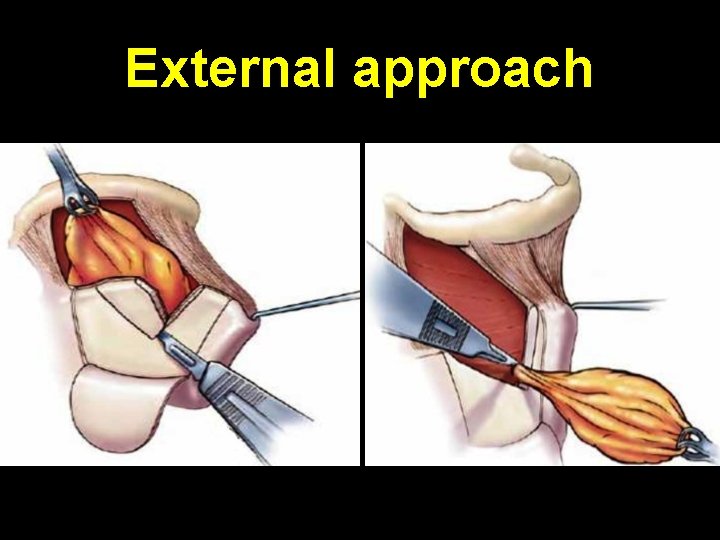
Congenital laryngocoele Air filled dilatation of ventricular sinus of Morgagni C/F: 1. Hoarseness or respiratory distress 2. Neck swelling es on Valsalva maneuver Investigation: 1. Plain X-ray soft tissue neck 2. Flexible laryngoscopy Treatment: 1. Endoscopic marsupialization 2. External excision by thyrotomy

Swelling es with Valsalva

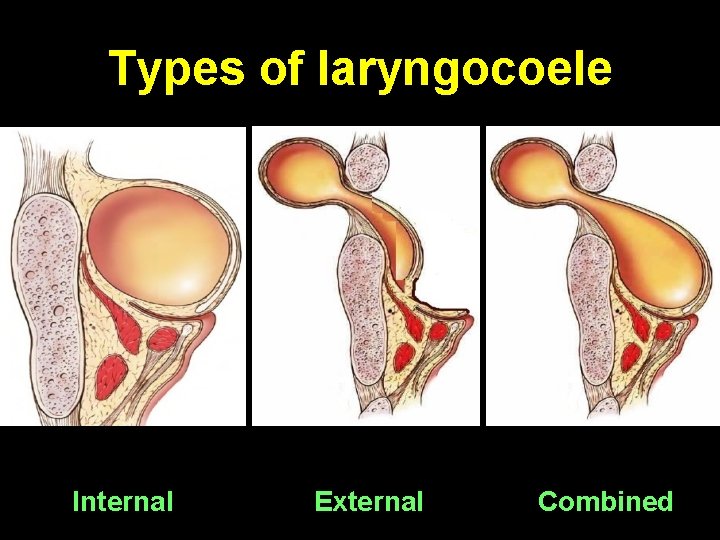
Types of laryngocoele • Internal (20%): contained entirely within endolarynx with bulge in false vocal fold & aryepiglottic fold • External (30%): only neck swelling without visible endolaryngeal swelling • Combined (50%): Also extends into anterior triangle of neck through foramen for superior laryngeal nerve & vessels in thyrohyoid membrane. Dumbbell shaped.

Types of laryngocoele Internal External Combined

X-ray neck A. P. view

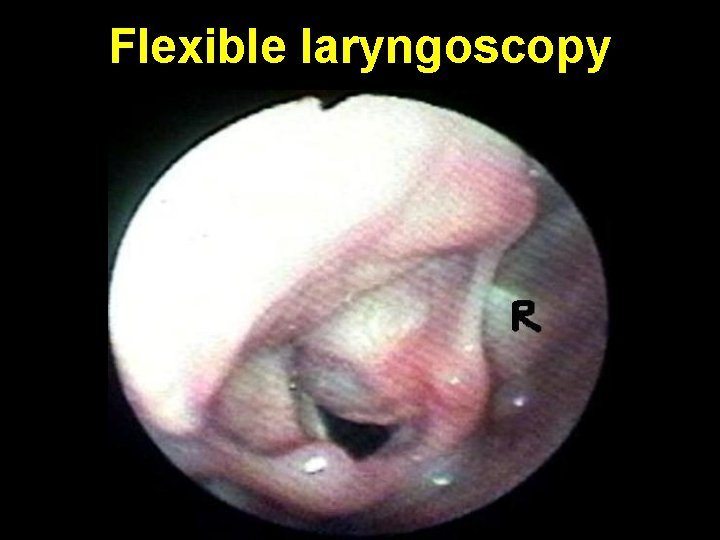
Flexible laryngoscopy

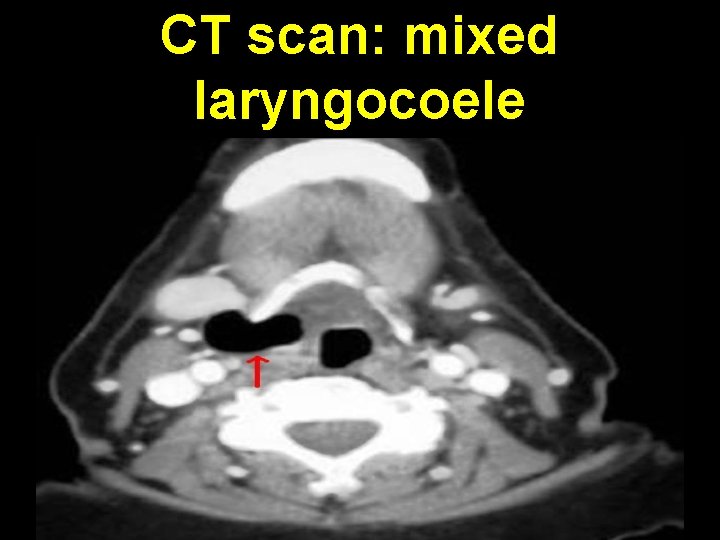
CT scan: mixed laryngocoele

Endoscopic marsupialization

External approach

Congenital saccular cyst • Due to obstruction of orifice of saccule in laryngeal ventricle • 40% congenital cysts found within hours of birth • 95% of infants have symptoms within 6 months • C/F: Inspiratory stridor improves on extension of head, cyanosis, feeding problem & failure to thrive

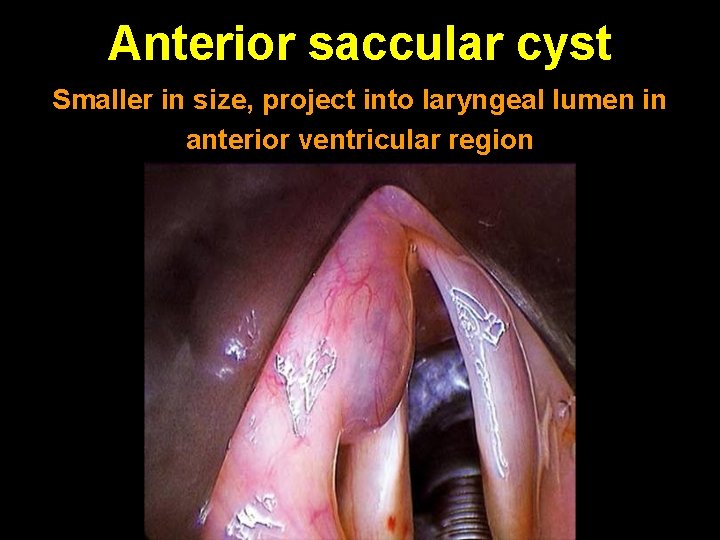
Anterior saccular cyst Smaller in size, project into laryngeal lumen in anterior ventricular region

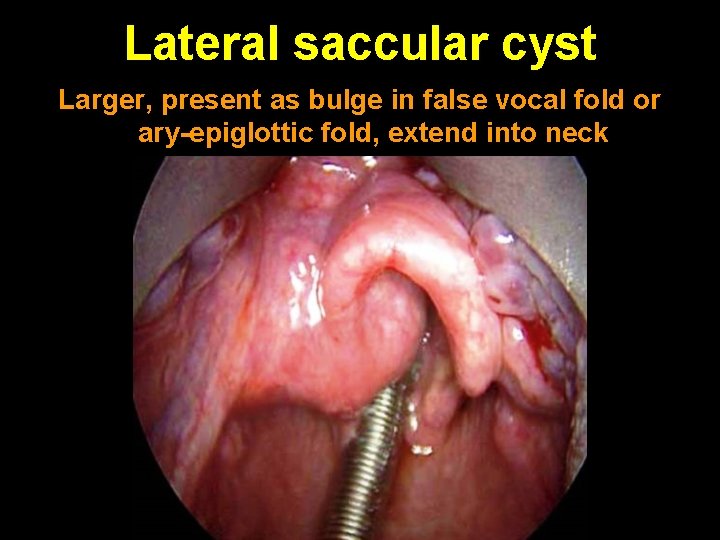
Lateral saccular cyst Larger, present as bulge in false vocal fold or ary-epiglottic fold, extend into neck

Treatment 1. Emergency tracheostomy for acute stridor 2. Endoscopic de-roofing or marsupialization: cold knife Laser-assisted 3. Endoscopic incision & drainage 4. Total excision: endoscopic laryngofissure approach

Glottic abnormalities

Congenital vocal cord palsy

Etiology 1. Idiopathic: most common 2. C. N. S. Lesions: Arnold-Chiari malformation, cerebral palsy, hydrocephalus, myelomeningocele, spina bifida, hypoxia 3. Birth trauma: a. cervical spine b. recurrent laryngeal nerve 4. Mediastinum lesions: a. tumors b. vascular malformation

Clinical Features Unilateral paralysis: 4 times common Hoarse, breathy cry aggravated by agitation Feeding difficulty Aspiration Bilateral paralysis: Biphasic stridor (worsens on agitation) + nearnormal phonation: abductor paralysis Lung aspiration + aphonia: adductor paralysis

Diagnosis: 1. Flexible laryngoscopy shows vocal fold palsy 2. Rigid bronchoscopy GA: other anomaly Treatment: Bilateral paralysis: 1. Vocal cord lateralization 3. Cordectomy 2. Cordotomy 4. Subtotal arytenoidectomy 5. Tracheostomy Unilateral paralysis: Observation

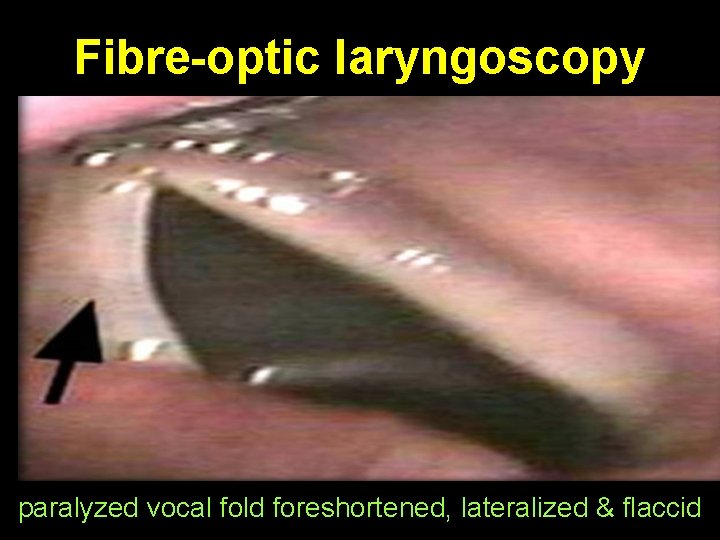
Fibre-optic laryngoscopy paralyzed vocal fold foreshortened, lateralized & flaccid

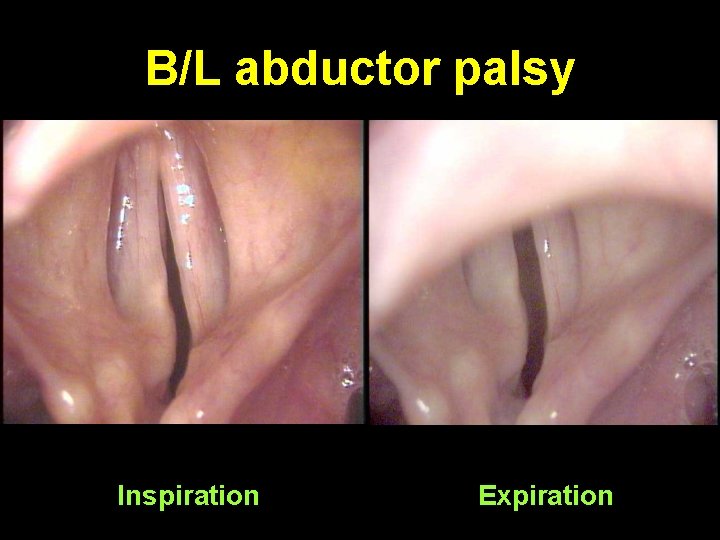
B/L abductor palsy Inspiration Expiration

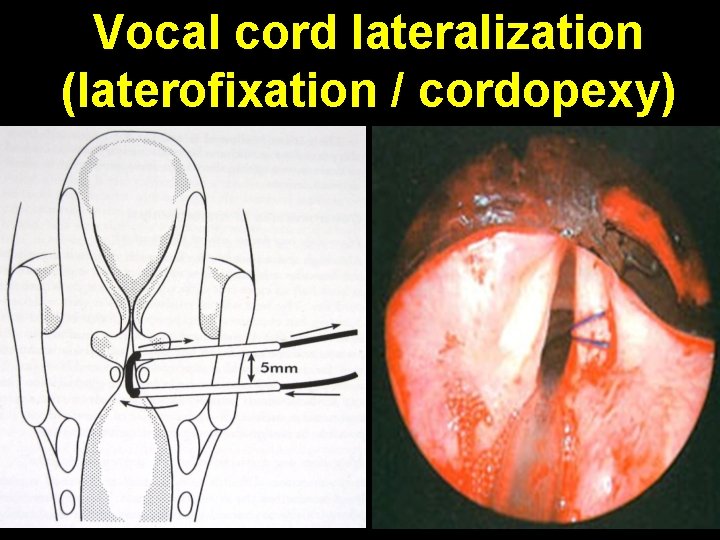
Vocal cord lateralization (laterofixation / cordopexy)

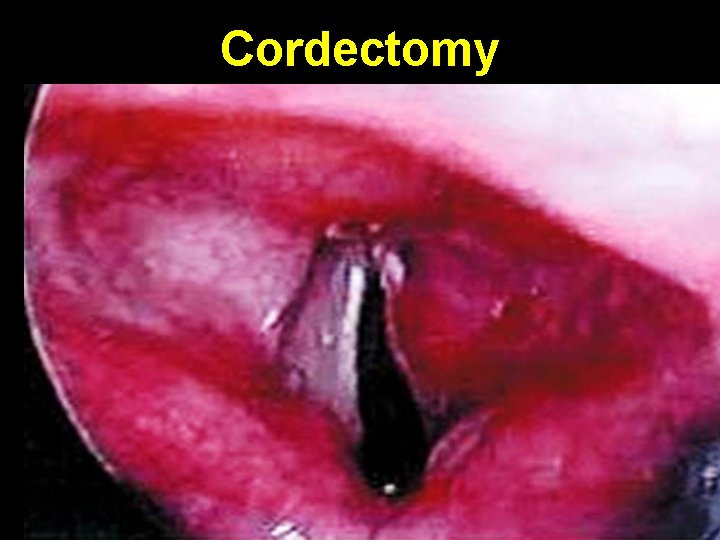
Cordectomy

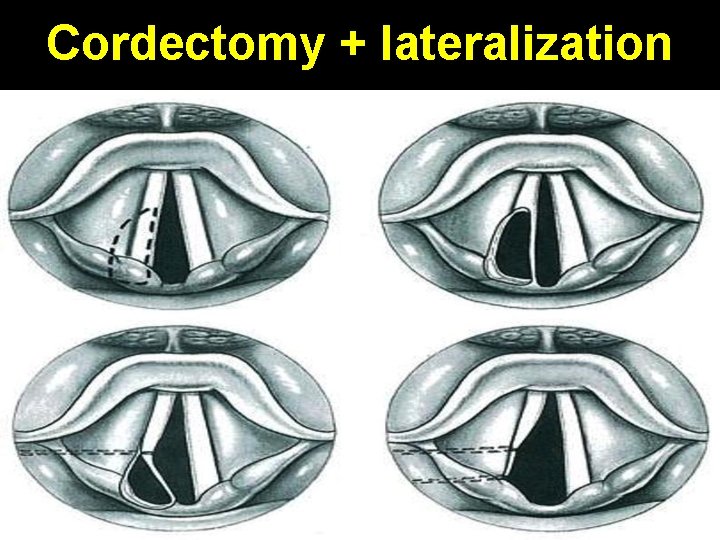
Cordectomy + lateralization

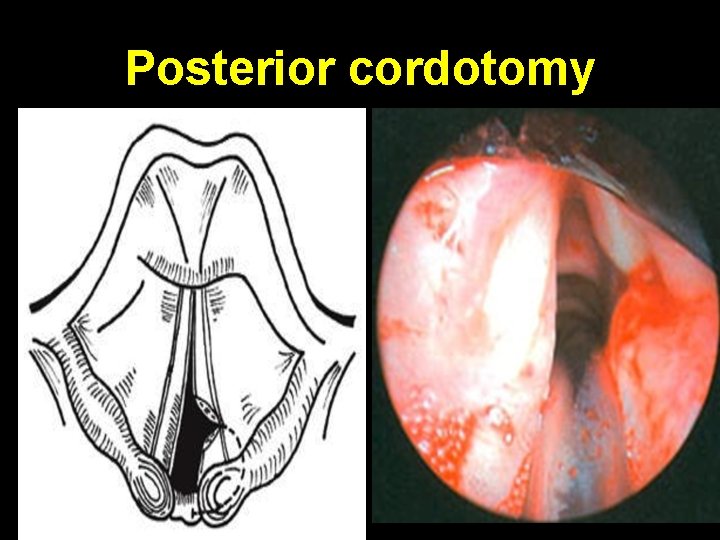
Posterior cordotomy

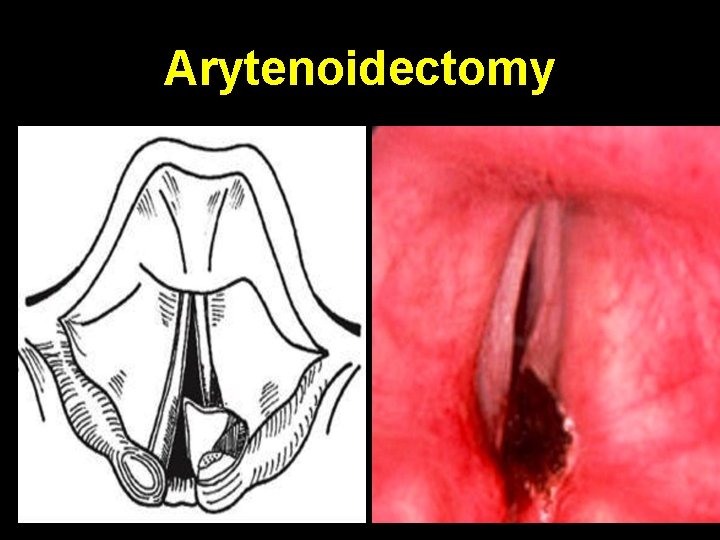
Arytenoidectomy

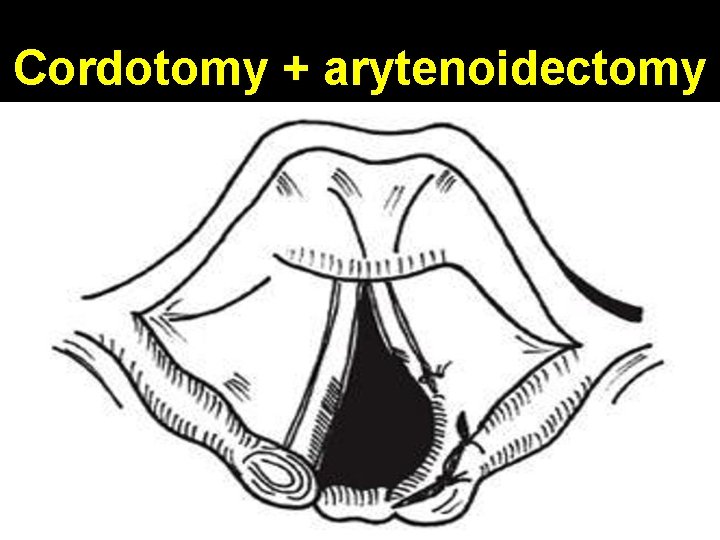
Cordotomy + arytenoidectomy

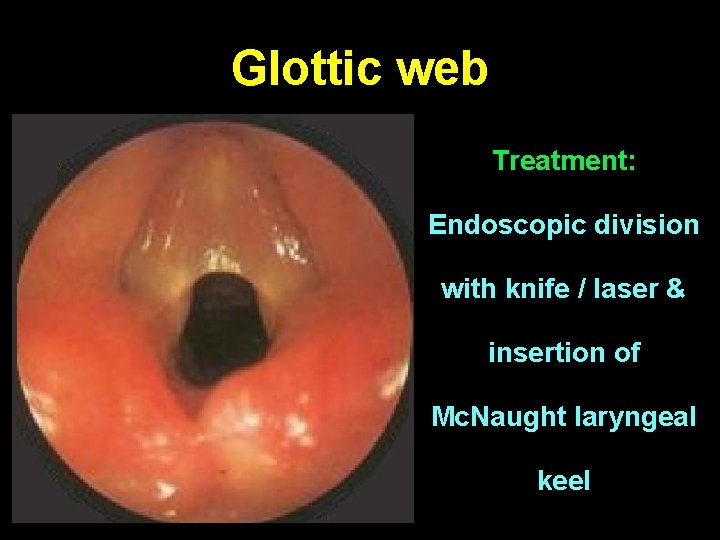
Glottic web Treatment: Endoscopic division with knife / laser & insertion of Mc. Naught laryngeal keel

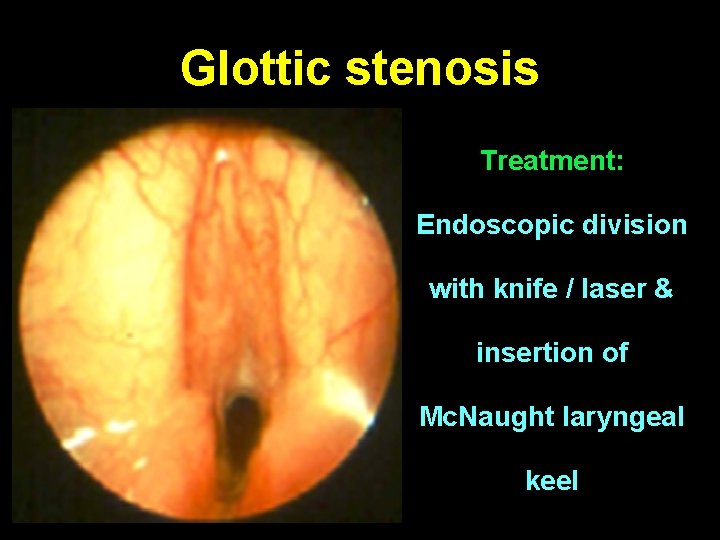
Glottic stenosis Treatment: Endoscopic division with knife / laser & insertion of Mc. Naught laryngeal keel

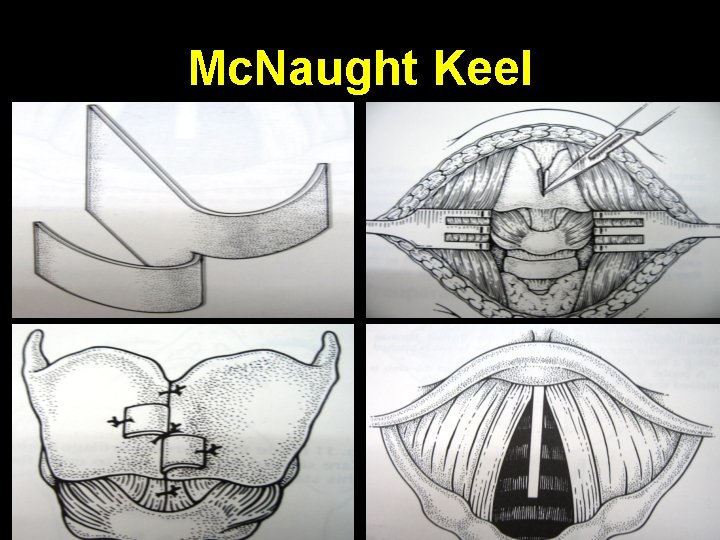
Mc. Naught Keel

Cri-du-chat syndrome • Cri – du – chat means cry of the cat • Partial depletion of short arm of chromosome 5 • High pitched mewing stridor • Diamond shaped glottic space, narrow vocal cords, curved & elongated supraglottis • Treatment: 1. Supportive care 2. Genetic counseling

Sub-glottic abnormalities

Congenital subglottic stenosis • Definition: diameter of subglottic lumen < 4 mm in term infant & < 3 mm in pre-term infant • Etiology: Incomplete recanalization of laryngotracheal tube during 3 rd month of gestation • Types: 1. Membranous: more common & mild form 2. Cartilaginous: less common & severe form • Clinical presentation: Symptoms appear in first few months of life. Biphasic stridor. Cry is normal.

Flexible laryngoscopy

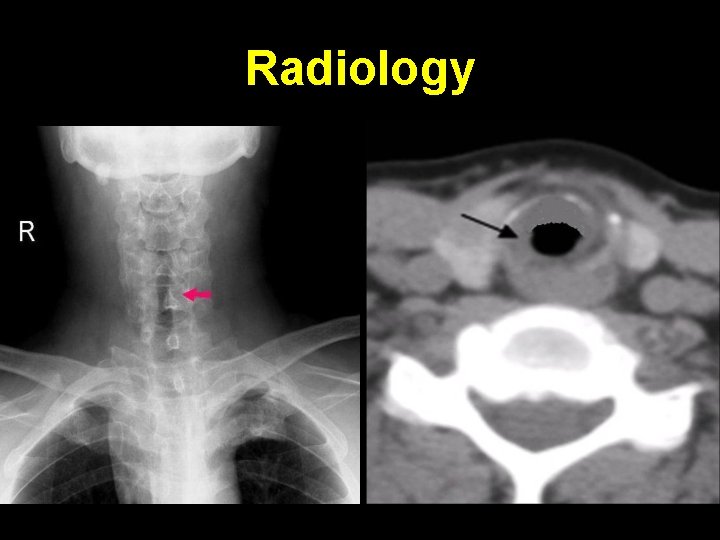
Radiology

Treatment Most cases resolve spontaneously by 4 years. Tracheostomy for significant stridor. Tube removed by 4 years when subglottic space widens. Laser ablation for membranous stenosis < 5 mm. Crico-tracheal resection & Laryngo-tracheo-plasty in patients who could not be decannulated.

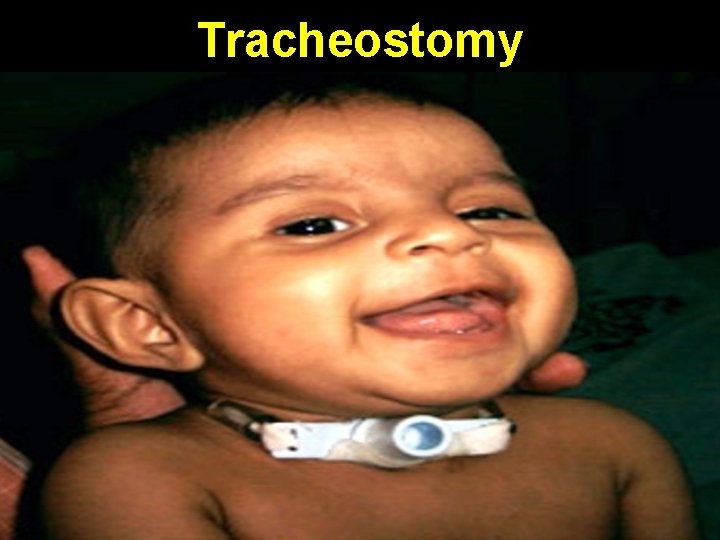
Tracheostomy

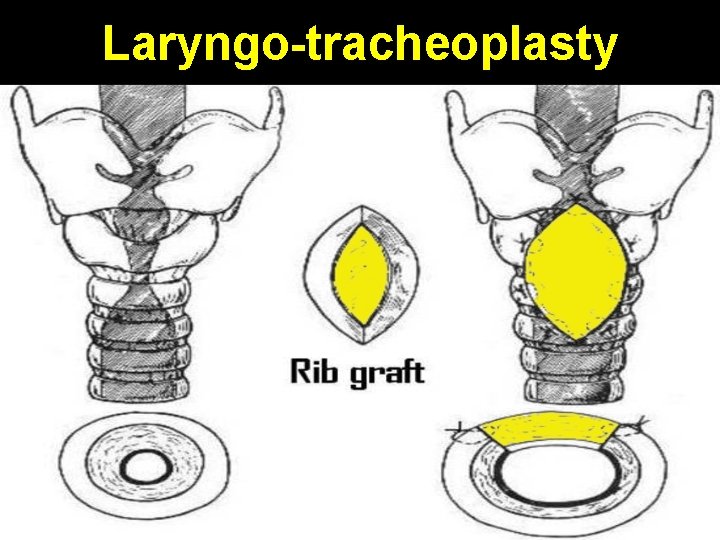
Laryngo-tracheoplasty

Subglottic hemangioma • Capillary hamartomas • Symptoms appear by age 2 -12 months • Biphasic stridor, barking cough & hoarse cry • 50% have cutaneous hemangiomas of head & neck • Flexible laryngoscopy: unilateral or bilateral lesion • Located postero-laterally in subglottis submucosa, pink-blue in color, sessile & easily compressible

Flexible laryngoscopy

Management Observation: for small lesions without stridor Tracheostomy: for significant airway obstruction. Tube kept till 5 years. Specific treatment: 1. Laser ablation 2. Cryosurgery 3. Sclerosing agent: intra-lesional injection 4. Open surgical excision

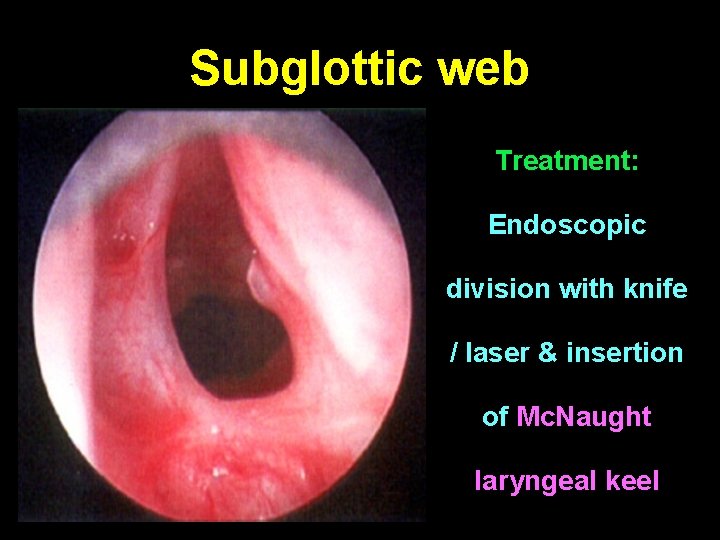
Subglottic web Treatment: Endoscopic division with knife / laser & insertion of Mc. Naught laryngeal keel

Evaluation of Stridor

Stridor vs. Stertor • Stertor is noisy respiration due to turbulent air flow through partially narrowed air passage above larynx • Stridor is noisy respiration due to turbulent air flow through partially narrowed air passage at or below level of larynx

Etiology for stertor Nasal: choanal atresia, ethmoid polyps Mandible: Pierre Robin syndrome Tongue: macroglossia, lingual thyroid Pharynx: adeno-tonsillar hypertrophy, retropharyngeal abscess, neoplasm Miscellaneous: Ludwig’s angina, Maxillo-facial #

Etiology for stridor

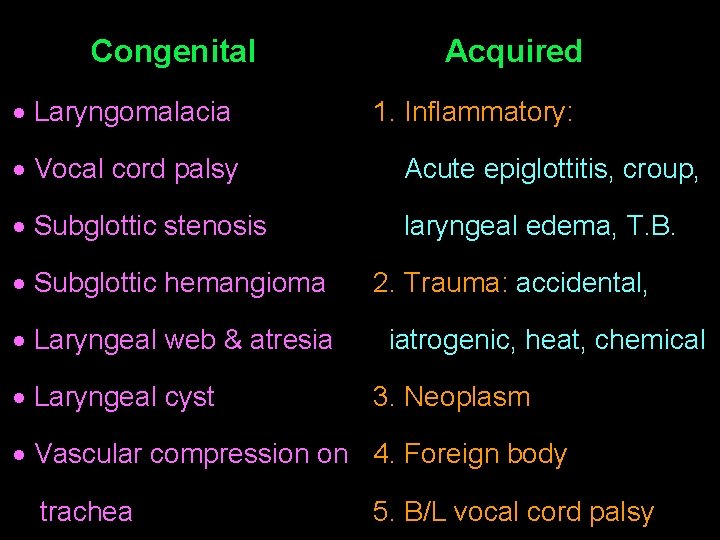
Congenital Laryngomalacia Acquired 1. Inflammatory: Vocal cord palsy Acute epiglottitis, croup, Subglottic stenosis laryngeal edema, T. B. Subglottic hemangioma Laryngeal web & atresia Laryngeal cyst 2. Trauma: accidental, iatrogenic, heat, chemical 3. Neoplasm Vascular compression on 4. Foreign body trachea 5. B/L vocal cord palsy

Causes of B/L vocal cord palsy • Thyroid surgery • Ca thyroid • Cancer cervical esophagus • Cervical lymphadenopathy

History Taking 1. Congenital or acquired after birth 2. Present only during sleep stertor 3. Related to feeding aspiration due to laryngeal paralysis, esophageal obstruction 4. Foreign body, blunt injury, endoscopy, intubation 5. Sudden onset foreign body, injury, infection 6. Long standing + progressive Laryngomalacia, laryngeal stenosis, neoplasm

Physical Examination 1. Respiratory timing of stridor: Inspiratory supraglottis or pharynx Biphasic glottis, subglottis or cervical trachea Expiratory lower trachea, bronchi or alveoli 2. Signs of airway resistance: nasal flaring, intercostal / subcostal / supraclavicular recession, cyanosis

Physical Examination 3. Associated fever: inflammatory cause 4. Stridor disappears in prone position: laryngomalacia, macroglossia, micrognathia, vascular compression of trachea 5. Resting respiratory rate: look for tachypnoea 6. Resting heart rate: look for tachycardia

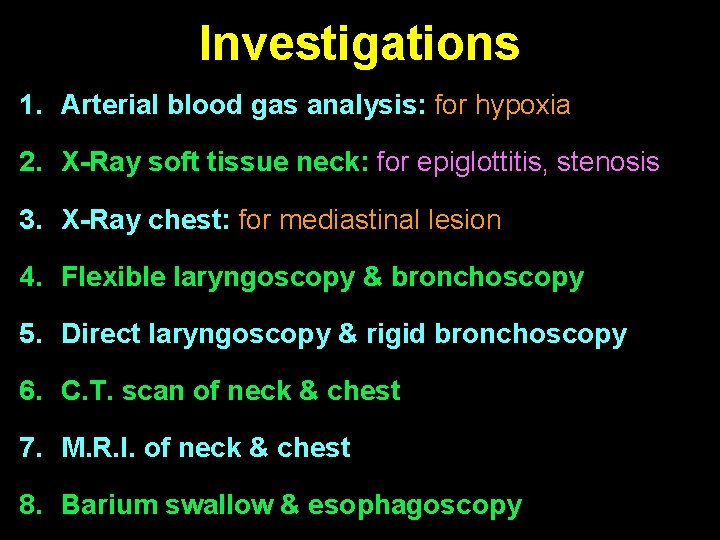
Investigations 1. Arterial blood gas analysis: for hypoxia 2. X-Ray soft tissue neck: for epiglottitis, stenosis 3. X-Ray chest: for mediastinal lesion 4. Flexible laryngoscopy & bronchoscopy 5. Direct laryngoscopy & rigid bronchoscopy 6. C. T. scan of neck & chest 7. M. R. I. of neck & chest 8. Barium swallow & esophagoscopy

Thank You