CONGENITAL INFECTIONS Intrauterine and Perinatal Infetions The major




















































- Slides: 65

CONGENITAL INFECTIONS Intrauterine and Perinatal Infetions

The major characteristics n Transplacental transmission n Various agents: viruses, bacteria, parasites n A similar clinical features: n multi-organ infection

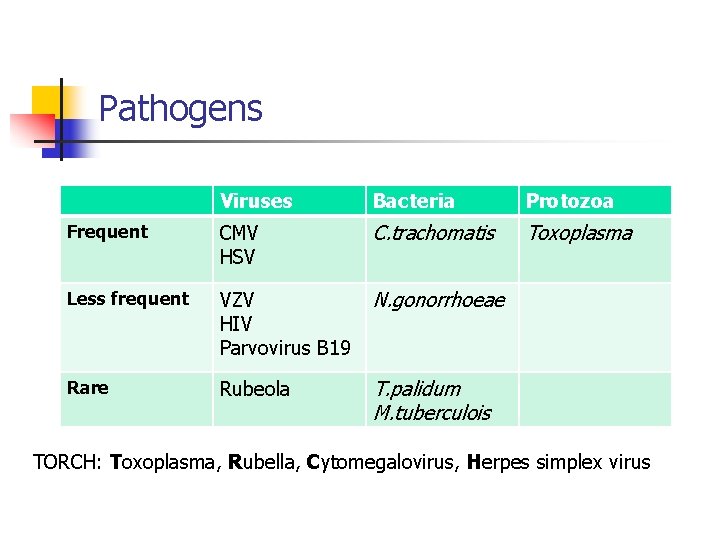
Pathogens Viruses Bacteria Protozoa Frequent CMV HSV C. trachomatis Toxoplasma Less frequent VZV HIV Parvovirus B 19 N. gonorrhoeae Rare Rubeola T. palidum M. tuberculois TORCH: Toxoplasma, Rubella, Cytomegalovirus, Herpes simplex virus

Clinical features n Generalized disease of the fetus / newborn n n n Intrauterine growth restriction Nonimmune hydrops (generalized edema) Anemia, leucopenia, thrombocytopenia Jaundice, hepto-splenomegaly Chorioretinitis, encephalitis Pneumonitis, myocarditis Congenital malforamtions n Depending on the time of infection and the pathogen

CYTOMEGALOVIRUS

Cytomegalovirus n The most frequent congenital infection n Infection in pregnancy: 35% risk for fetus n n n More symptoms on birth Reactivation of latent maternal CMV infection n n earlier gestation mother’s primary infection also may cause fetal infection ~1% of newborns with congenital CMV infection

CMV Symptomatic disease on birth (10%) n Low birth weight for gestational age n Jaundice and hepato-splenomegaly n Hepatitis (does not become chronic) n Blueberry muffin rash n Leucocoria (chorioretinitis) n Microcephaly n n intracerebral periventricular calcifications generally with no symptoms of encephalitis

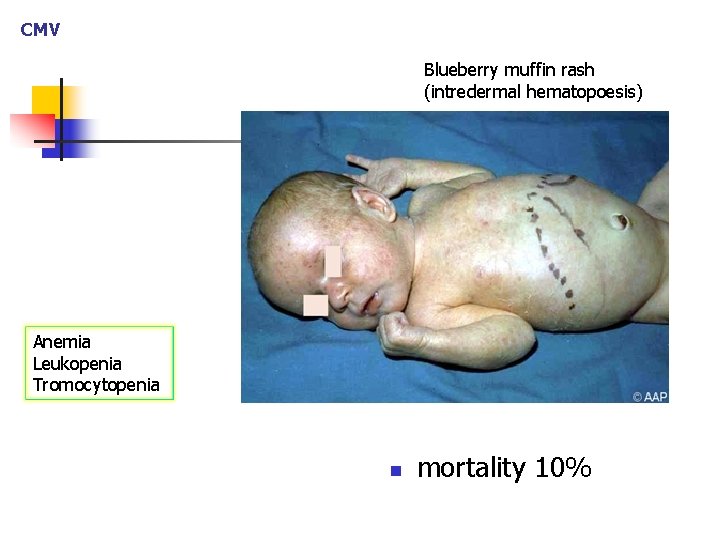
CMV Blueberry muffin rash (intredermal hematopoesis) Anemia Leukopenia Tromocytopenia n mortality 10%

Asymptomatic infection n 90% asymptomatic on birth n but ~ 10% of them develop: n n n sensorineural hearing loos (SNHL) chorioretinits later in childhood: disorders of psychomotor development

CMV The so-called “asymptomatic" infections: n n Chorioretinitis Hearing loss May be the only consequences! Screening is required! n They may affect the child’s development

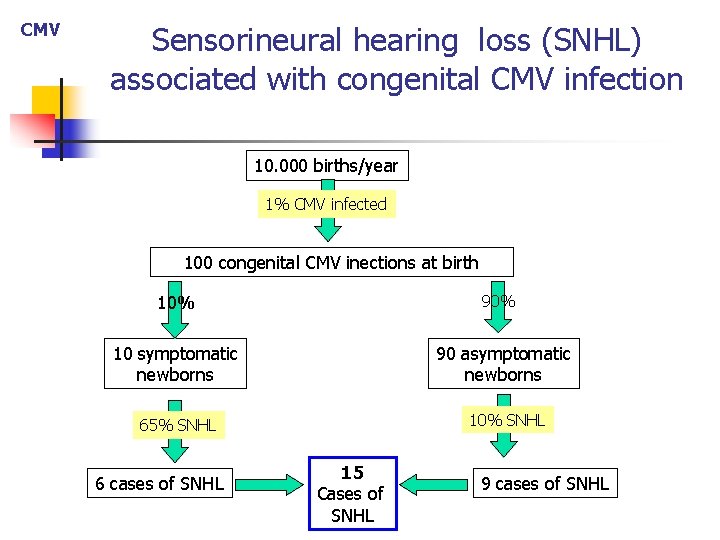
CMV Sensorineural hearing loss (SNHL) associated with congenital CMV infection 10. 000 births/year 1% CMV infected 100 congenital CMV inections at birth 10% 90% 10 symptomatic newborns 90 asymptomatic newborns 65% SNHL 10% SNHL 6 cases of SNHL 15 Cases of SNHL 9 cases of SNHL

CMV Diagnosis n DNK urin, saliva, blood, CSF n Culture of virus n n n standard culture = several weeks culture + monoclonal Ab detection = 24 h Serological tests n presence of Ig. M on birth = congenital infection

CMV Therapy n Ganciclovir n may halt the progression of hearing loss

TOXOPLASMOSIS

Toxoplasmosis Patogenesis n Usually during mother’s primary infection n n reactivation of latent infection - extremely rare Transmission rate = overall 30 -40% n earlier maternal infection = the lower risk for fetal infection n later maternal infection = hihgher risk for fetal infection n n because of better placental blood flow transmission rate near to birth term ≈90%

Toxoplasmosis Symptoms n Severity of fetal disease n n the earlier infection = the more severe simptoms High risk period = 10 -24 gestational week n n Developed placental blood flow Vulnerable fetal period

Toxoplasmosis “Asymptomatic” disease at birth In most newborns- with no obvious simptoms n But by detailed examinations can reveal: n Chorioretinitis n Intracerebral cortical calcifications n n with inflammatory CSF finding Signs of hydocephalus classic triad

Toxoplasmosis Symptomatic disease on birth: n n n Low birth weight Jaundice (early, within 24 h postnatally) Hepato-splenomegaly Maculopapular rash Triad: choriretinitis, cerebral calcifications, hydocephalus n seizures are frequent High risk for permanent neurological sequellae

Diagnosis n Serologically n Ig. G seroconversion, or 4 -fold rise n n 1 -2 months to achive peak Presence of Ig. M, Ig. A or Ig. E confirms diagnosis n PCR n histological examination of the placenta

Other diagnostic procedures n ophthalmologic examination n hearing testing (Auditory Evoked Potentials) n CT of brain n LP: CSF examination

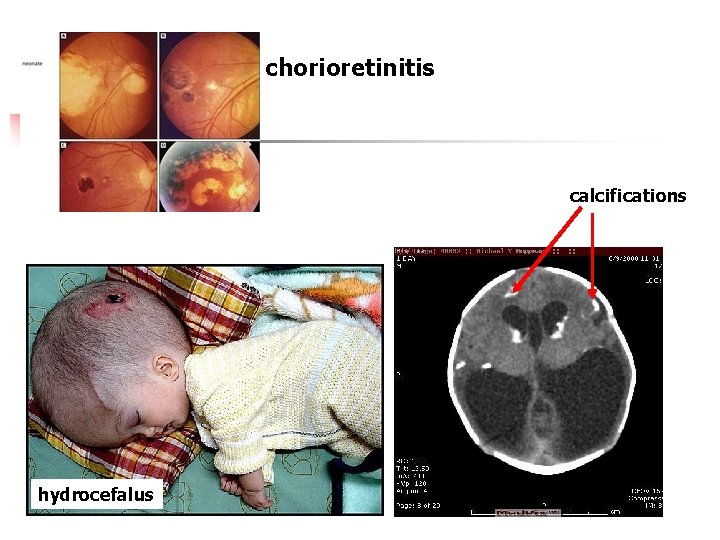
chorioretinitis calcifications hydrocefalus

Toksoplazma Therapy n Pyrimethamin + Sulfadiazin n n 12 months Therapy of infected pregnat women n if an infection is detected before birth

Toksoplazma Prevention n To prevent infection of pregnant women: n n Cooking of food or freezing or below -200 C Thorough hand hygiene: n n after preparing raw meat and vegetables after contact with cats

RUBELLA

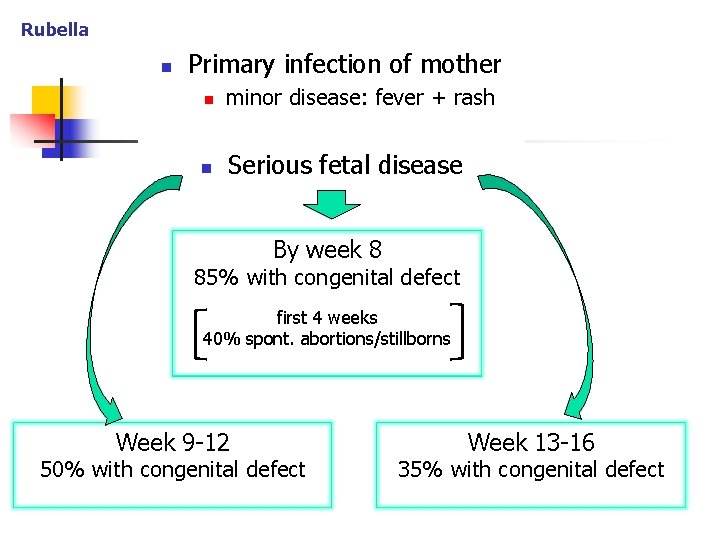
Rubella n Primary infection of mother n minor disease: fever + rash n Serious fetal disease By week 8 85% with congenital defect first 4 weeks 40% spont. abortions/stillborns Week 9 -12 50% with congenital defect Week 13 -16 35% with congenital defect

Rubella After gestational week 20 n congenital defects do not appear n but chronic infection (inflammation) is possiblle n Affected organs n n n Eyes Hearing CNS

Rubella Clinical features n Congenital malforamtions n Genealised disease on birth n “Asymptomatic” infectionon birth

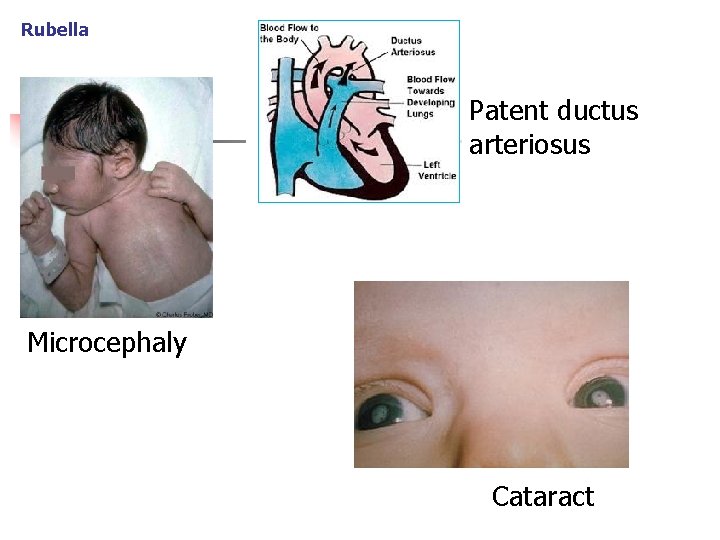
Rubella Congenital malformations n Cardiovascular n n patent ductus ateriosus Botagli pulmonary artery stenosis ventricular and atrial septal defects Eyes n Cataract, chorioretinitis, galucom n Hearing loos (SNHL) n Damage of CNS n n microcephaly, mental retardation spastic paralysis, ect. . .

Rubella Patent ductus arteriosus Microcephaly Cataract

Rubella Symptomatic infectionon birth: generalised newborn disease n n n Low bith weight Jaundice, hepatosplenomegaly Thrombocytopenia Purpuric (blueberry muffin) rash Penumonitis Menignoencephalitis

Rubella “Asymptomatic” infectionon birth n Often lower birth weight n Later may become apparent n n n SNHL glaucoma, cataract CNS damage: n n Behavioral disorders Mental retardation

Rubella Diagnosis Postnatally: 1. Serology - detection of antibodies n n Ig. M- evidence of fetal infection n produced only by child Ig. G- Initially can be maternal n later only child’s Ig. G remain 2. Viral culture (throat, urine, blood, CSF …)

Rubella Dijagnosis Prenatally 1. Viral culture of amniotic fluid 2. RNA hybridization from biopsied chorionic vill

Rubeola Prevention n MPR vaccine (live attenuated) 2. during 2 nd year of life at the beginning elementary school n Pregnant women - not to vaccinate: 1. n n viraemia and fetal infection is possible 3 mo. after vaccination pregnancy should be avoided CAUTION: virus is exreted by various body fluids for ≈ 1 year - Keep child away from unvaccinated pregnant woman -

HERPES SIMPLEX VIRUS TYPE 1 AND 2

HSV Epidemiology n 90% of HSV infections occurs during delivery n HSV-2 in 80% of cases n Most often symptoms of genital herpes are absent n n mother’s primary infection = high risk of trassmision recurrent genital heres = low risk of trasmission

Pathogensis n Intrauterine infection (rare) n n Transplacental trasmission from viremic mother dissemination to multiple organs n CNS- most freqently affected

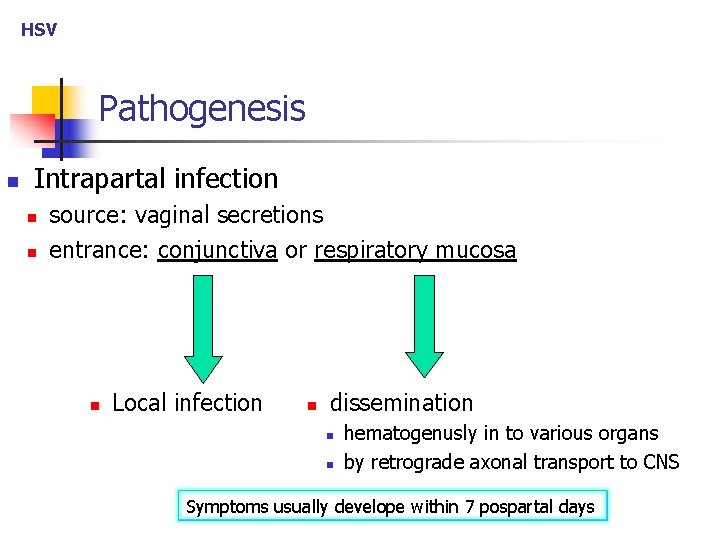
HSV Pathogenesis n Intrapartal infection n n source: vaginal secretions entrance: conjunctiva or respiratory mucosa n Local infection n dissemination n n hematogenusly in to various organs by retrograde axonal transport to CNS Symptoms usually develope within 7 pospartal days

HSV Clical features from Mild disease n vesicles or scarring of skin / mucous membranes …. to severe disease n generalized (disseminated) disease n encephalitis as the only manifestation n pneumonia as the only manifestation

HSV Disseminated disease n hepatitis, myocarditis, pneumonia, encefalitis n chorioretinitis, keratoconjunctivitis n rash (vesicles, bullae) in 70% n facilitate diagnosis

Diagnosis n Specimens: n n n swabs and aspirates of vesicles, conjunctiva, nasopharynx, rectum blood, CSF, urine, stool, Methods n n Viral culture PCR – evidence of viral DNA

Therapy n Aciclovir IV

Prevention: depending on circumstances of infection n n Primary infection of mother n risk for child = 50% n immediately introduce acyclovir therapy for mother!! mother Recurrent genital herpes n obtain swabs for viral dignosis n if symptoms are present - introduce acyclovir to child n otherwise - just follow up

SYPHILIS

Transmission n Hematogenous (transplacental) n n the most common Contact with mother’s chancre during birth n rare

Timing of sympomatic disease n Symptomatic at birth n Late neonatal onest n n Within 5 weeks postpartum Late onset n After 2 years of age

Symptomatic infection at birth n Stillbitrh n Generalised neonatal disease n Low birth weight, hepato-splenomegaly n Nonimmune hydrops + hemolytic anemia n Neutropenia and thromocytopenia

Late neonatal onset n Osteohondritis (metaphysitis), periostitis (new bone) n Rash: maculopapular desquamtive n Syphilitic rhinitis (hemorrhagic) n Hepatitis, lymphocytosis n Keratitis n CSF: pleocytosis + proteinorachia

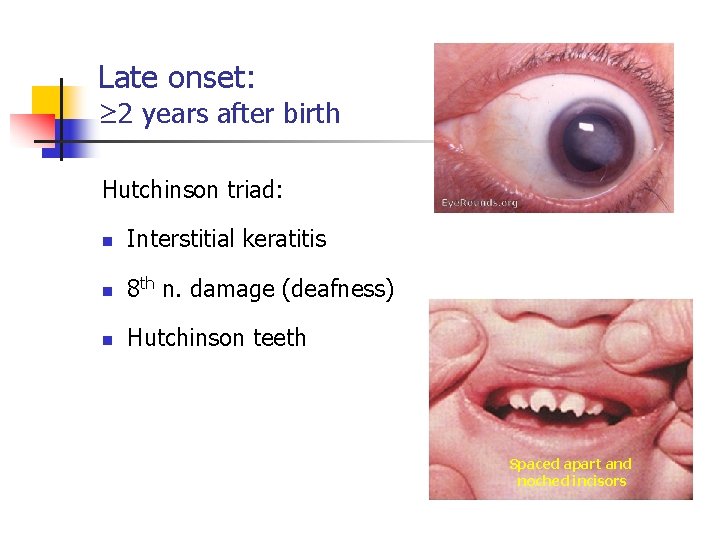
Late onset: ≥ 2 years after birth Hutchinson triad: n Interstitial keratitis n 8 th n. damage (deafness) n Hutchinson teeth Spaced apart and noched incisors

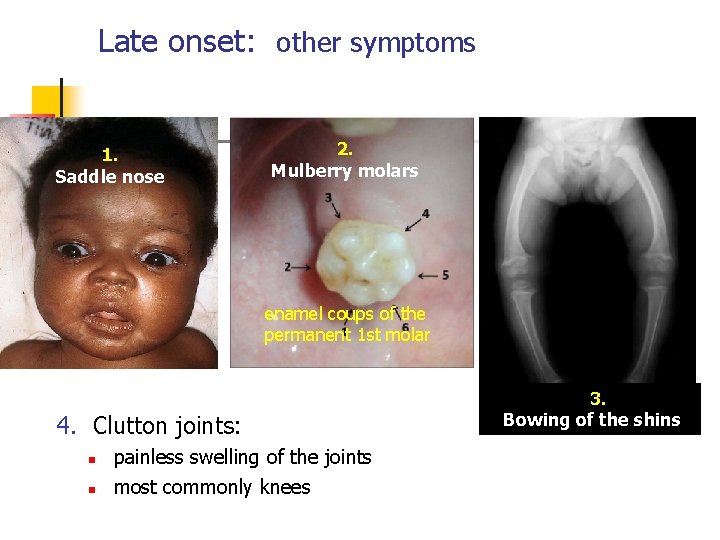
Late onset: other symptoms 1. Saddle nose 2. Mulberry molars enamel coups of the permanent 1 st molar 4. Clutton joints: n n painless swelling of the joints most commonly knees 3. Bowing of the shins

Diagnosis n Serology: n n n Non-treponemal Ab: VDRL, RPR Treponemal Ab: TPHA Who? n n All preganant women All newborns of positive mothers

Further evaluation of the child, if: n mother’s titers incease ≥ 4 -fold n child’s titers ≥ 4 -fold grater than mother’s titers n child of positive mother is asymptomatic n Infecion in late pregnacy- infant may incubate disease If diagnosis of congenital syphilis is estabilshed n LP and CSF serology should bi performed

Therapy n Penicillin G IV / 2 weeks Documeting cure n Falling Ab titers at month 3, 6 and 12 n In case of neurosyphilis: CSF Ab titers n every 6 months /3 years

CHLAMIDIA TRACHOMATIS

Epidemiology n Source: mother with genital infection n Infection occurs during childbirth n n risk for penumonia: up to 20% risk for conjunctivitis: up to 50%

Symptoms n Conjunctivitis n 5. -14. day of life n conjunctival redness, eyelids edema n discharge: watery, then purulent n duration: about 2 weeks n scars (pannus) are rare

n Pneumonia n occurrence: 2 -19 weeks of age No fever dyspnea, attacks of "staccato" cough n chest X-ray: n n diffuse interstitial infiltrations, and hypeinfaltions

Diagnosis n Laboratory findings are nonspecific n slightly higher % eosinophils Pneumonia n serologic evidence Conjunctivitis: conjunctival scraping n n n detection of antigens (DF, ELISA)- usualy Direct microskopy or culture PCR

Differential diagnosis Neisseria gonorrhoeae conjunctivitis n Earlier onset: within first 5 days postpatrum n more serious disease: corneal ulceration

Therapy of Chl. trachomatis n Erythromycin PO /14 dana n Conjunctivitis and penumonia Topical prophylaxis: useless

NEISSERIA GONORHHOEAE

n Conjunctivitis (ophtalmia neonatorum) n n most common Other manifestations: n n n Scalp abscesss Vaginitis Disseminated disease (sepsis, meningitis)

Ophtalmia neonatorum n Onset: within first 5 days of life n Symptoms: n n Early disease: similar to chlamydial conjunctivitis Later: corneal ulceration/perforation Caution! n n the child should be hospitalized disseminated disease should be excluded/treated

Therapy n n Ceftriaxon IM / one dose + Frequent saline eye irrigation n Topical antibiotic? : Needless! Recomanded simultaneous testings for STDs: n n n C. trachomatis Syphilis HIV and HBV

Prophylaxis n Topical administration of : n n n silver nitrate, erytromicyn, or tetracycline