Congenital defects of carbohydrate metobolism CLASSICAL GALACTOSEMIA Defective

Congenital defects of carbohydrate metobolism


CLASSICAL GALACTOSEMIA • Defective enzyme: Galactose-1 phosphate uridyltransferase (incidence 1: 40, 000) • Mechanism: Accumulation of galactose-1 -phosphate causes intracellular ATP depletion and very toxic for liver, kidney and brain.
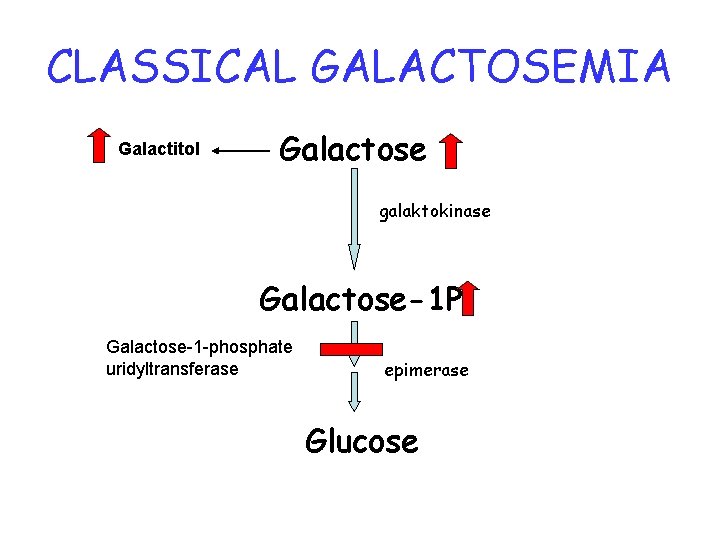
CLASSICAL GALACTOSEMIA Galactitol Galactose galaktokinase Galactose-1 P Galactose-1 -phosphate uridyltransferase epimerase Glucose

• Clinical findings: Progressive symptoms after start of milk feeds. Usually starting on the 3 rd and 4 th day. • Vomiting, diarrhea, jaundice, disturbances of liver function tests, death from severe liver and renal failure, sepsis (especially by E. Coli), bilateral cataracts (due to galactitol accumulation)

Diagnosis • Low galactose-1 -phosphate uridyltransferase activity (Beutler test) • High galactose and galactose-1 -phosphate levels (N: 0 -0. 3 mg/d. L) in serum or erythrocytes. • Renal tubular damage: Generalized aminoaciduria, albuminuria, • Reducing substances in urine (Fehling or Benedict test) due to glucosuria and galactosuria.

• Therapy: Lactose-free and galactose restricted diet throughout life. Keep galactose-1 -phosphate levels under 5 mg/d. L. • Complications: Mild mental retardation, ataxia, tremor; gonodal dysfunction, disturbed pubertal development (especially in girls)

EPIMERASE DEFICIENCY Galactitol Galactose galaktokinase Galactose-1 P Galactose-1 -phosphate uridyltransferase epimerase Glucose Most of the cases are asymptomatic. Symptomatic cases like classical galactosemia.
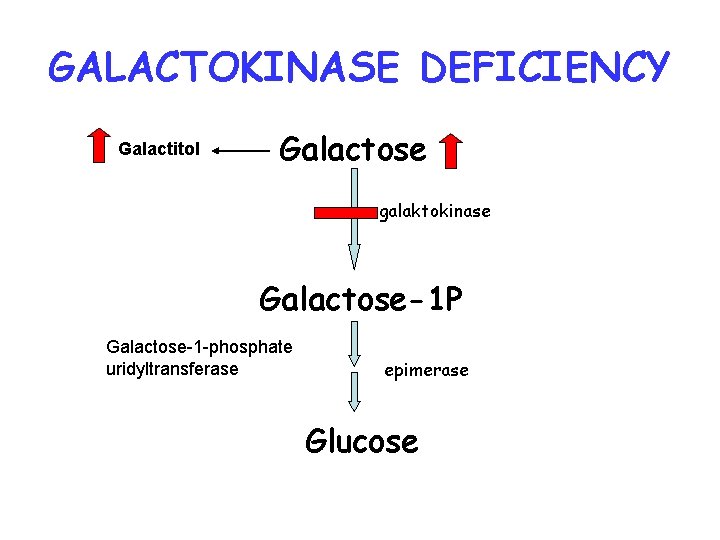
GALACTOKINASE DEFICIENCY Galactitol Galactose galaktokinase Galactose-1 P Galactose-1 -phosphate uridyltransferase epimerase Glucose

GALACTOKINASE DEFICIENCY Clinical findings • Rapidly progressing bilateral central cataract. Reversible in the first few weeks of life. • No hepatorenal damage Therapy: Lactose-free diet
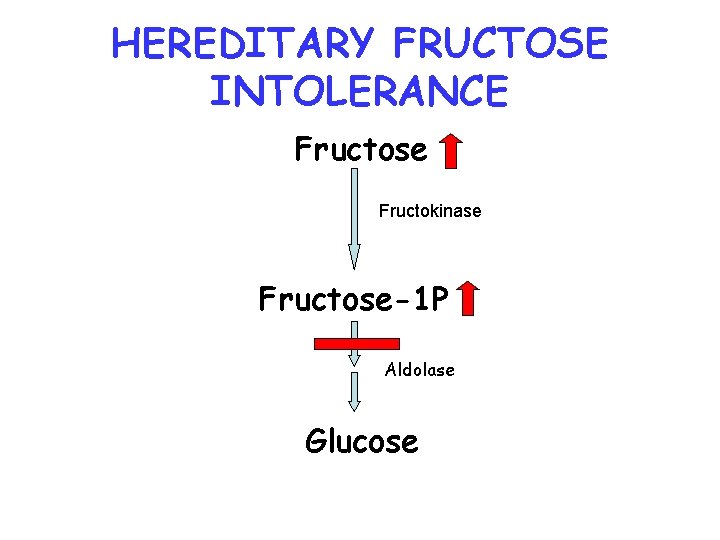
HEREDITARY FRUCTOSE INTOLERANCE Fructose Fructokinase Fructose-1 P Aldolase Glucose

HEREDITARY FRUCTOSE INTOLERANCE • Defective enzyme: Aldolase B (incidence 1: 20, 000) • Mechanism: Accumulation of fructose-1 phosphate causes intracellular ATP depletion and very toxic for liver, kidney and brain.

• Clinical findings: Symptoms after weaning or supplementary feeds. • Vomiting, apathy liver dysfunction with hepatomegaly, hypoglycemia (inhibition of glycogenolysis) renal tubular dysfunction, distribution of liver function tests, failure to thrive, aversion to fructose containing foods/sweets, no caries.

• Diagnosis: Clinical symptoms with fructose loading (dangerous!); positive effect of withdrawing fructose; enzyme studies. • Renal tubular damage: Generalized aminoaciduria, albuminuria, Reducing substances in urine (Fehling or Benedict test) due to glucosuria and galactosuria. • Therapy: Strict fructose restricted diet throughout life.

ESSENTIAL FRUCTOSURIA • Defective enzyme: Fructokinase • Clinical findings: asymptomatic. • Diagnosis: Positive reducing substance in urine (incidental finding)

Glycogen storage diseases


Glycogen storage diseases – Classification • Liver involvement and hypoglycemia (Type 0, I, VI) • Muscle involvement (Type II, V, VII) • Liver involvement, muscle involvement and hypoglycemia (Type III). • Liver cirrhosis: (Type III , Type IV).

GSD Type O • Defect: Liver glycogen synthase • Clinical: Convulsions in the early hours of morning • No Hepatomegaly • Hypoglycemia inresponsive to glucagon


Type I a (von Gierke)/ Clinic/Laboratory • Neonatal hypoglycemia • Lactic acidosis, ketosis • Hepatomegaly • Hyperuricemia gout • Hyperlipidemia • Lipid accumulation in the cheeks (doll facies).

Type I a (von Gierke)/Diagnosis • Hypoglycemia inresponsive to glucagon • Glucose challange test: Glucose (increase), Lactate (decrease) • Diagnosis: Low liver glucose-6 phosphatase levels.

GSD Type I a (von Gierke)/Therapy • Avoid hypoglycemia by means of continous carbohydrate intake. • Frequent meals (every 2 -3 hours in infants, 4 -6 hours in school age) • Slowly resorbed carbohydrates (raw –uncookedstarch) • Limited fructose, lactose, no sucrose, • Nights: Continous intake of glucose polymers (starch) via nasogastric tube

GSD Type Ib • Enzyme: Glucose-6 -phosphate transporter (edoplasmic reticulum) • Clinical: looks like GSD type Ia • Plus: neutropenia, leucocyte dysfunction, frequent infections, Crohn like inflammatory bowel disease. • Treatment of neutropenia: G-CSF and GMCSF

GSD type Ic and Id • Clinical: Similar GSD type Ia • Ic: Inorganic phospate transport defect (T 2 protein disorder) • Id: GLUT 7 microsomal transport defect

GSD type VI Hers disease • Enzyme: Liver phosphorylase defect • Clinical: Failure to thrive, hepatomegaly, mild hypoglycemia • Diagnosis: Elevated lactate and transaminases, enzyme studies: Liver, erythrocytes, leucocytes • Prognosis: Fairly good, often asymptomatic


GSD type VII Tarui disease • Enzyme: phosphofruktokinase (muscle, erythrocyte, platelets) • Severe myopathy • Postprandial exercize intolerance (does not respond to glucose infusion) • Mild hemolytic anemia • Hyperuricemia (post exercize) • PAS positive, abnormal amilopectin accumulation

GSD type IX • Enzyme: Phosphorylase kinase • X related liver form (most frequent) • AR liver and muscle form • AR liver form • Muscle form • Cardiac form
GSD type II (Pompe disease) • Enzyme: alpha-1, 4 -glucosidase (asid maltase); lysosomal enzyme; minimal role in glucose metabolism. • Storage of cholesterol esters and triglycerides. • İnfantile form : Severe cardiomyopathy and myopathy, hypotonia, hepatomegaly, failure to thrive, untreated fatal in the first year • Juvenile-adult form: Slowly progressing skeletal muscle weakness, no cardiomyopathy • Diagnosis; Vacuolated lymphocytes, EKG: PR-shortness and massive QRS waves, enzyme studies • Enzyme replacement therapy


GSDType III (Cori / Forbes disease) • Defective Enzyme: Debrancher enzyme= amylo-1, 6 -glucosidase accumulation of limit dextrin in liver and muscle. • Type IIIa: (Liver+muscle involvement): In infancy same as in GSD Type I; but normal lactate/uric acid, mild hypoglycemia, improvement in childhood, hepatomegaly, normal kidney size, failure to thrive; Progressive myopathy, cardiomyopathy, neuropathy • Type IIIb: (Only liver involvement) • Diagnosis: decreased alanine, leucine, isoleucine, elevated valine; increased transaminases and cholesterol. Enzyme studies: Liver, muscle, erythrocytes, fibroblasts • Therapy: Frequent feeding, maintain normoglycemia

GSD Type IV (Andersen disease) • Defective Enzyme: Branching enzyme = amylo-1, 4 -> • 1, 6 transglucosidase; accumulation of amylopectin like glycogen molecule • Classic form: failure to thrive, hepatomegaly, progressive liver disease -> cirhossis, liver failure, often fatal by age of 4 -5 years • Mild form; Non-progressive • Neuromuscular forms • Enzyme studies: Liver, muscle, erythrocytes, fibroblasts • Therapy: Liver Transplantation ?


GSD Type V (Mc. Ardle disease) • Enzyme: Muscle phosphorylase • Clinical: Adolescent/Adult onset; exercise intolerance, fatigue, muscle cramps, myoglobinuria • No postischemic hyperlactatemia, elevated CK • Diagnosis: muscle biopsy • Therapy: Avoid exessive exercise, creatine supplementation

Glucose transport defects

GLUT 1 deficiency • Clinical: Epileptic encephalopathy, microcephaly, psyhomotor retardation • Diagnosis: Fasting CSF: CSF glucose/ Blood glucose<0. 45; lactate: N, or decreased • Therapy: Ketogenic diet. • Avoid these drugs: barbiturates, ethanol, methylxantines • Prognosis: Satisfactory with early treatment

GSD tip XI (Fanconi-Bickel syndrome) • GLUT 2 defect • Clinically resembles GSD type Ia • Dwarfism, Fanconi syndrome, rickets • Fasting hypoglycemia (no response to glucagon), postprandial hyperglycemia, aminoaciduria, phosphaturia, glucosuria • Glycogen accumulation in liver and kidneys

Congenital glucose-galactose malabsorption • SGLT 1 deficiency • Severe intestinal glucose and galactose transport defects, mild renal transport defect. • Clinical: Severe neonatal diarrhoea, dehydration • Diagnosis: Mild glucosuria, reducing substance in stools, normal fructose tolerance • Therapy: Dietary replacement of gucose/galactose with fructose

Renal glucosuria • SGLT 2 deficiency • Renal transport defect of glucose and galactose • No intestinal defect • Benign glucosuria with normal blood glucose and absence of generalized tubular dysfunction. • Therapy: None

CYSTIC FIBROSIS

Kistik fibrozda solunum epitelinde görülen sıvı sekresyonu ve emilimindeki bozukluklar
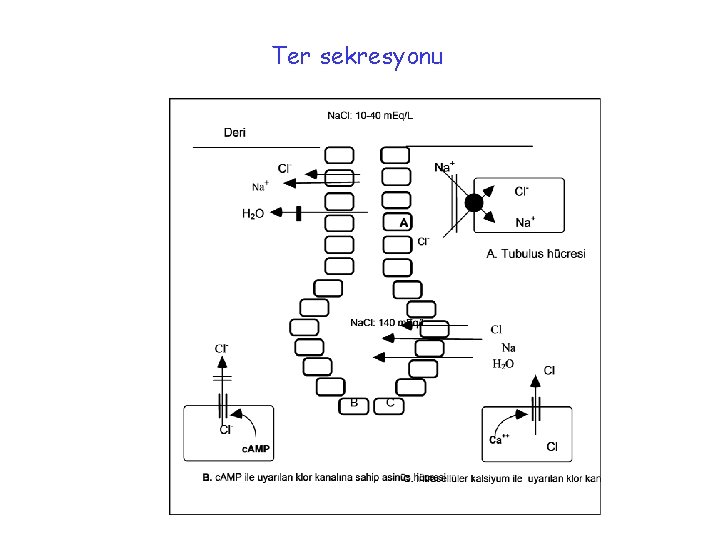
Ter sekresyonu

Cystic fibrosis-Genetics • Cystic fibrosis gene is localized in the long arm of 7 th chromosome (7 q 31. 2). • Cystic fibrosis gene codes cystic fibrosis transmembrane regulator (CFTR). • There are more than 600 mutations. The most frequent mutation is delta-F 508, 70 -80% in USA and 30% in Turkey) • Incidence: 1: 2500 in Caucasians, less frequent in Orientals where cholera is endemic. Incidence in Turkey is not known, but presumed to be high.

PATHOGENESIS • CTFR is inserted in the cell membranes and has the properties of ion channels. • In cystic fibrosis c. AMP-dependent chloride channels that regulate the water secretion and sodium channels regulate the water reabsorption are defective.

• Apical membranes of epithelial cells of exocrine glands are impermeable to chloride, and secondarily sodium and water. • Additionally epithelial cells reabsorb excessive amounts of sodium and secondarily water. • Decreased water secretion and increased water reabsorption (dehydrated secretions) lead obstruction, cysts and fibrosis in the exocrine glands (bronchial tree, pancreatic duct, gastrointestinal glands etc) with the exception of sweat gland.

• In sweat glands, chloride secretion and thereby the water secretion is normal in the secretory coil. • On the other hand sodium and secondarily chloride reabsorption by the ductus is decreased. • Therefore excessive amounts of salt are lost in the sweat (chloride levels are more than 60 m. Eq/L).

Kistik fibroz: Patogenez

CLINICAL MANIFESTATIONS • The most life threatening clinical features of CF, are pulmonary obstruction and infections. • Thick mucous secretions are associated with chronic obstructive lung disease predominantly involving the small airways. • Recurrent and persistent infections with Pseudomonas aeroginosa and cepecia (virtually diagnostic) and Staphylococcous lead to bronchiectasis and respiratory failure, often accompanied by cor pulmonale and death

CLINICAL MANIFESTATIONS • In 80 -90% of the patients exocrine pancreatic deficiency causes steatorhea and failure to thrive. • In 10 -20% of the patients, meconium ileus occurs in the neonatal period. Failure to pass meconium in the first 24 -48 hours of life. • Abdominal roentgenograms show dilated loops of bowel with a collection of granular groundglass material in the lower central abdomen.
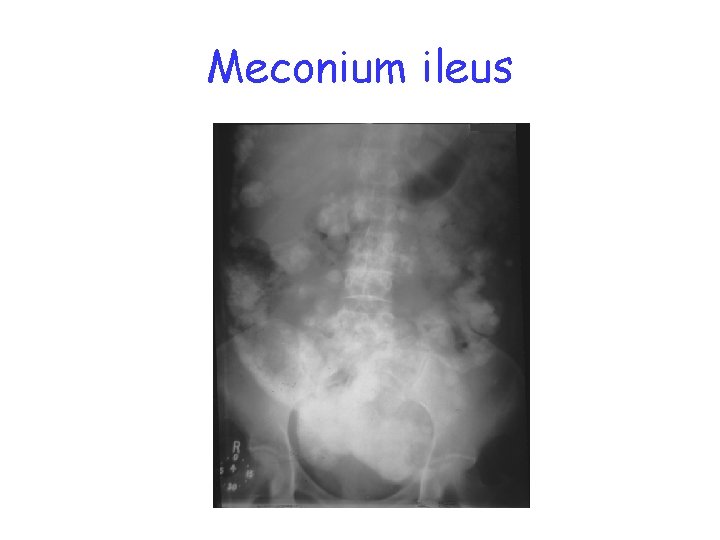
Meconium ileus

CLINICAL MANIFESTATIONS • Excessive lost of salt in the sweat leads hyponatremic dehydration in young children especially during high environmental temperature. • Secondary hyperaldosteronism causes hypopotasemia and metabolic alkalosis (Pseudo -Bartter syndrome). • 10% of patients diabetes mellitus develops, especially after the age of ten.

CRITERIA FOR DIAGNOSIS OF CYSTIC FIBROSIS • Typical pulmonary manifestations and/or • Typical gastrointestinal manifestations and/or • A history of cystic fibrosis in the family plus * Sweat chloride concentration >60 m. Eq/L and/or * Pathologic CTFR mutation on both chromosomes.

NEONATAL SCREENING • Most of the patients with CF can be identified by determination of immunoreactive tripsinogen in blood spots (Guthrie card). • This test is neither sufficiently sensitive nor spesific for CF. • This test is not valid after the age of three months (Serum tripsinogen levels decrease during progressive pancreatic damage).

Pulmonary therapy • The objective of pulmonary therapy is to clear secretions from airways and to control infections • Chest percussion + postural drainage • Bronchodilators: ß-sympathomimetic agents, teophylline • Expectorants: Are not effective, curcumin may be helpful (stimulation of Cl channel) • %3 -7 Na. Cl inhalation

Antibiotic therapy • Aerosol and/or intravenous: (Pseudomonas is more difficult to treat and rarely is eradicated) • Pseudomonas aeroginosa: amikasin, gentamycin, tobramycin, netilmycin, imipenem • Staphylococcous aereus: voncomycin, oxacillin

Nutritional therapy • High caloric diet (150% of normal calorie) without fat restriction • Pancreatic enzyme replacement • Fat-soluble vitamins (A, D, E, K) supplementation
- Slides: 57