Congenital and perinatal disorders of brain Genetic disorders

Congenital and perinatal disorders of brain • Genetic disorders • During pregnancy

Cerebral palsy • Neurodevlopmental nonprogressive lesion of the motor development of the child durineg prenatal, perinatal or postnatal damage of the brain • Affected - perception, cognition, communication, behaviour, epilepsy, musculosceletal problems

Cerebral palsy • Prevalence: 2 – 3/1000 • The most risk children – • Premature babies — particularly those who weigh less than 3. 3 pounds (1, 510 grams)

Cerebral palsy • 1. Prematur babies • 2. Intrauterine infections (toxoplazmosis, rubeola, cytomegalovirus, herpes, etc. . ), • 3. Developmental anomalies • 4. Intrauterine intoxication (alkohol, opiats, kokain, Pb, . . )

Cerebral palsy • 5. Fetal hypotrophy – chronic intrauterine hypoxy and malnutrition (mother´s hypertension, mother´s malnutrition, . . ) • 6. Intracranial bleeding • Unmaturated children – periventricular • Maturated children – hemispheral – hemispheres, thalamus, brainstem, cerebellum

Cerebral palsy • 7. hypoxic-ischemic damage • periventricular leukomalacia • Maturated - subcortical or parasagital leukomalacia

Cerebral palsy • Forms: • Spasticc – 65% • Dyskinetic-dystonicá (extrapyramidal) – 20% • Ataktic – 5% • Mixed forms

Cerebral palsy Spastic form • • Central motoneuron Diparetic – 30% Hemiparetic – 30% Kvadruspastic – 5% - mental retardation, epilepsy
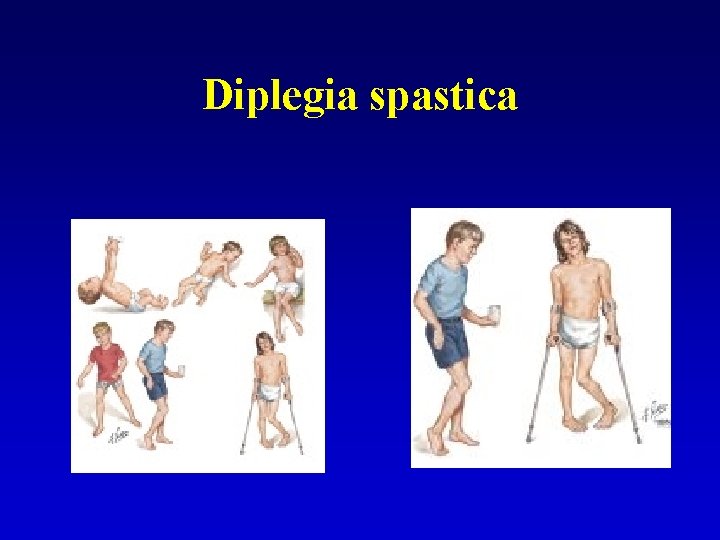
Diplegia spastica

Cerebral palsy Dyskinetic-dystonic form • Hyperkinetic – 20% • Dystonic – tonic contraction of extremity or all of the body • Bazálne ganglia • No mental retardation

Cerebral palsy Ataktic form • cerebellum • hypotonic syndrom, apathy, psychomotiric retardation

Cerebral palsy • 25% improvement • 50% improvent after physiotherapy – • Physiotherapy –Bobath and Vojta

Malformations and genetic abnormalities of brain

Dandy-Walker syndróm • Cystic enlargment of 4 th ventricle, hydrocephalus • Atresion of foramen Luschkae and Magendii, dysgenesis of cerebellar vermis
Arnold-Chiari malformation • Part of brainstem and cerebellar tonsils are below the level of foramen magnum • Sometimes hydrocephalus, spina bifida • Clinical feature – in adult age, bilateral pyramidal signs, lesions of cranial nerves, brainstem syndromes, syringomyely
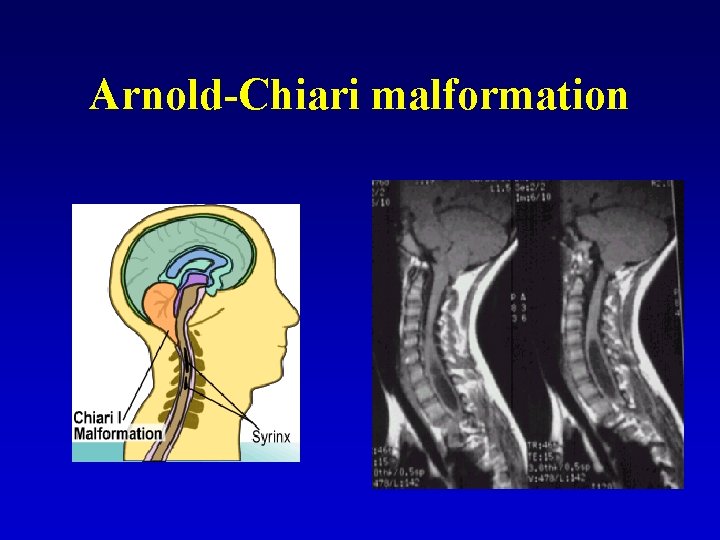
Arnold-Chiari malformation
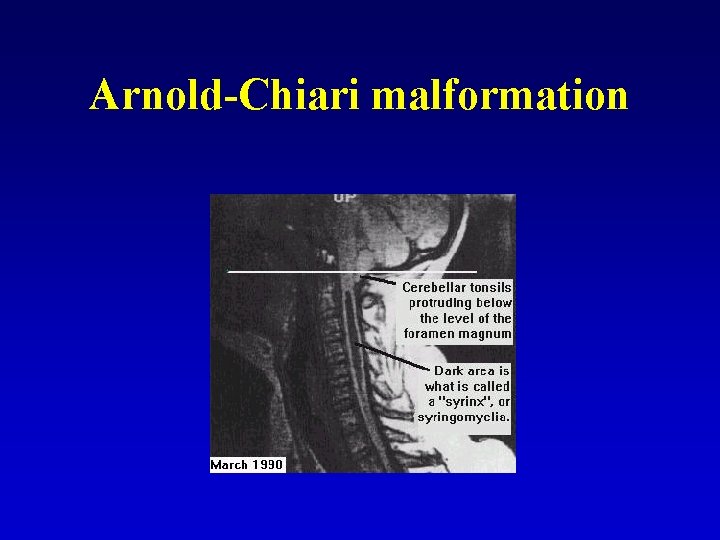
Arnold-Chiari malformation

Microcephalus • • Mental retardation Loss of hearing Spinocerebellar signs Risc for malignity

Meningoencephalocele, meningomyelocele • Development of neuronal tube – 19 th day of devolopment of faetus, occlusion of cranial and spinal end in the end of the 1 st month • Meninges and parts – from mesenchyma

Meningoencephalocele, meningomyelocele • Non connestions of bone spina bifida occulta (risc – low level of fol acid) • Herniation of meninges through defect in bone – meningocele • Brain and spine tissue in herniation – encefalo(myelo)meningocele • Part of ventricles in herniation – encefalo(myelo)meningocystocele




Meningoencephalocele, meningomyelocele • Neuronal tube is open, not covered– open anencephalus • Clinical feature – depends on localisation and severity • Spinal cord lesions - paraparesis paraplegia below the pathology of spinal cord incontinentia • Brainn lesions – depends on localisation

Meningoencephalocele, meningomyelocele • therapy • Surgery • Brain – meningocele and encefalomeningocele, • Spinal cord – good prognosis - operation during 1 st day



Meningoencephalocele, meningomyelocele • alfafetoprotein (child albumin in mother´s blood) • Malformation in 1 from 15 pregnancy with high levels • in 1 from 10 000 pregnancy with normal levels

Phakomatoses • Group of hereditary diseases affecting he skin and other organs as well as the brain

Tuberous sclerosis (Bourneville) • Mental deficit • Skin signs (adenoma sebaceum) • Brain lesions, lesions of kidney, heart, retina • Epileptic seizures • Intracranial calcifications • Autosomal dominant, chromosome 9

Tuberous sclerosis (Bourneville) • • Mental deficit – first 2 years Depigmental lesions of skin Naevus Pringle (adenoms) – in 1 st year Calcifications on X-ray - first 2 years Epi seazures - first 2 years Retina Brain lesions
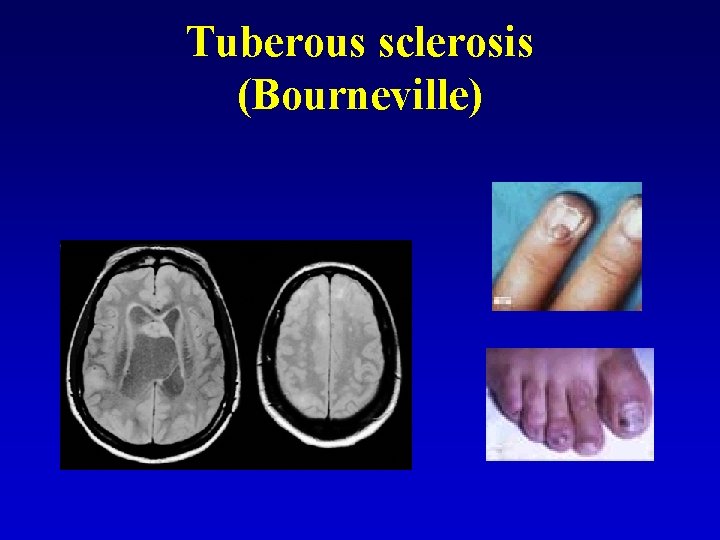
Tuberous sclerosis (Bourneville)

Tuberous sclerosis (Bourneville) Adenoma sebaceum

Encefalofacial angiomatosis (Sturge-Weber) • • • Cutaneous haematoma in face Seizures Mental retardation Hemiparesis X-ray – kalcifications at the convexity hemisfér (kalcifikácie v of hemisfers P-O • Autosomaly dominant

Encefalofacial angiomatosis (Sturge-Weber)
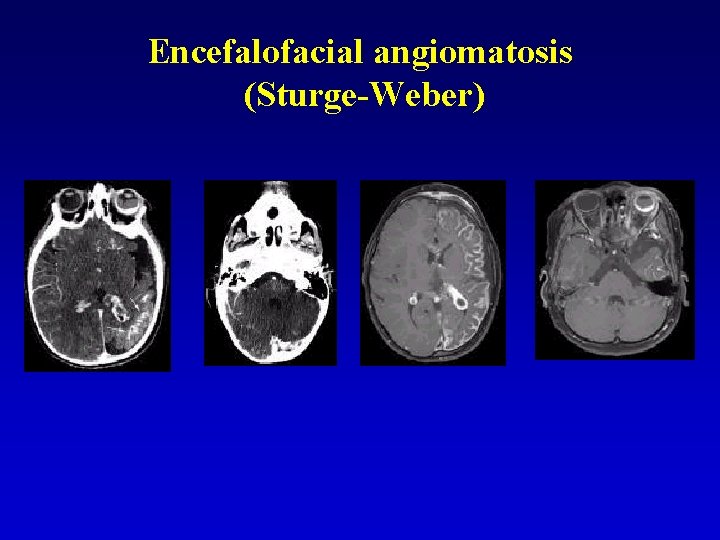
Encefalofacial angiomatosis (Sturge-Weber)
- Slides: 36