Conference will begin shortly Please stay on the

Conference will begin shortly. Please stay on the line as others join. 1

2018 Benefits Open Enrollment Effective January 1, 2018 2

Agenda • Medical plan: Traditional PPO • Medical plan: Federally-qualified High Deductible • • • Health Plan (HDHP) ◦ Health Savings Account (HSA) Dental, term life, accident and disability plans New Voluntary Vision Benefit Resources for your family BGCT Custom Landing Page How to enroll or make changes Q & A 3

Guide. Stone Brings Together Best-in-Class Providers Nationwide Medical Network Prescription Drug Pharmacy Worldwide Dental Network Life and Disability Benefits 4

Medical Plan Choices PPO – HC 3000, HC 2000 HDHP – HS 2800 5

Maximum Out-of-Pocket The below applies to plans with an aggregate deductible: • Out-of-pocket costs for all eligible, in-network services — including deductible and co-insurance — count toward the individual/family maximum. Maximum out-of-pocket limits vary by plan. Maximum limit • Once the individual/family reaches the MOOP limit, Guide. Stone covers all eligible, in-network health care expenses for the rest of the year. • The remaining amount of the family maximum out-of-pocket limit can be accumulated by one or all of the family members. • New Prescription Over the Counter fee does not apply. Note: Out-of-network expenses accumulate separately and do not contribute to the maximum out-of-pocket limit. Prescription drug Emergency room Urgent care Office visit Co-insurance Deductible 6

Wellness Benefit • Scheduled, in-network services are covered at 100% including scheduled lab and x-ray. • Well-child and adult annual preventive care both covered. • Immunizations covered for all ages according to schedule and available at doctor’s office and neighborhood pharmacy. • Recommendations are based on age and gender. • Services not listed on the Preventive Care Schedule such as EKGs and lung X-rays are not included in the 100% preventive exam. ◦ These services are included as diagnostic under deductible/ co-insurance benefits. • New wellness resources on Landing Pages. 7

Vision Exam Benefit • One annual eye health examination for each participant, including: ◦ Dilation ◦ Refraction for eyeglasses or contact lens prescription • Available at the Primary Care office visit level on PPO plans and applies towards deductible on HDHP plans. • No coverage for glasses, contacts or other eyewear. • Must use a BCBS in-network optical provider (optometrist or ophthalmologist) to receive benefit. 8
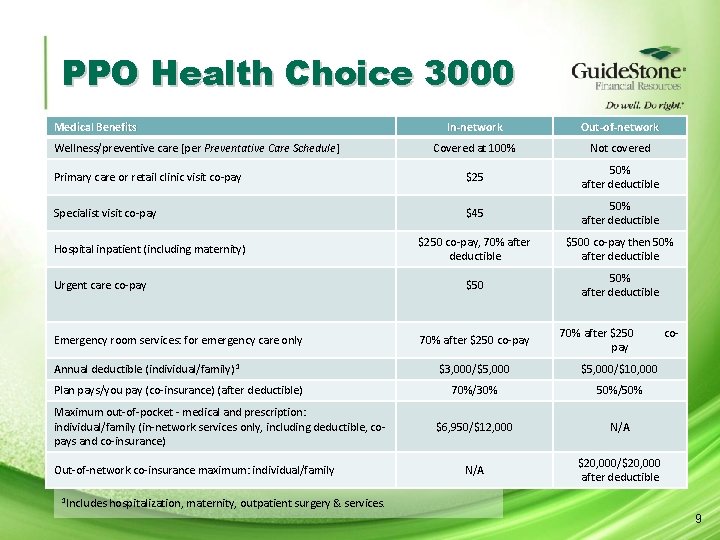
PPO Health Choice 3000 Medical Benefits In-network Out-of-network Covered at 100% Not covered Primary care or retail clinic visit co-pay $25 50% after deductible Specialist visit co-pay $45 50% after deductible $250 co-pay, 70% after deductible $500 co-pay then 50% after deductible $50 50% after deductible Wellness/preventive care [per Preventative Care Schedule] Hospital inpatient (including maternity) Urgent care co-pay Emergency room services: for emergency care only Annual deductible (individual/family) 1 Plan pays/you pay (co-insurance) (after deductible) Maximum out-of-pocket - medical and prescription: individual/family (in-network services only, including deductible, copays and co-insurance) Out-of-network co-insurance maximum: individual/family 1 Includes 70% after $250 co-pay 70% after $250 pay $3, 000/$5, 000/$10, 000 70%/30% 50%/50% $6, 950/$12, 000 N/A $20, 000/$20, 000 after deductible co- hospitalization, maternity, outpatient surgery & services. 9
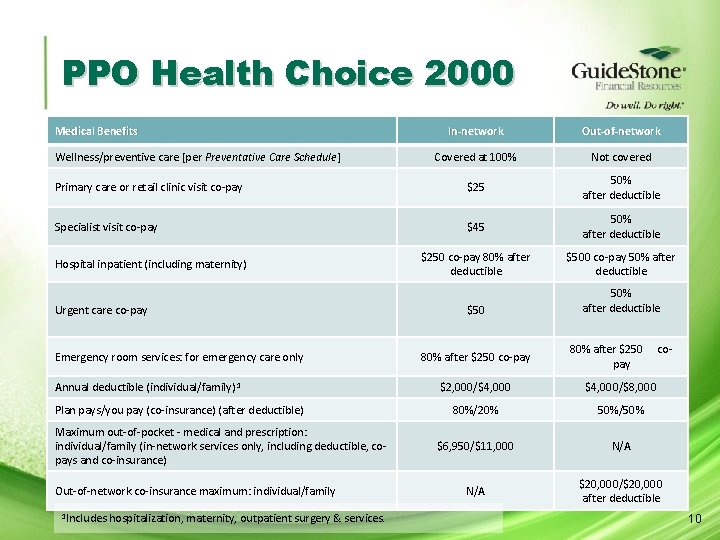
PPO Health Choice 2000 Medical Benefits In-network Out-of-network Covered at 100% Not covered Primary care or retail clinic visit co-pay $25 50% after deductible Specialist visit co-pay $45 50% after deductible $250 co-pay 80% after deductible $500 co-pay 50% after deductible $50 50% after deductible Wellness/preventive care [per Preventative Care Schedule] Hospital inpatient (including maternity) Urgent care co-pay Emergency room services: for emergency care only Annual deductible (individual/family) 1 Plan pays/you pay (co-insurance) (after deductible) Maximum out-of-pocket - medical and prescription: individual/family (in-network services only, including deductible, copays and co-insurance) Out-of-network co-insurance maximum: individual/family 1 Includes hospitalization, maternity, outpatient surgery & services. 80% after $250 co-pay 80% after $250 pay co- $2, 000/$4, 000/$8, 000 80%/20% 50%/50% $6, 950/$11, 000 N/A $20, 000/$20, 000 after deductible 10

Embedded Deductible PPO Plans • When one person in a family reaches the individual deductible level, that person moves to the coinsurance benefit level. • Other family members’ expenses accrue to meet the remaining family deductible before they move to the coinsurance benefit level. • Deductible, co-insurance and copayments accrue to meet the individual and family Maximum Out-of. Pocket. 11

Lab and X-ray Benefits PPO Plans Diagnostic X-ray or lab work at a doctor’s office • Office visit benefit applies when an in-network doctor performs lab work or X-ray in his or her office regardless of where the doctor has the lab work or X-ray processed or read Free-standing diagnostic X-ray or lab facility • You pay your deductible and co-insurance when you receive a diagnostic X-ray or lab work at a free-standing facility outside your physician's office. • This facility may be adjacent to or within the same suite as your doctor’s office. 12

Prescription Benefits PPO Plans Retail: 30 -day supply Mail Order: 90 -day supply Generic drug co-pay $15 $30 Preferred drug co-pay $50 $100 Non-preferred drug co-pay $75 $150 Prescription Benefits Retail available as 30 -day supply, mail order as 90 -day supply and specialty as 30 -day supply through mail order. If the cost of the prescription is less than the co-pay, the participant will pay the full cost of the prescription. Retail co-pays increase $10 after the second retail fill of maintenance drugs. The co-pay increase does not accumulate toward the deductible or the maximum out-of-pocket limit. If a non-generic drug is purchased when a generic is available, the participant must pay the generic co-pay plus the increase in drug cost of the non-generic drug over its generic equivalent. The increase in drug cost does not accumulate toward the deductible or the maximum out-of-pocket limit. 13

Prescription Benefits – Specialty Prescription Drugs PPO Plans Prescription Benefits 30 -day supply Specialty generic drug co-pay $50 Specialty preferred drug co-pay $75 Specialty non-preferred drug co-pay $100 14

Prescription Benefits PPO Plans Effective January 1, 2018 • You can fill your maintenance medications twice at the regular co-pay at a retail pharmacy. • Starting with your third fill at a retail pharmacy, there will be a $10 retail co-pay increase for many maintenance prescriptions. • Prescriptions filled via the online pharmacy will not be subject to the increased co-pay. • Your co-pay for retail and online will never be more than the cost of the drug. 15

HC 3000 Traditional PPO Plans Prescription Benefits • If a preferred or non-preferred drug is purchased when a generic drug is available, the cost difference will not apply toward the participant’s deductible or maximum out-of-pocket limit. After the deductible is met, the participant must pay the cost difference between the preferred/non-preferred drug and its generic drug equivalent, if available. If the cost of the prescription is less than the co-pay, the participant will pay the full cost of the prescription. 16

Flexible Spending Accounts – FSAs Benefits: Reduce taxable income! Cash available for unreimbursed medical expenses – up-front loan to yourself Requirements: Elections remain in effect for plan year (unless you have a qualified status change) “Use it or Lose it” requirement $500 carry over limit 2018 Maximum amount you can designate: $2, 600 17
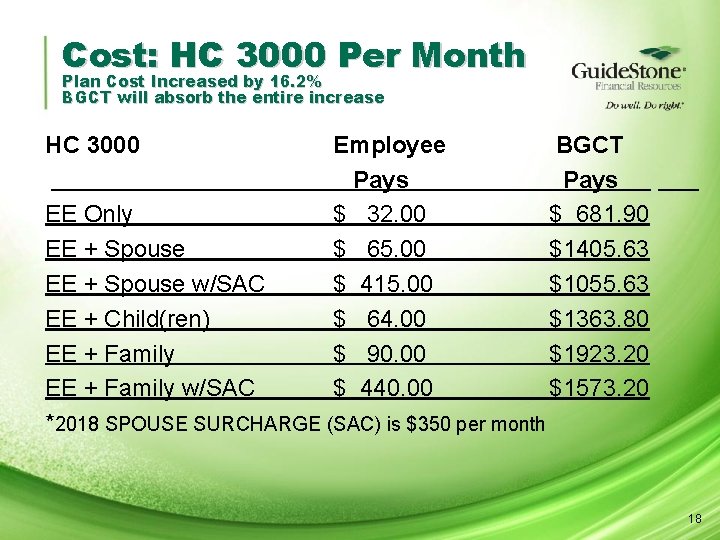
Cost: HC 3000 Per Month Plan Cost Increased by 16. 2% BGCT will absorb the entire increase HC 3000 Employee BGCT Pays. EE Only $ 32. 00 $ 681. 90 EE + Spouse $ 65. 00 $1405. 63 EE + Spouse w/SAC $ 415. 00 $1055. 63 EE + Child(ren) $ 64. 00 $1363. 80 EE + Family $ 90. 00 $1923. 20 EE + Family w/SAC $ 440. 00 $1573. 20 *2018 SPOUSE SURCHARGE (SAC) is $350 per month 18
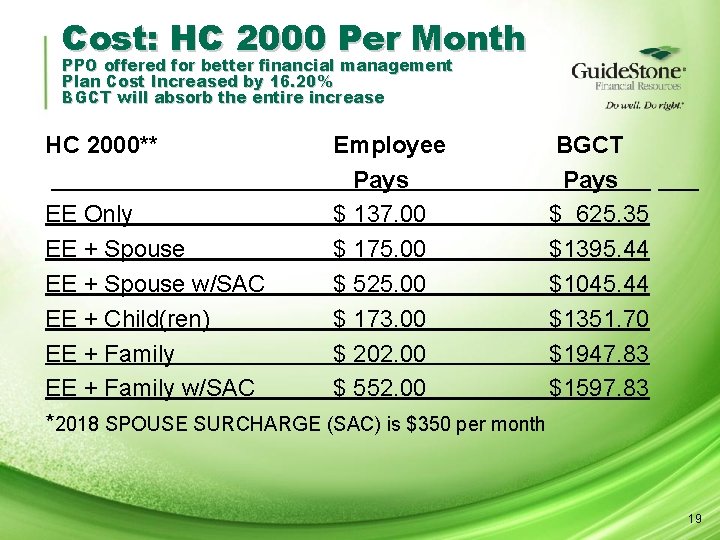
Cost: HC 2000 Per Month PPO offered for better financial management Plan Cost Increased by 16. 20% BGCT will absorb the entire increase HC 2000** Employee BGCT Pays. EE Only $ 137. 00 $ 625. 35 EE + Spouse $ 175. 00 $1395. 44 EE + Spouse w/SAC $ 525. 00 $1045. 44 EE + Child(ren) $ 173. 00 $1351. 70 EE + Family $ 202. 00 $1947. 83 EE + Family w/SAC $ 552. 00 $1597. 83 *2018 SPOUSE SURCHARGE (SAC) is $350 per month 19

What is a federallyqualified HDHP? • Medical plan design defined by federal government • No first dollar medical coverage with the exception of preventive services covered at 100% • Designed to be paired with a Health Savings Account (HSA) • Participants must pay out of pocket for all medical and RX services until they meet the deductible • After meeting the deductible, eligible medical or prescription drug claims are paid according to the plan by Guide. Stone. 20

HDHP Health Saver 2800 1 This plan is an HSA-qualified High Deductible Health Plan (HDHP) with a combined medical and prescription deductible. 2 For family coverage, one individual cannot be responsible for more than the 2018 ACA limit of $7, 350. 21
![Health Saver 2800 Medical Benefits In-network Out-of-network Wellness/preventive care [per Preventative Care Schedule] 100% Health Saver 2800 Medical Benefits In-network Out-of-network Wellness/preventive care [per Preventative Care Schedule] 100%](http://slidetodoc.com/presentation_image/33b44812ef2099fbade9d34ff66a14ba/image-22.jpg)
Health Saver 2800 Medical Benefits In-network Out-of-network Wellness/preventive care [per Preventative Care Schedule] 100% no deductible Not covered Primary care visit 80% after deductible 50% after deductible Specialist visit 80% after deductible 50% after deductible $250 after deductible then 80% $500 after deductible then 50% Urgent care visit 80% after deductible 50% after deductible Emergency room services: for emergency care only 80% after 250 copay 80% $250 copay $2, 800/$5, 600/$11, 200 80%/20% 50%/50% $5, 800/$11, 600 N/A $20, 000/$24, 000 Hospital Inpatient Annual deductible: individual/family Plan pays/individual pays (after deductible) Maximum out-of-pocket - medical and prescription: individual/family (in-network services only, including deductible and co-insurance) Annual co-insurance maximum: individual/family 1 This plan is an HSA-qualified High Deductible Health Plan (HDHP) with a combined medical and prescription deductible. 2 For family coverage, one individual cannot be responsible for more than the 2018 ACA limit of $7, 350. 22

Aggregate Deductible HDHP Plan Health Saver 2800 • If you have individual coverage and you meet the individual deductible, you move into the coinsurance benefit level of 80%. • If you have family coverage, there is no individual deductible. 1 ◦ All family medical costs count toward the family deductible. ◦ When the family deductible is met by one or a combination of family members, the entire family moves to the coinsurance benefit level of 80%. • Deductible and co-insurance accrue to meet the individual and family Maximum Out-of-Pocket. 1 For family coverage, one individual cannot be responsible for more than the 2018 IRS limit of $7, 350. 23
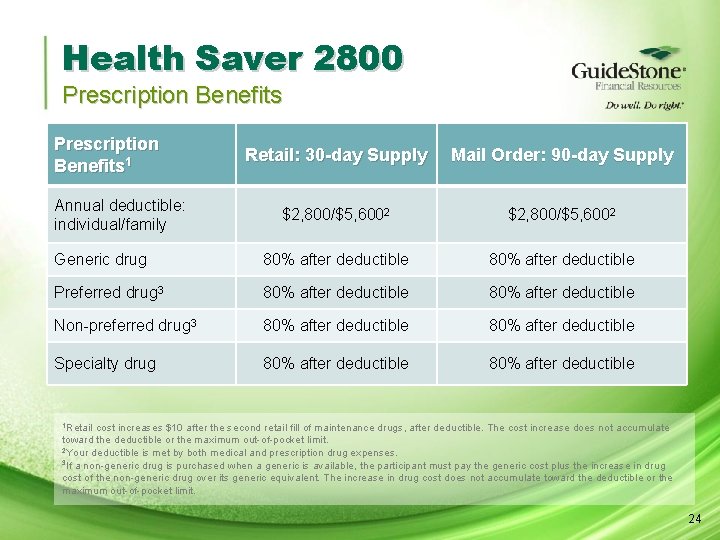

Health Saver 2800 Prescription Benefits 1 Retail: 30 -day Supply Mail Order: 90 -day Supply $2, 800/$5, 6002 Generic drug 80% after deductible Preferred drug 3 80% after deductible Non-preferred drug 3 80% after deductible Specialty drug 80% after deductible Annual deductible: individual/family 1 Retail cost increases $10 after the second retail fill of maintenance drugs, after deductible. The cost increase does not accumulate toward the deductible or the maximum out-of-pocket limit. 2 Your deductible is met by both medical and prescription drug expenses. 3 If a non-generic drug is purchased when a generic is available, the participant must pay the generic cost plus the increase in drug cost of the non-generic drug over its generic equivalent. The increase in drug cost does not accumulate toward the deductible or the maximum out-of-pocket limit. 24

Health Saver 2800 Prescription Benefits • Combined medical and prescription drug deductible • If a preferred or non-preferred drug is purchased when a generic is available, the cost difference will not apply toward the participant’s deductible or maximum out-of-pocket limit. After the deductible is met, the participant must pay the cost difference between the preferred/non-preferred drug and its generic equivalent, if available. 25
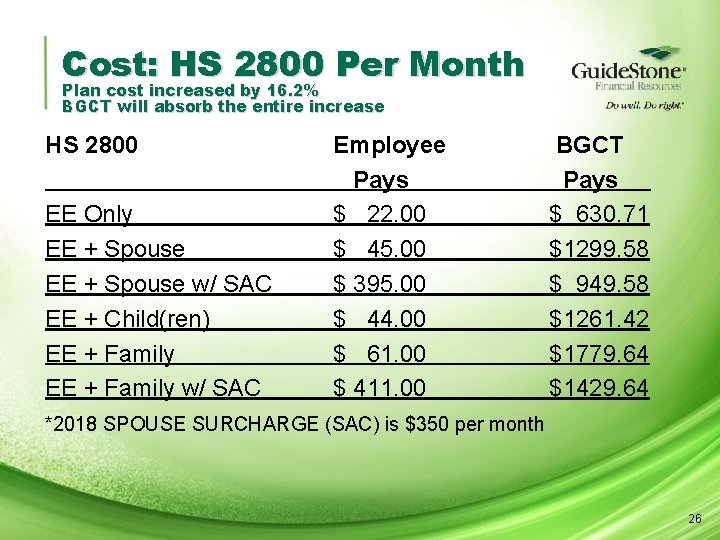
Cost: HS 2800 Per Month Plan cost increased by 16. 2% BGCT will absorb the entire increase HS 2800 EE Only EE + Spouse w/ SAC EE + Child(ren) EE + Family w/ SAC Employee Pays $ 22. 00 $ 45. 00 $ 395. 00 $ 44. 00 $ 61. 00 $ 411. 00 BGCT Pays. $ 630. 71 $1299. 58 $ 949. 58 $1261. 42 $1779. 64 $1429. 64 *2018 SPOUSE SURCHARGE (SAC) is $350 per month 26

How can this plan save me money? • Lowers your monthly cost of coverage (premium) • Has high co-insurance levels after you meet your deductible. Our HS 2800 is a 80/20 plan. • Gives you greater visibility into your actual health care costs, helping you be a smarter health care consumer. • Allows you to contribute to a tax-advantaged HSA and receive the BGCT contributions 27

Health Savings Account (HSA) 28

What is a Health Savings Account (HSA)? • Individually owned savings account where HSA funds roll over and can be saved for future medical or Medicare expenses — no “use it or lose it” rule • HSA has triple tax advantage: ◦ Employee contributions to HSA are tax free ◦ Disbursements for eligible medical expenses are non-tax ◦ Dividends on the HSA investment are taxdeferred • It’s your money — and it moves with you if you change employers 29

HSA Eligibility & Contributions Eligible • A person enrolled in a QHDHP Not Eligible • Covered by any other health plan, including your spouse’s health insurance. • Covered by your own or spouse’s Flexible Spending Account (FSA). • Enrolled in any part of Medicare or Tricare. • Received Veteran’s health benefits in the past 90 days. • Claimed as a dependent on another person’s tax return Contributions Individual $3, 450 Family $6, 900 30

HSA Contribution Rules • Employees age 55 and older can make “catch-up” contributions of $1, 000 per year • IRA funds may be used to open an HSA one time only • If you enroll in a HDHP mid-year, you may contribute up to full annual maximums • Note: If you terminate your HDHP coverage mid-year, eligible HSA contributions are based on number of months enrolled (prorated) 31
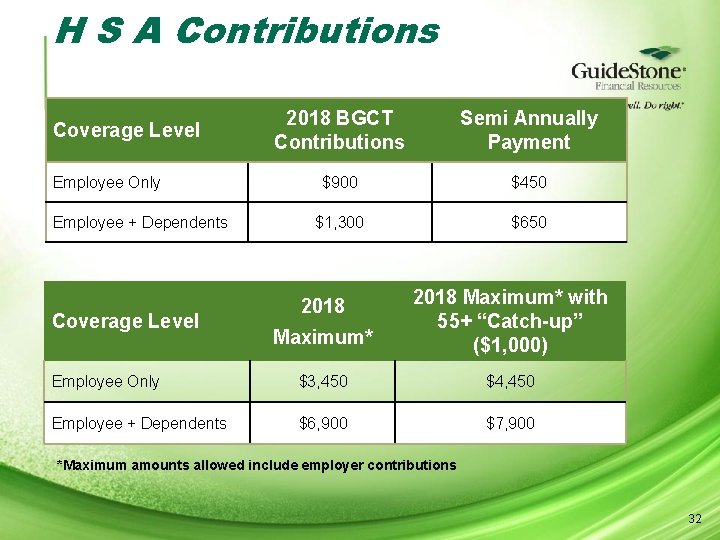

H S A Contributions Coverage Level Employee Only Employee + Dependents Coverage Level 2018 BGCT Contributions Semi Annually Payment $900 $450 $1, 300 $650 2018 Maximum* with 55+ “Catch-up” ($1, 000) Employee Only $3, 450 $4, 450 Employee + Dependents $6, 900 $7, 900 *Maximum amounts allowed include employer contributions 32

How do I use my HSA Dollars? • HSA disbursements can be used tax-free for qualified medical expenses: ◦ Section 213(d) items are reimbursable ◦ Over-the-counter drugs are eligible for reimbursement only with a prescription. • HSA disbursements can be used for your medical expense and your dependents’ medical expenses even if they are not covered under your plan 33

Limited Flexible Spending Accounts – LSAs If you are enrolled in the HS 2800 and desire to have a flexible spending account, your Flex account is limited to Dental and Vision Expenses until the deductible is reached. The same benefits and requirement apply to the LSA as with the FSA. 2018 Maximum amount you can designate: $2, 600 34

HSA Reimbursement Penalty • Two penalties apply to non-eligible Section 213(d) HSA reimbursement: ◦ 20% penalty on the amount withdrawn ◦ Income tax penalty at your income tax bracket on the amount withdrawn for non-eligible reimbursement. • You are responsible to keep receipts to substantiate all withdrawals were for eligible 213(d) expenses. 35

Teladoc’s U. S. board-certified doctors are available 24/7/365 to resolve many of your medical issues through phone or video consults. Set up your account today so when you need care now, a Teladoc doctor is just a call or click away. 1 -800 -TELADOC Remember: When asked for your group name say – Baptist General Convention of Texas to avoid any fees! 36

Dental Plans 37
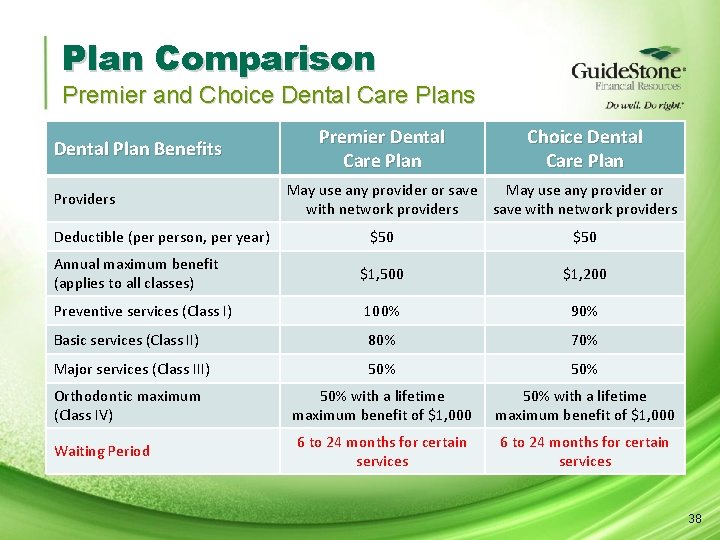
Plan Comparison Premier and Choice Dental Care Plans Dental Plan Benefits Providers Deductible (per person, per year) Premier Dental Care Plan Choice Dental Care Plan May use any provider or save May use any provider or with network providers save with network providers $50 Annual maximum benefit (applies to all classes) $1, 500 $1, 200 Preventive services (Class I) 100% 90% Basic services (Class II) 80% 70% Major services (Class III) 50% Orthodontic maximum (Class IV) 50% with a lifetime maximum benefit of $1, 000 6 to 24 months for certain services Waiting Period 38

Choosing a Provider Premier and Choice Dental Plans • You may use any provider • There are two tiers of network coverage: ◦ In-network Receive deepest discounts § Provider files claims § No balance billing ◦ Out-of-network § No discounts — charged the maximum reimbursable charge § Responsible for filing claims § Provider may balance bill § 39
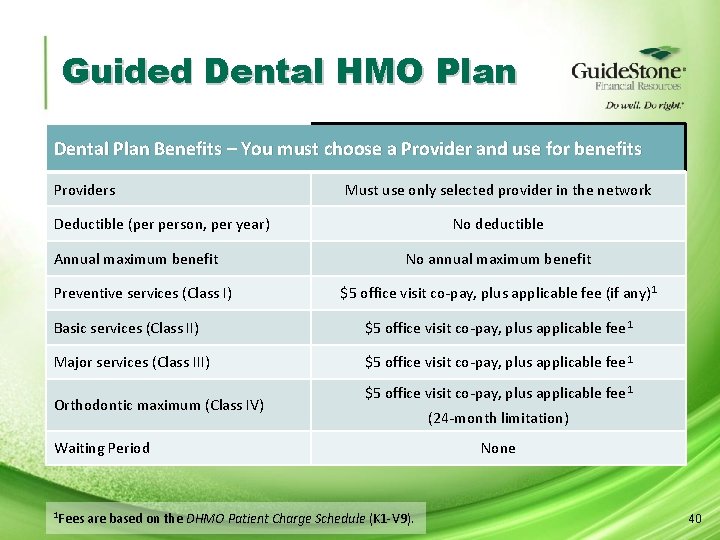

Guided Dental HMO Plan Dental Plan Benefits – You must choose a Provider and use for benefits Providers Must use only selected provider in the network Deductible (per person, per year) Annual maximum benefit Preventive services (Class I) No deductible No annual maximum benefit $5 office visit co-pay, plus applicable fee (if any)1 Basic services (Class II) $5 office visit co-pay, plus applicable fee 1 Major services (Class III) $5 office visit co-pay, plus applicable fee 1 Orthodontic maximum (Class IV) $5 office visit co-pay, plus applicable fee 1 Waiting Period 1 Fees are based on the DHMO Patient Charge Schedule (K 1 -V 9). (24 -month limitation) None 40

How is the Guided Dental HMO different? • You must choose a primary dentist or facility • You must use the plan dentists and specialists to receive benefits • Charges for services are based on a fee schedule • For an electronic version of this Patient Charge Schedule, visit www. Guide. Stone. Insurance. org 41
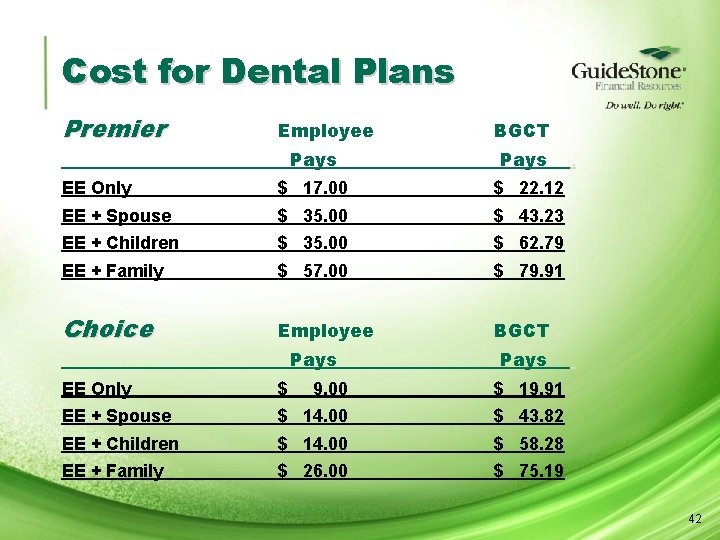
Cost for Dental Plans Premier Employee Pays BGCT Pays EE Only $ 17. 00 $ 22. 12 EE + Spouse $ 35. 00 $ 43. 23 EE + Children $ 35. 00 $ 62. 79 EE + Family $ 57. 00 $ 79. 91 Choice Employee BGCT Pays EE Only $ 9. 00 $ 19. 91 EE + Spouse $ 14. 00 $ 43. 82 EE + Children $ 14. 00 $ 58. 28 EE + Family $ 26. 00 $ 75. 19 . . 42
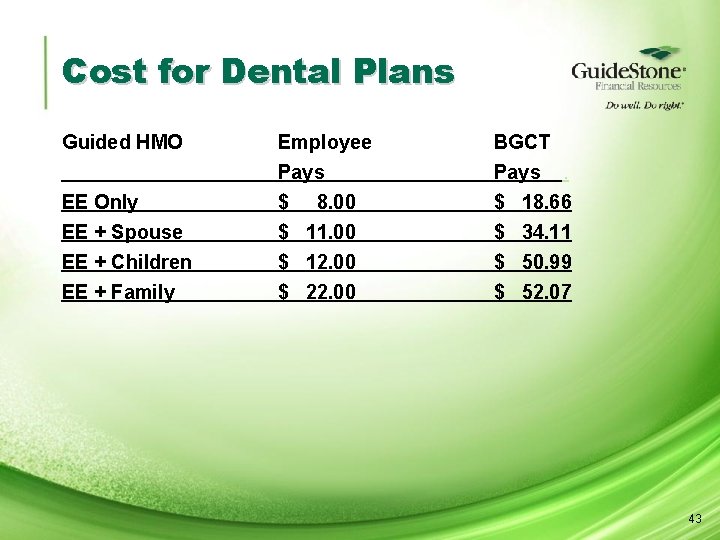
Cost for Dental Plans Guided HMO Employee Pays BGCT Pays. EE Only EE + Spouse EE + Children EE + Family $ 8. 00 $ 11. 00 $ 12. 00 $ 22. 00 $ $ 18. 66 34. 11 50. 99 52. 07 43

Term Life Plans 44

Life, LTD and ESADD No change to the percentages used to make calculations. If you turned 65 in 2017, you will see a difference in your Life insurance and SADD. HR will send you an email on reduced amounts. If you will turn 65 in 2018, your amounts will not reduce until January 2019. 45

Employee Term Life Employer-provided Coverage • Voluntary Employee Life: 4 X Salary • Voluntary optional life available with underwriting • Coverage amount in increments of one to four times annual salary • Maximum coverage of $750, 000 • Reduction at age 65 of 35%; further reduction at retirement to $20, 000 maximum 46

Employee Term Life Employer-provided Coverage Example: • Employee has $120, 000 Voluntary Employee Life (4 X Salary) • Premium for coverage is $33. 60 • BGCT pays 80% or $26. 88 • You pay 20% or $3. 36 per pay period 47

Spouse Term Life Employer-provided Coverage • Voluntary Basic term life: $25, 000 • Optional life available with underwriting • Total basic and optional life up to 50% of employee coverage • Maximum coverage level is $250, 000 • Employee death — life coverage may continue for dependents 48

Spouse Term Life Employer-provided Coverage Example: • Employee chooses Voluntary Basic $25, 000 Spouse Life coverage • Premium for coverage is $7. 00 • BGCT pays 80% or $5. 60 • You pay 20% or $0. 70 per pay period 49

Child Term Life Plan • • Voluntary $10, 000 coverage $0. 75 per month covers all eligible children Employee death — life coverage may continue for dependents (if employer so elects) 50

Child Term Life Plan Example: • Employee chooses Child Life $10, 000 coverage for all eligible children • Premium is $0. 75 • BGCT pays 80% or $0. 59 • You pay $0. 08 per pay period 51

Additional Benefits Term Life Plans • • Life Planning Financial & Legal Resources assist america® Accelerated benefit Portability or conversion of coverage 52

Accident Plans 53

Supplemental Accident Insurance Employer-provided Coverage • Voluntary Coverage for employee: $250, 000 • Voluntary Coverage for spouse: $125, 000 • Pays you or your beneficiary if you die or suffer a specified loss (eyesight, hand or foot, hearing, or speech) in an accident • Underwriting is not required • Participation in Employee Term Life Plan is not required 54

Supplemental Accident Insurance Employer-provided Coverage Example: • Employee chooses maximum Employee Voluntary Coverage of $250, 000 and spouse coverage at ½ that volume • Premium is $6. 25 ESADD and $3. 13 SSADD • BGCT pays 80% or $5. 00 for employee and $2. 50 for spouse • You pay $0. 63 per pay period for self, and $0. 31 for spouse 55

Disability Plans 56
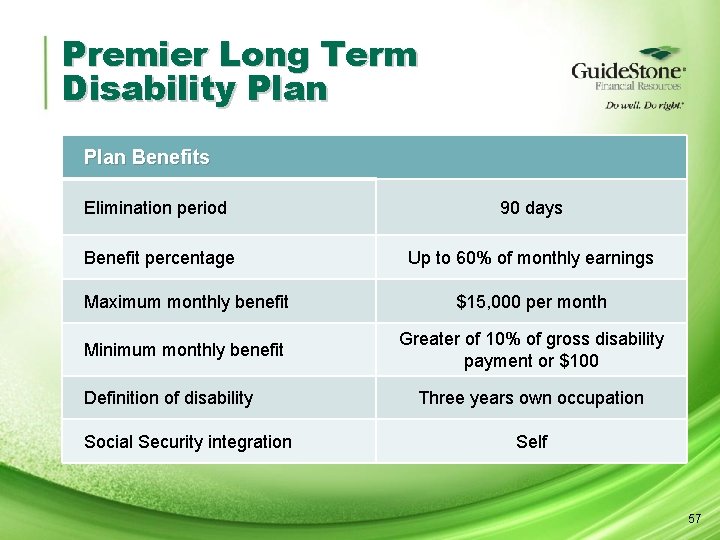

Premier Long Term Disability Plan Benefits Elimination period 90 days Benefit percentage Up to 60% of monthly earnings Maximum monthly benefit $15, 000 per month Minimum monthly benefit Greater of 10% of gross disability payment or $100 Definition of disability Social Security integration Three years own occupation Self 57

Additional Benefits Disability Plans • • Life Planning Financial & Legal Resources Survivor benefits Rehabilitation and Return to Work Program Loss schedule for full or partial losses 58

Vision Plan Vision Benefits Premier 1 Plan Examinations No charge for eye examination and most standard services No charge for contact lens evaluation, including fitting and followup 50, 000 provider locations nationwide Eyeglasses Choose frames for $25 from the Davis Visionworks collection or any frames using the generous frame allowance. Breakage warranty for repair or replacement for one year from the date of delivery. 59
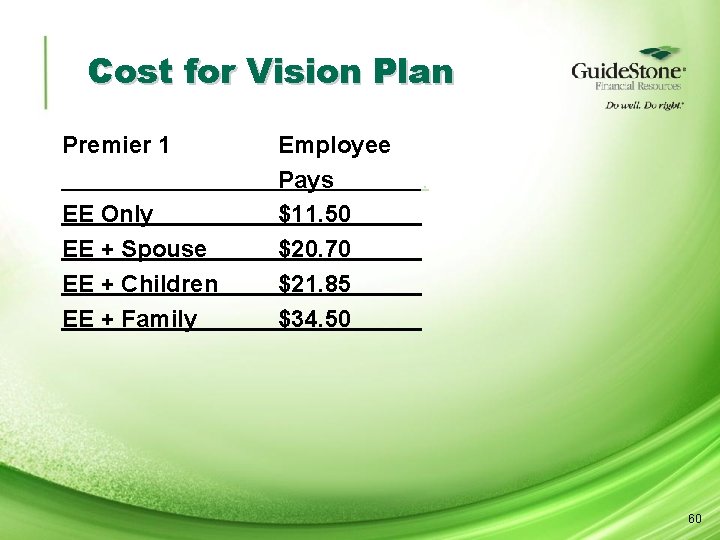

Cost for Vision Plan Premier 1 EE Only EE + Spouse EE + Children EE + Family Employee Pays $11. 50 $20. 70 $21. 85 $34. 50 . 60

Tools and Resources for Your Family 61

Guide. Stone Additional Benefits Highmark BCBS • My. Care Navigator (1 -888 -blue-428) Find the right doctor, schedule appointments and much more • Care Cost Estimator Comparison shop- more than 1, 600 common health services. See your Highmark BCBS account for details. • • • Blue 365 Discount program All Clear ID (1 -855 -229 -0079) for members victim to identity theft Vitals. Smartshopper- Get paid to shop for Health Care Cigna Dental • • Cigna Healthy Rewards Discount program Oral Health Integration Program (OHIP) Enhanced benefits. Go to Cigna account for details. 62

Blue 365® Highmark Blue Cross Blue Shield • Discounts on services and products plus valuable information you can use all year long • To access these discounts: ◦ Visit www. Highmark. BCBS. com ◦ Choose the Members tab and log in, or select “Register Now” ◦ Select the Your Coverage tab and go to “Member Discounts” • Highlight of available discounts : 63

My. Guide. Stone. org 1. Establish log-in on vendor websites ◦ www. Highmark. BCBS. com ◦ www. Express-Scripts. com ◦ www. my. Cigna. com 2. Go to www. Guide. Stone. org and establish log-in 3. Then sign in once at Guide. Stone and you’re done! Single point of access to everything you need: ◦ ◦ Review your insurance product details Download detailed plan booklets Find a provider Access wellness support and information 64

Vitals. Smartshopper Shop for quality lower cost health care to earn cash rewards from $25 to $500 and lower out of pocket cost 3 Simple Steps to use vitalssmartshopper 1. Shop for Care- Call 1 -866 -285 -7475 or access Vitals through HM BCBS member portal for the best price. 2. Complete the procedure at the location of your choice 3. Earn cash rewards- Smartshopper verifies the procedure and mails a reward check 65

Vitalssmartshopper Here are some examples of cash rewards* you can earn. Procedure MRI CT Scan Colonoscopy Mammogram Your Reward* Up to $100 Up to $150 Up to $ 50 • Call 1 -866 -285 -7475 • Access Vitals Smart. Shopper through the link on the Highmark Blue Cross Blue Shield member portal *Reward payments may be taxable 66

BGCT Landing Page • All benefits available here • Tools to make right choices • Wellness support to help you and your family improve health and reduce health care costs • Go to Guide. Stone. org/BGCT • Design Your Own Benefits Landing Page Password: Enroll. BCGT 2018 67

2018 Forms Required: 2018 Flex Enrollment Form 2018 H S A Contribution Form 2018 Spousal Certification Form *Employee Annual Change Request Form – **if plan changes made** *Waiver of Coverage Form Complete the Enrollment form via Google Docs. The Enrollment form will be emailed to each eligible employee * The Employee Annual Change Request form and the Waiver of Coverage form are also available on the BGCT Landing Page (Employee Benefits/Design Your Own Benefits/Next Steps) 68

DEADLINES 1 st Drawing for TWO $100 gift cards on November 3 rd 2 nd Drawing for TWO $25 gift cards on November 8 th All Forms are due by NOVEMBER 10, 2018. 69

This information only highlights the depth of coverage and benefits you can receive when you protect yourself with Guide. Stone Financial Resources. Limitations and exclusions apply. This material is a general summary of the plans. The official plan documents and contracts set forth the eligibility rules, limitations, exclusions and benefits. These alone govern and control the actual operation of the plan. In the event of a conflict with the description in this material, the terms of the official plan documents and contracts will control its operation. Guide. Stone Financial Resources of the Southern Baptist Convention reserves the right to change or cancel these programs at any time. This material does not imply an employment contract or guarantee of benefits. Medical underwriting could be required.
- Slides: 70