Concussion Management Current Concepts and Clinical Guidelines Brian

Concussion Management: Current Concepts and Clinical Guidelines Brian P Rieger, Ph. D Chief Psychologist & Clinical Assistant Professor Department of Physical Medicine & Rehabilitation University. Hospital SUNY Upstate Medical University Director, CNY Sports Concussion Center NYSPHSAA Concussion Team & Safety Committee NYS TBI Coordinating Council Public Education Committee February 2009

What is a concussion? n n Mild traumatic brain injury A disruption in normal brain function due to a blow or jolt to the head CT or MRI is almost always normal Invisible injury

Definition of Concussion American Congress of Rehabilitation Medicine n Blow or jolt to the head AND n Loss of consciousness (≤ 30 min) OR n Post-traumatic amnesia (≤ 24 hrs) OR n Neurological finding OR n n Alteration in mental state n n Slurred speech, diplopia, etc. Dazed or disoriented or confused After 30 minutes, an initial GCS of 13 -15

Outdated AAN Criteria for Sports-related Concussion Grade 1 Transient Confusion Symptoms resolve in <15 minutes No LOC Grade 2 Transient Confusion Symptoms last >15 minutes No LOC Grade 3 LOC: a) brief b) prolonged

Prague 2004 Guidelines (Mc. Crory et al. , 2004) § Simple concussion ü LOC < 1 minute ü resolves in 7 -10 days ü first concussion § Complex concussion ü LOC > 1 minute ü symptoms last longer than 7 – 10 days ü history of multiple concussions IOC • IIHF • FIFA

Prague 2004 Guidelines § No return to play in current game or practice § Return to play only when symptom free at rest and with exertion § Graduated return to play with exertional challenge § Recognition of differences in children § Neurocognitive testing recommended Manage each concussion individually

Epidemiology n n 1. 6 to 3. 8 million sports concussions each year in the United States Football, hockey, and soccer are the riskiest male team sports Up to 10% of high school football players suffer a concussion each year Soccer and lacrosse are the riskiest female team sports

Epidemiology n n In HS sports played by both sexes, girls have a higher rate of concussion Collegiate athletes have a higher rate of concussion than HS athletes Concussion represents a higher proportion of all injuries in HS athletes vs. collegiate Approximately 10% of sports concussions involve LOC

Multiple Concussions What are the risks ? § Second Impact Syndrome § § § A second concussion within 2 weeks of first Athlete is still symptomatic Mostly males < 21 years old Rapid increase in intracranial pressure Rare but almost always fatal § Possible cumulative effects § § § Increasing concussability Prolonged or incomplete recovery Increased risk of later depression or dementia How many is too many ?

Mechanisms of Injury n A complex physiological process induced by traumatic biomechanical forces Øsudden chemical changes Øtraumatic axonal injury § Structural brain imaging (CT or MRI) is almost always normal

Neurometabolic Cascade (Giza and Hovda 2001) n n n Abrupt neuronal depolarization Release of excitatory neurotransmitters Changes in glucose metabolism Altered cerebral blood flow The brain goes into an ENERGY CRISIS that usually last up to 7 – 10 days symptoms often get worse before they get better
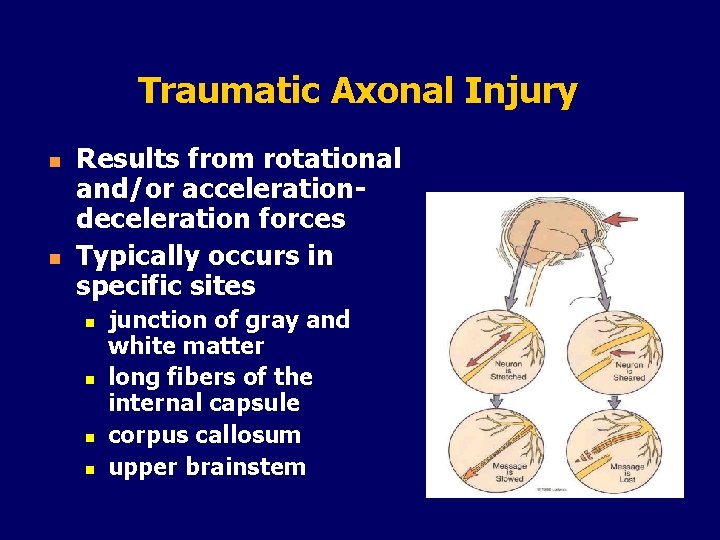
Traumatic Axonal Injury n n Results from rotational and/or accelerationdeceleration forces Typically occurs in specific sites n n junction of gray and white matter long fibers of the internal capsule corpus callosum upper brainstem

Common Physical Symptoms § Headache § Nausea and vomiting § Clumsiness and poor balance § Dizziness and lightheadedness § Blurred vision and light sensitivity § Fatigue and lack of energy § Sleep disturbance

Common Emotional Symptoms § Irritability § Anxiety § § § More extreme moods Easily overwhelmed Emotional and behavioral outbursts Personality change Lack of motivation

Common Cognitive Symptoms § § § § Feeling ‘dazed’ or ‘foggy’ or ‘fuzzy’ Easily confused Slowed processing Easily distracted Memory problems Trouble reading Poor mental stamina

Exertion effects § Symptoms are worsened by. . . ü mental effort ü environmental stimulation ü emotional stress ü physical activity

9 mos. after injury 6 mos. after injury Chen et al. (2004)

Recovery from Concussion § Full recovery in 7 -10 days. . . in most cases § About 95% recover in 3 months § Symptoms generally thought to have a primarily neurological basis at first § When symptoms persist, non-injury factors appear to play an increasingly significant role over time a ‘miserable minority’ experience complicated recovery
§ Outcome after concussion is difficult to predict § Early markers weakly related to recovery ü LOC ü GCS score ü PTA
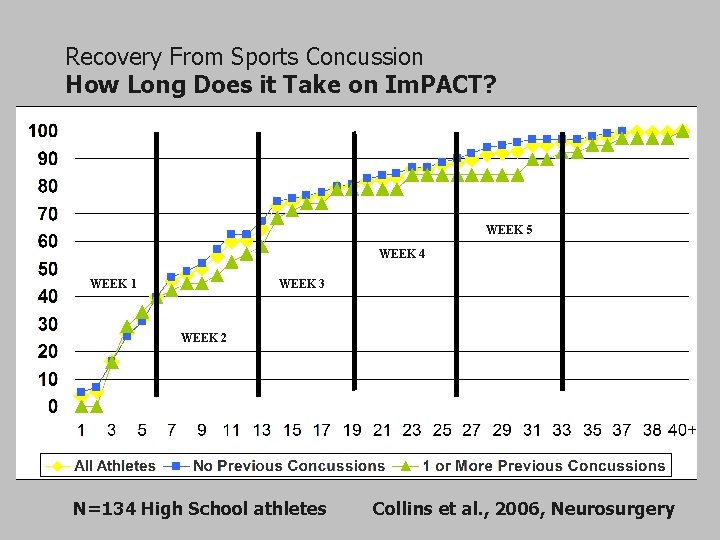
Recovery From Sports Concussion How Long Does it Take on Im. PACT? WEEK 5 WEEK 4 WEEK 1 WEEK 3 WEEK 2 N=134 High School athletes Collins et al. , 2006, Neurosurgery

Sideline Evaluation n n Head trauma (blow or jolt) LOC or amnesia for the trauma Focal neurologic finding Signs & Symptoms (SCAT card) n n Assess cognition n n 3 word recall Months backwards Standardized testing n n confused, wobbly, emotional. . . SAC BESS NO RETURN TO PLAY THAT DAY When in doubt—sit ‘em out

Prague Return to Play Guidelines Prague 2004 guidelines recommend that when a player shows ANY symptoms or signs of a concussion: § athlete should not return-to-play in the current game or practice § Athlete should be monitored for deterioration for 24 hours § return-to-play must follow a medically supervised stepwise process § athlete must be symptom-free at rest and after exertion

Prague Return to Play Progression 1. No activity, complete rest 2. Light aerobic exercise but no resistance training 3. Sport specific exercise and progressive addition of resistance training 4. Non-contact training drills 5. Full contact training and scrimmage after medical clearance 6. Game play Also should be symptom-free after mental exertion and have normal neruocognitive test results

Medical Protocol § Any athlete who suffers a concussion needs medical clearance before RTP § Anyone with a LOC should be evaluated that day § If confused or not fully conscious, transport by EMS with immobilization § Follow athlete until asymptomatic § First medical clearance is to begin RTP progression § If no return of symptoms with exertion, then final clearance for game play

It takes a team. . . § Athlete and parents § Athletic Trainer § Coaches and Athletic Director § Physician, school physician, and school nurse § Psychologist § Teachers and school administrators

Managing Complex Concussion § Consider referral to specialized provider or program if. . . § History of multiple concussions or other risk factors § Prolonged recovery (> 2 weeks) § Worsening symptoms

Neuropsychological Testing In Sports Concussion § Computerized tests that measure attention, memory, and processing speed (reaction time) § Sensitive to effects of concussion § Tests can be repeated multiple times to monitor recovery § Ideally, pre-injury baseline testing done for all athletes § Im. PACT, Cog. Sport, Head. Minder
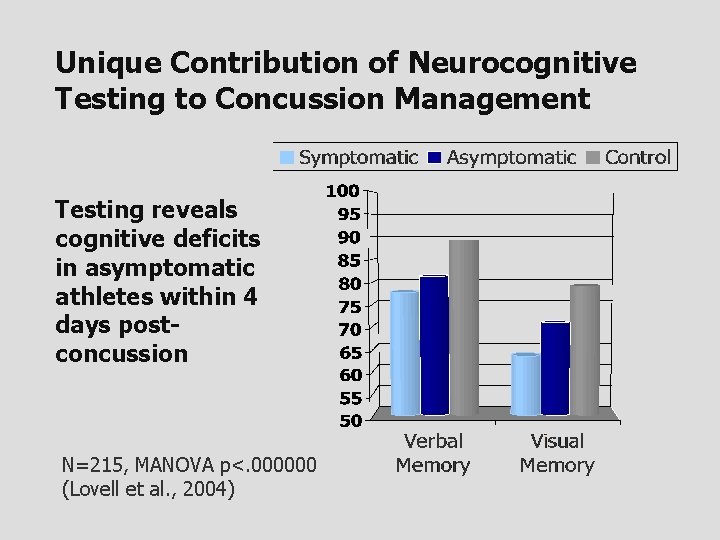
Unique Contribution of Neurocognitive Testing to Concussion Management Testing reveals cognitive deficits in asymptomatic athletes within 4 days postconcussion N=215, MANOVA p<. 000000 (Lovell et al. , 2004)

Guidelines for Return to School after Concussion § Out of school at first if necessary, and then gradual re-entry as tolerated § Avoid re-injury in sports, gym classs and crowded hallways or stairwells § Provide academic accommodations § Communicate and Educate

Academic Accommodations § Rest breaks during school in a quiet location (not always the nurse’s office) § Reduced course and work load § Drop unnecessary classes § Decrease homework § Avoid over-stimulation, (e. g. , cafeteria or noisy hallways) § Extra time and a quiet location for tests

Summary § CDC now recognizes sports concussion as a significant public health issue § Proper recognition and management of concussion can prevent serious problems § No RTP in current game or practice § No RTP until symptom free, at rest and with exertion § Manage every athlete and concussion individually § Neurocognitive testing is recommended

Remember to wear your helmet ! upstate. edu/concussion riegerb@upstate. edu

Concussion Management Program & CNY Sports Concussion Center University. Hospital Clinical Evaluation and Treatment Community Education Research upstate. edu/concussion riegerb@upstate. edu
- Slides: 33