Computed tomography and bronchoscopy in a patient with
Computed tomography and bronchoscopy in a patient with bronchiectasis List 5 common bacterial infections in patients with established bronchiectasis ► Mention the impact of such infections on patients lung function and outcome ► Recognize the role of CT scanning in detecting the etiology of bronchiectasis ► Recognize the role of bronchoscopy in detecting the etiology of bronchiectasis ► PA # 14: Bronchiectasis 1

Case description ► 70 year old man with chronic “seal barking” cough for 1 year ► Cough with congestion is worse at night and better with upright position ► Dyspnea ( WHO class II) ► Frequent hospitalizations for pneumonia and bronchitis PA # 14: Bronchiectasis 2

Case description ► Medications: ▪ Advair; Spiriva, Singulair, Prednisone 10 mg/day, Nasonex, Mucinex and Claritin; TOBI ► PMHx: ▪ eczema; asthma; multiple pneumonias PA # 14: Bronchiectasis 3
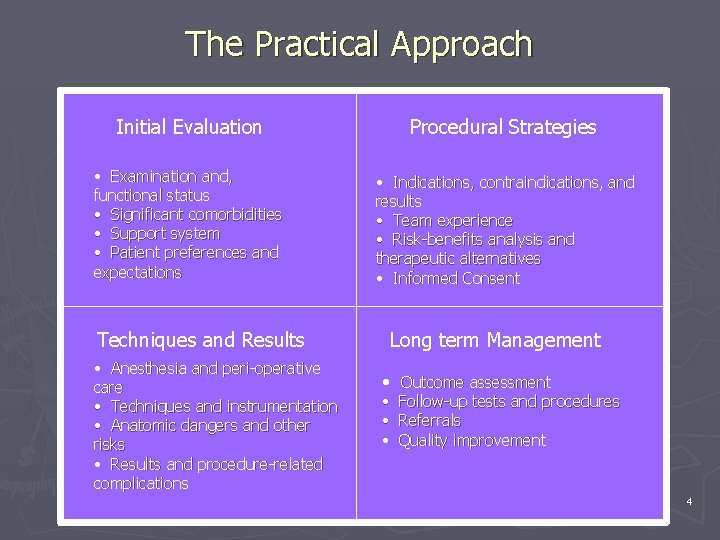

The Practical Approach Initial Evaluation Procedural Strategies • Examination and, functional status • Significant comorbidities • Support system • Patient preferences and expectations • Indications, contraindications, and results • Team experience • Risk-benefits analysis and therapeutic alternatives • Informed Consent Techniques and Results • Anesthesia and peri-operative care • Techniques and instrumentation • Anatomic dangers and other risks • Results and procedure-related complications Long term Management • Outcome assessment • Follow-up tests and procedures • Referrals • Quality improvement BI #. Practical Approach Title 4

Initial Evaluations ► Examination: early wheezing during expiration heard over trachea and bilateral rhonchi ► Pulmonary function tests: ▪ FEV 1 1. 93 L ( 51% predicted)=>2. 26 L ( 60% predicted) 17% improvement after bronchodilators ▪ FVC 2. 62 L (52% predicted)=> 3. 19 L ( 63% predicted) 22% improvement after bronchodilators ▪ TLC 98% predicted; RV 171% predicted; DLCO 89% predicted PA # 14: Bronchiectasis 5
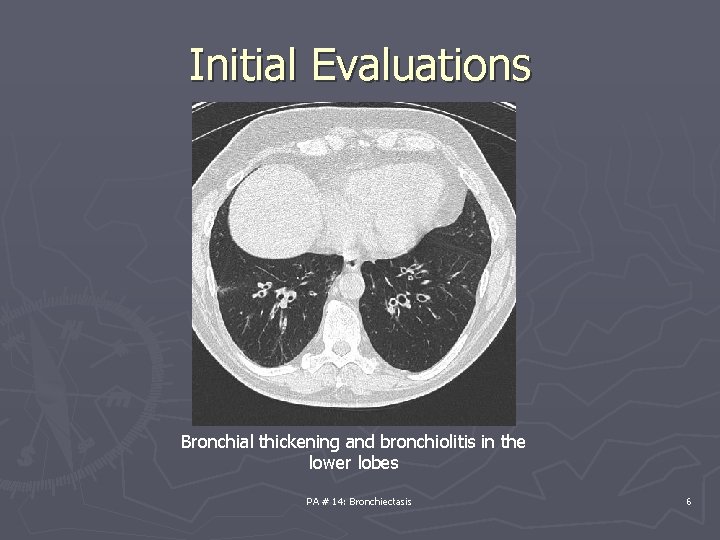
Initial Evaluations Bronchial thickening and bronchiolitis in the lower lobes PA # 14: Bronchiectasis 6

Procedural Strategies If bronchiectasis is truly focal (i. e. confined to one lobe), then it is highly unlikely that inherited or systemic causes will be responsible and so investigations can be tailored appropriately. PA # 14: Bronchiectasis Current Opinion in Pulmonary Medicine 2008, 14: 595– 599 7

Procedural Techniques and Results ► Autoantibody screen: ANA, ANCA, anti SSB, RF negative; ► CF testing for 97 mutations : negative ► Alfa 1 Antitrypsin 153 ( Normal) ► Ig. G, Ig. M, Ig. A and Ig. E were normal ► ESR 25 ( normal< 20) PA # 14: Bronchiectasis 8
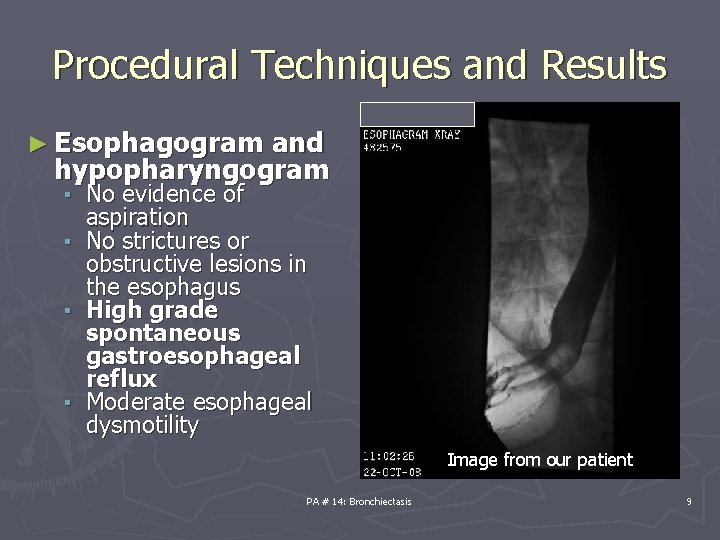
Procedural Techniques and Results ► Esophagogram and hypopharyngogram ▪ No evidence of aspiration ▪ No strictures or obstructive lesions in the esophagus ▪ High grade spontaneous gastroesophageal reflux ▪ Moderate esophageal dysmotility Image from our patient PA # 14: Bronchiectasis 9

Procedural Techniques and Results: Gastroesophageal Reflux and Bronchiectasis ► There is a high prevalence of GERD, usually asymptomatic, in patients with bronchiectasis ► The prevalence of GERD was 26% ► Only 27% of these patients had typical symptoms Koh WJ, Lee JH, Kwon YS, et al. Prevalence of gastroesophageal reflux disease in patients with nontuberculous mycobacterial lung disease. Chest 2007; 131: 1825– 1830. PA # 14: Bronchiectasis 10
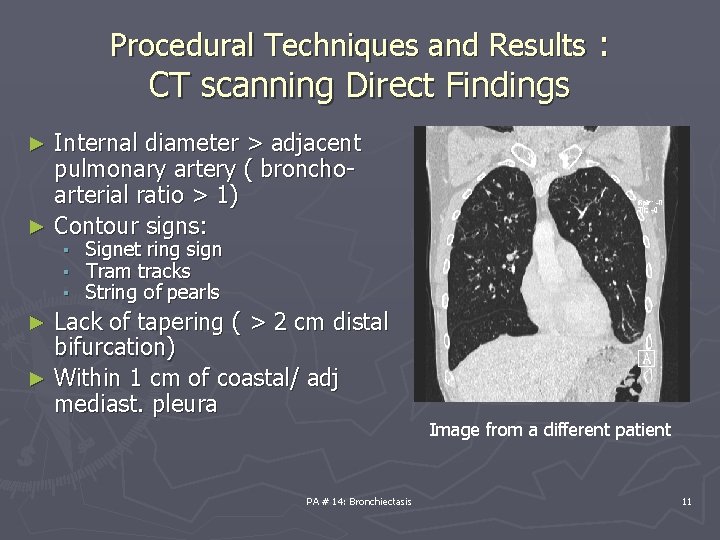
Procedural Techniques and Results : CT scanning Direct Findings Internal diameter > adjacent pulmonary artery ( bronchoarterial ratio > 1) ► Contour signs: ► ▪ ▪ ▪ Signet ring sign Tram tracks String of pearls Lack of tapering ( > 2 cm distal bifurcation) ► Within 1 cm of coastal/ adj mediast. pleura ► PA # 14: Bronchiectasis Image from a different patient 11
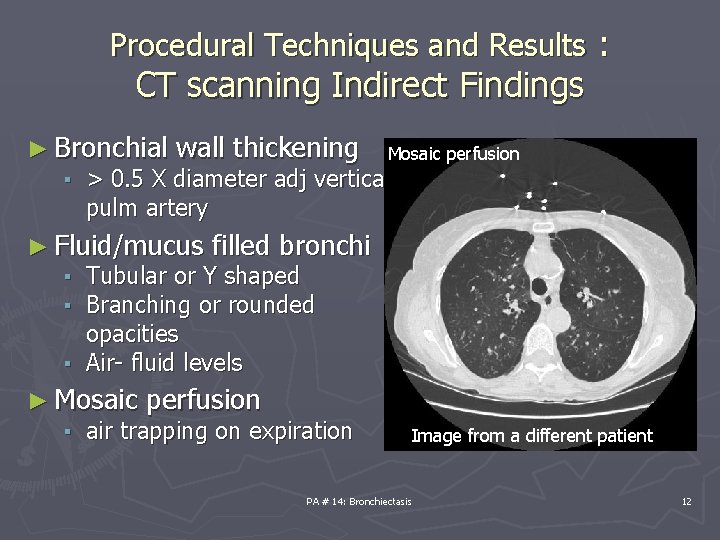
Procedural Techniques and Results : CT scanning Indirect Findings ► Bronchial wall thickening Mosaic perfusion ▪ > 0. 5 X diameter adj vertical pulm artery ► Fluid/mucus filled bronchi ▪ Tubular or Y shaped ▪ Branching or rounded opacities ▪ Air- fluid levels ► Mosaic perfusion ▪ air trapping on expiration Image from a different patient PA # 14: Bronchiectasis 12
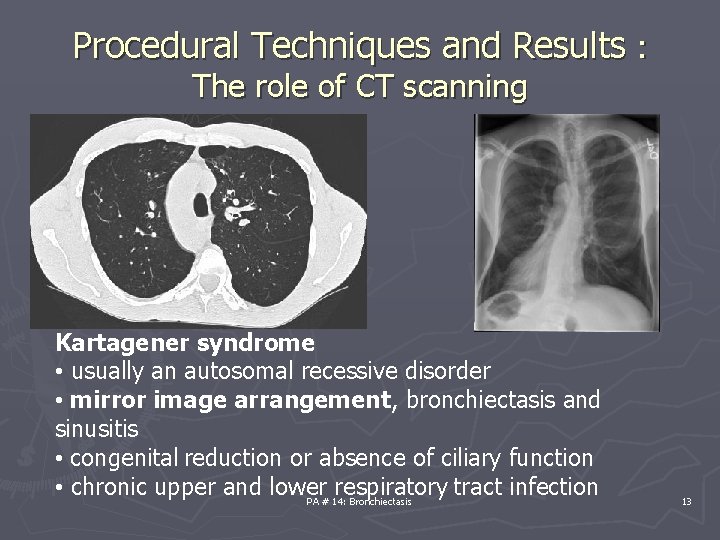
Procedural Techniques and Results : The role of CT scanning Kartagener syndrome • usually an autosomal recessive disorder • mirror image arrangement, bronchiectasis and sinusitis • congenital reduction or absence of ciliary function • chronic upper and lower respiratory tract infection PA # 14: Bronchiectasis 13
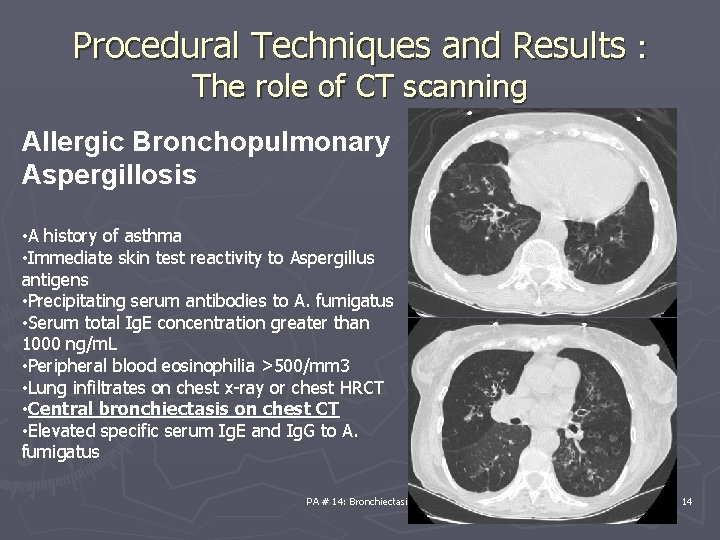
Procedural Techniques and Results : The role of CT scanning Allergic Bronchopulmonary Aspergillosis • A history of asthma • Immediate skin test reactivity to Aspergillus antigens • Precipitating serum antibodies to A. fumigatus • Serum total Ig. E concentration greater than 1000 ng/m. L • Peripheral blood eosinophilia >500/mm 3 • Lung infiltrates on chest x-ray or chest HRCT • Central bronchiectasis on chest CT • Elevated specific serum Ig. E and Ig. G to A. fumigatus PA # 14: Bronchiectasis 14

Differential Diagnosis of Bronchiectasis ► HRCT of limited value in diagnosis cause ► HRCT findings: ▪ Correct diagnosis in 45 -61% ▪ ▪ ▪ Central bronchiectasis ABPA Severe and extensive CF and ABPA Bilateral upper lobe CF and ABPA Unilateral upper lobe TB Lower lobes post infectious or impaired mucociliary clearance PA # 14: Bronchiectasis 15

Procedural Techniques and Results: Infections ► In this patient, the sputum cultures and BAL cultures showed: ▪ ▪ Stenotrophomonas Nocardia E. coli Aspergillus PA # 14: Bronchiectasis 16

Procedural Techniques and Results: Infections ► Infections play a prominent role in bronchiectasis exacerbations and probably in the baseline symptoms ► The reason for chronic infections and exacerbations in patients with bronchiectasis is the anatomic abnormality http: //www-medlib. med. utah. edu/Web. Path/LUNGHTML/LUNG 053. html PA # 14: Bronchiectasis Barker AF. Bronchiectasis. N Engl J Med 2002; 346: 1383– 93. 17
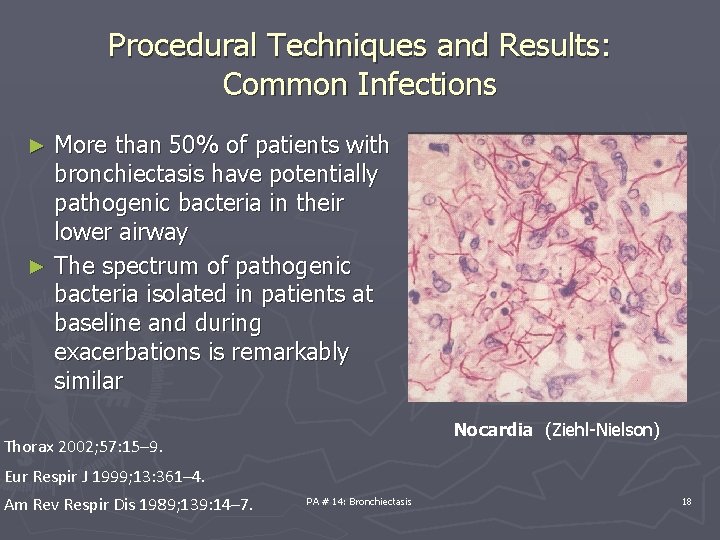
Procedural Techniques and Results: Common Infections More than 50% of patients with bronchiectasis have potentially pathogenic bacteria in their lower airway ► The spectrum of pathogenic bacteria isolated in patients at baseline and during exacerbations is remarkably similar ► Nocardia (Ziehl-Nielson) Thorax 2002; 57: 15– 9. Eur Respir J 1999; 13: 361– 4. Am Rev Respir Dis 1989; 139: 14– 7. PA # 14: Bronchiectasis 18
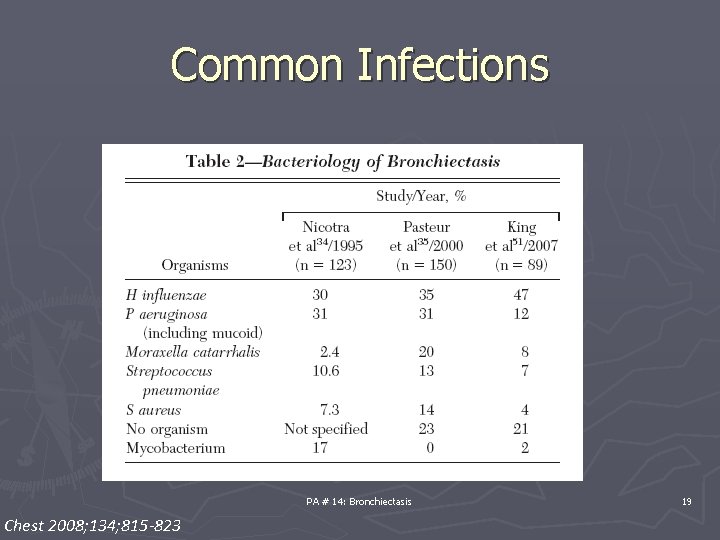
Common Infections PA # 14: Bronchiectasis Chest 2008; 134; 815 -823 19

Common pathogens in non cystic fibrosis bronchiectasis ►H influenzae 55% ► Pseudomonas aeruginosa 26% ► S pneumoniae 12% ► M catarrhalis Cabello H, Torres A, Celis R, et al. Bacterial colonization of distal airways in healthy subjects and chronic lung disease: a bronchoscopic study. Eur Respir J 1997; 10: 1137– 44. King PT, Holdsworth SR, Freezer NJ, et al. Microbiologic follow-up study in adult bronchiectasis. Respir Med 2007; 101: 1633– 8. PA # 14: Bronchiectasis 20

Less common pathogens in non cystic fibrosis bronchiectasis ► Enterobacteriaceae ► Nocardia ►S aureus ► NTM PA # 14: Bronchiectasis 21

Procedural Techniques and Results: Impact on outcome ►P aeruginosa correlates with more severe clinical disease in non CF bronchiectasis ▪ Chest 1998; 114: 1594– 8 ► Effect on lung function ▪ No change Eur Respir J 2006; 28: 974– 9 ▪ Decline of lung function include ►chronic colonization by Pseudomonas ►a history of severe exacerbations ►evidence of systemic inflammation aeruginosa ▪ Chest 2007; 132: 1565– 1572 PA # 14: Bronchiectasis 22

Bacteria and fungi that colonize and cause infection in CF ► Pseudomonas aeruginosa ► Staphylococcus aureus (including methicillin- resistant S aureus) ► Nontypeable Haemophilus influenzae ► Burkholderia cepacia complex ► Stenotrophomonas maltophilia ► Alcaligenes xylosoxidans ► Nontuberculous mycobacteria ► Pandoraea apista ► Aspergillus fumigatus ► Scedosporium apiospermum PA # 14: Bronchiectasis Infect Dis Clin N Am 21 (2007) 673– 695 23
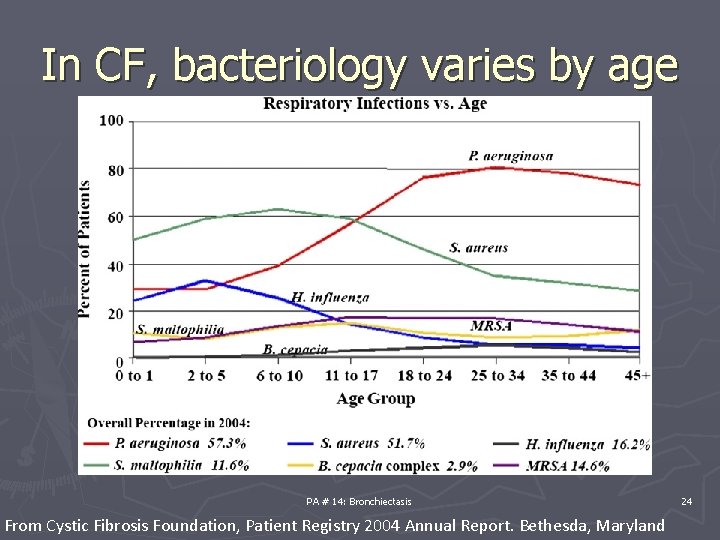
In CF, bacteriology varies by age PA # 14: Bronchiectasis From Cystic Fibrosis Foundation, Patient Registry 2004 Annual Report. Bethesda, Maryland 24

Bacteriology in CF ► Most patients with CF have polymicrobial chronic airway infection. ► In ananalysis of 595 patients, an average of 2. 9 pathogenic species per sputum were cultured Burns JL, Emerson J, Stapp JR, et al. Microbiology of sputum from patients at cystic fibrosis centers in the United States. Clin Infect Dis 1998; 27: 158– 63. PA # 14: Bronchiectasis 25

Bacteriology in CF: Pseudomonas ►P aeruginosa in CF: the most serious pathogen ► the mucus in CF is more viscid and of a greater depth, causing increased oxygen gradient across this layer ► An abnormal glycolipid, asialo. GM 1, functions as a receptor for P aeruginosa pilin and is increased in CF airway cells ► Pseudomonas aeruginosa also changes its lipopolysaccharide side chain structure, which could make it more resistant to antimicrobial peptides PA # 14: Bronchiectasis Infect Dis Clin N Am 21 (2007) 673– 695 26

Bacteriology in CF: Pseudomonas ► Being infected by mucoid P aeruginosa increases mortality and morbidity in CF children Emerson J, Rosenfeld M, Mc. Namara S, et al. Pseudomonas aeruginosa and other predictors of mortality and morbidity in young children with cystic fibrosis. Pediatr Pulmonol 2002; 34: 91– 100. PA # 14: Bronchiectasis 27

Bacteriology in CF: Staph. aureus ►S aureus is an uncommon isolate in bronchiectasis that is not caused by CF ► S aureus is common in CF (14. 6%) ▪ treatment of S aureus in sputum in CF Shah PL, Mawdsley S, Nash K, et al. Determinants of chronic infection with Staphylococcus aureus in patients with bronchiectasis. Eur Respir J 1999; 14: 1340– 4. Mc. Caffery K, Olver RE, Franklin M, et al. Systematic review of antistaphylococcal antibiotic therapy in cystic fibrosis. Thorax 1999; 54: 380– 3. PA # 14: Bronchiectasis 28

Bacteriology in CF: Burkholderia cepacia ►B cepacia colonization was associated with increased mortality at all levels of lung function in CF ► B cepacia remains resistant to most commonly used antibiotics Corey M, Farewell V. Determinants of mortality from cystic fibrosis in Canada, 1970– 1989. Am J Epidemiol 1996; 143: 1007– 17. PA # 14: Bronchiectasis 29

Bacteriology in CF: Other bacteria ► Stenotrophomonas maltophilia and Alcaligenes xylosoxidansare ▪ gram-negative bacilli and are recovered from CF airway cultures in 8% to 10% ▪ Do not affect mortality or severity of the course in CF Demko CA, Stern RC, Doershuk CF. Stenotrophomonas maltophilia in cystic fibrosis: incidence and prevalence. Pediatr Pulmonol 1998; 25: 304– 8. Tan K, Conway SP, Brownlee KG, et al. Alcaligenes infection in cystic fibrosis. Pediatr Pulmonol 2002; 34: 101– 4 PA # 14: Bronchiectasis 30

Bronchiectasis: The role of NTM ► NTM: well recognized cause of bronchiectasis ► NTM to be uncommon in non-CF bronchiectasis ► Bronchiectasis patients with NTM ▪ the incidence of Aspergillus-related lung disease was 33% as compared with 10% in control patients without NTM ► Prevalence of 13% for NTM in CF ▪ M avium complex 72% ▪ Mycobacterium abscessus 16% Kunst H, Wickremasinghe M, Wells A, et al. Nontuberculous mycobacterial disease and Aspergillus-related lung disease in bronchiectasis. Eur Respir J 2006; 28: 352– 7. Wickremasinghe M, Ozerovitch LJ, Davies G, et al. Non-tuberculous mycobacteria in patients with bronchiectasis. Thorax 2005; 60: 1045– 51. PA # 14: Bronchiectasis 31

Back to our patient… 1. Why does the patient have bronchiectasis and recurrent infections? 2. What diagnostic procedure should you do next? PA # 14: Bronchiectasis 32
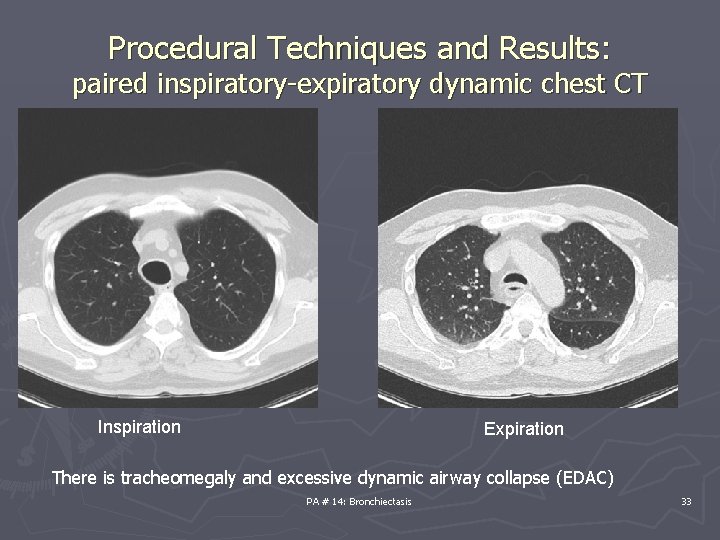
Procedural Techniques and Results: paired inspiratory-expiratory dynamic chest CT Inspiration Expiration There is tracheomegaly and excessive dynamic airway collapse (EDAC) PA # 14: Bronchiectasis 33
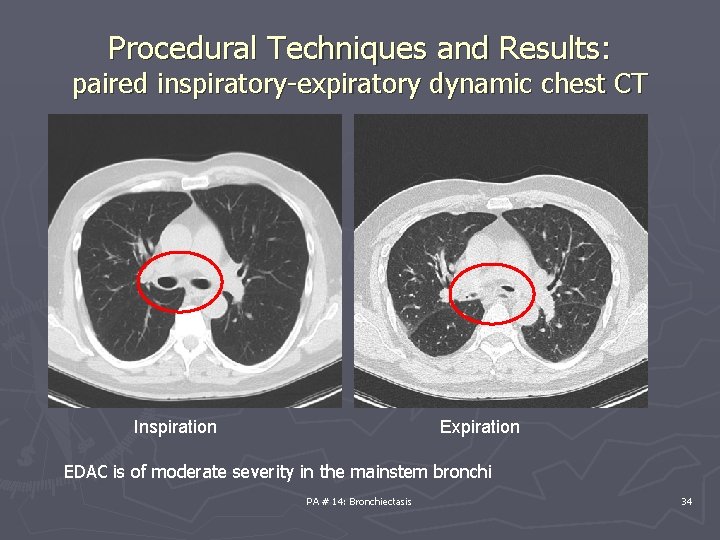
Procedural Techniques and Results: paired inspiratory-expiratory dynamic chest CT Inspiration Expiration EDAC is of moderate severity in the mainstem bronchi PA # 14: Bronchiectasis 34
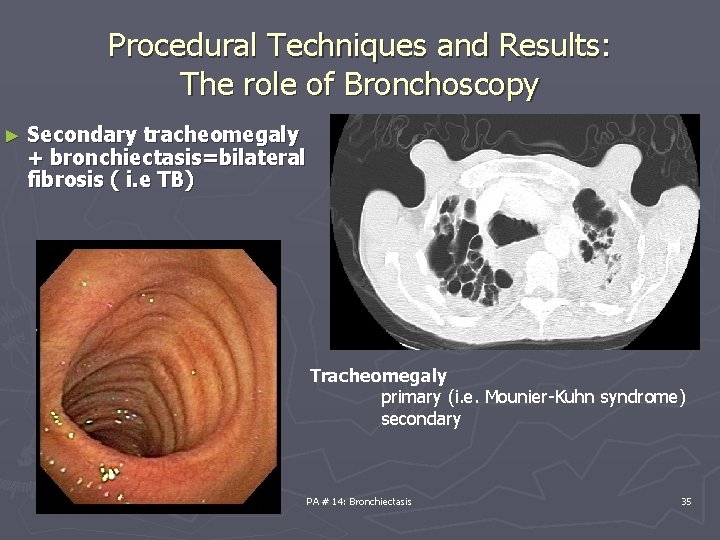
Procedural Techniques and Results: The role of Bronchoscopy ► Secondary tracheomegaly + bronchiectasis=bilateral fibrosis ( i. e TB) Tracheomegaly primary (i. e. Mounier-Kuhn syndrome) secondary PA # 14: Bronchiectasis 35
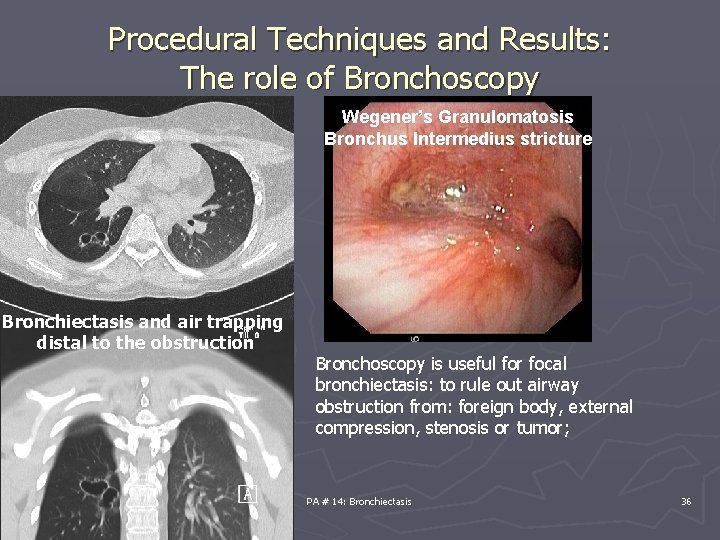
Procedural Techniques and Results: The role of Bronchoscopy Wegener’s Granulomatosis Bronchus Intermedius stricture Bronchiectasis and air trapping distal to the obstruction Bronchoscopy is useful for focal bronchiectasis: to rule out airway obstruction from: foreign body, external compression, stenosis or tumor; PA # 14: Bronchiectasis 36

Procedural Techniques and Results: The role of Bronchoscopy…back to our patient ► Primary (congenital) tracheobronchomegaly + bronchiectasis= Mounier- Kuhn Syndrome ▪ atrophy or absence of elastic fibers and smooth muscle cells ▪ 50% of patients show no symptoms until the third decade of life ▪ Dynamic bronchoscopy can reveal the expiratory central airway collapse PA # 14: Bronchiectasis Bateson EM, Woo-Ming M. Tracheo-bronchomegaly. Clin Radiol 1973; 24: 345– 58. 37
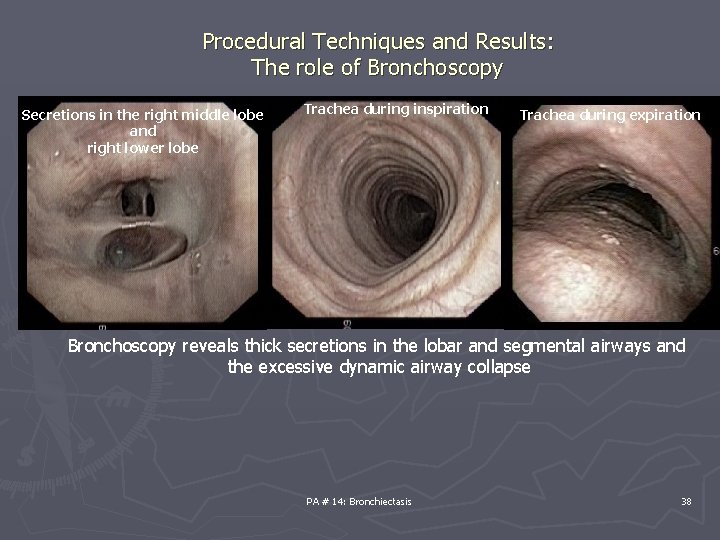
Procedural Techniques and Results: The role of Bronchoscopy Secretions in the right middle lobe and right lower lobe Trachea during inspiration Trachea during expiration Bronchoscopy reveals thick secretions in the lobar and segmental airways and the excessive dynamic airway collapse PA # 14: Bronchiectasis 38
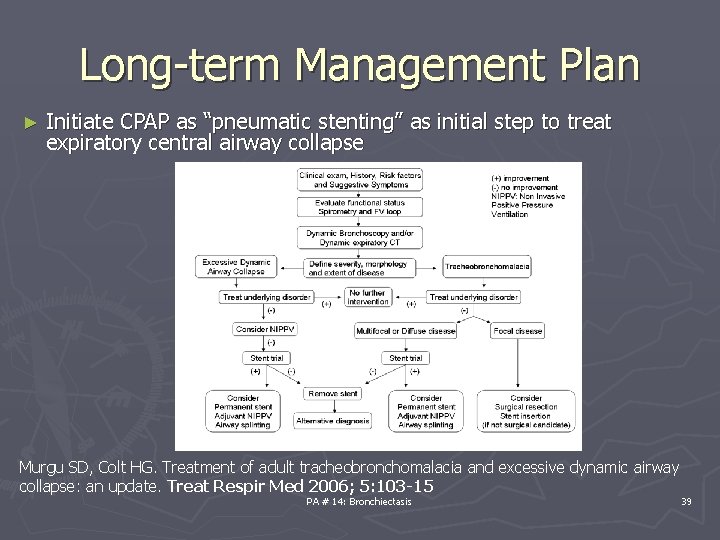
Long-term Management Plan ► Initiate CPAP as “pneumatic stenting” as initial step to treat expiratory central airway collapse Murgu SD, Colt HG. Treatment of adult tracheobronchomalacia and excessive dynamic airway collapse: an update. Treat Respir Med 2006; 5: 103 -15 PA # 14: Bronchiectasis 39

Long-term Management Plan ► “pneumatic stenting” ▪ Wiseman J Pediatr Surg 1985 ► FEFs measured at the same lung volumes did not differ for the different levels of CPAP ► CPAP affects forced flows primarily by increasing lung volume ▪ Davis S Am J Respir Crit Care 1998 40

Q 1: List 5 common bacterial infections in patients with established bronchiectasis ►H influenzae ► Pseudomonas aeruginosa ► S pneumoniae ► M catarrhalis ► S aureus PA # 14: Bronchiectasis 41

Q 2: Mention the impact of such infections on patients lung function and outcome ►P aeruginosa: ►B cepacia: ▪ associated with severe clinical disease in non CF bronchiectasis ▪ increases mortality and morbidity in CF ▪ associated with increased mortality at all levels of lung function in CF PA # 14: Bronchiectasis 42

Q 3: Recognize the role of CT scanning in detecting the etiology of bronchiectasis ► HRCT findings: ▪ Diffuse: location of bronchiectasis narrows the differential diagnosis ▪ Focal: bronchoscopy warranted to rule out endobronchial obstruction ► Paired inspiratory-expiratory dynamic CT: ▪ When expiratory central airway collapse is suspected PA # 14: Bronchiectasis 43

Q 4: Recognize the role of bronchoscopy in detecting the etiology of bronchiectasis ► Perform bronchoscopy if: ▪ Focal bronchiectais (i. e. foreign body) ▪ Detect infectious etiologies ►BAL/washings ►Transbronchial biopsies ( i. e. MAI) ▪ Endobronchial biopsies (i. e. PCD) ▪ Detect expiratory airway collapse (i. e. MKS) PA # 14: Bronchiectasis 44

All efforts are made by Bronchoscopy International to maintain currency of online information. All published multimedia slide shows, streaming videos, and essays can be cited for reference as: Bronchoscopy International: Practical Approach, an Electronic On. Line Multimedia Slide Presentation. http: //www. Bronchoscopy. org/Practical. Approach/htm. Published 2017 (Please add “Date Accessed”). Thank you PA # 14: Bronchiectasis 45

Prepared with the assistance of Septimiu Murgu M. D. , University of California, Irvine www. bronchoscopy. org PA # 14: Bronchiectasis 46
- Slides: 46