Compression first v CAB rather than ABC Layperson


Compression first v CAB rather than ABC - Layperson should be encouraged to provide chest compressions for anyone with a presumed cardiac arrest (Class I, B) - Growing evidences of the importance of chest compression - Setting up airway equipment takes time v Let’s change ABC mindset - ABC mindset may reinforce the idea that compressions should wait - Even when more than 1 rescuer is present 대한심폐소생협회

Hands-only CPR v Pros - No bystander CPR < Hands only CPR - Conventional CPR = Hands only CPR - Reluctance to perform mouth to mouth ventilation - May help overcome panic and hesitation to act v Why effective? - Ventilation is not important for first several minutes after arrest - If the airway is open, gasping and passive chest recoil can provide some air exchange 대한심폐소생협회

Hands-only CPR v Rescue breathing is important to noncardiac origin - Pediatric arrests Asphyxial cardiac arrest Prolonged cardiac arrest Conventional CPR is recommended for those specific situations (when capable of giving CPR with ventilations) (IIa, C) v Hands-only CPR is recommended to - Untrained layperson (dispatcher assisted CPR) - Trained but incapable of airway and breathing 대한심폐소생협회
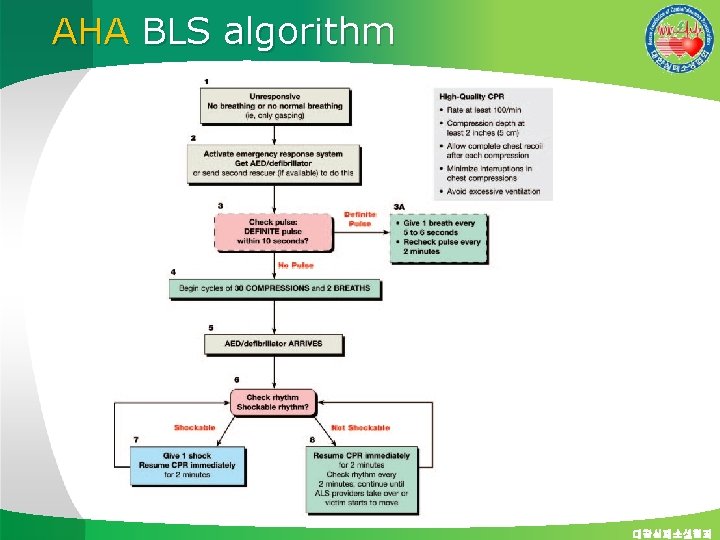
AHA BLS algorithm 대한심폐소생협회
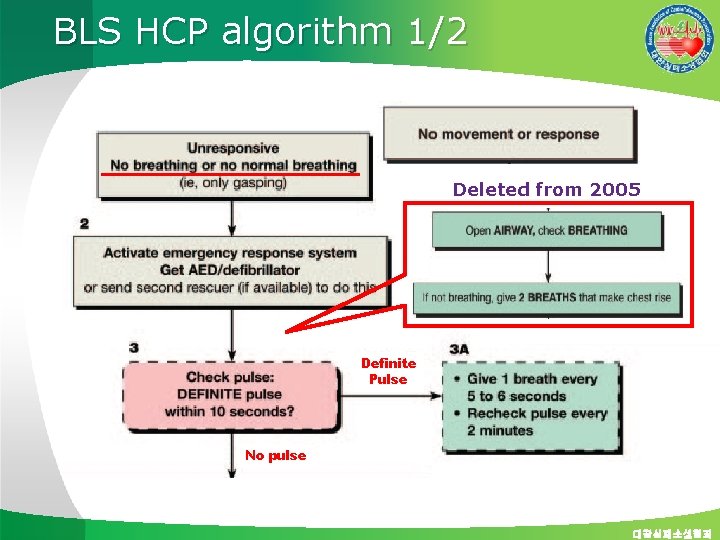
BLS HCP algorithm 1/2 Deleted from 2005 Definite Pulse No pulse 대한심폐소생협회
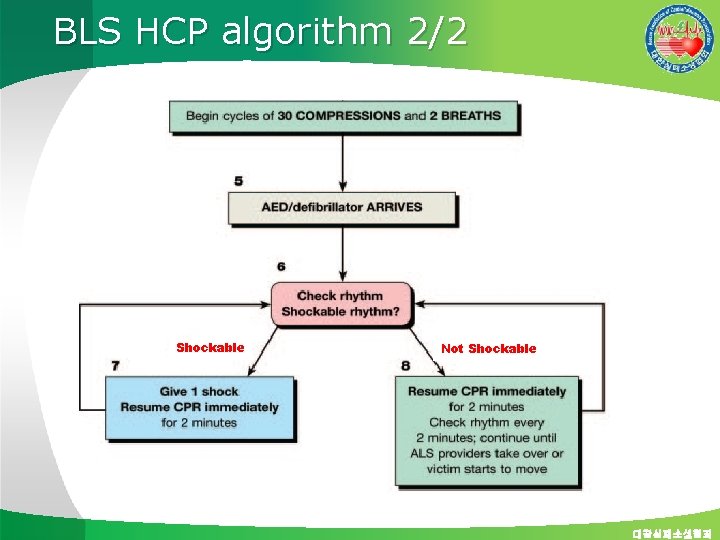
BLS HCP algorithm 2/2 Shockable Not Shockable 대한심폐소생협회
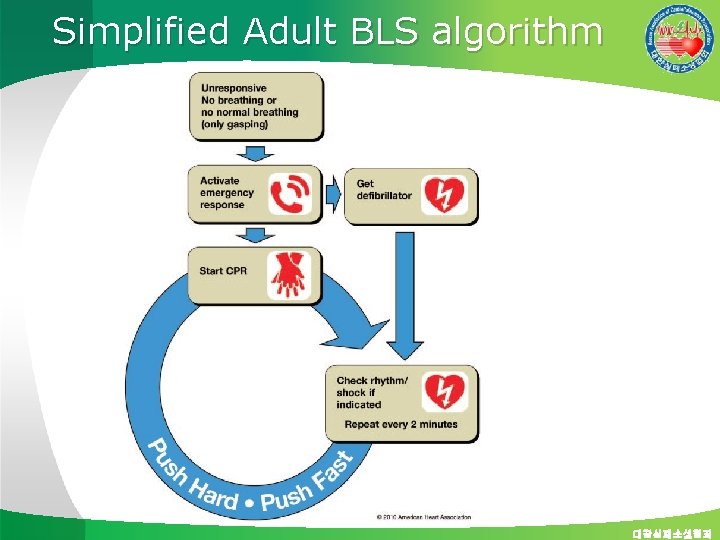
Simplified Adult BLS algorithm 대한심폐소생협회
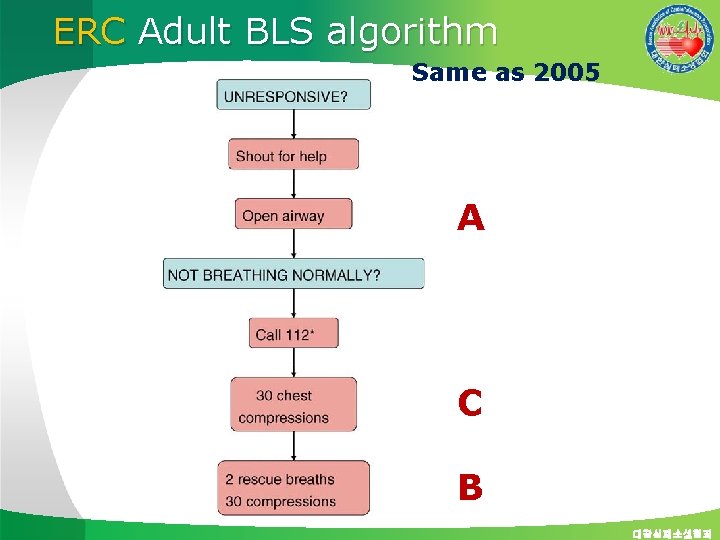
ERC Adult BLS algorithm Same as 2005 A C B 대한심폐소생협회

Patient position v Supine on a firm surface v Use of backboard - Traditionally recommended despite insufficient evidence - Care should be taken - to avoid delays in initiation of CPR - to minimize interruptions in CPR - to avoid line/tube displacement v Air-filled mattress - Should be deflated when performing CPR 대한심폐소생협회

Chest compression technique v Hand position - Lower half of the sternum (IIa, B) - “Place the heel of your hand in the center of the chest with the other hand on top” - Internipple line as a landmark is not reliable v Compression rate (speed) - At least 100 compressions per minute (IIa, B) - Compression pause should be minimized - Not exceeding 120 /min (ERC) v Compression depth - At least 5 cm (IIa, B) - Not exceeding 6 cm (ERC) 대한심폐소생협회

Compression ventilation ratio v 30: 2 - Based on consensus among experts (IIb, B) - Further validation of this guideline is needed v Once an advanced airway is in place - Continuous chest compressions without pauses for ventilation (IIa, B) - Provide ventilation every 6~8 seconds v Minimize interruption of chest compressions throughout the entire resuscitation (IIa, B) - 대한심폐소생협회

Decompression (chest recoil) v Complete chest wall recoil (IIa, B) - Incomplete recoil is common particularly when rescuers were fatigued v Adverse effect of incomplete recoil ↑intrathoracic pressure ↓coronary & cerebral perfusion ↓cardiac index, myocardial blood flow v Can be improved by - Electronic recording devices with real-time feedback - Lifting the heel of the hand slightly, but completely, off the chest 대한심폐소생협회

Duty cycle v Time spent compressing the chest v Duty cycle of 50% is recommended (IIb, C) - Reduced coronary perfusion is associated with a duty cycle of >50% - Duty cycles ranging between 20~50% can result in adequate coronary and cerebral perfusion - 50% is easy to achieve with practice v Compression relaxation times - Approximately equal (IIb, C) 대한심폐소생협회

Switching compressors v Fatigue and shallow compressions are common after 1 min of CPR - Rescuers may not recognize that fatigue is present for 5 min v Switch chest compressors approximately every 2 min (IIa, B) - Consider switching compressors during any intervention in 5 sec 대한심폐소생협회

Interruption of compression v Lay rescuers - Should not interrupt chest compressions to palpate pulses or check for ROSC (IIa, C) - Should continue CPR until an AED arrives, the victim wakes up, or EMS personnel take over CPR (IIa, B) v Healthcare providers - Should interrupt chest compressions as infrequently as possible and try to limit interruptions to no longer than 10 seconds (IIa, C) - Because of difficulties with pulse assessments, interruptions in chest compressions should be minimized 대한심폐소생협회

- Slides: 17