Complications of the Post Partal Period Postpartum Hemorrhage






















































- Slides: 56

Complications of the Post. Partal Period

Postpartum Hemorrhage ¡ Definition l l Early-postpartum hemorrhage of >500 cc within the first 24 hrs. postpartum Late-postpartum hemorrhage of >500 cc after the first 24 hrs postpartum

Postpartum Hemorrhage ¡ Predisposing Factors l l l l l Multiparity Macrosomia Bladder distention Oxytocin augmentation/induction Preeclampsia, Asian or Hispanic heritage Retained placenta Placenta previa Dysfunctional labor Prolonged 3 rd stage of labor

Postpartum Hemorrhage ¡ Causes l Early ¡ Uterine Atony l Most common 2 nd to over distention of uterus or tired muscle Lacerations in vagina ¡ Hematoma ¡ Uterine Inversion ¡

Postpartum Hemorrhage ¡ Causes l Late ¡ Retained placental fragments l ¡ Infection l ¡ Most common cause of late pp hemorrhage Backache, foul smelling lochia, leukorrhea Uterine Subinvolution l Fundal height is greater than expected, lochia fails to progress from rubra to serosa to alba normally.

Postpartum Hemorrhage ¡ Prevention l l l Adequate prenatal care Good nutrition Avoidance of traumatic procedures Risk assessment Early recognition and management of complications

Signs of Hemorrhage (Olds, 2008)

Postpartum Hemorrhage ¡ Nursing Care l Assessment ¡ Fundus-uterine massage if a soft, boggy uterus is detected ¡ urinary output-if inadequate ask pt. to void or catheterization may be required ¡ Vital signs ¡ Lochia-note color and amount l ¡ Weigh pads/chux Hgb/hct l A decrease in Hgb of 1. 0 -1. 5 g/dl or a decrease in HCT of 2 -4% reflects a blood lossof 450 -500 ml

Postpartum Hemorrhage ¡ Nursing Care l Intervention ¡ Fundal massage-immediate and most effective intervention ¡ Empty bladder ¡ Position with legs elevated ¡ Keep pt. informed ¡ Administer O 2 ¡ Notify PCP ¡ Initiate IV if none, in severe hemorrhage place second IV

Estimating Blood Loss Ideal Method=Weighing ¡ 250 cc l l ¡ 355 cc l ¡ 1 cup 5 cm clot (orange) 12 oz soda can 500 cc l l 2 cups 10 cm clot (softball)

Administer Uterotonics ¡ Medications used: l l l Pitocin (Oxytocin)—increase IV rate for bolus Methergine (Methylergonovine Maleate) adrenergic antagonist 0. 2 -0. 4 mg p. o. or 0. 2 mg q 2 -4 hr IM or IV ¡ Check BP due to risk of hypertensive crisis, (do not give to patients with PIH) Prostaglandins-for more critical situations ¡ Hemabate (Carboprost tromethaminie), (do not give to patients with Asthma) ¡ Prostin/15 M (dinoprostone) to decrease blood loss 2 nd to uterine atony. 250 mcgs (1 ml) IM repeated q 1. 5 -3. 5 hrs. ¡ Cytotec (misoprostol) 600 -1000 mcg rectally (only if others not available or have failed)

Nursing Care for postpartum hemorrhage ¡ Intervention l Patient teaching ¡ Provide clear explanations about condition and the importance for the need to recover ¡ Rise slowly to minimize orthostatic hypotension ¡ Encourage to sit while holding the newborn ¡ Encourage to eat foods high in iron ¡ Continue to observe for signs of hemorrhage or infection

Vulvar, Vaginal, and Pelvic Hematoma ¡ Causes l Results from an injury to a blood vessel without noticeable trauma to superficial tissue such as after a forceps delivery. Soft tissue (labia majora or perineal area) can hold 250 -500 cc’s of blood.

Hematomas ¡ Predisposing factors l l l l Preeclampsia Pudendal anesthesia First full-term birth Precipitous labor Prolonged seconds stage Macrosmia Forceps or vacuum assisted birth Vulvar varicosities

Vulvar Hematoma ¡ Symptoms l l l l l Severe pain-rectal pressure Area is very painful to touch Firm to touch Skin may be discolored-reddish Unable to void due to pressure on the urethra Can be hard to detect if hematoma is high in vagina Flank pain Abdominal pain Decreased lochia *signs of shock*

Hematomas ¡ Nursing intervention l Apply ice packs and analgesia ¡ ¡ Typically resolve on own over several days Medical treatment l For hematomas > 5 cm and those that expand ¡ Incision and drainage of hematoma is needed

Puerperal Infection ¡ Definition-infection with temp>100. 4 or 38 degrees on 2 occasions after 1 st 24 hours.

Puerperal Infection ¡ Predisposing factors l C-section l Prolonged premature ROM l Prolonged labor preceding c-section l Multiple VE l Compromised health status ¡ Low socioeconomic status, anemia, obesity, smoking, poor nutrition l FECG, IUPC l Obstetric trauma ¡ Episiotomy, lacerations l Chorioamnionitis l Vacuum, forceps l Manual removal of placenta l Diabetes mellitus

Puerperal Infection ¡ Assessment l l l R: redness E: edema E: ecchymosis D: discharge A: approximation

Puerperal Infection ¡ Signs/Symptoms l l l l Foul smelling lochia Increased temp >38. 4 p first 24 hrs pp Tenderness of fundus upon palpation Fever Malaise Abdominal pain Larger than expected uterus Tachycardia

Puerperal Infection Nursing Care ¡ Treatment/Prevention l l l Good perineal care Hygiene practices to prevent contamination of the perineum Thorough handwashing Sitz baths Adequate fluid intake Diet high in protein and vitamin C

Thromboembolic Disease Seen in 1% of vaginal deliveries and 2 -20% of c-sections ¡ Definition ¡ l Venous thrombosis is a clot in a superficial or deep vein (femoral vein is common site), dangerous when clot loosens from wall of vein and becomes an embolism, which can travel to the heart, brain, or lungs.

Thromboembolic Disease ¡ Thrombophlebitis l Occurs when a clot forms b/c of an inflammation of the vein wall-usually clot is more adherent to vein walls thus a lesser chance of becoming an embolism

Thromboembolic Disease ¡ Predisposing factor of clot formation l Increased amount of blood clotting factors, i. e. increased number of circulation platelets

Thromboembolic Disease (from Olds, 2008 ¡ Who is at risk

Thromboembolic Disease ¡ Symptoms l l l Positive homan’s sign-may occasionally be neg Redness, swelling, pain at site Low grade fever

Thromboembolic Disease ¡ Treatment l l l Local heat Elevate limb Bedrest Analgesics TED hose Anticoagulant (heparin. Coumadin)

Thromboembolic Disease Prevention ¡ ¡ ¡ ¡ Early ambulation TED hose, SCD’s No smoking Elevate legs when sitting Avoid prolonged standing or sitting (contribute to venous stasis) Avoid crossing legs Take frequent breaks while taking car trips

Pulmonary Embolism ¡ Definition l When a clot traveling through the venous system becomes lodged within the pulmonary circulatory system, causing an infarction or occlusion. ¡ IT IS LIFE THREATENING AND REQUIRES IMMEDIATE INTERVENTION

Pulmonary Embolism ¡ Etiology l ¡ Usually preceded by deep vein thrombosis Diagnosis l Verified by ¡ Abg’s, chest x-ray, and pulmonary angiogram

Pulmonary Embolism ¡ Symptoms l l l l Dyspnea Tachypnea and tachycardia Substernal, chest or pleuritic pain Cough Hemoptysis Apprehension Paleness or cyanosis or both

Pulmonary Embolism ¡ Treatment l ¡ Two primary goals ¡ Anticoagulation (IV Heparin) ¡ Cardiorespiratory support (O 2 per mask, Aminophylline, IV fluids) Additional treatment Fibrinolytic therapy (streptokinase or urokinase) may be used to lyse clots. ¡ Pain management may include IV narcotics (demerol or morphine) ¡ Arrhythmias may also require Lidocaine IV ¡

Cystitis (UTI) ¡ Etiology l ¡ Escherichia coli causative agent in most cases of postpartal cystitis Predisposing factors l l l Retention of residual urine Non aseptic technique during catheterization Bladder trauma from childbirth

Cystitis (UTI) ¡ Assessment l l l ¡ Frequency and urgency Dysuria Nocturia Hematuria Suprapubic pain Slightly elevated temperature Diagnosis l Clean catch urine midstream is obtained and sent for microscopic study and culture and sensitivity

Cystitis (UTI) ¡ Prevention/Nursing Care l l l l Good perineal hygiene Good fluid intake Frequent emptying of the bladder ¡ Assist the woman to a normal voiding position ¡ Provide medication for pain ¡ Perineal ice packs Frequent monitoring of the bladder Void before and after intercourse Cotton underwear Increase acidity of the urine Teach s/s of UTI

Cystitis (UTI) ¡ Treatment l Antibiotics ¡ Macrobid, Bactrim DS, Septra DS

Mastitis ¡ Etiology l Staphylococcus Aureus (found in infants nose and throat) ¡ Infection begins when bacteria invade the breast tissue after it has been traumatized or milk stasis occurs (milk acts as favorable medium for the invasion of bacteria)

Mastitis Predisposing factors

Mastitis ¡ Assessment l l l ¡ Breast consistency Skin color Surface temperature Nipple condition Presence of pain Signs and symptoms l l l Onset is sudden, p 10 days Site is unilateral Localized area, red, hot, swollen Pain is localized (often wedge shaped) Temperature. 38. 4 Flulike symptoms-fever, chills, ha, muscle aches

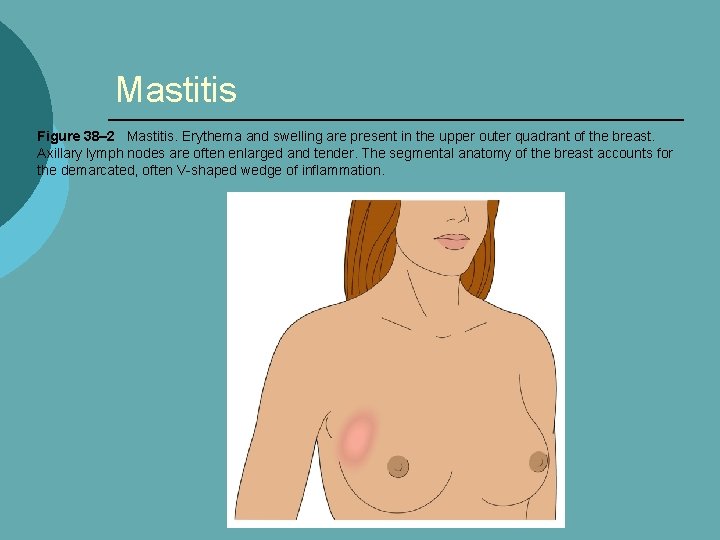
Mastitis Figure 38– 2 Mastitis. Erythema and swelling are present in the upper outer quadrant of the breast. Axillary lymph nodes are often enlarged and tender. The segmental anatomy of the breast accounts for the demarcated, often V-shaped wedge of inflammation.

Mastitis ¡ Prevention l l Proper feeding techniques Supportive bra worn at all times to avoid milk stasis Good handwashing Prompt attention to blocked milk ducts

Mastitis Nursing Care ¡ ¡ ¡ ¡ ¡ Teach mother how to pump if necessary Assist with feelings about being unable to breastfeed Referral to lactation consultant or La Leche League Bedrest for 24 hours Increase fluids Supportive bra Frequent feedings Warm compress analgesics

Mastitis treatment ¡ 7 -10 days of antibiotics l ¡ Penicillinase-resistant penicillin or cephalosporin Non-steroidal anti-inflammatory agents to treat fever and inflammation

Mastitis-Self care instructions Importance of regular, complete emptying of the breasts ¡ Good infant positioning and latch-on ¡ Principles of supply and demand ¡ Importance of taking a full course of antibiotics ¡ Report flu-like symptoms ¡

Postpartum Disorders Postpartum Blues ¡ Postpartum Depression ¡ Postpartum Psychosis ¡

Postpartum Psychiatric Disorders ¡ Assessment Depression scales Anxiety and irritability Poor concentration and forgetfulness Sleeping difficulties Appetite change Fatigue and tearfulness

Postpartum Blues ¡ “Baby” blues occurs 50 -75% of mothers l ¡ ¡ Characterized by mild depression interspersed with happier feelings. Signs and symptoms-sadness, crying but still able to feel happy Onset/duration l l l Transient Occur 4 -5 days pp and last for a few hours or at most 1 -2 days Not culture specific

Postpartum Depression ¡ 10 -15%of women are clinically depressed at 3 mo. pp. Only 2 -3% of these women are referred to a pychiatrist. 25% of mothers depressed in the first 3 mo. Are likely to develop chronic depression

Postpartum Depression ¡ Course of symptoms l l l l Get the blues->gets better->then in a few weeks, feels depressed (can last up to a year) Mother focuses on guilt and inadequacies of being a mother Chronic tiredness/exhaustion Tiredness/exhaustion Low spirits and low tolerance for stress Can lead to problems r/t baby (irritability and hostility) ***Some research show a relationship b/t maternal postnatal depression and cognitive development of the child and later behavior patterns***

Postpartum Depression ¡ Predisposing Factors/Risk Factors l l l l l Lack of social support (single mom, Yuppie mom) Previous dysmenorrhea Hx of previous pp depression Hx of miscarriage Sever attack of blues p birth Stress p birth ( marital or housing prob) Depression in 2 nd trimester of pregnancy Hx of illness Poor physical maternal health

Postpartum Depression Prevention

Postpartum Depression ¡ Treatment (must be multifaceted) l Psychotherapy Cognitive and supportive therapy ¡ Marital therapy ¡ Support groups as DAD’s (depression after delivery ¡ l Social support

Postpartum Depression Treatment cont’d l Medications-antidepressants (these work with mothers experiencing insomnia, agitation, and anxiety attacks) ¡ ¡ ¡ l Meds-antidepressants ( these work with mothers experiencing severe fatigue who are hard to “wake up” or act more despondent) ¡ ¡ ¡ l Sinequan (doxepin) Tofranil (imipramine) Desyrel (trazadone HCL) Norpramin (desipramine HCL) Prozac (fluoxetine HCL) Vivactil (protriptyline HCL) Medications-antimanic drugs (may be used to control hyperactivity or manicky behavior) ¡ Lithium or Tegretol

Postpartum Psychosis Occurs in 1 -2/1000 mothers ¡ Course symptoms ¡ l l l Manic state Delirium-confusion or dissociative episodes Delusion-see visions/hallucinations, hear voices often r/t baby

Postpartum Psychosis ¡ Risk factors l l l Previous puerperal psychosis Hx of bipolar disorder Prenatal stressors (lack of support, low socioeconomic status) Obsessive personality Family hx of mood disorder

Postpartum psychosis ¡ Treatment l l l Hospitalization-ideally on a psychiatric mother/baby unit seen in England Psychotherapy Medications-antipsychotic drugs Stelazine (trifluoperazine HCL) ¡ Haldol (haloperidol) ¡ Mellaril (thioridazine HCL) ¡