Complications of Diabetes Mellitus Chronic Hasan Aydin MD
![Complications of Diabetes Mellitus [Chronic] Hasan Aydin, MD Department of Endocrinology and Metabolism Yeditepe Complications of Diabetes Mellitus [Chronic] Hasan Aydin, MD Department of Endocrinology and Metabolism Yeditepe](https://slidetodoc.com/presentation_image_h2/04420201f14914157a46b80e6e80fcf5/image-1.jpg)
Complications of Diabetes Mellitus [Chronic] Hasan Aydin, MD Department of Endocrinology and Metabolism Yeditepe University Medical Faculty

Complications of Diabetes Mellitus Chronic complications • Microvascular – retinopathy – Nephropathy – neuropathy • Macrovascular – cerbrovascular, cardiovascular, peripheral vascular disease Acute complications – diabetic ketoacidosis – diabetic nonketotic, hyperosmolar coma – hypoglycemia

Introduction • Adults with diabetes have an annual mortality of 5. 4% (double the rate for non-diabetic adults) • Life expectancy is decreased on average by 5 -10 years • Although the increased death rate is mainly due to cardiovascular disease, deaths from non-cardiovascular causes are also increased. • • A diagnosis of diabetes immediately increases the risk of developing various clinical complications that are largely irreversible and due to microvascular or macrovascular

DM Complications Major Determining Factors Duration Glycemic Control Type 1 vs. Type 2
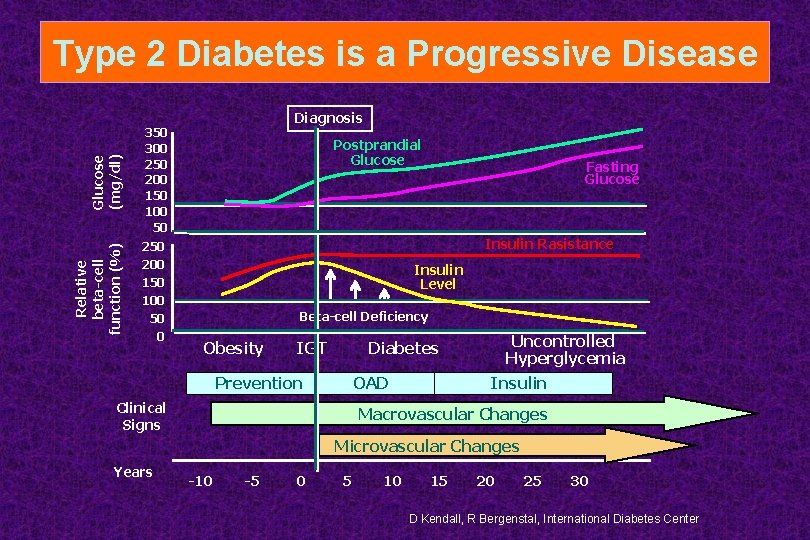
Relative beta-cell function (%) Glucose (mg/dl) Type 2 Diabetes is a Progressive Disease Diagnosis 350 300 250 200 150 100 50 Postprandial Glucose Insulin Rasistance 250 200 150 100 50 0 Fasting Glucose Insulin Level Beta-cell Deficiency Obesity IGT Uncontrolled Hyperglycemia Diabetes Prevention OAD Clinical Signs Insulin Macrovascular Changes Microvascular Changes Years -10 -5 0 5 10 15 20 25 30 D Kendall, R Bergenstal, International Diabetes Center
Type 2 DM Starts Years Before Diagnosis At the diagnosis of Type 2 DM 9. 9 - 20. 8% of pts have retinopathy Harris MI et al. Diab Care, 21: 1992. Hamman RF et al. Diabetes, 38: 1989 5 – 10% proteinuria Haffner SM et al. Diab Care, 12: 1989

Prevention is more rewarding than Management of Complications

Microvascular Complications

Microvascular Complications • Microvascular complications are specific to diabetes and do not occur without longstanding hyperglycaemia • Both T 1 DM and T 2 DM are susceptible to microvascular complications • The duration of diabetes and the quality of diabetic control are important determinants of microvascular disease

Microvascular Complications • A continuous relation exists between glycaemic control and the incidence and progression of microvascular complications. • HTN and smoking also have an adverse effect on microvascular outcomes.

“Tight Glycemic Control” reduces microvascular and macrovascular complications
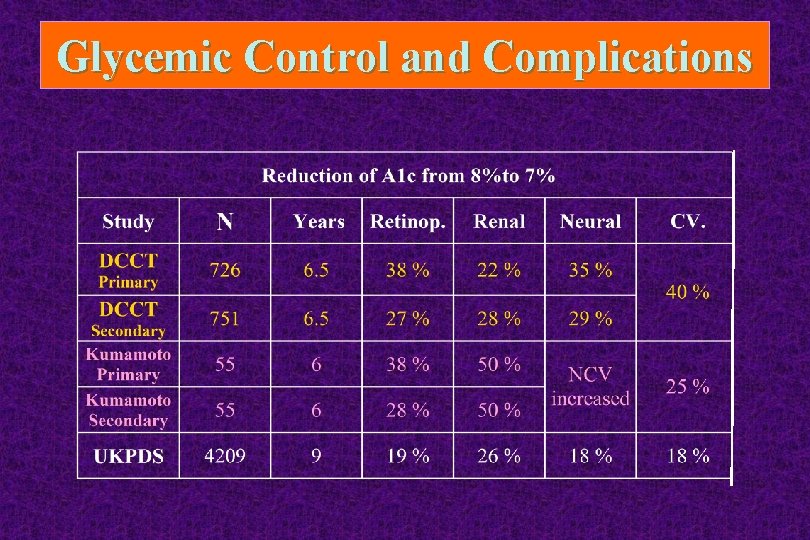
Glycemic Control and Complications
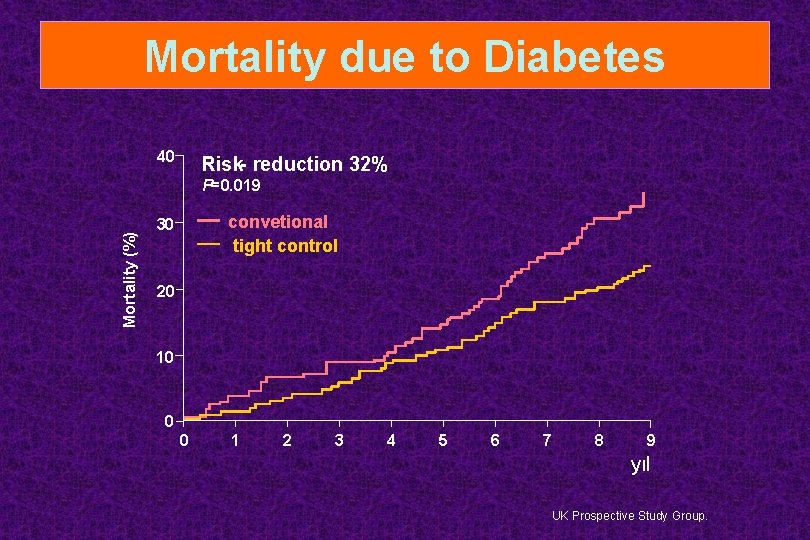
Mortality due to Diabetes 40 Risk- reduction 32% Mortality (%) P=0. 019 convetional tight control 30 20 10 0 0 1 2 3 4 5 6 7 8 9 yıl UK Prospective Study Group.
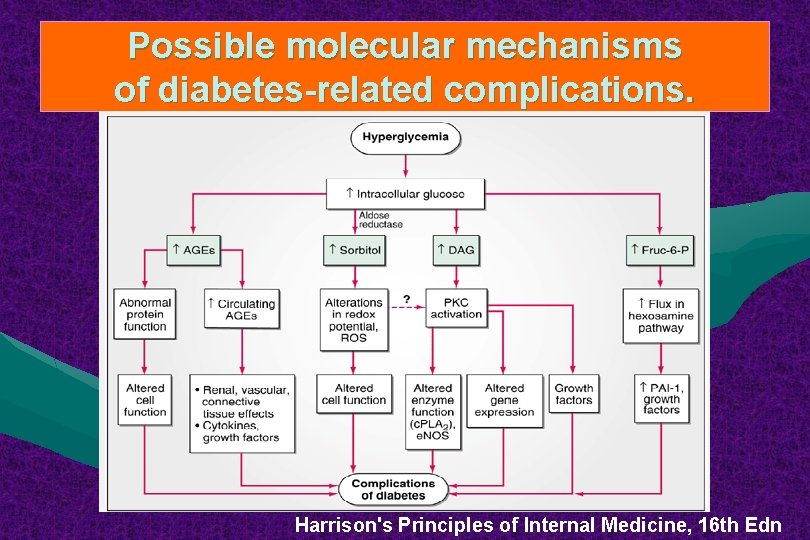
Possible molecular mechanisms of diabetes-related complications. Harrison's Principles of Internal Medicine, 16 th Edn
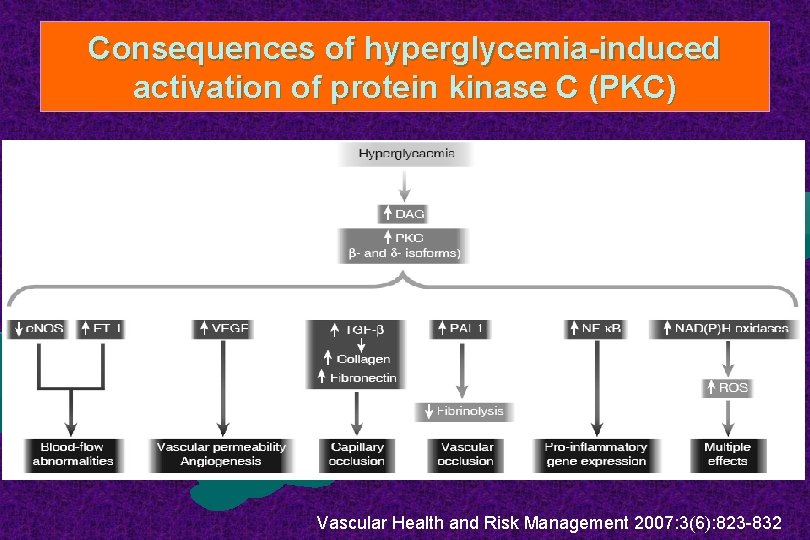
Consequences of hyperglycemia-induced activation of protein kinase C (PKC) Vascular Health and Risk Management 2007: 3(6): 823 -832
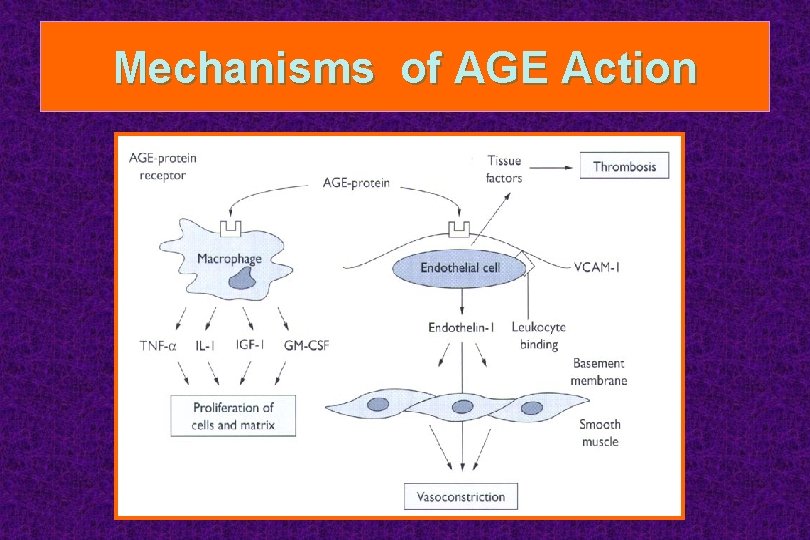
Mechanisms of AGE Action

Pathophysiology of Microvascular Disease • Structural changes – thickening of the capillary basement membrane • Functional changes – increased capillary permeability – increased blood flow and viscosity – disturbed platelet function • Chemical changes in basement membrane composition – increased type IV collagen and its glycosylation products

Diabetic Retinopathy

Retinopathy • Diabetic retinopathy is a progressive disorder • It is the commonest cause of blindness in age 30 -69. • Damage to the retina arises from a combination of microvascular leakage and microvascular occlusion • A fifth of p’ts with newly discovered type 2 diabetes have retinopathy at the time of diagnosis.

Retinopathy • In type 1 diabetes, vision threatening retinopathy almost never occurs in the first five years after diagnosis or before puberty. • After 15 years, however, almost all type 1 diabetes and two thirds of type 2 diabetes have background retinopathy • Vision threatening retinopathy is usually due to neovascularisation in type 1 diabetes and maculopathy in type 2 diabetes.

Retinopathy • Depending on the relative contribution of leakage or capillary occlusion, maculopathy is divided into three types: – exudative maculopathy (when hard exudates appear in the region of the macula), – ischaemic maculopathy (characterised by a predominance of capillary occlusion which results in clusters of haemorrhages) – edematous maculopathy (extensive leakage gives rise to macular edema).

Classification of Diabetic Retinopathy • Neovascularization (4 categories) – Nonproliferative (NPDR) 1. Early to moderate NPDR 2. Severe NPDR (preproliferative) – Proliferative (PDR) 1. Non-high-risk PDR 2. High-risk PDR
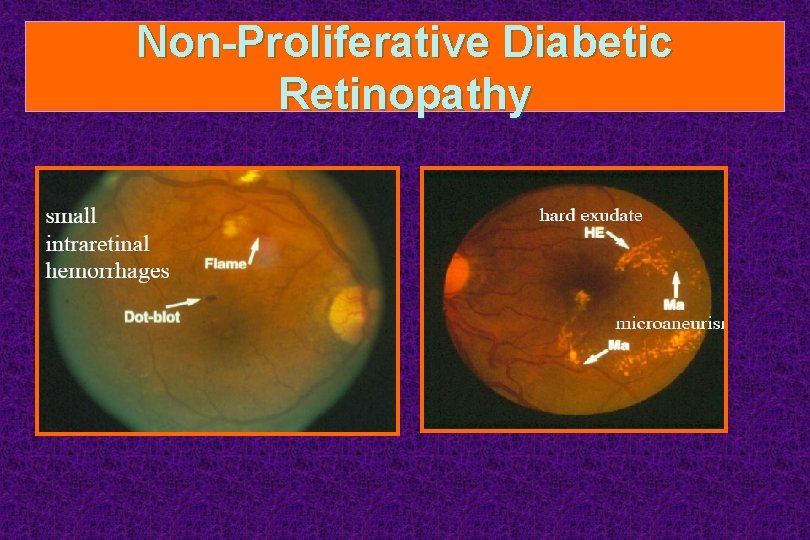
Non-Proliferative Diabetic Retinopathy
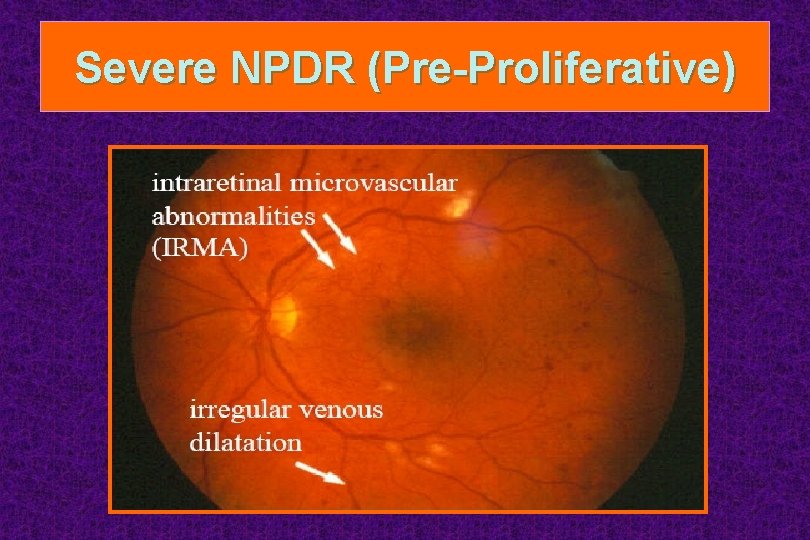
Severe NPDR (Pre-Proliferative)
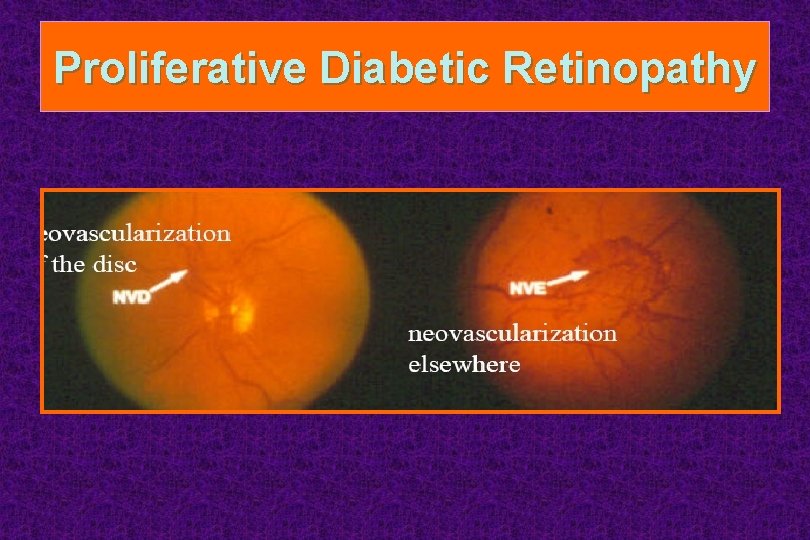
Proliferative Diabetic Retinopathy
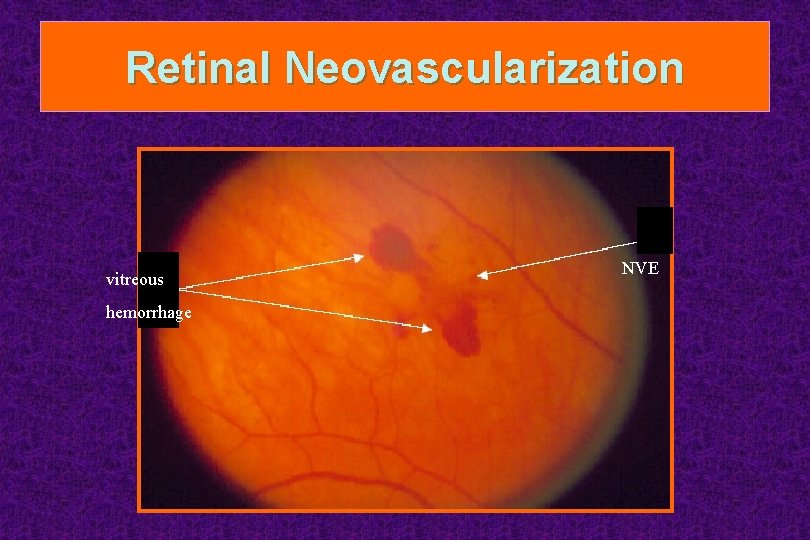
Retinal Neovascularization vitreous hemorrhage NVE
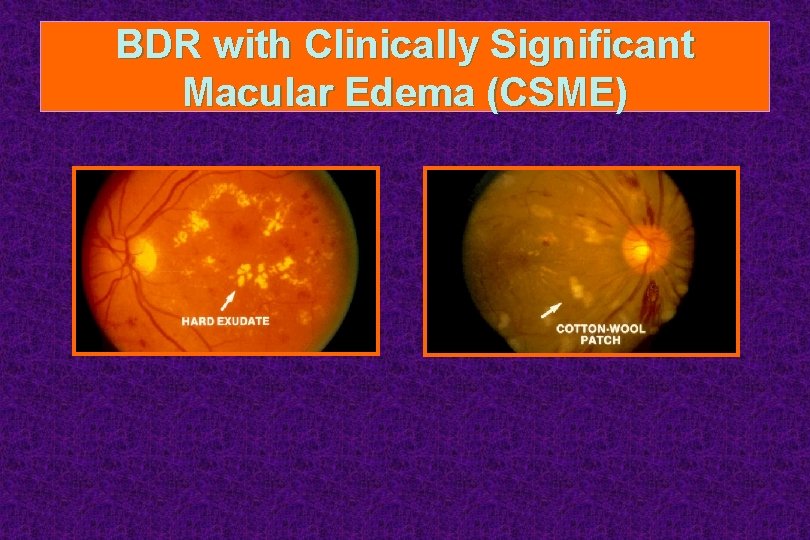
BDR with Clinically Significant Macular Edema (CSME)
Treatment of Diabetic Retinopathy (Systemic) • Control – Blood sugar – Blood pressure – Cholesterol • Treat – Heart failure – Kidney failure – Avoid smoking
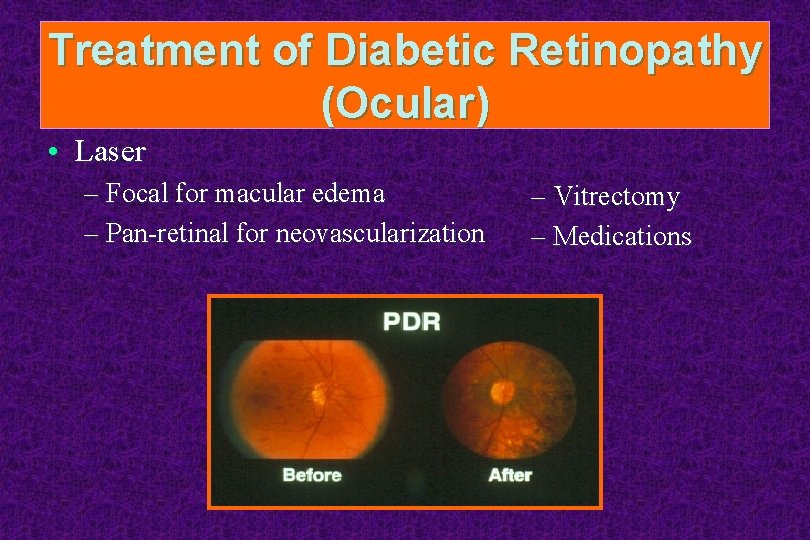
Treatment of Diabetic Retinopathy (Ocular) • Laser – Focal for macular edema – Pan-retinal for neovascularization – Vitrectomy – Medications
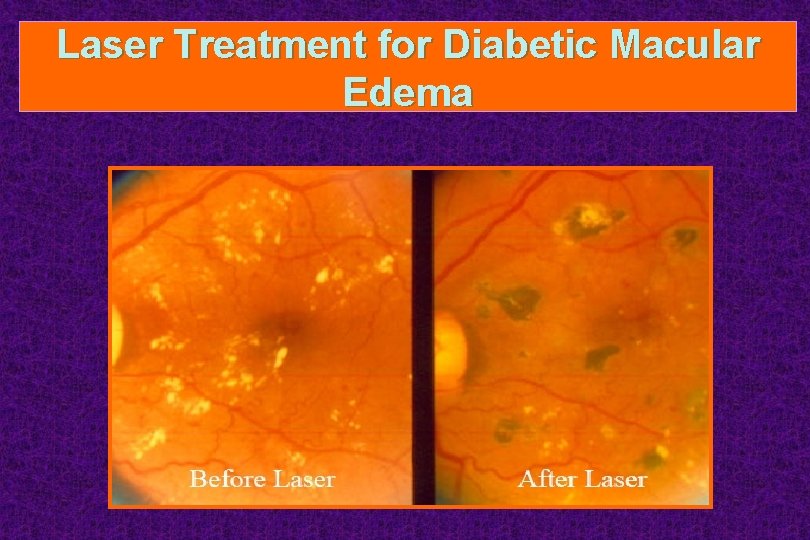
Laser Treatment for Diabetic Macular Edema
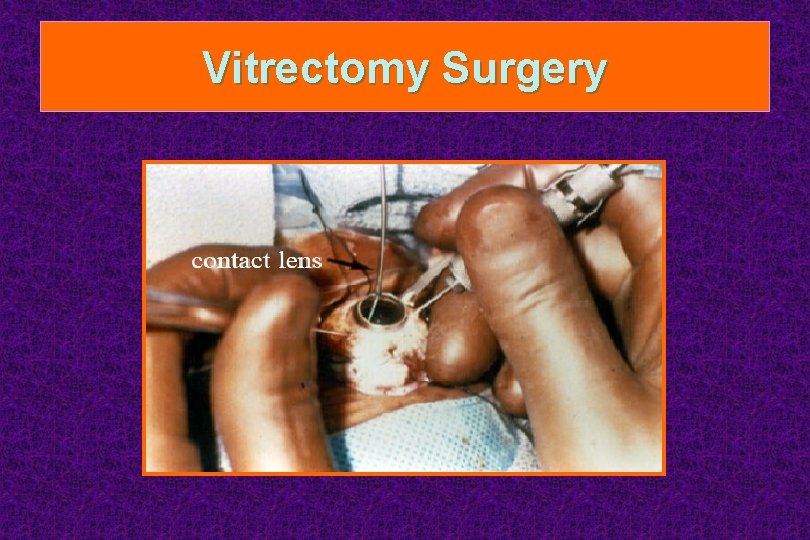
Vitrectomy Surgery

Diabetic Nephropathy
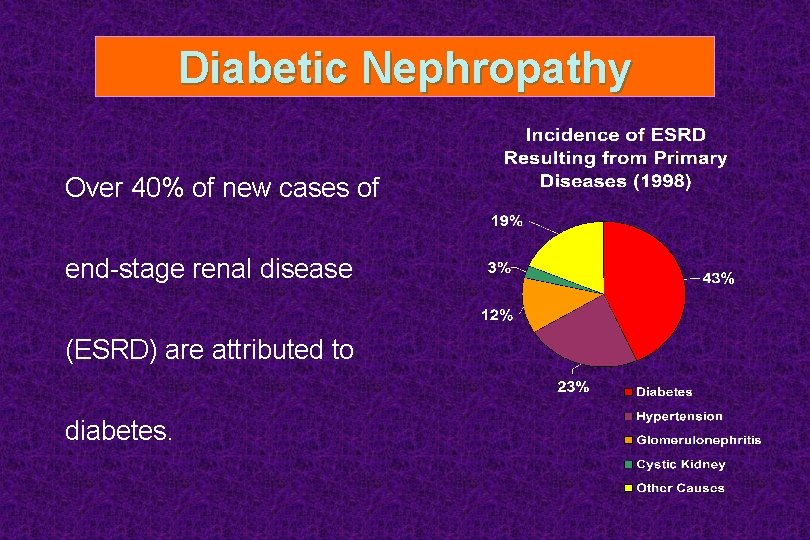
Diabetic Nephropathy Over 40% of new cases of end-stage renal disease (ESRD) are attributed to diabetes.

Nephropathy • Diabetic nephropathy is characterised by proteinuria >300 mg/24 h, increased BP, and a progressive decline in renal function. • In the early stages, overt disease is preceded by a phase known as incipient nephropathy (or microalbuminuria), in which the urine contains trace quantities of protein (not detectable by traditional dipstick testing). • Microalbuminuria is defined as an albumin excretion rate of 30 -300 mg/24 h and is highly predictive of overt

Treatment of Diabetic Nephropathy • Hypertension Control • Goal: lower blood pressure to <140/90 mm. Hg – Antihypertensive agents • Angiotensin-converting enzyme (ACE) inhibitors – captopril, enalapril, lisinopril, benazepril, fosinopril, ramipril, quinapril, perindopril, trandolapril, moexipril • Angiotensin receptor blocker (ARB) therapy – candesartan cilexetil, irbesartan, losartan potassium, telmisartan, valsartan, esprosartan • Calcium channel blockers

Treatment of Diabetic Nephropathy • Glycemic Control – Preprandial blood glucose 80 -120 mg/dl – A 1 C <6. 5% – Postprandial blood glucose <140 mg/dl – Self-monitoring of blood glucose (SMBG) – Medical Nutrition Therapy • Restrict dietary protein to RDA of 0. 8 g/kg body weight per day

Treatment of End-Stage Renal Disease There are three primary treatment options for individuals who experience ESRD: 1. Hemodialysis 2. Peritoneal Dialysis 3. Kidney Transplantation

Diabetic Neuropathy

Diabetic Neuropathy · About 60 -70% of people with diabetes have mild to severe forms of nervous system damage, including: - Impaired sensation or pain in the feet or hands - Slowed digestion of food in the stomach - Carpal tunnel syndrome - Other nerve problems · More than 60% of nontraumatic lower-limb amputations in the United States occur among people with diabetes.

Diabetic Neuropathy • Damage to nerve fibres and capillaries • Symptoms depend on nerves involved – Motor fibres → Muscular weakness – Sensory fibres → Loss of sensation • also prickling, tingling, aching and pain – Autonomic fibres → loss of function • functions not under conscious control such as digestion, bladder, genitals, cardiovascular.

Diabetic Neuropathy • Other Consequences – Diabetic foot (15% of all diabetics) – Compression neuropathies • eg carpal tunnel syndrome • Risk factors – Smoking, >40 years old, poor glucose control – Affects Type 1 and Type 2

Classification of Diabetic Neuropathy • Symmetric polyneuropathy • Autonomic neuropathy • Polyradiculopathy • Mononeuropathy

Symmetric Polyneuropathy • Most common form of diabetic neuropathy • Affects distal lower extremities and hands (“stocking-glove” sensory loss) • Symptoms/Signs – Pain – Paresthesia/dysesthesia – Loss of vibratory sensation

Complications of Polyneuropathy • Ulcers • Charcot arthropathy • Dislocation and stress fractures • Amputation

Treatment of Symmetric Polyneuropathy • Glucose control • Pain control – Alphalipoic acid – Anticonvulsants (gabapentin, pregabalin) – Tricyclic antidepressants – Topical creams • Foot care

Autonomic neuropathy • Affects the autonomic nerves controlling internal organs – Peripheral – Genitourinary – Gastrointestinal – Cardiovascular • Is classified as clinical or subclinical based on the presence or absence of

Peripheral Autonomic Dysfunction • Contributes to the following symptoms/signs: – Neuropathic arthropathy (Charcot foot) – Aching, pulsation, tightness, cramping, dry skin, pruritus, edema, sweating abnormalities – Weakening of the bones in the foot leading to fractures

Peripheral Autonomic Dysfunction • Treatment – Foot care/elevate feet when sitting – Eliminate aggravating drugs (tranquilizers, antidepressants, diuretics) – Reduce edema • midodrine • diuretics – Support stockings – Screen for CVD
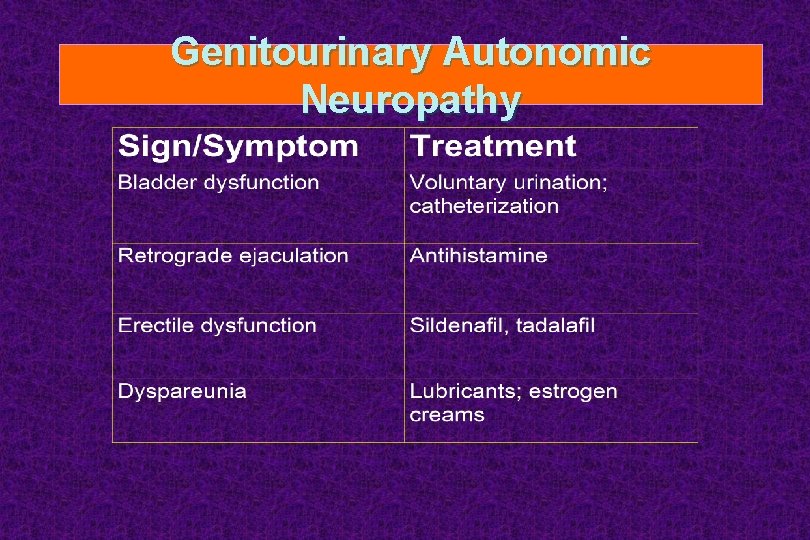
Genitourinary Autonomic Neuropathy

Gastrointestinal Autonomic Neuropathy • Symptoms/Signs – Gastroparesis resulting in anorexia, nausea, vomiting, and early satiety – Diabetic enteropathy resulting in diarrhea and constipation • Treatment – Other causes of gastroparesis or enteropathy should first be ruled out – Gastroparesis - Small, frequent meals, metoclopramide, erythromycin – Enteropathy - loperamide, antibiotics, stool softeners or dietary fiber

Cardiovascular Autonomic Neuropathy • Symptoms/Signs – Exercise intolerance – Postural hypotension • Treatment – Discontinue aggravating drugs – Change posture (make postural changes slowly, elevate bed) – Increase plasma volume

Polyradiculopathy • Lumbar polyradiculopathy (diabetic amyotrophy) – Thigh pain followed by muscle weakness and atrophy • Thoracic polyradiculopathy – Severe pain on one or both sides of the abdomen, possibly in a band-like pattern • Diabetic neuropathic cachexia – Polyradiculopathy + peripheral neuropathy

Mononeuropathy • Peripheral mononeuropathy – Single nerve damage due to compression or ischemia – Occurs in wrist (carpal tunnel syndrome), elbow, or foot (unilateral foot drop) – Symptoms/Signs • • numbness edema pain prickling

Mononeuropathy • Cranial mononeuropathy – Affects the 12 pairs of nerves that are connected with the brain and control sight, eye movement, hearing, and taste – Symptoms/Signs • • • unilateral pain near the affected eye paralysis of the eye muscle double vision • Mononeuropathy multiplex

MACROVASCULAR COMPLICATIONS
Macrovascular Complications • Angina. • Myocardial infarction. • Transient ischaemic attacks. • Cerebrovascular accident. • Claudication lower limb. • Neuropathy / infection.

Macrovascular Complications • Atherosclerotic disease accounts for most of the excess mortality in diabetes. • In the UKPDS, fatal cardiovascular events were 70 times more common than deaths from microvascular complications. • The relation between glucose concentrations and macrovascular events is less powerful than for microvascular disease; • Smoking, BP, proteinuria, and cholesterol concentration are more important risk factors for atheromatous large vessel disease in diabetes.

Macrovascular Complications • Hyperlipidaemia is no more common in well controlled type 1 diabetes than it is in the general population. • In type 2 diabetes, total and LDL concentrations are also similar to those found in non-diabetic people, but type 2 diabetes is associated with a more atherogenic lipid profile, in particular low

Macrovascular Complications • HTN affects at least half of diabetes. • In UKPDS, tight BP control (mean 144/82 mm Hg) achieved significant reductions in the risk of stroke (44%), heart failure (56%), and diabetes related deaths (32%), as well as reductions in microvascular complications (for example, 34% reduction in progression of retinopathy). One third of p’ts required three or more antihypertensive drugs to maintain a target BP <150/85 mm Hg. • In another recent study (hypertension optimal treatment study) rates of CV events in type 2 diabetes were reduced even further when combination treatment was used to aim for target diastolic BP <80 mm Hg.

Unmodifiable Risk Factors • Age >50 • Gender • Hereditary

Modifiable Risk Factors • Smoking • Inactivity • Nutrition • Obesity (BMI > 30) • Excessive smoking & alcohol intake

Medical Risk Factors • Hypertension (BP>130/80 mm. Hg) • High cholesterol • Poor glycemic control (Hb. A 1 c>7%) • Microalbuminuria

Coronary Heart Disease • The incidence and severity of coronary heart disease events are higher in diabetes, and several clinical features are worth noting. • The diabetes subgroups in the major secondary prevention studies of cholesterol reduction (Scandinavian simvastatin survival study (4 S) and cholesterol and recurrent events (CARE) trial) show a beneficial effect of statins.
Peripheral Vascular Disease • Atheromatous disease in the legs, as in the heart, tends to affect more distal vessels—for example, the tibial arteries—producing multiple, diffuse lesions that are less straightforward to bypass or dilate by angioplasty. • Medial calcification of vessels ( Mönckeberg's sclerosis ) is common

Stroke • 85% of acute strokes are atherothrombotic, and the rest are haemorrhagic (10% primary ICH , 5% SAH ). • The risk of atherothrombotic stroke is two to three times higher in diabetes, but the rates of haemorrhagic stroke and TIA are similar to those of the non-diabetic population. • Diabetes are more prone to irreversible rather than reversible ischaemic brain damage, small lacunar infarcts are common.

Stroke • Stroke p’ts with diabetes have a higher death rate and a poorer neurological outcome with more severe disability. • Maintaining good glycaemic control immediately after a stroke is likely to improve outcome, but the long term survival is reduced because of a high rate of recurrence. • Antihypertensive treatment is effective in preventing stroke.

Erectile Dysfunction • A common complication of diabetes, occurring in up to half of men aged over 50 years (compared with 15 -20% in age matched non-diabetic men), although the exact prevalance is unknown because of likely underreporting. • Pathogenesis is multifactorial, with autonomic neuropathy, vascular insufficiency, and psychological factors contributing to the clinical picture. The condition causes appreciable social and psychological problems for many p’ts, and its importance should not be underestimated. • Sildenafil, Tadalafil, which is reported to have a 50 -70% success rate in diabetes, is an important advance.

DIABETIC FOOT SYNDROME
Foot Problems and Diabetes • Neuropathy – Peripheral: loss of protective sensation – Autonomic: loss of ability to sweat – Motor: loss of structure/muscle tone • Peripheral Vascular Disease – Impaired circulation in legs and feet – Increased incidence of inflammation and infection – High risk of ulcers, gangrene and amputations when person also has neuropathy
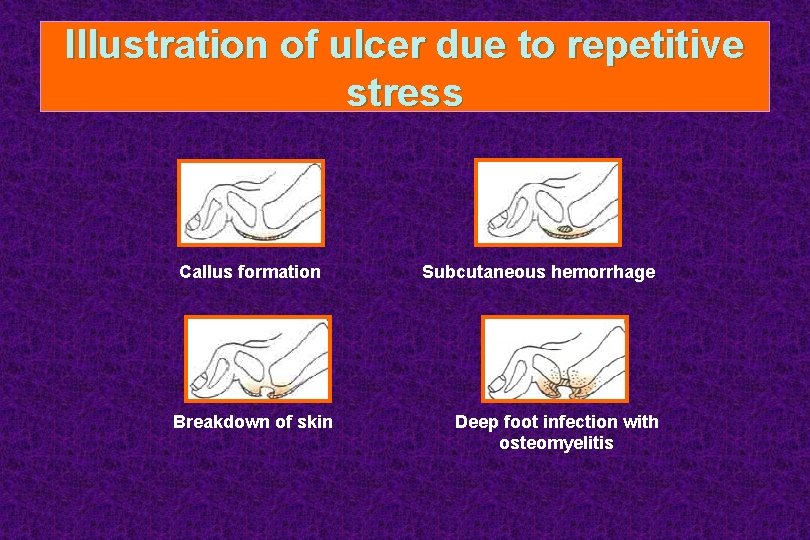
Illustration of ulcer due to repetitive stress Callus formation Breakdown of skin Subcutaneous hemorrhage Deep foot infection with osteomyelitis
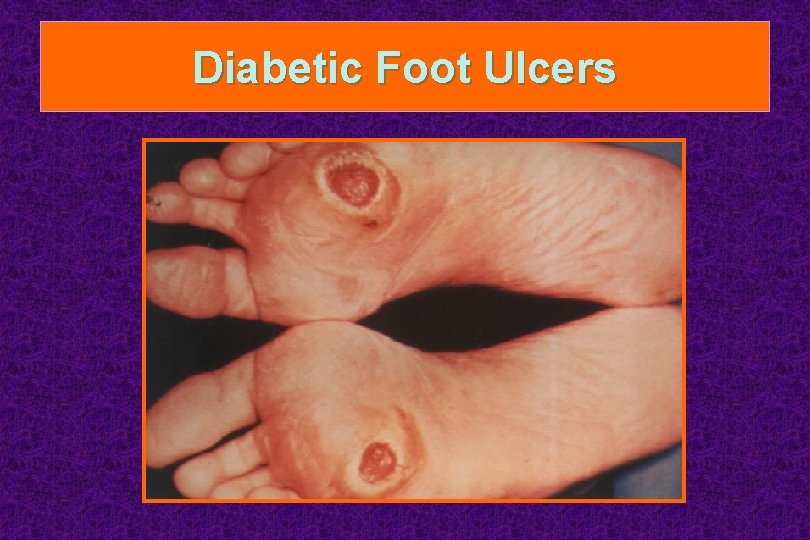
Diabetic Foot Ulcers
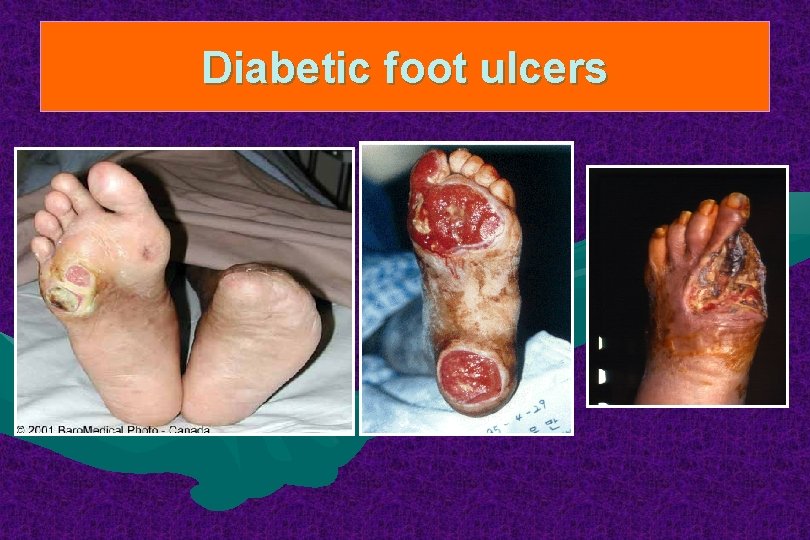
Diabetic foot ulcers
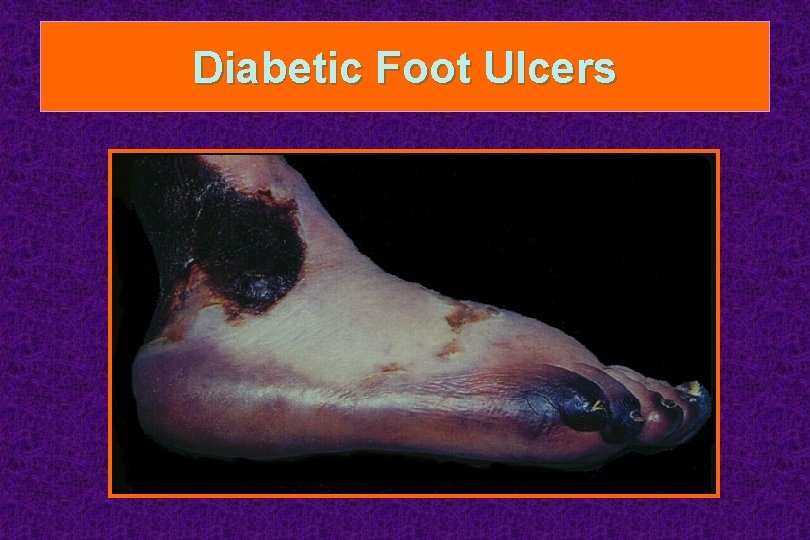
Diabetic Foot Ulcers
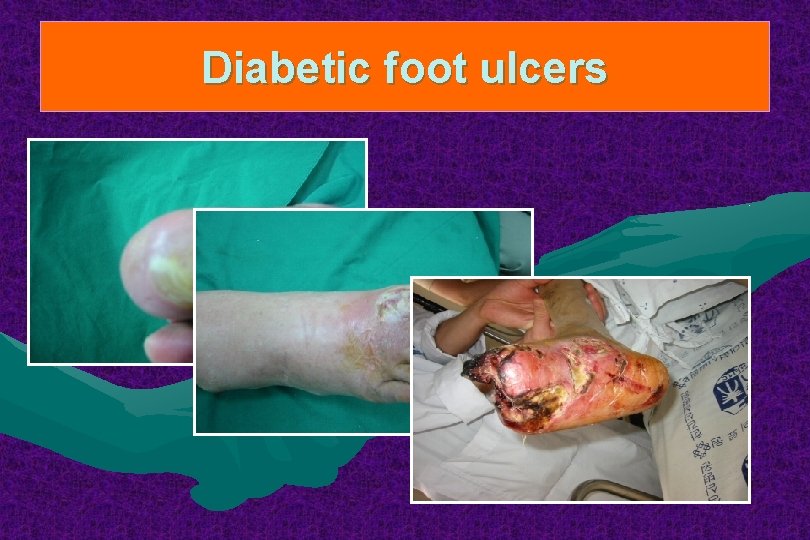
Diabetic foot ulcers

Prevention • Foot exam by a health professional at every medical visit • Comprehensive exam annually – Vascular – Musculoskeletal – Skin and soft tissue • Education

Thank You!
- Slides: 76