Complications of Adult Onset Stills Disease in a

























- Slides: 30

Complications of Adult Onset Still’s Disease in a patient presenting with fever of unknown origin Diane Mar, MD Division of Immunology & Rheumatology Stanford University Hospital & Clinics

Learning Objectives �Describe an “atypical” rash in Still’s disease �Discuss life threatening complications associated with Adult Onset Still’s Disease with a focus on secondary hemophagocytic lymphohistiocytosis �Review treatment options for Still’s disease associated with macrophage activation syndrome

Case Presentation � 50 F without significant past medical history who presents with persistent fever

Prior to admission �A week and half prior to admission she develops a sore throat with cough �The next day she takes an Advil and develops an immediate, itchy rash with scratches on her back bottom thighs �The following day she has joint pain to knees and ankles, wrist and myalgias of upper arms, thighs. �Then it goes away

�A day or two later she develops a fever �Fever comes and goes for four days �Symptoms persist so comes to the emergency room where she is admitted

ROS � � � � Fever Sore throat (resolved) Pruritic rash (resolved) Joint pain (wrist, knees ankles, resolved) Intermittent hair loss Heavy blood clots during her menstruation for 6 -8 months. Now resolved Diarrhea Short of breath No Raynaud’s No dysphagia No oral ulcers No photosensitivity No history of clotting or miscarriages No chest pain

Case Presentation PMH: � None PSH: � None Meds � Ibuprofen PRN Family Medical History: � Mother had rheumatoid arthritis Social History: � No recent travel outside the US � Never smoker, occasional alcohol � Married

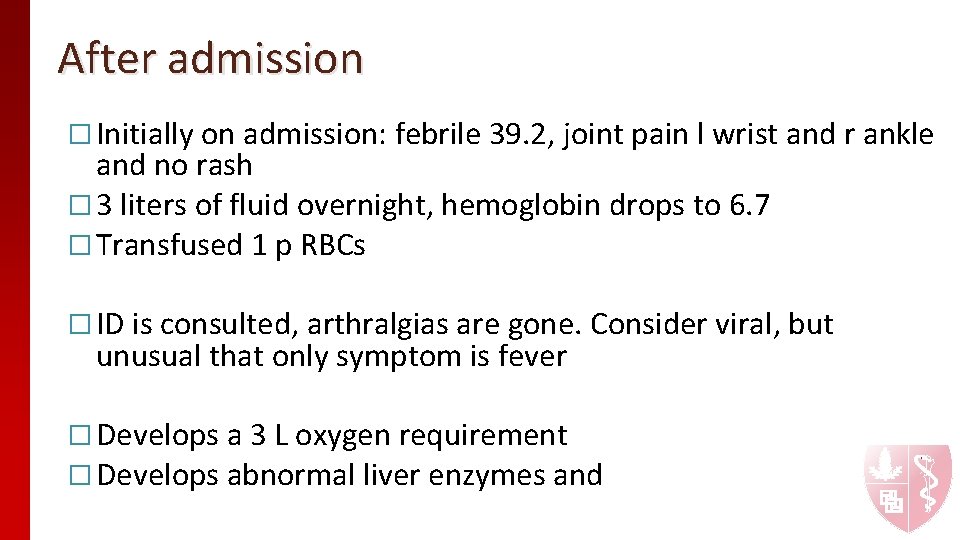
After admission � Initially on admission: febrile 39. 2, joint pain l wrist and r ankle and no rash � 3 liters of fluid overnight, hemoglobin drops to 6. 7 � Transfused 1 p RBCs � ID is consulted, arthralgias are gone. Consider viral, but unusual that only symptom is fever � Develops a 3 L oxygen requirement � Develops abnormal liver enzymes and


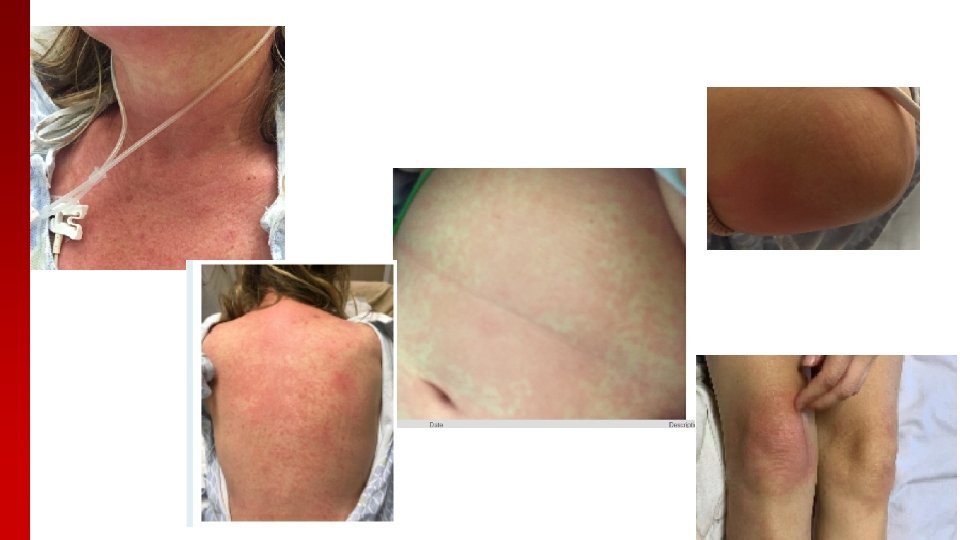
Physical Exam � � � VITALS: T 103. 1 F, HR 142, BP 131/63, RR 26, 95% on 3 L, Wt 56. 6 kg General Appearance: Uncomfortable HEENT: no oral ulcers Neck: no cervical lymphadenopathy Lungs: rales bilaterally. Tachypneic. Difficulty with full sentences Cardiac: tachycardic, no m/r/g Abdomen: soft, NT Extremities: 2+ DP pulses, no edema Neuro: A&Ox 3, Strength is 10/10 in all extremities Skin: Warm, dry. Blanchable maculopapular rash of chest, back, face and surrounding elbows MSK: full range of motion. No tenderness of joints. Small effusion in bilateral ankles, left wrist, her bilateral PIPs. No tenderness

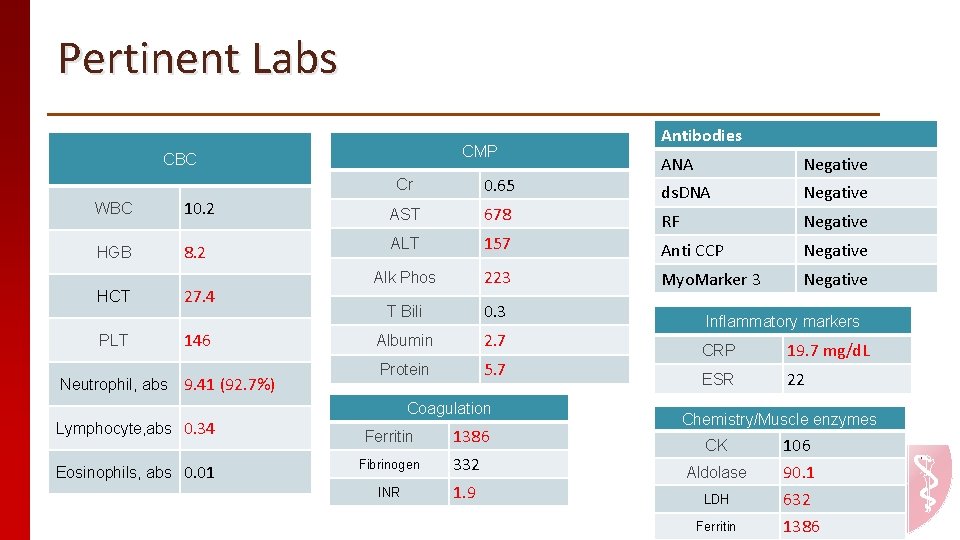
Pertinent Labs CMP CBC WBC 10. 2 HGB 8. 2 HCT PLT Neutrophil, abs 27. 4 146 9. 41 (92. 7%) Lymphocyte, abs 0. 34 Eosinophils, abs 0. 01 Antibodies ANA Negative ds. DNA Negative RF Negative Cr 0. 65 AST 678 ALT 157 Anti CCP Negative Alk Phos 223 Myo. Marker 3 Negative T Bili 0. 3 Albumin 2. 7 Protein 5. 7 Coagulation Ferritin 1386 Fibrinogen 332 INR 1. 9 Inflammatory markers CRP 19. 7 mg/d. L ESR 22 Chemistry/Muscle enzymes CK 106 Aldolase 90. 1 LDH 632 Ferritin 1386

Over a course of three days… � Ferritin 1389 38, 265 77, 735 � AST 38 4053 5525 � ALT 11 607 815 � INR 2. 2 � D-dimer>20 � fibrinogen 163 <30 � PTT – 81 � Platelets 127

Imaging CT chest, abdomen, pelvis with contrast – numerous and mildly enlarged mediastinal lymph nodes – nonspecific, trace pleural effusions with mild interstitial pulmonary edema, periportal and gallbladder wall edema, fluid filled colon suggestive of diarrheal disease with no evidence of colitis Pet scan – negative for metabolically active malignancy, Abnormally increased hypermetabolism of the spleen, nonspecific for an ongoing hematologic disorder.

ID workup Labs � Procal 24 � Quantiferon indeterminate � GI PCR negative C diff negative Respiratory panel negative Hepatitis B, C negative Mono negative, EBV test suggestive of past infection Parvovirus negative CMV negative � Blood cultures negative � � � Also negative: � Hepatitis E � Hsv � Herpes virus 6 � Herpes virus 8 � vzv � Strongyloides � Adenovirus � Phagocytophilum � Syphilis, hiv � Coxsackie

pathology �SPARSE INTERFACE DERMATITIS WITH SUPRABASAL DYSKERATOSIS �Path demonstrates shows necrotic keratinocytes within the mid to upper epidermis and mild basal vacuolar change �Could be consistent with Still’s as well as viral, drug induced

Liver biopsy �Severe hepatocellular necrosis �No evidence of viral hepatitis. No features suggestive of HLH �Can be seen in drug effect, infections, ischemic injury �Suspect an unusual manifestation of Still’s

�Hematology: given rapid rise in ferritin, concern for secondary hemophagocytic lymphohistiocytosis (HLH) as well as disseminated intravascular coagulation (DIC). �Elevated IL-2, triglycerides consistent with diagnosis �Bone marrow biopsy also shows HLH

Clinical course � She is started on dexamethasone 16 mg (85 mg prednisone) � anakinra 100 mg s. Q � Defervesces in the next day � persistent coagulopathy two days later (requiring multiple cryoprecipitate transfusions) � Once bone marrow biopsy prelim results, she is given two doses of etoposide

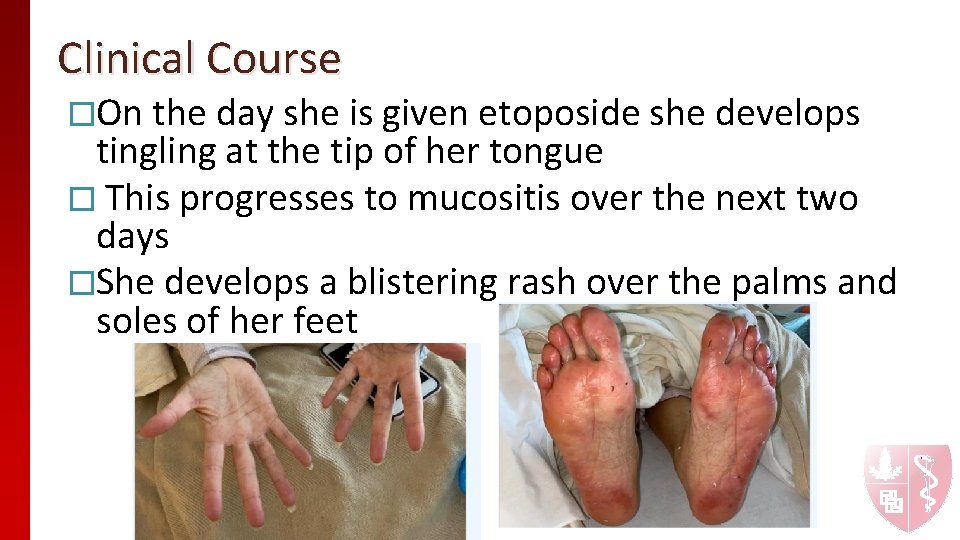
Clinical Course �On the day she is given etoposide she develops tingling at the tip of her tongue � This progresses to mucositis over the next two days �She develops a blistering rash over the palms and soles of her feet

�Dermatology evaluates and timing is not consistent with etoposide reaction and severity is out of proportion to what would be expected �Hematology and dermatology suspect Kawasaki like rash secondary to HLH �This eventually resolves with supportive care

Adult Onset Still’s Disease diagnosis � Most commonly either Yamaguchi’s criteria or Fautrel’s � Fever >39, arthralgias, leukocytosis > 10 k/neutrophilia >80% PMN, typical rash � Also: pharyngitis, splenomegaly/lymphadenopathy, liver enzyme abnormalities, ferritin < 20% glycosylated, negative RF/ANA 1– 3 � Exclusion criteria: infectious, malignancy, inflammatory disease 3 � Usually associated with a “typical” rash – evanescent, salmon-pink, nonpruitic, maculopapular � Pathology: sparse superficial, perivascular infiltrate with neutrophils and lymphocytes below a normal epidermis 41

Atypical Rash in AOSD � Most commonly: persistent, erythematous/brown, pruritic papules and plaques � Linear configuration/dermatographism 4 thought to be secondary to Koebner phenomenon � Urticaria, linchenoid like, prurigo pigmentosa-like, dermatomyositis-like, lichen amyloidosis -like, vesiculopustular eruptions, peau d’orange rashes have also been reported 1 5 � Back, chest, abdomen, face/neck 1 5 � prevalence ranges from 14 -78% depending on the study but is thought to be more common than previously thought 51

Atypical rash in AOSD �Can occur both with and without the typical rash 4 in more than half the patients 5, but usually appears concurrently with systemic symptoms 5 �Il- 6 and IL-18 possibly implicated in persistent rash 4 �Usually associated with hyperferritinemia 5

Histopathology � Singly or grouped necrotic keratinocytes in the upper epidermis and sparse superficial dermal inflammatory infiltrate (neutrophils, lymphocytes, occasional eosinophils) in absences of vasculitis, mild vacuolar involvement of basal epidermis with dyskeratotic keratinocytes, subcorneal neutrophils and nuclear dust, eosinophils are rare. Dermal mucin deposition is also seen 1, 4– 6 � Wide differential for this type of histopathology but Lee et al suggested that single or grouped necrotic keratinocytes in the upper one half of the epidermis in association with neutrophilic/lymphocytic infiltrate in the upper dermis is very distinct as opposed to other rashes with distribution in the lower epidermis and greater prominence of vacuolar alteration of the basal cells or lymphocytic infiltration 1 � This rash is commonly mistaken for a drug rash but with an atypical history and typically will have a lack of eosinophils 1

Atypical rash in AOSD �Typically resolves with steroids, but may require may potent immunosuppression 45 �Usually patients have more persistent, severe systemic signs and may raise concern for MAS, 1, 2, 4, 5 TTP or DIC. In particular, the dermatomyositis like rash may suggest a poor outcome 1

Life threatening complications � reactive hemophagocytic syndrome or macrophage activation syndrome � disseminated intravascular coagulopathy � thrombotic thrombocytopenic purpura � myocarditis, acute respiratory syndrome, tamponade, diffuse alveolar hemorrhage 2, 7 � pulmonary arterial hypertension � poor prognostic factors include rash, polyarthritis – particularly hips and shoulders, pleuritis, interstitial pneumonia, ferritin elevation, failure of fever to subside after 3 days of corticosteroid treatment 7

Macrophage activation syndrome (MAS) or reactive hemophagocytic syndrome (secondary hemophagocytic lymphohistiocytosis) 10 -22% mortality rate with a prevalence between 12 -14% in Still’s patients 7 � An uncontrollable activation of the reticulo-endothelial system with phagocytosis of hematopoietic cells by macrophages � T cell activation and proliferation with cytokine storm 1, 6, 7 � High fever, lymphadenopathy, hepatosplenomegaly, CNS dysfunction � Pancytopenia, elevated ferritin (typically >5000), triglyceridemia, liver enzyme elevation, elevated Il-2 R and low NK cell function � Early MAS: persistent fever, falling platelets, falling ESR, hyperferritinemia, increased liver enzymes, hypofibrinogenemia, hypertriglyceridemia 7, 8. Elevated AST has also been noted in patients with juvenile JIA complicated by MAS 7 �

Treatments in AOSD is associated with MAS Multiple cytokines thought to be involved. 7 � treatment has included IV corticosteroids, cyclosporine, etoposide for refractory cases 2, 7, 8 � IL-1 inhibition has also been used for treatment, such as anakinra up to 100 -200 mg daily, rilonacept, and canakinumab. 2, 7 � Il-6 – thought to track with disease 1. Toclizumab has been reported to be effective in management of associated MAS with AOSD 2, 7. � Il-18 – thought to possible be the initiating factor and tracks with disease 1. It has also been noted to have be significantly elevated in patients with MAS 7 Tadekinig alfa, a recombinant IL-18 binding protein, is currently in a trial 2, 9 � No clear data for TNF inhibitors, may be ineffective. 27 �

Conclusion �Atypical persistent and pruritic rashes can be seen in Still’s disease. Dermatopath can be helpful in identifying these rashes �Macrophage activation syndrome is one of the feared complications in Still’s disease �AOSD associated with MAS can be treated with IV steroids, cyclosporine, Il-1 inhibition, Il-6 inhibition and etoposide in refractory cases �Il-18 inhibition is a promising target for the future

Bibliography � � � � � 1. Lee JYY, Hsu CK, Liu MF, Chao SC. Evanescent and Persistent Pruritic Eruptions of Adult_Onset Still Disease: A Clinical and Pathologic Study of 36 Patients. Semin Arthritis Rheum. 2012; 42(3): 317 -326. doi: 10. 1016/j. semarthrit. 2012. 05. 003 2. Feist E, Mitrovic S, Fautrel B. Mechanisms, biomarkers and targets for adult-onset Still’s disease. Nat Rev Rheumatol. 2018; 14(10): 603 -618. doi: 10. 1038/s 41584 -018 -0081 -x 3. Mitrovic S, Fautrel B. New Markers for Adult-Onset Still’s Disease. Jt Bone Spine. 2018; 85(3): 285 -293. doi: 10. 1016/j. jbspin. 2017. 05. 011 4. Sun NZ, Brezinski EA, Berliner J, et al. Updates in adult-onset Still disease: Atypical cutaneous manifestations and associations with delayed malignancy Presented at the Medical Dermatology Society Meeting, Denver, CO, March 20, 2014. J Am Acad Dermatol. 2015; 73(2): 294 -303. doi: 10. 1016/j. jaad. 2015. 04. 063 5. Garcia FJN, Pascual M, López De Recalde M, et al. Adult-onset Still’s disease with atypical cutaneous manifestations. Med (United States). 2017; 96(11): 1 -8. doi: 10. 1097/MD. 0000006318 6. Kikuchi N, Satoh M, Ohtsuka M, Yamamoto T. Persistent pruritic papules and plaques associated with adult-onset Still’s disease: Report of six cases. J Dermatol. 2014; 41(5): 407 -410. doi: 10. 1111/1346 -8138. 12426 7. Efthimiou P, Kadavath S, Mehta B. Life-threatening complications of adult-onset Still’s disease. Clin Rheumatol. 2014; 33(3): 305 -314. doi: 10. 1007/s 10067 -014 -2487 -4 8. Lenert A, Yao Q. Macrophage activation syndrome complicating adult onset Still’s disease: A single center case series and comparison with literature. Semin Arthritis Rheum. 2016; 45(6): 711 -716. doi: 10. 1016/j. semarthrit. 2015. 11. 002 9. Gabay C, Fautrel B, Rech J, et al. clinical trial on the safety and efficacy of tadekinig alfa ( IL-18 BP ) in adult-onset Still ’ s disease. 2018: 840 -847. doi: 10. 1136/annrheumdis-2017 -212608