Complicated OSAS BY AHMAD YOUNES PROFESSOR OF THORACIC

Complicated OSAS BY AHMAD YOUNES PROFESSOR OF THORACIC MEDICINE Mansoura Faculty of Medicine Stephan Eisenschenk, MD Department of Neurology

Complication • Complication is an unfavorable evolution of a disease, or a therapy. • The disease can become : 1 - Worse in its severity ( Show a higher number of signs, symptoms ) 2 - Become widespread throughout the body or affect other organ systems ( A new disease may appear as a complication to a previous existing disease). 3 - Iatrogenic complication (drugs , devices or surgery ) may produce adverse effects by itself. 2 Stephan Eisenschenk, MD Department of Neurology

International classification of sleep disorders, criteria for OSA: Diagnosis = A + B + D or C + D A. At least one of the following applies: i. Complaints of daytime sleepiness, unrefreshing sleep , fatigue, or insomnia. ii. Awakenings with breath-holding, gasping, or choking. iii. Bed partner reports loud snoring or breathholding during the patient’s sleep. 1 V. HTN, CAD, AF, CHF, Type 2 DM, STROKE B. Polysomnography shows the following: i. Scoreable respiratory events (apneas + hypopneas + RERAs)/hr of sleep ≥ 5/hr. ii. Evidence of respiratory effort during all or a portion of each respiratory event. 3 Stephan Eisenschenk, MD Department of Neurology

International classification of sleep disorders, criteria for OSA: Diagnosis = A + B + D or C + D C. Polysomnography shows the following: i. Scoreable respiratory events (apneas + hypopneas + RERAs)/hr of sleep ≥ 15/hr. ii. Evidence of respiratory effort during all or a portion of each respiratory event. D. The disorder is not better explained by: another current sleep disorder, medical or neurologic disorder, medication use, or substance use disorder. 4 Stephan Eisenschenk, MD Department of Neurology

Grades of OSAS Mild : AHI between 5 and 14 events /h n Moderate: AHI between 15 and 29 events /h n Severe: AHI 30 events or more/hour. • OSAS is recognized as a complex and heterogeneous disorder. This heterogeneity exists in the domains of: 1 - The presenting symptoms. 2 - Physiologic etiology. 3 - Comorbid conditions. 4 - Important outcomes. n 5 Stephan Eisenschenk, MD Department of Neurology

OSAS Phenotypes • Despite this recognition, the diagnosis, assessment of severity, management of OSA remains intimately linked to a single indicator, the AHI. • Classify the disorder into smaller, more homogeneous categories , referred to as “phenotypes, ” can be based on clinical, pathophysiologic, or molecular characteristics. • Enhanced phenotyping (based on clinical, pathophysiologic, or molecular characteristics ) can improve 1 - understanding of mechanisms 2 -patient selection for clinical trials 3 - personalized treatments. 4 - prognosis 6 Stephan Eisenschenk, MD Department of Neurology

OSAS Phenotypes • The absence of a consistent definition for the term “phenotype” in some cases may also lead to lack of clarity. • Ideally, the phenotype serves as an expression of an “endotype, ” a subtype of disease defined by “a unifying and consistent 1 -natural history 2 - clinical picture 3 - pathophysiological characteristics, 4 -genetics 5 -predictable response to general and specific therapies that impact relevant patient outcomes” 7 Stephan Eisenschenk, MD Department of Neurology

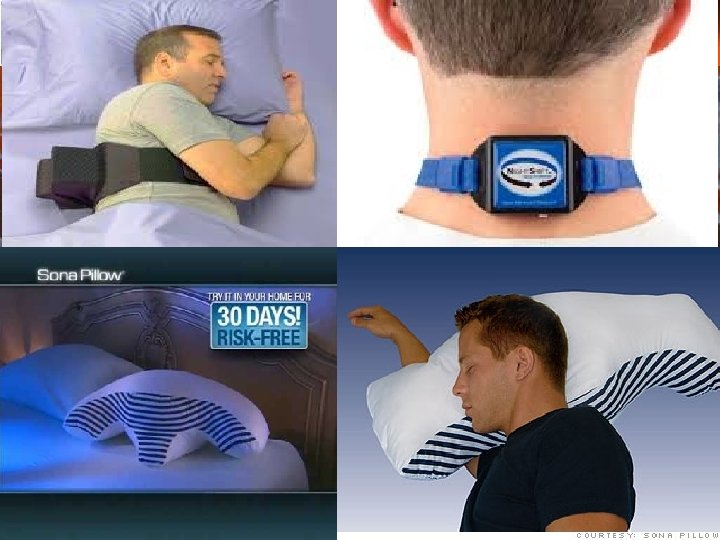
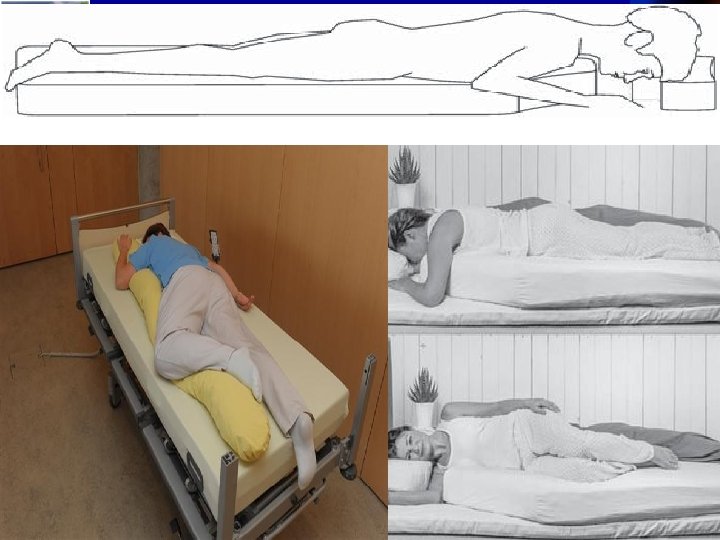
Potential clinically relevant OSA phenotypes • Patients with positional OSA (supine AHI that is at least twice that in non-supine position) tend to be younger, have lower BMI, and lower AHIs compared to their non-positional counterparts. • Short-term studies (1 month follow up) suggest that auto-set PAP use is associated with improved sleepiness and wakefulness among supine-predominant patients in comparison to CPAP , lending credence to idea that fixed PAP may not be optimal in all OSA patients with similar AHIs. • REM AHI ≥ 15 was associated with both prevalent risk of hypertension. The increased risk was present even among those with an overall AHI < 5. 8 Stephan Eisenschenk, MD Department of Neurology
Stephan Eisenschenk, MD Department of Neurology
Stephan Eisenschenk, MD Department of Neurology
11 Stephan Eisenschenk, MD Department of Neurology

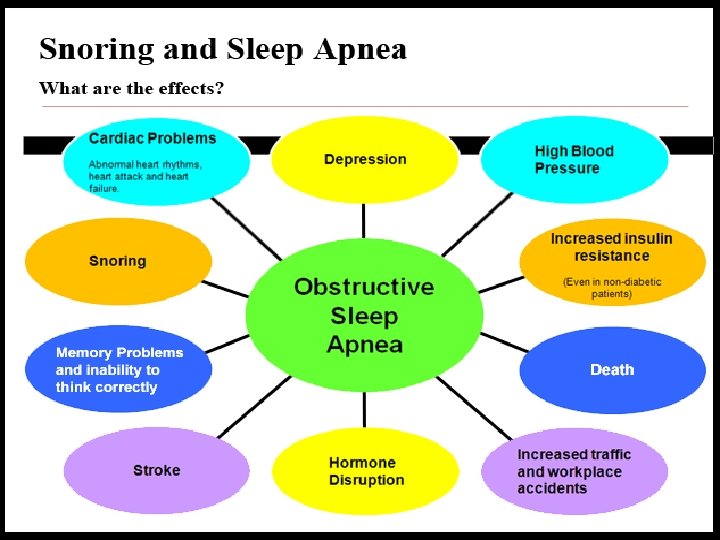
Complicated OSAS • • • Nocturnal HTN. CHF(Mixed SLEEP APNEA Syndrome). Insulin resistence. Motor car accidents. Anxiety and depression. Insomnia. GERD. Hypoventilation. Periodic limb movements of sleep (PLMS). Epiglottic collapse. Residual excessive daytime sleepiness 12 Stephan Eisenschenk, MD Department of Neurology
13 Stephan Eisenschenk, MD Department of Neurology

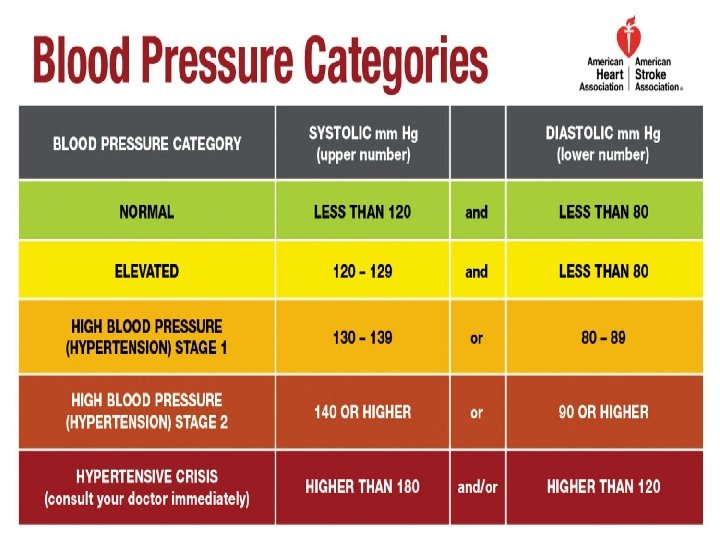
Circadian Blood Pressure Rhythm • Type of circadian BP rhythm is defined as proportion of the nocturnal average BP fall to daytime average BP value. • If it is <10%, then it is referred to as a nondipping pattern, if it is 10– 20%, it is referred to as dipping pattern. • Nocturnal average BP fall > 20% of daytime average BP values is referred to as extreme dipper pattern. • The increase instead of decrease of average BP values between average nighttime and daytime values is known as reverse dipper pattern. European Society of Hypertension (ESH) and the European Society of Cardiology (ESC). 2013 14 Stephan Eisenschenk, MD Department of Neurology

Nocturnal Hypertension • Isolated nocturnal hypertension (i. e. , nighttime BP ≥ 120/70 mm Hg and day-time <130/80 mm Hg) was associated with a higher risk of total mortality and all cardiovascular events compared with normotension. • Nighttime BP was a better predictor of outcomes than day-time, daynight BP ratio and the dipping status (Dipping , Extreme dipping , Non-dipping and Reverse-dipping). 15 Stephan Eisenschenk, MD Department of Neurology
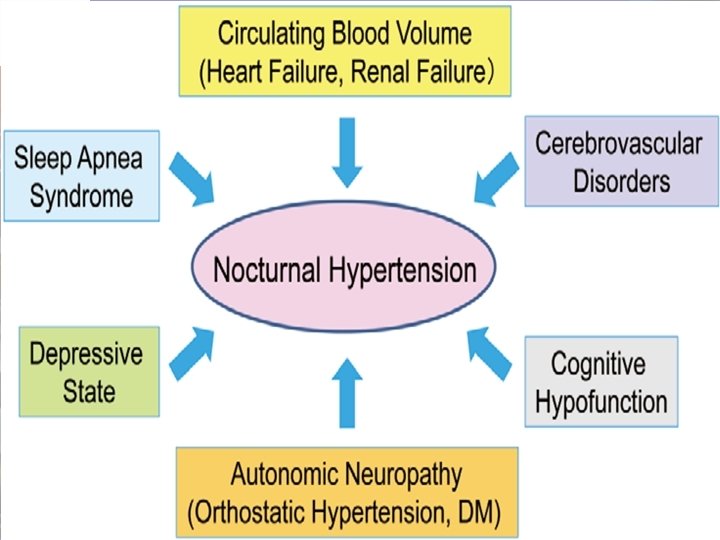
16 Stephan Eisenschenk, MD Department of Neurology

Measurement of Pulse Transit Time • An electrocardiogram and a pulse oximetry are standard techniques applied during a sleep study, and these procedures also permit the detection of the pulse wave or curve. • From these two recordings, the pulse transit time (PTT) can be estimated, thus providing continuous BP measurement. • Variations in BP can be recorded by monitoring changes in PTT. • A sudden increase in BP involves an increase in vascular tone that increases the rigidity of the arterial wall and shortens the PTT. • A reduction in BP involves a reduction in vascular tone that translates to an increase in PTT 17 Stephan Eisenschenk, MD Department of Neurology

How to Diagnose Nocturnal Hypertension • Since the speed of the pulse wave is related with arterial elasticity (which, in turn, is associated with age, vascular disease, etc. ), it is important to adjust the pulse wave speed to the BP of each subject and calibrate the measurement. For this purpose, after the PSG was arranged and set up , the patient was instructed to lie down (with a resting time of 5 min in a sitting position), and BP was measured with a sphygmomanometer on three separate occasions with an interval of at least 5 min between measurements. Measurements were taken on the arm contralateral to the one carrying the pulse oximeter (to avoid any modification in the pulse wave speed). 18 Stephan Eisenschenk, MD Department of Neurology

How to Diagnose Nocturnal Hypertension • Since the PSG recording was already in progress, when each BP measurement was obtained with the patient awake, a mark was simultaneously made on the sleep study recording so that the BP value obtained with the sphygmomanometer at that specific time could be inserted later and correlated with the PTT at the same time. • This personalized calibration method optimized measurements by monitoring the influence of the patient’s arterial rigidity. • Making three measurements provides an additional quality control by avoiding artifact areas in the calibration. 19 Stephan Eisenschenk, MD Department of Neurology

How to Diagnose Nocturnal Hypertension • From this ratio, systolic and diastolic blood pressure (SBP and DBP, respectively) can be calculated automatically throughout the whole sleep recording for each patient using the DOMINO software, version 2. 5. 0. • The next morning, a report of the SBPs and DBPs observed during the night was issued along with the PSG report, and the patient was classified as hypertensive or nonhypertensive, using the cut-off point suggested by the guidelines for nocturnal ABPM (120/70 mm. Hg). 20 Stephan Eisenschenk, MD Department of Neurology

Pulse transit time is calculated from the R wave to the midpoint of the rise of the pulse wave in the plethysmography sensor. EGG: electrocardiogram recording R-wave is identified; Plethys: plethysmographic wave recorded by pulse oximeter. 21 Stephan Eisenschenk, MD Department of Neurology

What is Mixed Sleep Apnea Syndrome? (Complex Sleep Apnea) • Mixed sleep apnea syndrome is a combination of both obstructive and central sleep apnea syndromes (obstructive AHI >central AHI and central AHI>5/H). eg. In CHF , stroke, renal failure • Some patients being treated for obstructive sleep apnea with the use of CPAP machines or Bilevel PAP without back up rate develop central sleep apnea upon PAP therapy. • Treatment: Low level CPAP , Bilevel with back up rate or adaptive servo-ventilation (anti-cyclic servo-ventilation) 22 Stephan Eisenschenk, MD Department of Neurology
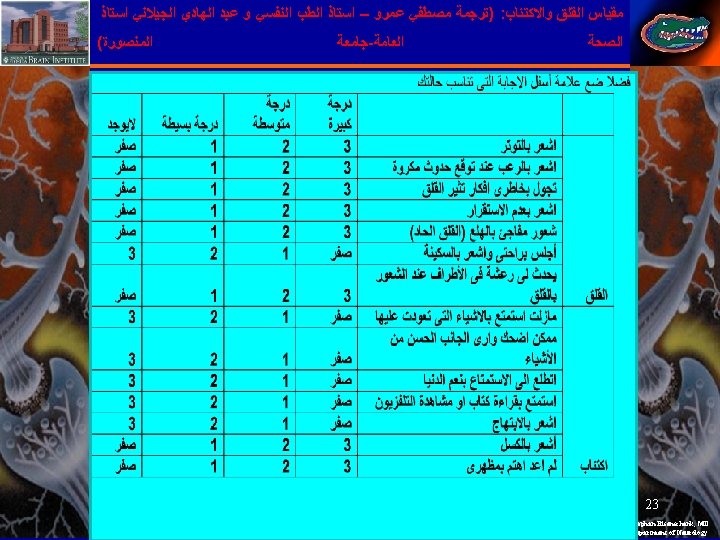

Scoring Hospital Anxiety And Depression Scale • • • Total score: Depression (D) ______ Anxiety (A) _______ 0 -7 = Normal 8 -10 = Borderline abnormal (borderline case) • 11 -21 = Abnormal (case) 24 Stephan Eisenschenk, MD Department of Neurology

What is CPAP Claustrophobia? • • If you are afraid to sleep with your CPAP mask on, or you have feelings of claustrophobia, panic attacks or anxiety with your CPAP, don't get discouraged because 11 to 28% of patients have this problem when they start the CPAP treatment. Your body's struggle to breathe every night so producing large amounts of stress hormones adrenaline - that will circulate through your body. It takes some nights of good sleep on CPAP without apnea episodes - to clear all the stress hormones out of your body. After you get used to CPAP, you'll be amazed at how much calmer you are going to feel and 25 Stephan Eisenschenk, MD Department of Neurology

Causes and Risk Factors for CPAP Claustrophobia • What kind of fears you have when you try to sleep with the CPAP mask? • Is it the idea of having something on your face? • Are you worried about strangulation from the hose by your neck? • Is it because you can't see far? • Is the weight of the CPAP mask bother you? • Do you have fear of CPAP mask from a previous experience sending you in a panic? NB. Please , be patient with the patient. 26 Stephan Eisenschenk, MD Department of Neurology

Prevalence and predictors of sleep related accidents in Egyptian commercial drivers with SRBD • There was a high prevalence of SRBD (81. 8%) , 63. 6% for OSA , 18. 2% for OHS in professional drivers attending Mansoura Sleep Disordered Breathing Unit. • Wide neck circumference (>40 cm ) was the best risk factor for SRBD. • The prevalence of one or more co-morbidities was high (67. 8%) and the risk of accident or near accident was also high 67. 8% with lower slow wave sleep% , REM sleep % and sleep efficiency% as independent predictors. (This study was supported by a grant of Egyptian academy of scientific research and technology in collaboration with Mansoura University) 27 Stephan Eisenschenk, MD Department of Neurology

GERD In OSAS • GERD occur more common in OSAS patients as compared to controls (40% versus 10%). • It is recommended for sleep specialist to inquire about GERD symptoms in patients with OSAS. • Also gastroenterologists must inquire about OSAS symptoms in patients with GERD especially those not responding to proton pump inhibitor. Gastro-esophageal reflux in obstructive sleep apnea Amr Badr-El Din, Gad El-Hak N, Younis A, Mostafa M, Mohmad Abdel-Hady 28 Stephan Eisenschenk, MD Department of Neurology

OSAS COMORBIDITIES • Hypoventilation , Daytime (Pa. Co 2>45 mm. Hg and very severe COPD, Neuromuscular diseases) and Nocturnal (end tidal Co 2 or transcutaneous Co 2 >55 mm. Hg or >50 mm. Hg provided it is >10 mm. Hg above daytime for >10 minutes) • Obstructive sleep apnoea is the largest contributory factor to the etiopathogenesis of OHS: as OSA is present in about 90%of OHS , and elimination of OSA results in eucapnia in many patients even without any significant alteration in the body mass index. 29 Stephan Eisenschenk, MD Department of Neurology
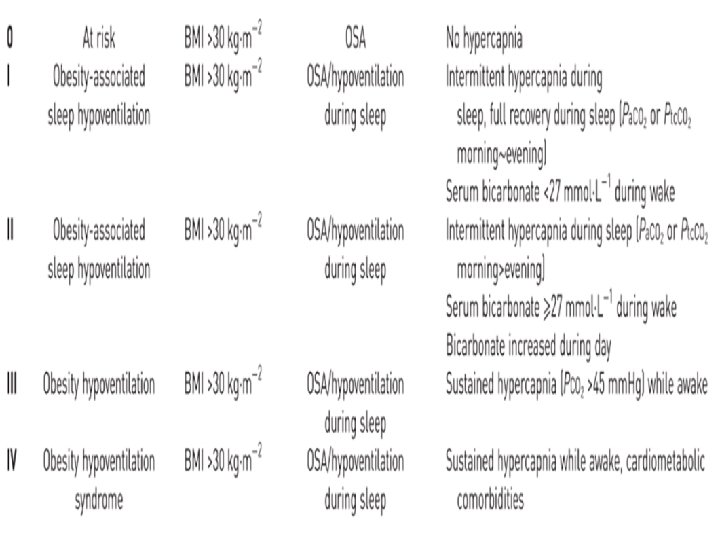
30 Stephan Eisenschenk, MD Department of Neurology

OSAS with comorbid Insomnia • OSAS and insomnia are two of the most commonly encountered sleep disorders. • The comorbidity of OSA and insomnia, also referred to as ‘Sleep apnea plus’ , and the prevalence of insomnia in sleep apnea reporting prevalence rates ranging from 7. 3% to 57. 6%. • It is well recognized that both OSA and insomnia are -independently associated with cardiovascular disease; and psychiatric disorders. • The co-occurrence of OSA and insomnia has an additive effect on the comorbidities that have been independently associated with both of these conditions. 31 Stephan Eisenschenk, MD Department of Neurology

OSAS with comorbid Insomnia • The arousals and sleep fragmentation associated with apnea can result in sleep maintenance insomnia. • The frequent complant of sleep onset insomnia associated with OSA relate to conditioning secondary to the significant sleep fragmentation associated with sleep apnea. • Roughly half of insomnia cases comorbid with these disorders when treated with CBTi reached non clinical levels of insomnia according to subjective insomnia, sleep quality, 32 Stephan Eisenschenk, MD Department of Neurology

OSAS with comorbid Insomnia • CPAP management is the mainstay of treatment for OSA, improves nocturnal breathing and decreases the arousals and awakenings associated with apnea. • CPAP can result in sleep onset insomnia related to poor mask and pressure tolerance. Less frequently, mask intolerance can result in sleep fragmentation. • Effective management of OSA requires aggressive and effective management of the insomnia related to sleep apnea and its treatments. 33 Stephan Eisenschenk, MD Department of Neurology
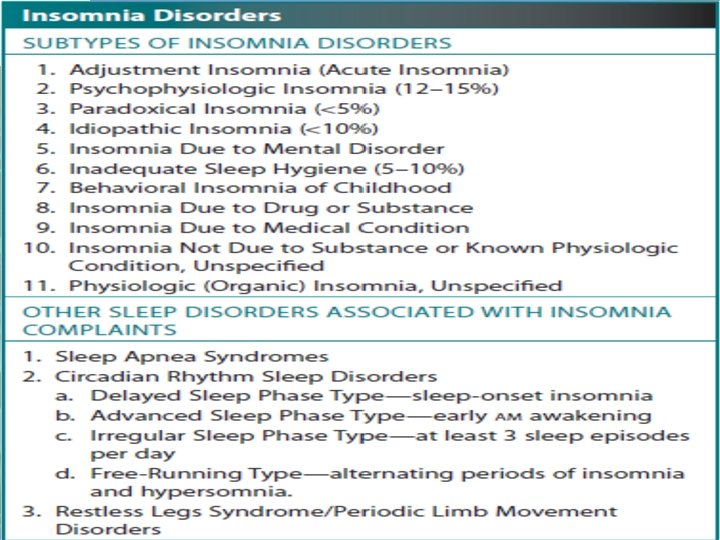
34 Stephan Eisenschenk, MD Department of Neurology
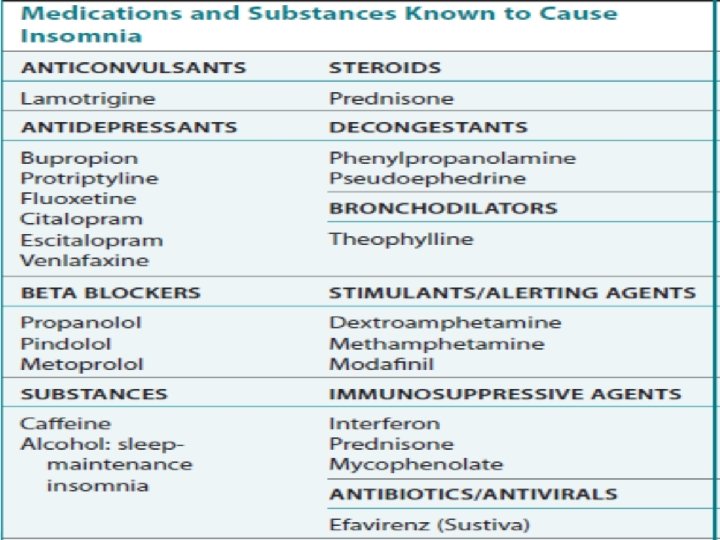
35 Stephan Eisenschenk, MD Department of Neurology

36 Stephan Eisenschenk, MD Department of Neurology

“Z”hypnotics • The new non benzodiazepine BZRAs (zolpidem, zaleplon, eszopiclone), known as the “Z” hypnotics, have less anxiolytic and myorelaxant activity compared with BZs. • zaleplon (SIESTA), Zolpidem (ZODIUM), and Eszopiclone(night calm) ARE non-BZ BZRA AND has less tolerance, respiratory depression, and rebound insomnia compared to BZs. • zolpidem and zaleplon have minimal anxiolytic or muscle relaxant activity, Eszopiclone appears to have more anxiolytic effects. 37 Stephan Eisenschenk, MD Department of Neurology
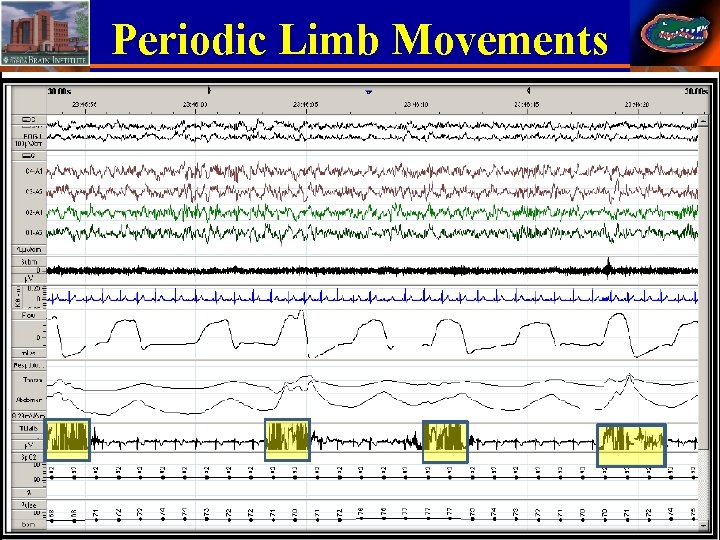
Periodic Limb Movements 38 Stephan Eisenschenk, MD Department of Neurology
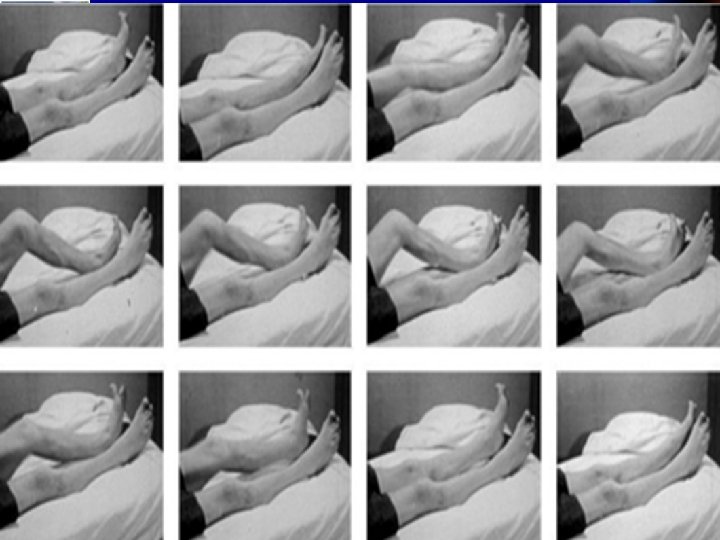
39 Stephan Eisenschenk, MD Department of Neurology
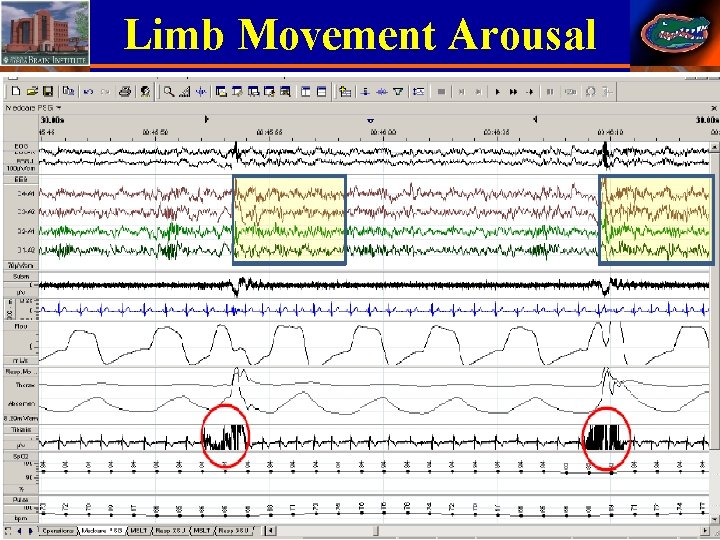
Limb Movement Arousal 40 Stephan Eisenschenk, MD Department of Neurology
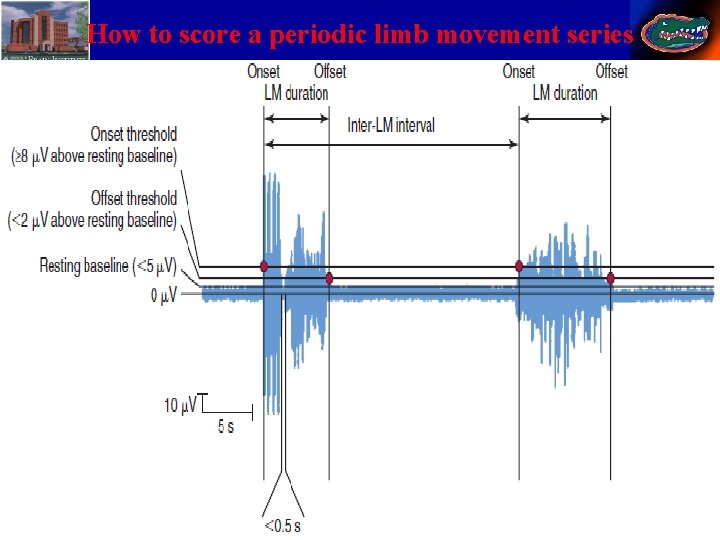
How to score a periodic limb movement series 41 Stephan Eisenschenk, MD Department of Neurology

Recommended movement events • Number of Periodic limb movement of sleep (PLMS) with arousals. • PLMS index (PLMSI) = PLMS x 60 / total sleep time. • PLMS arousal index (PLMSAr. I) = PLMS with arousal x 60 / total sleep time. • PLMS>15/hour + symptoms is pathologic. 42 Stephan Eisenschenk, MD Department of Neurology
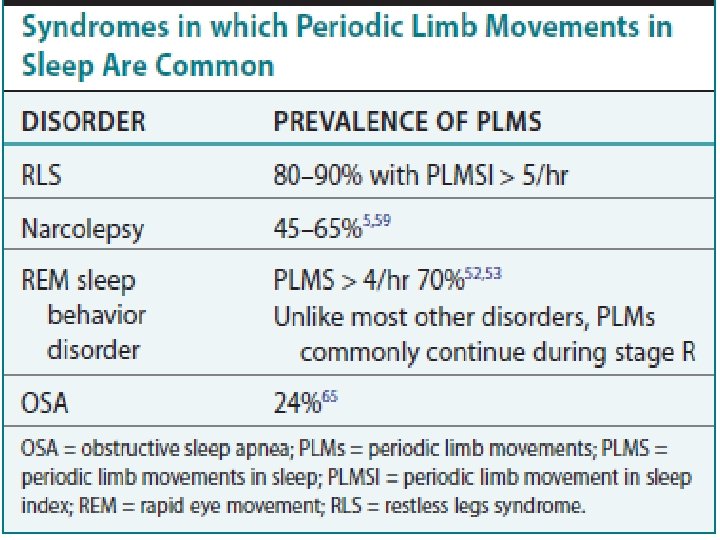

43 Stephan Eisenschenk, MD Department of Neurology

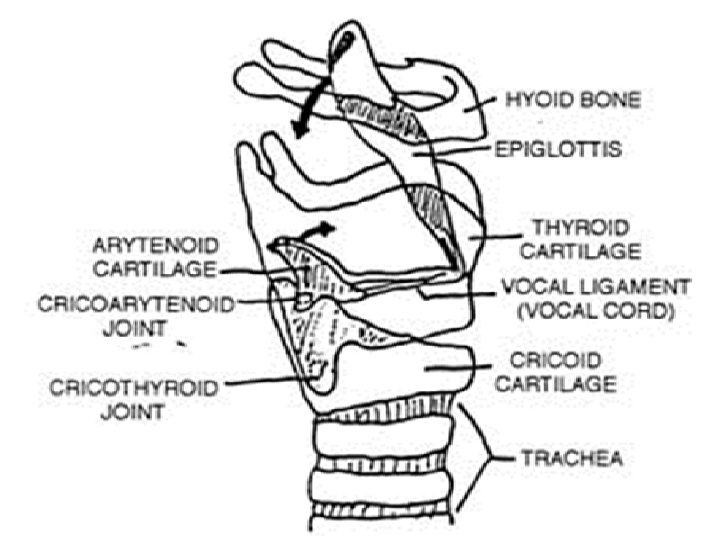
Epiglottic Prolapse • Epiglottis prolapse during inspiration is an unusual cause of airway obstruction and a rare cause of OSA. The epiglottis can be seen large and floppy closing like a door over the laryngeal inlet during inspiration. • In laryngomalacia the entire larynx collapses including the epiglottis. • These patients cannot tolerate CPAP, their obstruction gets worse and suffocated while wearing CPAP. In fact CPAP therapy is contraindicated in laryngeal OSA. 44 Stephan Eisenschenk, MD Department of Neurology
45 Stephan Eisenschenk, MD Department of Neurology

Laryngomalacia • Laryngomalacia, is a congenital abnormality of the laryngeal cartilage. • It is a dynamic lesion resulting in collapse of the supraglottic structures during inspiration, leading to airway obstruction. • It is thought to represent a delay of maturation of the supporting structures of the larynx. • Laryngomalacia is the most common cause of congenital stridor and is the most common congenital lesion of the larynx. 46 Stephan Eisenschenk, MD Department of Neurology
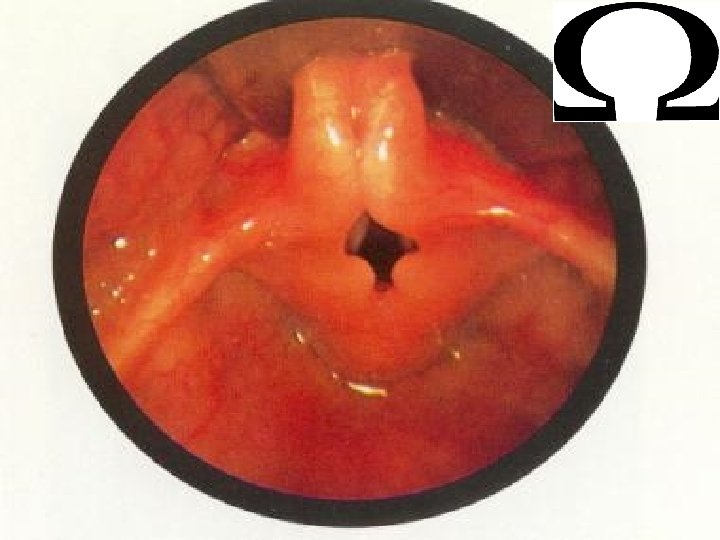
47 Stephan Eisenschenk, MD Department of Neurology
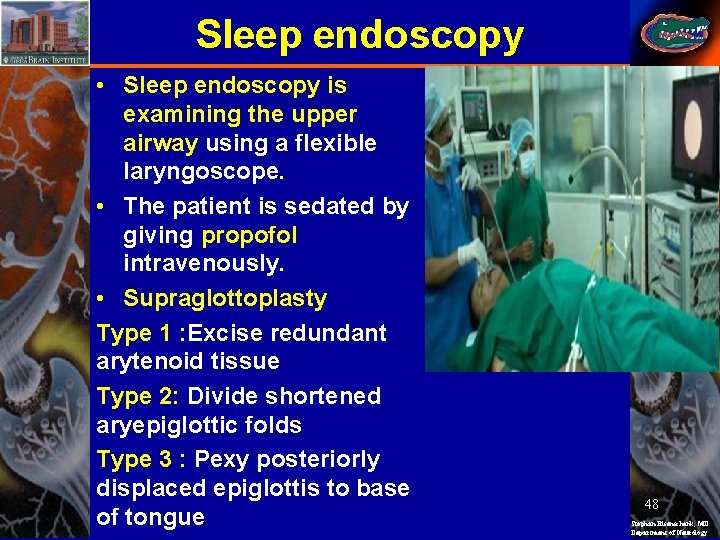
Sleep endoscopy • Sleep endoscopy is examining the upper airway using a flexible laryngoscope. • The patient is sedated by giving propofol intravenously. • Supraglottoplasty Type 1 : Excise redundant arytenoid tissue Type 2: Divide shortened aryepiglottic folds Type 3 : Pexy posteriorly displaced epiglottis to base of tongue 48 Stephan Eisenschenk, MD Department of Neurology

Residual Excessive Daytime Sleepiness • Residual excessive sleepiness (RES) is common (43. 4%) in compliant patients with OSAS on CPAP. • The predictors for the occurrence of RES on CPAP are younger age (54. 15 10. 1 versus 59. 23 10. 7 and P-value 0. 001)) , higher baseline ESS and lower CPAP usage percent. • The recommended use of CPAP for resolution of RES is >7 hours for >97% of nights 49 Stephan Eisenschenk, MD Department of Neurology

Residual Excessive Daytime Sleepiness • The commonest causes of RES are 47. 2 without PLMS (Depression , Insomnia , BIISS, RLS, shift work disorder, drug induced somnolence and rarely narcolepsy) followed by 45. 9 with PLMS (RLS, PLMD, and rarely narcolepsy) followed by 6. 9% of unknown cause of RES. Predictors for residual excessive sleepiness in patients with OSAS on CPAP. Epthal M D, . Panagis D, Rexford M , Ahmad Y, Mohammad S, Adrian. J. Egyptian Journa of chest diseases and tuberculosis , 2019 50 Stephan Eisenschenk, MD Department of Neurology

51 Stephan Eisenschenk, MD Department of Neurology
- Slides: 51