Compliance with Section 1557 of the Affordable Care

Compliance with Section 1557 of the Affordable Care Act (ACA) When Caring for Limited English Proficiency (LEP) and Trans Patients 1

Introduction Sarah Hesler, CMI, Language Services Manager University of Kentucky, UK Health. Care Pronouns: She, Hers Catherine Masoud, CHPC, Compliance Manager Office of Corporate Compliance University of Kentucky, UK Health. Care Pronouns: She, Hers 2

026771998 Disclosure • We are NOT attorneys! • This presentation is intended to provide general information on regulations, policies, and procedures related to caring for patients with diverse identities, cultures, and backgrounds. • The views and opinions included in this presentation are solely those of the presenters and do not necessarily represent the views or opinions of their associated entity. • We have no relevant financial or nonfinancial relationships to disclose. 3

Objectives • Define Section 1557 of the Affordable Care Act (ACA) • Describe areas of focus relevant to individuals who identify with multiple, overlapping social categories • Demonstrate interpersonal and system-level factors that contribute to health disparity • Discuss inclusive possibilities as well as challenges when caring for LEP and trans patients 4

What is Section 1557? It is the nondiscrimination provision of the Affordable Care Act (ACA). It prohibits discrimination on the basis of race, color, national origin, sex, age or disability in certain health programs and activities. 5

Builds on long-standing and familiar Federal civil rights laws • Title VI of the Civil Rights Act of 1964 – prohibits discrimination on the basis of race, color, and national origin in programs and activities receiving federal funding. Requirements state “no one” in the United States shall: § Be excluded from participation in § Be denied the benefits of; or § Be subjected to discrimination • Title IX of the Education Amendments of 1972 • Section 504 of the Rehabilitation Act of 1973 • Age Discrimination Act of 1975 6

Codified at 42 U. S. C. § 18116 Section 1557 statute extends nondiscrimination protections to individuals participating in: • Any health program or activity, any part of which receives funding from HHS • Any program or activity that HHS administers under Title I of the ACA, such as the Federally-facilitated Marketplace • Health Insurance Marketplaces and all plans offered by insurers that participate in those Marketplaces 7

Notable provisions as originally published • Section 1557 is the First Federal civil rights law to broadly prohibit sex discrimination in health programs and activities • HHS clarified that sex discrimination includes, but is not limited to, discrimination based on an individual’s sex, including pregnancy, related medical conditions, termination of pregnancy, gender identity and sex stereotypes • Cannot deny or limit sex-specific health services 8

Important Dates for Section 1557 • Section 1557 has been in effect since its enactment in March 2010 and HHS Office for Civil Rights has been enforcing the provision since it was enacted. • The Office for Civil Rights (OCR) final regulation implementing Section 1557 was published in the Federal Register on May 18, 2016 9

Regulation and Litigation • December 2016 Texas federal court blocks HHS from enforcing gender identity and pregnancy termination provisions • June 2019 Notice of Proposed Rulemaking, among other things proposed to repeal the 2016 Rule’s definition of “on the basis of sex” in its entirety • October 2019 Texas federal court issues final decision vacating gender identity and pregnancy termination provisions in 2016 rule (Franciscan Alliance v. Azar) • January 2020 Franciscan Alliance plaintiffs seek to have entire 2016 rule set aside in 5 th Circuit appeal 10

Regulation and Litigation • June 2020 Trump administration issues final regulations • June-July 2020 five (5) lawsuits filed challenging Trump administration regulations • August 2020 NY federal court blocks administration from implementing provisions eliminating sex stereotyping in 2020 rule (Walker v. Azar) • September 2020 DC federal court blocks administration from implementing provisions eliminating sex stereotyping and adopting religious exemptions in 2020 rule (Whitman-Walker v. HHS) 11
Regulation and Litigation Four and a half years of fluid regulatory interpretations and litigation “on the basis of sex” 12

Key Dates for Regulation and Litigation • Most recent on January 19, 2021, the U. S. District Court for the District of North Dakota Eastern Division issued an Order in the consolidated cases of (Religious Sisters of Mercy v. Azar, and Catholic Benefits Association v. Azar) citing Religious Freedom Restoration Act and entitles plaintiffs to permanent injunctive relief from the provision of coverage of gender-transition procedures under Section 1557 13

Focus Our Focus is on: • Sex as it relates to LGBTQ* • National origin as it relates to Limited English Proficiency (LEP) • Disability as it relates to Deaf and hard of hearing “NONDISCRIMINATION ON THE BASIS OF RACE, COLOR, NATIONAL ORIGIN, SEX, AGE, OR DISABILITY IN HEALTH PROGRAMS OR ACTIVITIES RECEIVING FEDERAL FINANCIAL ASSISTANCE AND PROGRAMS OR ACTIVITIES ADMINISTERED BY THE DEPARTMENT OF HEALTH AND HUMAN SERVICES UNDER TITLE I OF THE PATIENT PROTECTION AND AFFORDABLE CARE ACT OR BY ENTITIES ESTABLISHED UNDER SUCH TITLE” 14

Challenges of Operationalizing • Frequent Changes • Staying informed • Updating policies and procedures • Training and education • Unconscious bias, prejudice, preference or intolerance • Maintaining accurate materials (print and on-line) 15

Limited English Proficiency, Deaf, and Hard of Hearing Considerations: • Safety and quality in health care requires clear communication between patients and providers. Clear provider-patient communication is essential for patient centeredness. • Level, type and manner of language assistance is dependent on the relevant facts, which may include the operations and capacity of the covered entity. 16

Capability, Requirement, and Procedure • The ability to enter patient’s preferred language in EHR. • TJC requires preferred language to be captured at registration. • Section 1557 requires qualified medical interpreters and information written in other languages. • Identify patient’s preferred language as soon as possible • Enter preference in EHR • Contact Language Services for interpreter or use available tools • Post on white board, add visible flag on chart and door 17

Examples of EHR Capability 18

Requirements for Language Access Covered entities must provide meaningful access for individuals with limited English proficiency. Language assistance services must: • Be provided free of charge to the individual • Be accurate and timely • Protect the privacy and independence individual 19

Requirement – Language Assistance A covered entity must adhere to certain quality standards in delivering language assistance services. For instance, a covered entity may not: • Require an individual to provide his or her own interpreter. • Rely on a minor child to interpret, except in a life threatening emergency where there is no qualified interpreter immediately available. • Rely on interpreters that the individual prefers when there are competency, confidentiality or other concerns. • Rely on unqualified bilingual or multilingual staff. • Use low-quality video remote interpreting services. 20

Requirement – Taglines • Covered entities are required to post taglines in the top 15 languages spoken by individuals with limited English proficiency for the state that indicate the availability of language assistance ATTENTION: If you speak [Bengali], language assistance services, free of charge, are available to you. 21

Tools and Solutions Use different tools or interpreting modalities for a system-wide approach • Video remote interpreting (VRI) – VRI mobile units • Phone interpreting access incorporated into communication platforms like paging systems or intra-web networks (Vocera, Voalte) • Dedicated staff phone interpreters for high volume languages • Directed calls for high volume languages, dedicated incoming call lines 22

Tools and Solutions • Recorded prompts in multiple languages for imaging machines • Dubbed videos for patient education • In-language texts and appointment reminders • Combine on-site staff interpreting with video and phone interpreting for comprehensive language access 23

Examples Interpreting services may include on-site as well as remote services for phone and video Services should be adapted for changing workflows: • Telehealth outpatient visits • Hospital rounding • Clinic appointments • Follow-up phone calls for lab results and post-discharge checks 24
Balancing Activities VRI In person 25

Written Translations • Essential documents must be completed by a qualified translator, but is not the only method of ensuring clear communication. • Auxiliary tools and visual aids may support effective communication. 26

Another Reason • Effective communication results in better health outcomes* • Communication barriers for LEP patients result in longer hospital stays and higher rates of readmission without interpreters. • LEP patients have higher rates of adverse events and poorer outcomes than English-speaking patients. v The Joint Commission: Advancing Effective Communication, Cultural Competence, and Patient-and Family. Centered Care: A Roadmap for Hospitals. Oakbrook Terrace, IL: The Joint Commission, 2010. v US Dept. of Health and Human Services, Improving Patient Safety Systems for Patients With Limited English Proficiency, Agency for Healthcare Research and Quality, 2012. 27

Social Determinants of Health “These social structures and economic systems include the social environment, physical environment, health services, and structural and societal factors. ”-CDC Bathrooms are just the beginning Communicating with patients is essential 28

Safe, Inclusive and Patient-Centered Care • Hospitals and clinics where all patients feel welcome can better meet their patients’ needs. • Collect SO/GI data as part of the registration process. • Apply proper codes to medical claims and be able to prove medical necessity. • Move beyond the checkbox and use data to identify gaps in care and disparities faced by LGBTQ* patients. • Clinicians – considerations related to care and treatment • Non-clinical staff – communicating with patients • Patients – it is important to communicate information 29

Trans patients • The World Professional Association for Transgender Health recommends medical documentation include preferred name, gender identity and pronoun preference as well as an inventory of medical transition history and current anatomy. • The American Medical Association’s (AMA) House of Delegates approved a policy that will encourage electronic health record (EHR) vendors to modify their systems to be more inclusive for transgender patients. 30

Capability, Policy and Procedure • The ability to register patient with legal and preferred name • EHR functionality (male, female, non-conforming, or transgender) • Use of alias, requirements for incorporating preferred name • Use preferred name gender for communicating with patient 31
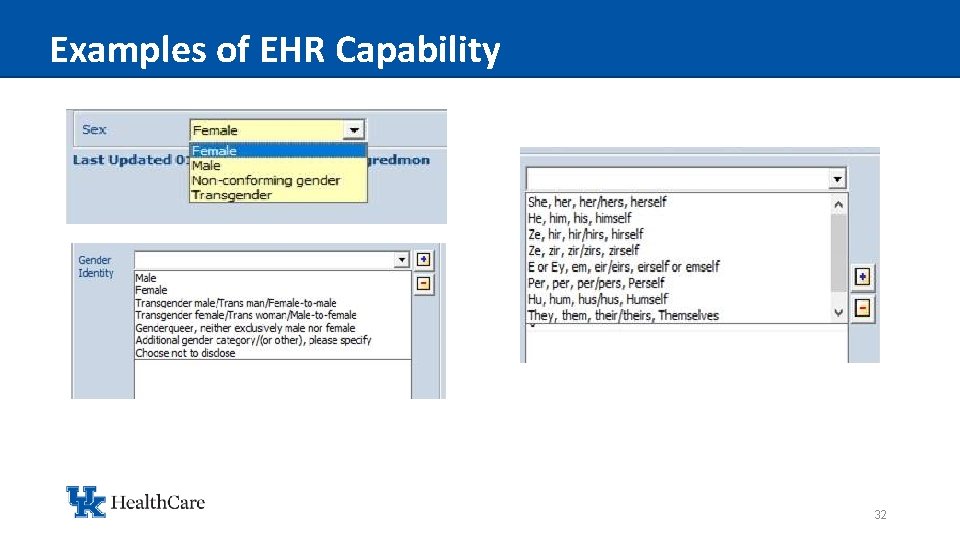
Examples of EHR Capability 32

LGBTQ* Healthcare 101 “Heterosexism is an assumption made by individuals and by larger societal institutions (the law, medicine, healthcare, education, etc. ) that all people are heterosexual, and that only heterosexual relationships are natural” • No one asked/it was assumed I was straight and/or cisgender • The forms I filled out had no spot for gender identity or sexual orientation • Fear of being discriminated against, receiving poor quality treatment, or being refused treatment • Unsure if it’s safe to come out to healthcare provider • Past negative encounters with healthcare providers 33

LGBTQ* Health Disparities • LGBTQ* • youth are more likely to attempt suicide, experience victimization and homelessness. • elderly face additional disparities due to isolation and lack of social services • as a whole have higher rates of tobacco, alcohol, and other substance abuse • Lesbian individuals are less likely to get cancer screenings • Lesbian & bisexual individuals are more likely to be overweight or obese • MSM higher risk of contracting HIV or other STI’s, especially among communities of color • Transgender individuals experience an increased risk of violence, victimization, HIV/STI’s, suicide attempts and mental health issues. 34

LGBTQ* Health Disparities • Health care providers are often unfamiliar with the queer and non-binary community and do not know how to discuss their unique needs. There is little research into their specific and unique health care needs. • Queer & non-binary individuals face disparities based on lack of understanding both within and outside of the community. They are often required to place themselves into a box or gender binary where they do not feel they belong either because they identify as both make and female or neither. 35

Gender Myths – change / include culture myths • You can tell someone is transgender just by looking at them. • All transgender people want to have surgery. • All transgender people identify as a man or woman. • All transgender people and change their name. • All transgender people have known since early childhood. • Transgender people cannot be heterosexual or straight. • It’s okay to “out” someone to others as transgender. 36

Sex / Gender / Sex Stereotypes • Sex refers to a person's biological status and is typically categorized as male, female or intersex. There a number of indicators of biological sex, including sex chromosomes, gonads, internal reproductive organs and external genitalia. • Gender identity means an individual's internal sense of gender, which may be male, female, neither, or a combination of male and female. • Sex stereotypes means stereotypical notions of masculinity or femininity. 37

Sexual Orientation ≠ Gender Identity § Distinct concepts § Sexual Orientation: “An inherent or immutable enduring emotional, romantic or sexual attraction to other people” § Gender Identity: “One’s innermost concept of self as male, female, a blend of both or neither – how individuals perceive themselves and what they call themselves. One's gender identity can be the same or different from their sex assigned at birth” 38

Effective Communication is Important! • Gender Inclusive Descriptors: Partners • Sexual Orientation • Gender Identity • Could you describe… • Please tell me about… • How would you like to be called… • Pronouns: binary, singular they, nouns vs. pronouns 39

Best Practice • Don’t assume! Ask patients what they prefer to be called and ask who is in the room with them. Use the terms that they use. • Use gender inclusive pronouns until you know a patient’s pronouns. • Create an environment of accountability with co-workers. • If you make a mistake, a quick sincere apology can help diffuse the situation. • Seek opportunities for additional trainings. 40

Summarily • Laws have changed and will most likely change again. • Healthcare facilities adjust accordingly and align policies to comply. • Some entities may have policy and procedure that is more expansive than Section 1557 requires. • We believe: • In order to provide safe, inclusive and compliant patient-centered care, you must communicate effectively. • As healthcare professionals we are allies and advocates for patients. 41

Questions 42

Contact Information Sarah Hesler (859) 218 -0455 sarah. hesler@uky. edu Catherine Masoud (859) 218 -5748 catherine. masoud@uky. edu 43

References • American Psychological Association. (n. d. ). Definitions related to sexual orientation and gender diversity in APA documents. Retrieved from https: //www. apa. org/pi/lgbt/resources/sexuality-definitions. pdf • Centers for Disease Control and Prevention. (2014). NCHHSTP Social Determinants of Health. Retrieved from https: //www. cdc. gov/nchhstp/socialdeterminants/definitions. html • Healthy People 2020. (2014). Lesbian, gay, bisexual, and transgender health. Retrieved from https: //www. healthypeople. gov/2020/topics-objectives/topic/lesbian-gay-bisexual-and-transgender-health • Human Rights Campaign. (2018). Glossary of terms. Retrieved from https: //www. hrc. org/resources/glossary-ofterms#stq=gender&stp=1 • Lavender Health. (n. d. ). Articles. Retrieved from https: //lavenderhealth. org/articles/ • Lavender Health. (n. d. ). Frequently asked questions about LGBTQ education. Retrieved from https: //lavenderhealth. org/education/faqs/ • National LGBT Health Education Center. (2015). Providing welcoming services and care for LGBT people. Retrieved from https: //www. lgbthealtheducation. org/wp-content/uploads/Learning-Guide. pdf • National LGBT Health Education Center. (n. d. ). Resources and suggested readings. Retrieved from https: //www. lgbthealtheducation. org/lgbt-education/lgbt-health-resources/#top • University of Colorado (n. d. ). Pronouns 101. Retrieved from https: //www. uccs. edu/lgbtresourcecenter/pronouns-101 44

Thank you!
- Slides: 45