Complex tibial plateau fractures AO Trauma Advanced Principles

Complex tibial plateau fractures AO Trauma Advanced Principles Course

Learning objectives • Assess complexity and outline a staged approach to treating soft tissues • Define the role of damage control and describe definitive surgery • Compare the pros/cons of conventional and locked plating, single or dual plating, and the role of indirect reduction • Evaluate the role of bone graft substitutes for periarticular defects • Identify common complications • List key outcome publications

Principles for soft-tissue management • Staged treatment of a tibial plateau fracture is better than an infected one • A malunited tibial plateau fracture is easier to manage than a stiff knee
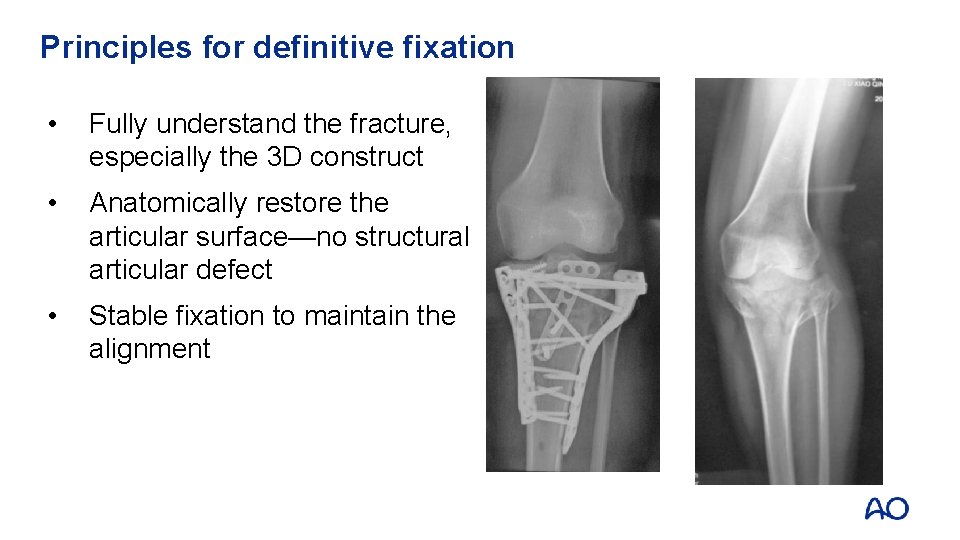
Principles for definitive fixation • Fully understand the fracture, especially the 3 D construct • Anatomically restore the articular surface—no structural articular defect • Stable fixation to maintain the alignment
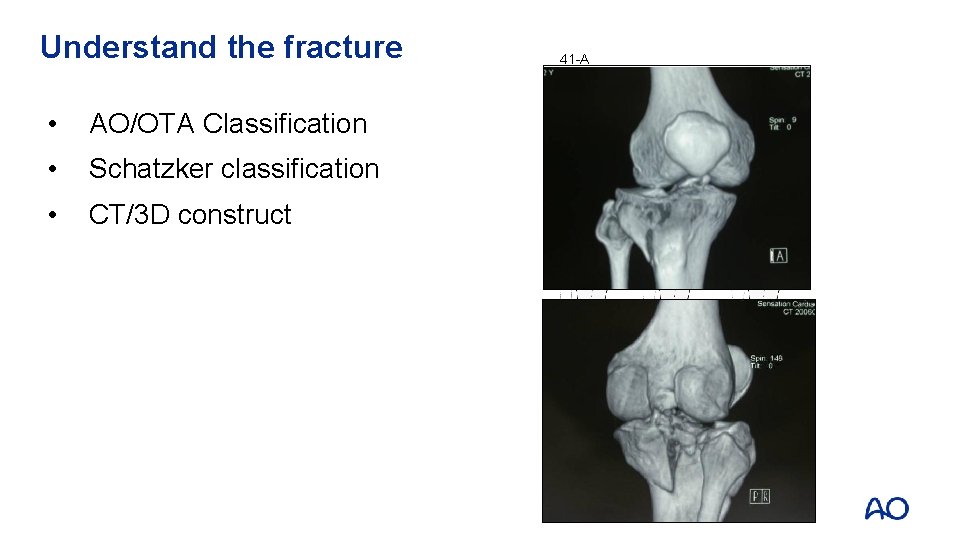
Understand the fracture • AO/OTA Classification • Schatzker classification • CT/3 D construct 41 -A A 1 A 2 A 3 B 2 B 3 C 2 C 3 41 -B B 1 41 -C C 1
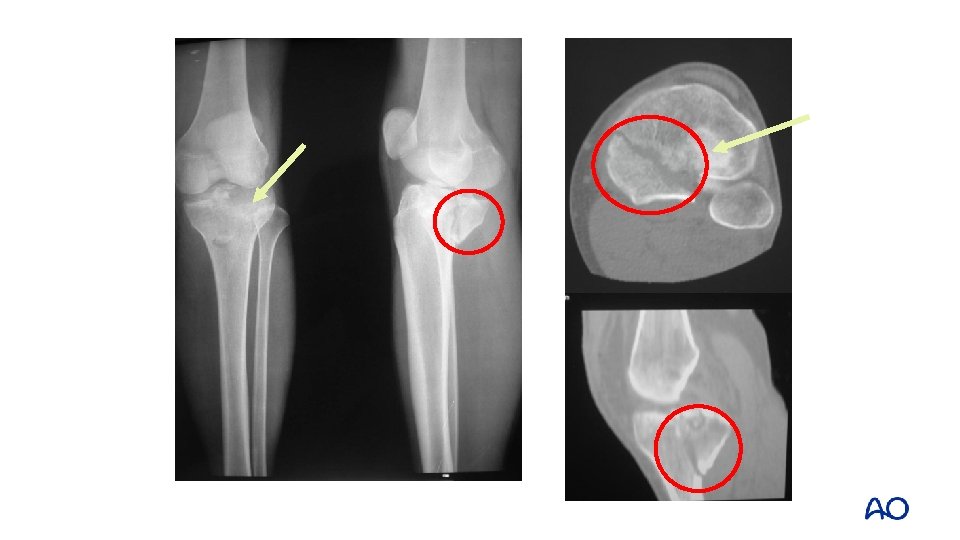
A P
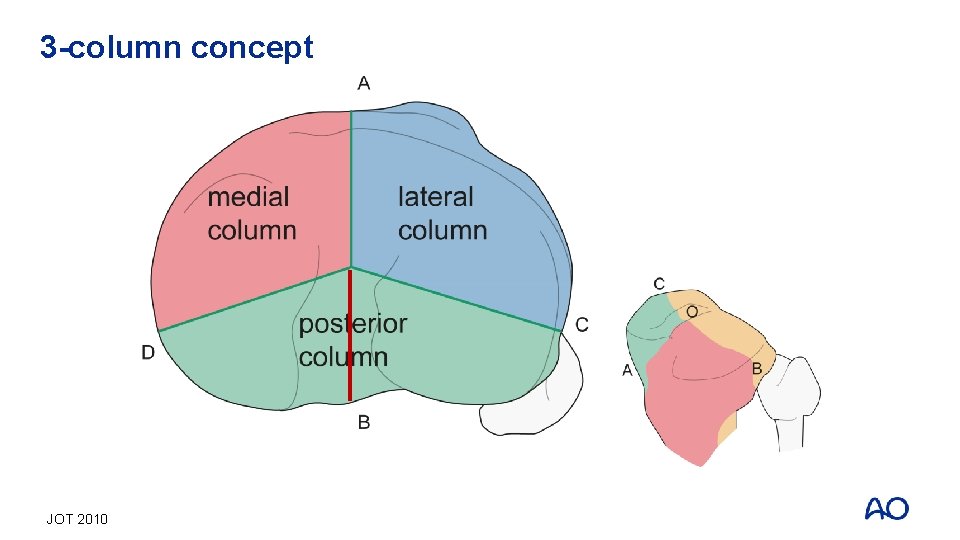
3 -column concept JOT 2010
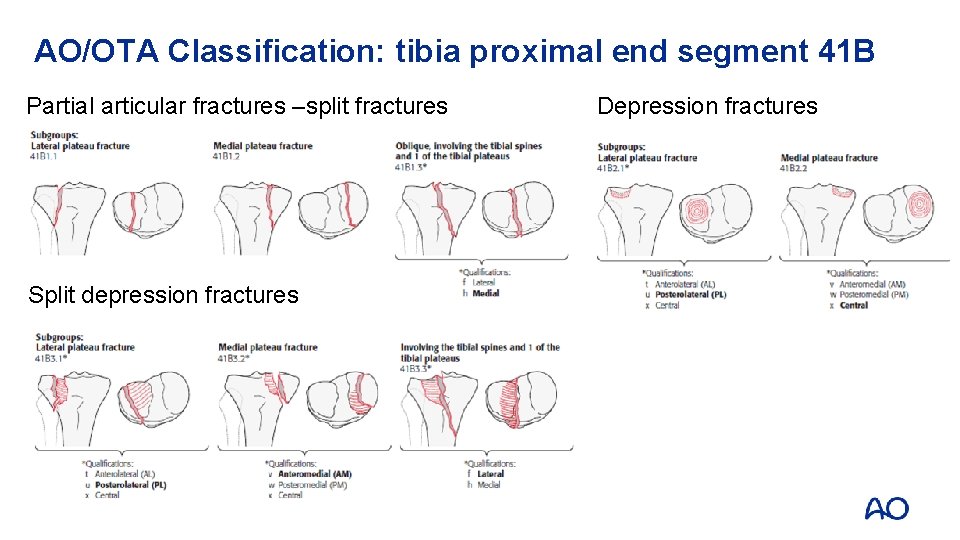
AO/OTA Classification: tibia proximal end segment 41 B Partial articular fractures –split fractures Split depression fractures Depression fractures
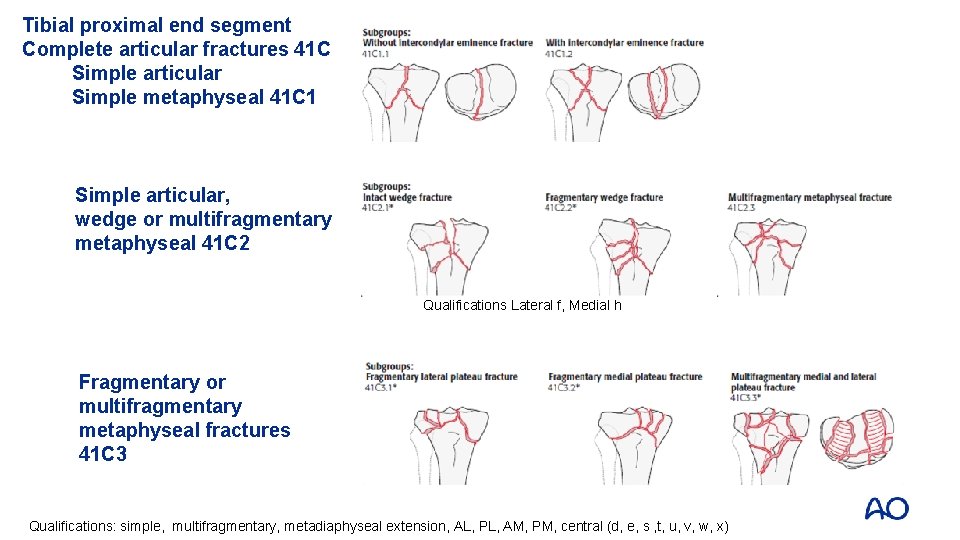
Tibial proximal end segment Complete articular fractures 41 C Simple articular Simple metaphyseal 41 C 1 Simple articular, wedge or multifragmentary metaphyseal 41 C 2 Qualifications Lateral f, Medial h Fragmentary or multifragmentary metaphyseal fractures 41 C 3 Qualifications: simple, multifragmentary, metadiaphyseal extension, AL, PL, AM, PM, central (d, e, s , t, u, v, w, x)
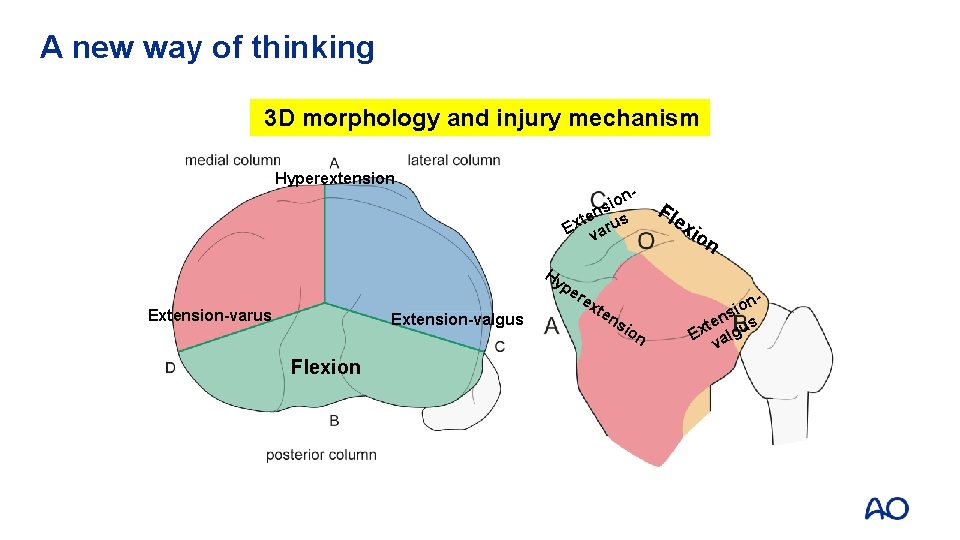
A new way of thinking 3 D morphology and injury mechanism Hyperextension - ion s ten us x E var Hy pe Extension-varus Extension-valgus Flexion re Fl ex io n xt en sio n no i ns s e t Ex algu v
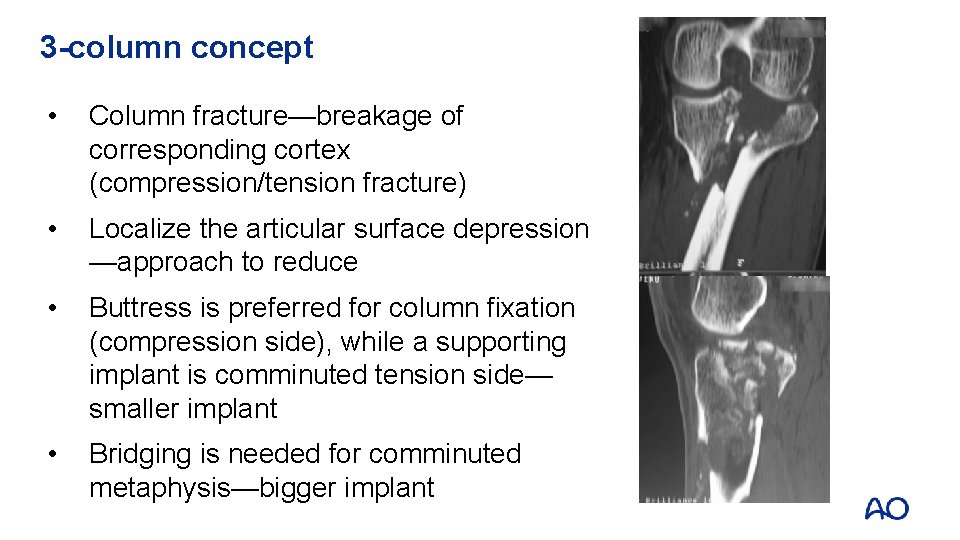
3 -column concept • Column fracture—breakage of corresponding cortex (compression/tension fracture) • Localize the articular surface depression —approach to reduce • Buttress is preferred for column fixation (compression side), while a supporting implant is comminuted tension side— smaller implant • Bridging is needed for comminuted metaphysis—bigger implant
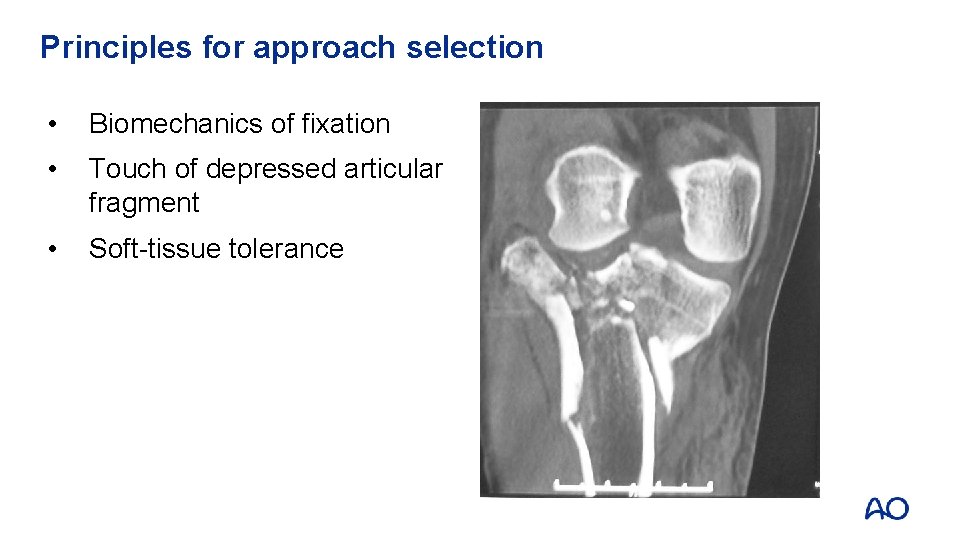
Principles for approach selection • Biomechanics of fixation • Touch of depressed articular fragment • Soft-tissue tolerance
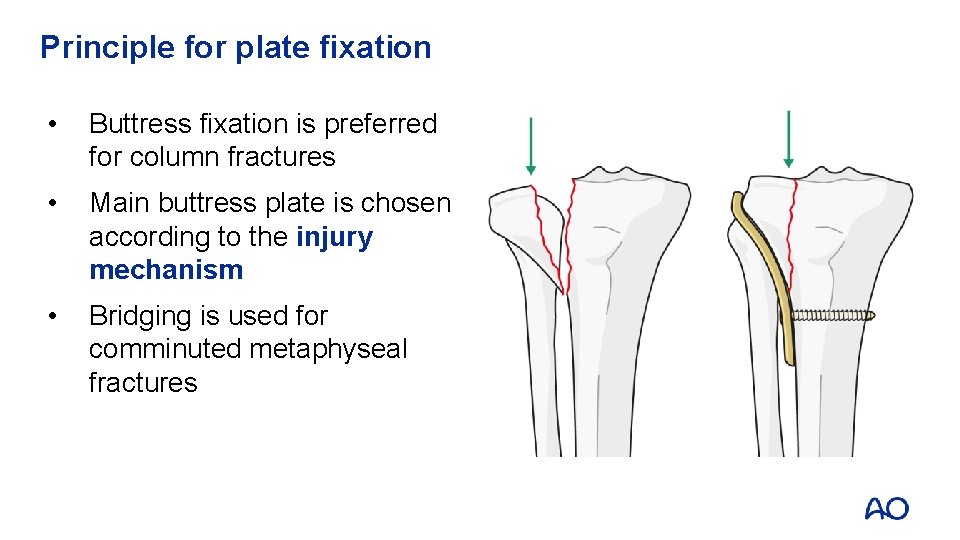
Principle for plate fixation • Buttress fixation is preferred for column fractures • Main buttress plate is chosen according to the injury mechanism • Bridging is used for comminuted metaphyseal fractures
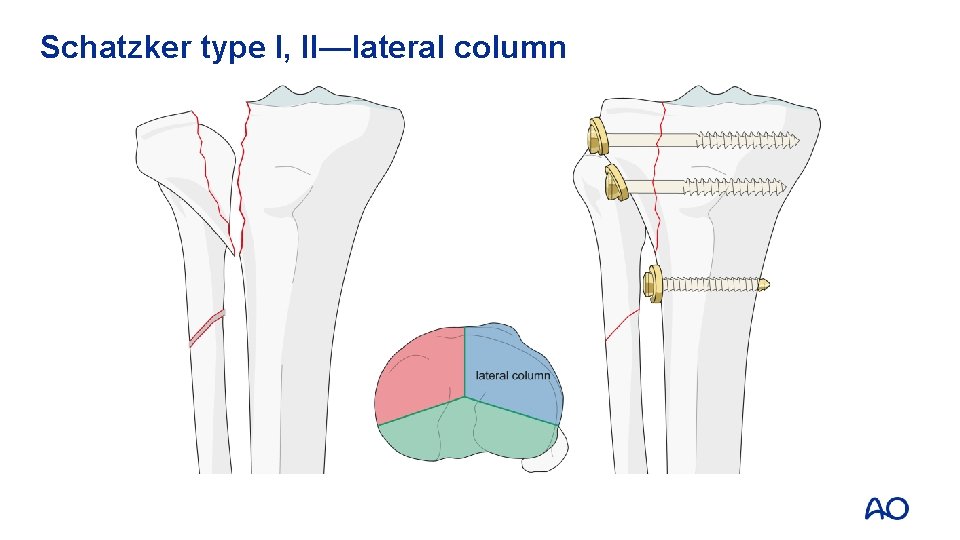
Schatzker type I, II—lateral column
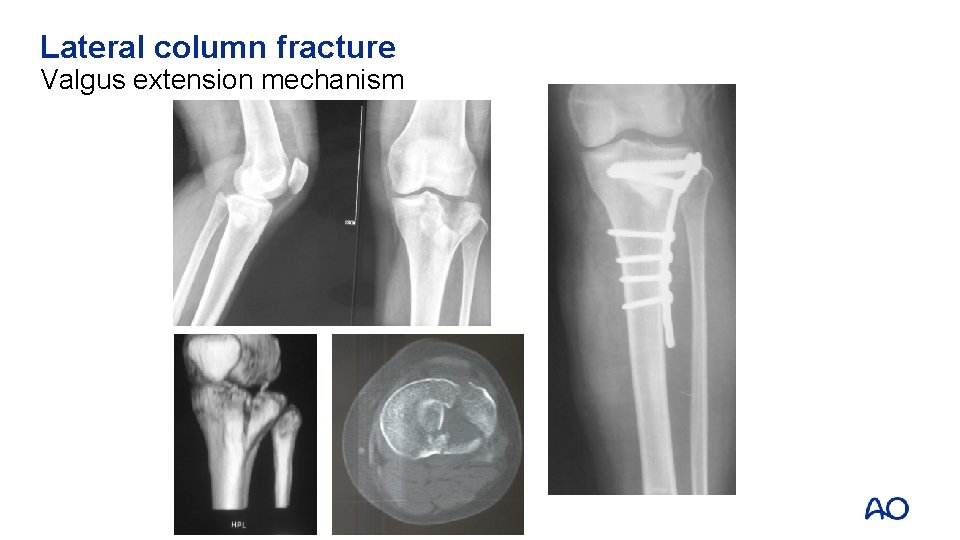
Lateral column fracture Valgus extension mechanism
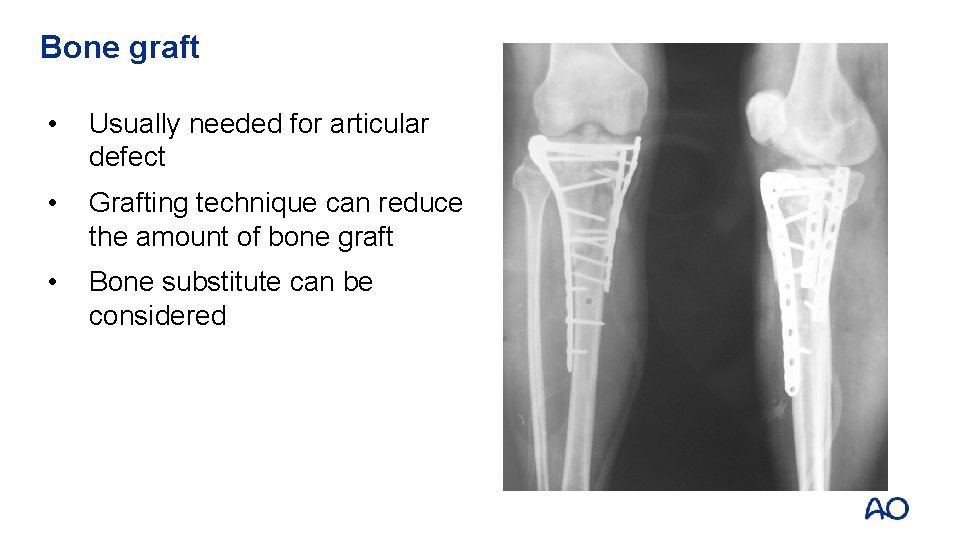
Bone graft • Usually needed for articular defect • Grafting technique can reduce the amount of bone graft • Bone substitute can be considered
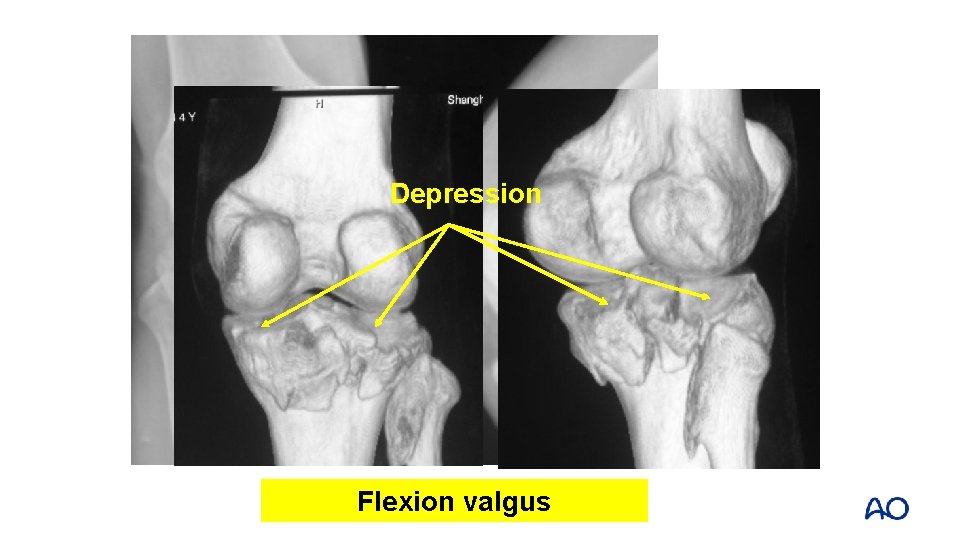
Depression Flexion valgus
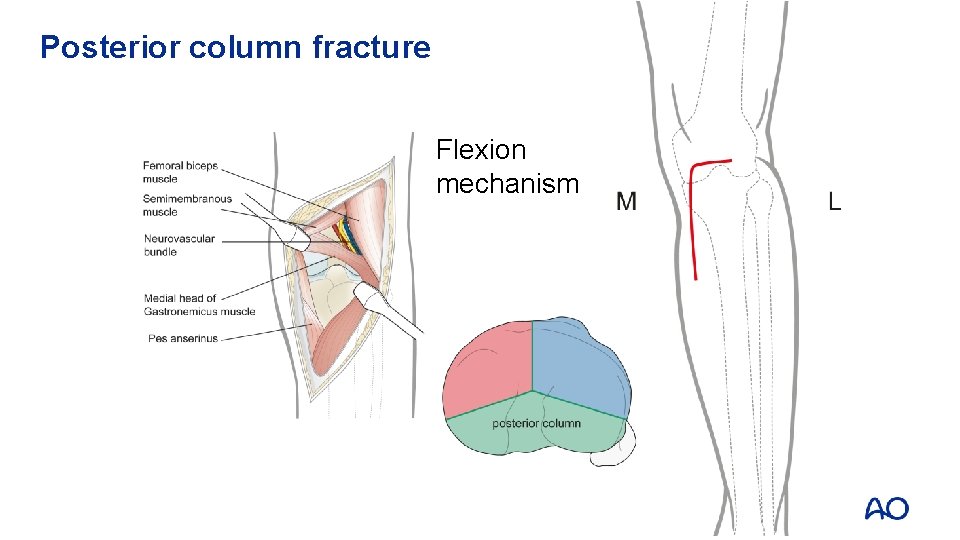
Posterior column fracture Flexion mechanism M L
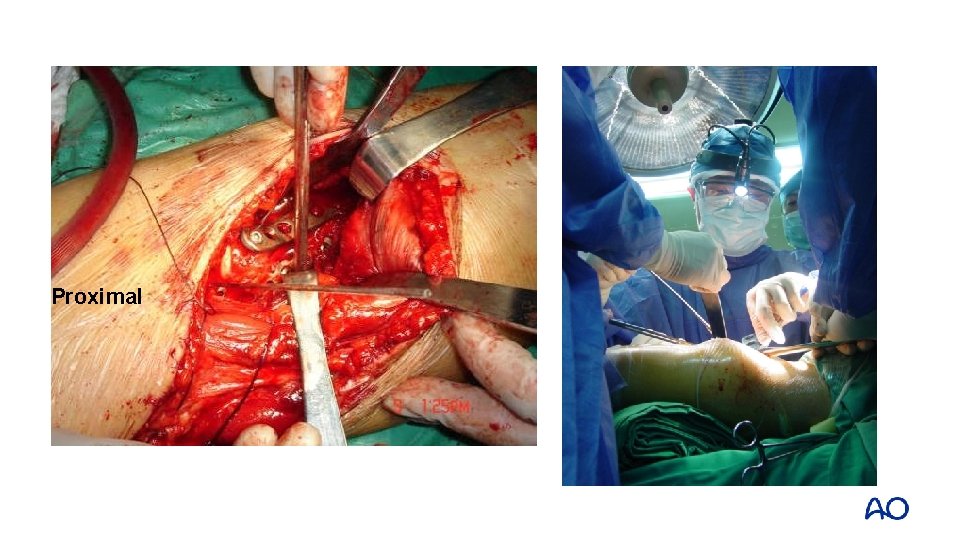
Proximal
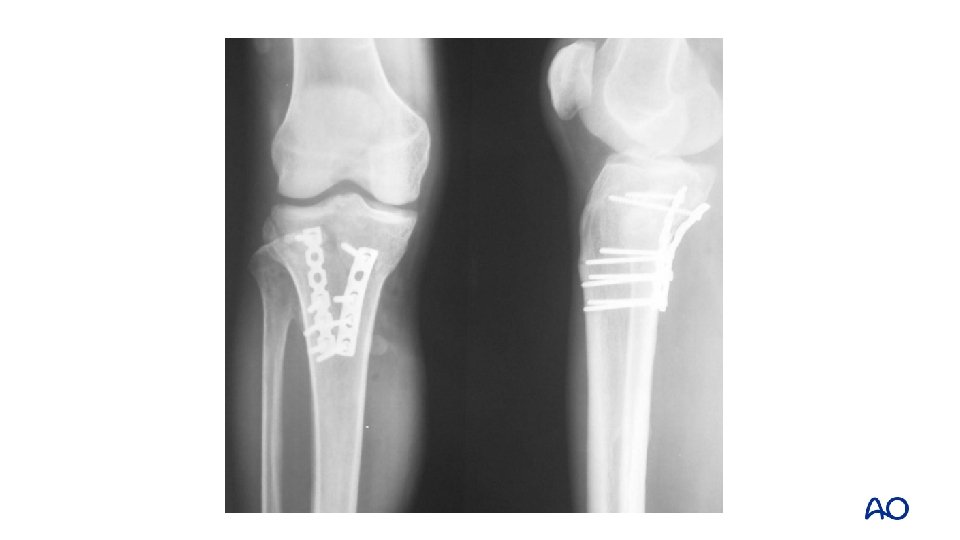
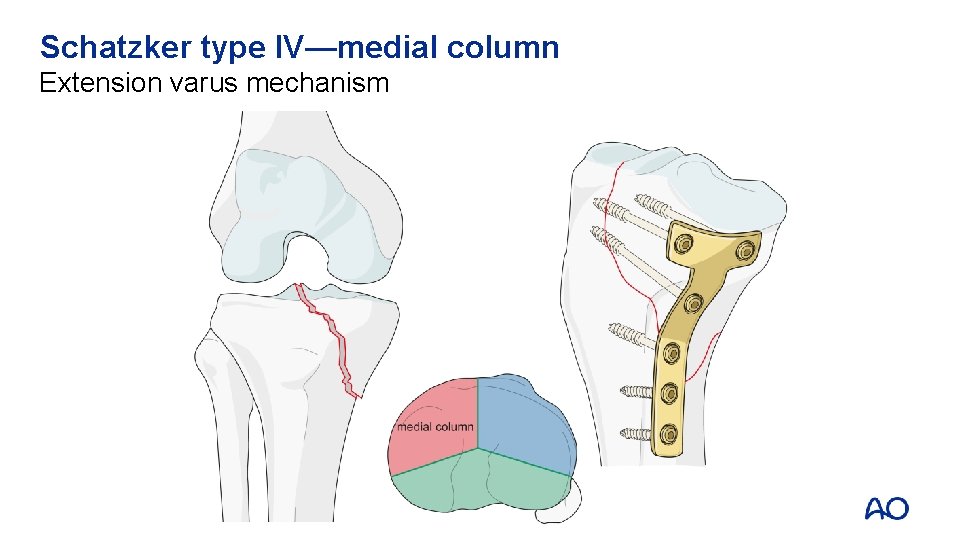
Schatzker type IV—medial column Extension varus mechanism
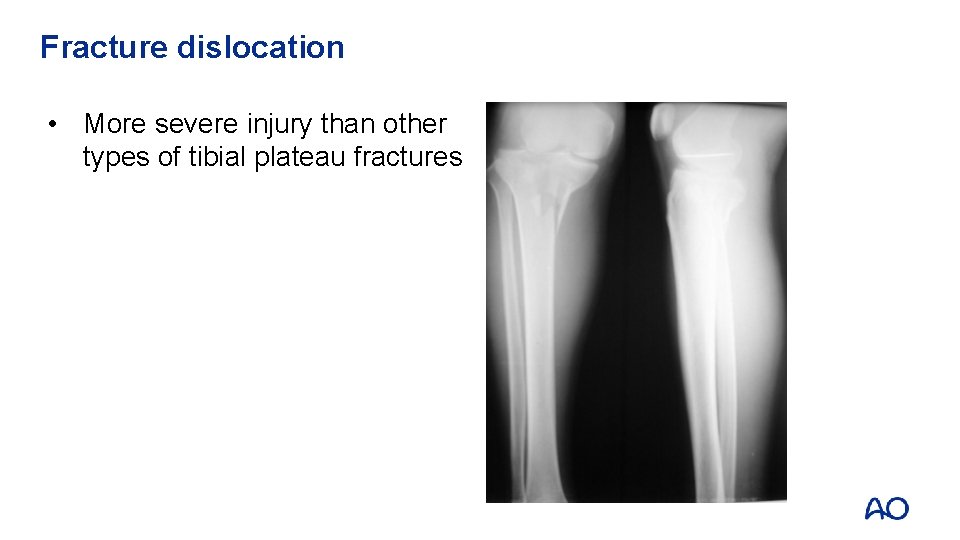
Fracture dislocation • More severe injury than other types of tibial plateau fractures
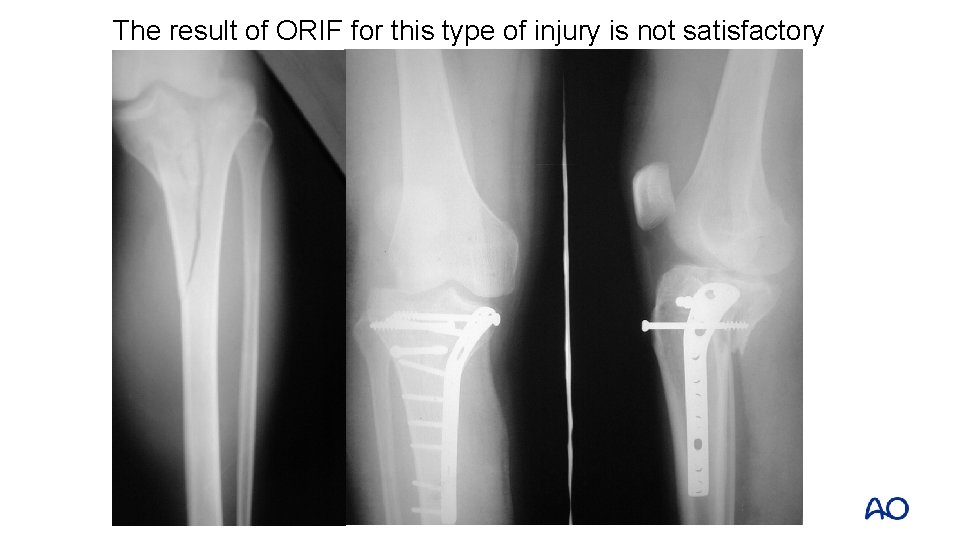
The result of ORIF for this type of injury is not satisfactory
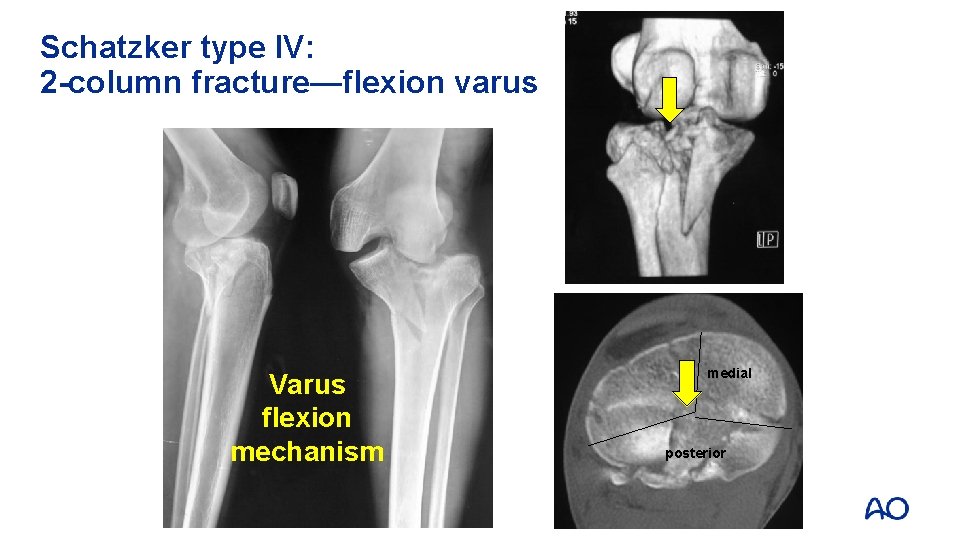
Schatzker type IV: 2 -column fracture—flexion varus Varus flexion mechanism medial posterior
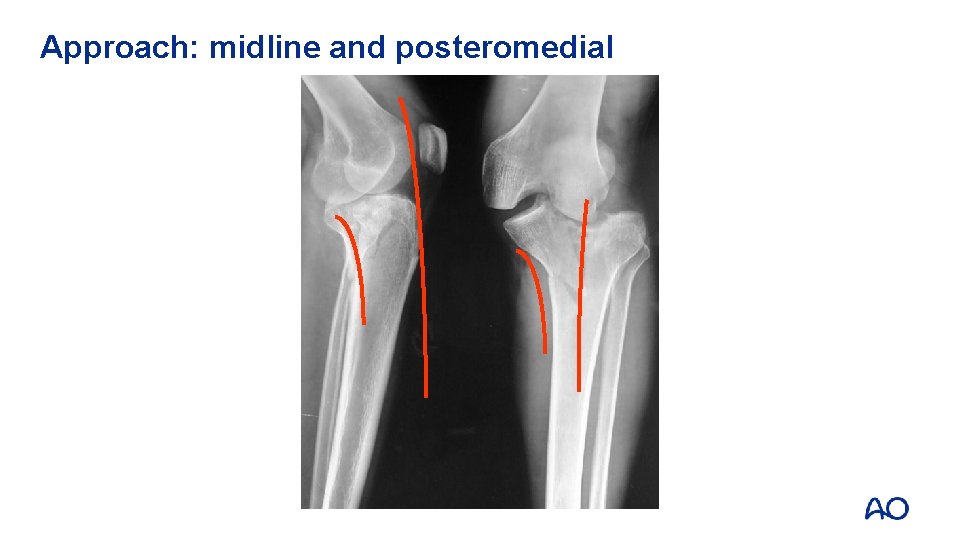
Approach: midline and posteromedial
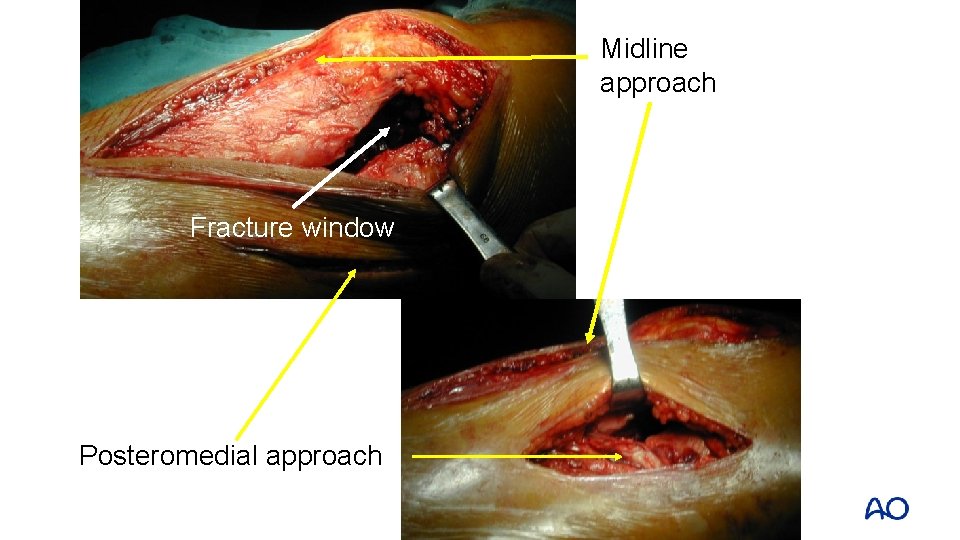
Midline approach Fracture window Posteromedial approach
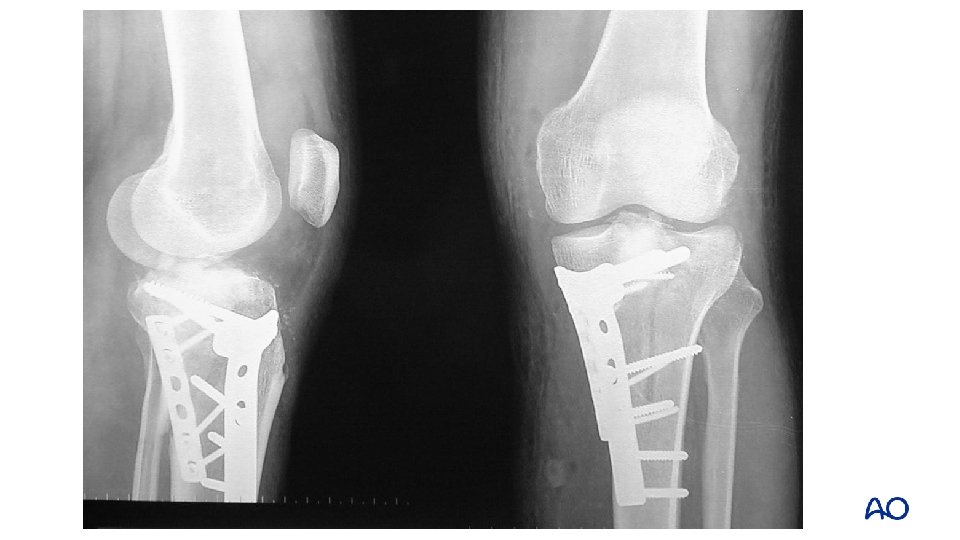
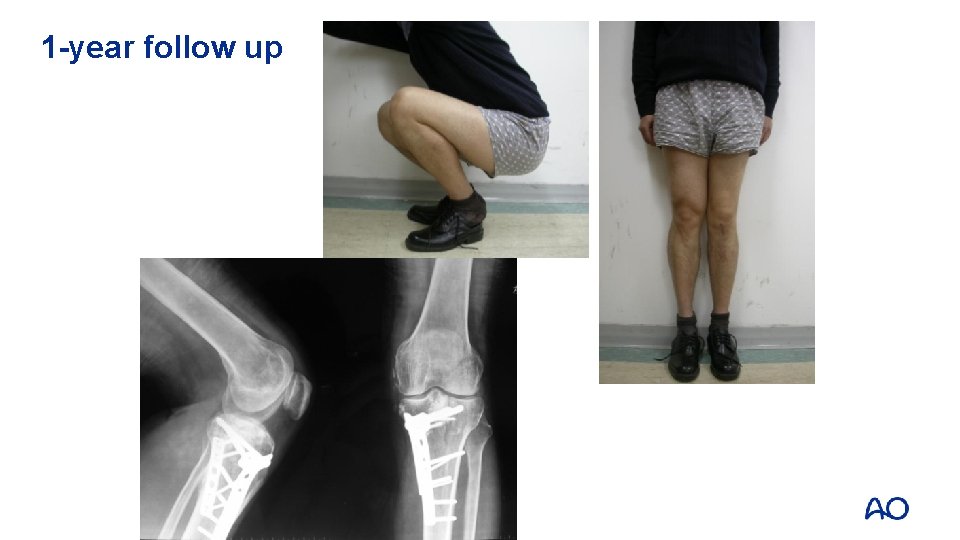
1 -year follow up
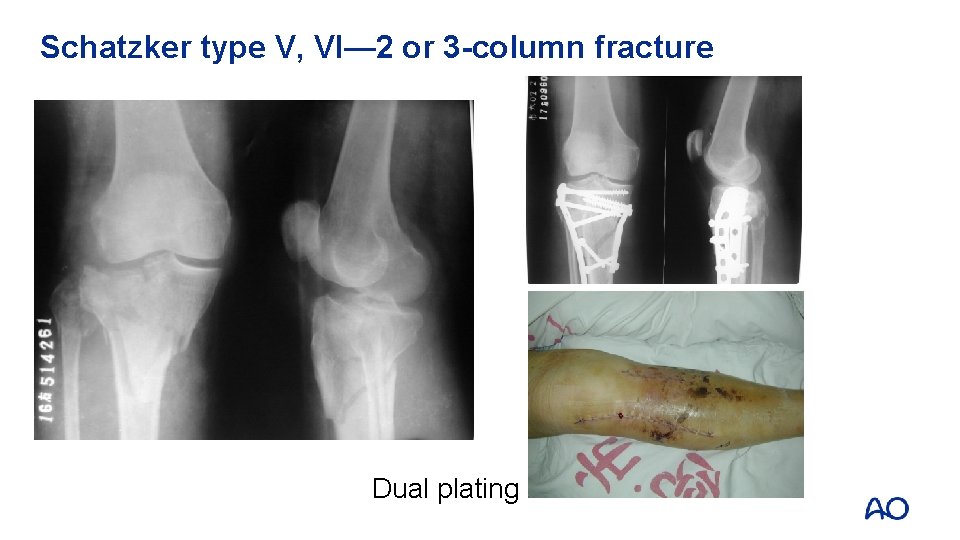
Schatzker type V, VI— 2 or 3 -column fracture Dual plating
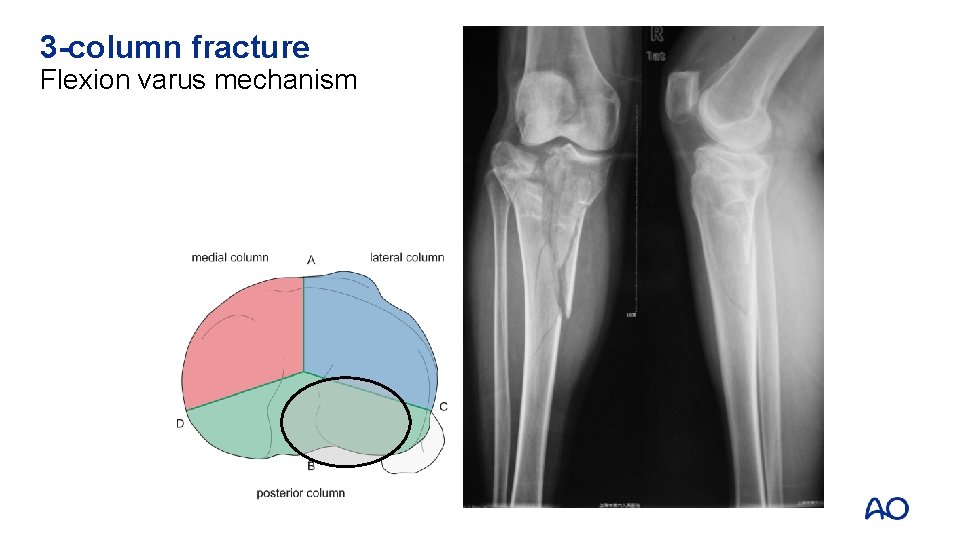
3 -column fracture Flexion varus mechanism
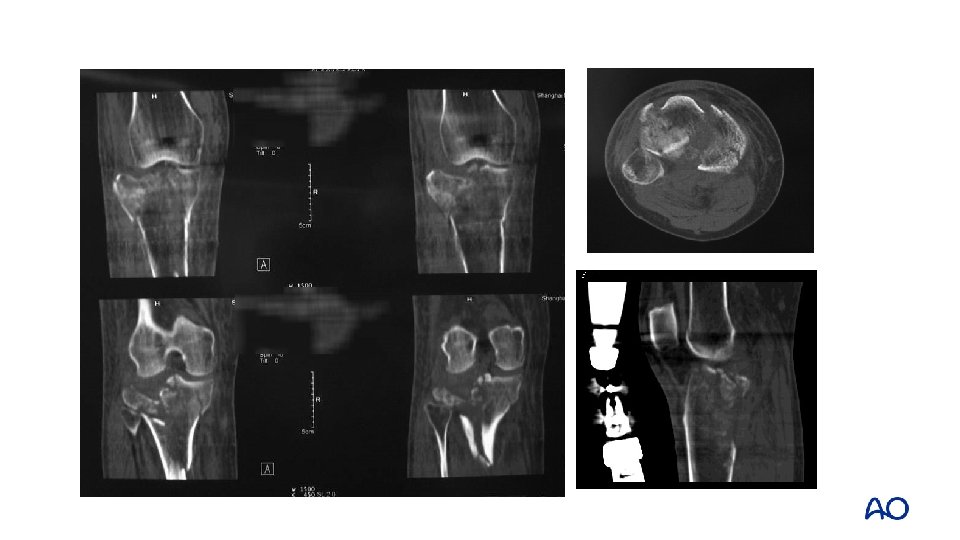
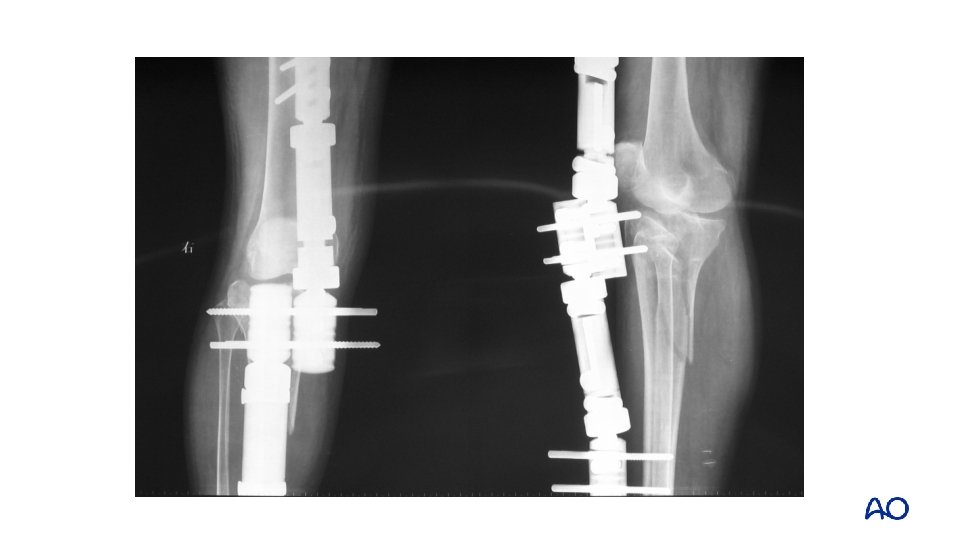
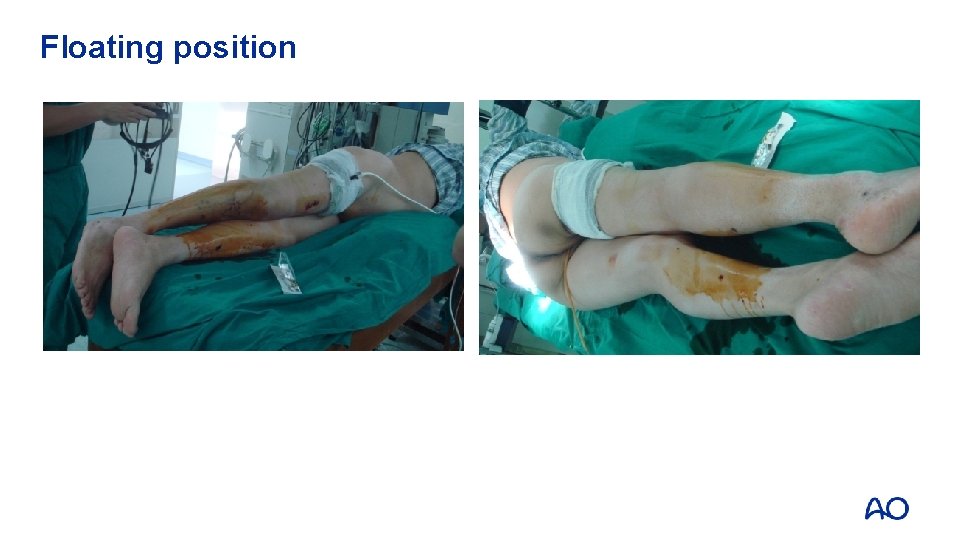
Floating position
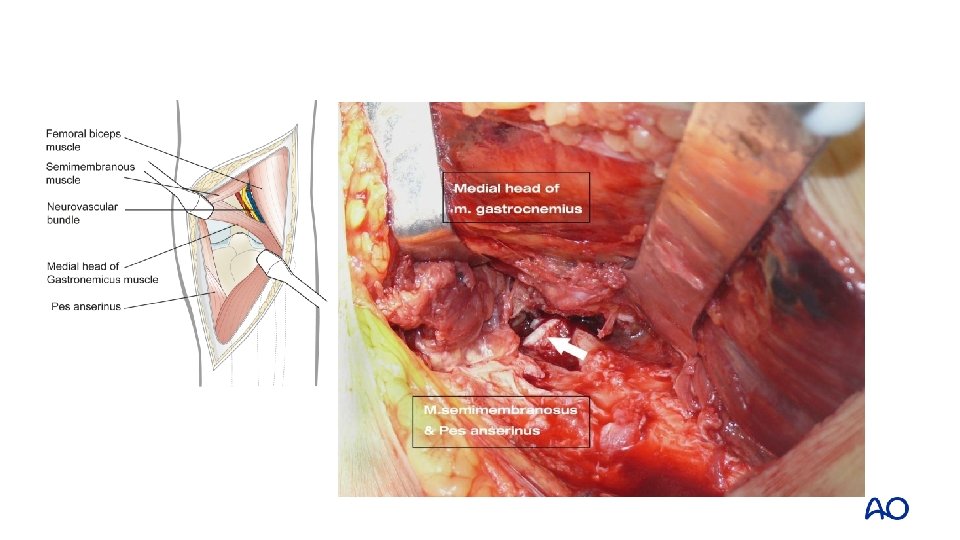
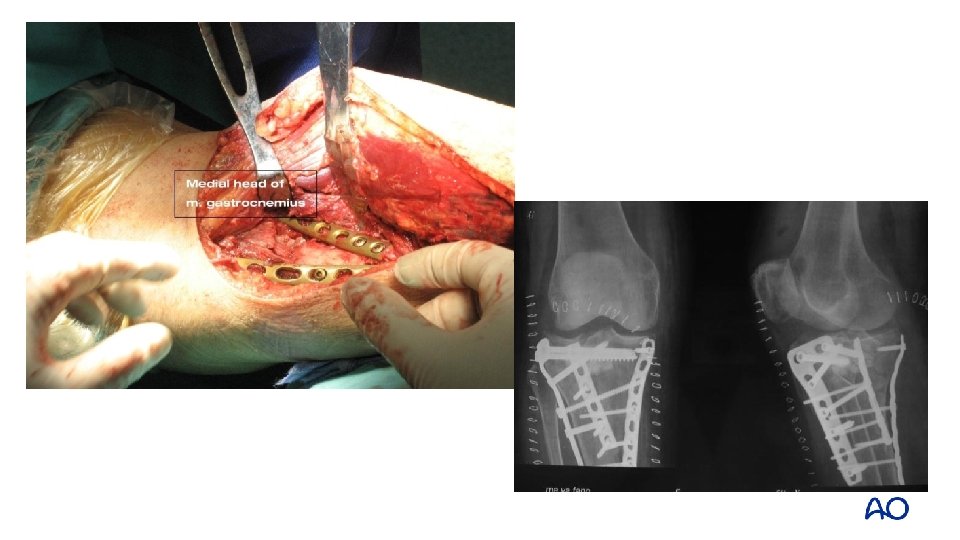
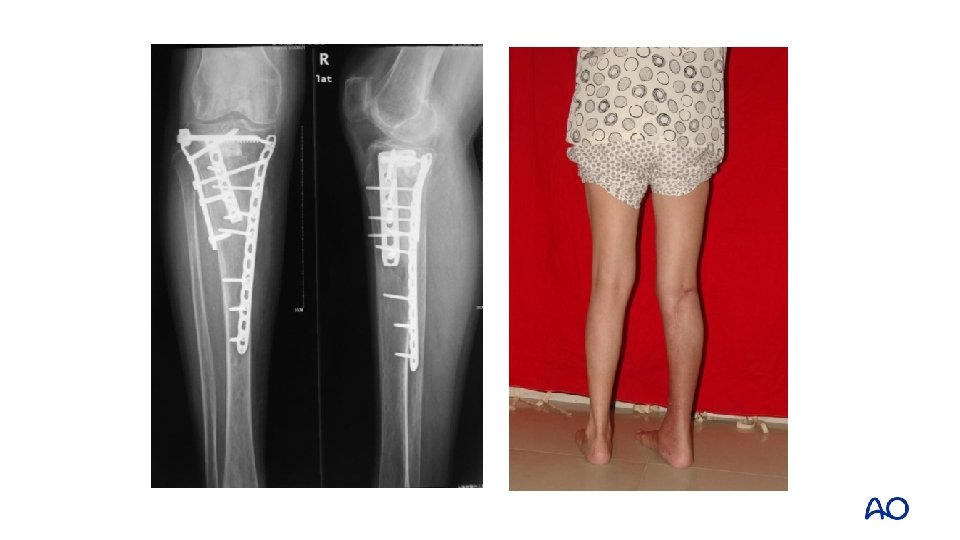


Take-home messages • Fully understanding the fracture is essential for decision making and definitive fixation • Approach selection and fixation should take into account the soft tissue, mechanism of injury, and 3 D morphology • 3 D classification and injury mechanism provides a new way of thinking for the treatment of tibial plateau fractures
- Slides: 38