Compatibility Testing Ahmad Shihada Silmi Msc FIBMS IUG

Compatibility Testing Ahmad Shihada Silmi Msc, FIBMS IUG

? What is compatibility testing Also called pretransfusion testing Ø Purpose: Ø l Ø To select blood components that will not cause harm to the recipient and will have acceptable survival when transfused If properly performed, compatibility tests will confirm ABO compatibility between the component and the recipient and will detect the most clinically significant unexpected antibodies

? Compatibility testing Ø There are several components of compatibility testing l l l Proper specimen collection Reviewing patient transfusion history ABO, Rh, and antibody testing (screen/ID) Crossmatching Actual transfusion

Compatibility testing Ø Can be divided into 3 categories: l l l Preanalytical procedures Serological testing Postanalytical procedures

Pre-analytical phases Ø Patient identification Ø Specimen collection Ø Review of patient history

Patient Identification Ø Must confirm recipient’s ID from bracelet ON the patient l l http: //www. usatoday. com/tech/news/techinnovations/2006 -07 -17 -chips-everywhere_x. htm Full patient name and hospital number Name of physician

Sample Identification The sample should also have the full patient name, hospital number, and physician Ø Date and time of collection, phlebotomist’s initials Ø All of this should be on the request form and the sample Ø
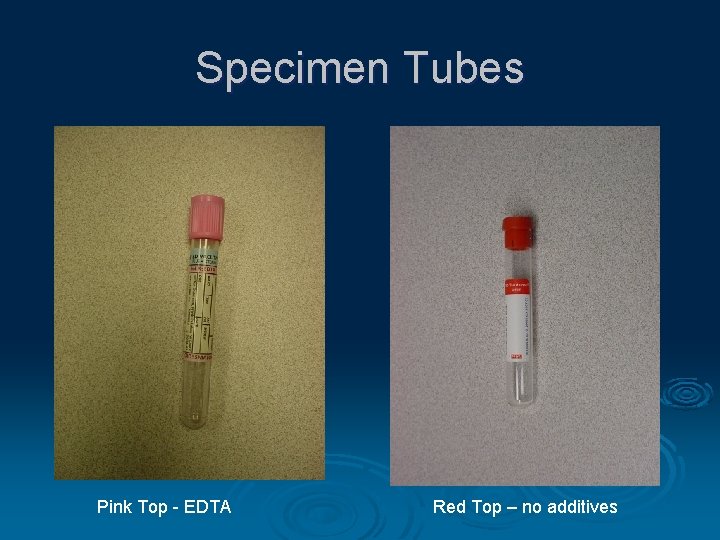
Specimen Tubes Pink Top - EDTA Red Top – no additives

Specimen Collection Collected in tube with EDTA or no additives Ø If the venipuncture causes hemolysis, the sample may be rejected Ø True hemolysis in the patient is the result of complement activation Ø Samples are labeled at the bedside (pre-labeling is not recommended) Ø A record of individuals who collect (or test) the specimens should be documented in order to “backtrack” in case of an error Ø

Specimen Collection Ø If the sample is drawn from an IV line, the IV infusion should be stopped 5 -10 minutes prior to blood drawing and the first 10 m. L discarded Ø Testing should be performed on samples less than 72 hours or else complement dependent antibodies may be missed (complement can become unstable)

Getting the history Ø Look at recipient’s records for any prior unexpected antibodies Ø Previous transfusion reactions

Serological Testing Ø 3 tests: l l l ABO/Rh Antibody detection/identification Crossmatch

ABO/Rh Typing Ø In the ABO typing, the forward and reverse MUST match Ø In the Rh typing, the control must be negative Ø Both of these will indicate what type of blood should be given

Antibody screen and/or ID The antibody screen will detect the presence of any unexpected antibodies in patient serum Ø If antibodies are detected, identification should be performed using panel cells (with an autocontrol) Ø l l l IS 37° (LISS) AHG If an antibody is present, units negative for the antigen must be given Ø Proceed to the crossmatch… Ø

Crossmatching Ø Purpose: l l Prevent transfusion reactions Increase in vivo survival of red cells Double checks for ABO errors Another method of detecting antibodies

Crossmatch Ø Two types of crossmatches l l Major – routinely performed in labs Minor – not required by AABB since 1976
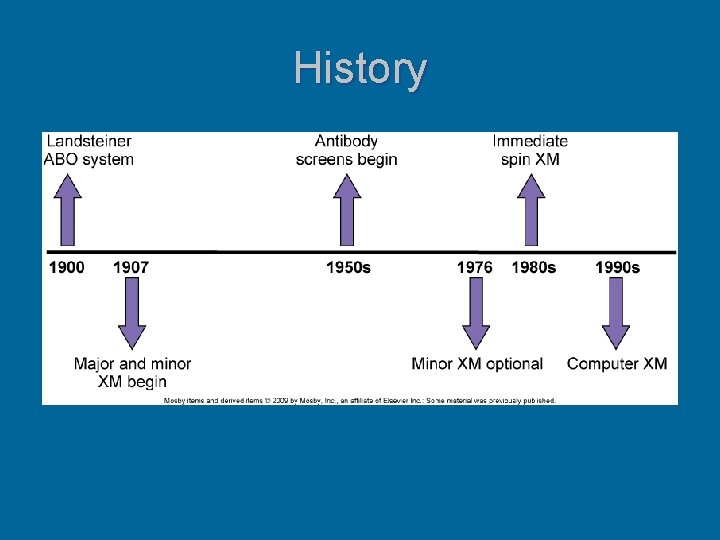
History

Major vs Minor Crossmatch Ø Why is the minor crossmatch unnecessary? Donated units are tested for antibodies l Most blood is transfused as packed cells, having little antibodies l

Crossmatches Ø The AABB and FDA develop the standards for blood banking Ø According to the AABB Standards: The crossmatch “shall use methods that demonstrate ABO incompatibility and clinically significant antibodies to red cell antigens and shall include an antiglobulin phase”
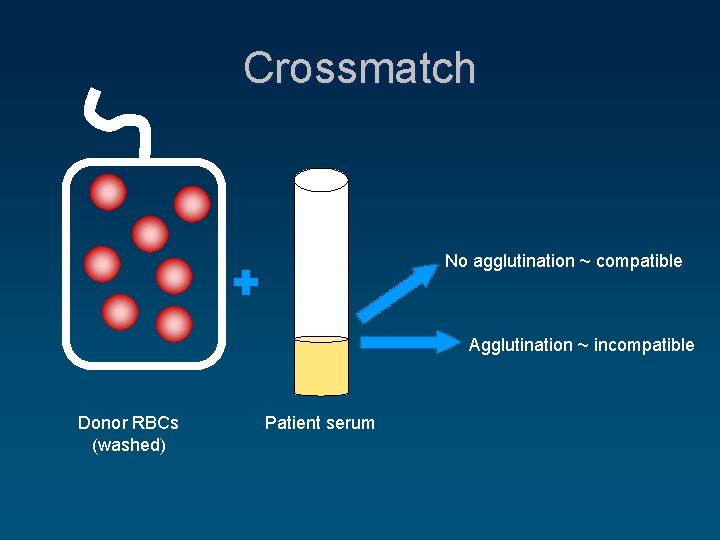
Crossmatch No agglutination ~ compatible Agglutination ~ incompatible Donor RBCs (washed) Patient serum
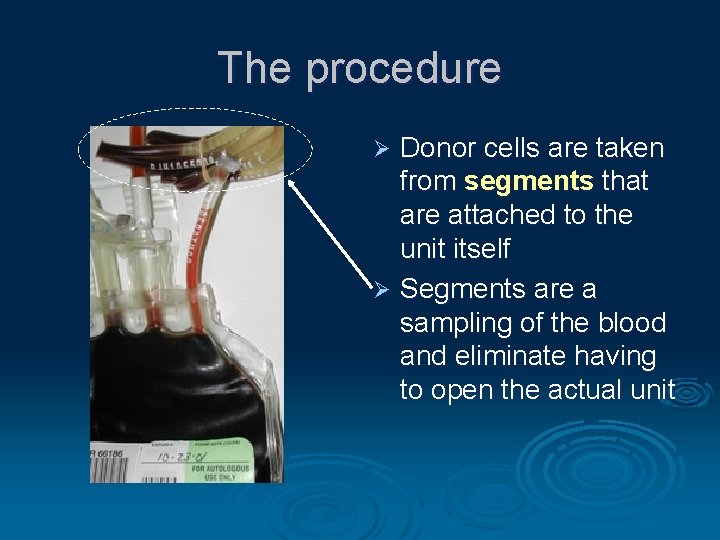
The procedure Donor cells are taken from segments that are attached to the unit itself Ø Segments are a sampling of the blood and eliminate having to open the actual unit Ø

Units of whole blood with segments attached

Procedure Ø ABO/Rh typing is FIRST performed Ø Antibody Screen is performed next….

Crossmatch Procedure Ø if antibodies are NOT detected: l l l Only immediate spin (IS) is performed using patient serum and donor blood suspension This fulfills the AABB standard for ABO incompatibility This is an INCOMPLETE CROSSMATCH Ø If antibodies ARE detected: l l l Antigen negative units found and X-matched All phases are tested: IS, 37°, AHG This is a COMPLETE CROSSMATCH
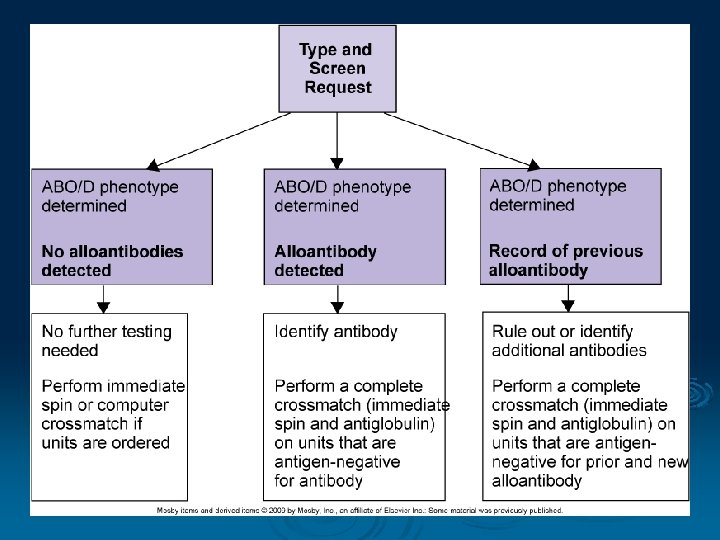

…Crossmatches Will Verify donor cell ABO compatibility Detect most antibodies against donor cells Will Not Guarantee normal survival of RBCs Prevent patient from developing an antibody Detect all antibodies Prevent delayed transfusion reactions Detect ABO/Rh errors

Incompatible crossmatches Antibody Crossmatch screen Cause Resolution Pos Neg Antibody directed against antigen on screening cell ID antibody, select antigen negative blood Neg Pos Antibody directed against antigen on donor cell which may not be on screening cell OR donor unit may have Ig. G previously attached ID antibody, select antigen negative blood OR perform DAT on donor unit Pos Antibodies directed against both screening and donor cells Antibody ID, select antigen negative blood

Additional Information on Types of Compatibility Tests Manual (IS and IAT) Gel Technology Electronic (Computerized) Cross match Red cell Affinity Column Technology (Re. ACT) Solid Phase Adherence Assays (SPAA)
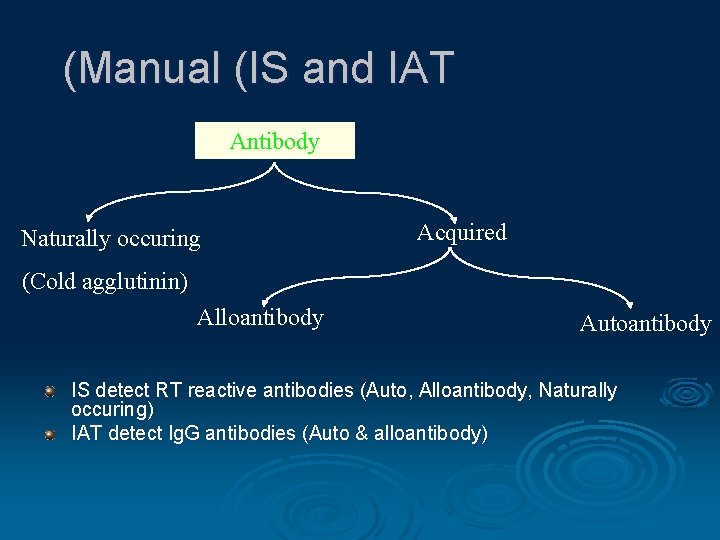
(Manual (IS and IAT Antibody Naturally occuring Acquired (Cold agglutinin) Alloantibody Autoantibody IS detect RT reactive antibodies (Auto, Alloantibody, Naturally occuring) IAT detect Ig. G antibodies (Auto & alloantibody)

Gel Technology Patient serum, and 1% of suspended RBCs in LIM are dispensed into the o microtube and incubated at 37 C for 15 minutes. The card containing the microtubes is then centrifuged at a controlled speed for 10 minutes. At the start of centrifugation the cells are separated from the serum; then they meet the AHG contained in the microtube. Finally the cells are trapped by the gel (if agglutinated) or pellet to the bottom of the tube.

X Match Phases clinically insignificant such as anti- M, -N, -Lea, This phase is usually Leb, and -I. read only macroscopically PHASE PURPOSE IS detection Ig. M cold agglutinin 37 o. C, LISS Ig. G Abs AHG OCC Ig. G Abs DETECTS Most ABO incompatibilities for agglutination This phase is read Potent Rh Abs microscopically for Rh, Duffy, Kidd, added to all negative ` agglutination tests and must AHG absence, inadequacy, or neutralization produce a positive result others Sensitized RBCs

Limitations of Pretransfusion Testing Hemolytic transfusion reaction, if the patient's antibody is too weak to be detected. Standard antibody detection methods such as the indirect antiglobulin test require several 100 antibody molecules per red cell to produce detectable reactions. A hemolytic transfusion reaction due to patient misidentification. For example, group A red cells (meant for transfusion to a group O recipient) will be compatible in vitro tests with an incorrect specimen drawn from a group A person.

Limitations of Pretransfusion Testing Hemolytic transfusion reaction if donor red cells are inadvertently hemolysed before entering the patient, e. g. , red cells hemolysed by an improperly functioning blood warmer or red cells hemolysed by contact with an ice pack in a transport container. Nonhemolytic transfusion reactions such as allergic, febrile, and other reactions. Pretransfusion test are meant to detect only red cell antibodies.

Incompatible cross match ABO incompatibility Recheck patient and blood unit ABO group Clinically Significant Ab DAT & IAT

Antibody Detection

IAT is used to detect clinically significant Ig. G antibodies bound to RBCS in vitro. Detection of free Abs in patient's serum. Clinically significant Ig. G Abs cause hemolysis or reduce survival of transfused RBCs, like D, c, E, K, k, JKa, JKb, FYa, FYb , S, s. Unimportant Abs: I, P 1, Lea, Leb, M, N. Those Abs are Unimportant due to ØMostly cold reactive (Ig. M) ØCould be neutralized

IAT is principally used for Ø Ab detection Ø Ab investigation (identification) Ø Ab titration Ø Compatibility testing Ø Phenotyping for some RBCs antigens

Reagent used in IAT Characteristics of RBCs reagent: Three cell reagent sets, Serocyte I, III. RBCs antigens corresponding to important and clinically significant Abs. The reagent cells are suspended in saline and 2%-5% antibiotic. Expired reagent should not be used. An antigram defining phenotype of reagent cell must included with every cell. All reagent should be stored at 1 -6 o. C.

Performance IAT o Most clinically significant Abs react at 37 C, RT and IS are not required. AHG is usually monospecific Ig. G No need for polyspecific AHG. Because Anti C will detect Abs during the incubation phase. Anti C enhance the detection of cold agglutinin such as anti I, anti P that are non significant Abs and not important in transfusion. Delaying transfusion in critical situations.

Interpretation Result of IAT Negative IAT Ø OCC Positive: Report IAT negative Positive IAT Perform: l l Ab identification. Ab titration.

Interpretation Result of IAT Low titer, and weak reactive Abs are failed to be detected Using commercial reagents include RBCs that express important antigens in double dose, as JK (a + b -), JK Fy and Fy (a + b -), Fy (a + b -) cells. Avoiding use of LISS enhance reactivity of cold reactive Abs causing difficulties in detection clinically significant Abs. Increase amount of serum to increase amount of Abs.

Ø Its not a life threatening situation when an unexpected clinically important Abs to an RBCs Ags in a blood unit is not detected, Because Ø The plasma volume is small, and Abs will be diluted in recipient circulation Ø Unlikely to cause significant destruction to recipient's RBCs.

Antibody Identification

Ø 0. 3% - 2. 8% of the population are Ab makers, they produce clinically significant Ab. Ø Pregnancy and transfusion are the common cause of immunization to RBCs Ags.

Serological Properties Abs of blood groups vary in importance and significance due to serological properties Ø Temperature phase 37 o. C reactive Abs as anti D, c, E, K, k, JKa, JKb, FYa, FYb , S, s. Cold agglutinin as anti Lea, Leb, I, P 1, M, N. Inducing HDN and HTR Ø Activation complement. Ø Neutralizing by soluble blood group Ags Ø

Problems Encountered Autoantibody directed against own cell Ags Elution solution Ig. G Abs can be dissociated from RBCs membrane Ags by physical or chemical means, some procedures destroy membrane, some leave it intact. Supernatant fluid (elute) contain the autoantibodies which can be identified. .

Problems Encountered Combination of auto and alloantibody solution Treatment with ZZAP (Adsorption) ZZAP effectively removes autoantibodies (digestion) allowing more complete absorption of autoantibodies from patient's serum, allowing detection and identification of alloantibody. Chemically treated allogenic RBCs Treated RBCS with proteolytic enzymes, alter some Ags

Problems Encountered Weak or non reacted with any or some cell reagent. Variable reaction Solution Variable expression of Ags (P , Lewis) Ags deteriorate on storage (Duffy, P 1, M, Lewis) Duffy, MNS) Abs is reacting with more than one Ag. • Use new cell reagent DDCCee 3+ Ddccee 1+ 1 • Use double dose of corresponding Ags, (Rh, Kidd,

Post-analytical phase

Post-analytical phase Involves labeling, inspecting, and issuing the blood unit Ø Labeling form includes patient’s full name, ID number, ABO/Rh of patient and unit, donor #, compatibility results, and tech ID Ø Form is attached to the donor unit and only released for the recipient Ø The unit is visually inspected for abnormalities, such as bacterial contamination, clots, etc Ø
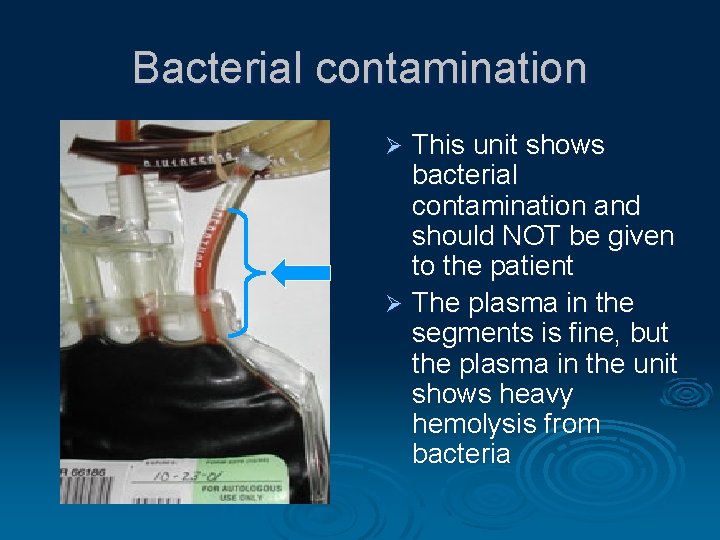
Bacterial contamination This unit shows bacterial contamination and should NOT be given to the patient Ø The plasma in the segments is fine, but the plasma in the unit shows heavy hemolysis from bacteria Ø

Issuing blood Ø When it’s time to release a blood product to the nurse or physician, a few “checks” must be done l l l Requisition form Comparing requisition form donor unit tag blood product label Name of persons issuing and picking up blood Date and time of release Expiration date

? What if the unit is unused Ø Blood can be returned if it is not needed for transfusion Ø Unit closure has to remain unopened Ø Storage temperature must have remained in the required range (1° to 10°C for RBCs) Ø If not at correct temp, unit must be returned within 30 minutes of issue

Infusion Device
Blood Warmer

Special Circumstances

Emergency Release Ø In an emergency (ER or OR), there may not be enough time to test the recipient’s sample Ø In this case, blood is released only when signed by the physician (O negative) Ø The tag must indicate it is not crossmatched Ø Segments should be retained for Xmatching Ø Every detail is documented (names, dates. . )

Emergency Release Once the specimen is received, ABO/Rh typing and antibody screening should be performed Ø Crossmatching the segments from the released unit should be tested Ø In addition, the lab may crossmatch additional units as a precaution if more blood is needed Ø If death should occur, testing should be complete enough to show that the death was unrelated to an incompatibility Ø

What can be given in an emergency? Ø Group O Rh-negative red cells or AB plasma l l l Emergency release Women below or of childbearing age Or if in doubt Ø Group O Rh-positive red cells l l Used as a substitution Male or elderly females

Massive transfusion Defined as a transfusion approaching or exceeding the recipient’s own blood volume (about 5 liters or 10 -12 units in an adult male) within 24 hour period Ø The original sample no longer represents the patient’s condition Ø Complete crossmatch not necessary (if no antibodies were detected originally) Ø Give ABO identical units Ø l If antibodies were originally ID’s, continue to give antigen negative units

Appropriate units to give Ø ABO compatible should always be given first Patient’s Type O A B AB 1 st Choice O A Other Choices None O B O AB are “universal donors”, A, B, they O can donate to any blood • Group O individuals group because they have no A or B antigens • Group AB individuals are “universal recipients”, they can receive blood from any group because they do not have A or B antibodies
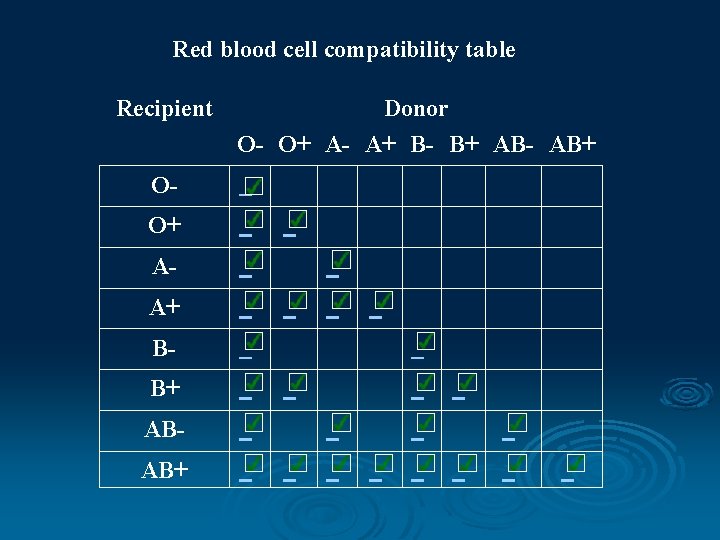
Red blood cell compatibility table Recipient Donor O- O+ A- A+ B- B+ AB- AB+ O- O+ A- A+ B- B+ AB- AB+
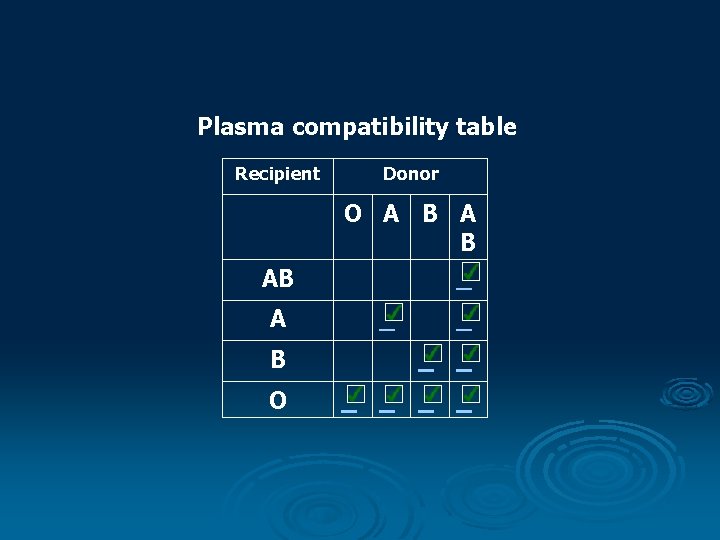
Plasma compatibility table Recipient AB A B O Donor O A B

Type & Screen Used to conserve blood inventory On average, a surgical procedure uses about 1 unit of RBCs, however, many times the units are on “hold” in the lab and will not be needed (reducing inventory) Ø For this reason, only a type & screen are performed and if any blood is needed, the sample can be retrieved for crossmatching (only the IS phase is required) Ø If antibodies are identified, then antigen negative blood is reserved or crossmatched Ø Ø

Neonatal Transfusion A neonate who is <4 months old does not have antibodies Ø ABO/Rh compatible blood is given Ø However, if clinically significant antibodies are detected, they are usually maternal and antigen negative units are given Ø Either infant or maternal serum can be used for the crossmatch Ø Pedipacks are small aliquots of larger units and prepared by the donor facility or hospital lab for infant transfusion Ø

Autologous crossmatching Ø Autologous refers to a donation from the recipient for later use Ø Special procedures/protocols must be available so that the autologous unit is found and transfused to the recipient Ø Pretransfusion testing procedures vary

Other components Ø Other components to be given do not need to be crossmatched because they have been thoroughly screened for antibodies l l l Frozen plasma Platelet concentrate Cryoprecipitate Platelets pheresis Granulocyte concentrates Ø Give ABO compatible units

…New Technologies Ø The electronic crossmatch Ø According to the AABB, the following must be fulfilled: l l Critical elements of the information system have been validated on-site. No clinically significant antibodies are detected in the current blood sample and there is no record of clinically significant antibodies in the past

(Computer crossmatch (cont’d The patient's ABO group and Rh type has been done twice and entered in the computer Ø The donor ABO/Rh have been confirmed and entered in the computer. The donor unit identification number, component name, and ABO/Rh type must also be entered in the computer Ø The computer system will alert the technologist to ABO & Rh discrepancies between information on the donor label and results of donor confirmatory testing Ø
June, 1938
- Slides: 70