Company Logo Update in COPD for family physician











![Combine these assessments [symptoms + risk of AE] for the purpose of improving management Combine these assessments [symptoms + risk of AE] for the purpose of improving management](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-16.jpg)






![Available medication in Thailand v Short acting bronchodilator [SABA , SAMA] Berodual Ventolin SABA+SAMA Available medication in Thailand v Short acting bronchodilator [SABA , SAMA] Berodual Ventolin SABA+SAMA](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-26.jpg)
![Available medication in Thailand v Combined ICS/LABA Seretide [fluticasone/salmeteral] Symbicort [Formoterol/Budesonide] Available medication in Thailand v Combined ICS/LABA Seretide [fluticasone/salmeteral] Symbicort [Formoterol/Budesonide]](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-27.jpg)
![Available medication in Thailand v Methylxanthines Theophylline v PDE-4 inhibitors Roflumilast Doxophylline [Puroxan] Available medication in Thailand v Methylxanthines Theophylline v PDE-4 inhibitors Roflumilast Doxophylline [Puroxan]](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-28.jpg)

















- Slides: 56

Company Logo Update in COPD for family physician and nurse Karjbundid Surasit MD

www. themegallery. com Company Logo


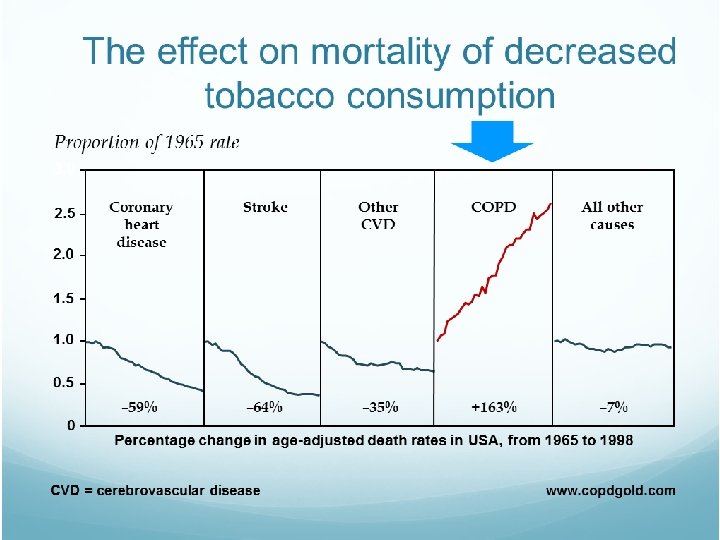
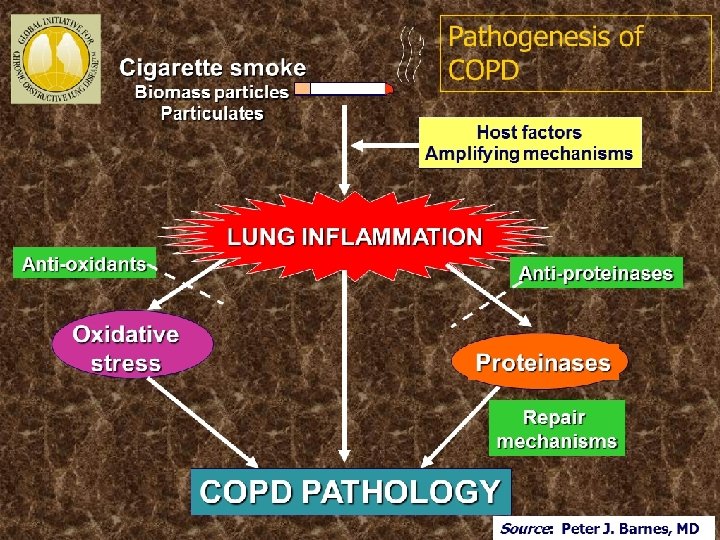
Definition of COPD 2015 GOLD 2015 v COPD, a common preventable and treatable disease, is characterized by persistent airflow limitation that is usually progressive and associated with an enhanced chronic inflammatory response in the airways and the lung to noxious particles or gases. v Exacerbations and comorbidities contribute to the overall severity in individual patients. • Comorbidities Cardiovascular diseases / Osteoporosis Comorbidities / Respiratory infections / Anxiety and Depression / Diabetes / CA Lung © 2015 Global Initiative for Chronic Obstructive Lung Disease

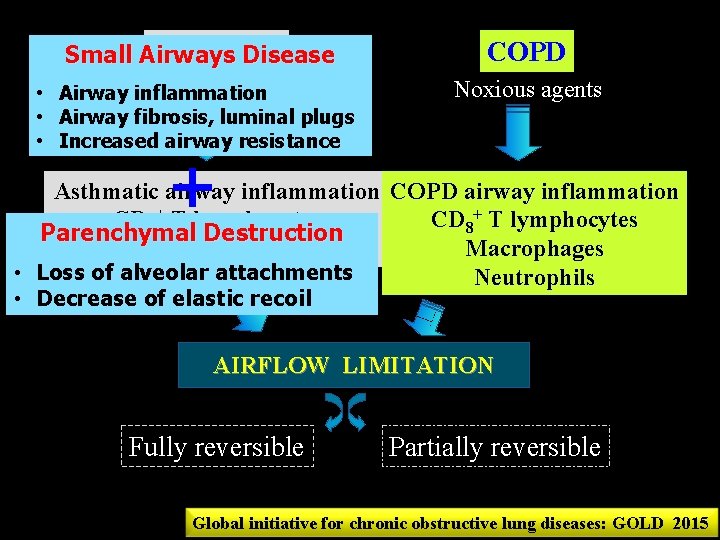
ASTHMA Small Airways Disease agents • Airway. Sensitizing inflammation COPD Noxious agents • Airway fibrosis, luminal plugs • Increased airway resistance + Asthmatic airway inflammation COPD airway inflammation CD 4+ T lymphocytes CD 8+ T lymphocytes Parenchymal Destruction Eosinophils Macrophages • Loss of alveolar attachments Neutrophils • Decrease of elastic recoil AIRFLOW LIMITATION Fully reversible Partially reversible Global initiative for chronic obstructive lungwww. themegallery. com diseases: GOLD 2015

www. themegallery. com Company Logo

Risk Factors for COPD Genetics Nutrition Asthma/airway hyperreactivity Low socio economic status Childhood respiratory Infections Aging Populations


Clues of COPD History v Chronic cough -/+ productive v Progressive , gradual) except exacerbation( v Weight loss v Smoking history , Family Hx of COPD v Occupation PE v Bilateral scattered wheeze v Rhonchi (audible through stethoscope) v Prolonged expiration v Over-inflation of the chest v Short cricosternal distance < 3 cm v Increased AP diameter > 5: 7 v Sign of pulmonary hypertension in late stage pulmonary hypertension

www. themegallery. com Company Logo

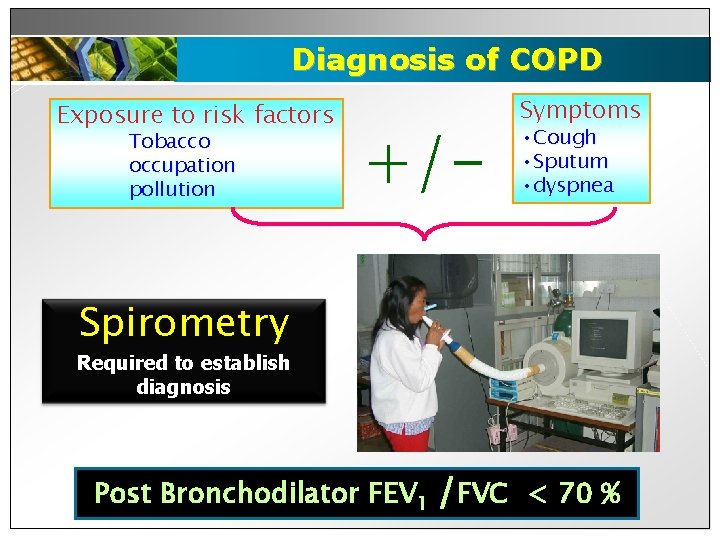
Diagnosis of COPD Exposure to risk factors Tobacco occupation pollution +/- Symptoms • Cough • Sputum • dyspnea Spirometry Required to establish diagnosis Post Bronchodilator FEV 1 /FVC < 70 %

New GOLD guideline 2015 Thai guideline 2010

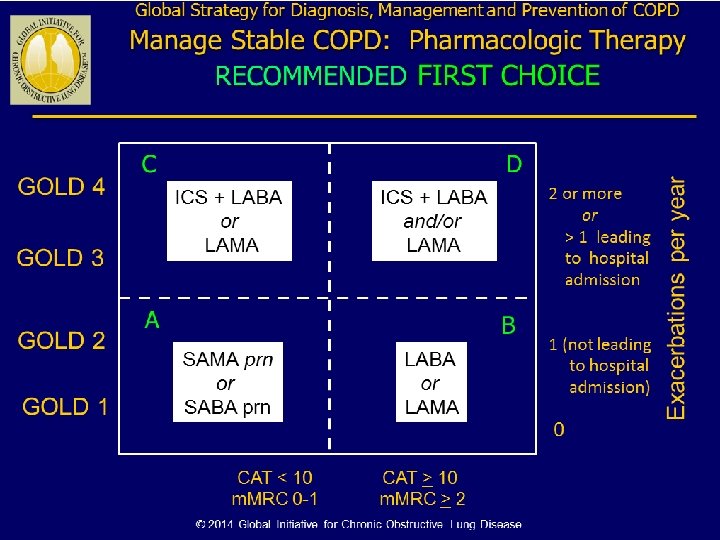
Global Strategy for Diagnosis, Management and Prevention of COPD Assessment of COPD § Assess symptoms § Assess degree of airflow limitation using spirometry § Assess risk of exacerbations § Assess comorbidities GOLD 2014

Assess symptoms Company Logo

www. themegallery. com Company Logo
![Combine these assessments symptoms risk of AE for the purpose of improving management Combine these assessments [symptoms + risk of AE] for the purpose of improving management](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-16.jpg)
Combine these assessments [symptoms + risk of AE] for the purpose of improving management of COPD Company Logo

www. themegallery. com 1. Assess symptoms first 2. Assess risk of exacerbations next Company Logo

Goal of therapy § Relieve symptoms § Improve exercise tolerance § Improve health status § Prevent disease progression § Prevent and treat exacerbations § Reduce mortality GOLD 2015 Reduce symptoms Reduce risk

www. themegallery. com Company Logo

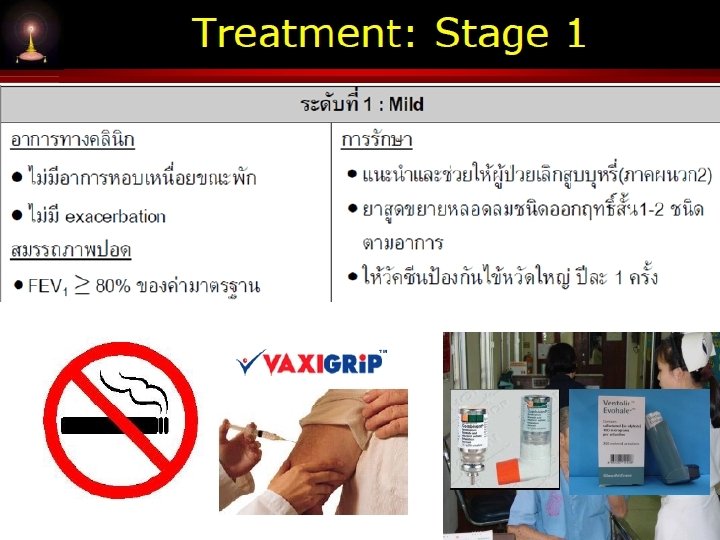
www. themegallery. com Smoking cessation + Physical activity + vaccination in all groups Pulmonary rehabilitation Company Logo in patient with impaired activity of daily living

www. themegallery. com Company Logo

www. themegallery. com , Peripheral edema due to right sided heart failure Company Logo

www. themegallery. com Company Logo

www. themegallery. com Company Logo

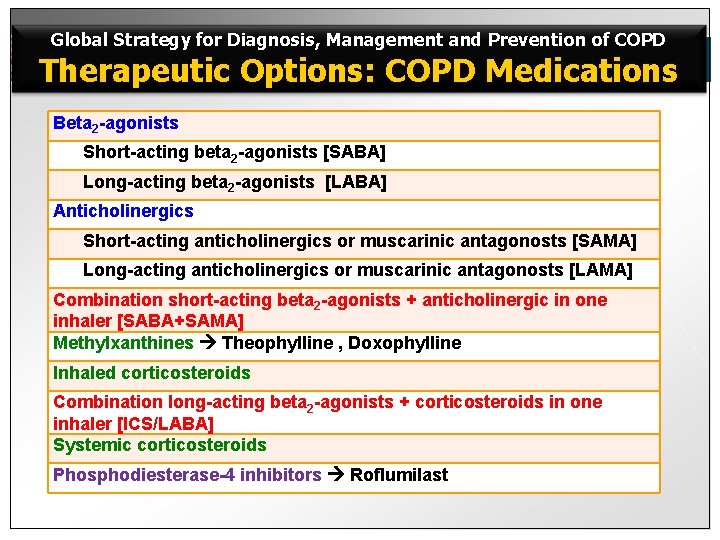
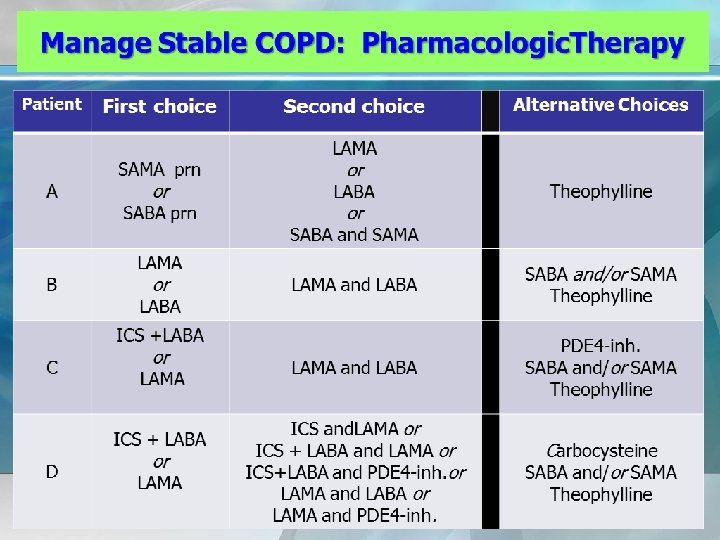
Global Strategy for Diagnosis, Management and Prevention of COPD Therapeutic Options: COPD Medications Beta 2 -agonists Short-acting beta 2 -agonists [SABA] Long-acting beta 2 -agonists [LABA] Anticholinergics Short-acting anticholinergics or muscarinic antagonosts [SAMA] Long-acting anticholinergics or muscarinic antagonosts [LAMA] Combination short-acting beta 2 -agonists + anticholinergic in one inhaler [SABA+SAMA] Methylxanthines Theophylline , Doxophylline Inhaled corticosteroids Combination long-acting beta 2 -agonists + corticosteroids in one inhaler [ICS/LABA] Systemic corticosteroids Phosphodiesterase-4 inhibitors Roflumilast
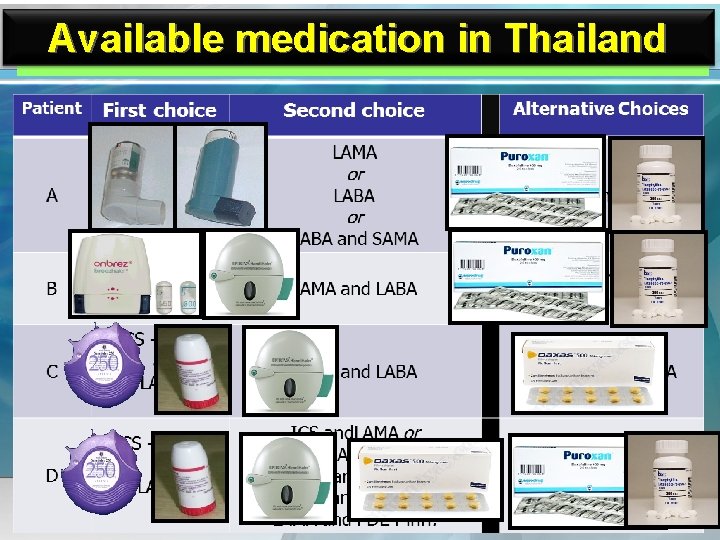
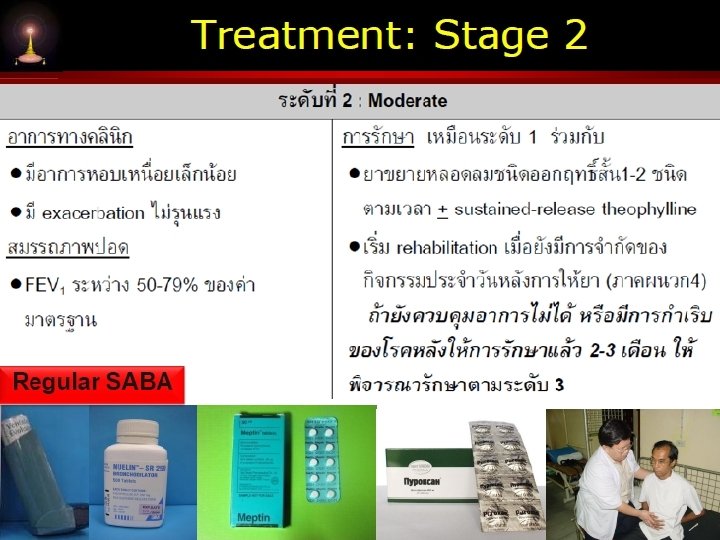
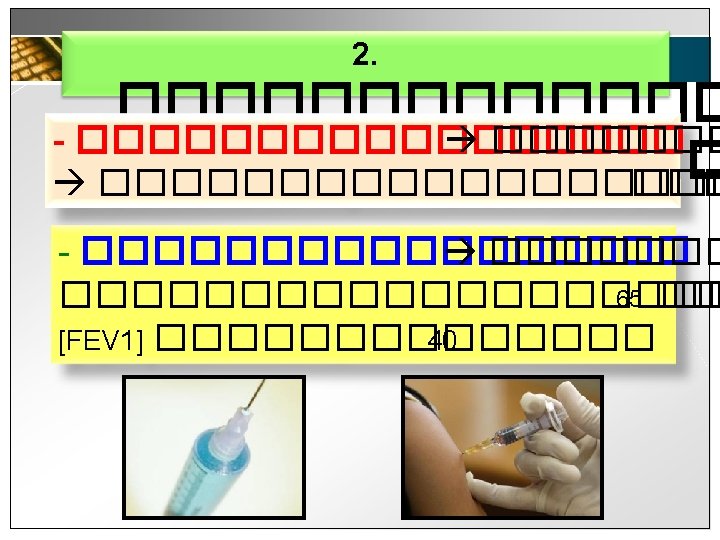
![Available medication in Thailand v Short acting bronchodilator SABA SAMA Berodual Ventolin SABASAMA Available medication in Thailand v Short acting bronchodilator [SABA , SAMA] Berodual Ventolin SABA+SAMA](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-26.jpg)
Available medication in Thailand v Short acting bronchodilator [SABA , SAMA] Berodual Ventolin SABA+SAMA SABA v Long acting bronchodilator Indacaterol [Onbrez] : LABA Tiotropium [spiriva] : LAMA
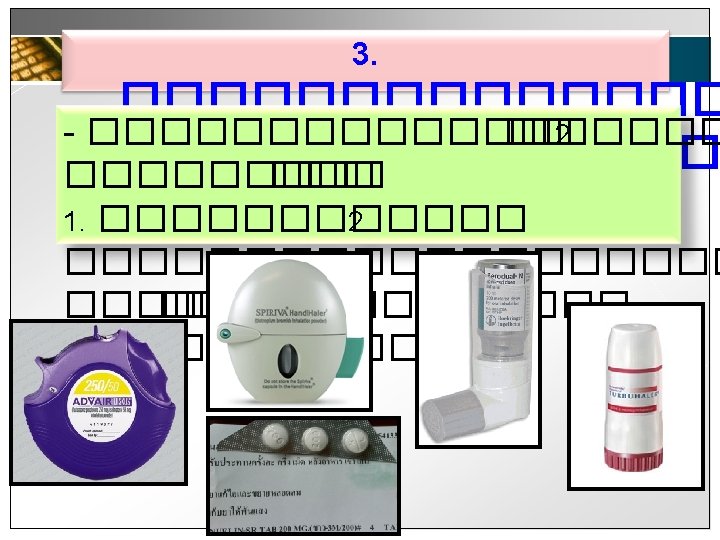
![Available medication in Thailand v Combined ICSLABA Seretide fluticasonesalmeteral Symbicort FormoterolBudesonide Available medication in Thailand v Combined ICS/LABA Seretide [fluticasone/salmeteral] Symbicort [Formoterol/Budesonide]](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-27.jpg)
Available medication in Thailand v Combined ICS/LABA Seretide [fluticasone/salmeteral] Symbicort [Formoterol/Budesonide]
![Available medication in Thailand v Methylxanthines Theophylline v PDE4 inhibitors Roflumilast Doxophylline Puroxan Available medication in Thailand v Methylxanthines Theophylline v PDE-4 inhibitors Roflumilast Doxophylline [Puroxan]](https://slidetodoc.com/presentation_image/243d406e158ce002cd63079ccd192102/image-28.jpg)
Available medication in Thailand v Methylxanthines Theophylline v PDE-4 inhibitors Roflumilast Doxophylline [Puroxan]

www. themegallery. com Available medication in Thailand Company Logo

Thai guideline 2010

www. themegallery. com Company Logo

www. themegallery. com Company Logo

www. themegallery. com Company Logo

www. themegallery. com Company Logo

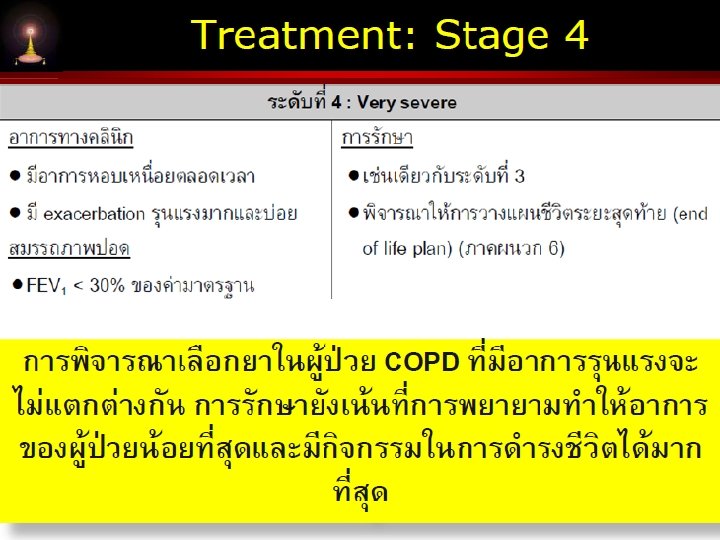
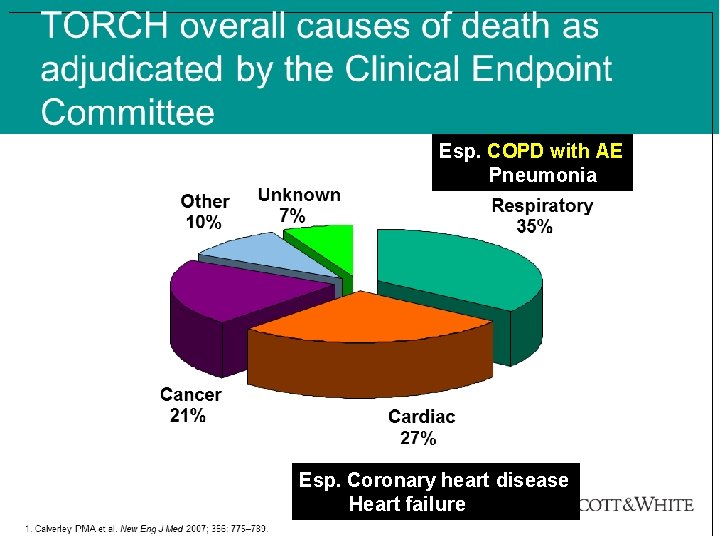
www. themegallery. com Esp. COPD with AE Pneumonia Esp. Coronary heart disease Heart failure Company Logo

www. themegallery. com Company Logo

Update in COPD AE prevention Patient with COPD At risk for acute exacerbation of COPD Eg. Hx of frequent AE in last year , severe COPD Non-pharmacological therapies and vaccination Pharmacological Inhaled therapies Recommended • Annual influenza vaccine • Pulmonary rehabilitation [AECOPD ≤ 4 week] • Education and case • management Recommended • LABA • LAMA • ICS + LABA Suggested • Pneumococcal vaccine • Smoking cessation Pharmacological oral therapies Suggested • Long term macrolides • Systemic corticosteroids in first 30 days after AE • PDE inhibitors • Theophylline • N-acetylcysteine or carbocysteine CHEST 2015; 147 ( 4 ): 894 - 942









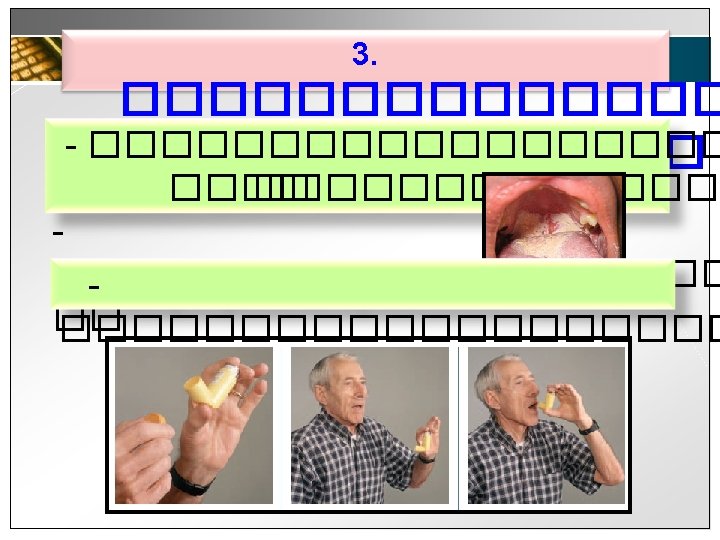
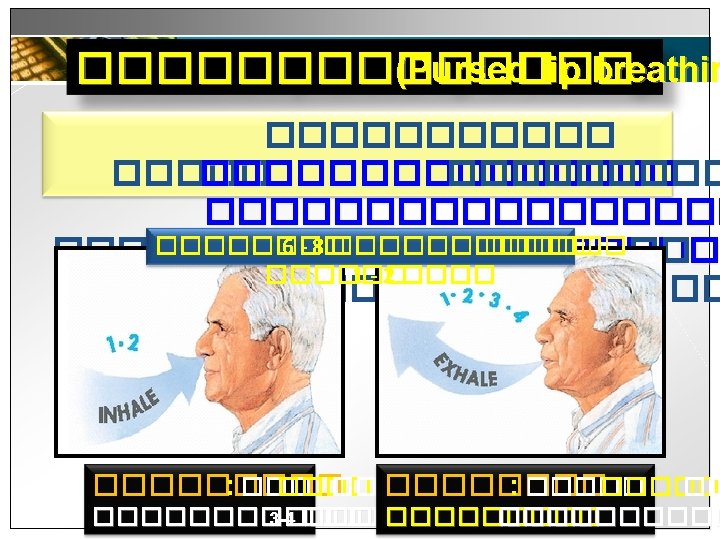
6. ����������������� (Pursed lip breathing ������ (Huff coughing or Forced Expiratory technique( ���


������� (Pursed lip breathin


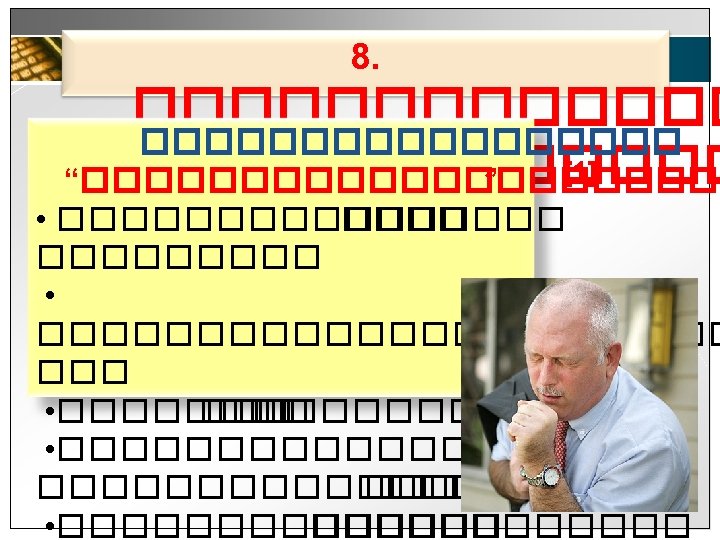
������ (Forced expiratory technique(





Question ? ?

Company Logo