CommunityDriven Tuberculosis Interventions for Aboriginal Communities Jessica Harper

Community-Driven Tuberculosis Interventions for Aboriginal Communities Jessica Harper & Nash Dhalla February 19, 2015 Hyatt Regency Vancouver

Conflict of Interest: Neither presenter (Nash Dhalla, RN, BSc. N or Jessica Harper, RN, BSc. N) have any affiliation financial or otherwise, with a commercial or other industry interest that may bias our presentation.

Outline 1. 2. 3. 4. TBSAC: Who we are What is TB? TST vs IGRA Feasibility of Portable Incubator in LTBI testing 5. Challenges 6. Next Steps

TB Services in BC • Centralized: pharmacy, labs, database, physician consultant, and nurse consultant services provided by TB Services, BC Centre for Disease Control • TB Services for Aboriginal Communities (TBSAC): provides TB services to Health Centers located onreserve, funded and delivered in partnership with First Nations Health Authority (FNHA). 4
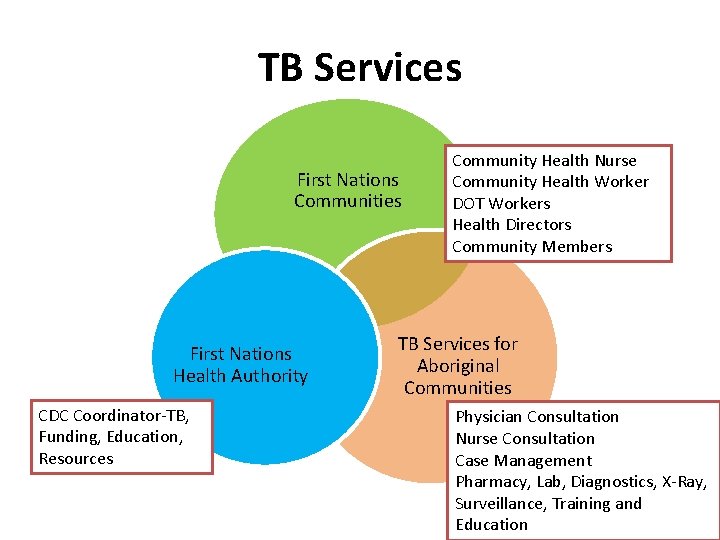
TB Services First Nations Communities First Nations Health Authority CDC Coordinator-TB, Funding, Education, Resources Community Health Nurse Community Health Worker DOT Workers Health Directors Community Members TB Services for Aboriginal Communities Physician Consultation Nurse Consultation Case Management Pharmacy, Lab, Diagnostics, X-Ray, Surveillance, Training and Education

TB Team BCCDC (TBSAC) • Dr. Victoria Cook, TBSAC Physician • Shawna Buchholz, Clinical Nurse Educator • Nash Dhalla, Nurse Consultant • Karen Beinhaker, Nurse Consultant FNHA, Health Protection • Jessica Harper, CDC Coordinator, TB 6

Background: What is TB? • • • Mycobacterium tuberculosis Airborne disease Generally infects the lungs In BC: incidence rate of ~7 per 100 000 Symptoms: coughing, fever, weight loss, night sweats • Curable and Preventable!

Background: What is LTBI? • “Sleeping” Latent TB infection (LTBI): – Infected with bacteria? – Symptoms present? – Infectious? YES NO NO • A healthy individual infected with LTBI has a 5 -10% risk of developing active TB over their lifetime (BCCDC TB Control Manual, 2012)
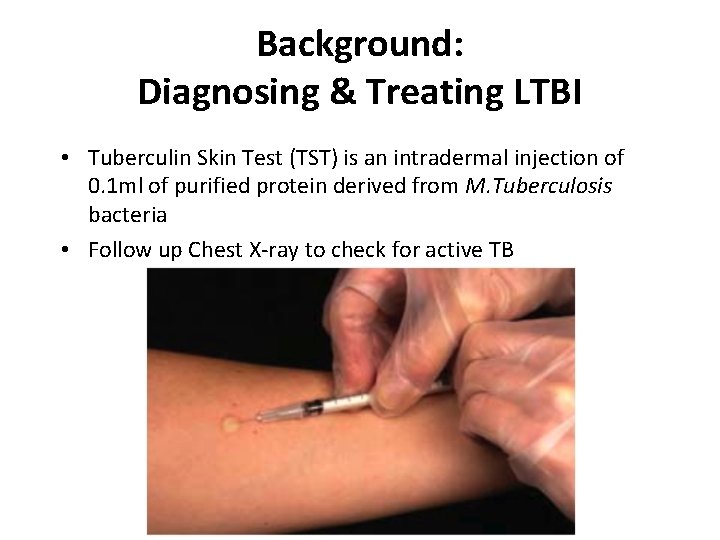
Background: Diagnosing & Treating LTBI • Tuberculin Skin Test (TST) is an intradermal injection of 0. 1 ml of purified protein derived from M. Tuberculosis bacteria • Follow up Chest X-ray to check for active TB

Background: Diagnosing & Treating LTBI • Recommended for preventative therapy: – Isoniazid for 9 months – 270 doses OR – Rifampin for 4 months – 120 doses • Decision to start treatment is based on: – Context of TST – likelihood of false positive – Reason client was being tested – Risk of progression to active disease – Ability to adhere to medication – Possible intolerance to medication – Alcohol use, desire for pregnancy, etc. (BCCDC TB Control Manual, 2012)

The IGRA Test • Interferon Gamma Release Assay (IGRA) • Detects interferon gamma released from WBC • Two tests: Quantiferon Gold and T-Spot • BC: offered in Vancouver, New Westminster, Victoria, Prince George and Kelowna
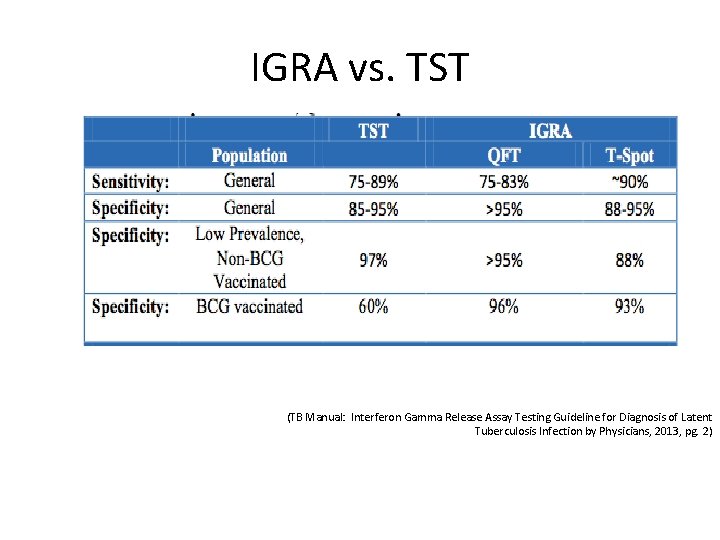
IGRA vs. TST (TB Manual: Interferon Gamma Release Assay Testing Guideline for Diagnosis of Latent Tuberculosis Infection by Physicians, 2013, pg. 2)
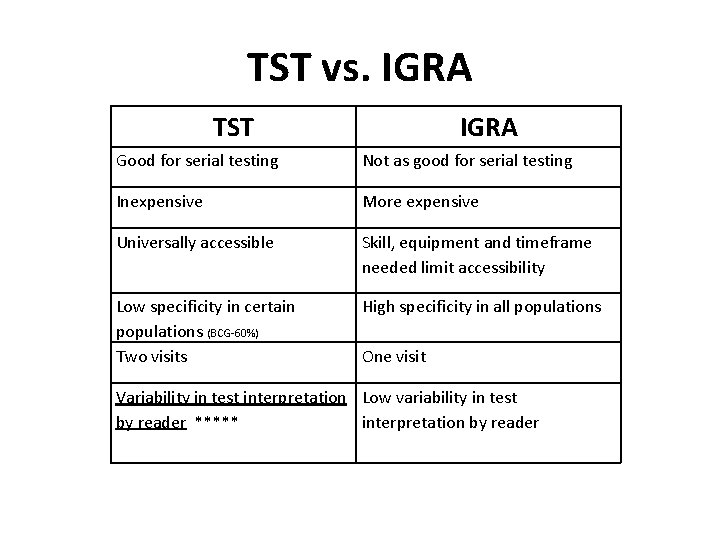
TST vs. IGRA TST IGRA Good for serial testing Not as good for serial testing Inexpensive More expensive Universally accessible Skill, equipment and timeframe needed limit accessibility Low specificity in certain populations (BCG-60%) Two visits High specificity in all populations One visit Variability in test interpretation Low variability in test by reader ***** interpretation by reader

WHY IGRA? • To identify the proportion of patients in whom treatment for LTBI could be avoided because an IGRA test was negative yet a TST test was positive. • To determine if there is a statistically significant difference in treatment adherence between BC residents who have had LTBI confirmed with an IGRA test and those whose diagnoses was made using a TST only.

IGRA Feasibility In First Nations Communities • Currently IGRA is offered at the BCCDC, in New Westminster, Victoria, Kelowna and Prince George • Increase access to testing for patients who are less likely/able to travel for testing: – Remote communities – Outbreak investigation – Enhanced communities • Identify and treat true LTBI • Are communities interested in the IGRA test?

IGRA testing: Feasibility • TBSAC Team & Community Leaders discussed IGRA – Based on enhanced community survey – Strong links with HCP – Geographic location – IGRA available in Canada 2007 with strong evidence base – BCG Factor – Community engagement

Results: Feasibility Test ü Community approval ü Meet with BCCDC lab to agree on expectations of how samples are delivered ü Develop detailed protocol on sample collection, processing and transportation to lab – – – Confirm site visit date(s) Conduct site visit & feasibility test Determine results Summarizing results Lessons learned

Vision of the FNHA In partnership with BC First Nations Communities the FNHA TBSAC program is working towards the Vision of: “Healthy, Self-determining and Vibrant BC First Nations Children, Families and Communities. ”

Acknowledgements BCCDC- Zoonotic Lab Yvonne Simpson Muhammad Morshed Quantine Wong FNHA and TBSAC team April Mac. Naugton Dr. Isaac Sobol Dr. Victoria Cook Jane Lopez Maggie Wong Shawna Buchholz Karen Beinhaker • • First Nations Communities Healthcare Professionals Community members Community leaders Thank You!

Contact Information TBSAC Nurses: • Nash Dhalla: (604)707 -2695 Nash. dhalla@bccdc. ca • Karen Beinhaker: (604)7072732 karen. beinhaker@bccdc. ca • Shawna Buchholz: (250)8784928 Shawna. buchholz@bccdc. ca FNHA Nurse: • Jessica Harper: (604)693 -6955 jessica. harper@fnha. ca TBSAC Fax: (604)707 -2690 TBSAC Toll Free: 1 -888 -569 -2299 FNHA Health Protection Toll Free: 1 -844 -364 -2232 20

Thank You!
- Slides: 21