CommunityBased Care Coordination The Pathways Hub Model Why
Community-Based Care Coordination The Pathways Hub Model

Why we need Community Based Care Coordination? ½ ⅓ ½ 15 MORE THAN of patients can’t state their diagnosis when leaving the hospital MORE THAN of patients can’t explain their medications LESS THAN of patients saw a primary care physician within 2 weeks of leaving the hospital patients has an adverse event transitioning from hospital to home IN

Reducing Risk for Communities 3
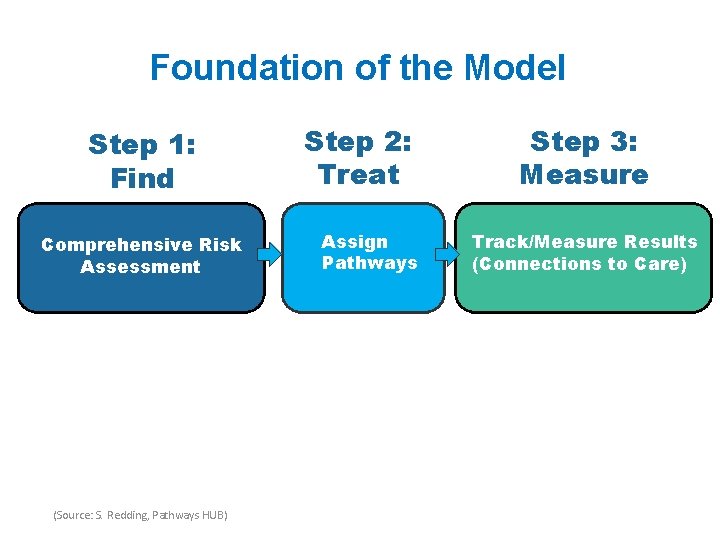
Foundation of the Model. Step 1: Find Comprehensive Risk Assessment (Source: S. Redding, Pathways HUB) Step 2: Treat Assign Pathways Step 3: Measure Track/Measure Results (Connections to Care) 4

Pathways Community Hub
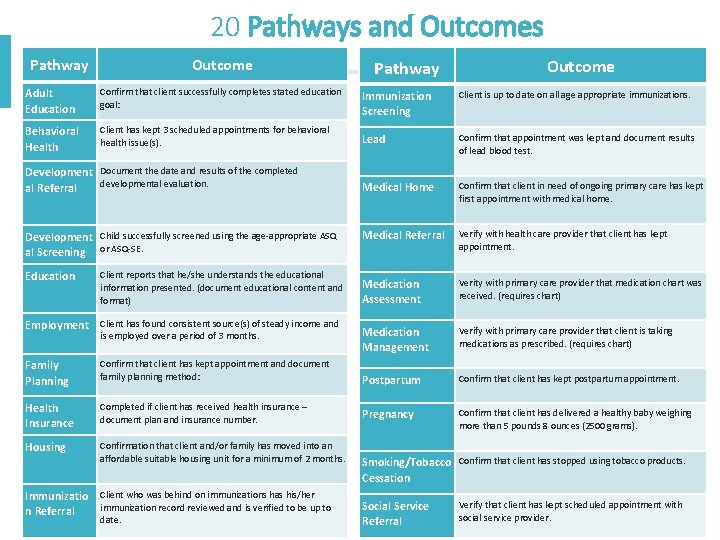

20 Pathways and Outcomes Pathway Outcome Adult Education Confirm that client successfully completes stated education goal: Immunization Screening Client is up to date on all age appropriate immunizations. Behavioral Health Client has kept 3 scheduled appointments for behavioral health issue(s). Lead Confirm that appointment was kept and document results of lead blood test. Medical Home Confirm that client in need of ongoing primary care has kept first appointment with medical home. Medical Referral Verify with health care provider that client has kept appointment. Medication Assessment Verity with primary care provider that medication chart was received. (requires chart) Medication Management Verify with primary care provider that client is taking medications as prescribed. (requires chart) Development Document the date and results of the completed developmental evaluation. al Referral Development Child successfully screened using the age-appropriate ASQ al Screening or ASQ-SE. Education Client reports that he/she understands the educational information presented. (document educational content and format) Employment Client has found consistent source(s) of steady income and is employed over a period of 3 months. Family Planning Confirm that client has kept appointment and document family planning method: Postpartum Confirm that client has kept postpartum appointment. Health Insurance Completed if client has received health insurance – document plan and insurance number. Pregnancy Confirm that client has delivered a healthy baby weighing more than 5 pounds 8 ounces (2500 grams). Housing Confirmation that client and/or family has moved into an affordable suitable housing unit for a minimum of 2 months. Immunizatio n Referral Client who was behind on immunizations has his/her immunization record reviewed and is verified to be up to date. Smoking/Tobacco Confirm that client has stopped using tobacco products. Cessation Social Service Referral Verify that client has kept scheduled appointment with social service provider.
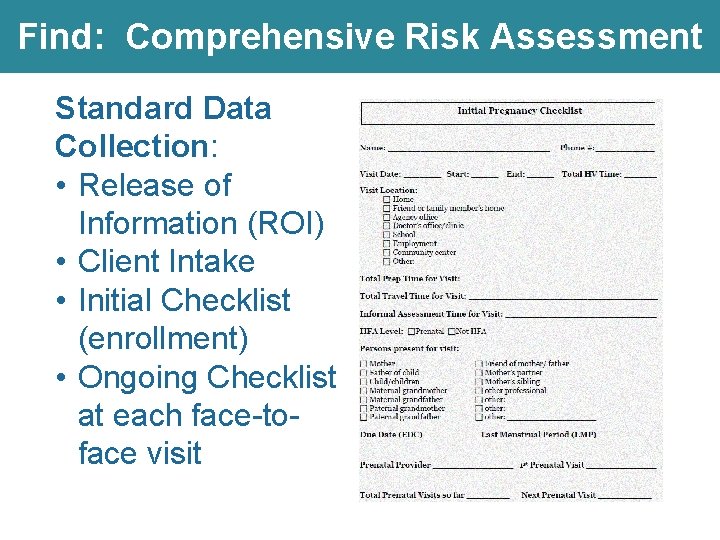

Find: Comprehensive Risk Assessment Standard Data Collection: • Release of Information (ROI) • Client Intake • Initial Checklist (enrollment) • Ongoing Checklist at each face-toface visit
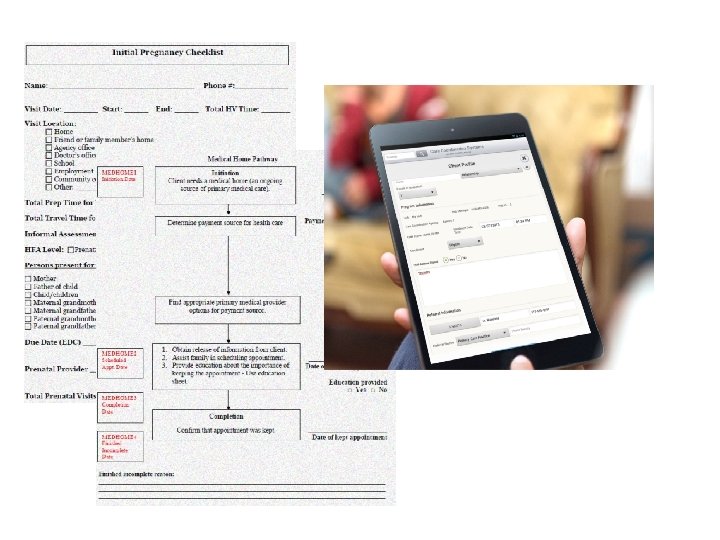
Data Collection 9
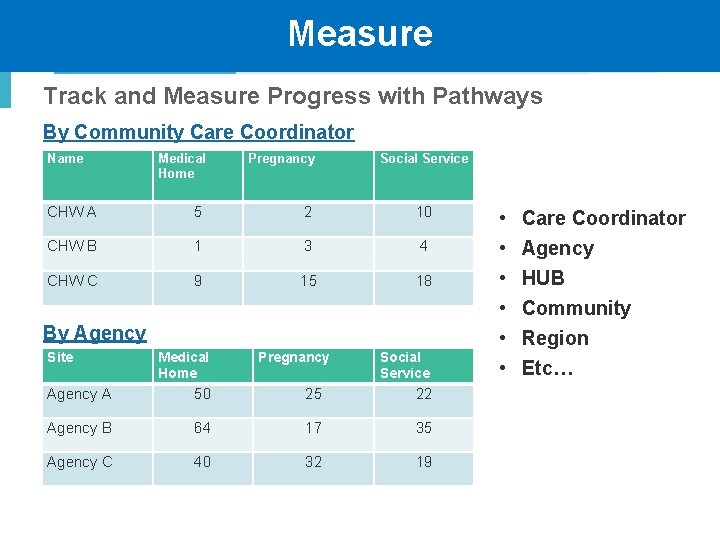
Measure Track and Measure Progress with Pathways By Community Care Coordinator Name Medical Home Pregnancy Social Service CHW A 5 2 10 CHW B 1 3 4 CHW C 9 15 18 By Agency Site Medical Home Pregnancy Social Service Agency A 50 25 22 Agency B 64 17 35 Agency C 40 32 19 • • • Care Coordinator Agency HUB Community Region Etc… 10

The Role of the HUB • • • “Air traffic control” for community based care coordination agencies (CCAs) Streamlines referrals Eliminates duplication Uses common data collection across all contracted CCAs (Client Intake, Checklists, Pathways, Tools) Develops contracts with payers – payment for Pathways Develops contracts with CCAs to pay for care coordination services Gives feedback to Referral Partners (client found, enrolled, etc. ) Works closely with Pathfinder Community Hub Advisory Council to review data, gaps in services, identify priorities Quality improvement plan to identify areas of need within the network of CCAs Obtains national Pathways Community HUB certification and participates with partner HUBs

Key Points of a HUB • The HUB cannot employ its own care coordinators. • There is only one Pathways Community HUB in a community or region. • The HUB must be an independent legal entity or an affiliated component of a legal entity. • The HUB must be based in the community or region it serves. • There must be a Community Advisory Board made up of members reflecting the community or region the HUB serves 12

Distinctions between Pathways & HUB Pathways, the model - Patient-centered, care coordination tool - Identifies and “translates” patient risks - Measured outcomes - Payments for measured Pathway outcomes Community HUB - Tracks Pathways (outcomes) across agencies - Eliminates duplication - Streamlines referrals - Provide infrastructure for community-based care coordination - Involve braided funding – Pathways can be purchased by different funders 13

Care Coordination Agency (CCA) Role Contracts with the BHT HUB to provide community based care coordination services Commits to having a full-time equivalent community health worker (CHW), or Care Coordinator Commits to having a supervisor for CHW/CC Understands all requirements of participating in HUB network: • Attends all required trainings; 230 hours which includes 5 days of Community Care Coordination and 5 days of Pathways and CCS Platform training, along with 2 -4 weeks of practicum. • Attends all required meetings. • Uses data platform to collect all data within timeline established by HUB. • Participates in quality improvement.
Our Tools. Checklists assess eligibility and identify access to care, financial issues and health improvement barriers Pathways work through barriers; provide documentation and accountability for the patient, agency and health system

Pathways HUB Connect enables organized and efficient community care coordination. 16
Pathways Risk. Q tm Health Behavioral Health Social Patient Activation Family & Personal Health Management Financial
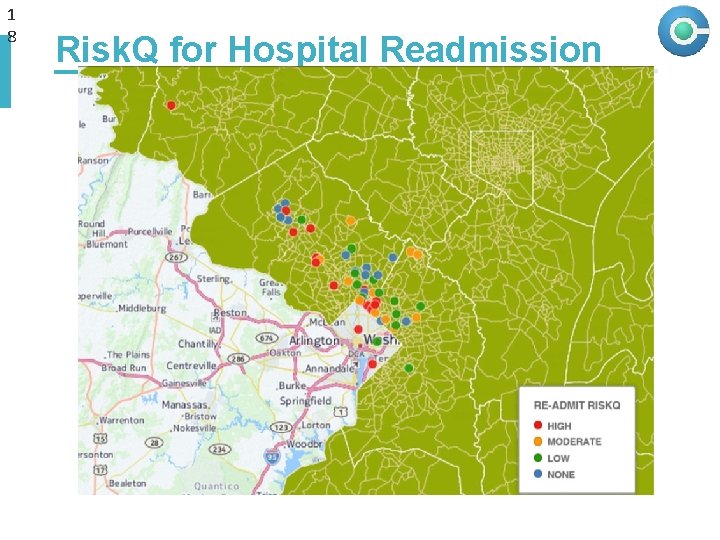
1 8 Risk. Q for Hospital Readmission

Pathways Mobile Real-time Pathways and SDOH information from the community 19

Care Coordination Payer Role • Payers are Managed Care Organizations, Foundations, City Governments and/or County Governments who contracts with the Hub • Establishes contracts based on population covered and Pathways and Tools that are compensated • Uses Outcome Based Units (OBUs) to develop payment strategy

Ferry County Pilot Outcomes RECIDIVISM • Reduction in recidivism in Ferry County Jail by 20% by December 2018 Ferry County recidivism rate is 62% (Ferry County data 2015) National statistics show that 43% of all inmates return to prison within three years of their release (Pew, 2011) Ferry County is 274% higher incarcerated than Washington State average (Vera. org, 2013) COST • Reduction in cost of providing jail health services in Ferry County by 20% by December 2018 Annual County Budget $2 million / Annual Jail Budget $800, 000 / Annual Jail Health Services $45, 000 (Ferry County data 2015) ED DIVERSION • Reduction of emergency department utilization for ambulatory sensitive conditions in target population in Ferry County from 20% to 16% of all ED visits by December 2018 (both inmates and their families) National emergency department overuse is $38 billion in wasteful health care spending; 56% or roughly 67 million visits, are potentially avoidable. Significant Savings, average cost of an ED visit is $580 more than the cost of an office health care visit (National Quality Forum, 2016) YTD 2018: 8 new clients of the 21 currently active 44 completed pathways, respective RVUs: 78. 5 1 Care Coordinating Agency, Rural Resources Our goal is to serve 60 clients by 12/31/2018.

The Hub 2018 Spokane County Planning Spokane County is contracting with BHT to implement a Jail Transitions Pathways pilot. • This is funded via a Department of Justice Grant, just under $1 million. • Pathways is one of the strategies being used for Re-Entry • Target population: individuals transitioning out of jail. • Planning steps include a BHT RFP process to contract two Care Coordinating Agencies who will employ one FTE Care Coordinator and Supervisor each • BHT will use the funding to subsidize, a portion, of the care coordinator salaries and outcome based payments for the 2 year period. • The Hub will coordinate a Pathways and Care Coordination Systems training for mid-October • Launch date – The Hub will receive and route referred clients in November 2018 GOAL: at least 200 clients through the course of the grant 2 Care Coordinating Agencies BHT’s goal is to serve 200 clients annually starting in 2019

The Hub and Collaborative Planning • To implement the Medicaid Transformation Projects, BHT will utilize a county based Community Health Transformation Collaboratives (Collaboratives) structure • BHT utilizes a technical council model to recommend setting and programmatic priorities for each of the selected 4 projects. The Hub Council recommended and the board approved, a policy allowing each collaborative a choice on population focus: Jail Transition or High Risk Pregnant Moms) • The BHT Board of Directors have allocated funds to support proof of concepts in each county that includes: • MTP funds will support all initial Hub start up costs (technology, training, staffing) and a subsidize 3 month start up stipend as outcomes are achieved • Expectation of MCOs to share costs for outcomes (Year 1 -25%, Year 2 -50%, Year 3 -75%) • Rural CCOs will receive a monthly stipend and lower per outcome payment ($15) to offset small population and Spokane will receive ($25) • Collaboratives have included their decisions into their Collaborative Transformation Plans submitted.

The Hub Council • The Community-Based Care Coordination Advisory Council (Hub Council) are primary care, behavioral health, county, public health, and social determinant of health service providers who are responsible for identifying needs and aligning resources and infrastructure of the region. • The Council is co-chaired by VOA Executive Director Fawn Schott (community member) and Rural Resources Executive Director, Greg Knight (board member) • A key goal of the Council is to align data infrastructure, better coordinate community resources and launch efforts to better weave care coordination funding • Additionally, the Hub Council will also work to align community based activities with Health Homes, Hot Spotters, Diabetes Care Coordination, etc. Ø One example is the Spokane Fire Department’s CARES team; a volunteer team of EWU MSW students whose care coordination work serves mostly Medicare clients; they are looking for a structured care coordination model and case management platform. The overall program is currently paid through Spokane City funding.

The Hub - MCOs and IT considerations As with other care coordination models such as Health Homes, BHT views the Pathways model as complementing existing MCO care coordination efforts. Wherever possible, The Hub would like to align referral processes and resources. BHT is working with other ACHs and DOH for a shared services agreement of the CCS platform and training resources. Other needs such as statewide alignment of a Pathways evaluation is also being discussed with other ACHs.

Overview of Approved Funding This set of projects is designed to be a Proof of Concept > Effectively “prove” this concept by staying true to the model that is based on Care Coordinating Agencies at risk for success via achievement of the Pathways Outcomes; We are focused on two target populations for the duration of the Medicaid Transformation Waiver per Board Policy: People transitioning out of Jail and Pregnant Moms We expect: > > > Each Collaborative will select one target populations Waiver $to pay for the start up costs for technology, consulting and capacity payments to partners to get started. Expect to have a shared investment with partners who benefit from the success of the project, by Year 4 we expect to have shared savings model in place. We want MCO’s to join us in the partnership. , it is our intent to partner with each MCO, but if an MCO chooses not to partner, referring agencies will note this and It’s the intent of BHT to seek out additional funding to support Pathway outcome payments.
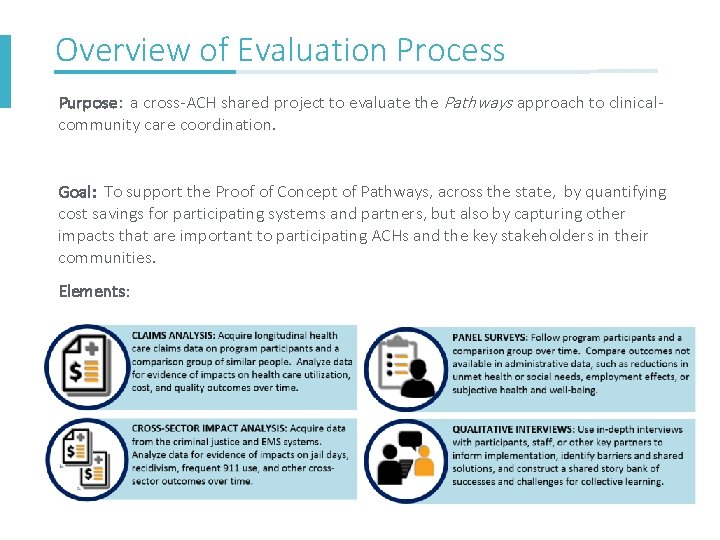
Overview of Evaluation Process Purpose: a cross-ACH shared project to evaluate the Pathways approach to clinicalcommunity care coordination. Goal: To support the Proof of Concept of Pathways, across the state, by quantifying cost savings for participating systems and partners, but also by capturing other impacts that are important to participating ACHs and the key stakeholders in their communities. Elements:

Hub leadership: Alison Poulsen, Executive Director Alison@betterhealthtogether. org Jenny Slagle, Director of Community Services jenny@betterhealthtogether. org Justin Botejue, Senior Project Manager justin@betterhealthtogether. org
- Slides: 27