Communityacquired Hospitalacquired Antimicrobial stewardship program ASP RDUAMR ASP


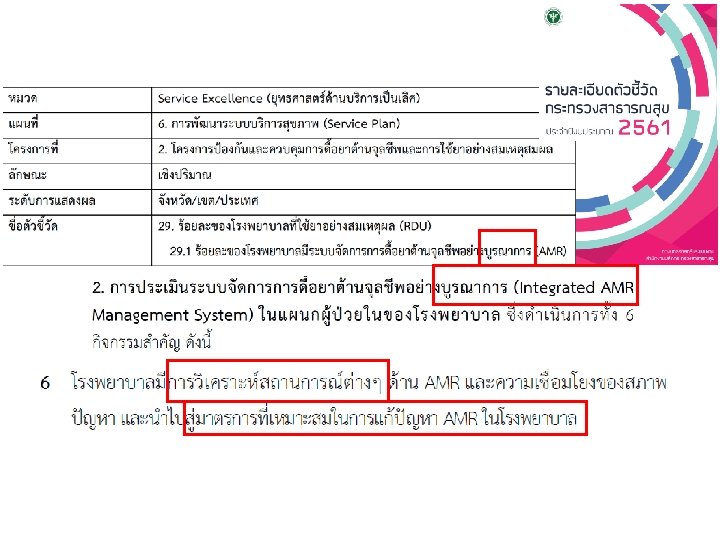

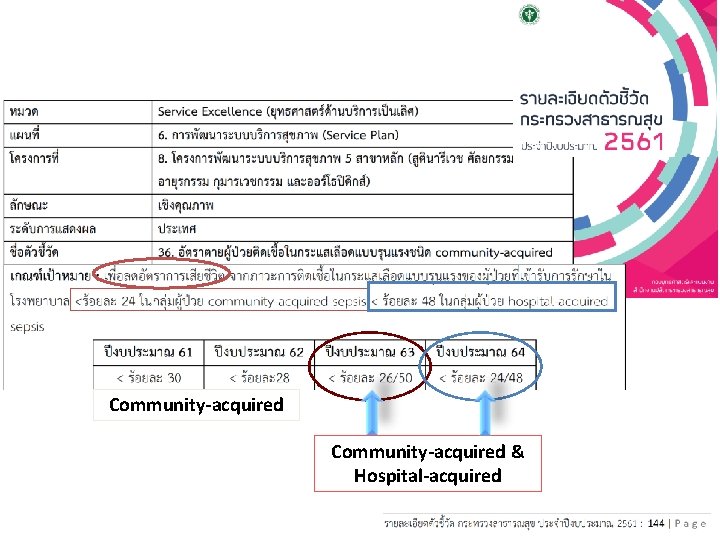
Community-acquired & Hospital-acquired
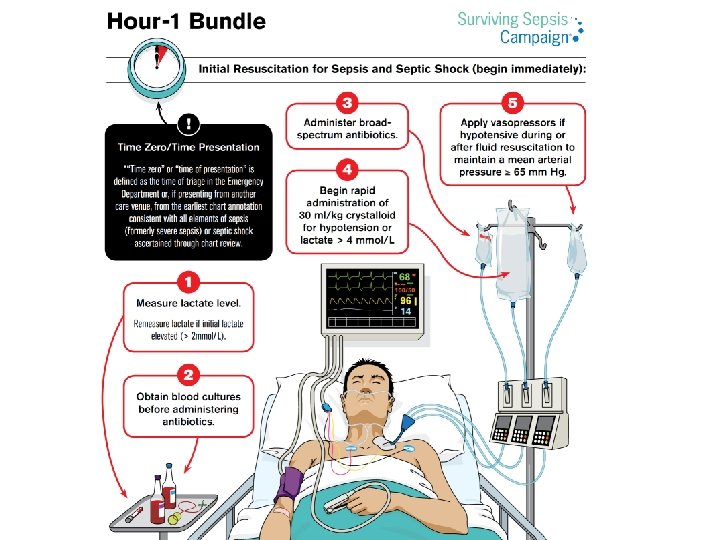
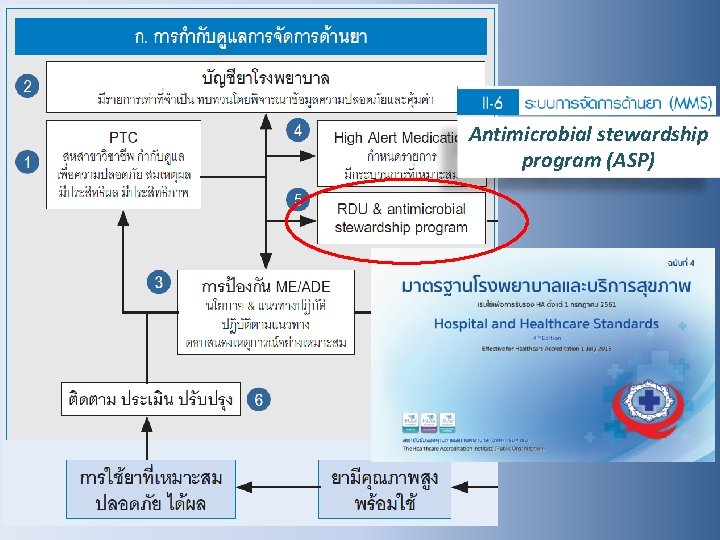
Antimicrobial stewardship program (ASP)

RDU-AMR ������������� �� ทไมจำเปน ASP วตถประสงค : �� Spectrum-Number-Duration (S-N-D) ASP DUE ๑. Pre-authorization; controlled/restricted: S-N-D STM; Systematic work -out IDV STM IDV; Individualized work- out ๒. Dose adjustment ; N-D ๓. Unnecessarily duplicative therapy : S-N-D ๔. Drug-Drug interaction: N-D ๕. Antibiotic “time outs : : S-N-D ๖. Switch therapy (IV to PO): S-N-D ๗. Dose optimization: D ๘. Escalation & De-escalation N-D . Time to Appropriate ATB within 1 hr & Sepsis bundle Individualized �������� SEPSIS

ตวช วดท 6 7 8 9 21 ชอ ตวชวด RDU 61 รอยละ ATB ��������������� รอยละ ATB ������������������������� อตราการตดเชอดอยาในกระแสเลอด [���������� : Staphylococcus aureus, Streptococcus pneumoniae, Enterococcus faecium, Acinetobacter spp. , Pseudomonas spp. E. coli, K. pneumoniae, Salmonella spp. ] กลมยาทเฝาตดตามการ ดอ : Fluoroquinolone (FQ), Beta-lactam (Penicicillin, Third gen. ceph. , Carbapenem)
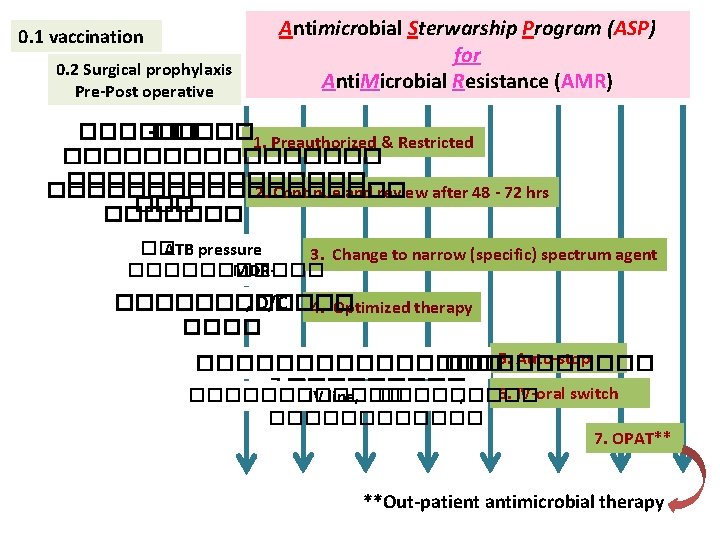
0. 1 vaccination 0. 2 Surgical prophylaxis Pre-Post operative Antimicrobial Sterwarship Program (ASP) for Anti. Microbial Resistance (AMR) ������ -����� 1. Preauthorized & Restricted ������������������ 2. Continue and review after 48 - 72 hrs ������� �� ATB pressure 3. Change to narrow (specific) spectrum agent ������ MDRPDR ������ , D/C 4. Optimized therapy �������������� ��� 5. Auto-stop 7 ��� 6. IV-oral switch ������ IV ������� line, ������ 7. OPAT** **Out-patient antimicrobial therapy

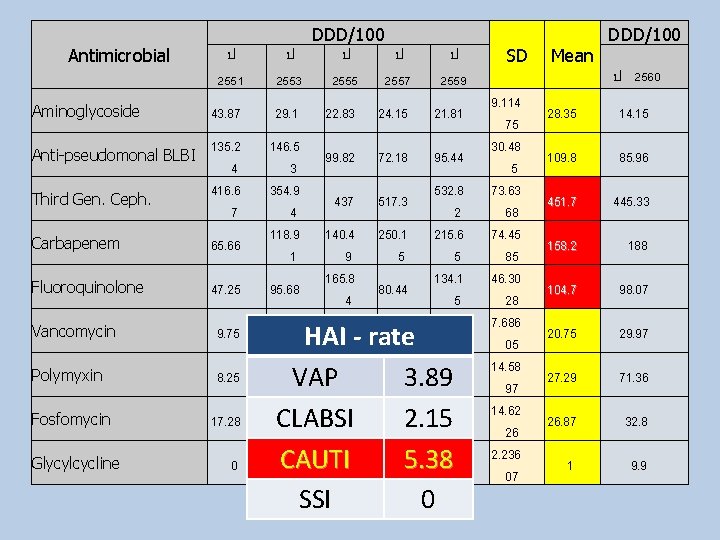
Antimicrobial Aminoglycoside Anti-pseudomonal BLBI Third Gen. Ceph. ป 2551 DDD/100 ป ป ป 2553 2555 2557 43. 87 29. 1 135. 2 4 416. 6 7 146. 5 3 354. 9 4 118. 9 1 Carbapenem 65. 66 Fluoroquinolone 47. 25 95. 68 ป 2559 22. 83 24. 15 21. 81 99. 82 72. 18 95. 44 437 517. 3 140. 4 9 165. 8 4 250. 1 5 80. 44 532. 8 2 215. 6 5 134. 1 5 15. 77 HAI 24. 42 - rate 26. 11 Vancomycin 9. 75 Polymyxin 8. 25 17. 3 VAP 31 34. 753. 89 45. 17 Fosfomycin 17. 28 10. 17 28. 76 CLABSI 29. 52. 15 48. 64 CAUTI 5 0 SSI 05. 38 0 Glycylcycline 0 27. 7 0 SD 9. 114 75 30. 48 5 73. 63 68 74. 45 85 46. 30 28 7. 686 05 14. 58 97 14. 62 26 2. 236 07 Mean DDD/100 ป 2560 28. 35 14. 15 109. 8 85. 96 451. 7 445. 33 158. 2 188 104. 7 98. 07 20. 75 29. 97 27. 29 71. 36 26. 87 32. 8 1 9. 9
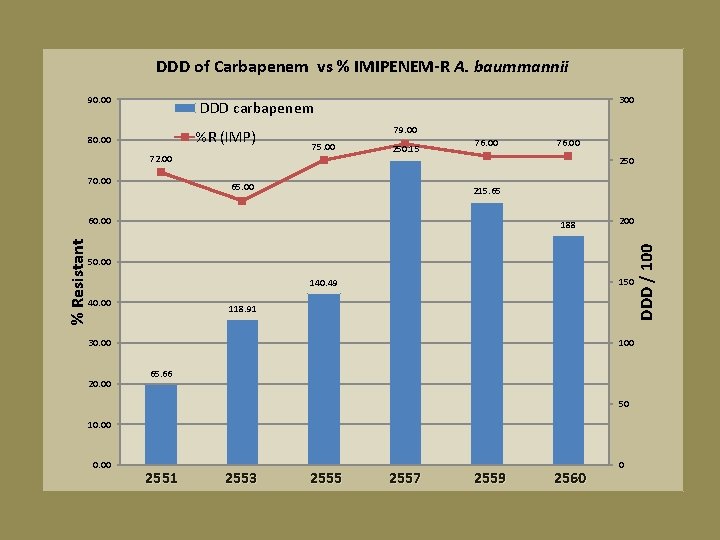
DDD of Carbapenem vs % IMIPENEM-R A. baummannii 300 DDD carbapenem %R (IMP) 80. 00 72. 00 70. 00 79. 00 75. 00 250. 15 65. 00 76. 00 250 215. 65 60. 00 % Resistant 76. 00 188 200 50. 00 150 140. 49 40. 00 118. 91 30. 00 20. 00 100 65. 66 50 10. 00 2551 2553 2555 2557 2559 2560 0 DDD / 100 90. 00
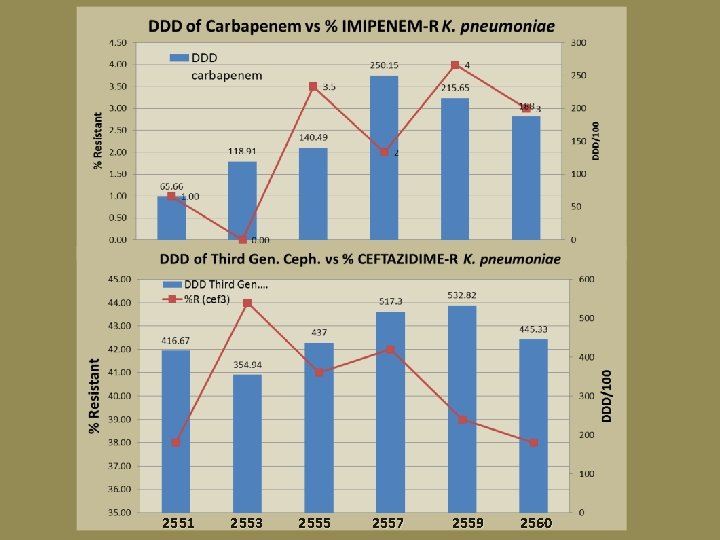
2551 2553 2555 2557 2559 2560
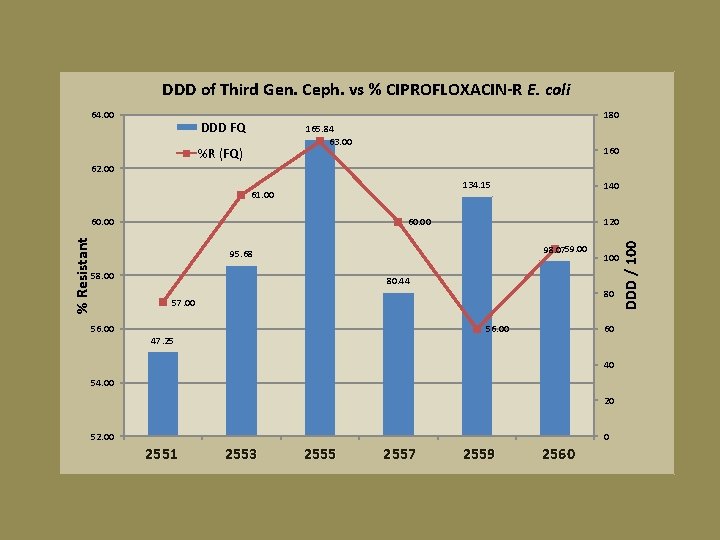
DDD of Third Gen. Ceph. vs % CIPROFLOXACIN-R E. coli 64. 00 180 DDD FQ 165. 84 63. 00 %R (FQ) 160 62. 00 134. 15 % Resistant 60. 00 140 60. 00 120 98. 0759. 00 95. 68 58. 00 80. 44 80 57. 00 56. 00 100 56. 00 47. 25 60 40 54. 00 20 52. 00 0 1 2551 2 2553 3 2555 4 2557 5 2559 6 2560 DDD / 100 61. 00

AMR pathogen (DATA) list of RDU-AMR strategies ����������������� ����� Gram negative Bacteria 1. A. baumannii: colistin , carbapenem-R 2. P. aeruginosa: colistin-R, carbapenem-R, Pip. Taz-R 3. E. coli: carbapenem-R, ceftriaxone-R (ESBL), CIPROFLOXACIN-R 4. K. pneumoniae: carbapenem-R, ceftriaxone-R (ESBL), colistin-R 5. Salmonella spp: ciprofloxacin-R, ceftriaxone-R (ESBL), colistin-R Gram Positive Bacteria 1. Enterococcus: vancomycin-R 2. S. aureus, methicillin-R, vancomycin-I and R 3. S. pneumoniae: penicillin-R, macrolide-R, 3 rd gen ceph -R
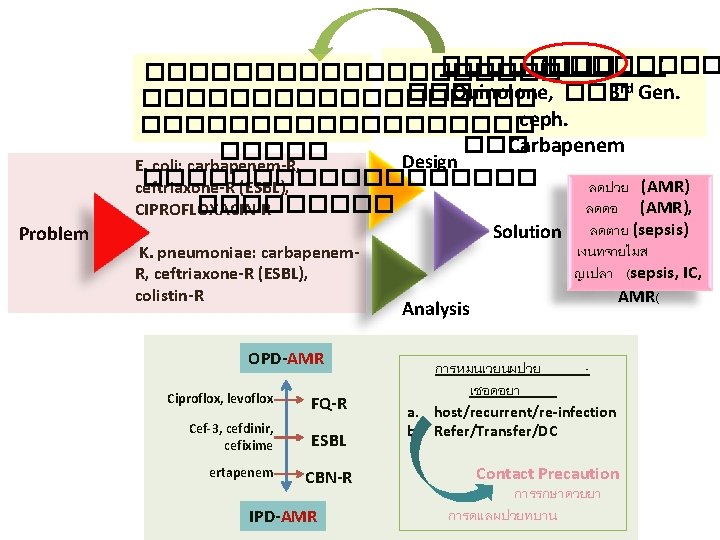
�������� ( ���������� ��� Quinolone, ��� 3 rd Gen. ��������� ceph. ��������� ��� Carbapenem ����� Design E. coli: carbapenem-R, ��������� ลดปวย (AMR) ceftriaxone-R (ESBL), ����� ลดดอ (AMR), CIPROFLOXACIN-R Problem K. pneumoniae: carbapenem. R, ceftriaxone-R (ESBL), colistin-R OPD-AMR Ciproflox, levoflox FQ-R Cef-3, cefdinir, cefixime ESBL ertapenem CBN-R IPD-AMR Solution Analysis การหมนเวยนผปวย เชอดอยา ลดตาย (sepsis) เงนทจายไมส ญเปลา (sepsis, IC, AMR( - a. host/recurrent/re-infection b. Refer/Transfer/DC Contact Precaution การรกษาดวยยา การดแลผปวยทบาน


Bay watch – experiences in Reventing Pharmacy and Therapeutic committee
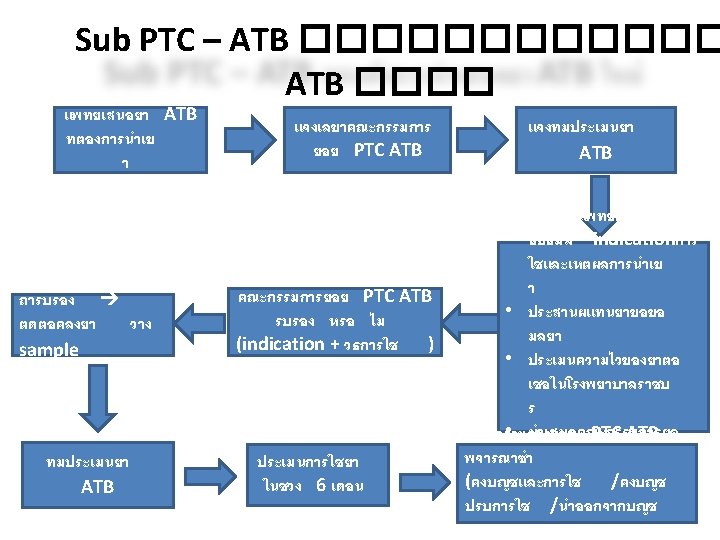
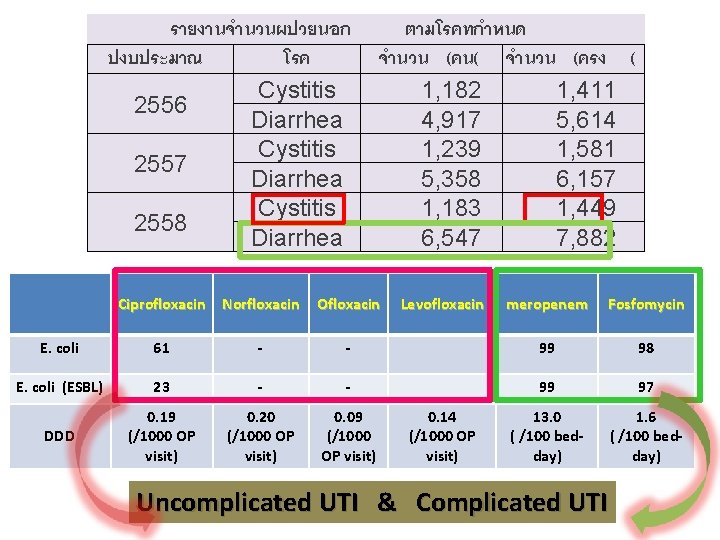
รายงานจำนวนผปวยนอก ปงบประมาณ โรค Cystitis 2556 Diarrhea Cystitis 2557 Diarrhea Cystitis 2558 Diarrhea ตามโรคทกำหนด จำนวน (คน( จำนวน (ครง ( 1, 182 1, 411 4, 917 5, 614 1, 239 1, 581 5, 358 6, 157 1, 183 1, 449 6, 547 7, 882 Ciprofloxacin Norfloxacin Ofloxacin E. coli 61 - E. coli (ESBL) 23 DDD 0. 19 (/1000 OP visit) Levofloxacin meropenem Fosfomycin - 99 98 - - 99 97 0. 20 (/1000 OP visit) 0. 09 (/1000 OP visit) 13. 0 ( /100 bedday) 1. 6 ( /100 bedday) 0. 14 (/1000 OP visit) Uncomplicated UTI & Complicated UTI
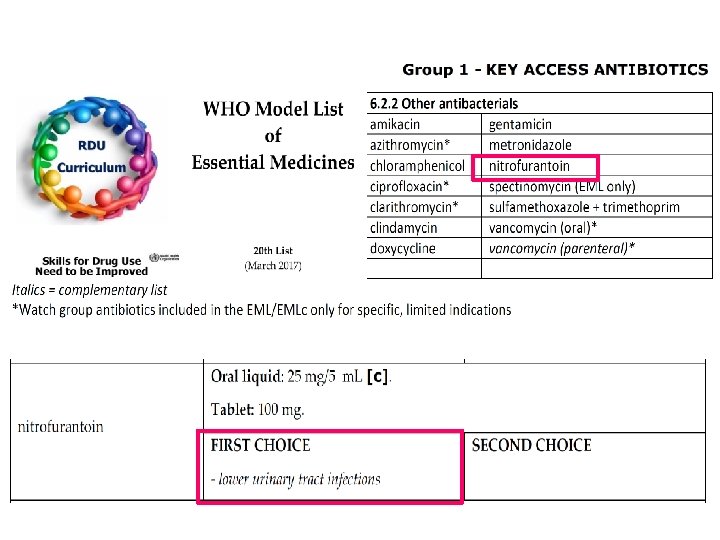

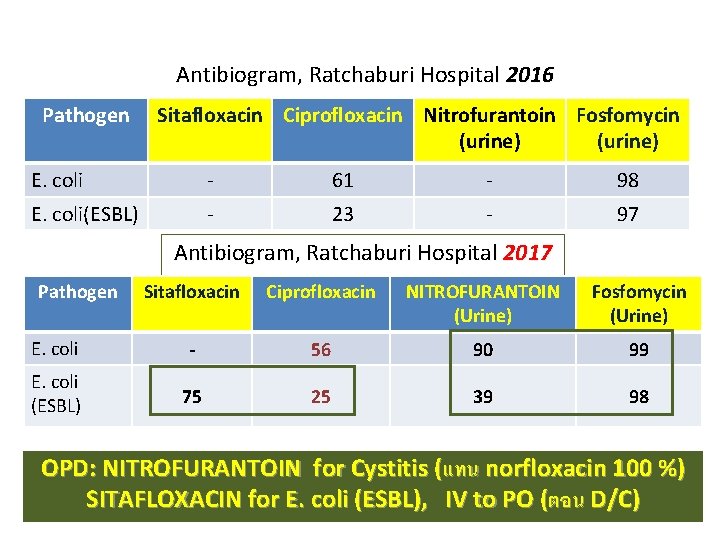
Antibiogram, Ratchaburi Hospital 2016 Pathogen Sitafloxacin Ciprofloxacin Nitrofurantoin Fosfomycin (urine) E. coli - 61 - 98 E. coli(ESBL) - 23 - 97 Antibiogram, Ratchaburi Hospital 2017 Pathogen Sitafloxacin Ciprofloxacin NITROFURANTOIN (Urine) Fosfomycin (Urine) E. coli - 56 90 99 E. coli (ESBL) 75 25 39 98 OPD: NITROFURANTOIN for Cystitis (แทน norfloxacin 100 %) SITAFLOXACIN for E. coli (ESBL), IV to PO (ตอน D/C)
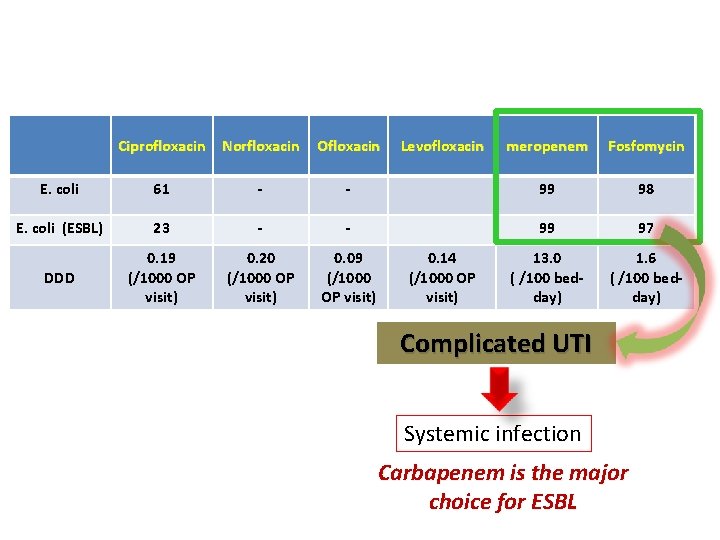
Ciprofloxacin Norfloxacin Ofloxacin E. coli 61 - E. coli (ESBL) 23 DDD 0. 19 (/1000 OP visit) Levofloxacin meropenem Fosfomycin - 99 98 - - 99 97 0. 20 (/1000 OP visit) 0. 09 (/1000 OP visit) 13. 0 ( /100 bedday) 1. 6 ( /100 bedday) 0. 14 (/1000 OP visit) Complicated UTI Systemic infection Carbapenem is the major choice for ESBL
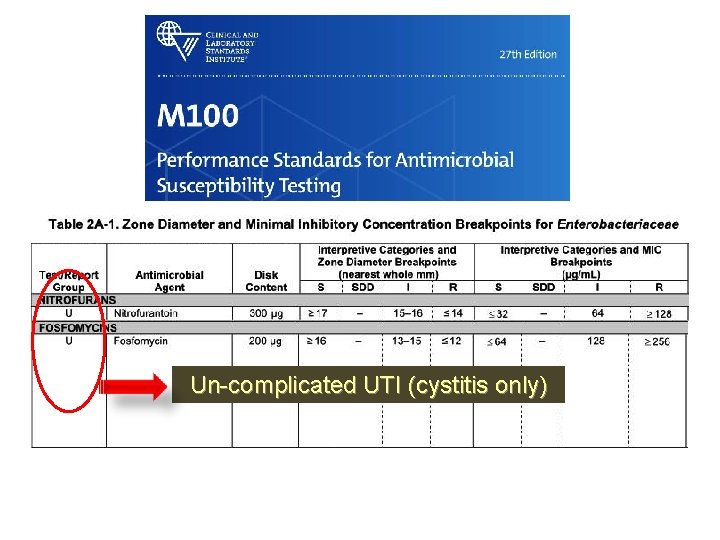
Un-complicated UTI (cystitis only)
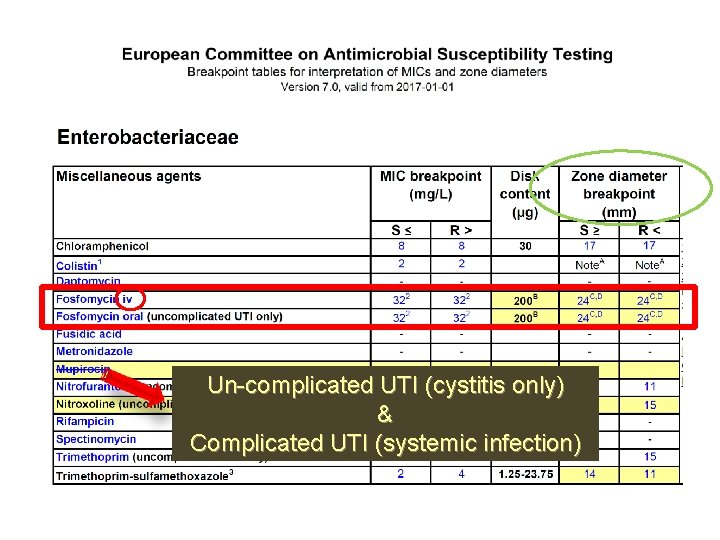
Un-complicated UTI (cystitis only) & Complicated UTI (systemic infection)
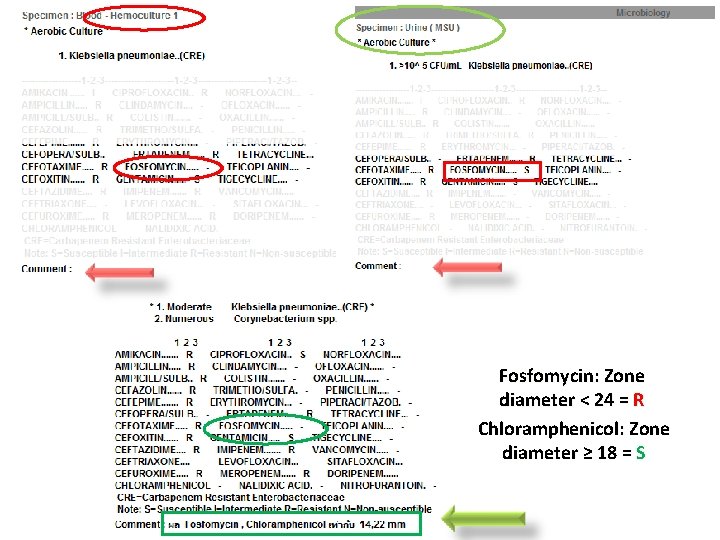
Fosfomycin: Zone diameter < 24 = R Chloramphenicol: Zone diameter ≥ 18 = S
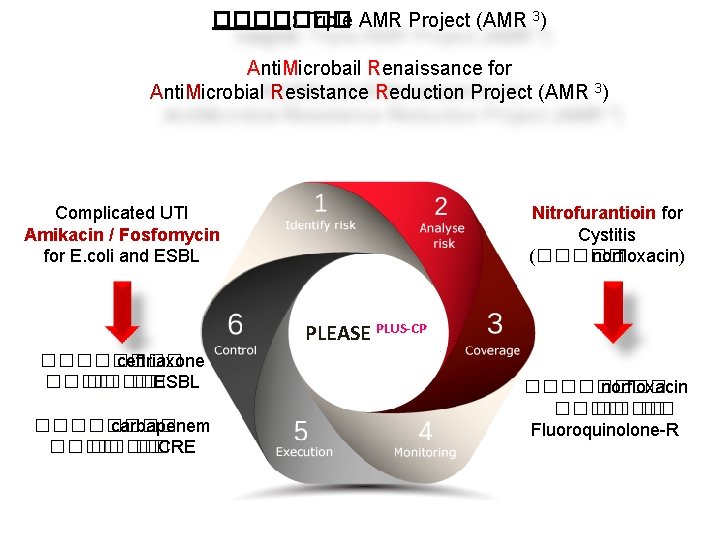
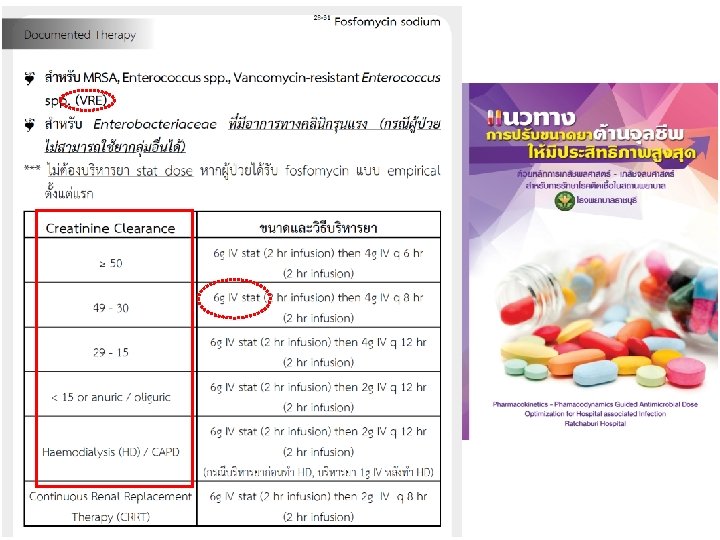
������� : Triple AMR Project (AMR 3) Anti. Microbail Renaissance for Anti. Microbial Resistance Reduction Project (AMR 3) Complicated UTI Amikacin / Fosfomycin for E. coli and ESBL Nitrofurantioin for Cystitis (����� norfloxacin) PLEASE PLUS-CP ���� ceftriaxone ���� �� ESBL ���� carbapenem ���� �� CRE ���� norfloxacin ���� �� Fluoroquinolone-R


The Measurement of Antimicrobial Use Evaluation (AUE)
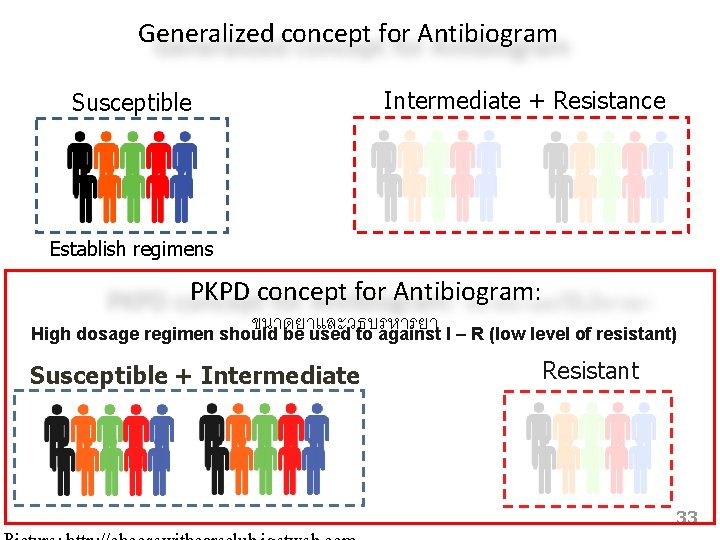
Generalized concept for Antibiogram Susceptible Intermediate + Resistance Establish regimens PKPD concept for Antibiogram: ขนาดยาและวธบรหารยา High dosage regimen should be used to against I – R (low level of resistant) Susceptible + Intermediate Resistant 33
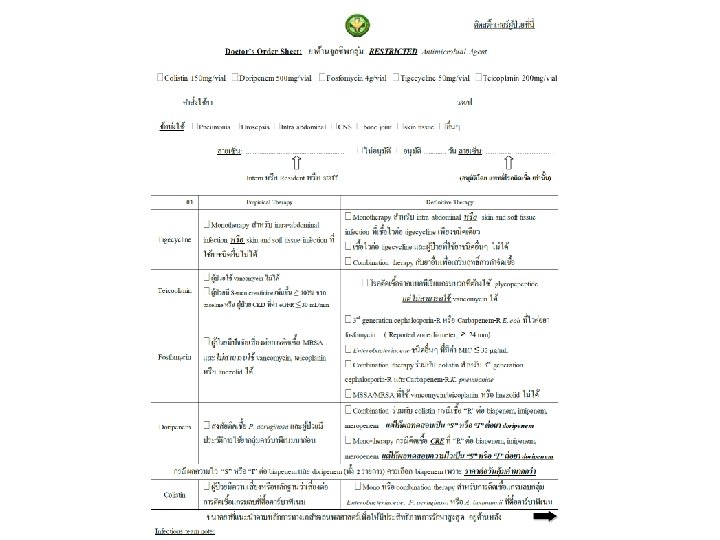



For daily Learning (Education)
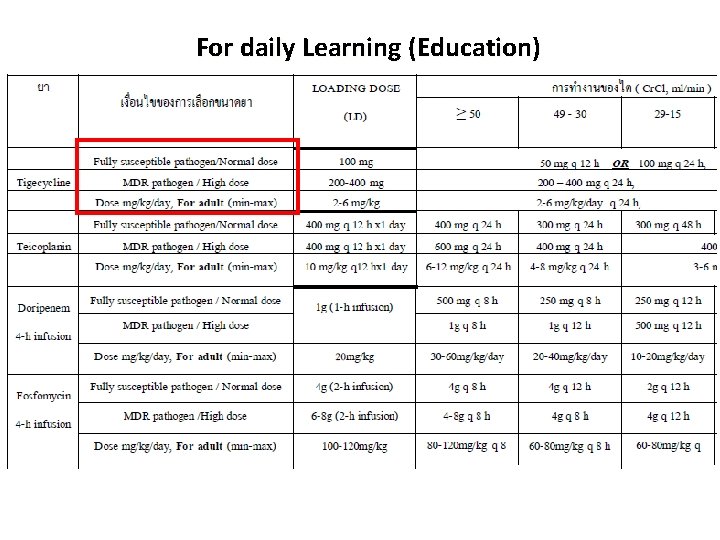
For daily Learning (Education)


Definition of In Appropriate empirical Antimicrobial Therapy (IAAT) included the element Definitive (Document) Therapy Antimicrobials with “S” to pathogen within 24 -48 hr Empirical Therapy Pathogen were not found: Clinical response Pathogen were found: S to pathogen BMC Infectious Diseases 2017; 17: 279. , Infect Dis Report 2017; 9: 6821. , Int J Antimicrob Agent 2017; 49: 617.



Drug-Resistant Tuberculosis Ratchaburi Hospital First regimen DST report Duration New regimen 7. 86 weeks (0 -20 weeks)

- Slides: 45