Community Outreach Stroke Rehab Program A Partnership Between

Community Outreach Stroke Rehab Program A Partnership Between William Osler Health System + Home & Community Care March 2018

System Challenges and the Need for Change Prior State & Known Challenges: § Lack of integrated stroke rehab services in Central West region § Lengthy waitlists for outpatient neuro rehab § Limited services available from homecare § Length of stay in hospitals impacting patient flow 2

OUR PILOT: Enhanced Access to Community Stroke Rehab Funded through Pay for Results (P 4 R) Funding from CW LHIN § Original Timeline: October 16 to March 31, 2018 § P 4 R Aims: • Lower hospital admission/readmission • Decrease ED or inpatient LOS • Improve access to primary, home & community care • Strategic alignment with LHIN and best practices • Partnerships – right care, right place 3
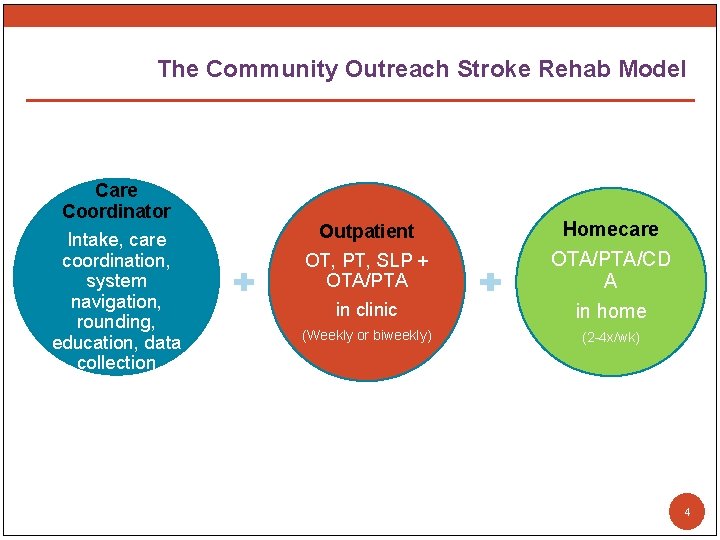
The Community Outreach Stroke Rehab Model Care Coordinator Intake, care coordination, system navigation, rounding, education, data collection OT, PT, SLP + OTA/PTA in clinic Homecare OTA/PTA/CD A in home (Weekly or biweekly) (2 -4 x/wk) Outpatient 4

Treatment Expectations § Estimated 2 -5 visits per week, per discipline (PT, OT, SLP) § Patient goals-driven (COPM) § 8 -12 week treatment cycle § Therapists can provide interventions both in-home and in-clinic § Homecare PTA, OTA, CDA’s provide ongoing interventions in the home 5

Evaluation of the Program As of early March 2018: § 64 patients enrolled into COSR • 27 completed program to date • 37 patients currently on active caseload § Average length of stay in the COSR was 9 weeks § Outcome measures • Length of stay data • Canadian Occupational Performance Measure (COPM) • Patient satisfaction survey 6
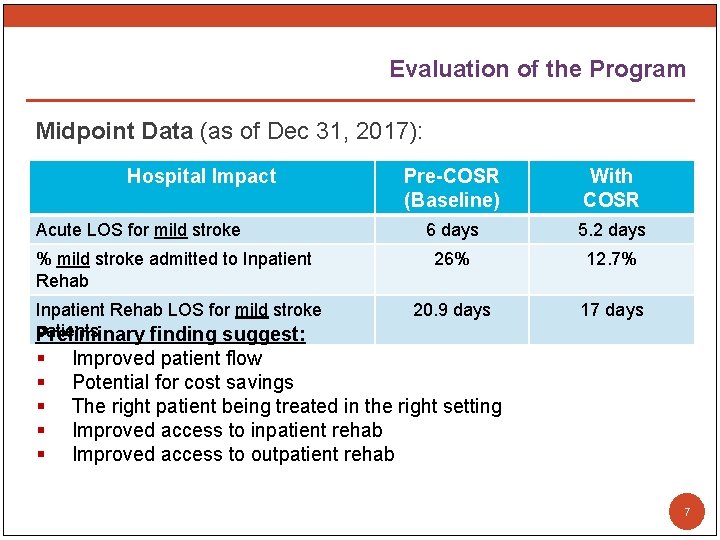
Evaluation of the Program Midpoint Data (as of Dec 31, 2017): Hospital Impact Pre-COSR (Baseline) With COSR 6 days 5. 2 days % mild stroke admitted to Inpatient Rehab 26% 12. 7% Inpatient Rehab LOS for mild stroke patients Preliminary finding suggest: 20. 9 days 17 days Acute LOS for mild stroke § § § Improved patient flow Potential for cost savings The right patient being treated in the right setting Improved access to inpatient rehab Improved access to outpatient rehab 7

Evaluation of the Program Patient Experience: § At discharge, satisfaction/feedback surveys were administered, along with the COPM outcome measure All of the participants agreed that: § § Time between hospital discharge and first visit was acceptable Pleased with the frequency of visits Pleased with the intensity of therapy Patients also described their journey with COSR to be collaborative, educational, individualized, and helped them to adapt to life after a stroke 8

Closing Thoughts § Outpatient and community therapy is cost-effective compared to inpatient length of stay § “Make the system fit the patient, don’t make the patient fit the system” § Innovation and collaboration between hospital and community § Investing in Outpatient/Community Rehab reduces stress on acute care while improving patient experience, satisfaction, and quality of life 9

Questions? 10
- Slides: 10