COMMUNITY MENTAL HEALTH REHABILITATION SERVICES CMHRS OHCC PROVIDER

COMMUNITY MENTAL HEALTH REHABILITATION SERVICES (CMHRS) OHCC PROVIDER ORIENTATION 2018

Who is Optima Health? • Virginia Based Health Plan – Offices in Virginia Beach, Richmond, and Roanoke with homebased employees located statewide. • Not-for-Profit organization in operation since 1984 • Provide coverage for approximately 450, 000 members, and growing! – Offering plans for commercial members, government programs (Medicaid & Medicare), Behavioral Health, and EAP • Subsidiary of Sentara Healthcare

Optima Health Products Commonwealth Coordinated Care Plus Plan (CCC+) Optima Health Community Care Virginia Medicaid Plans Optima Family Care/FAMIS Medicare Advantage Plans Optima Medicare HMO Optima Community Complete (DSNP) Individual & Family Plans Optima. Fit® Narrow Network Plans Optima. Select. SM Traditional Commercial Plans Vantage (HMO) Plus (PPO) Point of Service (POS) Integrated Account-based Product Lines Equity (HSA) Design (HRA) Self-funded Options for Large and Small Employer Group Tiered Plans Optima. Direct. SM

Introducing: Optima Health Community Care A Virginia Medicaid Managed Long Term Services and Supports (MLTSS) Product • • Optima Health is a statewide Medicaid MLTSS provider for individuals enrolled in the DMAS CCC Plus program. Individuals included in the program are Medicaid members with complex health issues, including those who are elderly or disabled, whether they may be in their home, an assisted living facility, or nursing facility.

Long Term Services and Supports (LTSS) • LTSS services that are efficiently utilized enable Members to retain autonomy and to function at their highest level. • • These services promote living in the least restrictive environment. • LTSS providers that offer quality, reliable and caring services are critical to the health and safety of our Members/Caregivers. LTSS services can be temporary or long-term and must be reassessed as needs change. To help ensure the effective delivery of LTSS services and community based care, Optima Health has partnered with CENTIPEDE (a division of HEOPS, Inc. ), a leader in networks and support services for MLTSS providers.

Community Mental Health Rehabilitation Services (CMHRS) As of Jan 1, 2018, Optima Health manages the following CMHRS services: • Mental Health Case Management • Therapeutic Day Treatment (TDT) for Children • Day Treatment/ Partial Hospitalization for Adults • Crisis Intervention and Stabilization • Intensive Community Treatment • Mental Health Skill-building Services (MHSS) • Intensive In-Home • Psychosocial Rehab • Behavioral Therapy • Mental Health Peer Supports (Individual and Group) To participate with Optima Health for CMHRS, providers must be contracted and processed through our Licensure, CAP, Audit and Review. This includes providers who are already participating with Optima Health for other services or products.

Community Mental Health Rehabilitation Services (CMHRS) For a detailed listing of the CMHRS codes and rates, please refer to the DMAS CCC+ Rate Setting website: OTHER FEE-FOR-SERVICE (FFS) Please also always refer to the Provider Manual, available on the Optima Health Provider Portal, under Education. To participate with Optima Health for CMHRS, providers must be contracted and processed through our Licensure, CAP, Audit and Review. This includes providers who are already participating with Optima Health for other services or products.

Optima Health Community Care Model of Care Optima Health Community Care facilitates personcentered care, featuring the following benefits: • Coordination and management of all aspects of physical health, behavioral health, long-term care and community-based services. • Access to a Care Coordinator who will work with the member, their caregivers, providers and community-based resources to ensure necessary care. • Support of an Interdisciplinary Care Team, including caregivers, doctors, nurses, counselors or others chosen by the member. • Regular care assessments and individualized care plans. The primary goal for Optima Health Community Care is to assure members receive the highest quality integrated services and supports they need in the most appropriate (least restrictive) setting. 8

Care Coordination and Providers: A Partnership

Care Coordination • • • Member, Provider, and Care Coordinator work together to provide the right service at the right time in the right amount based on each Member’s identified needs and preferences. Care coordinators schedule Interdisciplinary Care Team meetings and invite provider participation. Providers bring valuable insights into Member’s needs and services to meet these needs. Care Coordinators ensure services are authorized during continuity of care period and authorize future services. Care Coordinators work with Member, caregivers, and providers to identify social determinants and solutions to meet Member’s goals. Care Coordinators will request from providers: plans of care, DMAS forms, Supervisory forms, LOC, and other required DMAS/CMS forms as per contract.

Assessing Member Needs • Optima Health Community Care performs an extensive health assessment on every new Member on enrollment and throughout the year. • • This assessment looks at the Member from a biopsychosocial perspective. • Care Coordinators conduct Face to Face assessments and in-person care planning and care team meetings for members receiving LTSS services. • Regional transition coordinators are engaged for continuity of care, transitions from NF to community, and as a resource. • OHCC is a required reporter for suspected child and adult abuse and neglect. Please report all incidences to APC/CPS and communicate with the OHCC Care Coordinator. More information on identifying child and adult abuse can be found in the Clinical Reference section of optimahealth. com/providers CCC Plus is different in that social determinants are also identified and addressed.

Critical Incident Reporting All incidents must be reported within 24 hours, using the CCC+ Critical Incident Report Form found on the DMAS website. Critical incidents include: • Medication Errors • Severe injury (temporary harm or permanent) • Suspected Mental Abuse (APS/CPS Mandatory report) • Theft • Financial Exploitation (APS/CPS Mandatory report) • Death/Incarceration of a Member • Suspected physical abuse (APS/CPS Mandatory report) • Neglect (APS/CPS Mandatory report) • Exploitation (APS/CPS Mandatory report) • Other (documented deviation from the standards of care which results in a harmful/adverse event)

Promoting Health and Wellness • Optima Health Community Care works with Members and providers to promote health and wellness through: • • • Smoking Cessation Patient Education Weight Management Chronic Disease Management Added Benefits for CCC Plus members: dental, vision, hearing, diabetic foot care, memory care, assistive devices, home security, pest control, home delivered meals, respite for caregivers, and more* • Identifying community solutions for socialization, support, and healthy living * Limitations may apply

Contacting Care Coordinators Optima Health Community Care Coordination: 1 -866 -546 -7924 This is a call line monitored by Care Coordinator Techs who will either assist caller, forward to a Care Coordinator, or escalate call as required. Care Coordinators are available Monday through Friday, 8: 00 a. m. – 5: 00 p. m. and on-call after hours.

Doing Business with Optima Health

Provider Portal: Optimahealth. com Optima. Health. com offers providers instant access to resources and tools to optimize doing business with Optima Health…. Access what you need, when you need it. ü Drug formularies and pharmacy authorization forms ü Medical authorization forms ü Easy enrollment for Electronic Funds Transfer (EFT) ü Provider Manuals ü Provider newsletter and important updates ü Clinical guidelines and reference tools ü Provider Education tools ü Secure business transactions through Provider Connection

Provider Connection is the Optima Health self service, online provider tool for secure transactions through optimahealth. com. Available 24 hours a day, 7 days a week - so you can do business when it’s convenient for you. With secure sign in to Provider Connection, you can: ü Verify member eligibility and benefits ü Check claims status ü Submit reconsiderations ü View/download payment remittance advices ü View PCP membership reports ü Access C 3 – Clear Claims Connection ü Coming Soon… Submit and review authorization requests Provider Connection registration is available to all practitioners, administrators, and office staff of contracted network providers.

Provider Connection Registration To register for Provider Connection: • Visit optimahealth. com/providers • Click on “Sign In/Register” • Complete the Provider Connection registration form. You will receive an email within 10 days with your confidential user name and password. Ø User names and passwords are confidential and should not be shared. All users must register and access Provider Connection with their own login information.

Duo Security – Two Step Login Optima Health has adopted a Two-Step Login process through Duo Security to strengthen information security efforts. • • Duo Two-Step Login provides an extra layer of security by requiring a second authentication method of verifying the user’s identity after signing in to Provider Connection. The second method is something the user has physical access to - like a cell phone, tablet, or landline. This prevents anyone but the user from logging in, even if they know the user's username and password. All Provider Connection users will be prompted to enroll with Duo Security upon first login to Provider Connection. If you experience technical difficulties with Duo enrollment or login, please contact Provider Relations for support.

Member Eligibility and Benefits

Verifying Member Eligibility/Benefits Optima Health strongly recommends verifying each member’s eligibility and benefits prior to rendering services. This is an important step in ensuring reimbursement. Verification may be obtained by: : Virginia Medicaid Provider Portal : Provider Connection on optimahealth. com or – Provider Relations 1 -844 -512 -3172 – Care Coordinators 1 -866 -546 -7924 CMHRS is currently a covered benefit for OHCC members only. Beginning August 2018, this benefit will extend to Optima Family Care Medallion 4. 0 members on a roll in basis by region.

Optima Health Community Care Plan ID Card 22

Optima Health Plan ID Cards 23
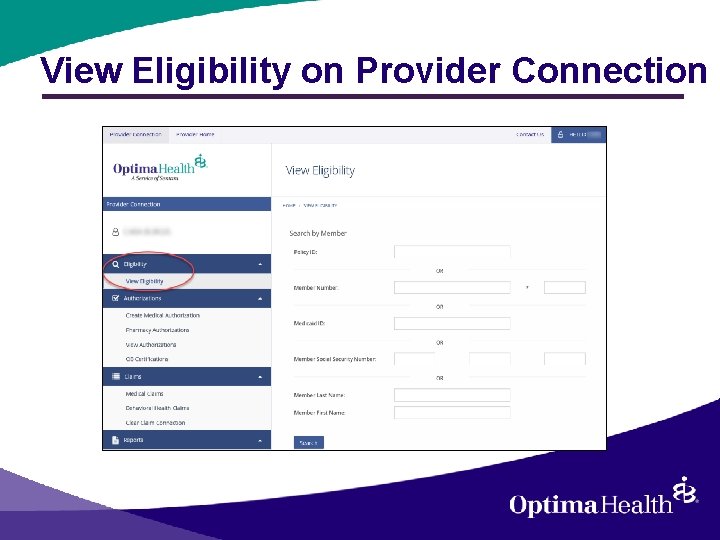
View Eligibility on Provider Connection
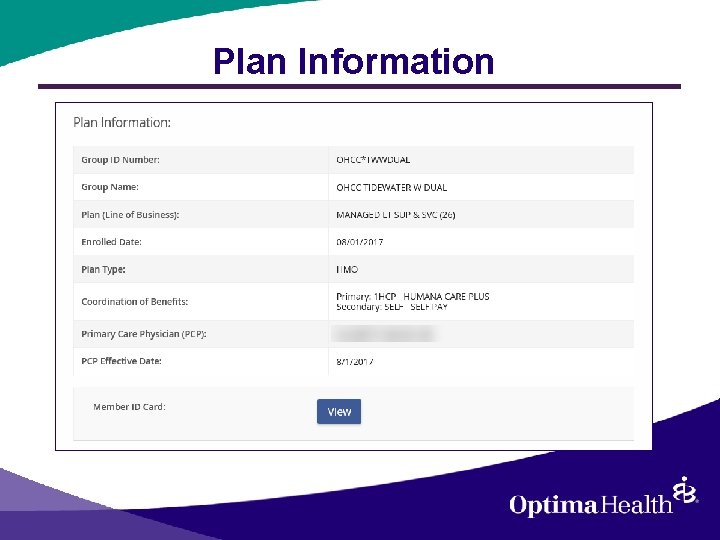
Plan Information

Authorizations

CMHRS Pre-Authorization ALL CMHRS services require Authorization or Registration. • OHCC uses the DMAS standardized CMHRS Service Authorization/Registration forms for CCC Plus. The forms are available in the OHCC Authorization Forms section of www. optimahealth. com/provider and on the DMAS website at CMHRS Transition • Authorization requests should be submitted through the Authorization Portal or faxed to the Optima Health number specified on the authorization/registration form. : Authorization status can be viewed on Provider Connection Members must meet specific medical necessity criteria as defined by DMAS. Requests are reviewed on an individual basis to determine length of treatment and service limits.
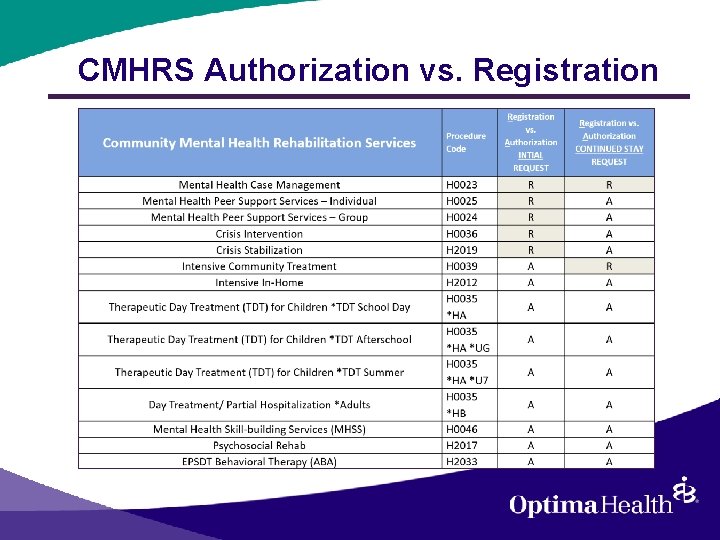
CMHRS Authorization vs. Registration

Continuity of Care • Members may maintain their current CMHRS provider for up to 90 days. • Optima Health will honor service authorizations issued by DMAS or the DMAS contractor (Magellan of Virginia) prior to enrollment for the length of the authorization or up to 90 days, which ever comes first. • On or after April 1, 2018, the Continuity of Care period is reduced to 30 days. • Authorizations will be extended as necessary pending the provider’s contract with Optima Health or to ensure a safe and effective transition to an in-network Optima Health provider.

Billing and Reimbursement

Claims and Billing : Preferred method of claims filing is electronic • We accept claims through any clearinghouse that can connect through Payerpath/Allscripts using Optima Health Payor ID# 54154 or 5415 M • We are also now accepting electronic claims through Availity* using Optima Health Payor ID# 5415 M • Any paper claims should be mailed to: Behavioral Health Claims PO Box 1440 Troy, MI 48099 -1440 * Submission through Availity is only available to CMHRS and Nursing Facility/Skilled Nursing facility Providers » Timely filing deadline on all claims is 365 days from the date of service. This includes any corrections, reconsiderations, and/or appeals » Turnaround time for clean (correctly submitted) claims: • 14 days

CMS 1500 Claim Form NPI and Taxonomy: • The Organizational NPI (Type 2) should always be listed in box 33 A. No number is required in box 33 B. • The rendering provider’s NPI number should be listed in the bottom (unshaded) portion of box 24 J • – For services billed under the umbrella of the CMHRS organization or CSB this should be the organizational NPI (Type 2). – For services provided by a licensed ABA Therapist, already credentialed, you will use the individual NPI (Type 1) in Box 24 J. For all claims, the upper, shaded portion of 24 J should contain Taxonomy 261 QM 0801 X for these service. Claims submitted without this taxonomy numbers may take longer to process.
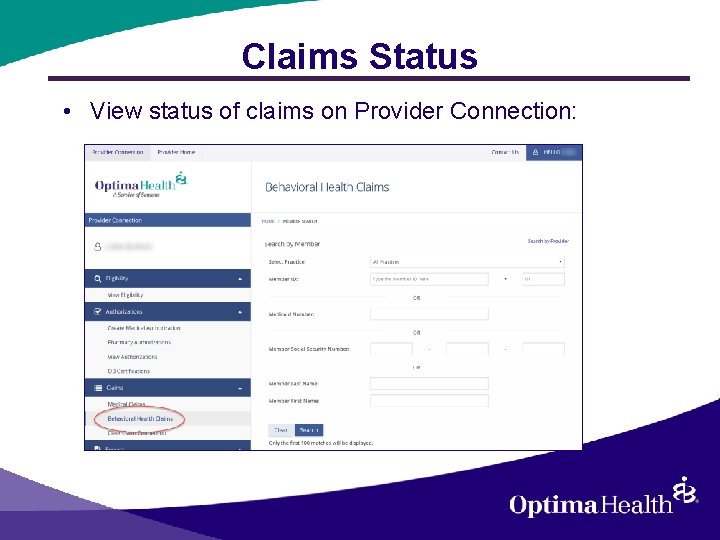
Claims Status • View status of claims on Provider Connection:

Provider Remits • Obtaining Remits for Participating Providers: – Providers can obtain the remits through their existing clearinghouse relationship OR – Providers can obtain remits through the secure Provider Connection • Obtaining Remits for Non Participating Providers – Providers can obtain the remits through their existing clearinghouse relationship – You may also be able to obtain a printed copy of your remits through our Provider Relations at 1 -844 -512 -3172

Reconsiderations/Corrected Claims A request for reconsideration is submission of a corrected claim for the same patient, date of service(s) and/or procedure(s) that had previously been denied. • Reconsiderations for claims filed on a CMS 1500 must state “Reconsideration” or “Corrected claim” in box 19. • Reconsiderations can be requested online through Provider Connection (for claims that require correction to CPT, Diagnosis, Place of Service, Quantity, and Charges) – Be sure to reconsider the ENTIRE claim • Paper requests for reconsideration of a claim denial must include the claim or copy of the remit, any supporting documentation, and the “Provider Reconsideration Form, ” found on www. optimahealth. com

Appeals and Refunds Appeals Process • If your claim denial is upheld after the reconsideration process, you have the option to file an appeal. • Appeals may be submitted in writing within 365 days from the date of service. Detailed information and supporting written documentation should accompany the appeal. Appeals should be sent to: Optima Health Appeals Dept. P. O. Box 62876 Virginia Beach, VA 23466 -2876 • A decision will be rendered within 45 business days of receipt of the appeal request. Refund Process • When sending a refund, please send a copy of the remit, reason claim was paid in error, and check to: Optima Health Recovery Unit PO Box 61732 Virginia Beach, VA 23466

Electronic Funds Transfer (EFT) Benefits of EFT: ü Safer, more secure, and efficient method of claims payment ü Funds are deposited within 24 hours after payments are processed ü Clean claims are paid within an average of 7 days when submitted electronically and payment made through EFT ü You will be notified via email when deposit is made to your bank account • This notice is sent to the email address supplied on the EFT enrollment form. Enroll Today!

EFT Enrollment It is easy to begin taking advantage of the benefits of Electronic Funds Transfer / Electronic Remittance Advice (EFT/ERA). • Sign up for EFT/ERA with the Electronic Payment/Remittance Authorization Agreement in the “Billing & Claims” section of optimahealth. com/providers • If you have any questions, please email the team at: EFT_ERA_Inquiry@sentara. com

Provider Changes and Updates

Notification of Provider Updates 60 days notice is required for all provider changes, including: ü ü ü Panel status / accepting new patients Contact information (address, phone, email, etc. – for all locations) Provider relocation or joining/leaving practice Tax ID change (need a new/current W-9) Name change Please submit changes to Optima Health as soon as possible by completing the Behavioral Health Provider Update Form on optimahealth. com/providers or contacting your Network Educator.

Requesting Network Participation

Provider Participation All providers requesting participation with Optima Health to offer CMHRS services to OHCC members must be complete the Licensure, CAP, Audit (LCAR) review and be contracted by Optima Health for CMHRS, even if already contracted for other services or products. Upon each license renewal, service location renewal, or address change/addition, an additional LCAR is required. • CMHRS Providers are contracted as an organization (agency) type provider and all services are billed under the organization’s NPI. Except for ABA practitioners, individuals within the CMHRS organization are not required to be credentialed by Optima Health.

CMHRS Provider Application Process ü Access Optima Health Provider Application Packets on the Contact Us page of optimahealth. com/providers. ü Complete and submit the CMHRS Application Packet. • If Behavioral Therapy services are offered, each licensed ABA practitioner must also complete the Behavioral Health New Provider Application Packet (and CAQH application). ü Review your application packet in full before submission. Optima Health is unable to accept incomplete applications. Optima Health will: ü Review and verify required information and attachments ü Contact you for any contracting needs and/or revisions ü Notify you of your effective date once LCAR is approved The LCAR may take between 90 -120 days upon receipt of a complete and accurate application.

CAQH – ABA Practitioners only • • • Licensed ABA practitioners must be individually credentialed by the Optima Behavioral Health Credentialing Committee. A Behavioral Health New Provider Application Packet must be submitted to initiate the credentialing process. Optima Health utilizes the Council for Affordable Quality Healthcare (CAQH) Proview application for all individual practitioner credentialing. * – CAQH applications must be complete and accurate (with all supporting documentation attached) – Incomplete applications cannot be accepted for consideration Access the CAQH Pro. View application on www. caqh. org The CAQH Proview application is used for re-credentialing (no less than every 36 months). Providers are responsible for keeping CAQH and attachments up to date. *CAQH is not required for Ancillary, Facility, or other Organizational/Agency type providers that bill for services under the facility/organization’s NPI.

Provider Education and Resources

Education on optimahealth. com Visit optimahealth. com/providers for ongoing education, training, and CME opportunities.

provider. NEWS The quarterly Provider Newsletter is distributed by email. The current (and archived) editions are available on the Updates section of optimahealth. com/providers. Sign up to receive the newsletter at providernews@optimahealth. com

Other Important Resources • Provider Reference Manual and Supplements: optimahealth. com/providers • DMAS CMHRS Transition: http: //www. dmas. virginia. gov/Content_pgs/mltss-trn. aspx • Important Websites: optimahealth. com dmas. virginia. gov https: //www. cms. gov/

Contact Us

Optima Health Community Care **New Contact Numbers** Please use these numbers for all Optima Health Community Care inquiries. Provider Relations 1 -844 -512 -3172 Clinical Care Services Pre-Auth Medical/Pharmacy: 1 -888 -946 -1167 Behavioral Health: 1 -888 -946 -1168 Care Coordination 1 -866 -546 -7924 After Hours Program 1 -844 -387 -9420

We look forward to working with you!
- Slides: 51