Communication Models in Palliative CareEnd of Life Care



















- Slides: 32

Communication Models in Palliative Care/End of Life Care Ping fen Tang Professor of Nursing Kunming Medical University, China

Role of Communication Skills • Effective symptom control is impossible without effective communication. • Communication as a major component of the delivery of all medical, and particularly palliative care. Kaplan SH, Greenfield S, Ware JE: Impact of the doctor-patient relationship on the outcomes of chronic disease. In Stewart M, Roter D (eds): Communicating with Medical patients. Newbury Park, Sage Publication, 2001

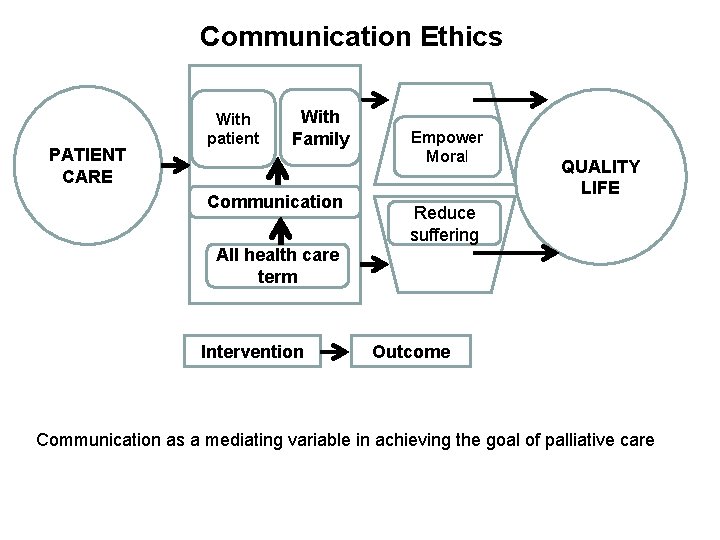
Communication Ethics PATIENT CARE With patient With Family Communication Empower Moral QUALITY LIFE Reduce suffering All health care term Intervention Outcome Communication as a mediating variable in achieving the goal of palliative care

Overview of the COMFORT Model Wittenberg-Lyles and colleagues developed an evidence-based communication model that elaborates seven principles of communication. Wittenberg-Lyles E, Goldsmith J, Ferrell B, Ragan S. Communication in Palliative Nursing. New York, NY: Oxford Un iversity Press; 2013.

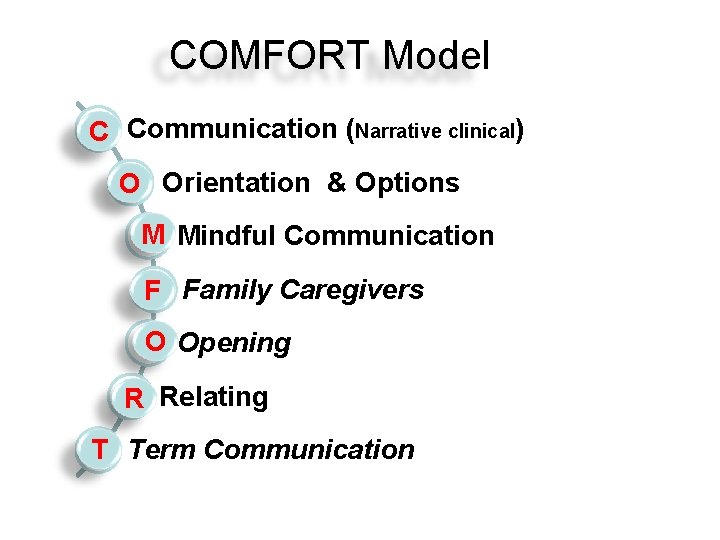
COMFORT Model C Communication (Narrative clinical) O Orientation & Options M Mindful Communication F Family Caregivers O Opening R Relating T Term Communication

Communication (3 Rs) Reflection on the patient before illness Remember the patient as an individual Re-author the story

Orientation and Options Question to determine family orientation Use plain language planner for palliative care Question to understand patient/family culture

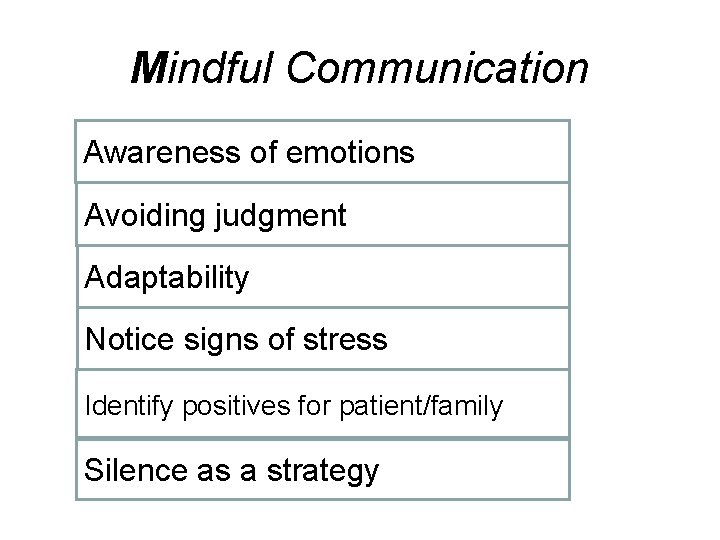
Mindful Communication Awareness of emotions Avoiding judgment Adaptability Notice signs of stress Identify positives for patient/family Silence as a strategy

Family Caregivers Caregiver communication tool Patient & Family communication need Concern/response: Pain Prompt/response: Assessment

Openings Address the topic Comment on topic Incorporating quality of life Spiritual review

Relating Checklist AMEN Question

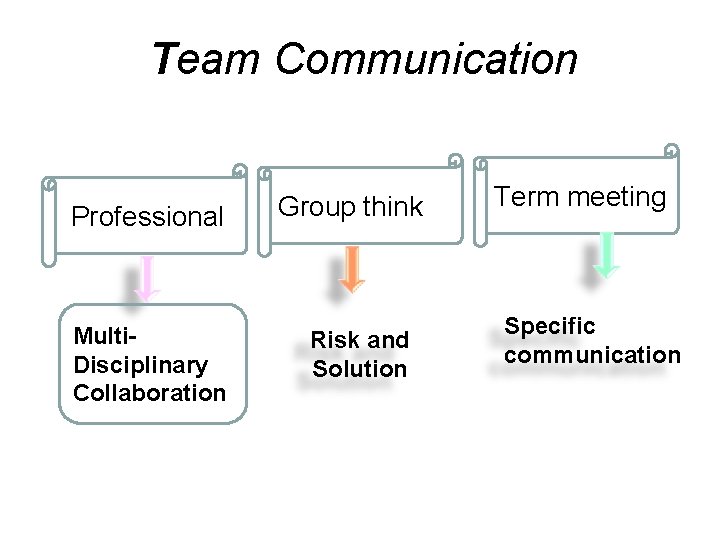
Team Communication Professional Multi. Disciplinary Collaboration Group think Risk and Solution Term meeting Specific communication

Giving bad news to patients/families need different communication skills because the cultural differently.

In many countries, including most Asian countries and some southern Europe, decisions about what is told to a patient and the care received is made by the family. Johnson M. R. D. (2009). End of life care in ethnic minorities. Providers need to overcome their fear of dealing with people from different backgrounds. British Medical Journal 338, a 2989


Breaking Bad News • Bad news can best be defined as any news that adversely affects the patient's view of his or her future. Buckman R: Breaking bad news: Why is it still so difficult? BMJ 288: 1597 -1599, 1984

Breaking Bad News Mode SPIKES • WALTER F. BAILE, 2000 ABCDE • Rabow MW, Mcphee, 1999

• • Arrange S: Setting for some privacy • • Involve significant others& Sit down • • Make connection and establish rapport with the patient • • Manage time constraints and interruptions P: Perception of condition/ seriousness • Determine what the patient knows about the medical or what is suspected. “Before you tell, ask. ”, Listen to the patient’s level of comprehension • • Accept denial but do not confront at this stage I: Invitation from patient to give information • Ask patient if wishes to know the medical and/or treatment • Accept patient’s right not to know • Offer to answer questions later if s/he wishes K: Knowledge give medical factor E: Explore emotions & sympathize Strategy & summary • Consider educational level, socio-cultural background, current emotional • • Give information in small chunks, warn the patient bout to give bad news • • Check whether the patient understood what you said & Respond reactions • • Give any positive aspects first • Prepare to give an empathetic response: • • 1. Identify emotion expressed by the patient (sadness, silence, shock etc. ) • • 2. Identify cause/source of emotion • • 3. Give the patient time express his or her feelings • • Patients who have a clear plan for the future are less likely to feel anxious and uncertain-so clarify their understanding • • Close the interview

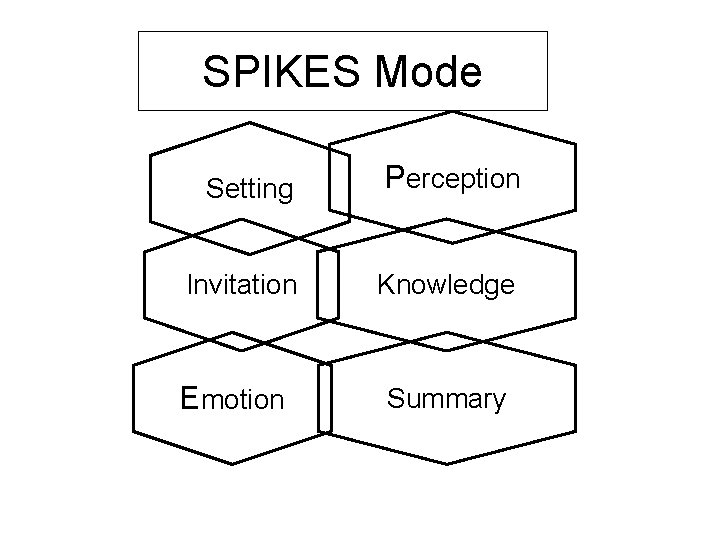
SPIKES Mode Setting Perception Invitation Knowledge Emotion Summary

• The SPIKES protocol has been designed specifically for these purposes and will allow the physician to assess the patient's expectations before going on to share the information. Curtin S, MCCONNELL M. Teaching dental student how to deliver bad news: SPIKES model [J]. J Dent Educ, 2012, 76(3): 360 -365

Case

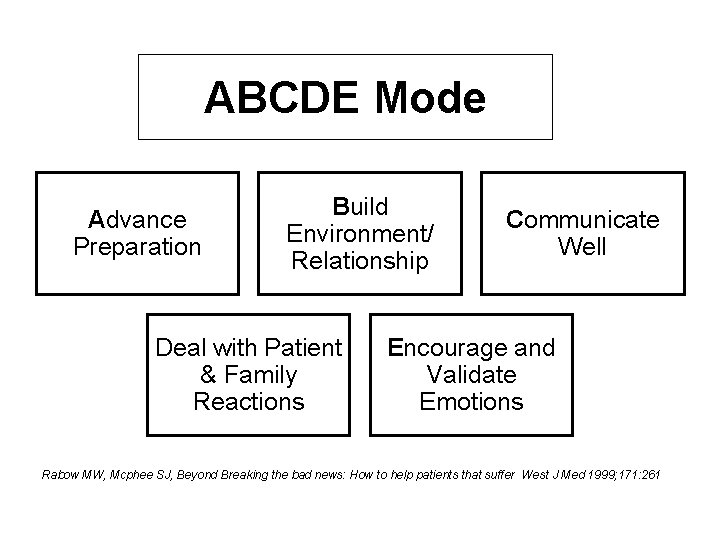
ABCDE Mode Advance Preparation Build Environment/ Relationship Deal with Patient & Family Reactions Communicate Well Encourage and Validate Emotions Rabow MW, Mcphee SJ, Beyond Breaking the bad news: How to help patients that suffer West J Med 1999; 171: 261

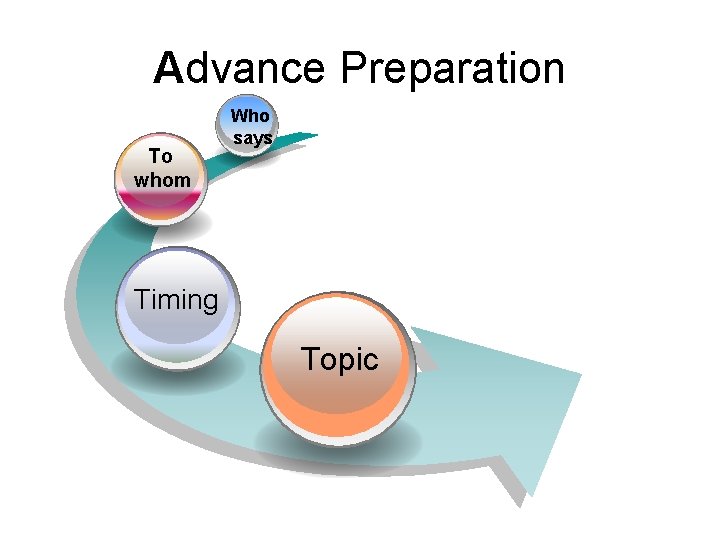
Advance Preparation To whom Who says Timing Topic

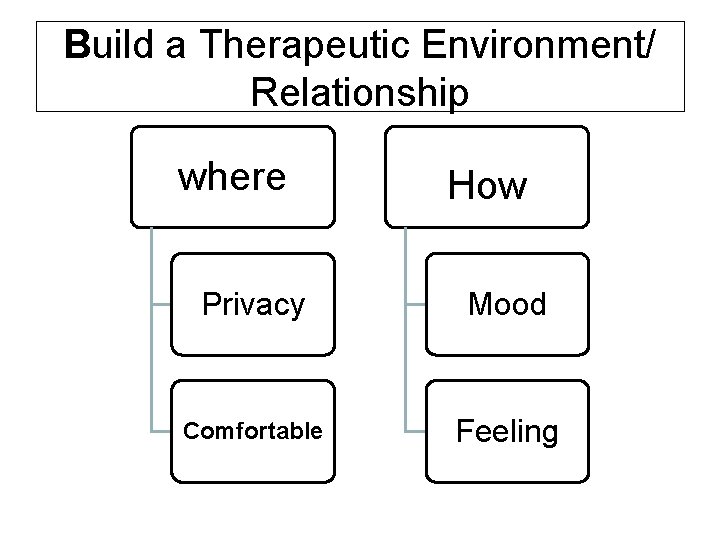
Build a Therapeutic Environment/ Relationship where How Privacy Mood Comfortable Feeling

Communicate Well Perspective others Individuals different Step by step

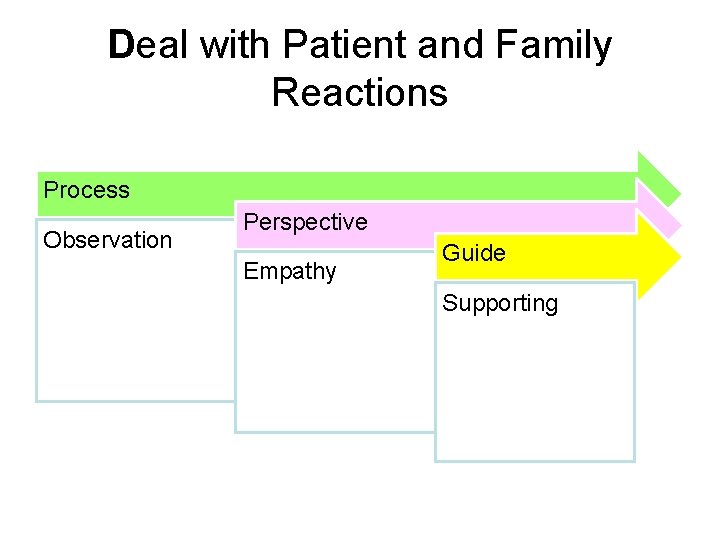
Deal with Patient and Family Reactions Process Observation Perspective Empathy Guide Supporting

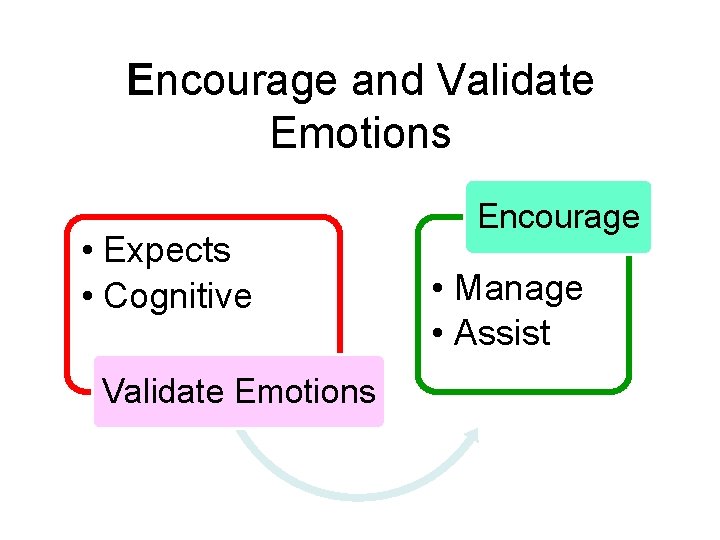
Encourage and Validate Emotions • Expects • Cognitive Validate Emotions Encourage • Manage • Assist


The so-called "death café" movement started 2011 in London by Jon Underwood, who was inspired by the writings of Swiss sociologist Bernard Crettaz.

Death Coffee of Kunming British Death Coffee Guide Traditional Chinese Cultural Multidisciplinary Teams Monthly Coffee Activities

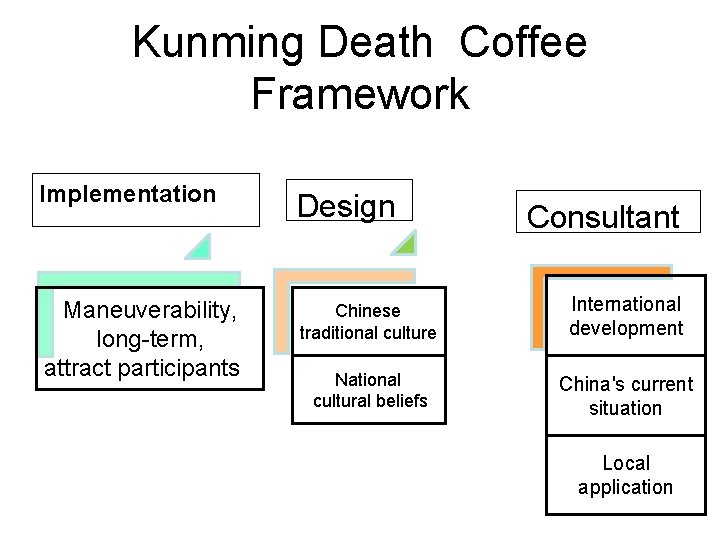
Kunming Death Coffee Framework Implementation Design Maneuverability, long-term, attract participants Chinese traditional culture International development National cultural beliefs China's current situation Consultant Local application

Thank you!