Communication following an Acquired Brain Injury Sarah Chatterton

Communication following an Acquired Brain Injury Sarah Chatterton, Independent Speech & Language Therapist Helen Cullimore, Speech & Language Therapist, Bristol Royal Hospital for Children helen. cullimore 2@UHBristol. nhs. uk

Service Development for Paediatric ABI. �‘it has been shown that paediatric Brain Injury often does not resolve completely and difficulties can persist or emerge which may have an impact upon education and social integration later in life’ (RCSLT Resource Manual for Commissioning and Planning Services for SLCN, 2010). �So. . a care pathway is needed to recognise this – challenging amongst community caseloads. �Consequences: eg. of young people in custody, 65 -70% will have experienced a traumatic brain injury (Justice Secretary Mr Grayling)

Cases referred at BCH. . �Severe – Moderate TBI, mostly RTA, falls. (Severe GCS 3 -8, >6 hrs LOC, Moderate GCS 9 -12, 20 mins to 6 hrs LOC, Mild GCS 13 -15, 0 -20 mins LOC) �Tumour – Mostly posterior fossa �CVA – due to AVM / FMD �Meningitis / septicaemia /encephalitis (ADEM, NMDA Receptor) / cerebral abscess �Epilepsy surgery �Inhalation burns �Spinal surgery / foramen magnum decompression. �Hypoxic Ischemic brain injury �Cases admitted for diagnostic work up – some eventually diagnosed as ‘non-organic’ cause for symptoms. GCS = Glasgow Coma Score, LOC = Loss of consciousness.

Pathways of management. . � Swallow / communication assessment, regular review & advice. Resume premorbid function. Discharged with advice & contact no. � Discharged from hospital with ongoing SLT needs. Local inpatient / community facilities sought – rarely adequate if existing. � Remain at BCH for ‘neurorehabilitation’ while medical, home & social, therapy & education set up for discharge. � Children discussed at weekly MDM & Discharge Planning Meetings held for long-term / complex cases.
What happens if a developing brain is injured?
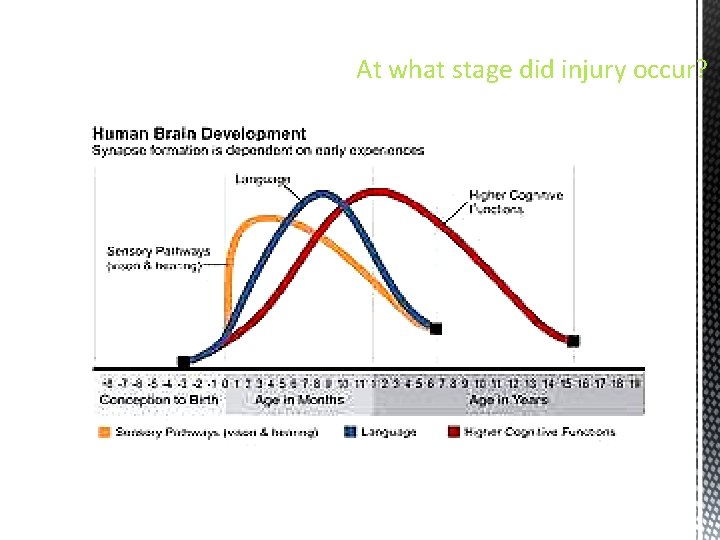
At what stage did injury occur?

Assessment. . � Case History – Including development, pre-existing strengths / weaknesses / disorders. Educational level / involvement of other services. � Pre-operative assessment in tumour cases where possible. � Post ABI progress / observations. � PTA status & ? Communication impairment affecting results. � MDM information.

Communication Assessment… �Informal & selected subtests appropriate tool. All developmental but ABI tools exist (Tadworth Court have some). Age ‘norms’ rarely useful (multiple factors affect performance, peaks & troughs of function, often bares little relation to functional performance, can be unnecessarily disheartening to child & family if ‘bad’ and set unrealistic expectations and inadequate support if ‘good’. �Assessments include. . CELF-4, Preschool CELF, Mount Wilga, PALPA, Preschool Language Scales-3, Test of Word Finding, BPVS, Phonological Screening Assessment, FDA, WHIM, SMART, Functional Assessment of verbal reasoning & executive strategies. �Communication aids service /my small store via charity funds! (Communication Aids have joined to one service, in Bristol, Paeds still at Claremont School, Adults moved to Cribbs Causeway with wheelchair services from Frenchay Hospital).

Type and extent of changes � Site and severity of injury. � Previous abilities and personality. � Stage of development at time of injury. � Impact of injury on emotional, physical, sensory and cognitive functions. � Support network for the individual and their family to aid rehabilitation and reintegration.

Range of Communication Changes & Case Studies. . �Speech production-acquired dyspraxia, dysarthria, dysphonia. May be so severe that little / no speech is possible (or if tracheostomy& unable to use speaking valve). Communication aids / non-verbal strategies may be needed. (cases DE, RW, CT, SS) �Receptive and expressive language (Spoken & written)-aphasia, slowed processing, higher level & social language disorder, close link with cognitive & behavioural impairments. (case JS) �Cerebellar Mutism / Posterior Fossa Syndrome, Post Traumatic Mutism. (TS) �Cognitive Communication Disorders-beyond language, such as effects of mood change, impulsivity, altered self esteem, emotional lability, stress. (cases CW, BT, SR)

More on Cognitive Communication Disorders § “Those communicative disorders that result from deficits in linguistic and nonlinguistic cognitive processes” - The American Speech and Language-Hearing Association, 1988.

Continued. . � Common, persistent difficulty following TBI due to structures prone to injury (ie. Frontal lobes) � Even subtle problems can have a massive effect on functioning. � Not necessarily accompanied by ‘aphasic’ type features, therefore, people may do misleadingly well do well on standard language assessments.

Cognitive processes may include. . � Impaired attention, perception, memory. � Inflexibility, impulsivity, disorganised thinking. � Slowed processing of complex information. � Problems learning new information. � Inefficient retrieval of stored information. � Ineffective problem solving or judgement. � Inappropriate social behaviour. � Impaired executive functioning.

How does this manifest? § Inability to filter out distractions / attend to a task. § Difficulty understanding and remembering spoken information. § Difficulty understanding jokes, puns sarcasm, hints, metaphors. § Rambling, imprecise language with poor sequencing and topic maintenance. § Repetitive or inappropriate conversation, and poor turn taking.
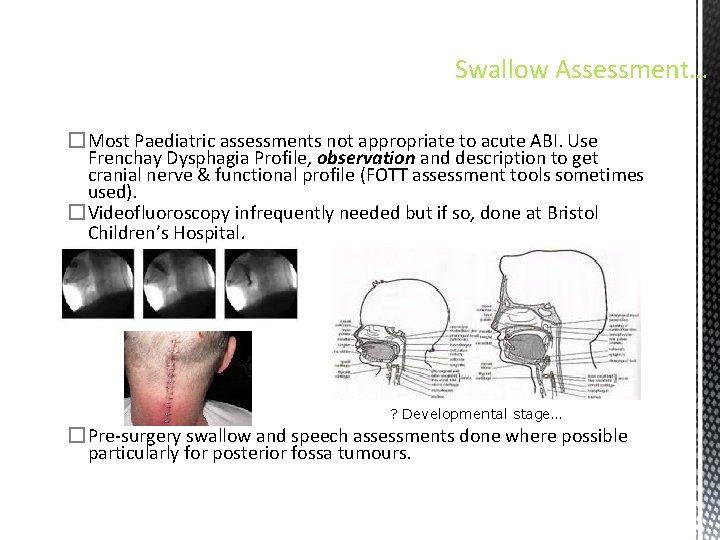
Swallow Assessment… �Most Paediatric assessments not appropriate to acute ABI. Use Frenchay Dysphagia Profile, observation and description to get cranial nerve & functional profile (FOTT assessment tools sometimes used). �Videofluoroscopy infrequently needed but if so, done at Bristol Children’s Hospital. ? Developmental stage… �Pre-surgery swallow and speech assessments done where possible particularly for posterior fossa tumours.

Inpatient Rehabilitation. . § Often via and with family, play team, school room staff, links with OT / PT. § Communication – Computer based (REACT /Step by Step aphasia therapy, speech viewer, ‘speech sounds on cue’ dyspraxia prog easy games, ziko world, spot on games), strategies, card / board /object games / tasks. § I Pads increasingly used – multiple uses. § Swallowing – FOTT, chewy pouches & tubes, messy food play, texture, taste, temp, feeding style / tools.

What happens in Rehabilitation? gadgets photos drink Joint sessions FUN ! noise games Mirror Assessment Tools food

Take Aways… § Self Advocacy DVD “Personally I think that dvd was huge in his transition back to school and helped show the professionals that took over to understand Seb and what he finds difficult. We have found it useful to watch and measure progress against, as it's incredible and sometimes when you see small bits each day you forget how much they equate too. We also used the dvd to explain to a new autistic child in his year Sebs story. He was quite mean at points saying "he didn't care he had been in hospital " etc and this just helped explain the seriousness of his accident and injuries”. - Seb’s Mum § Tip Card § Reports § Communication / ‘get out’ cards § Ideas for therapy & strategies in school / at home.

Out patient rehabilitation A continuation of inpatient rehabilitation. . . Intensive therapy Blocks of therapy Programme setting with review Monitoring with advice It may be needed for many years with each stage of development presenting new challenges § It needs to be delivered across all environments to ensure consistency and generalisation of skill. § Skills may need to be taught in each environment individually. § § §

Common features of the community ABI paediatric caseload § Spiky profile § Variability in skills over time § Comprehension very dependent on levels of fatigue and attention § Word finding difficulties § Rigidity of concept formation § Difficulty learning time concepts § Difficulties with abstract language § Conversation initiation § Disinhibition when speaking § Sensation changes within the mouth – affecting eating and drinking and / or saliva management § Oro-motor control changes – affecting eating and drinking and/ or speech and /or saliva management

Conversation initiation § § § i. Pad – calendar apps Photo boards / visual displays Photo key rings Strategies – looking around the room / at the person speaking to for ‘clues’ about what to say Context dependent scripts Question cards ‘Wh’ question words Games in which need to ask questions: Guess who, 20 questions, Headbanz Role play Scaffolding of conversation Music Adapted speaking circles

Sensory oro-motor skills § Use of tactile tools to address difficulties in sensation, oro-motor weakness or difficulties in planning the movements of the tongue, lips, soft palate etc. § Detailed assessment and specific and finely graded programme is developed. § Programme needs to be delivered on a daily basis approx 15 -20 mins per day

Useful References… § Children With Traumatic Brain Injury – a parent’s guide. The special needs collection. Ed. Lisa Schoenbrodt. Woodbine House 2001. § Pediatric Traumatic Brain Injury, Proactive intervention. Jean L Blosser & Roberta De. Pompei. Singular Publishing Group, Inc. 1994 § Head Injury Rehabilitation, Children & Adolescents. Mark Ylvisaker. College Hill Press 1985. § Lash publications § Head Injury, A Practical Guide. Trevor Powell. Winslow 1994. § Living Skills for the Brain-Injured child and Adolescent. Julie M Buxton & Kelly B Godfrey. The Speech Bin, inc. 1999. § The Source for Pediatric Dysphagia. Nancy B Swigert. Lingui. Systems 1998.

References continued… § Acquired Neurological Speech/Language Disorders in Childhood. Bruce E Murdoch. Taylor & Francis 1990. § Feeding and Swallowing Disorders in infancy. Lynn Wolf & Robin Glass. Therapy Skill Builders 1992. § Eating and Drinking Difficulties in Children. A Guide for Practitioners. April Winstock. Speech mark 2005. § Communication, How Communication Changes over Time. ‘Tip Card’ leaflet. Roberta De. Pompei & Jean Blosser. Lash & Associates Publishing/Training inc. 1998.
- Slides: 24