Common Transient Neonatal Dermatoses Harpers Textbook of Pediatric

Common Transient Neonatal Dermatoses Harper’s Textbook of Pediatric Dermatology Presented by : M. Shahsavari

Neonatal desquamation • postmaturity in the neonate, and sometimes dysmaturity • In healthy full - term neonates, increased epidermal desquamation is also present during the first 3 months, with an overall prevalence of 39. 5% • In extreme cases, because of similarities with the collodion baby syndrome, a congenital ichthyosis may be considered

• in cases of postmaturity desquamation, there is no ectropion, no eclabium and the gloved appearance is lacking • in massive desquamation should alert the doctor to X - Linked recessive hypohidrotic dysplasia


Harlequin colour change • • • transient erythema involving one - half of the infant ’ s body with simultaneous blanching of the other side and a sharp demarcation on the midline the pathophysiology remains unknown in the subgroup of infants with HCC and non – epileptic tonic seizures triggered by abnormal painful stimulations (PEPD), it has been show that the disorder is produced by mutations in the SCN 9 A gene
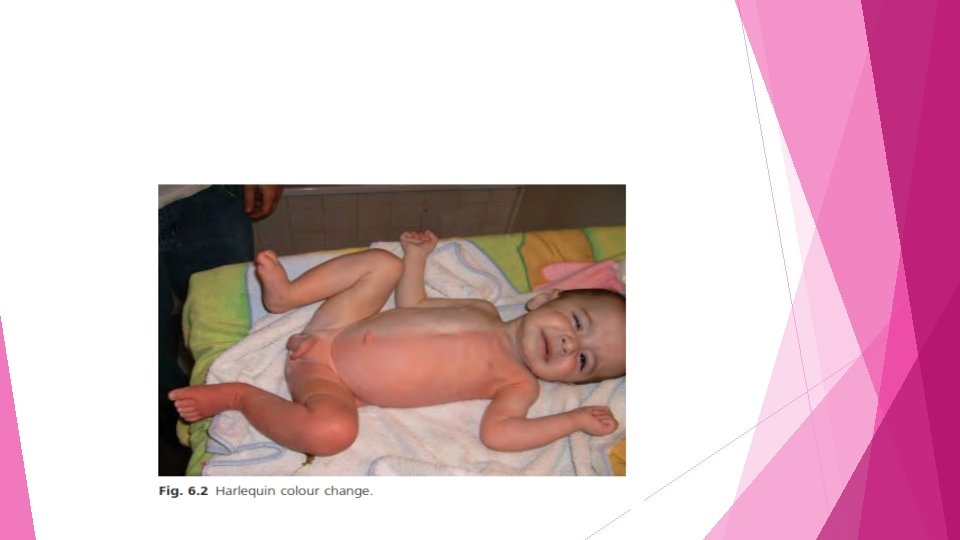

• Premature infants are more commonly affected than full term infants v. Flushing and isolated HCC • Harlequin colour change usually occurs on the third or fourth day of life, though it has been noted up until the 21 st day of life • The midline demarcation of the erythema and the transitory colour changes (30 s to 20 min) are diagnostic

• • • the face and genitalia are usually spared The tongue and lips are unaffected Turning the infant on the other side may induce blanching of the red side and reddening of the pale side

v. Paroxysmal extreme pain disorder ( PEPD ) • Typical flares are precipitated by perineal pain or stimulation, such as insertion of a thermometer into the anus, and consist of stiffening in flexion position, turning pale, and screaming inconsolably, followed by hemicorporeal flushing • after the attack, infants may experience intense sweating, and neurological examination is normal between attacks

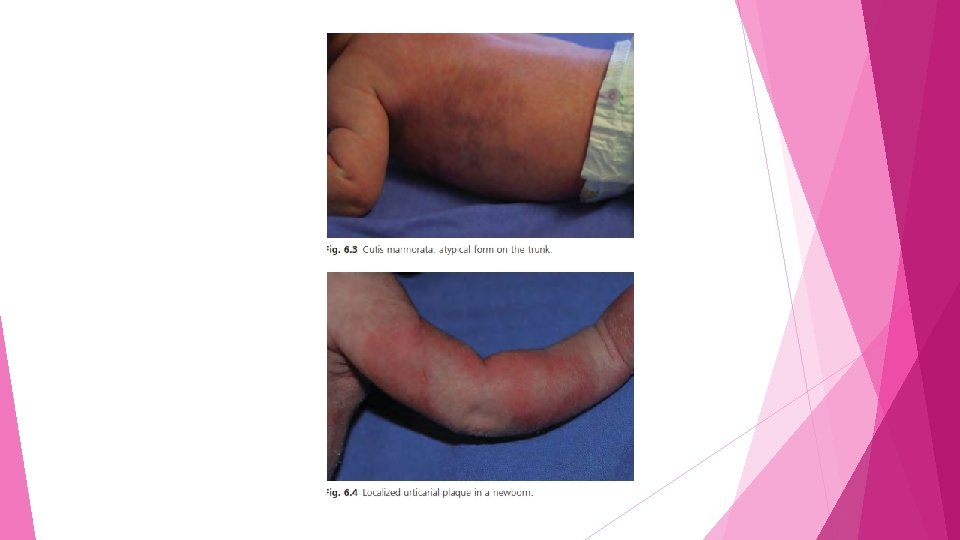
• Changes in skin colour should subside after the third week in common HCC, and during the first years in PEPD v. Differential diagnosis and treatmen • capillary malformation • cutis marmorata telangiectatica congenita • Transient dermatographism • No treatment is required • carbamazepine therapy may be effective to reduce the frequency of the flares

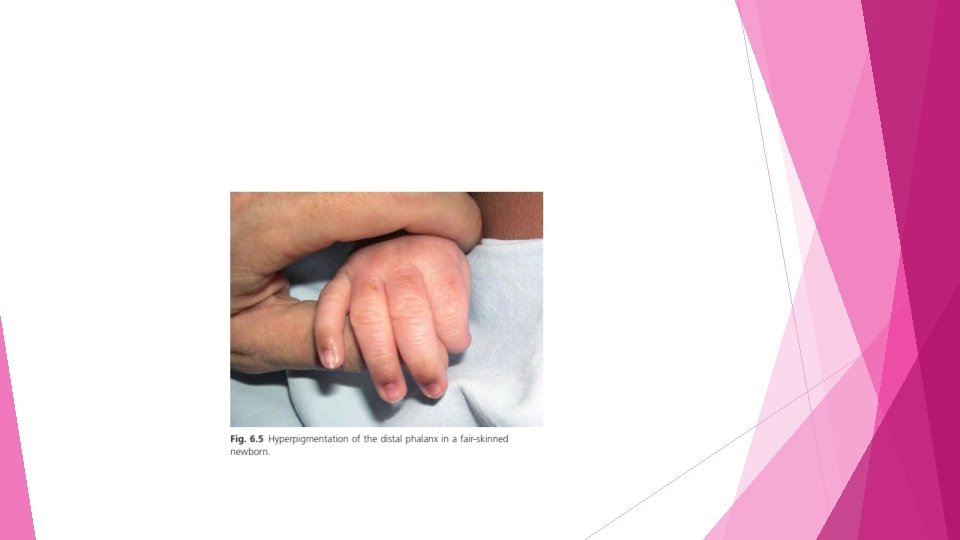
Transient localized hyperpigmentation • • • The maturation of the pigmentary system is not completed at birth and some areas may appear markedly hyperpigmented It is usually a prominent feature of dark - skinned newborns, but it has also been observed in fair skinned newborns Most frequently involved: The genital area(scrotum) the dorsal surfaces of the distal phalanges of both hands and feet are the most frequently involved

• Less frequently, other body areas may be involved, including nipple and areola, helix, umbilicus, and sometimes large skin folds • Perineal or periungual hyperpigmentation is considered as a physiological melanic pigmentation mainly observed during the first year of life and declining around the age of 2 years

Sterile transient neonatal papulopustular eruptions

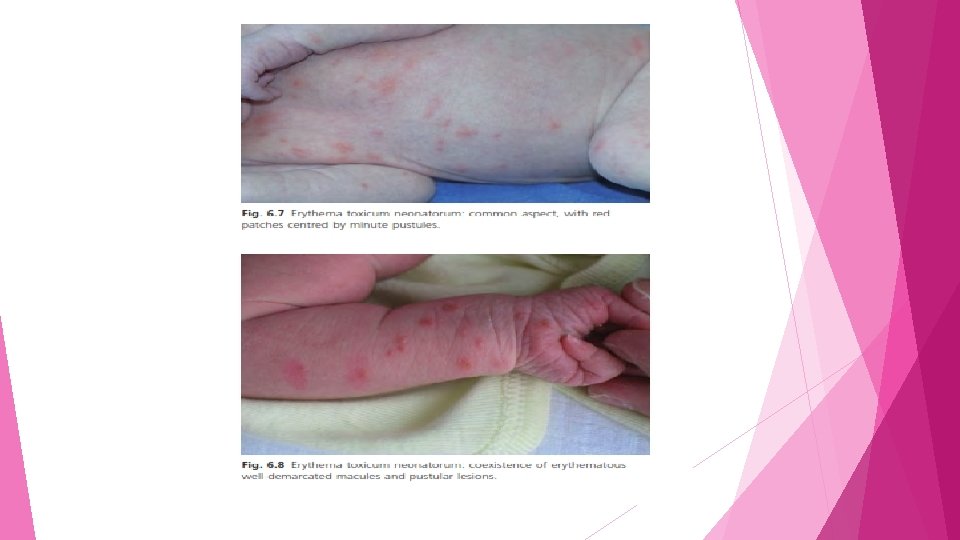
Erythema toxicum neonatorum ( ETN) • the most common transient rash in healthy term neonates, affecting 43% of the newborns • It is characterized by small erythematous macules with or without a central papule or pustule • ETN arises between the first and fourth days of life and lasts 2 or 3 days and delayed onset, as late as 10 days of age in term infants, has also been observed

• Duration is brief, usually 2 – 3 days. Pustular eruptions persist longer • Relapses and ETN - like eruptions after the end of the first month may occur rarely v Two types of eruptions are encountered • The most frequent clinical type consists of collections of erythematous and papular lesions (70% of cases). (flea bite ’picture)

• In 30% of cases the eruption is predominantly pustular, occasionally surrounded by a small erythematous rim • Lesions are located mostly on the trunk, with a predilection for the back, but are readily found on the upper arms, thighs and face, where they may predominate • • The palms and soles are relatively spared Atypical cases of ETN with pustules localized to the genital areas have been reported


v. Aetiology • The cause of ETN is not yet established 1. too long exposure with the meconium 2. According to Leiner , many newborn infants with the condition have dyspeptic disorders; thus, he proposed the term erythema toxicum ’ because he postulated that systemic absorption of enterotoxins accounted for the rash

3. the allergic theory(Eosinophilia in skin biopsies and blood) 4. a reaction to mechanical stimulation or simple pressure 5. the incidence of ETN increases with maturity, as determined by birthweight, gestational age or breast hypertrophy grade in the mother

• the incidence is controversial, and ranges from 30% to 70% • • • no predilection according to sex A lower incidence was found in black children the incidence is positively correlated with several parameters of maturity, including birthweight, and also with the number of pregnancies
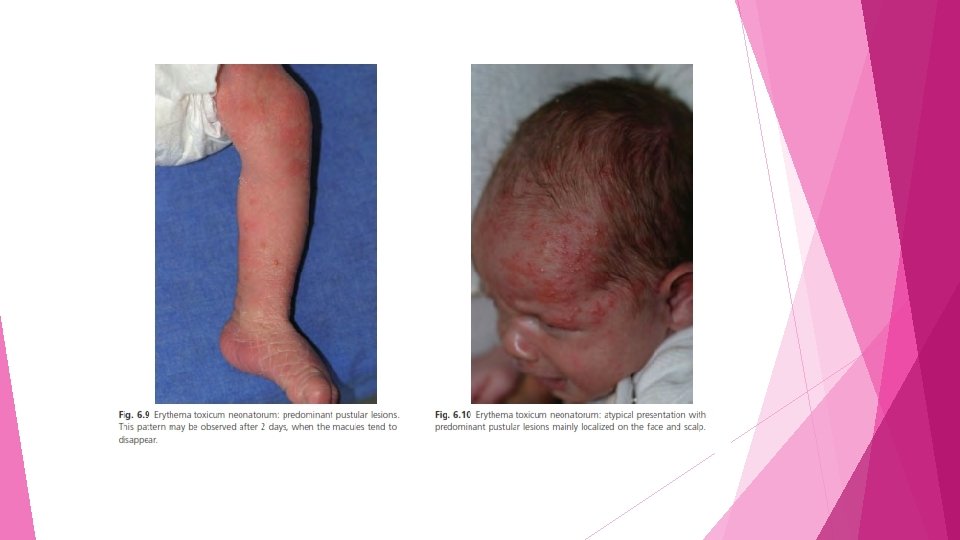

v. Differential diagnosis. • generalized sepsis(poor feeding and other signs of serious illness) • viral diseases and Candida infection (Tzanck smear) • • • incontinentia pigmenti Eosinophilic pustular folliculitis Atypical forms of self - healing histiocytosis

• Job – Buckley syndrome may present at birth with eosinophilic eruption, as may Omenn severe combined immunodeficiency • Acropustulosis of infancy may also, rarely, begin at birth or in the first 3 weeks, and pustules may contain eosinophils. Most cases, however, are characterized by a neutrophilic infiltrate and onset after the neonatal period. The location of lesions and the relapsing course permits a diagnosis.

v. Pathology • In macular erythematous lesions, edema of the upper • • dermis was associated with a mild cellular infiltration of eosinophils and neutrophils in a perivascular or diffuse distribution in papules, more edema and cellular infiltration is found, with a predominance of eosinophilic leucocytes Of cells filling the pustule, 70 – 95% are eosinophils Treatment. No treatment is necessary or indicated administration of an antihistamine, Pyribenzamine, to a series of 75 babies with ETN was found to reduce by half the duration of the rash

Transient pustular melanosis • characterized by pustules that are present at birth and evolve into areas of macular pigmentation • • more common in black neonates The content of the pustules is mostly neutrophilic, and the duration of the rash, especially the pigmentation, is longer

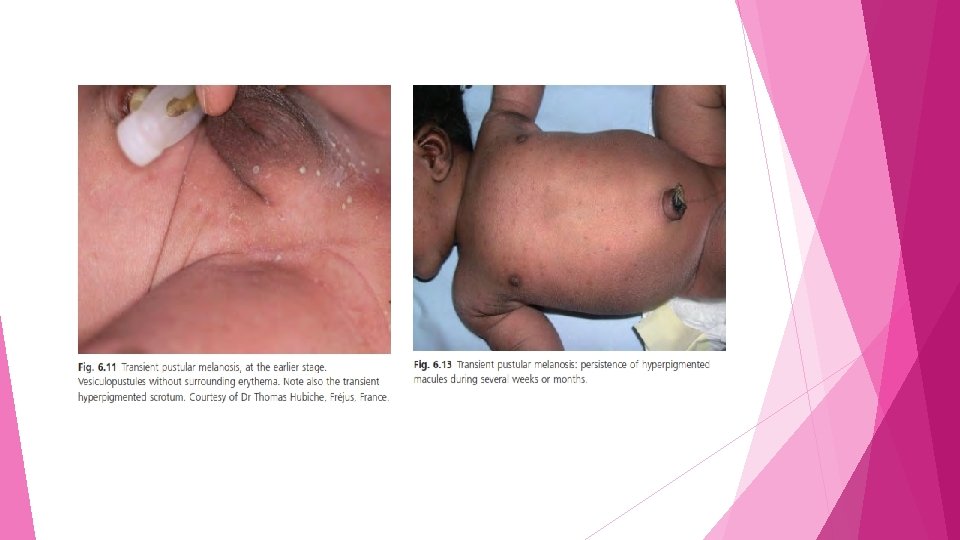
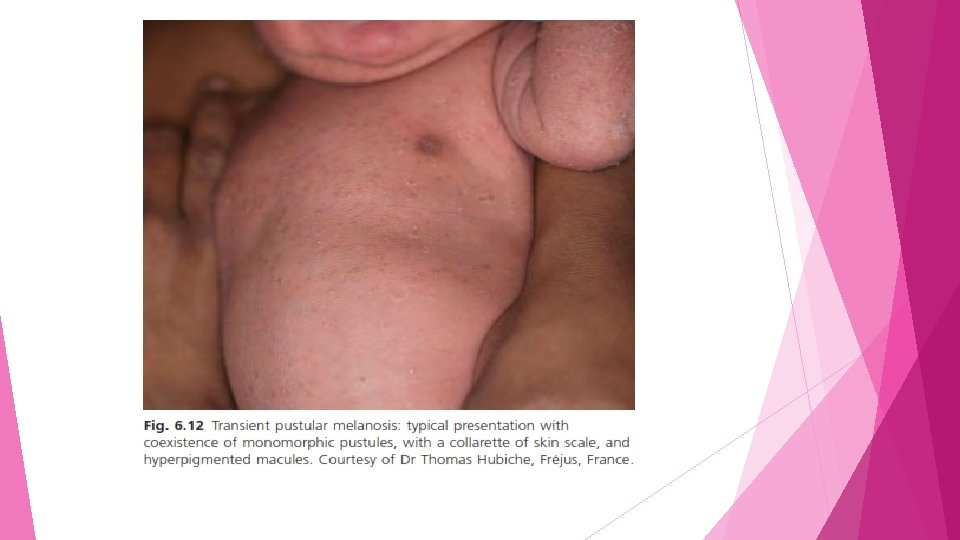
• • Lesions are located on the chin, neck, nape, upper chest, lower back and buttocks but also on the lower abdomen and medial side of the thighs Rarely, scalp, palms and soles are involved In typical cases, at the onset, pigmented macules coexist with flaccid vesiculopustules they rupture easily, leaving a collarette of fine white scale , Individual pustules dry out and may leave a flat brownish crust

• Unscratched crusts may persist for a few weeks, and in darker - skinned patients pigmented freckles may persist for a few months (lentiginosis neonatorum) v. Aetiology • The higher incidence in black neonates may be related to an accelerated stimulation of native melanocytes due to cytokines and to release of growth factor by cells in the epidermal infiltrate

• • • Pathology fontana – Masson staining reveals an increased amount of melanin in the basal and suprabasal layers Most characteristically, the subcorneal pustule contains polymorphonuclear leucocytes and scattered eosinophils In the dermis, eosinophils and/or neutrophils may be seen around capillaries and around the upper portion of the hair follicle No treatment is required

Miliaria • occlusion of sweat ducts at various levels, resulting in leakage of sweat in the epidermis or papillary dermis 1. strong connection between the use of occlusive agents such as ethyl chloride spray, iontophoresis of various chemicals, ultraviolet irradiation and occlusive plastic wraps and the induction of miliaria crystallina or rubra in adult volunteers subjected to warm conditions

2. A causative role for cutaneous bacteria has long been suspected (Staphylococcus epidermidis ) 3) an initial functional or ultrastructural obstruction damages the acrosyringium and leads to the reparative formation of a parakeratotic plug which perpetuates the disease process

Miliaria crystallina ( sudamina) • 1 – 2 mm superficial clear non - inflammatory vesicles, resembling drops of water, which are asymptomatic • common in the summer months and is also noted in infants housed in incubators • Lesions occur mostly on the forehead, and on the sixth to seventh day of life • • They spread over the scalp in a few hours Onset before the fourth day of life is exceptional

• congenital cases have been reported, attributed to a maternal febrile illness prior to delivery, as well as to the moist occlusive environment of amniotic fluid and vernix caseosa • in congenital cases, the lesions are generalized but spare the palms, soles and mucosae

Miliaria rubra ( prickly heat) and miliaria profunda • • Miliaria rubra occurs later than miliaria crystallina • outbreaks may be preceded by episodes of miliaria crystalline • • occurs mostly in hot, humid conditions Typical onset is between the 11 th and 15 th days of life It usually affects sites of friction or occlusion, such as the neck and face, but also occurs on the trunk
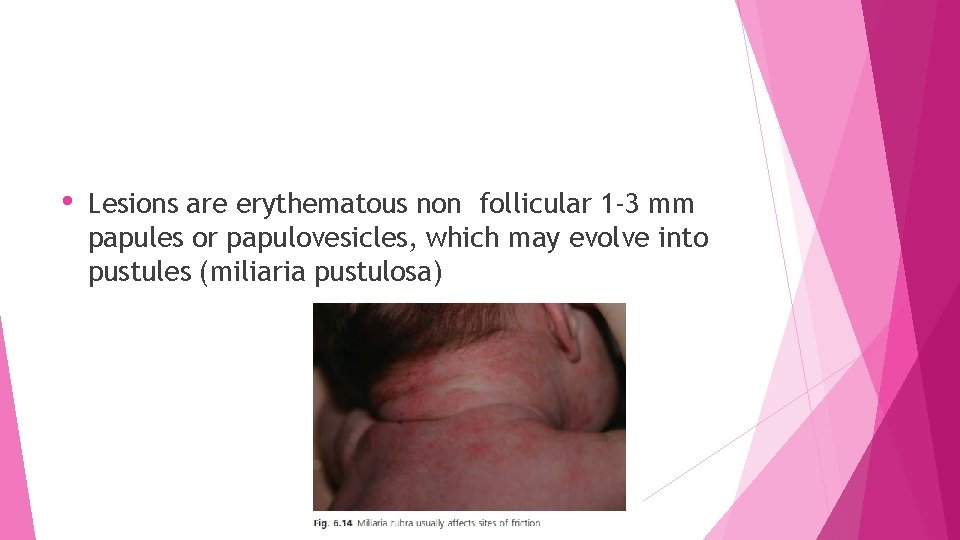
• Lesions are erythematous non follicular 1 -3 mm papules or papulovesicles, which may evolve into pustules (miliaria pustulosa)

v. Miliaria profunda • firm, pale papules on the trunk and extremities • may follow miliaria rubra • unusual in newborns • In miliaria rubra, the level of ductal obstruction is intraepidermal • In miliaria profunda, eccrine ducts are obstructed at the dermoepidermal junction

• in type I pseudohypoaldosteronism, pustular miliaria rubra is considered to be a specific cutaneous finding( salt - losing crises ) v. Treatment • the patient should be removed from the warm and humid environment • Cool bathing and air conditioning are the best therapeutic measures

• In the case of suspicion of superinfection, antibiotics may be started • chlorhexidine cleansing solution or a topical antibiotic (such as erythromycin or clindamycin) may beadvised • One case of extensive miliaria profunda responded to isotretinoin therapy

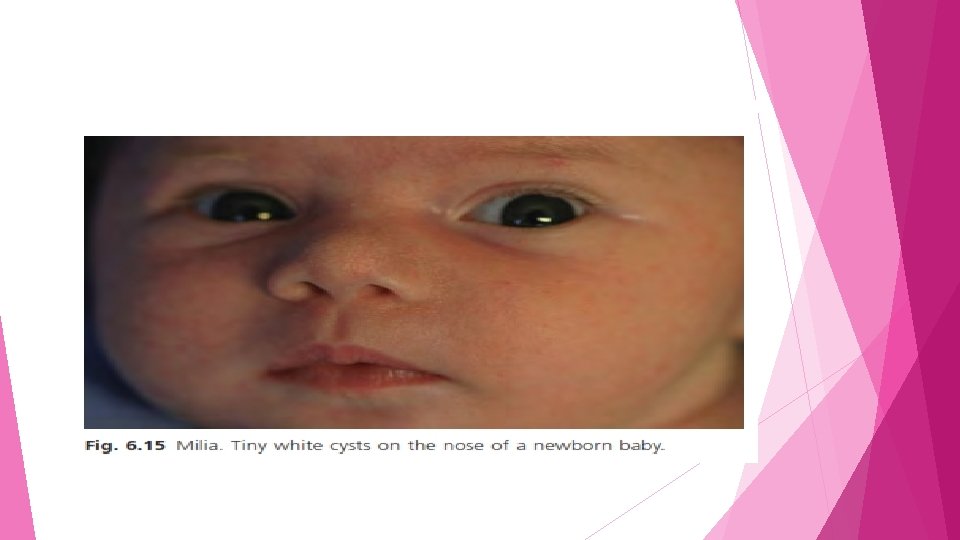
Milia: Bohn and Epstein pearls • the most common transient skin disorders in neonatal (30 -40 %) • 1– 2 mm white or yellow papules on the nose, chin, cheeks and forehead • • The nose is predominantly affected • Milia are epidermal cysts derived from the pilosebaceous follicle Less commonly, lesions may occur on the trunk and extremities

• • • they are normally spontaneously extruded in a few weeks Persistent or extensive milia are seen in Marie Unna hypotrichosis, orofacial - digital syndrome type I, Basan syndrome, and the X – linked Bazex –Dupré –Christol disease, which is also characterized by hypotrichosis

• Epstein pearls – epidermal cysts on the palate – are present in the majority of newborn infants • When they occur on the alveolar margins, they are termed Bohn cysts

Perianal dermatitis • an area of erythema centred on the anus and occasionally accompanied by erosion and bleeding • • Prevalence : 4% to 18. 9% • It is observed between the fourth and seventh days of life • 6. 5 times more frequent in premature babies usually attributed to formula milk feeding in the newborn and abnormal faecal p. H

Adnexal polyp of neonatal skin • • 4. 1% of Japanese neonates • • it detaches spontaneously small, usually solitary, skin tag situated around the nipple Two cases of persistent lesions, in a 53 - and a 370 - day - old - infant, have been reported
- Slides: 48