Common Problems in the Female Athlete Jennifer Roth

Common Problems in the Female Athlete Jennifer Roth, MD Family & Sports Medicine Consultant Mayo Clinic Florida

DISCLOSURE Relevant Financial Relationships None Off Label Usage None

Benefits of Athletics • Improved physical fitness • Enhanced self-esteem • Improved physical and mental health • Promotion of peak bone mass • Encourage team building and leadership skills

Title IX Patsy T Mink Equal Opportunity in Education Act • June 23, 1972 • "No person in the United States shall, on the basis of sex, be excluded from participation in, be denied the benefits of, or be subjected to discrimination under any education program or activity receiving Federal financial assistance. . . " • —United States Code Section 20
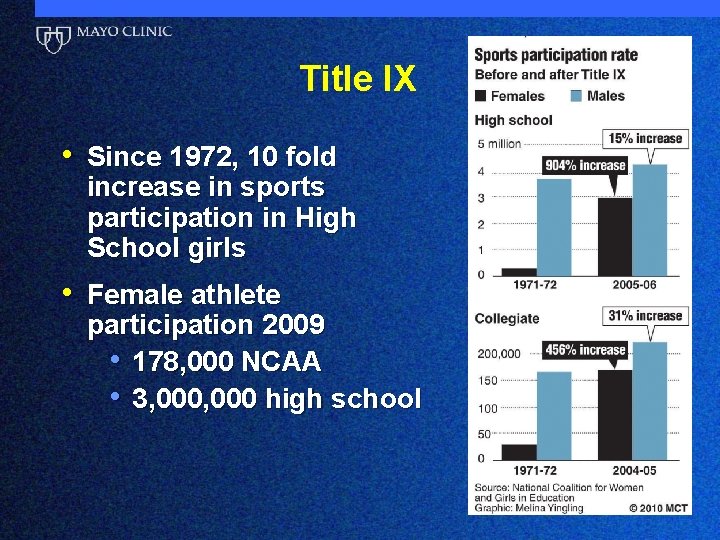
Title IX • Since 1972, 10 fold increase in sports participation in High School girls • Female athlete participation 2009 • 178, 000 NCAA • 3, 000 high school

Sex Differences • Children- • similar characteristics and body mass • Growth phases Females Growth Spurt 9 -10 yo Males 12 -15 yo Puberty ~2. 5 cm growth Peak growth after menarche phase Height Maturation 16 -17 yo 20 -21 yo

Sex Differences • Strength • Equal muscle • fiber ratio, but females have smaller fibers After puberty, women only have small amount of increase in strength AGE (yrs) % Strength Female vs Male Birth- 10 11 -12 100% equal 90 13 -14 15 -16 85 75 Greydanus, D The Adolescent Female Athlete, Ped Clin N Am, 2010
Sex Differences • Body composition • Female ~25% body fat vs 14% male • Male greater muscle mass due to • androgen effect Performance • For same body weight (and training), FEMALES have • Smaller heart lower stroke volume • Lower blood pressure • Smaller lungs decreased VO 2 max • Lower blood volume, lower Hgb • …decreased endurance performance

Knee Injuries Common to the Female Athlete • Patellofemoral Pain (PFPS) • Anterior Cruciate Ligament (ACL) tears

ACL Tears- Why more common in females? • NCAA female athletes 2 -8 x more likley to sustain ACL tear than males • Anatomy • Hormonal • Biomechanical • Environmental 10

ACL Tears in Female Athletes • Noncontact Injury 85% > Contact 15% • 29% Planting/cutting • 28% Straight knee landing • 26% One-step landing with knee in hyperextenison 11 11

ACL Tears in Female Athletes ANATOMY • 2 bundles- resist anterior translation of tibia relative to femur • Female ACLs smaller in size • Decreased intracondylar knotch width in females http: //www. scoi. com/aclrecon. htm 12

ACL Tears in Female Athletes HORMONES • Estrogen receptors found in fibroblasts, decreases collagen formation • High levels of estrogen may decrease neuromuscular control • may increase laxity • Injury rate highest during preovulatory phase compared to postovulatory 13

ACL Tears in Female Athletes BIOMECHANICS • “Miserable Malalignment” • excessive foot pronation • pes planus • external tibial rotation • Q-angle >15 deg • Femoral anteversion • Hypoplastic VMO • Heel valgus angulation 14
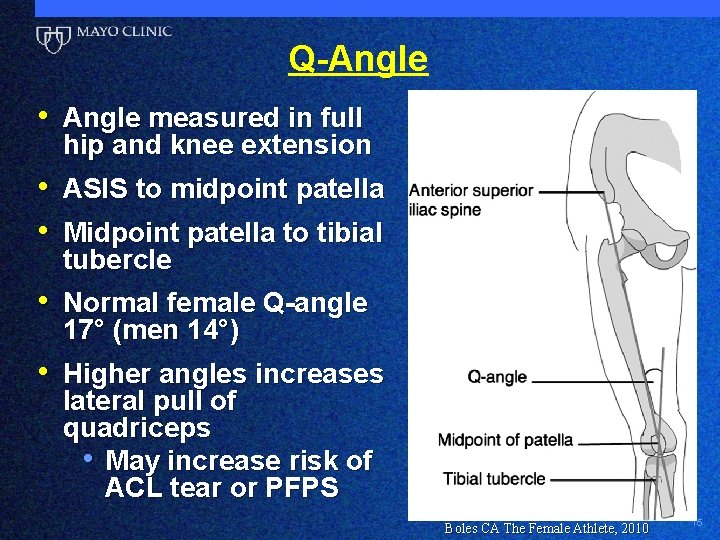
Q-Angle • Angle measured in full hip and knee extension • ASIS to midpoint patella • Midpoint patella to tibial tubercle • Normal female Q-angle 17° (men 14°) • Higher angles increases lateral pull of quadriceps • May increase risk of ACL tear or PFPS 15 Boles CA The Female Athlete, 2010 15
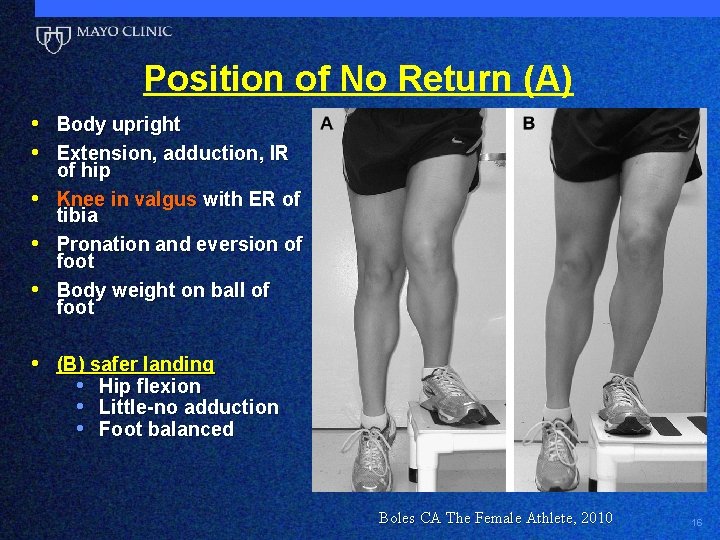
Position of No Return (A) • Body upright • Extension, adduction, IR • • • of hip Knee in valgus with ER of tibia Pronation and eversion of foot Body weight on ball of foot • (B) safer landing • Hip flexion • Little-no adduction • Foot balanced Boles CA The Female Athlete, 2010 16

Position of No Return http: //www. exercisebiology. com/index. php/site/articles/how_to_prevent_acl_injuries 17
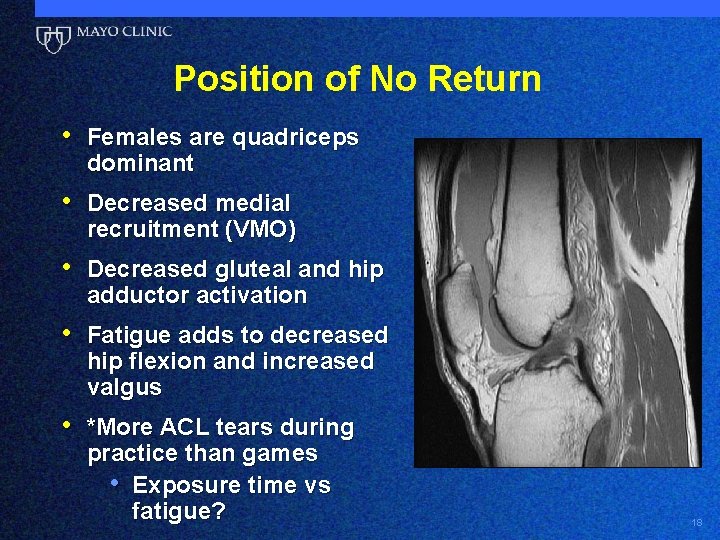
Position of No Return • Females are quadriceps dominant • Decreased medial recruitment (VMO) • Decreased gluteal and hip adductor activation • Fatigue adds to decreased hip flexion and increased valgus • *More ACL tears during practice than games • Exposure time vs fatigue? 18

ACL Tears in Female Athletes ENVIRONMENT • Surface • Drier surfaces increases • friction Artificial turf mixed results • Shoe type • Cleat size and pattern • Knee braces • INEFFECTIVE to prevent • ACL tear Long term may decrease quad strength 19

ACL Treatment Surgical vs Nonsurgical • Surgical • Younger, active athletes • Autograft vs allograft • Nonsurgical • Older, less active • Increased risk early degenerative changes 20

ACL Tear Prevention • PEP Programs • (Prevent injury Enhance Performance) • Increased hamstring strength • Increases dynamic stability of ACL • Appropriate warm up • Landing techniques • Hamstring • strengthening 21
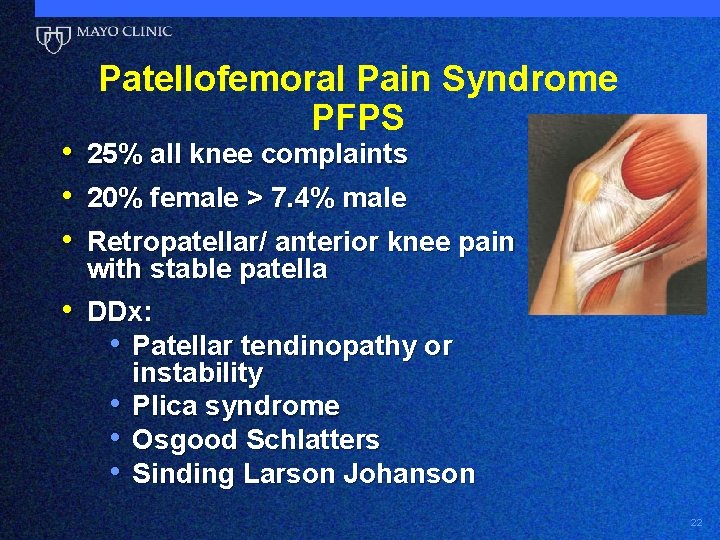
• • • Patellofemoral Pain Syndrome PFPS 25% all knee complaints 20% female > 7. 4% male Retropatellar/ anterior knee pain with stable patella • DDx: • Patellar tendinopathy or • • • instability Plica syndrome Osgood Schlatters Sinding Larson Johanson 22

PFPS: Causes • Quad dysfunction • VMO to vastus lateralus imbalance • Static Malalignment • Q-angle • Larger angle increased lateral • • forces Femoral neck anteversion, external tibial torsion, hyperpronation Extensor mechanism malalignment • Patellar maltracking • Dynamic Malalignment- cutting & landing • Hip adduction and internal rotation, contralateral pelvic drop 23
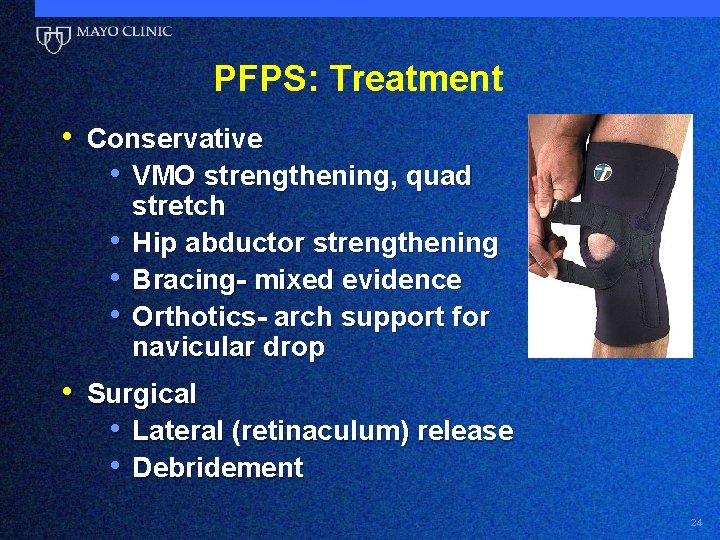
PFPS: Treatment • Conservative • VMO strengthening, quad • • • stretch Hip abductor strengthening Bracing- mixed evidence Orthotics- arch support for navicular drop • Surgical • Lateral (retinaculum) release • Debridement 24
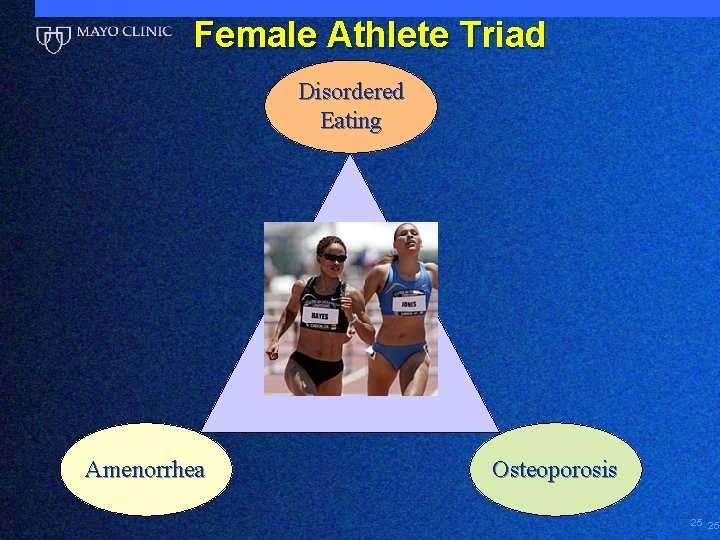
Female Athlete Triad Disordered Eating Amenorrhea Osteoporosis 25 25

Female Athlete Triad • 1992 - ACSM Task Force on Women's Issues • Identified 3 interrelated disorders • 1997 - ACSM Position Statement • Classic definition • Defined prevalence & consequences • Call for research • 2007 - ACSM Position Statement- revised • Low energy availability is key disorder • Athletes can exist along a spectrum 26 26

Energy Availability Menstrual Function Bone Health 27 27
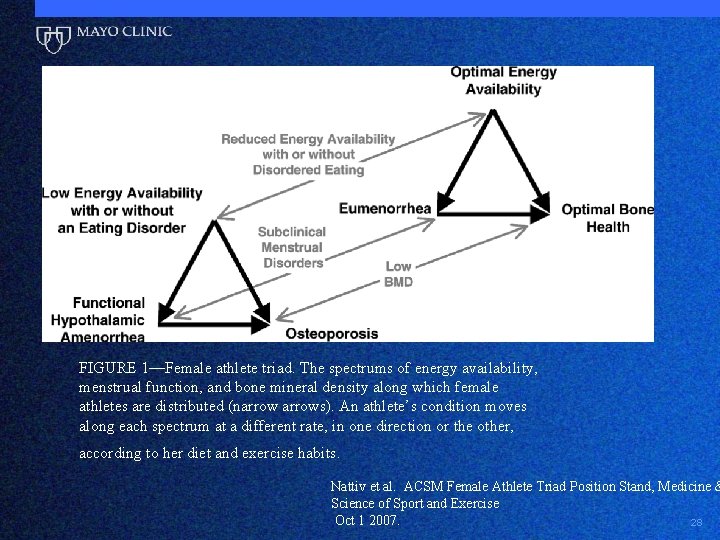
FIGURE 1—Female athlete triad. The spectrums of energy availability, menstrual function, and bone mineral density along which female athletes are distributed (narrows). An athlete’s condition moves along each spectrum at a different rate, in one direction or the other, according to her diet and exercise habits. Nattiv et al. ACSM Female Athlete Triad Position Stand, Medicine & Science of Sport and Exercise Oct 1 2007. 28
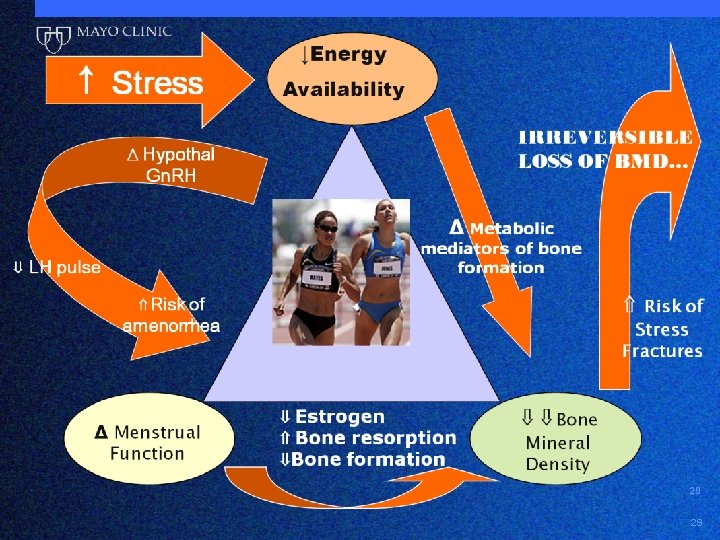
29

Female Athlete Triad Risk Factors/ Red Flags • Sports that emphasize appearance • Ballet, figure skating, gymnastics, cheerleading • Pressure to maintain low body mass for optimal performance • Cross country, swimming, martial arts • Overtraining • Outside scheduled practice or until • exhaustion Training even if sick or injured • Traumatic event: injury, poor performance, coach 30
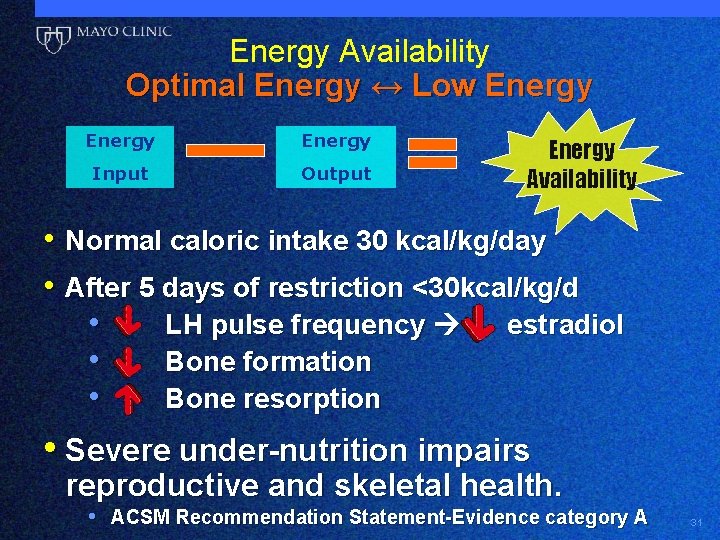
Energy Availability Optimal Energy ↔ Low Energy Input Output Energy Availability • Normal caloric intake 30 kcal/kg/day • After 5 days of restriction <30 kcal/kg/d • LH pulse frequency estradiol • Bone formation • Bone resorption • Severe under-nutrition impairs reproductive and skeletal health. • ACSM Recommendation Statement-Evidence category A 31

Disordered Eating • More prevalent in sports that emphasize: • Appearance- gymnastics, figure skating, diving, cheerleading • Leanness- track & field, crew, distance running • *ACSM Evidence Statement A • Food restriction • Ex: high fat, protein, • carbs Binge/Purge • Self induced, diet pills, laxatives, diuretics, excessive exercise 32

Eating Disorders (DSM-IV) • Anorexia nervosa • Restrictive eating • Distorted view that pt is overweight • Intense fear of gaining weight • >15% underweight (BMI <18. 5) • Amenorrhea is a DSMIV criteria • Bulimia nervosa • Normal weight range • Binge purge > 2 times/week • Eating disorder NOS 33

Anorexia Athletica • Distinctly associated w sports training: • Perfectionism • Compulsiveness • Competitiveness • High self motivation • Menstrual disturbances • Unhealthy weight control (at least ONE) • Fasting, vomiting, diet pills, laxatives, diuretics 34

Menstrual Function Eumenorrhea ↔ Amenorrhea • Oligomenorrhea: menses occurring >35 day cycles • Amenorrhea: menses occurring >90 day cycles • Primary: delay in the age of menarche >15 yo in • a girl with secondary sexual characteristics • Or- absence of any secondary sexual characteristics by age 14 • Competition in sports at younger ages ex: gymnastics, skating, cheerleading Secondary: cessation of menses after menarche • Most common form of athletic amenorrhea 35

Menstrual Function Eumenorrhea ↔ Amenorrhea • Prevalence of menstrual dysfunction: • General population 2 -5% • Female athletes 6 -79% • Mechanism: ENERGY DEFECIT functional hypothalamic amenorrhea • Hypothalamic-pituitary-ovarian axis • Suppression of Gn. RH • Via stress, energy deficit or decreased leptin during calorie restriction • Decrease in LH pulse frequency • Decrease in circulating estrogen 36

Bone Mineral Density Optimal Bone Health ↔ Osteoporosis • Post-menopausal Adults: • accelerated bone mineral loss • Hypoestrogen state • Adolescent Athletes: • failure to accumulate optimal BMD • Hypoestrogen, but also decreased growth factors (GH, insulin, cortisol, leptin, TSH) • Athletes in weight bearing sports should have 515% HIGHER BMD than non-weight bearing sports… • Bone loss may occur rapidly in the first 2 -3 years after menstrual disturbance ~ 4% per year 37

Bone Mineral Density Optimal Bone Health ↔ Osteoporosis Postmenopausal (WHO recs) Premenopausal Athletes (ACSM recs) Osteopenia T-score <-2. 5 SD -1. 0 > T-score > -2. 5 SD Z-score < -2. 0 “Low BMD for age” PLUS -1. 0 > Z-score >-2. 0 Risk Factors PLUS Risk Factors • Risk Factors: • Nutritional deficits • Hypoestrogenism • Stress fractures T-score: mean of zero, compares to peak BMD of healthy young woman. Z-score: relative to age, better correlation for young females <20 yrs old 38
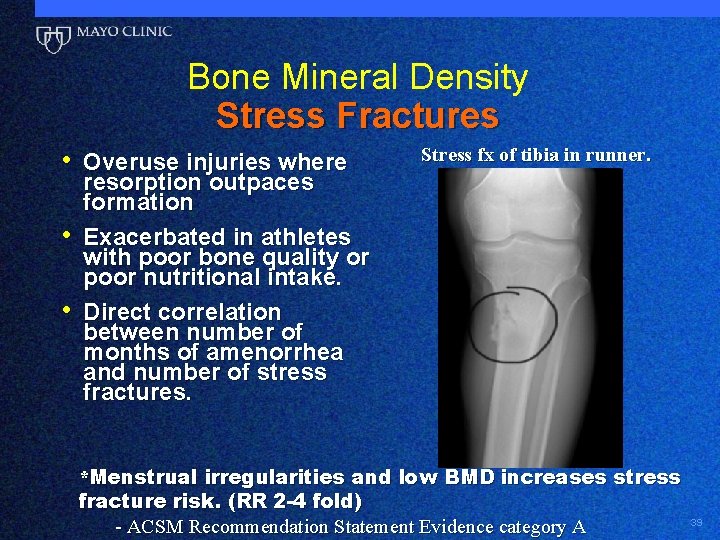
Bone Mineral Density Stress Fractures • Overuse injuries where • • Stress fx of tibia in runner. resorption outpaces formation Exacerbated in athletes with poor bone quality or poor nutritional intake. Direct correlation between number of months of amenorrhea and number of stress fractures. *Menstrual irregularities and low BMD increases stress fracture risk. (RR 2 -4 fold) - ACSM Recommendation Statement Evidence category A 39
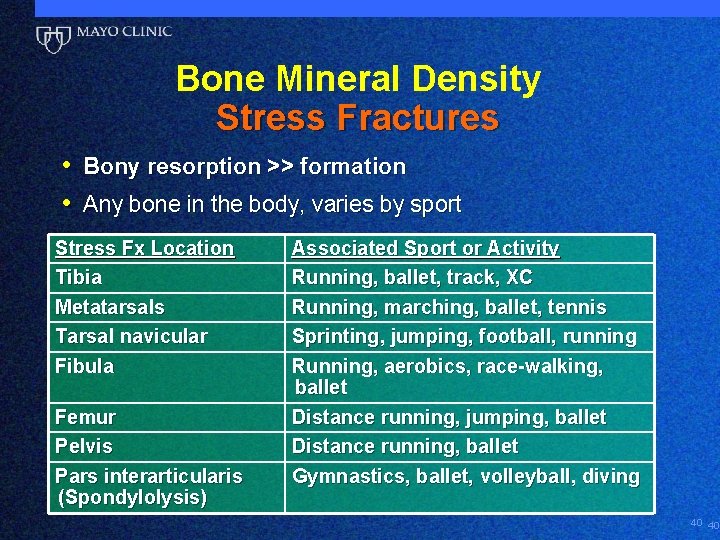
Bone Mineral Density Stress Fractures • Bony resorption >> formation • Any bone in the body, varies by sport Stress Fx Location Tibia Metatarsals Tarsal navicular Fibula Femur Pelvis Pars interarticularis (Spondylolysis) Associated Sport or Activity Running, ballet, track, XC Running, marching, ballet, tennis Sprinting, jumping, football, running Running, aerobics, race-walking, ballet Distance running, jumping, ballet Distance running, ballet Gymnastics, ballet, volleyball, diving 40 40
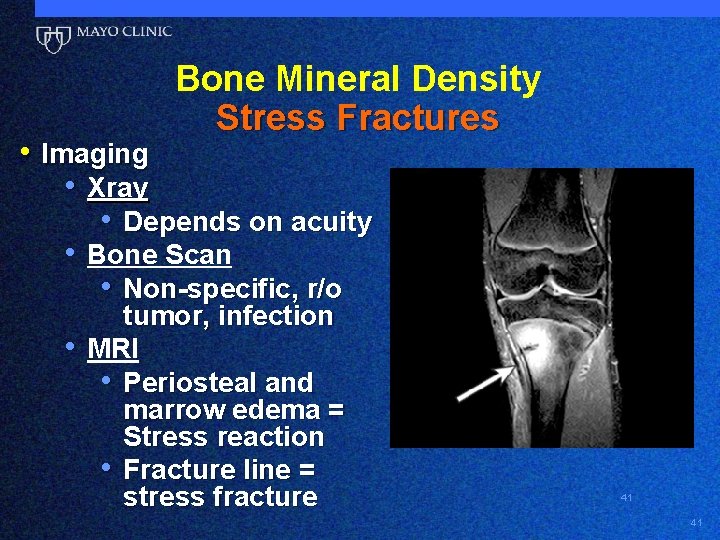
Bone Mineral Density Stress Fractures • Imaging • Xray • Depends on acuity • Bone Scan • Non-specific, r/o • tumor, infection MRI • Periosteal and marrow edema = Stress reaction • Fracture line = stress fracture 41 41

Female Athlete Triad Detection • Screening is continuous… • Detection of one component should trigger • • • investigation for all three Screening questions address • Menstrual hx • Dietary behaviors • Mental health/perception/outside pressures • Injuries (*stress fx) Lab testing (if indicated) • ** ßhcg, TSH, LH/FSH, Chem 7, prolactin Imaging (if indicated) • DXA scan • Xray vs bone scan vs MRI (determine acuity) 42 42

Female Athlete Triad Treatment • Multidisciplinary • Team physician • PA or NP • Registered Dietitian • Mental Health Provider • ATC • Coaches • Parents/family • *ACSM Evidence C • EDUCATION!! • Optimizing energy availability • Nutritional requirements • Maximize bone mineral health • Importance of weight bearing activity • Menstrual function • NOT “normal” to miss a few periods while training… 43 43

Female Athlete Triad Treatment • Overall Increase energy availability • energy intake energy expenditure • Disordered Eating • Refer to mental health practitioner • Supplements: Ca, Vit D, Vit K, protein • Must comply w tx for sport participation • Meds: SSRI plus cognitive behavioral therapy • *not Wellbutrin! 44 44

Female Athlete Triad Treatment • Functional Hypothalamic Amenorrhea • Weight gain is key to normalize menses and • • increase BMD. OCPs - delay and reduce likelihood of restoring regular menstrual cycle OCPs will not normalize metabolic factors that impair bone formation. If BMD declines in athlete >16 yo w persistent FHA, despite adequate nutrition and body weight • OK to consider OCP to minimize further bone loss No guidelines for OCPs in athletes <16 yo 45 45

Female Athlete Triad Treatment • Stress Fracture treatment • **REST** until pain free • Restoration of adequate nutrition & menstrual • cycle GRADUAL return to play Few surgical indx (poor vascular supply) • Femoral neck, base 5 th MT, tarsal navicular • Low Bone Mineral Density • Bisphonates should NOT be used • Unproven efficacy in women of child-bearing • age • Bisphonates may reside in bone for years potential harm to developing fetus * In FHA, increases in BMD are more closely associated with increases in weight than with OCP/HRT. • *ACSM Evidence Statement, Category C 46 46
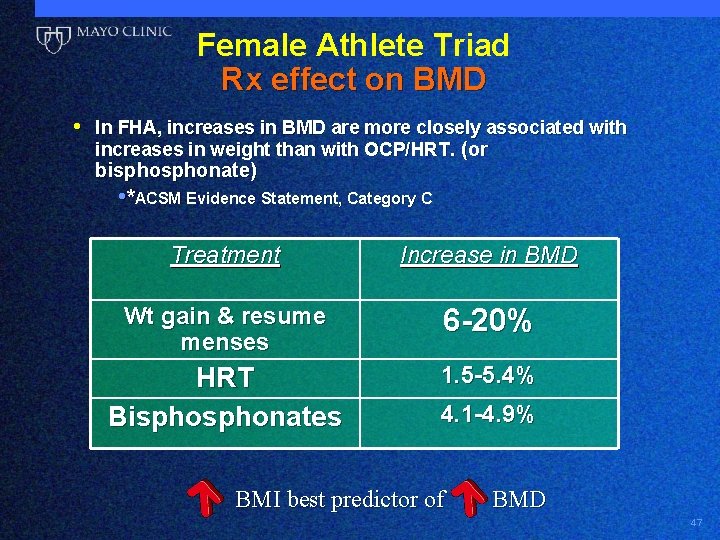
Female Athlete Triad Rx effect on BMD • In FHA, increases in BMD are more closely associated with increases in weight than with OCP/HRT. (or bisphonate) • *ACSM Evidence Statement, Category C Treatment Increase in BMD Wt gain & resume menses 6 -20% HRT Bisphonates 1. 5 -5. 4% 4. 1 -4. 9% BMI best predictor of BMD 47

Heat Related Illness • Females sex NOT considered increased risk for heat related illness • Risk factors ~ 3 athletes/year die • Children • Generate more heat, slower acclimatization, higher SA to body • Obesity • Illness (fever) • Prescription drugs (NSAIDs, diuretics, SSRI) • Environment- heat, humidity 48

Heat Related Illness Definitions • Heat Illness • Minor sx of edema, cramping, lightheaded • Tx: move to cooler area, shade, Na supp, rehydration, supine position • Heat Exhaustion • Multisystemic sx of dizziness, nausea, • • vomiting, weakness, tachycardia Core temp 38 -40. 0 C (<104 F) Tx- as above, monitor closely 49

Heat Related Illness Definitions • Heat Stroke • Symptoms of heat exhaustion AND Core temp >40 C (104 F) • MEDICAL EMERGENCY • Tx: Immediate cooling • Ice water immersion, cool NS • Cool to 102 F before transfer 50
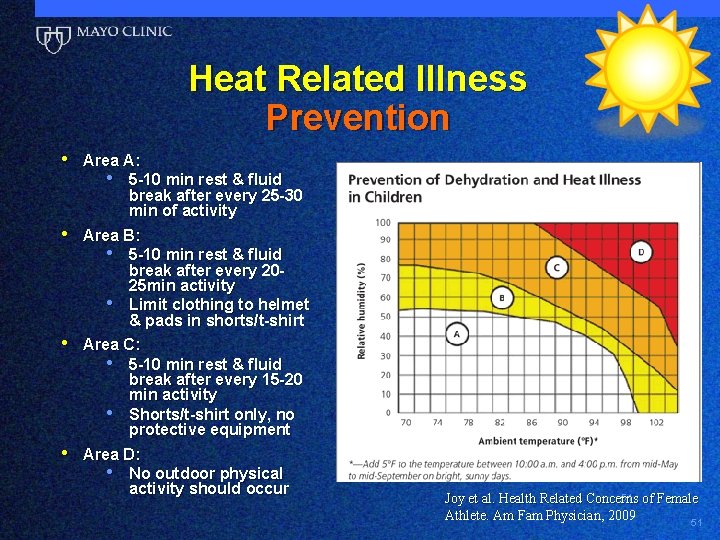
Heat Related Illness Prevention • Area A: • 5 -10 min rest & fluid break after every 25 -30 min of activity • Area B: • 5 -10 min rest & fluid • break after every 2025 min activity Limit clothing to helmet & pads in shorts/t-shirt • Area C: • 5 -10 min rest & fluid • break after every 15 -20 min activity Shorts/t-shirt only, no protective equipment • Area D: • No outdoor physical activity should occur 51 of Female Joy et al. Health Related Concerns Athlete. Am Fam Physician, 2009 51

Concussion 52

Concussion Background & Definition • Complex process affecting the brain due to direct or indirect trauma • Rapid onset of symptoms and signs of neurocognitive functions that resolve spontaneously over time • Functional NOT structural disturbance • Imaging studies NORMAL by definition • Resolution follows sequential course • Zurich 2008 ACSM Consensus • Abandoned grading scales • 80 -90% resolve within 7 -10 days 53

Concussion High Risk Populations • Children & Adolescents • Longer recovery time • NCAA 3 days vs High School >7 days • Women • Report more symptoms • Dizziness, fatigue, concentration • disturbance, lightheaded • Headaches- migraines more common • Post-concussive migraine= longer recovery Longer recovery ~ 7 days longer than men • Colvin 2009 54
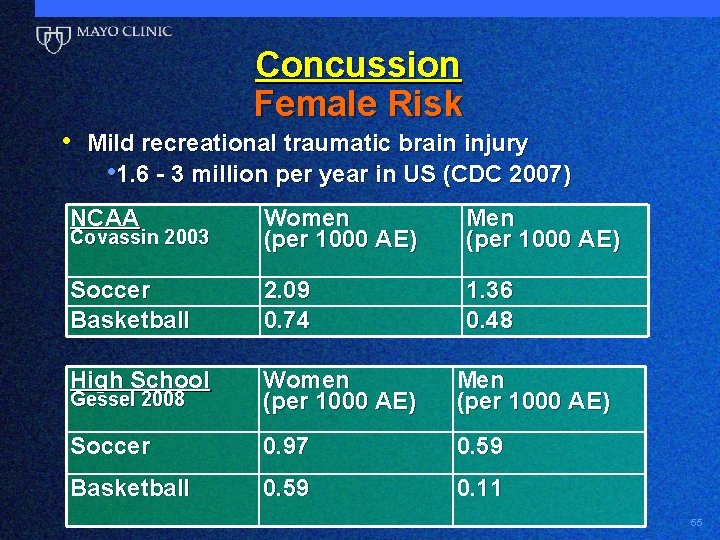
Concussion Female Risk • Mild recreational traumatic brain injury • 1. 6 - 3 million per year in US (CDC 2007) NCAA Covassin 2003 Women (per 1000 AE) Men (per 1000 AE) Soccer Basketball 2. 09 0. 74 1. 36 0. 48 High School Gessel 2008 Women (per 1000 AE) Men (per 1000 AE) Soccer 0. 97 0. 59 Basketball 0. 59 0. 11 55

Concussion Assessment • Sideline (SCAT 2) • Sideline Concussion Assessment Test • Symptom & balance scoring • Remove from play • Avoid 2 nd Impact Syndrome • Must be symptom free with slow, progressive RTP program 56

Concussion Neurocognitive Testing • Computer based testing • Assess baseline (pre-season) to post • • concussion Certified health care professional interpretation Compared to baseline and age-based normative data • Comprehensive neuropsychologic testing • Persistent sx for 4 -8 weeks • Specialist referral • Recommend MRI imaging 57

Concussion Cognitive differences by sex • At baseline • Women perform better on tasks involving verbal memory and perceptual motor speed • Men - better at visuospatial ability • Post- concussion • Women report more symptoms • Slower reaction time • Longer recovery (up to 7 days) 58

Concussion Mechanism for Female Risk • • • Greater angular acceleration on head impact Decreased neck girth (49%) Decreased neck strength (30%) • Tierney 2010 • Females larger ball to head ratio • Estrogen effect- mixed. . . • Neuroprotective vs deleterious • animal studies 59

Concussion Return to Play • RTP individualized • Step-wise progressive RTP program • Symptom free, NC test at baseline • Light aerobic activity • Increased with sprinting • Full practice before game • Game play • **Must progress sx FREE or start at prior step 60

Take home message… • Female participation in sports is expanding with many benefits • ACL tears continue to plague female sports • Consider PEP prevention programs • Suspect PFPS for anterior knee pain • Recognition of red flags and negative energy balance is key to dx Female Athlete Triad • Treatment is multifactorial • Identify and aggressively treat heat illness, but females not considered at increased risk • Concussion risk higher in females with longer recovery time • Tx must be individualized for safe RTP 61

References • • • • Bennel K, Alleyne J. Women and Activity- Related Issues Across the Lifespan. Clinical Sports Medicine. Australia, Mc. Graw Hill (2007) 749 -769. Boles C, Ferguson C. The Female Athlete. Radiol Clin N Am 48 (2010) 1249 -1266. Covassin T, Elbin RJ. The Female Athlete: The role of gender in the assessment and management of sport-related concussion. Clin Sports Med 30 (2011) 125 -131. Colvin A et al. The role of concussion history and gender in recurvery from soccer-related concussion. Am J Sports Med 37 (2009) 1699 -1704. Greydanus D, Omar H, Pratt H. The adolescent female athlete: Current concepts and conundrums. Pediatric Clinics of North America 57 (2010) 697 -718. Ireland ML, Ott S. Special concerns of the female athlete. Clin Sports Med 23 (2004) 281298. Mc. Crory P, Meeuwisse Q et al. Consensus Statement on Concussion in Sport: the 3 rd International Conference on Concussion in Sport held in Zurich, Nov 2008. Brit J Sports Med 43 (2009) Suppl I i 76 -84 Nattiv a, Loucks A, Manore M et al. ACSM Position Stand: The Female Athlete Triad. Med Sci Sports & Ex. (2007) 1867 -77. Rauh M, Nichols J et al. Relationships among injury and disordered eating, menstrual dysfunction and low bone mineral density in high school athletes: A prospective study. Jour Athletic Training 45 (2010) 243 -252. Renstrom P et al. Non-contact ACL injuries in female athletes: an International Olympics Committee current concepts statement. Brit Jour Sports Med 42 (2008) 394 -412. Tierney RT et al. Gender differences in head-neck segment dynamic stabilization during head acceleration. Med Sci Sports Exerc 37 (2005) 272 -9. Thijs Y, et al. Relationship between hip strength and frontal plane posture of the knee during a forward lunge Br J Sports Med (2007); 41: 723 -727 Zebis M et al The effects of neuromuscular training on knee joint motor control during sidecutting in female elite soccer and handball players. Clin J Sport Med. 18 (2008). 329337.
- Slides: 62