Common neonatal disorders PRESENTED BY Mrs Benazeera Lecturer

Common neonatal disorders PRESENTED BY Mrs. Benazeera Lecturer, YNC Dept. Child Health Nursing

Common neonatal disorders and congenital disorders

Learning objectives 1. List down the common neonatal disorders 2. Identification of neonatal disorder 3. List down the common congenital disorders

Birth injuries üCaput succedaneum üCephalhematoma üFractures üFacial paralysis üErb’s/Brachial palsy
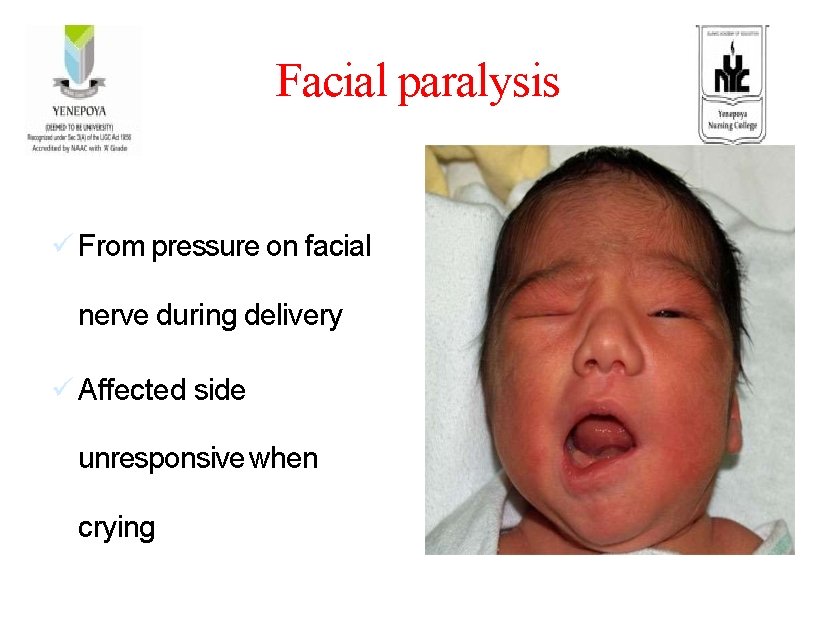
Facial paralysis ü From pressure on facial nerve during delivery ü Affected side unresponsive when crying
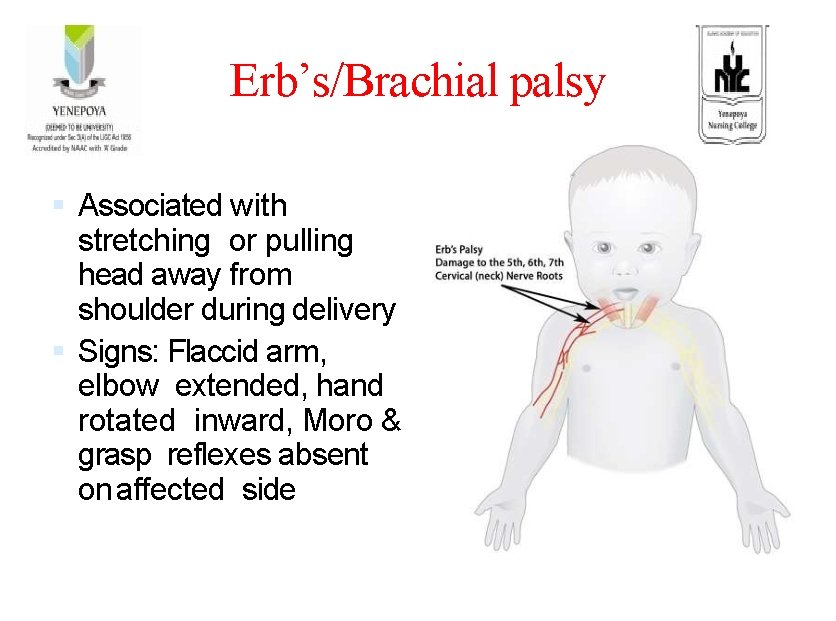
Erb’s/Brachial palsy Associated with stretching or pulling head away from shoulder during delivery Signs: Flaccid arm, elbow extended, hand rotated inward, Moro & grasp reflexes absent on affected side

Disorders related to physiological factors Hyperbilirubinemia Hemolytic disease of the newborn Respiratory distress syndrome
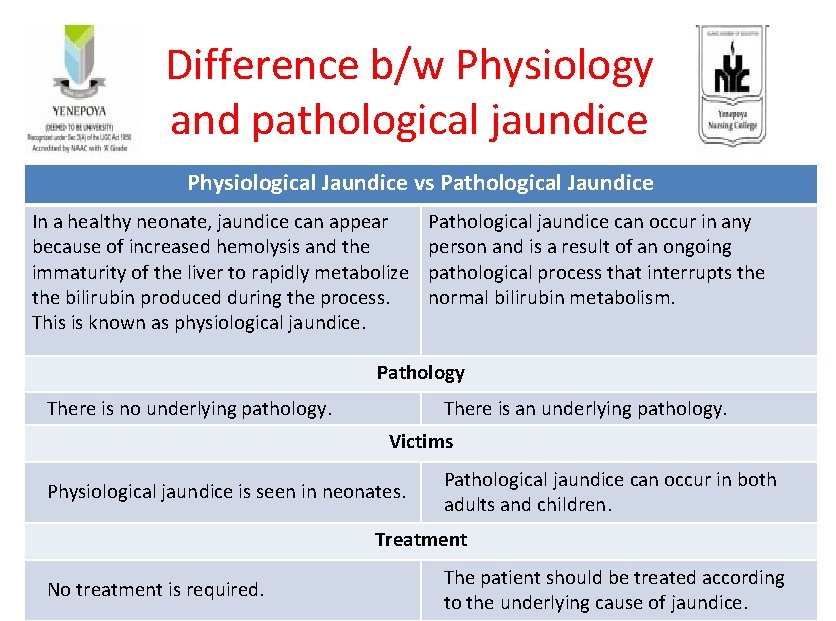

Difference b/w Physiology and pathological jaundice Physiological Jaundice vs Pathological Jaundice In a healthy neonate, jaundice can appear because of increased hemolysis and the immaturity of the liver to rapidly metabolize the bilirubin produced during the process. This is known as physiological jaundice. Pathological jaundice can occur in any person and is a result of an ongoing pathological process that interrupts the normal bilirubin metabolism. Pathology There is no underlying pathology. There is an underlying pathology. Victims Physiological jaundice is seen in neonates. Pathological jaundice can occur in both adults and children. Treatment No treatment is required. The patient should be treated according to the underlying cause of jaundice.

Disorders related to infectious process Sepsis Necrotizing enterocolitis

Disorders related to maternal conditions Infants of diabetic mothers

Infants of diabetic mothers

C/M • Clinical manifestations of IDM: Large for gestational age Very plump and full faced Abundant vernix caseosa Pleothora Listlessness and lethargy Large placenta and umblical cord Possibly meconium stained at birth

HAEMOLYTIC DISEASE q. Rh INCOMPATIBILITY q. ABO INCOMPATIBILITY
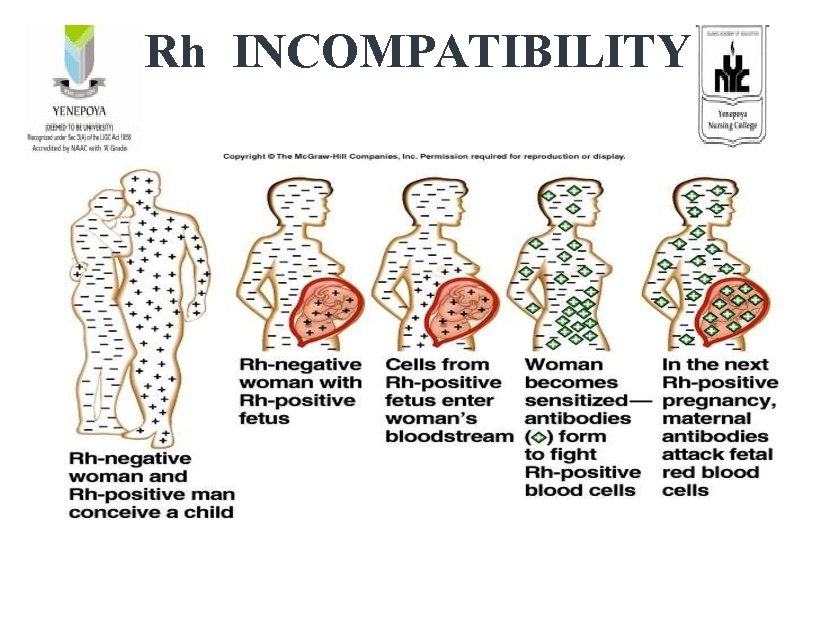
Rh INCOMPATIBILITY
![PROPHYLACTIC MEASURE Prophylactic vaccinations- [ANTI-D GAMAGLOBULIN] • During every pregnancy • After a miscarriage PROPHYLACTIC MEASURE Prophylactic vaccinations- [ANTI-D GAMAGLOBULIN] • During every pregnancy • After a miscarriage](http://slidetodoc.com/presentation_image_h/24c2f3b2e199bea083013d222a7b6ed3/image-15.jpg)
PROPHYLACTIC MEASURE Prophylactic vaccinations- [ANTI-D GAMAGLOBULIN] • During every pregnancy • After a miscarriage or abortion • After prenatal tests such as amniocentesis and chorionic villus biopsy • After injury to the abdomen during pregnancy

IDENTIFICATION AND NURSING MANAGEMENT OF COMMON CONGENITAL DISORDER

Congenital anomalies (birth defects) can be defined as structural or functional anomalies (e. g. metabolic disorders) that occur during intrauterine life and can be identified prenatally, at birth or later in life.

• According to the World Health Organization (WHO) in 2017, an estimated 270 000 deaths during the first 28 days of life were reported due to congenital anomalies globally.

IDENTIFICATION ü Preconception screening ü Peri-conception screening: v. First trimester screening: is a combination of two tests performed between 11 th and 13 th weeks of pregnancy:

Second trimester screening: Second trimester screening tests are advised between 15 th and 20 th weeks of pregnancy. Triple screen test/ quad screening Anomaly Ultrasound Amniocentesis: [Down syndrome, muscular dystrophy, sickle cell anaemia, thalassemia and cystic fibrosis.

NURSING ACTION • Avoid harmful drugs and medical radiation during pregnancy • Increasing and strengthening education of health staff

• Chorionic villus sampling (CVS): chromosomal disorders such as Down syndrome • Cordocentesis: also called percutaneous umbilical blood sampling, ------foetal abnormalities after 17 weeks of pregnancy.

Nursing management 1. ü ü Primary prevention Family welfare services Maintaining good preconception health women Promoting healthy lifestyle measures Controlling pre-conceptional medical conditions/diseases ü Avoiding environmental exposure to hazardous substances

Secondary prevention • Genetic counseling

Tertiary prevention • Is directed towards the early detection and management of problem once a child with a birth defect is born.

REFERENCE • Wong Perry, Hockenberry and Lowdermilk Wilson (2006), Maternal Child Nursing Care, 3 rd edition, Mosby Elsevier Publications. • Emily Wone Mckinney, Sharon Smith Murray, Jean Weiler Ashwill (2009), Maternal Child Nursing, 3 rd edition, Saunders Elsevier Publications. • Susan A. Orshan (2008), Maternity, Newborn and Womens Health Nursing, 1 st edition, Lippincott Williams and Wilkins.
- Slides: 27