Common Injection Techniques In PMR Part II Buttock

Common Injection Techniques In PM&R- Part II
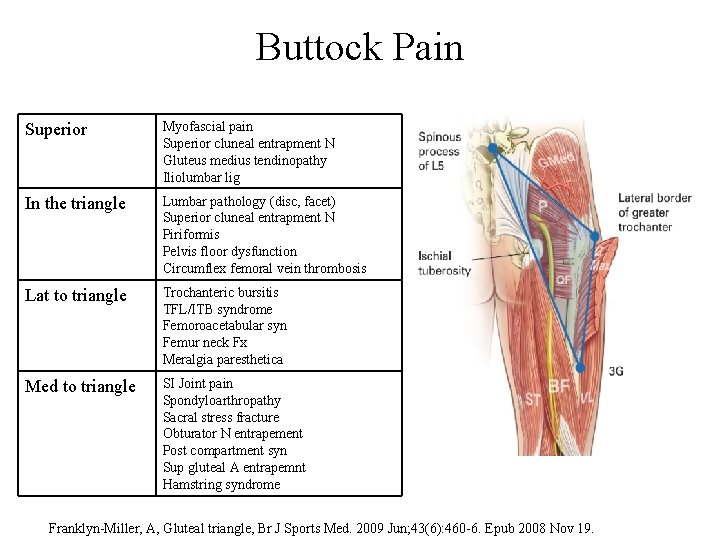
Buttock Pain Superior Myofascial pain Superior cluneal entrapment N Gluteus medius tendinopathy Iliolumbar lig In the triangle Lumbar pathology (disc, facet) Superior cluneal entrapment N Piriformis Pelvis floor dysfunction Circumflex femoral vein thrombosis Lat to triangle Trochanteric bursitis TFL/ITB syndrome Femoroacetabular syn Femur neck Fx Meralgia paresthetica Med to triangle SI Joint pain Spondyloarthropathy Sacral stress fracture Obturator N entrapement Post compartment syn Sup gluteal A entrapemnt Hamstring syndrome Franklyn-Miller, A, Gluteal triangle, Br J Sports Med. 2009 Jun; 43(6): 460 -6. Epub 2008 Nov 19.
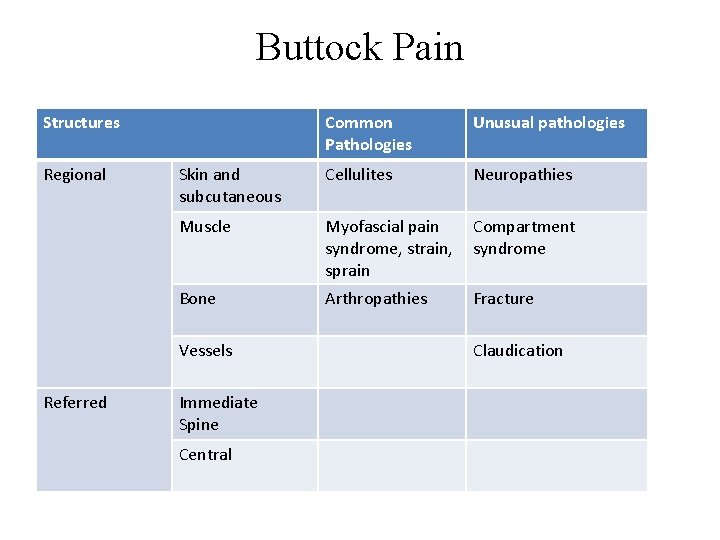
Buttock Pain Structures Regional Common Pathologies Unusual pathologies Skin and subcutaneous Cellulites Neuropathies Muscle Myofascial pain syndrome, strain, sprain Compartment syndrome Bone Arthropathies Fracture Vessels Referred Immediate Spine Central Claudication
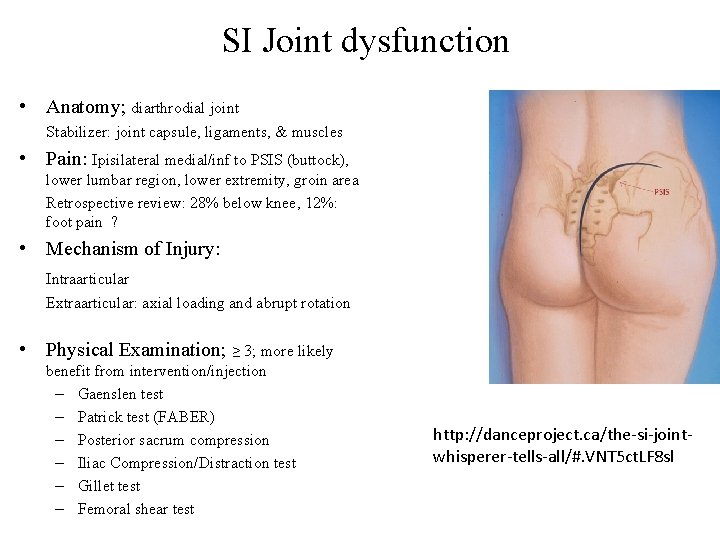
SI Joint dysfunction • Anatomy; diarthrodial joint Stabilizer: joint capsule, ligaments, & muscles • Pain: Ipisilateral medial/inf to PSIS (buttock), lower lumbar region, lower extremity, groin area Retrospective review: 28% below knee, 12%: foot pain ? • Mechanism of Injury: Intraarticular Extraarticular: axial loading and abrupt rotation • Physical Examination; ≥ 3; more likely benefit from intervention/injection – Gaenslen test – Patrick test (FABER) – Posterior sacrum compression – Iliac Compression/Distraction test – Gillet test – Femoral shear test http: //danceproject. ca/the-si-jointwhisperer-tells-all/#. VNT 5 ct. LF 8 sl
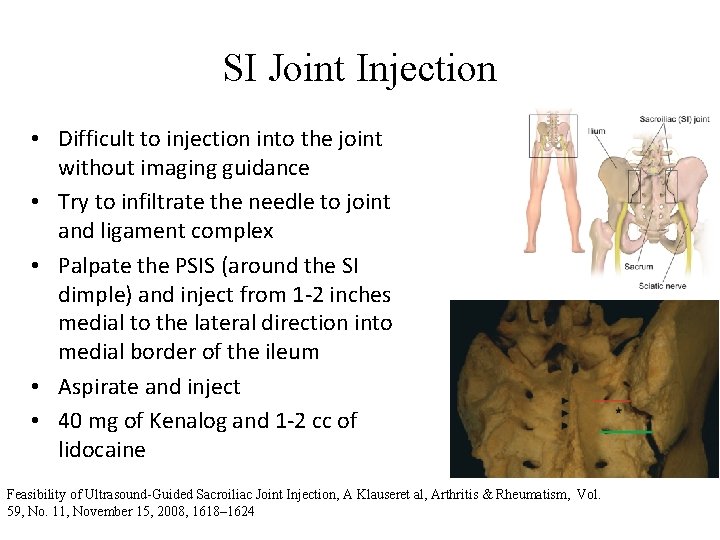
SI Joint Injection • Difficult to injection into the joint without imaging guidance • Try to infiltrate the needle to joint and ligament complex • Palpate the PSIS (around the SI dimple) and inject from 1 -2 inches medial to the lateral direction into medial border of the ileum • Aspirate and inject • 40 mg of Kenalog and 1 -2 cc of lidocaine Feasibility of Ultrasound-Guided Sacroiliac Joint Injection, A Klauseret al, Arthritis & Rheumatism, Vol. 59, No. 11, November 15, 2008, 1618– 1624
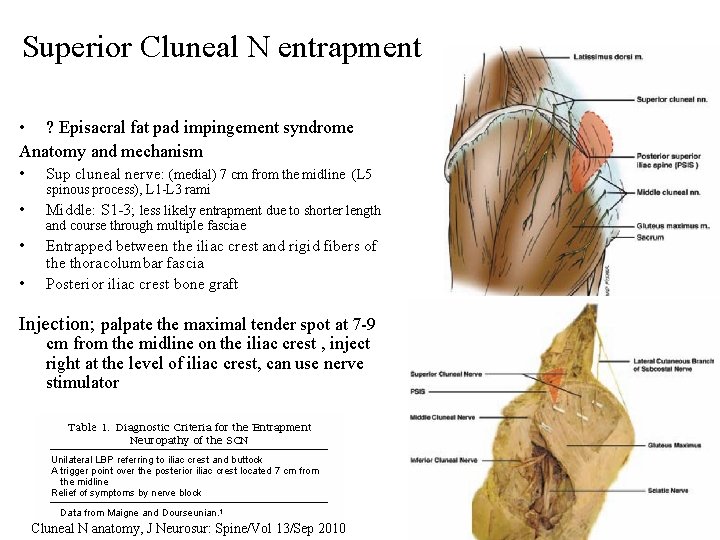
Superior Cluneal N entrapment • ? Episacral fat pad impingement syndrome Anatomy and mechanism • • Sup cluneal nerve: (medial) 7 cm from the midline (L 5 spinous process), L 1 -L 3 rami Middle: S 1 -3; less likely entrapment due to shorter length and course through multiple fasciae Entrapped between the iliac crest and rigid fibers of the thoracolumbar fascia Posterior iliac crest bone graft Injection; palpate the maximal tender spot at 7 -9 cm from the midline on the iliac crest , inject right at the level of iliac crest, can use nerve stimulator Cluneal N anatomy, J Neurosur: Spine/Vol 13/Sep 2010
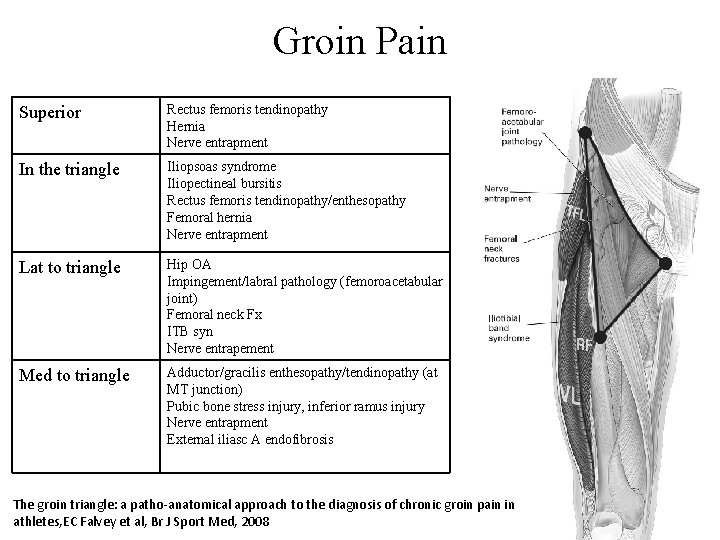
Groin Pain Superior Rectus femoris tendinopathy Hernia Nerve entrapment In the triangle Iliopsoas syndrome Iliopectineal bursitis Rectus femoris tendinopathy/enthesopathy Femoral hernia Nerve entrapment Lat to triangle Hip OA Impingement/labral pathology (femoroacetabular joint) Femoral neck Fx ITB syn Nerve entrapement Med to triangle Adductor/gracilis enthesopathy/tendinopathy (at MT junction) Pubic bone stress injury, inferior ramus injury Nerve entrapment External iliasc A endofibrosis The groin triangle: a patho-anatomical approach to the diagnosis of chronic groin pain in athletes, EC Falvey et al, Br J Sport Med, 2008
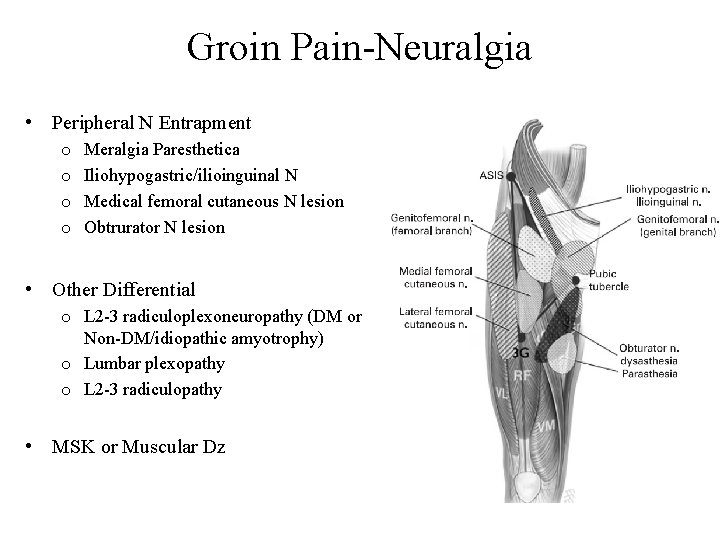
Groin Pain-Neuralgia • Peripheral N Entrapment o o Meralgia Paresthetica Iliohypogastric/ilioinguinal N Medical femoral cutaneous N lesion Obtrurator N lesion • Other Differential o L 2 -3 radiculoplexoneuropathy (DM or Non-DM/idiopathic amyotrophy) o Lumbar plexopathy o L 2 -3 radiculopathy • MSK or Muscular Dz
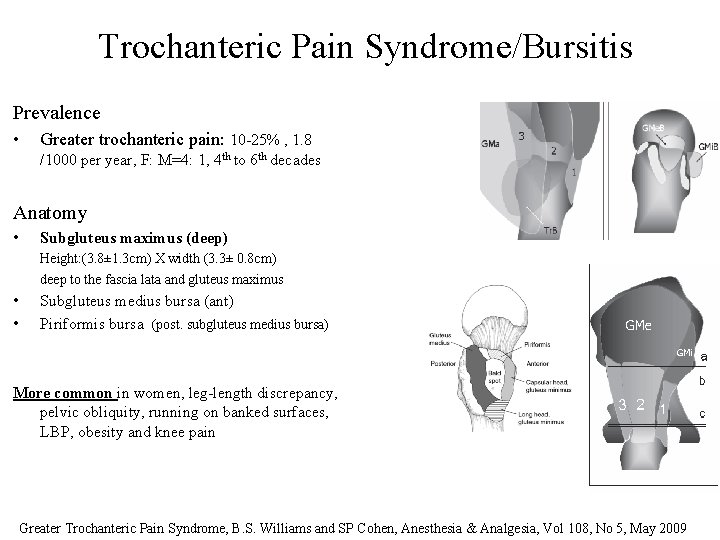
Trochanteric Pain Syndrome/Bursitis Prevalence • Greater trochanteric pain: 10 -25% , 1. 8 /1000 per year, F: M=4: 1, 4 th to 6 th decades Anatomy • Subgluteus maximus (deep) Height: (3. 8± 1. 3 cm) X width (3. 3± 0. 8 cm) deep to the fascia lata and gluteus maximus • • Subgluteus medius bursa (ant) Piriformis bursa (post. subgluteus medius bursa) More common in women, leg-length discrepancy, pelvic obliquity, running on banked surfaces, LBP, obesity and knee pain Greater Trochanteric Pain Syndrome, B. S. Williams and SP Cohen, Anesthesia & Analgesia, Vol 108, No 5, May 2009

Trochanteric Pain Syndrome/Bursitis Symptoms & Examination • • Lateral hip/buttock pain 50% of patient: radiating pain along the lateral aspect of the thigh to the knee Point tenderness (posterolateral to GT) Active resistant to abduction/external rotation Differential • • Gluteus medius tear/ tendinosis LS radiculopathy > Femoral head osteonecrosis, stress fracture ? Sup cluneal/subcostal neuropathy Injection • • Palpate the greater trochanter and inject the 3. 5 inch needle all the way down to the trochanter and withdraw a little to feel the loss of resistance 40 mg of kenalog and 5 cc of 1% lidocaine
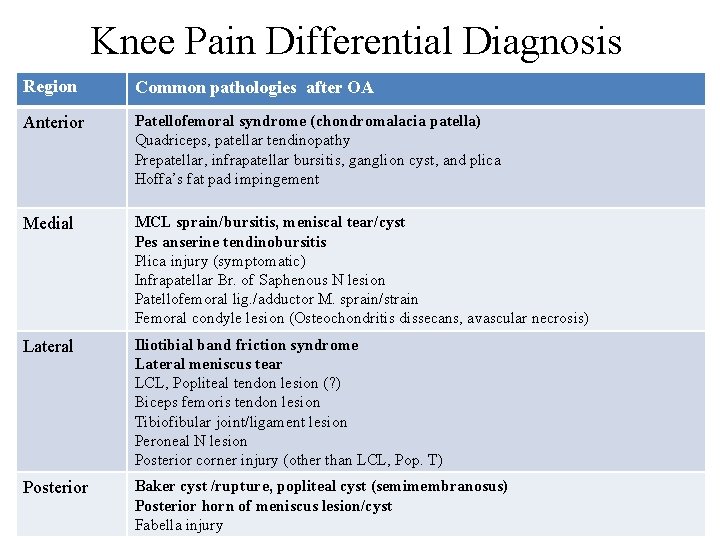
Knee Pain Differential Diagnosis Region Common pathologies after OA Anterior Patellofemoral syndrome (chondromalacia patella) Quadriceps, patellar tendinopathy Prepatellar, infrapatellar bursitis, ganglion cyst, and plica Hoffa’s fat pad impingement Medial MCL sprain/bursitis, meniscal tear/cyst Pes anserine tendinobursitis Plica injury (symptomatic) Infrapatellar Br. of Saphenous N lesion Patellofemoral lig. /adductor M. sprain/strain Femoral condyle lesion (Osteochondritis dissecans, avascular necrosis) Lateral Iliotibial band friction syndrome Lateral meniscus tear LCL, Popliteal tendon lesion (? ) Biceps femoris tendon lesion Tibiofibular joint/ligament lesion Peroneal N lesion Posterior corner injury (other than LCL, Pop. T) Posterior Baker cyst /rupture, popliteal cyst (semimembranosus) Posterior horn of meniscus lesion/cyst Fabella injury http: //www. aium. org/resources/guidelines/musculoskeletal. pdf
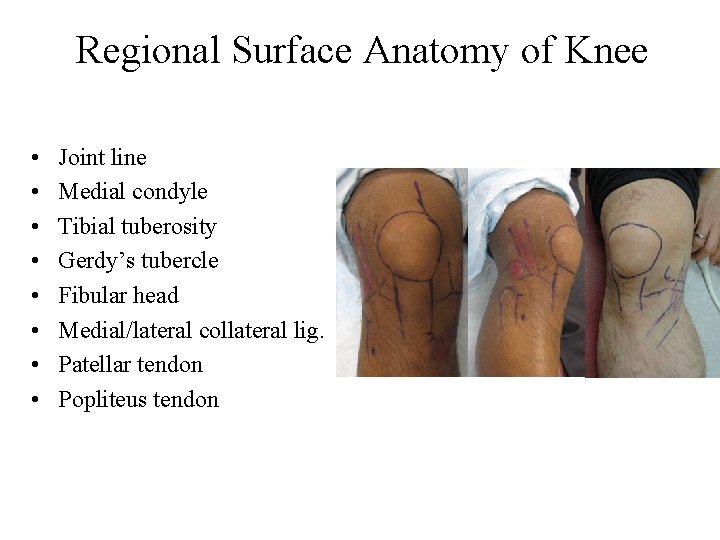
Regional Surface Anatomy of Knee • • Joint line Medial condyle Tibial tuberosity Gerdy’s tubercle Fibular head Medial/lateral collateral lig. Patellar tendon Popliteus tendon

Knee Effusion and Injection • Effusion o Fluid ; normally seen in suprapatellar recess o Medial or lateral parapatellar recess • Knee injection with/without imaging guidance o Aspiration/steroid injection Vs steroid injection o Viscosupplementation o Platelet rich plasma • Adverse Effect of Injection o Infection, hyperglycemia in DM, etc o Less local complication with image guidance (fat tissue atrophy, local depigmentation, tendon rupture, nerve injection etc) o Osteonecrosis; rare Berkoff DJ et al, Clinical utility of ultrasound guidance for intra-articular knee injections: Clinical interventions in aging 2012; 7: 89 -95.
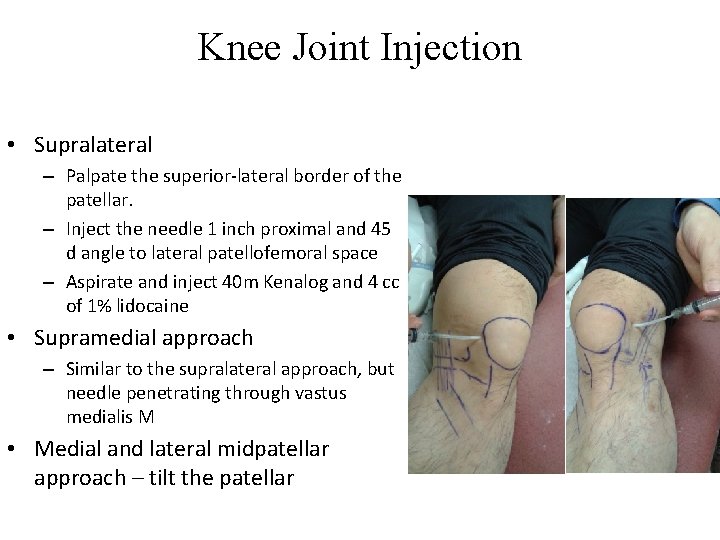
Knee Joint Injection • Supralateral – Palpate the superior-lateral border of the patellar. – Inject the needle 1 inch proximal and 45 d angle to lateral patellofemoral space – Aspirate and inject 40 m Kenalog and 4 cc of 1% lidocaine • Supramedial approach – Similar to the supralateral approach, but needle penetrating through vastus medialis M • Medial and lateral midpatellar approach – tilt the patellar

Knee Osteoarthritis • Most common cause of knee pain • Increase with age • Varus deformity/valgus deformity with monocompartmental OA • X ray is less sensitive and specific than physical examination • Steroid injection: level II, for short term effect • Orthotics; unloader, heel wedge/insole Grade 0 1 2 3 Suri P, Morgenroth DC, Hunter DJ. Epidemiology of osteoarthritis and associated comorbidities. PM&R. 2012; 4: S 10 -S 19 4 5 The Kellgren and Lawrence Normal Doubtful narrowing of joint space and possible osteophytic lipping Definite osteophytes and possible narrowing of joint space Moderate multiple osteophytes, definite narrowing of joint space and some sclerosis and possible deformity of bone ends Large osteophytes, marked narrowing of joint space, severe sclerosis, and definite deformity of bone ends Ahlback joint space narrowing (less than 3 mm) joint space obliteration minor bone attrition (0 -5 mm) moderate bone attrition (5 -10 mm) severe bone attrition (more than 10 mm)

Pseudogout • • Common in elderly Intra or periarticular deposition of calcium pyrophosphate crystals. Acute-subacute pain with swelling/effusion, no preceding injury or trauma Knee (most common), hip (symphysis pubis), wrist (TFCC), GH joint, elbow, and ankle o Hyaline and meniscal cartilage • Role of US o Valid imaging technique for CPPD o More sensitive than plain radiograph • Intraarticular joint injection with 40 mg Kenalog and 5 cc of 1% lidocaine "Crystal clear"-sonographic assessment of gout and calcium pyrophosphate deposition disease. , Grassi W et al, Semin Arthritis Rheum. 2006 Dec; 36(3): 197 -202. 2006 Sep 29
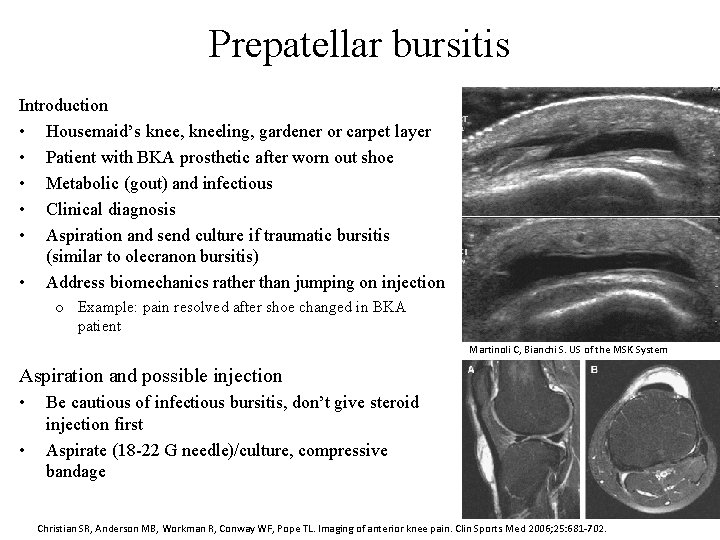
Prepatellar bursitis Introduction • Housemaid’s knee, kneeling, gardener or carpet layer • Patient with BKA prosthetic after worn out shoe • Metabolic (gout) and infectious • Clinical diagnosis • Aspiration and send culture if traumatic bursitis (similar to olecranon bursitis) • Address biomechanics rather than jumping on injection o Example: pain resolved after shoe changed in BKA patient Martinoli C, Bianchi S. US of the MSK System Aspiration and possible injection • • Be cautious of infectious bursitis, don’t give steroid injection first Aspirate (18 -22 G needle)/culture, compressive bandage Christian SR, Anderson MB, Workman R, Conway WF, Pope TL. Imaging of anterior knee pain. Clin Sports Med 2006; 25: 681 -702.
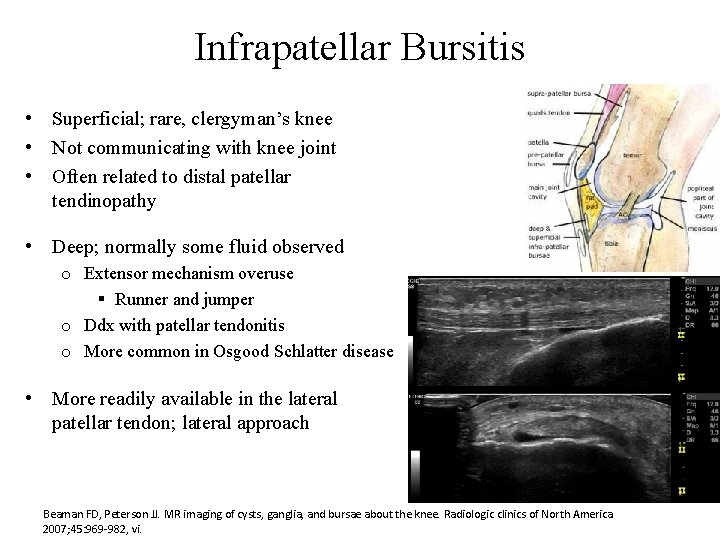
Infrapatellar Bursitis • Superficial; rare, clergyman’s knee • Not communicating with knee joint • Often related to distal patellar tendinopathy • Deep; normally some fluid observed o Extensor mechanism overuse § Runner and jumper o Ddx with patellar tendonitis o More common in Osgood Schlatter disease • More readily available in the lateral patellar tendon; lateral approach Beaman FD, Peterson JJ. MR imaging of cysts, ganglia, and bursae about the knee. Radiologic clinics of North America 2007; 45: 969 -982, vi.
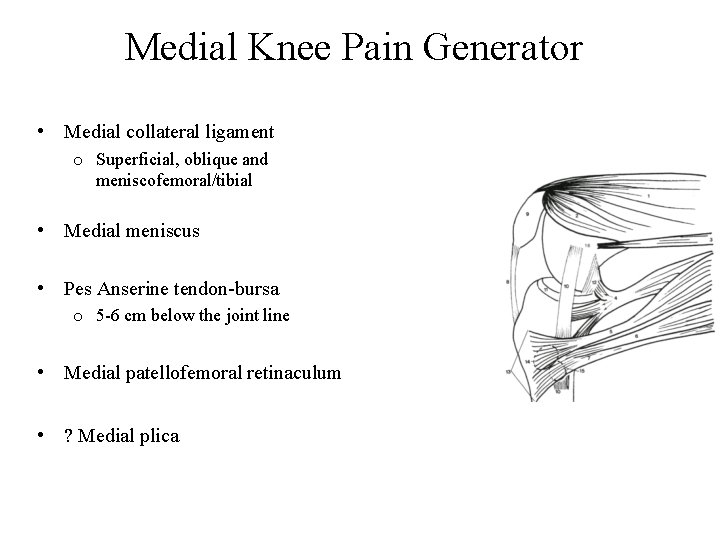
Medial Knee Pain Generator • Medial collateral ligament o Superficial, oblique and meniscofemoral/tibial • Medial meniscus • Pes Anserine tendon-bursa o 5 -6 cm below the joint line • Medial patellofemoral retinaculum • ? Medial plica

Pes Anserine Tendinobursitis • Pes (foot) Anserinus (goose) o Knee flexor and secondary internal rotation of tibia o Against rotatory and valgus stress • Presentation o o Fluid filled anserine bursa: Ususual More common in RA or type II DM Medial/Posteromedial knee pain Tenderness below the joint line • DDx o Osteoarthritis, often coexisting o Medial meniscal injury/cyst (posterior horn) or MCL injury/bursitis, juxtaarticular bone cysts, semimembranosus bursitis • Injection o 5 -7 cm below the joint line and needle into the periosteum and withdraw it as loss of resistance Pes Anserine bursitis: incidence in symptomatic knees and clinical presentation, Skeletal Radiol (2005) 34: 395– 398
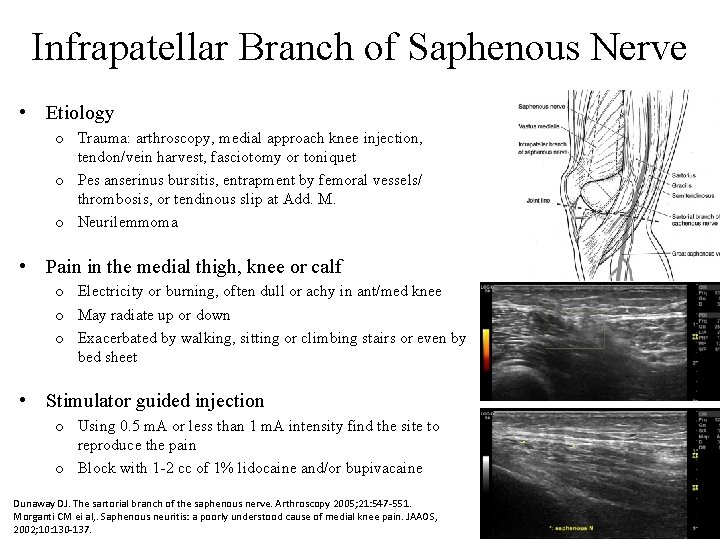
Infrapatellar Branch of Saphenous Nerve • Etiology o Trauma: arthroscopy, medial approach knee injection, tendon/vein harvest, fasciotomy or toniquet o Pes anserinus bursitis, entrapment by femoral vessels/ thrombosis, or tendinous slip at Add. M. o Neurilemmoma • Pain in the medial thigh, knee or calf o Electricity or burning, often dull or achy in ant/med knee o May radiate up or down o Exacerbated by walking, sitting or climbing stairs or even by bed sheet • Stimulator guided injection o Using 0. 5 m. A or less than 1 m. A intensity find the site to reproduce the pain o Block with 1 -2 cc of 1% lidocaine and/or bupivacaine Dunaway DJ. The sartorial branch of the saphenous nerve. Arthroscopy 2005; 21: 547 -551. Morganti CM ei al, . Saphenous neuritis: a poorly understood cause of medial knee pain. JAAOS, 2002; 10: 130 -137.
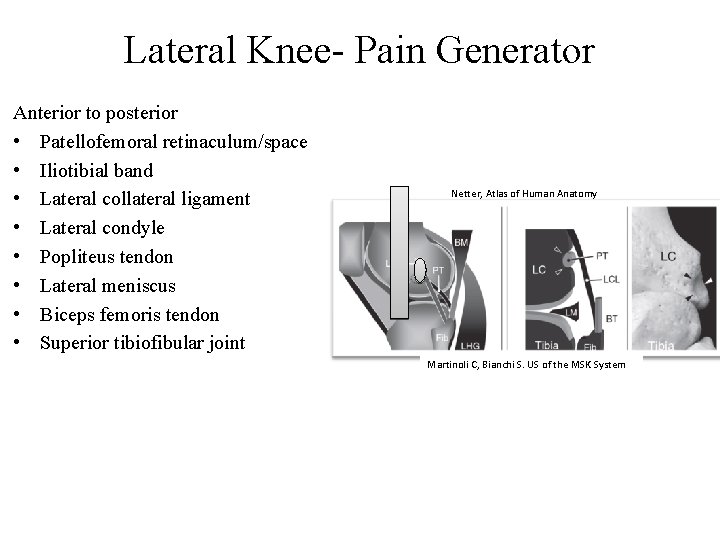
Lateral Knee- Pain Generator Anterior to posterior • Patellofemoral retinaculum/space • Iliotibial band • Lateral collateral ligament • Lateral condyle • Popliteus tendon • Lateral meniscus • Biceps femoris tendon • Superior tibiofibular joint Netter, Atlas of Human Anatomy Martinoli C, Bianchi S. US of the MSK System
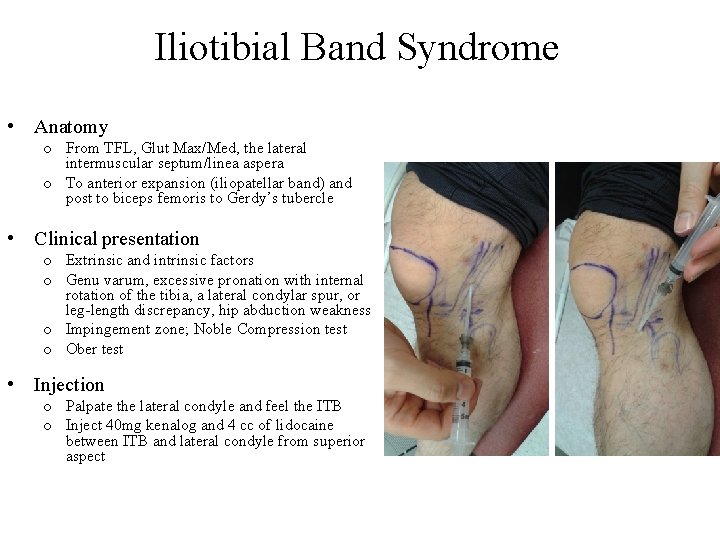
Iliotibial Band Syndrome • Anatomy o From TFL, Glut Max/Med, the lateral intermuscular septum/linea aspera o To anterior expansion (iliopatellar band) and post to biceps femoris to Gerdy’s tubercle • Clinical presentation o Extrinsic and intrinsic factors o Genu varum, excessive pronation with internal rotation of the tibia, a lateral condylar spur, or leg-length discrepancy, hip abduction weakness o Impingement zone; Noble Compression test o Ober test • Injection o Palpate the lateral condyle and feel the ITB o Inject 40 mg kenalog and 4 cc of lidocaine between ITB and lateral condyle from superior aspect
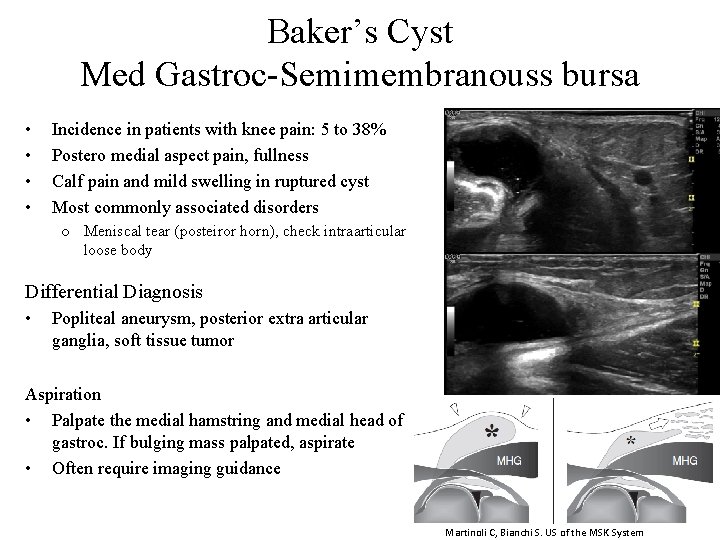
Baker’s Cyst Med Gastroc-Semimembranouss bursa • • Incidence in patients with knee pain: 5 to 38% Postero medial aspect pain, fullness Calf pain and mild swelling in ruptured cyst Most commonly associated disorders o Meniscal tear (posteiror horn), check intraarticular loose body Differential Diagnosis • Popliteal aneurysm, posterior extra articular ganglia, soft tissue tumor Aspiration • Palpate the medial hamstring and medial head of gastroc. If bulging mass palpated, aspirate • Often require imaging guidance Martinoli C, Bianchi S. US of the MSK System
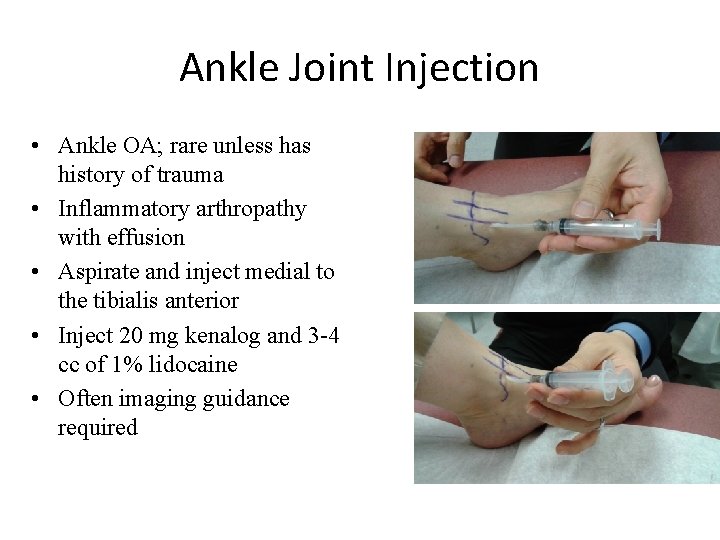
Ankle Joint Injection • Ankle OA; rare unless has history of trauma • Inflammatory arthropathy with effusion • Aspirate and inject medial to the tibialis anterior • Inject 20 mg kenalog and 3 -4 cc of 1% lidocaine • Often imaging guidance required

Musculoskeletal Ultrasonography in PMR • Advantages o Availability (Bed side) o Correlating with the clinical examination o Dynamic view o No radiation o Cost: ? • Disadvantages o Operator dependent, steep learning curve o Limitation Ø Intraarticular structures Ø Beyond the bone Ø Body habitus/deep structure • Therapeutic o Ultrasound guided injection to the peripheral joint, surround structures and nerves o Other applications Ø Education • Diagnostic o Musculoskeletal conditions o Peripheral Neuromuscular conditions
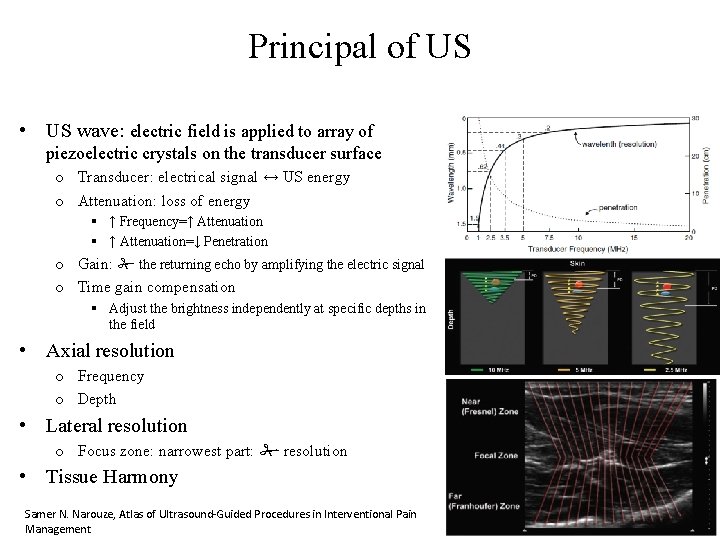
Principal of US • US wave: electric field is applied to array of piezoelectric crystals on the transducer surface o Transducer: electrical signal ↔ US energy o Attenuation: loss of energy § ↑ Frequency=↑ Attenuation § ↑ Attenuation=↓ Penetration o Gain: the returning echo by amplifying the electric signal o Time gain compensation § Adjust the brightness independently at specific depths in the field • Axial resolution o Frequency o Depth • Lateral resolution o Focus zone: narrowest part: resolution • Tissue Harmony Samer N. Narouze, Atlas of Ultrasound-Guided Procedures in Interventional Pain Management
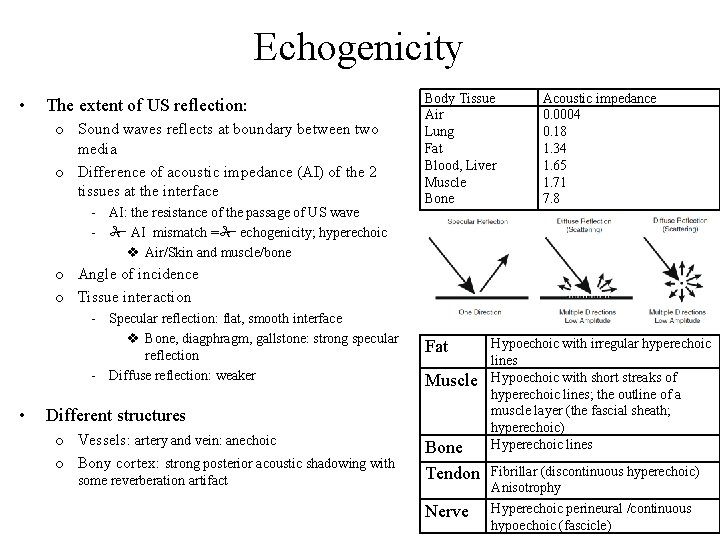

Echogenicity • The extent of US reflection: o Sound waves reflects at boundary between two media o Difference of acoustic impedance (AI) of the 2 tissues at the interface - AI: the resistance of the passage of US wave - AI mismatch = echogenicity; hyperechoic v Air/Skin and muscle/bone Body Tissue Air Lung Fat Blood, Liver Muscle Bone Acoustic impedance 0. 0004 0. 18 1. 34 1. 65 1. 71 7. 8 o Angle of incidence o Tissue interaction - Specular reflection: flat, smooth interface v Bone, diagphragm, gallstone: strong specular reflection - Diffuse reflection: weaker • Fat Muscle Different structures o Vessels: artery and vein: anechoic o Bony cortex: strong posterior acoustic shadowing with some reverberation artifact Bone Tendon Nerve Hypoechoic with irregular hyperechoic lines Hypoechoic with short streaks of hyperechoic lines; the outline of a muscle layer (the fascial sheath; hyperechoic) Hyperechoic lines Fibrillar (discontinuous hyperechoic) Anisotrophy Hyperechoic perineural /continuous hypoechoic (fascicle)

Sonographic Artifacts • Anisotrophy o When this variation in ultrasound interaction with the fibrillar tissues, oblique course • Shadowing o US beam is reflected, absorbed, or refracted: bone or calcium, foreign body and gas • Posterior acoustic enhancement o US beam less attenuated compared to the adjacent tissues; fluid & PPN sheath tumors o Hyperechoic compared to the adjacent structures • Posterior reveberation o When the surface of a surface is smooth and flat; bone or a metal foreign object o The sound beam reflects back and forth between the smooth surface and the transducer A series of linear reflective echoes extending deep to the structure • Beam width artifact o US beam too wide compared with the object being imaged Basic Appearance of Ultrasound Structures and Pitfalls, S Mc. Donald et al, Phys Med Rehabil Clin N Am (2010) 461– 79
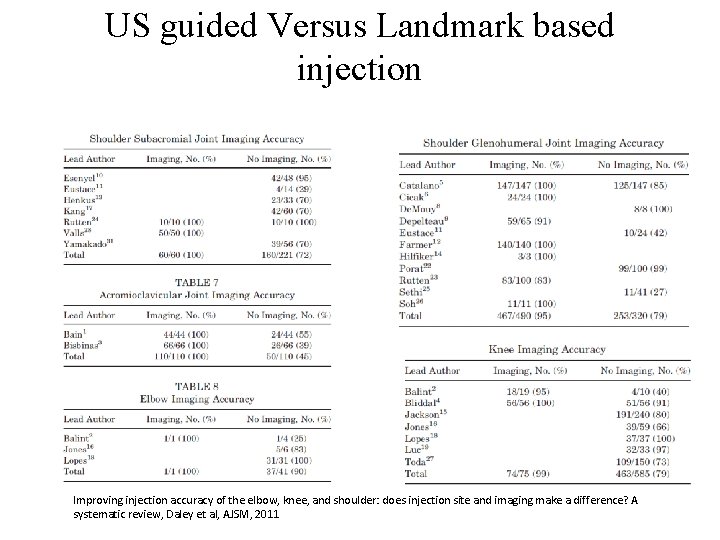
US guided Versus Landmark based injection Improving injection accuracy of the elbow, knee, and shoulder: does injection site and imaging make a difference? A systematic review, Daley et al, AJSM, 2011

Ultrasound In EMG Laboratory • Complementary Role o Real time anatomic/structural evaluation § CTS &Ulnar neuropathy at elbow § Fibular N and tibial N § Evaluation of etiological causes o Assisting diagnosis § Atypical finding § When it is not able to localize § Needle localization o Concomitant musculoskeletal causes § MSK Mimicker o Injection Zaidman CM, Seelig MJ, Baker JC, Mackinnon SE, Pestronk A. Detection of peripheral nerve pathology: comparison of ultrasound and MRI. Neurology 2013; 80: 1634 -1640.
Limitation of Ultrasound • ? Adding time and expense • Operator dependent g. Regulating/credentialing the operator g. Protocol based • Limited penetration – Deeper structure and obese patient g ? Patient selection and limit indications • Varying image resolution depending on the machine and transducer – Better hardware

Limitation of US Application in EMG • Quantification o Chronic compressed nerve • Change in size (enlarged) and hypoechoic – Severe CTS; CSA increased – ? Inverted U shape relationship between the nerve enlargement/ echogenicity and severity of compressive neuropathy • Nerve trunk versus branches • Echogenicity Characteristics of surrogate markers 1. Validity (technical/clinical) 2. Responsiveness to disease and treatment 3. Measurement precision a. Biological variation b. Acquisition process 4. Convenience; speed of use, portability, patient tolerance 5. Cost o Varying from instrument and software o Human visual perception/coded cognitively in exponential manner Mayans, D. , Cartwright, M. S. and Walker, F. O. , Neuromuscular ultrasonography: quantifying muscle and nerve measurements, Phys Med Rehabil Clin N Am, Vol 23, Issue 1 Kasius, K. M. , Claes, F. , Verhagen, W. I. and Meulstee, J. , Ultrasonography in severe carpal tunnel syndrome, Muscle Nerve, 2012, Vol 45, Issue 3
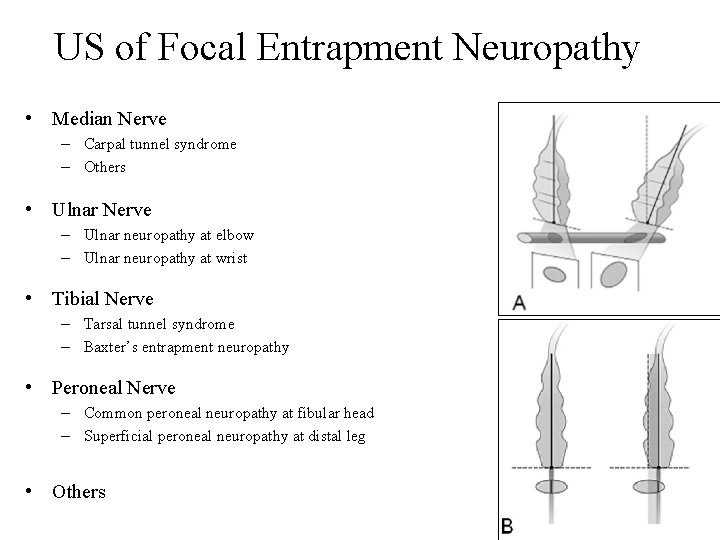
US of Focal Entrapment Neuropathy • Median Nerve – Carpal tunnel syndrome – Others • Ulnar Nerve – Ulnar neuropathy at elbow – Ulnar neuropathy at wrist • Tibial Nerve – Tarsal tunnel syndrome – Baxter’s entrapment neuropathy • Peroneal Nerve – Common peroneal neuropathy at fibular head – Superficial peroneal neuropathy at distal leg • Others

US in Peripheral Polyneuropathy • Concept similar to EMG approach • MRI and Ultrasound – Imaging modality of choice for peripheral nerve – Nerve lesion in difficult to evaluate by EMG – Characterize soft tissue structure – Differentiate tumor • Size criteria – Demyelinating neurompathy more enlargement than axonal. – Polysegmental enalargement • Morphological correlates of nerve conduction block in CIDP – CMT type 1 A; greatly increased nerve cross sectional area • US of Muscle – Pattern of muscles involvement – The earliest US abnormalities: 10 -14 days Zaidman CM, Seelig MJ, Baker JC, Mackinnon SE, Pestronk A. Detection of peripheral nerve pathology: comparison of ultrasound and MRI. Neurology 2013; 80: 1634 -1640.
- Slides: 35