Common Infectious Diseases in Child Care Presented by

Common Infectious Diseases in Child Care Presented by: Sharon Auclerc, RN Gateway District Health Department

Class Objectives � What child care providers should know about common infectious diseases � Identify ways illnesses are spread within a child care center � Learn to practice standard precautions � Identify reportable diseases

Respiratory Syncytial Virus (RSV) Infection � RSV is a common respiratory illness that affects persons of any age � Most common cause of bronchiolitis and pneumonia in infants and children under age of 2 � Spreads quickly and more so in the winter months

RSV Symptoms � Similar to mild cold with low-grade fever, cough, watery eyes, runny nose, nasal stuffiness, and sneezing � Severe form will include wheezing

RSV Symptoms in Infants � In cases where infants are a few weeks old, the symptoms may be more severe than in older children � Premature infants and infants born with heart, lung, or immune system problems are at higher risk for RSV � Infants may show tiredness, irritability, and loss of appetite � Episodes of apnea (breathing stops) may occur as well

RSV How it Spreads � Close contact with droplets containing RSV that are expelled from the nose and mouth � Touching of the secretions from the nose and mouth � Touching hands, tissues, or other items soiled with the secretions and then touching your nose, mouth, or eyes

RSV Incubation/Contagious Period Ø It takes 2 to 8 days, but usually 4 to 6 days, from the time a person is exposed until symptoms start Ø The virus is usually found in the respiratory secretions for 3 -8 days, although some infants can spread RSV for as long as 3 to 4 weeks

RSV Temporary Exclusion � Child should be excluded from child care until *fever with behavior change is resolved and child is well enough to participate in routine activities * Without fever reducing medication

RSV Treatment � If child has symptoms of RSV, the parents should be encouraged to consult child’s health care provider for diagnosis and treatment. There is a lab test that will confirm RSV � Symptomatic treatment � Hospitalization may be required � RSV is a viral illness and antibiotics will not be effective � Never give aspirin or salicylate-containing medication to children under 18 years of age because of the potential risk for Reye’s Syndrome

RSV Prevention/Control � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and teach children to do this � Dispose of tissue after one use � WASHING YOUR HANDS with soap and warm running water is the best way to prevent the spread of communicable diseases � Do not share cups, glasses, or eating utensils � https: //www. youtube. com/watch? v=feg. Zz. YZgk. U

RSV Prevention/Control continued � Clean and disinfect commonly touched surfaces (door knobs, refrigerator handles, water faucets, cupboard handles) at least daily � Clean and sanitize mouthed toys, objects, and surfaces at least once daily and when soiled

Croup � Croup refers to several fairly common respiratory illnesses that affect young children � Usually children ages 3 months thru 3 years � Most illnesses occurring during the second year of life � Croup occurs year-round depending on the virus causing the illness

Croup Causes � Many different viruses but most commonly the Parainfluenza virus Type 1 � Since many different viruses can cause the illness, a child could have the croup more than once

Croup Symptoms � Runny nose, sore throat, mild cough, and fever � Hoarseness and deepening non-productive cough � Rapid breathing, sitting forward in bed to cough, or making a noise when taking a breath may also occur � Symptoms worsen at night � Illness last 3 -4 days but may have cough longer. (hospitalization may occur if severe symptoms)

Croup How it Spreads � Touching secretions from the nose or mouth of the infected person and/or touching hands, tissues, or other items soiled with the secretions and then touching your eyes, nose, or mouth

Croup Incubation/Contagious Period � Could take up to 10 days after exposure for early symptoms to develop and days later for the cough to occur � Child is contagious just before the symptoms begin and for as long as the acute symptoms last � https: //www. youtube. com/watch? v=s 7 qomu X 0 Gjw

Croup Temporary Exclusion � Until fever with behavior change is gone and child is well enough to participate in routine activities

Croup Treatment � Croup is a viral illness and antibiotics will not be effective � Never give aspirin or salicylate-containing medication to children under 18 years of age

Croup Prevention/Control � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and dispose of tissues after one use � WASH YOUR HANDS with soap and warm running water � Clean and disinfect commonly touched surfaces at least daily � Clean and sanitize mouthed toys, objects, and surfaces at least once daily and when soiled

Conjunctivitis (Pinkeye) � Redness and inflammation of the membrane (conjunctiva) that covers the eye and lines the inner surface of the eyelid � Common infection in young children

Conjunctivitis Causes � Bacteria � Viruses � Allergies � Eye injuries � Chemicals

Conjunctivitis Symptoms � Redness and itching of the eye � Pain and discharge (depending on the cause) � Non-purulent conjunctivitis is redness of eyes with a clear, watery eye discharge but without fever, eye pain or eyelid redness � Purulent conjunctivitis is redness of eyes or eyelids with thick white or yellow eye discharge and eye pain

Conjunctivitis How it Spreads � Touching the secretions from the eyes, nose, or mouth of infected persons

Conjunctivitis Incubation/Contagious Period � 1 to 12 days after exposure for symptoms to begin (usually 1 to 3 days) � The person remains contagious till symptoms are no longer present

Conjunctivitis Temporary Exclusion Do not exclude from child care unless; � The child is not well enough to participate in routine activities � The child meets other exclusion criteria such as fever with behavior change � There is a recommendation of the health department or the child’s health care provider

Conjunctivitis Prevention/Control � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and dispose of tissues after one use � Encourage child not to rub eyes � Keep child’s eyes wiped free of discharge � WASH YOUR HANDS with soap and warm running water after contact with eye drainage � Wear gloves when administering eye medication and then wash your hands � Clean and sanitize mouthed toys, objects, and surfaces at least daily

Conjunctivitis Diagnosis/Treatment � Notify child’s parent/guardian to consult with child’s health care provider for diagnosis and possible treatment � If prescribed, may treat with antibiotics (ointment or drops) � Antibiotics are not required to return to child care. Most children get better after 5 -6 days without treatment

Fifth Disease (Human Parvovirus B 19) � Mild common illness caused by a virus � Immunity increases with age; 50 -80% of adults are immune � Outbreaks happen frequently in schools and child care centers

Fifth Disease Symptoms � Rash � Possible low-grade fever � Possible sore throat � “Slapped cheek” appearance � After rash starts on cheeks, it will move to arms, upper body, buttocks, and legs � Very fine lacy pink rash � Usually fades within four days on face � Rash on body takes 3 to 7 days to fade

Fifth Disease Symptoms continued � Rash may come and go for days or even weeks when the person is exposed to sunlight or heat � Adults (especially women) may have pain, redness and swelling of the joints � Joint pain and swelling may last 1 -3 months � Children that have a weakened immune system may become very ill and require medical care
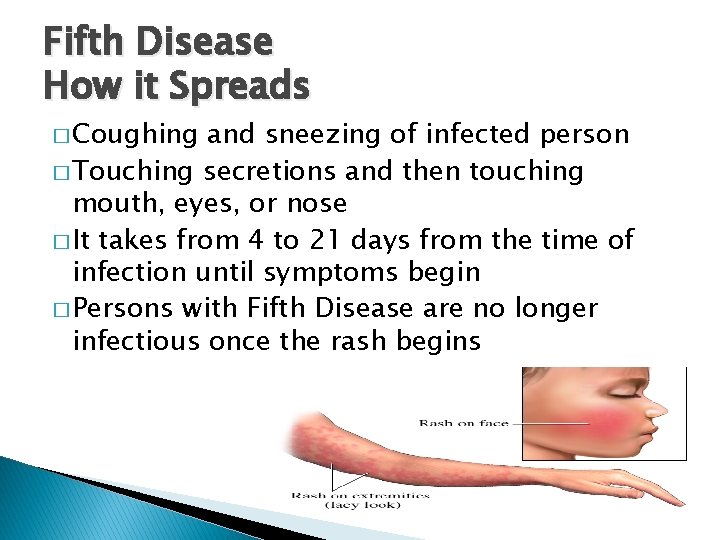
Fifth Disease How it Spreads � Coughing and sneezing of infected person � Touching secretions and then touching mouth, eyes, or nose � It takes from 4 to 21 days from the time of infection until symptoms begin � Persons with Fifth Disease are no longer infectious once the rash begins

Fifth Disease Diagnosis � Lab test can confirm

Fifth Disease Treatment � No treatment is needed

Fifth Disease Prevention and Control � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and dispose of tissues after one use � WASH YOUR HANDS with soap and warm running water � Clean and disinfect commonly touched surfaces at least daily � Those who are pregnant, have a weakened immune system, have sickle cell anemia, or other blood disorders should notify their health care provider if exposed

Hand, Foot, and Mouth Disease � Viral Infection � Blister-like rash involving hands, feet and mouth � Occurs mostly in children less than 10 years old � Mostly in summer and fall months. � Outbreaks may occur especially in schools and child care centers
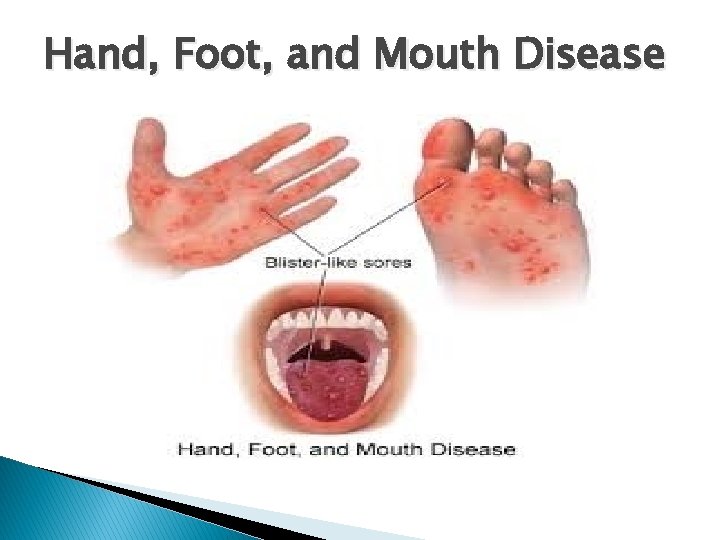
Hand, Foot, and Mouth Disease
Hand, Foot, and Mouth Disease Cause � Coxsackievirus most often A 16

Hand, Foot, and Mouth Disease Symptoms � Low-grade fever for 1 -2 days � Runny nose � Possible sore throat � Blister-like rash in mouth, on the sides of the tongue, inside the cheeks, and the gums, may last 7 to 10 days � Rash will occur on palms and fingers of the hands and soles of the feet � Usually self-limited but in rare cases can be fatal to infants

Hand, Foot, and Mouth Disease How it Spreads � Virus leaves the body through the stool of infected person and enters another person when hands, food, or objects (toys) contaminated with stool are placed in the mouth (fecal-oral route) � Spread through droplets (airborne route) during sneezing and coughing � (Direct contact route) and respiratory secretions
Hand, Foot, and Mouth Disease Incubation/Contagious Period � It usually takes 3 -6 days after exposure for symptoms to begin � Contagious during first week of illness and possibly for several weeks after illness � Virus may be shed for several weeks in stool � Even if they do not seems sick, they may still be carrying the virus
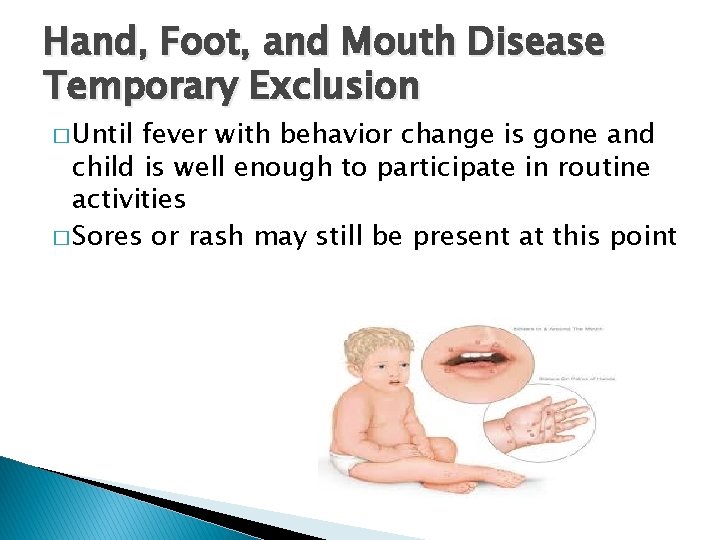
Hand, Foot, and Mouth Disease Temporary Exclusion � Until fever with behavior change is gone and child is well enough to participate in routine activities � Sores or rash may still be present at this point

Hand, Foot, and Mouth Disease Treatment � No specific treatment is needed

Hand, Foot, and Mouth Disease Prevention/Control � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and dispose of tissues after one use � WASH YOUR HANDS with soap and warm running water; after using toilet; changing diapers; or handling anything soiled with stool, secretions from the mouth or nose, fluid from blisters; before preparing or eating food � Monitor children’s hand washing after they use the toilet or have been diapered
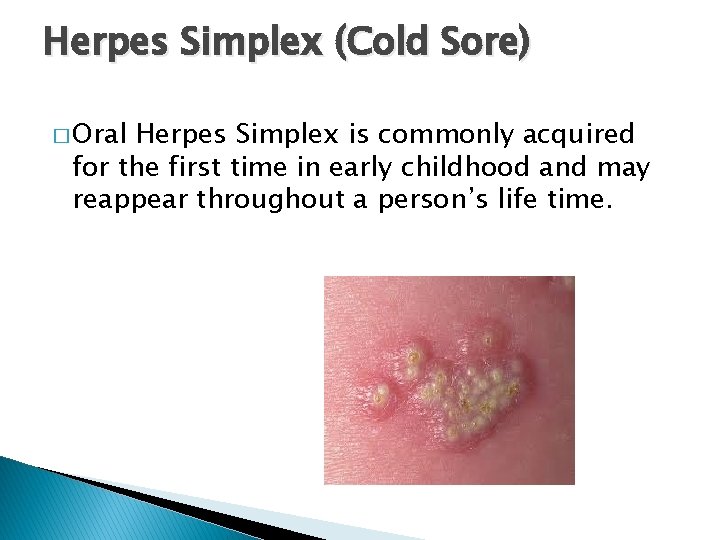
Herpes Simplex (Cold Sore) � Oral Herpes Simplex is commonly acquired for the first time in early childhood and may reappear throughout a person’s life time.
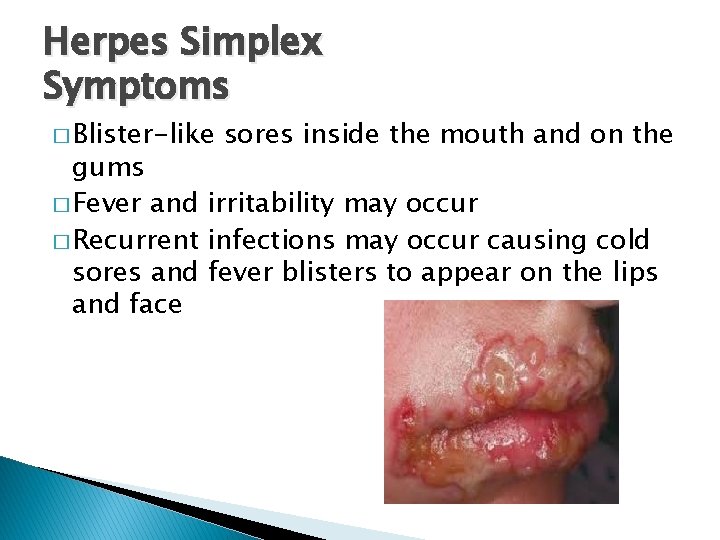
Herpes Simplex Symptoms � Blister-like sores inside the mouth and on the gums � Fever and irritability may occur � Recurrent infections may occur causing cold sores and fever blisters to appear on the lips and face

Herpes Simplex Symptoms continued � Some children may have the virus in their bodies but do not develop symptoms � Herpes simplex virus can also cause infections of the eye, fingers, and central nervous system

Herpes Simplex How it Spreads � Person-to-person contact � Through direct contact with saliva (kissing) � Touching the fluid from the blisters or sores � Personal items should not be shared!

Herpes Simplex Incubation/Contagious Period � Takes 2 to 14 days from time a person is exposed to develop symptoms � It is contagious up to 2 weeks and occasionally up to 7 weeks � Recurrent infection usually in 3 to 5 days

Herpes Simplex Temporary Exclusion � For a Primary Infection, exclude children in child care who do not have control over their saliva (drooling) until mouth sores are gone � For a Recurrent Infection, (fever blisters and cold sores) do not exclude

Herpes Simplex Treatment/Prevention � Topical medication may be prescribed � Encourage children not to touch the sores � WASH YOUR HANDS! � Wear gloves when touching the sores � Do not kiss and infected person on or near the mouth when sores are present � Clean and sanitize mouthed toys, objects, and disinfect surfaces at least daily and when soiled
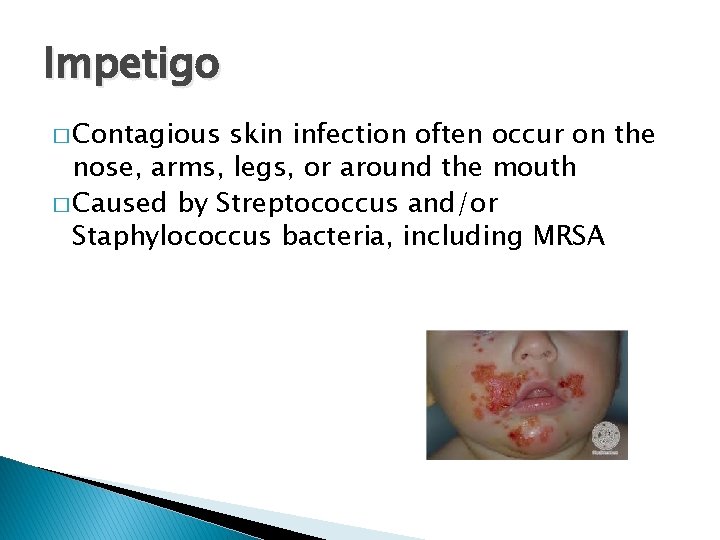
Impetigo � Contagious skin infection often occur on the nose, arms, legs, or around the mouth � Caused by Streptococcus and/or Staphylococcus bacteria, including MRSA

Impetigo Symptoms � Break in the skin (insect bite, cut etc. ) � Sores form on the skin and may develop and produce a thick, golden- yellow discharge that dries, crusts, and sticks to the skin � Rarely problems such as kidney disease or cellulitis (skin infection) may develop if not properly treated

Impetigo How it spreads � Person-to-person through touching the fluid from the sores � Rarely through touching contaminated objects

Impetigo Incubation/Contamination Period � Usually takes 1 to 10 days from the time of exposure until symptoms begin � Contagious until the sores are healed or until treated with antibiotics for 24 hours

Impetigo Diagnosis/Treatment � Recommend to parent/guardian that child see their health care provider if they have open sores or an undiagnosed rash � Usually treated with topical antibiotics (applied directly to the site of sore) � Oral or injectable antibiotics may also be prescribed for more severe cases

Impetigo Prevention/Control � WASH YOUR HANDS with soap and warm running water after each contact with sores � Wear gloves if applying ointment to site. � Cover sores whenever possible to prevent spread � Discourage child from scratching infected areas � Do not share towels, washcloths, or clothing � Clean, sanitize, and disinfect surfaces

Methicillin-Resistant Staphylococcus Aureus (MRSA) � Staph is a common bacteria found in the nose and on the skin of healthy people � When bacteria are resistant to an antibiotic, it means that antibiotic will not kill the bacteria � MRSA was first identified in health care facilities � Now MRSA is found among young healthy people in the community, this is called community-acquired MRSA

MRSA Symptoms � Usually skin infections that typically cause local redness and warmth of the infected area with or without pus/drainage � Commonly in sites of visible skin trauma (cuts, abrasions etc. ) � Also in areas such as boils, impetigo, cellulitis, and wound infections � May cause more serious infections, such as pneumonia, bloodstream infections, or bone infections

MRSA How it Spreads � Contact with hands, skin drainage, pus, or secretions from the nose of a person who is infected or colonized with MRSA � Contagious as long as colonization's lasts � Person with draining infections are shedding more bacteria and are more infectious

MRSA Temporary Exclusion � If draining sores are present and cannot be completely covered and contained with a clean, dry bandage � If the person cannot maintain good personal hygiene � If sores are draining, children should not participate in activities or contact sports where skin-to-skin contact is likely to occur until the sores are healed

MRSA Treatment � See health care provider for diagnosis and treatment � Many infections can be treated with the drainage of pus � Antibiotics may be needed � More serious infections may require hospitalization and IV antibiotics

MRSA Prevention/Control � WASH YOUR HANDS with soap and warm running water � Wear gloves when touching any draining sores or changing bandages � Dispose of bandages in a plastic bag immediately to prevent contamination of surfaces

MRSA Prevention/Control continued � Keep wounds clean and dry and covered with bandages, making sure all four corners of bandage are secure � Do not share personal items � Wash bedding separately from other laundry in hot water with detergent. Dry in hot dryer � Food handlers with open sores should wear waterproof disposable gloves
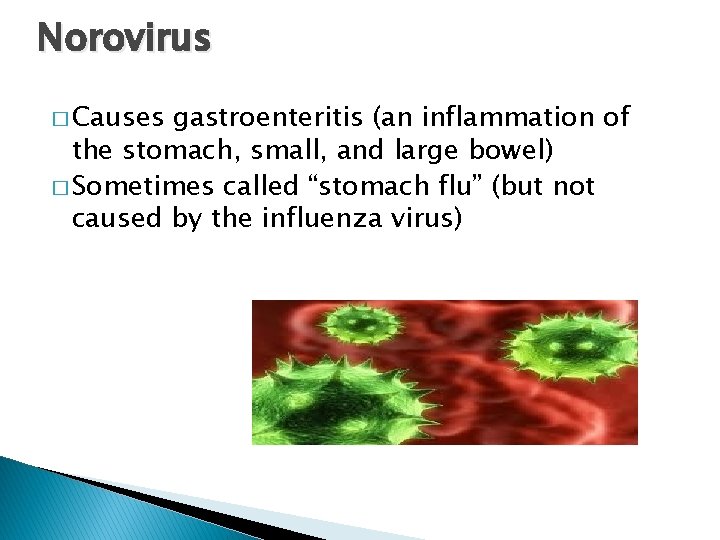
Norovirus � Causes gastroenteritis (an inflammation of the stomach, small, and large bowel) � Sometimes called “stomach flu” (but not caused by the influenza virus)

Norovirus Cause � Norwalk virus or Norwalk-like-virus

Norovirus Symptoms � Watery diarrhea and vomiting � Fever, headache, and muscle aches � Fatigue and stomach cramps � Mild to moderate with symptoms lasting from 24 -48 hours

Norovirus How it Spreads � Leaves body thru the stool of infected person � Enters body when the person touches a contaminated object and transfers it into their mouth � Poor hand washing after using the bathroom or changing diapers � Eating food contaminated with the virus � Person-to-person contamination often spreads virus in families, schools, childcare settings etc.

Norovirus Incubation/Contagious Period � Takes 10 to 50 hours, usually from 24 to 48 hours from the time a person is exposed until symptoms develop � Contagious when the symptoms are present and up to 72 hours after vomiting and/or diarrhea has stopped

Norovirus Temporary Exclusion � Until diarrhea and vomiting have stopped � Anyone with vomiting and diarrhea should not use pools, swimming beaches, recreational water parks, spas, or hot tubs for at least 72 hours after diarrhea and/or vomiting symptoms have stopped

Norovirus Diagnosis/Treatment � Diagnosis may be confirmed with a lab test � Dehydration may happen quickly in young children, and treatment for dehydration may be needed as determined by child’s health care provider

Norovirus Prevention/Control � WASH YOUR HANDS! � Monitor children’s hand washing after they use the toilet or are diapered � Clean and disinfect diapering area and potty chairs after each use � Clean, and disinfect bathrooms, toilets, sinks, at least once daily and when soiled. Sanitize mouthed toys � Do not use water tables for play during outbreaks
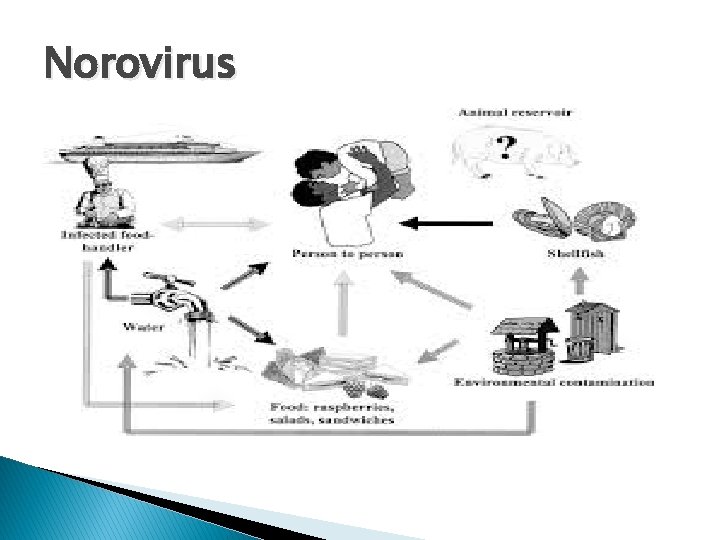
Norovirus

Pertussis (Whooping Cough) � Serious illness (especially in young, unvaccinated children) � Adults and older children may be the source of infection in young children � Concern is that in recent years, more adults, adolescents, and school-aged children have been contracting pertussis � http: //www. bing. com/videos/search? q=whoo ping+cough+video+baby+cdc&view=detail& mid=38 EEE 5 D 0 D 16 C 9291773338 EEE 5 D 0 D 16 C 92917733&FORM=VIRE 1

Pertussis Cause � Bordetella Pertussis bacteria

Pertussis Symptoms � Runny nose, sneezing, mild cough, and possible low-grade fever � After a week or two a persistent cough develops, which causes an explosive bursts of coughing, which sometimes ends in a highpitched whoop and vomiting � Coughing attacks occur more frequently at night

Pertussis Symptoms continued � Coughing attacks usually increase during the first two weeks of illness and then remain the same for 2 or 3 weeks before gradually decreasing � Infants may develop pneumonia and ear infections � May occur in vaccinated children but usually in a milder form

Pertussis Symptoms continued � Older children and adults have a less typical cough; however, it is usually persistent and may lead to vomiting or a whoop � http: //www. webmd. com/children/pertussiswhooping-cough-10/coughing-sounds

Pertussis How it Spreads � Coughing or sneezing of infected person � Spread thru air droplets and is breathed in by another person

Pertussis Incubation/Contagious Period � Takes 4 -21 days, usually 7 -10 days from exposure until symptoms appear � Contagious when cold-like symptoms appear and before persistent and explosive bursts of coughing starts � Person remains contagious until three weeks after explosive bursts of coughing begin � Those treated with antibiotics are contagious until 5 days of treatment are completed

Pertussis Temporary Exclusion � 5 days after appropriate antibiotic treatment begins � If not treated with antibiotics, then the exclusion from child care should be 21 days after the onset of cough � People who develop the symptoms of Pertussis within 21 days of exposure should stay home and call their health care provider

Pertussis Diagnosis � Lab test should be done to confirm � Nasal swab

Pertussis Prevention/Control � Report within 24 hours to your local public health department � They will determine if preventative antibiotics are needed if someone in you facility develops Pertussis

Pertussis Prevention/Control continued � Check immunization records for children and staff � Tdap is recommended for adults having close contact with infants less than 12 months old � CDC recommends immunization for each pregnancy, preferably during the third trimester

Pertussis Prevention/Control continued � Always cover nose and mouth with tissue or your sleeve when you cough/sneeze and dispose of tissues after one use � WASH YOUR HANDS with soap and warm running water � Clean and disinfect commonly touched surfaces (door knobs, refrigerator handles, water faucets, cupboard handles) at least daily � Clean and sanitize mouthed toys, objects, and surfaces at least once daily and when soiled

Pertussis Treatment � Antibiotics shorten the time a person can give it to others, but may do little to lessen the symptoms � Antibiotics are usually not given to people who have had a cough for more than 21 days because they will no longer be helpful

Sources � Hennepin Infectious Disease in Child Care Settings and Schools http: //www. health. state. mn. us/handhygiene/ schools/daycaremanual. html � American Academy of Pediatrics Managing Infectious Diseases in Child Care and Schools, A Quick Reference Guide 3 rd Edition � Kentucky Child Care Health Consultation Program (CCHC) http: //www. kentuckycchc. org/
- Slides: 86