Coma head injury Judita Capkova MD Ph D















![PRESSURE [mm. Hg] INTRACRANIAL PRESSURE (ICP) 40 De-compensation phase Compensation Phase Transition phase 0 PRESSURE [mm. Hg] INTRACRANIAL PRESSURE (ICP) 40 De-compensation phase Compensation Phase Transition phase 0](https://slidetodoc.com/presentation_image_h/1ecbea85a3f3a604e88d8ad28e251aa3/image-19.jpg)









- Slides: 42

Coma, head injury Judita Capkova, MD. Ph. D. Jozef Firment, MD. Ph. D. Department of Anaesthesiology & Intensive Care Medicine Šafárik University Faculty of Medicine, Košice

Coma Is a „state of unarousable unresposiviness“ (of unconsciousness from which the patient cannot be aroused) • No evidence of arousal: no spontaneous eye opening, no speech, voluntary limb movement • Unresponsive to external stimuli, although abnormal postures may be • GCS – level of consciousness, coma: GCS ≤ 8 Firment • Involuntary movements (seizures) may occur 2

GLASGOW COMA SCALE Decerebrate posturing Firment Decorticate posturing 3

Causes of coma Metabolic Toxic Infection Structural lesions with or • Focal brainstem signs • Lateralizing cerebral signs • Meningeal irritation without -toxic, metabolic causes usually do not produce focal signs - infections, structural lesions produce focal signs 4 Firment • •

Coma without focal/lateralizing neurological signs • Anoxia/ hypoperfusion • Metabolic: e. g. Hypo/-hyperglycaemia, acidosis/alkalosis, • • • Intoxications: e. g. alcohol, opiates, benzodiazepines, . . Endocrine : hypothyreoidism Hypo- or hyperthermia Epilepsy Hypertensive encephalopathy Firment hepatic or renal failure 5

Coma with focal/lateralizing neurological signs ( due to brainstem or cerebral dysfunction) • Vascular : cerebral haemorrhage or infarction • Supra or infratentorial space-occupying lesion: tumour, haematoma, abscess • Meningitis, encephalitis • Subarachnoid haemorrhage Firment Coma with meningism 6

Immediate management 1. Stabilize the patient ABC • Open the airway, breathing. give oxygen, stabilise the cervical spine as required • OTI, ventilation ? (GCS ≤ 8) p. O 2, p. CO 2 • Support the circulation: correct hypotension (colloids, • Treat seizures (diazepam, phenytoin) - CMRO 2 • Take blood for glucose, U+Es, calcium, liver enzymes, albumin, clotting screen, FBC, toxicology (+urine) Firment inotropes), CVP? 7

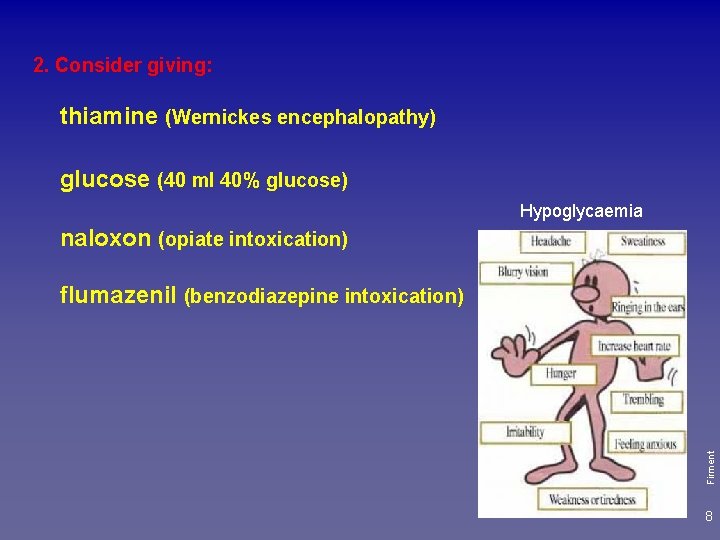
2. Consider giving: thiamine (Wernickes encephalopathy) glucose (40 ml 40% glucose) Hypoglycaemia naloxon (opiate intoxication) Firment flumazenil (benzodiazepine intoxication) 8

3. Examine patient: History General examination • Core temperature, heart rate, rhythm, BP, respiratory pattern, breath, skin, heart, abdomen, fundi Is there meningism? – neck stiffness (inflammation, Asses GCS Look for evidence of brainstem dysfunction Are there lateralizing signs? Firment blood) 9

Test brainstem dysfunction Pupillary response Corneal reflex Spontaneous eye movements Oculocephalic response/Doll’s head manoeuvre Oculovestibular response Swallowing reflex Respiratory pattern Firment • • 10

Motor function: • Decerebrate posturing – pontine damage Decorticate posturing Decerebrate posturing Firment • Decorticate posturing – lesions above the pons 11

4. Plan for further investigations: Firment 1. Brainstem function intact: urgent CT head scan : - lesions (subdural haematoma, . . ), - normal – lumbar puncture, CSF analysis 12

4. Plan for further investigations: 1. Brainstem function intact: urgent CT head scan : - lesions (subdural haematoma, . . ), - normal – lumbar puncture, CSF analysis 2. Brainstem function not intact: Signs ICH (intracranial hypertension): - early: headache, vomiting, seizures, focal neurology, papilloedema - late: incr. BP, bradycardia, coma, Cheyne Stokes breathing, apnoe. - if herniation syndrome appears to be progressing rapidly - if herniation syndrome appears to be progressing not so rapidly – mannitol and CT, surgeon Firment mannitol, hyperventilation, surgeon 13

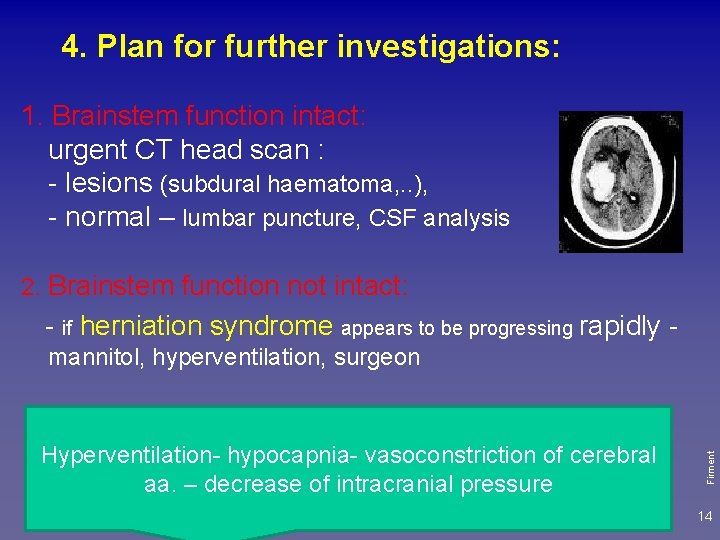
4. Plan for further investigations: 1. Brainstem function intact: urgent CT head scan : - lesions (subdural haematoma, . . ), - normal – lumbar puncture, CSF analysis 2. Brainstem function not intact: - if herniation syndrome appears to be progressing rapidly - if herniation syndrome appears to be progressing not so rapidly – mannitol and CT vasoconstriction of cerebral Hyperventilationhypocapniaaa. – decrease of intracranial pressure Firment mannitol, hyperventilation, surgeon 14

Head injury (HI) • Primary brain injury : - brain lacerations, contusions, diffuse axonal injury due to accelaration or deceleration Firment - the neurones lost at the time of HI are lost forever 15

Secondary injury: • Due to raised intracranial pressure (ICP) and inadequate cerebral perfusion • Systemic : Intracranial: • Hypoxaemia • Hypotension • Hypercarbia • Severe hypocapnia • Pyrexia, . . • Anaemia • Hyper/hypoglycaemia • Haematoma (extradural, subdural, intracerebral) • Brain swelling/ oedema • Cerebral ischemia (vasospasm, seizures) • Inflammatory mediators Firment • Causes of secondary brain injury : 16

Prevention of secondary injury is the aim of the treatment. Firment Prevention therapy may improve outcome. 17

Firment INTRACRANIAL COMPENSATION FOR EXPANDING MASS 18
![PRESSURE mm Hg INTRACRANIAL PRESSURE ICP 40 Decompensation phase Compensation Phase Transition phase 0 PRESSURE [mm. Hg] INTRACRANIAL PRESSURE (ICP) 40 De-compensation phase Compensation Phase Transition phase 0](https://slidetodoc.com/presentation_image_h/1ecbea85a3f3a604e88d8ad28e251aa3/image-19.jpg)
PRESSURE [mm. Hg] INTRACRANIAL PRESSURE (ICP) 40 De-compensation phase Compensation Phase Transition phase 0 VOLUME Up to 15 mm. Hg, above 40 malignant oedema Firment 20 19

INCREASED ICP • Normal ICP 0 -10 mm. Hg • ICP > 15 -20 mm. Hg treatment is required • Causes of raised ICP: - Increased extracellular fluid: cerebral oedema - Increased cerebral blood flow : hypoxia, hypercarbia, . . (vasodilatation) : venous obstruction in the neck, coughing, . . - Increased CSF volume : hydrocephalus, . . . Firment - Increased cerebral venous volume 20

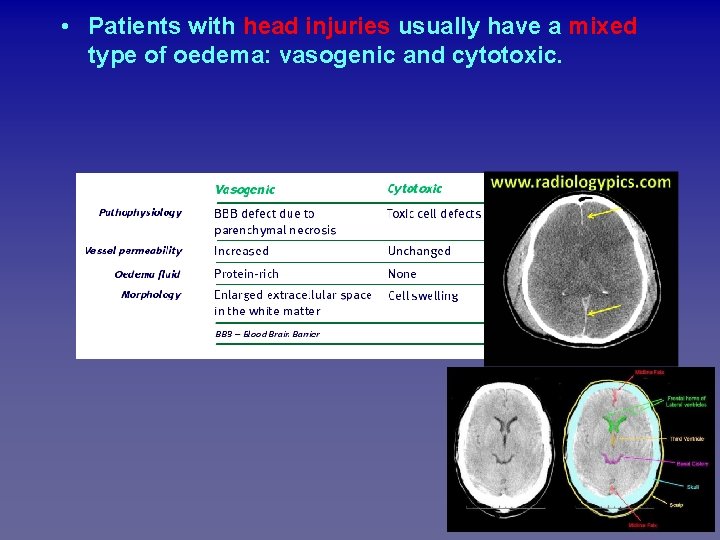
Firment • Patients with head injuries usually have a mixed type of oedema: vasogenic and cytotoxic. 21

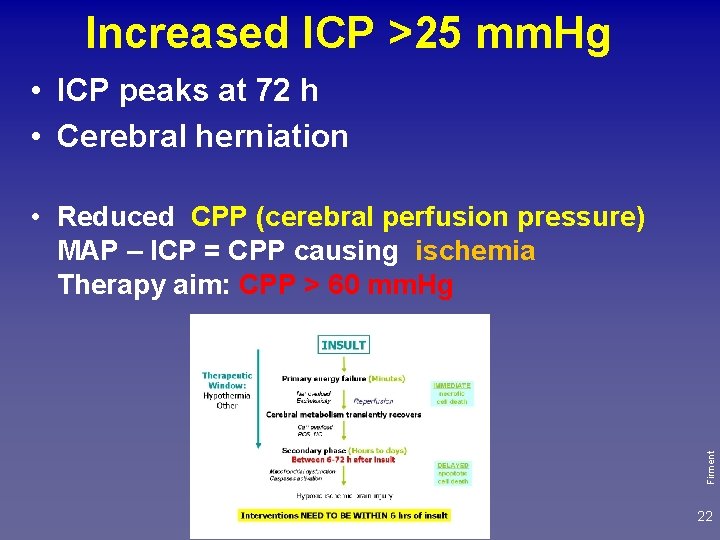
Increased ICP >25 mm. Hg • ICP peaks at 72 h • Cerebral herniation Firment • Reduced CPP (cerebral perfusion pressure) MAP – ICP = CPP causing ischemia Therapy aim: CPP > 60 mm. Hg 22

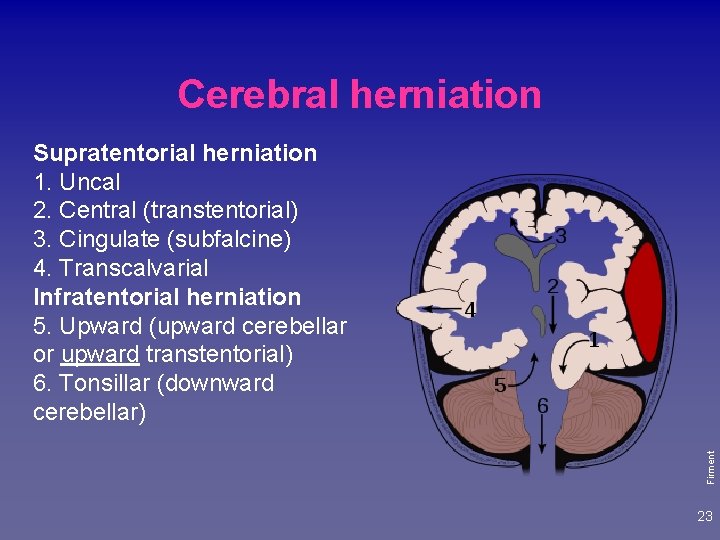
Cerebral herniation Firment Supratentorial herniation 1. Uncal 2. Central (transtentorial) 3. Cingulate (subfalcine) 4. Transcalvarial Infratentorial herniation 5. Upward (upward cerebellar or upward transtentorial) 6. Tonsillar (downward cerebellar) 23

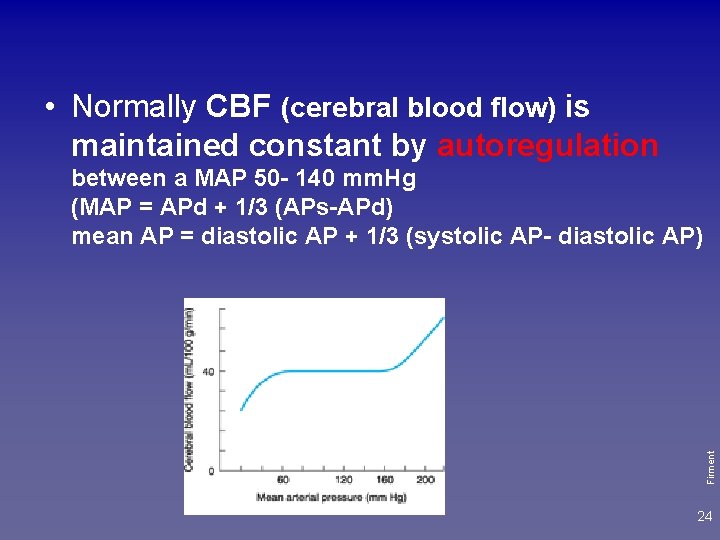
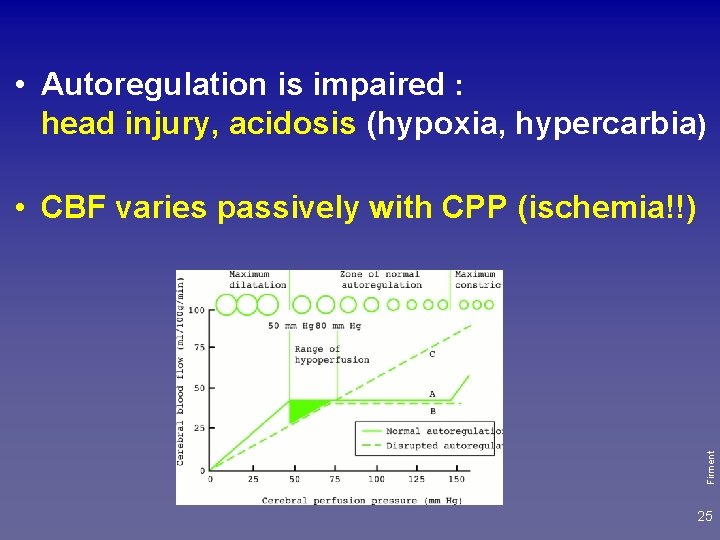
• Normally CBF (cerebral blood flow) is maintained constant by autoregulation Firment between a MAP 50 - 140 mm. Hg (MAP = APd + 1/3 (APs-APd) mean AP = diastolic AP + 1/3 (systolic AP- diastolic AP) 24

• Autoregulation is impaired : head injury, acidosis (hypoxia, hypercarbia) Firment • CBF varies passively with CPP (ischemia!!) 25

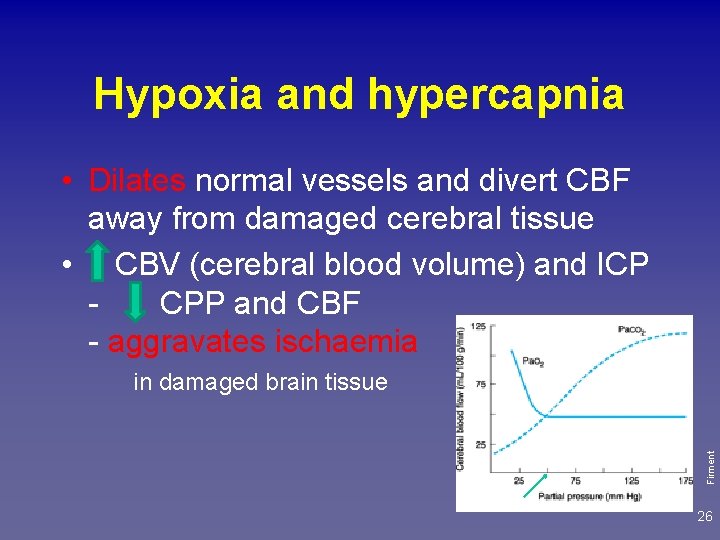
Hypoxia and hypercapnia • Dilates normal vessels and divert CBF away from damaged cerebral tissue • CBV (cerebral blood volume) and ICP CPP and CBF - aggravates ischaemia Firment in damaged brain tissue 26

Hypocapnia • Constricts normal vessels CBV and ICP • !! Severe hypocapnia – exccess vasoconstriction – ischaemia in normal tissue Recommended: normal Pa CO 2 4, 6 – 5, 3 k. Pa (35 -40 mm. Hg) Firment CPP and CBF 27

Raised ICP: immediate management • Open the airway, intubation, mechanical ventilation, keep Pa CO 2 3, 3 – 4, 0 k. Pa (25 -30 mm. Hg) • Correct hypotension: colloids, infusions of inotropes • • • Take blood for glucose, U+Es, calcium, liver enzymes, albumin, clotting screen, FBC Firment • • CPP < 70 mm. Hg is critical ! Spinal immobilisation- all pt Detect other injuries: 50% have potentially lethal thoracic or abdominal injuries Treat seizures (increase O 2 consumption) Sedation (paralysis) prevent ICP elevation in agitated pt 28

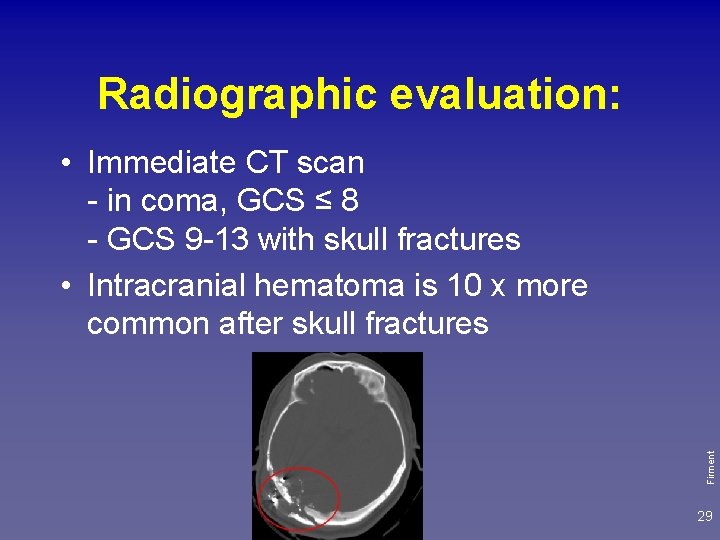
Radiographic evaluation: Firment • Immediate CT scan - in coma, GCS ≤ 8 - GCS 9 -13 with skull fractures • Intracranial hematoma is 10 x more common after skull fractures 29

Monitoring • GCS is adequate in mild injuries • ICP intracranial pressure – severe HI Firment • Cerebral oxygen saturation Sj. O 2 jugular venous bulb fibreopthic catheter Sj. O 2 < 55% inadequate (low) CBF 30

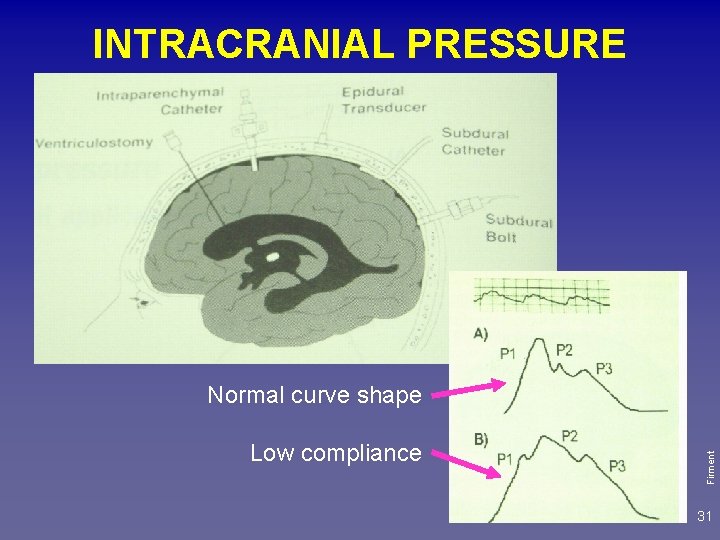
INTRACRANIAL PRESSURE Low compliance Firment Normal curve shape 31

Management MAP > 70 mm. Hg ICP < 15 mm. Hg CPP > 60 mm. Hg and oxygenation: Sat. O 2 > 90%, Sj. O 2 >55% Firment • Prevention of secondary injury is the aim: optimise CBF: MAP – ICP = CPP 32

1. Reduce ICP: • Hyperventilation : Pa. CO 2 3, 3 – 4 k. Pa (25 -30 mm. Hg) not routinelly only if herniation appears • Loop diuretics (furosemid 20 -40 mg i. v. ), osmotic agents (mannitol 0, 5 -1 g/kg )- reduce ICP • Improved venous drainage: midline haed position + 30°elevation, • Ventriculostomy drainage/decompressive surgery – if other fails • No corticosteroids Firment !! suctioning, PEEP, physiotherapy increase thoracic venous p. 33

2. Reduce cerebral metabolism: • Avoid hyperglycaemia (BS 4 -7 mmol/l) hyperglycaemia increase cerebral lactate production • Prophylactic anticonvulsants • Adequate analgesia and sedation: benzodiazepines, propofol, thiopentone • Antipyretics and cooling Firment (33 -34 °C maybe neuroprotective) 34

Treat complications: • Avoid nasogastic tubes in basilar skull fracture Firment • Hypotalamic injury : inappropriate ADH secretion – diabetes insipidus • Meningitis – ATB 35

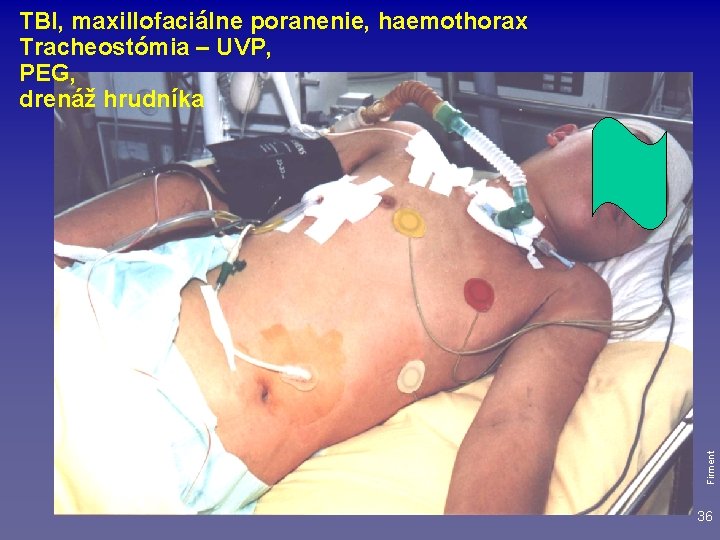
Firment TBI, maxillofaciálne poranenie, haemothorax Tracheostómia – UVP, PEG, drenáž hrudníka 36

jcapkova@capko. sk Firment Thank you! 37

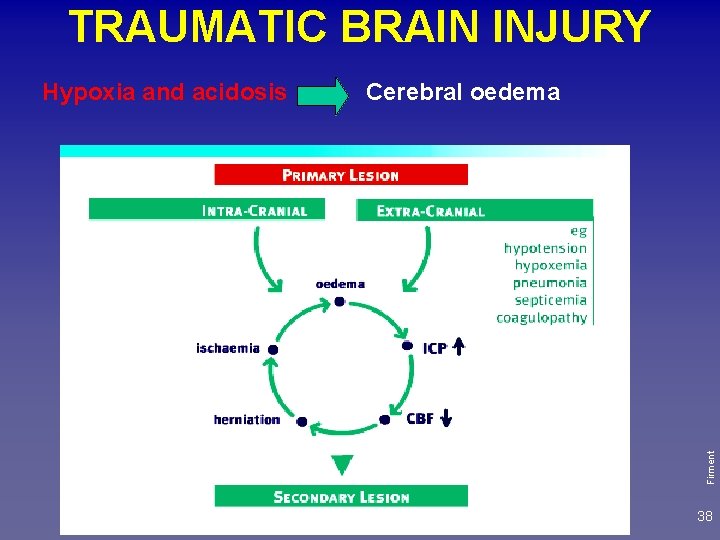
TRAUMATIC BRAIN INJURY Cerebral oedema Firment Hypoxia and acidosis 38

1. Stabilize the patient: ABC give oxygen, support circulation, treat seizures, stabilise the cervical spine as required 2. Consider giving thiamine, glucose (40 ml 40% glucose), naloxon, flumazenil 3. Examine patient 4. Plan for further investigations Firment Immediate management 39

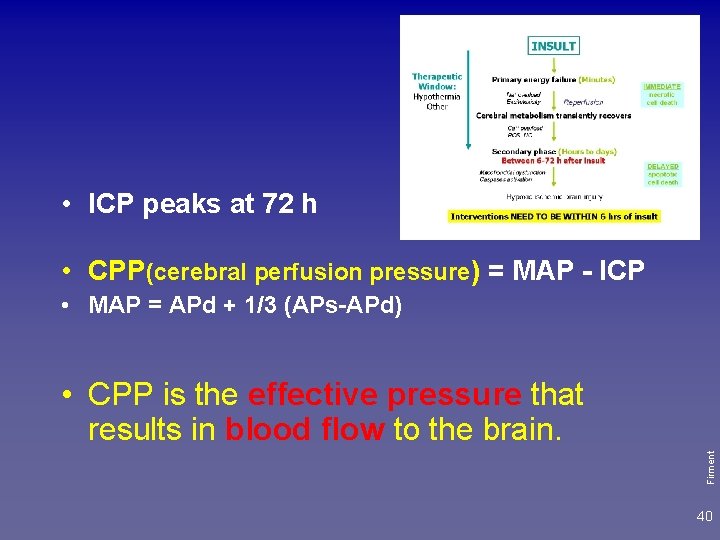
• ICP peaks at 72 h • CPP(cerebral perfusion pressure) = MAP - ICP • MAP = APd + 1/3 (APs-APd) Firment • CPP is the effective pressure that results in blood flow to the brain. 40

CPP(cerebral perfusion pressure) = MAP - ICP • CBF (cerebral blood flow) is maintained constant by autoregulation (between a MAP 50140 mm. Hg). Autoregulation is impaired : head injury, acidosis (hypoxia, hypercarbia) Firment CBF varies passively with CPP (ischemia!!) Therapy aim: CPP < 70 mm. Hg is critical ! 41

5. Progress in monitoring • Regular and frequent observations of vital signs and neurological state • Emergency treatment of raised ICP (intracranial pressure) headache, vomiting, seizures, focal neurology, papilloedema - late: incr. BP, bradycardia, coma, Cheyne Stokes breathing, apnoe. Firment Signs ICH (intracranial hypertension): - early: 42