Columbia Suicide Severity Rating Scale What is it

Columbia Suicide Severity Rating Scale

What is it? • The Columbia Suicide Severity Rating Scale (C-SSRS) is an evidence-based suicide risk screening assessment tool recommended in the Joint Commission Best Practice Library. • Mental health training is not required to administer the screening • Successfully used for screening by hospitals, outpatient areas, first responders, military • Built into Epic exactly as it is designed 2

Why do it? • Identifying patients at risk for suicide is one of the 2017 Joint Commission National Patient Safety Goals (NPSG. 15. 01) • Highest suicide rates in the nation in 30 years • 10 th leading cause of death in the U. S. • 2 nd leading cause of death among those aged 10 – 24 3
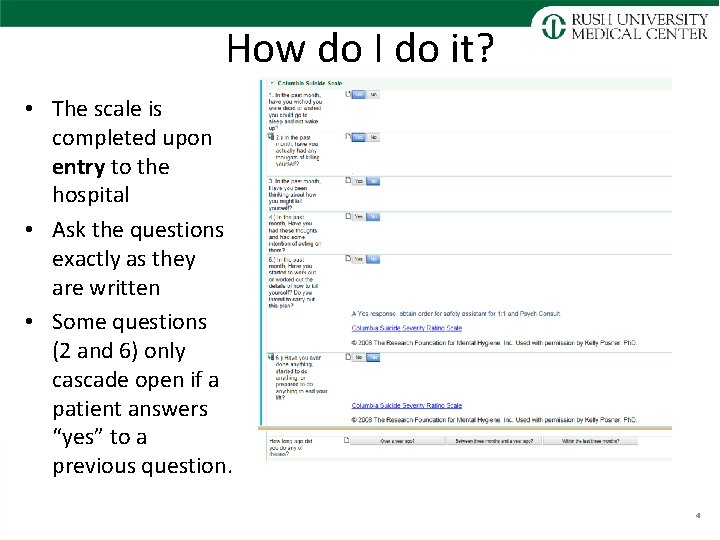
How do I do it? • The scale is completed upon entry to the hospital • Ask the questions exactly as they are written • Some questions (2 and 6) only cascade open if a patient answers “yes” to a previous question. 4

How do I do it? • Actions are required of you if the patient answers “yes” to a question. The Chart below describes your responsibility • Use largest number question with a “yes” answer to drive action of care Question # Action for “Yes” Response #1 Notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge #2 Notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge #3 #4 Contact Psychiatric RN Liaison Ask admitting service to assess patient safety; suggest psychiatric consult #5 Initiate 1: 1, ask admitting service to order psych consult (required) DETAILED ON THE NEXT SLIDE #6 < 1 week: initiate 1: 1, ask admitting service to order psychiatric consult 1 week – 3 months: Contact Psychiatric RN Liaison > 3 months, notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge 5

How do I do it? • Question #5 addresses active suicidal ideation with a plan and intent to act. “Have you started to work out or worked out the details of how to kill yourself? Do you intend to carry out this plan” • If a patient answers “yes” to question 5: 1. Initiate a safety assistant 2. Alert the physician 3. Ask him or her to enter an order for: 1. Suicide risk 2. 1: 1 monitoring 3. A psychiatric consult. 6

Question Your patient answers “yes” to questions 1, 2, and 3 on screening, but “no” to 4, 5, and 6. What do you do? a. Put the patient with a 1: 1 safety assistant b. Call/page the psych nurse liaison c. Notify Case Management d. A and C Question # Action for “Yes” Response #1 Notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge #2 Notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge #3 #4 Contact Psychiatric RN Liaison Ask admitting service to assess patient safety; suggest psychiatric consult #5 Initiate 1: 1, ask admitting service to order psych consult (required) #6 < 1 week: initiate 1: 1, ask admitting service to order psychiatric consult 1 week – 3 months: Contact Psychiatric RN Liaison > 3 months, notify Case Manager/Social Worker to provide outpatient behavioral health information at discharge 7

References • Centers for Disease Control and Prevention. (2016). Leading Causes of Death. Retrieved from https: //www. cdc. gov/nchs/fastats/leading-causes-of -death. htm • National Alliance on Mental Illness. (2017). Risk of Suicide. Retrieved from http: //www. nami. org/Learn-More/Mental-Health-Conditions/Related. Conditions/Suicide • National Alliance on Mental Illness. (2017). Mental Health by the Numbers. Retrieved from http: //www. nami. org/Learn-More/Mental-Health-By-the. Numbers • The Columbia Lighthouse Project. (2016). About the Scale. Retrieved from http: //cssrs. columbia. edu/the-columbia-scale-c-ssrs/about-the-scale/ • The Joint Commission. (2017). Hospital National Patient Safety Goals. Retrieved from https: //www. jointcommission. org/assets/1/6/2017_NPSG_HAP_ER. pdf 8
- Slides: 8