Colorectal Cancer Prof Clement F Kiire MBCh B

Colorectal Cancer Prof Clement F. Kiire MBCh. B, MMed, MRCP(UK), FRCP(London), FRCP(Glasgow), FRCP(Edinburgh), FCP(SA), FESG, MD(Makerere)

Learning Objectives �Describe cancer the significance of colon �Identify the factors and conditions associated with colon cancer �Describe the treatment options

Colorectal Cancer � 90% of cases occur after age 50 � Third leading cause of cancer in the US � Second leading cause of cancer death � Average lifetime risk for developing this cancer is 6% � Men and women are affected equally � Women are more likely to have right sided colonic adenomas � Distributed evenly among racial groups � Africans and Hispanics have a lower survival rate
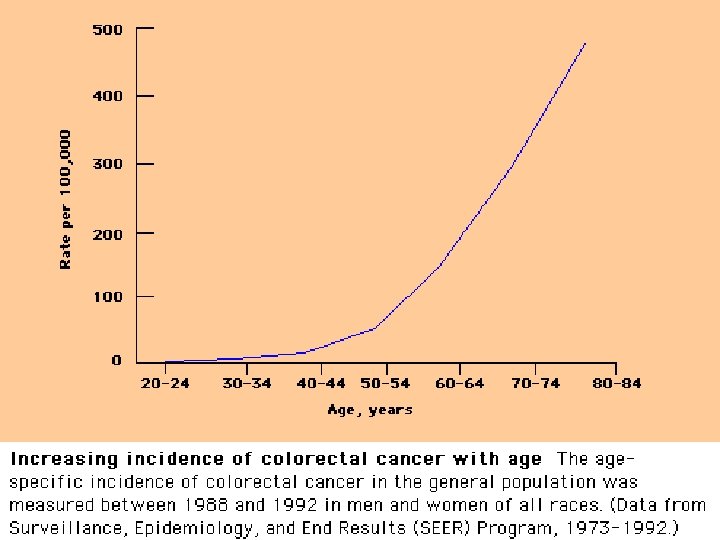
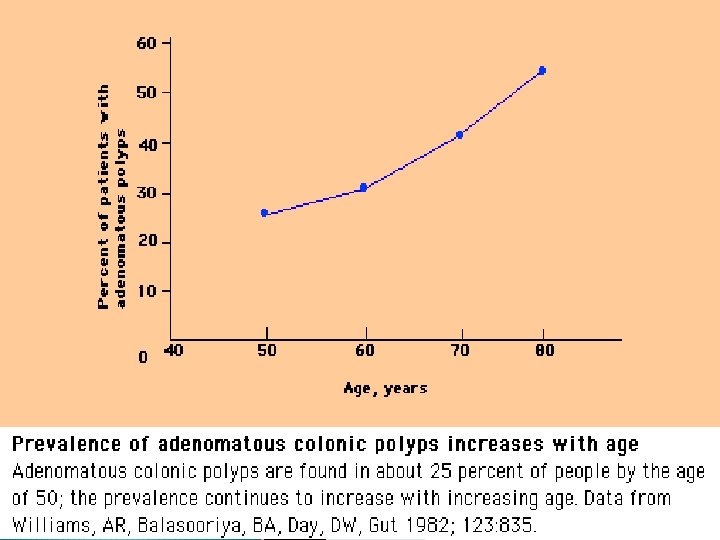
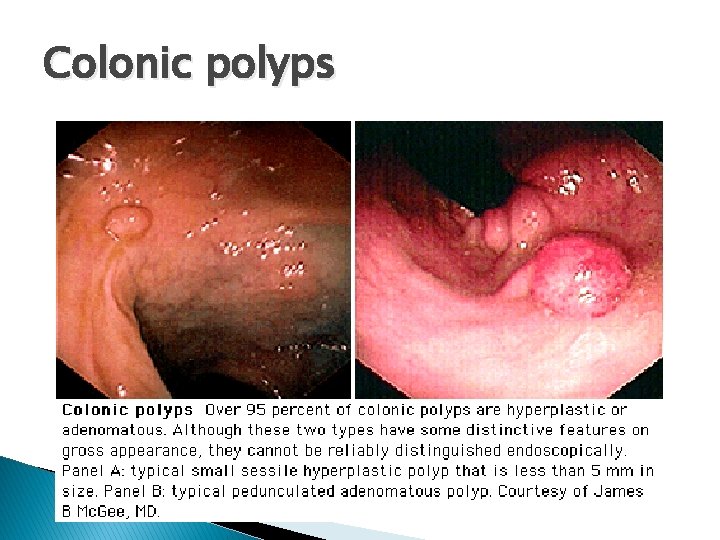
Colonic polyps

Risk Factors • • • Age >50 yrs High fat, low fiber diet IBD – Chronic ulcerative colitis and Crohn’s disease Familial adenomatous polyposis (FAP) Hereditary nonpolyposis colorectal cancer (HNPCC) Hamartomatous polyposis syndromes Peutz-Jegher’s syndrome Juvenile polyposis Family history – colorectal adenomas, colorectal cancer Personal history of colorectal adenomas; ureterosigmoidostomy; breast, ovarian and uterine cancers
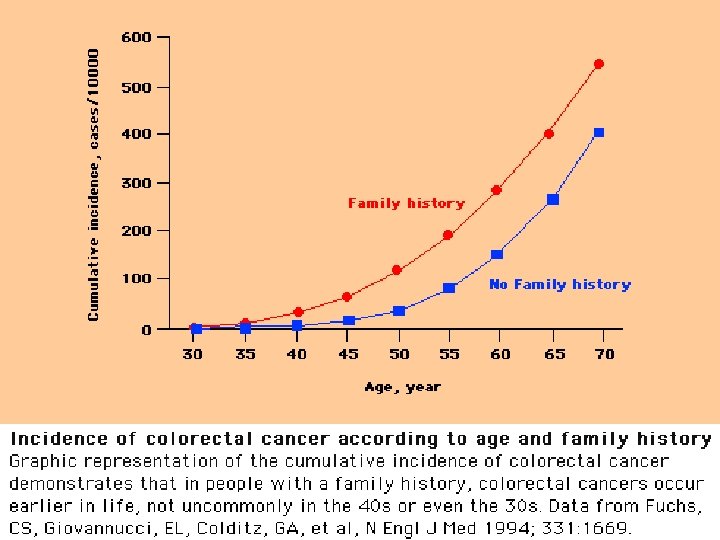
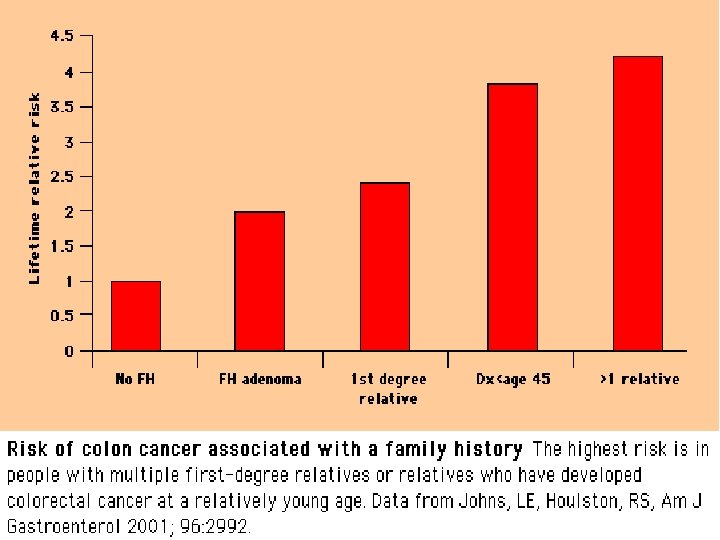
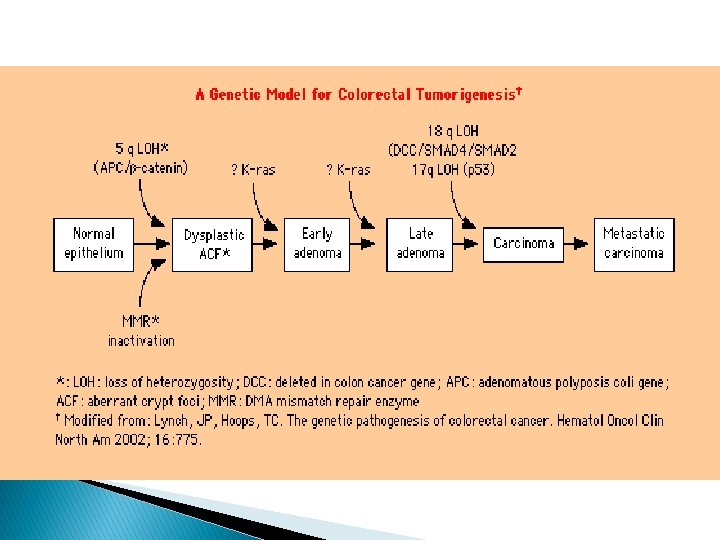
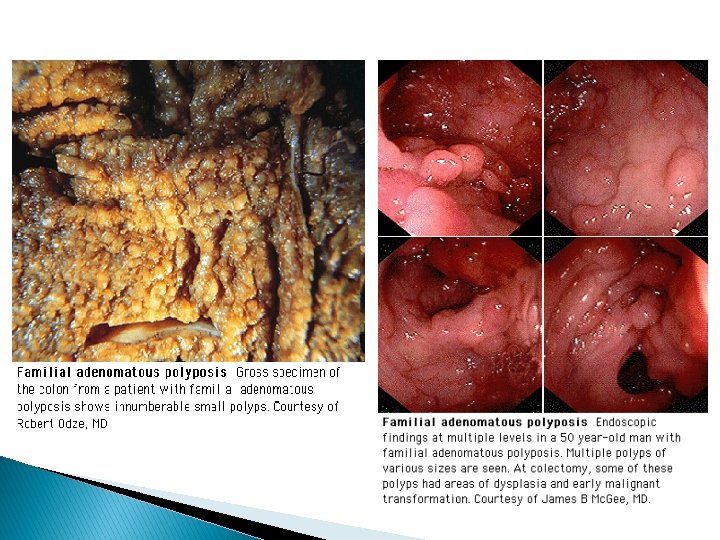

Factors associated with increased risk of CRC � Lack of physical activity � Consumption of red meat � Obesity � Cigarette smoking � Alcohol use Factors associated with decreased risk of CRC � Foods containing folic acid � ASA and other NSAIDs � Postmenopausal HRT � Ca supplementation � Selenium � Consumption of fruits, vegetables and fiber

Clinical Presentation Depends on tumour location: �Proximal (right-sided) lesions present with symptoms caused by anaemia: fatigue, weight loss, shortness of breath, lightheadedness, mahogany faeces caused by occult bleeding �Distal (left-sided) lesions present with symptoms of obstruction: changes in BM pattern, post-prandial colicky abdominal pain, fresh rectal bleeding.

Clinical Manifestations � Abdominal pain - 44% � Change in bowel habit - 43% � Fresh rectal bleeding or melaena - 40% � Weakness - 20% � Anaemia without other gastrointestinal symptoms - 11% � Weight loss - 6% � Some patients have more than one abnormality � 15 -20% of patients have distant metastatic disease at the time of presentation

DIAGNOSTIC TESTS � Digital rectal exam (DRE) � Barium enema (BE) with or without air contrast � Sigmoidoscopy, rigid type or flexible fiber optic type � Colonoscopy (or colon endoscopy) � Computed tomography (CT) � Transrectal ultrasound (TRUS) � Magnetic resonance imaging (MRI) � Laparotomy

DIAGNOSTIC TESTS � Digital rectal exam (DRE) � Barium enema (BE) with or without air contrast: used primarily to locate deformities of intestinal topography � Sigmoidoscopy, rigid type or flexible fiber optic type: used to visualize local rectal tumors or for routine screening � Colonoscopy (or colon endoscopy): Direct visual examination of the colon and rectum detects early polypoid tumors preoperatively and recurrences post-resection; Multiple biopsies may be performed at time of study to increase sensitivity.

DIAGNOSTIC TEST CONT’D • Computed tomography (CT): Used to stage disease and identify metastases • Transrectal ultrasound (TRUS): An excellent choice for preoperative staging of rectal carcinomas • Magnetic resonance imaging (MRI): very useful for diagnosing metastatic disease • Laparoscopy: Useful in detecting metastases to abdominal regions (especially omentum or liver) that often remain undetected by current imaging techniques
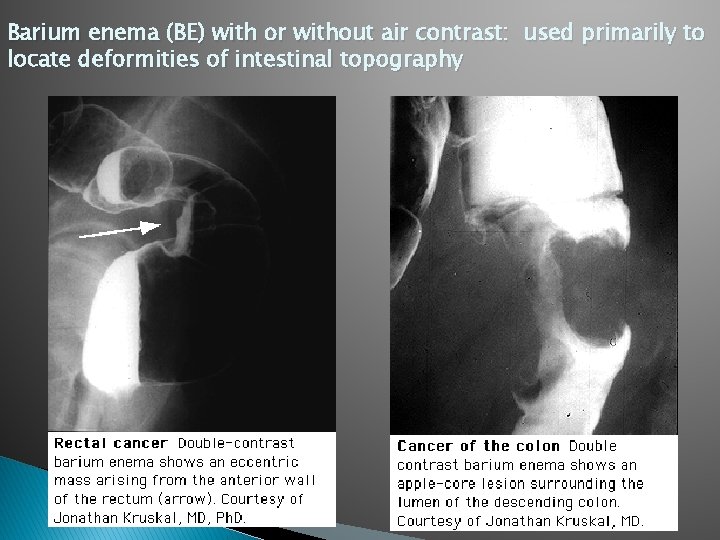
Barium enema (BE) with or without air contrast: used primarily to locate deformities of intestinal topography
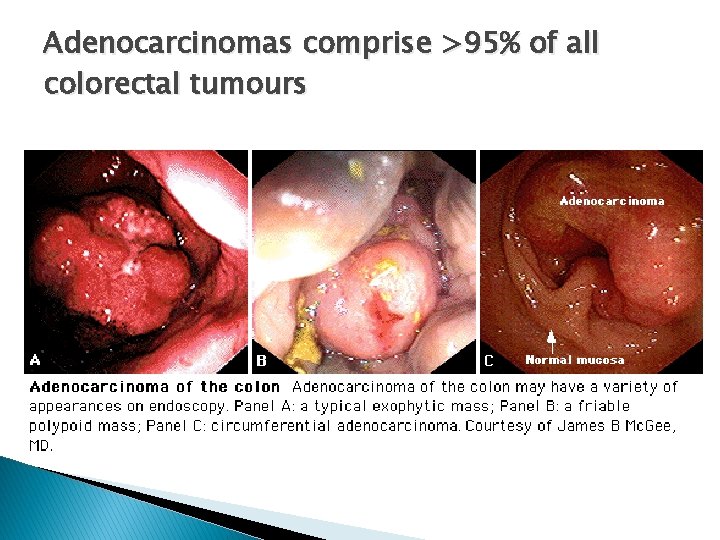
Adenocarcinomas comprise >95% of all colorectal tumours

Tumour markers Carcinoembryonic antigen (CEA) Carbohydrate antigen (CA) 19 9, CA 50, and CA 195 � � have a low diagnostic ability to detect primary CRC overlap with benign disease low sensitivity for early stage disease have prognostic utility An expert panel on tumour markers convened by the American Society of Clinical Oncology (ASCO) recommended that serum CEA levels not be used as a screening test for colorectal cancer

TNM Staging Classification of CRC Primary tumour (T) � TX - Primary tumour cannot be assessed � T 0 - No evidence of primary tumour � Tis - Carcinoma in situ: intraepithelial or invasion of lamina propria � T 1 - Tumour invades submucosa � T 2 - Tumour invades muscularis propria � T 3 - Tumour invades through the muscularis propria into the subserosa or into nonperitonealized pericolic or perirectal tissues � T 4 - Tumour directly invades other organs or structures, and/or perforates visceral peritoneum

TNM Staging Classification of CRC cont’d � Regional lymph nodes (N) � NX - Regional lymph nodes cannot be assessed � N 0 - No regional lymph-node metastasis � N 1 - Metastasis in 1 to 3 regional lymph nodes � N 2 - Metastasis in 4 or more regional lymph nodes

TNM Staging Classification of CRC Cont’d � Distant metastasis (M) � MX - Distant metastasis cannot be assessed � M 0 - No distant metastasis � M 1 - Distant metastasis

Prognosis and 5 -year survival rates for colon cancer � Stage � Stage I (T 1 -2 N 0) - 93% IIA (T 3 N 0) - 85% IIB (T 4 N 0) - 72% IIIA (T 1 -2 N 1) - 83% IIIB (T 3 -4 N 1) - 64% IIIC (N 2) - 44% IV - 8%

Guidelines for screening adults aged 50 years or older and at average risk of CRC � Faecal occult blood test (FOBT) every year ◦ Occult stool testing must be repeated at least 3 times on different stool samples. ◦ Diet must be free of peroxidase activity (turnips & horseradish). ◦ Tests may need to be repeated if there is a history of: �usage of possible gastric irritants such as salicylates, other anti-inflammatory agents �haemorrhoids �diverticulitis �peptic ulcer disease (PUD) or other cause of GI bleeding

Key elements in screening people with an average risk of CRC Symptoms require diagnostic work up � Offer screening to men and women aged 50 and older � Stratify patients by risk � Options should be offered � Follow up of positive screening test with diagnostic colonoscopy � Appropriate and timely surgery for detected cancers � Follow up surveillance required after polypectomy and surgery � Providers need to be proficient � Encourage participation of patients �


Blood work that may be indicated � Complete blood count (CBC) � Liver chemistries � Carcinoembryonic antigen level (CEA) � C-Reactive protein (CRP)

Blood work that may be indicated � Complete blood count (CBC) Anemia may be a symptom of right-sided bowel cancer � Liver chemistries: Abnormal liver enzyme results may suggest metastatic disease

Blood work that may be indicated � Carcinoembryonic antigen level (CEA): ◦ Normal value: 0 -2. 5 mg/ml; up to 10 mg/ml in tobacco smokers ◦ Useful in establishing diagnosis and recurrence for tumours that secrete CEA and in following disease progression ◦ Because colon lesions are not likely to secrete CEA, it is not a highly reliable indicator of colon cancer ◦ If CEA is elevated, return to normal levels is expected to occur within 48 hours after complete tumour excision

Blood work that may be indicated �C-Reactive protein (CRP): ◦ Increased plasma concentration of CRP is associated with subsequent development of colon cancer ◦ Preliminary findings are consistent with the established association between colon cancer and inflammatory bowel disease (IBD) ◦ CRP research is ongoing and full corroboration of suggestive findings has not been established

Genetic testing � Genotyping (APC gene test) should be used when other diagnostic avenues have been exhausted � Medically necessary in presence of strong family history for familial adenomatous polyposis (FAP), attenuated familial adenomatous polyposis (AFAP), or hereditary non-polyposis colorectal cancer (HNPCC)

Differential diagnosis Benign lesions Crohn’s colitis Diverticulosis Endometriosis Solitary rectal ulcer Lipoma Tuberculosis Amoebiasis Cytomegalovirus Fungal infection Extrinsic lesion Arterio-venous malformations Adenomatous polyps◦ Premalignant neoplasm ◦ Morphological typestubular, tubulovillous, villous Ischemic colitis Infarcted colon Megacolon Haemorrhoids Malignant lesions Adenocarcinoma Lymphoma Carcinoid tumor Kaposi’s sarcoma Prostate cancer

Treatment Options Surgical excision: mainstay of curative Rx � Specific procedure depends on the anatomic location of the cancer, but typically involves hemi-colectomy � Surgical resection of affected bowel with clear margins, along with the adjacent mesentery and at least 12 regional nodes � For rectal tumours, total meso-rectal excision with a distal surgical margin of at least 2 cm is recommended � For tumours that are located within 6 cm of the anal verge, or involve the anal sphincter, wide surgical resection with abdominoperineal resection and permanent colostomy is recommended � Local excision, for palliative treatment or

Treatment Options Radiation therapy: � Postoperative radiation, with or without chemotherapy, significantly reduces local recurrence rates � Common regimen incorporates infusional 5 fluorouracil (5 -FU) as a radiosensitizer to boost the efficacy of pelvic radiation � Administered as 45 -55 Gy over 5 weeks � Repeated as needed

Treatment Options Systemic chemotherapy � 5 -FU has been the mainstay of systemic chemotherapy for CRC � Capecitabine was approved in 2001 as firstline therapy for metastatic CRC � Irinotecan (Camptosar), Oxaliplatin (Eloxatin), Bevacizumab, Cetuximab

Treatment Options Electrocoagulation � Mostly palliative treatment for rectal carcinomas � Curative for small subset of patients Palliative Care • For advanced incurable cancers

CONCLUSION • • • Colorectal Cancer is one of the leading Cancers in the world. It is a major cause of morbidity and mortality. It is caused by a combination of environmental lifestyle issues and genetic causes. Increasing Cancer rates in developing Countries including Uganda. Need for a national Cancer plan for all Cancers including Colorectal Cancer.
- Slides: 38