COLORECTAL CANCER Infusion Reactions INTRODUCTION Albert 83 M

COLORECTAL CANCER Infusion Reactions

INTRODUCTION Albert, 83 M § § Retired fashion designer and entrepreneur Presented to Cabrini Brighton for C 6 chemotherapy Metastatic CRC with liver met FOLFOX 6 regimen with good effect

HOPC Nov 2014 § U/S and CT-CAP revealed extensive metastatic disease involving entire liver § Suspected to be secondary to a previously resected sigmoid polyps Initial presentation § § § Persistent nausea, anorexia and generalised weakness Bowel symptoms of constipation Weight loss 5 kg Denied symptoms of liver disease Deranged LFT

HOPC Hx of colonic polyps § Routine colonoscopy for many years Dec 2012 § Polypectomy with histopathology revealing adenocarcinoma § Follow-up CT showed no evidence of nodal or distant metastasis § Follow-up colonoscopy all clear

HOPC Referral to A/Prof. Gary Richardson § Work-up § § PET scan – bowel and liver involvement Tumour markers – CEA and CA 19 -9 Liver core biopsy – moderately differentiated adenocarcinoma Colonoscopy + biopsy – recurrent adenocarcinoma § CRC grade IVA

CHEMOTHERAPY FOLFOX 6 regimen § Oxaliplatin, Leucovorin, 5 FU, Bevacizumab § Serum CEA § LFTs Side effects § § § § Fatigue – exercise tolerance and sleep Bowel symptoms GORD Infusion reaction Weight stable Hypertension well controlled Nil other significant chemo toxicity

PAST MEDICAL HISTORY Ongoing issues § Hyperlipidaemia – on Lipitor § IHD and hypertension – on Coversyl and Tenormin Inactive issues § Gout – on prophylactic allopurinol § AF – asymptomatic since 1999 § Meningioma – excised in 1997 NKDA

SOCIAL HISTORY Lives at home with wife § Breast cancer Previously IADL § Golfed twice weekly, walked 18 holes § Cleaner fortnightly Currently more fatigable § Golf once a week, requires buggy § Still gardens One daughter § Lives nearby and helps

SUMMARY Albert 83 M § Currently C 6 of FOLFOX 6 regimen for metastatic CRC with liver met § Has been progressing well on treatment with decline in serum CEA and improvement in LFTs § Has had relatively minor side effects from chemo § But most recently had an infusion reaction that settled with antihistamines, and since have had oxaliplatin removed from regimen

ISSUES 1. Metastatic CRC with liver met § Chemotherapy and post-chemo management 2. Medical management of IHD 3. Decline in function and exercise tolerance § EP and OT assessment 4. Social issues § § Age Assistance with ADL

INFUSION REACTION

INFUSION REACTION Definition § An unexpected reaction that cannot be explained by the known toxicity profile of the drug Virtually all chemotherapeutic agents have the potential to initiate an infusion reaction

SIGNS AND SYPMTOMS Standard Infusion Reactions (SIRS) § Cutaneous § Flushing, itching, urticaria ± angioedema § Respiratory § Cough, nasal congestion, SOB, chest tightness, wheeze, hypoxia § Cardiovascular § Dizziness or syncope, tachycardia, hypotension, hypertension § Gastrointestinal § N/V, abdo pain and diarrhoea § Neuromuscular § Sense of impending doom, tunnel vision, dizziness, seizures, severe back/chest/pelvic pain Anaphylaxis if more severe

TIMING AND RISK FACTORS Usually occurs during or within a few hours of drug infusion Occasionally one to two days after administration Infusion reactions found to be more common in these settings § § IV administration After multiple cycles of certain agents Prior infusion reactions to drug of same chemical class History of multiple drug allergies

COMMONLY IMPLICATED AGENTS Taxanes Platinum Doxorubicin L-asparaginase Procarbazine Etoposide Bleomycin Cytarabine Ixabepilone
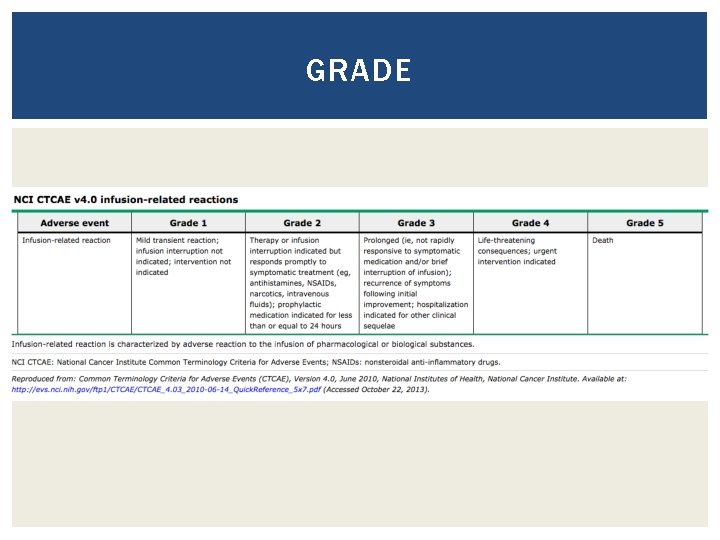
GRADE

MANAGEMENT OF SIR Immediate § Symptomatic management ± resuscitation Rechallenge § Reduced infusion rate § Premedication Desensitisation techniques

OXALIPLATIN AND PLATINUM DRUGS Classic type 1 Ig. E-mediated allergic reaction Characterised by § Pruritus, urticaria, bronchospasm, facial swelling and hypotension § Abdominal pain, nausea, vomiting and diarrhoea are also relatively common in platinum drug-induced anaphylaxis One study of 272 patients receiving oxaliplatin found 48 (18%)patients who developed infusion reaction despite prevention regimen of famotidine and dexamethasone 3 Another study suggested benefit from higher doses of dexamethasone in conjunction with H 1 and H 2 receptor blockers (7% vs. 20% reaction rate)
- Slides: 18