Collective Mental Health Response How can the community











- Slides: 26

Collective Mental Health Response How can the community pull together to best support peoples’ mental well being?

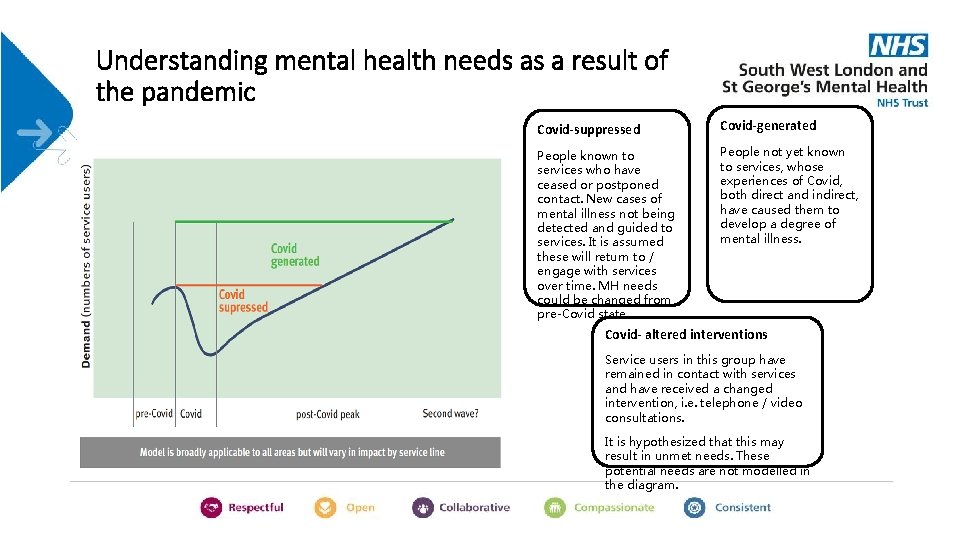
Understanding mental health needs as a result of the pandemic Covid-suppressed Covid-generated People known to services who have ceased or postponed contact. New cases of mental illness not being detected and guided to services. It is assumed these will return to / engage with services over time. MH needs could be changed from pre-Covid state People not yet known to services, whose experiences of Covid, both direct and indirect, have caused them to develop a degree of mental illness. Covid- altered interventions Service users in this group have remained in contact with services and have received a changed intervention, i. e. telephone / video consultations. It is hypothesized that this may result in unmet needs. These potential needs are not modelled in the diagram.

Covid-Suppressed Need • Joint promotion of mental health services with SWL CCG - social media - radio - text messaging • Checks on recently discharged patients • ORCHID Emergency Unit

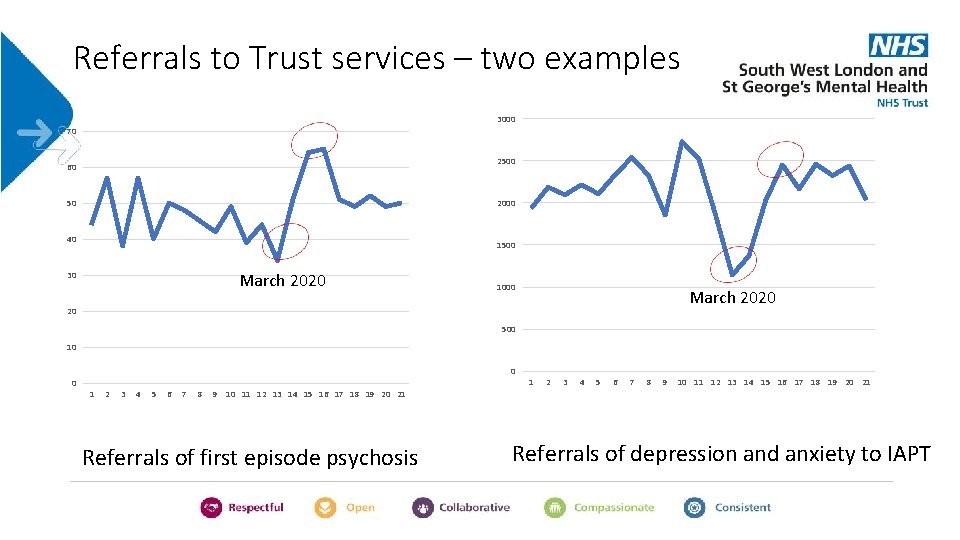
Referrals to Trust services – two examples 3000 70 2500 60 2000 50 40 1500 March 2020 30 1000 March 2020 20 500 10 0 0 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 Referrals of first episode psychosis Referrals of depression and anxiety to IAPT

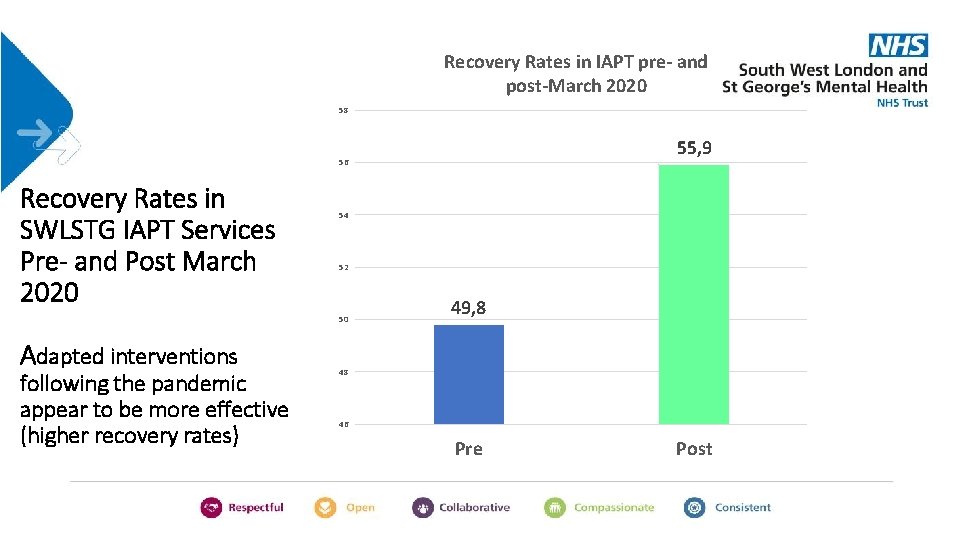
Recovery Rates in IAPT pre- and post-March 2020 58 55, 9 56 Recovery Rates in SWLSTG IAPT Services Pre- and Post March 2020 54 52 50 Adapted interventions following the pandemic appear to be more effective (higher recovery rates) 49, 8 48 46 Pre Post

Forecasting needs and risks in the UK Source: Centre for Mental Health October, 2020 1 Population group People with pre-existing mental health conditions Mental health condition Research Percentage of Predicted extra determined people who demand for increase may access services (percentage) services (% of population group ) Moderate-severe anxiety 67% 50% 33% Moderate-severe depression 56% 61% 34% Amber Confidence Rating

Forecasting needs and risks in the UK Population group Mental Health Condition Research determined increase (%) Predicted extra demand for services (% of population group) General population no pre-existing MHPs Mod-sev anxiety 16% 4% Mod-sev depression 22% 6% Healthcare workers PTSD High psychological distress 14% 45% 3. 5% 10% People recovering from severe Covid-19 Anxiety 40% 10% Depression 30% 7. 5% PTSD 24% 6%

Forecasting needs and risks in the UK* Population group Mental Health Condition Research determined increase (%) Predicted extra demand for services (% of population group) Bereaved Prolonged grief disorder PTSD 10% 2. 5% 14% 3. 5% Major Depressive Disorder 8% 2% People economically affected by COVID

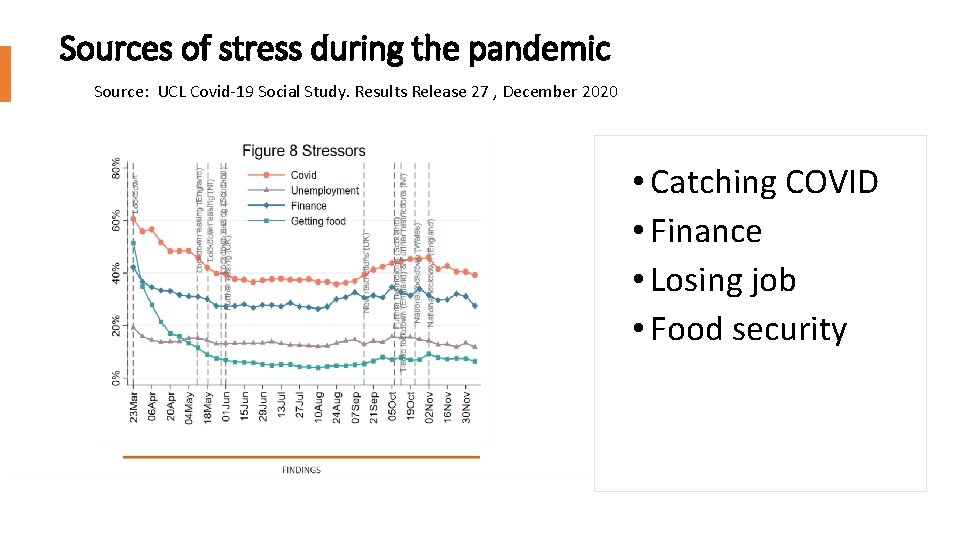
Sources of stress during the pandemic Source: UCL Covid-19 Social Study. Results Release 27 , December 2020 S • Catching COVID • Finance • Losing job • Food security

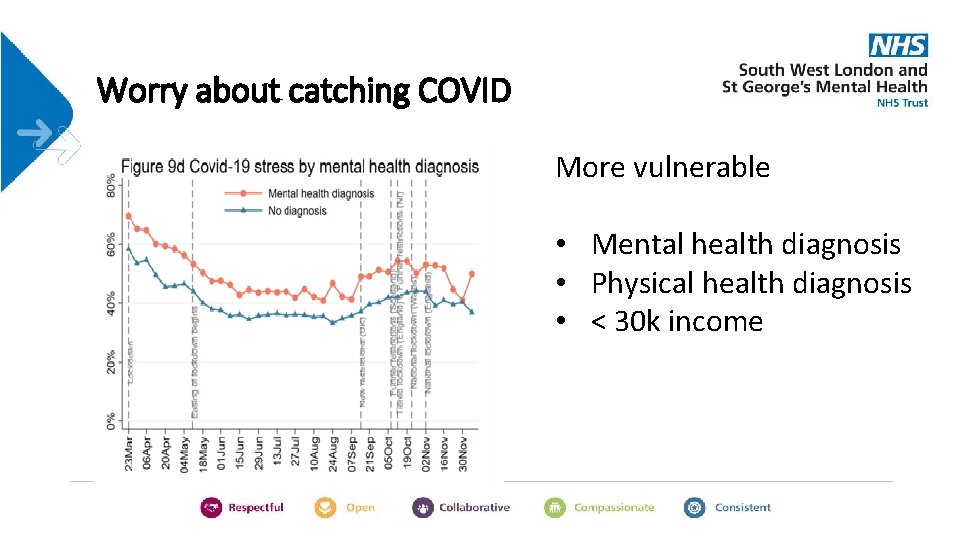
Worry about catching COVID More vulnerable • Mental health diagnosis • Physical health diagnosis • < 30 k income

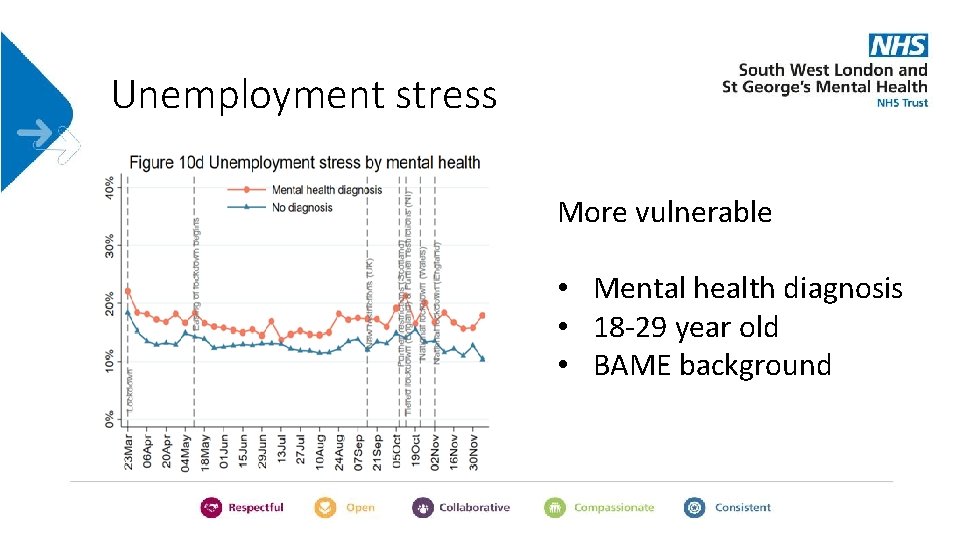
Unemployment stress More vulnerable • Mental health diagnosis • 18 -29 year old • BAME background

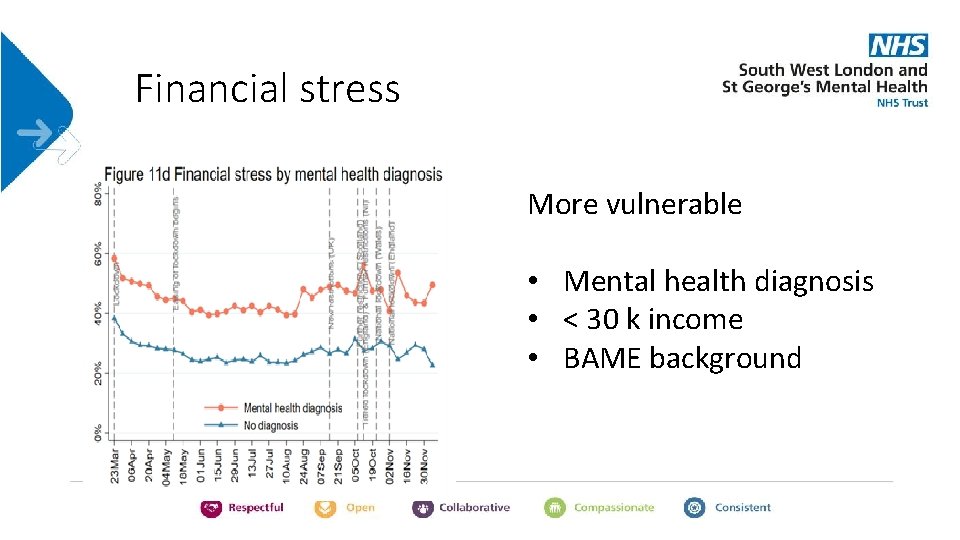
Financial stress More vulnerable • Mental health diagnosis • < 30 k income • BAME background

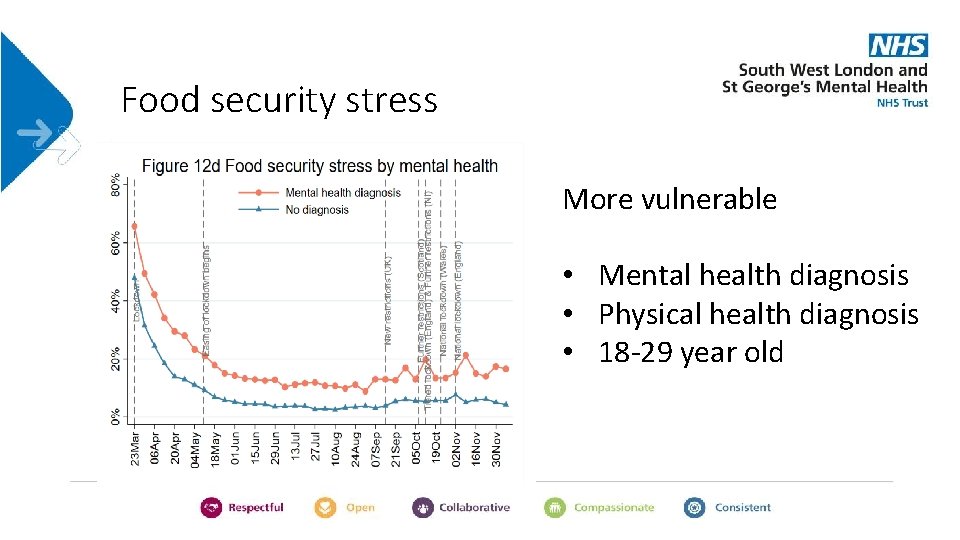
Food security stress More vulnerable • Mental health diagnosis • Physical health diagnosis • 18 -29 year old

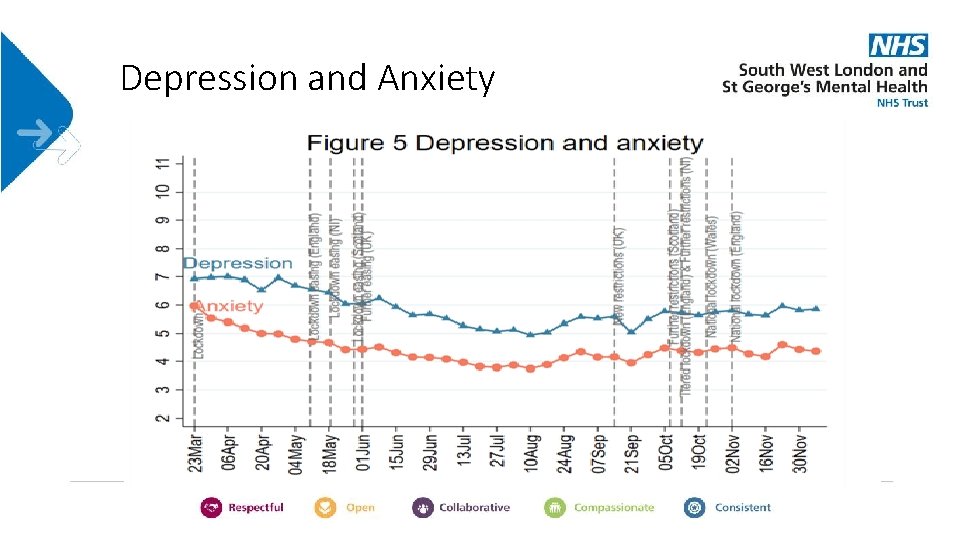
Depression and Anxiety

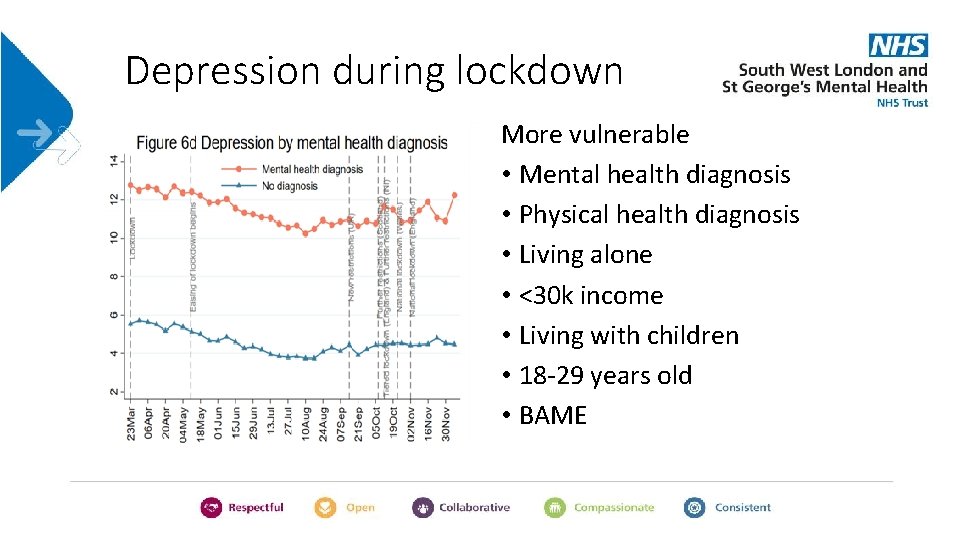
Depression during lockdown More vulnerable • Mental health diagnosis • Physical health diagnosis • Living alone • <30 k income • Living with children • 18 -29 years old • BAME

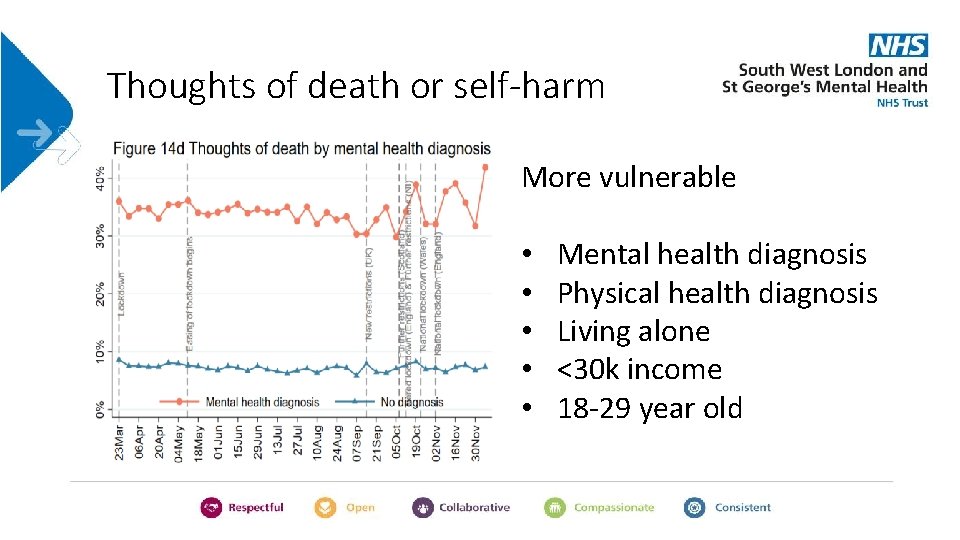
Thoughts of death or self-harm More vulnerable • • • Mental health diagnosis Physical health diagnosis Living alone <30 k income 18 -29 year old

Depression and Anxiety More vulnerable • Mental health diagnosis • Physical health diagnosis • Lower incomes • BAME backgrounds • Living alone • Younger people

What about trauma? PTSD • Health Care Workers • People in ICU • Bereaved

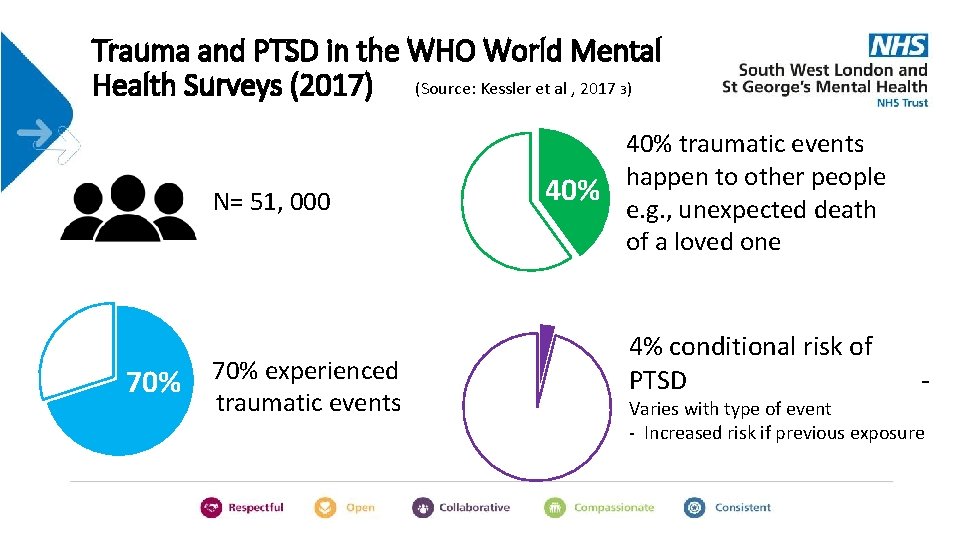
Trauma and PTSD in the WHO World Mental Health Surveys (2017) (Source: Kessler et al , 2017 ) 3 40% traumatic events happen to other people 40% e. g. , unexpected death of a loved one N= 51, 000 70% 70% experienced traumatic events 4% conditional risk of PTSD 70% - Varies with type of event - Increased risk if previous exposure

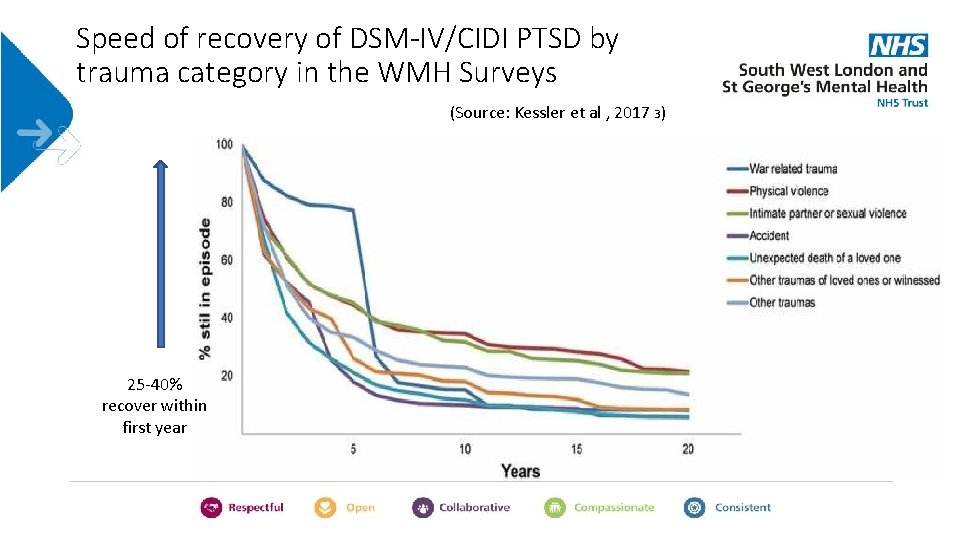
Speed of recovery of DSM-IV/CIDI PTSD by trauma category in the WMH Surveys (Source: Kessler et al , 2017 3) 25 -40% recover within first year

Trauma and increased risk of mental health problems This slide shows the increased risk a number of mental health and related problems which people experience following exposure to traumatic events. The number in each circle represents the increase in risk of this type of problem. (Source: Lewis et al, 2019) 4 Suicide attempt 4. 85 Trauma Network traumas* Physical assault Witnessing assault Bullying Sexual assault Threat Accident Illness Witnessing threat 3. 52 2. 64 Other drug dependence Psychotic symptoms Cannabis dependence 2. 25 2. 21 * Network traumas refer to traumatic events affecting someone in the participant’s network that they learned details of, but did not directly experience or witness Self harm 3. 61 Generalized anxiety Majordisorder 2. 16 2. 21 depressive disorder Alcohol dependence

The MH impact of COVID-19 Following humanitarian disaster* Increase in Key Issues • Severe MHPs • PTSD Maintain and increase access to SMHS • Depression and anxiety • Substance abuse • Domestic violence • Change in help seeking behavior • Distress (some may have acute stress disorder) • Isolation and loneliness Some people at increased risk of problems (those who are always more vulnerable to stressors) Most people can be helped through supportive , safe relationships with others they trust Most people will show no enduring negative effects Multi-sectoral &, interagency framework • effective coordination across 4 domains of intervention (next slide) • provide acute and longterm focus • mobilise existing resources that can provide a sustained response • target those who are more vulnerable • identify useful practices • flag potentially harmful practices • clarify how different approaches complement one another IASC Inter-Agency Standing Committee

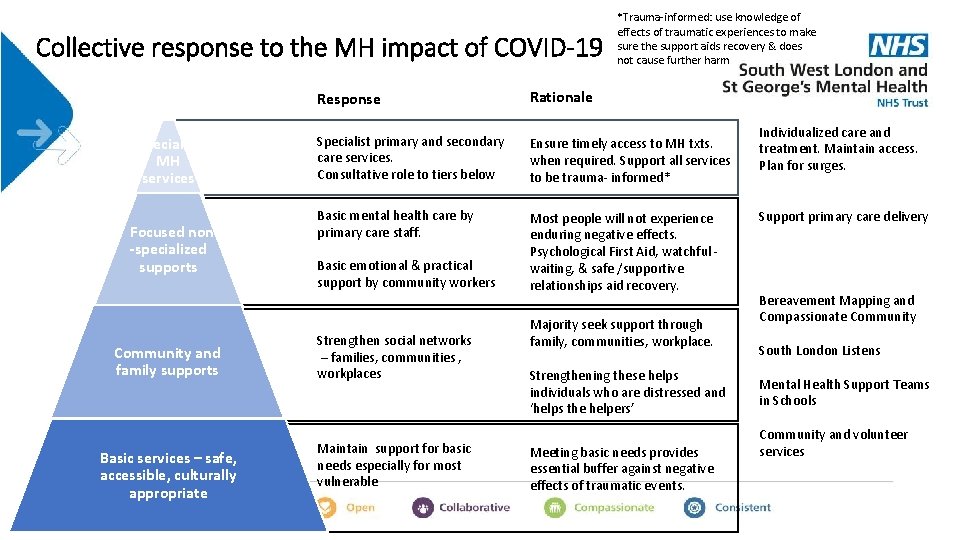
Collective response to the MH impact of COVID-19 Specialist MH services Focused non -specialized supports Community and family supports Basic services – safe, accessible, culturally appropriate *Trauma-informed: use knowledge of effects of traumatic experiences to make sure the support aids recovery & does not cause further harm Response Rationale Specialist primary and secondary care services. Consultative role to tiers below Ensure timely access to MH txts. when required. Support all services to be trauma- informed* Basic mental health care by primary care staff. Most people will not experience enduring negative effects. Psychological First Aid, watchful waiting, & safe /supportive relationships aid recovery. Basic emotional & practical support by community workers Strengthen social networks – families, communities , workplaces Maintain support for basic needs especially for most vulnerable Majority seek support through family, communities, workplace. Strengthening these helps individuals who are distressed and ‘helps the helpers’ Meeting basic needs provides essential buffer against negative effects of traumatic events. Individualized care and treatment. Maintain access. Plan for surges. Support primary care delivery Bereavement Mapping and Compassionate Community South London Listens Mental Health Support Teams in Schools Community and volunteer services

Community stress and resilience: key areas to focus 1. Essential to ensure peoples basic needs are met: • Food, hydration, medical treatments, sleep and rest- self care, hope and routine 2. Build upon peoples resilience- most people will recover (Importance of not pathologizing) • Spaces to talk to each other about how we are coping and what works. Talk about community stress (Rather than collective trauma) • Being clear about the fact that people will potentially feel stresses, anxious and/or depressed at moments during this time, and that when this tips into being a more persistent feeling that there is help readily available (see next slide) • Bereavement support and counselling • Mental health/psychological first aid https: //www. futurelearn. com/courses/psychological-first-aid-covid 19/1? utm_campaign=fl_phecovidpsych_2020&utm_medium=futurelearn_organic_pres srelease&utm_source=fl_pr_outreach

Six key actions Keep mental health services accessible & trauma-informed Continue to plan for surges in demand Support primary care to continue delivering good mental health care Prioritize our most vulnerable Strengthen families, workplaces, communities - support, safe, trust Meet basic needs - buffer against stress

References 1. Covid-19 and the nation’s mental health: Forecasting needs and risks in the UK. Centre for Mental Health, October 2020 2. Fancourt, D. , Bu, F. , Wan. Mak, H. & Steptoe, A. University College London Covid 19 Social Study. Results Release 27. December 2020 3. Kessler, R. C. , Aguilar-Gaxiola, S. Alonso, J. et al. (2017). Trauma and PTSD in the WHO World Mental Health Surveys. European Journal of Psychotraumatology, Oct. 27: 8 (Supp 5) 4. Lewis, S. , Arseneault, L. , Caspi, A. et al. (2019). The epidemiology of trauma and post-traumatic stress disorder in a representative cohort of young people in England Wales. Lancet Psychiatry 2019; 6: 247– 56