Collapsing Trachea Mark Bohling DVM Diplomate American College

Collapsing Trachea Mark Bohling, DVM Diplomate, American College of Veterinary Surgeons Assistant Professor of Surgery University of Tennessee College of Veterinary Medicine

What is Tracheal Collapse? • Normal airflow dynamics in respiration • Inspiration • Expansion of chest by muscles of respiration • Pressure gradient - chest negative • Effect on the air conduit: Ø Thorax - expansion Ø Neck - compression • Expiration • Reverse effects

History of Collapsing Trachea in Veterinary Medicine • Described as early as 1960 • Review of early treatments • Single plastic tube • Ventral chondrotomy • Modified ventral chondrotomy • Dorsal membrane plication

Tracheal Collapse in Other Species • Tracheal collapse in human beings • History • Dates to 1930’s • Similarities • Softening of tracheal cartilage • Lateral collapse (same as dorsoventral in dogs) • Differences • Classification Ø Primary vs secondary collapse Ø Pediatric vs adult collapse

Tracheal Collapse in Other Species • Tracheal collapse in large animals • Horses • Congenital • Secondary to laryngeal paralysis • Cattle • Acquired neonatal • Tracheal collapse in birds • Bordetella avium in turkeys

Tracheal Collapse in the Dog • Miniature breeds • Middle aged to older • Other risk factors • More pronounced in obese individuals
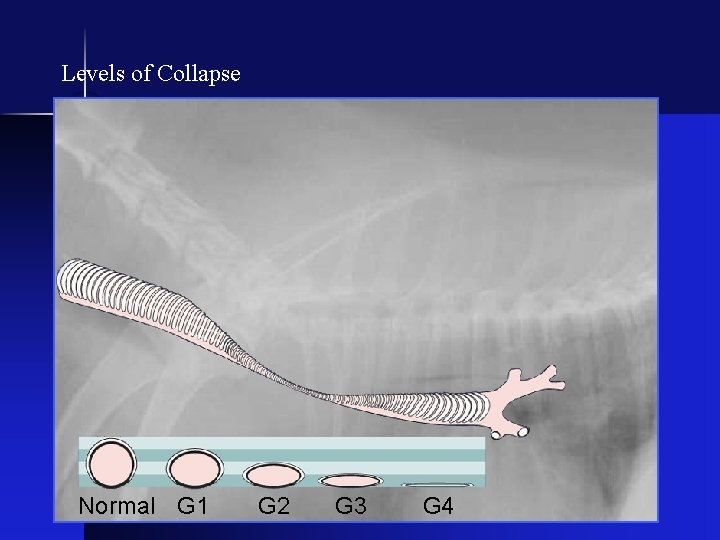
Levels of Collapse Normal G 1 G 2 G 3 G 4
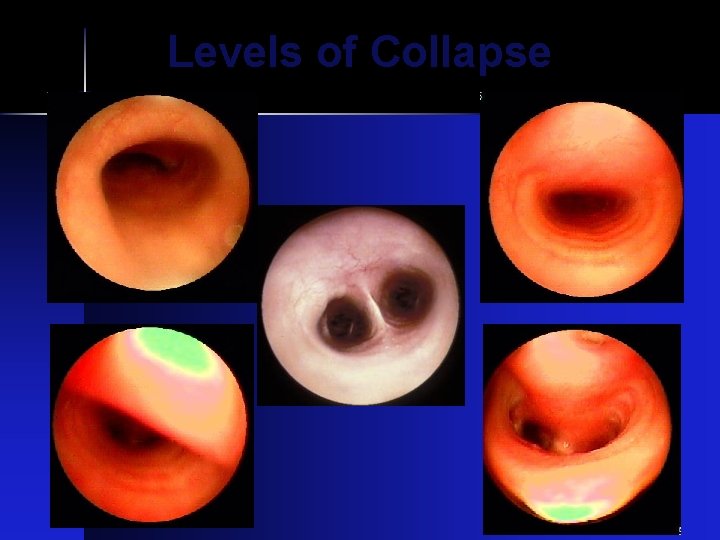
Levels of Collapse

Clinical Signs • Chronic, dry nonproductive cough (honking) • Intermittent dyspnea (worsens with excitement) • Cyanosis & syncope in severe cases • Inspiratory/ expiratory dyspnea • Prone to heat stroke

Clinical Signs

Pathophysiology • Disease causes the trachea rings to weaken • Dorsal ligament and trachealis muscle weaken and stretch • Trachea changes from oval tube to a flattened conduit

Etiology • Congenital • Nutritional tracheomalacia • Obesity • Bacterial infection • Neurologic • Chronic airway disease • Idiopathic – “who knows why”

Diagnosis • Tracheal palpation • Radiographs (inspiratory / expiratory ) • Fluoroscopy • Tracheoscopy
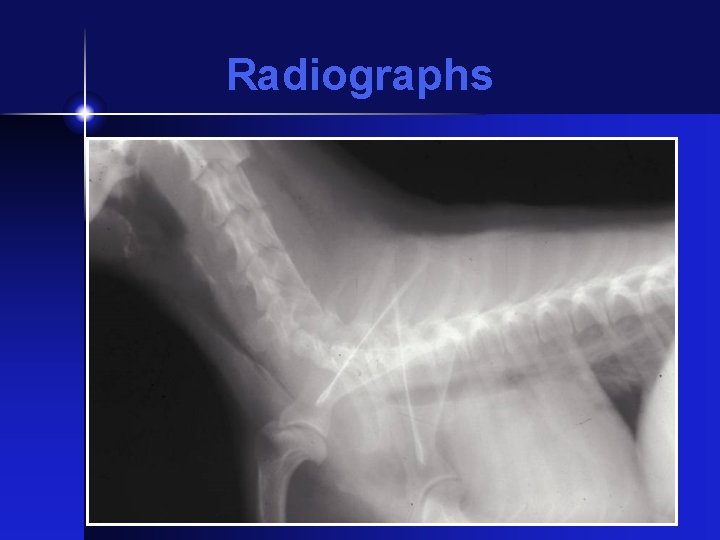
Radiographs
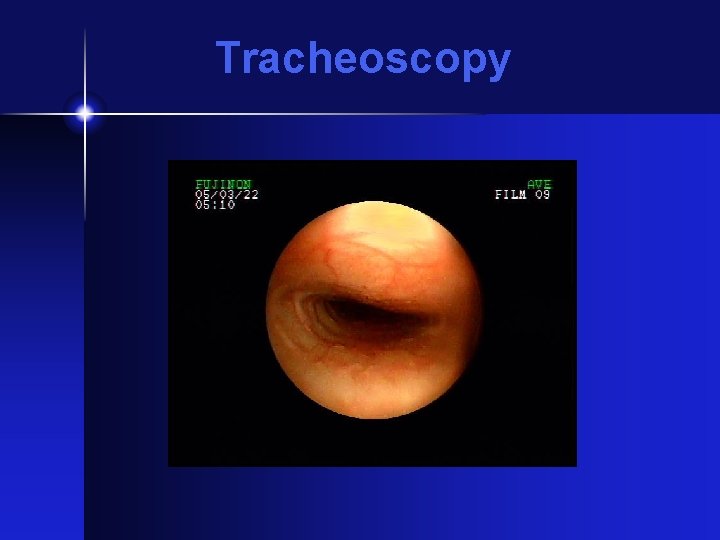
Tracheoscopy

Medical Management • Cough suppression (Hydrocodone, butorphanol) • Bronchial dilators (Aminophylline, terbutaline) • Sedation (Acepromazine) • Weight loss

Medical Management • Help control symptoms • Can not be cured • Disease usually progressive
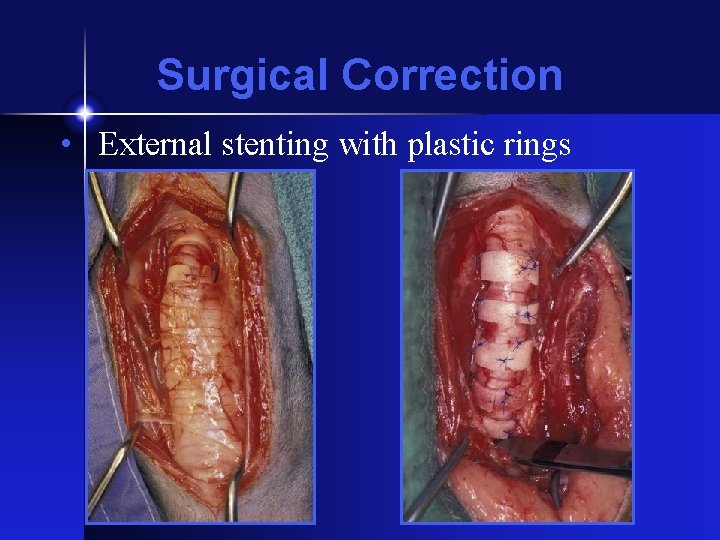
Surgical Correction • External stenting with plastic rings
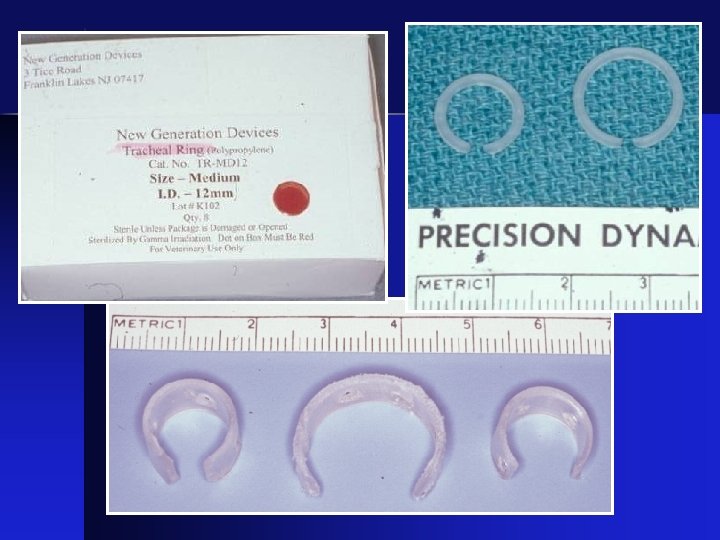
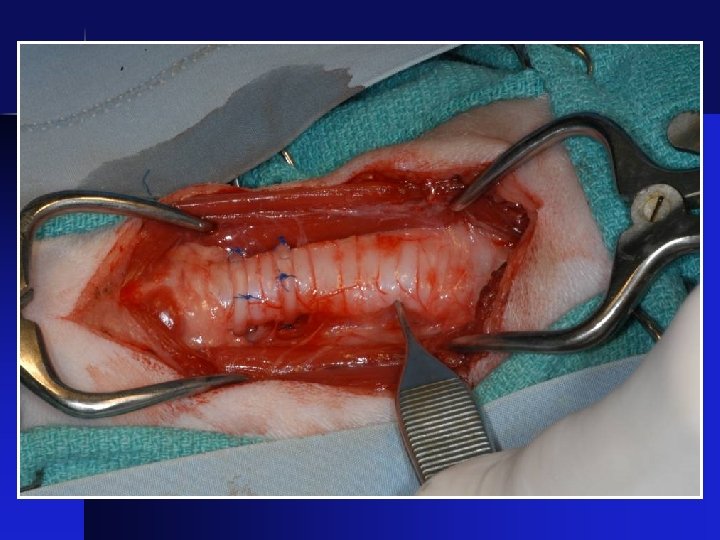
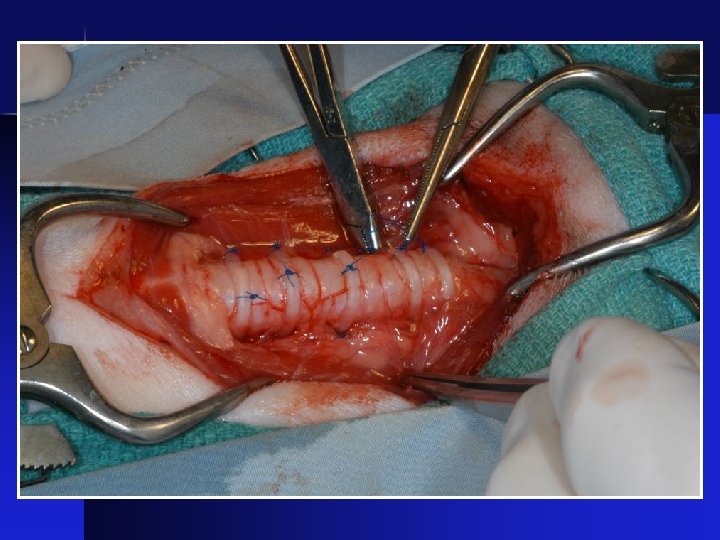
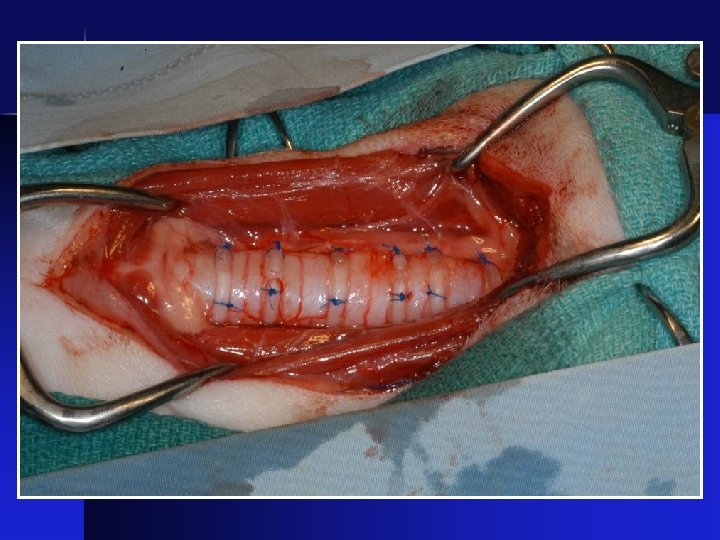
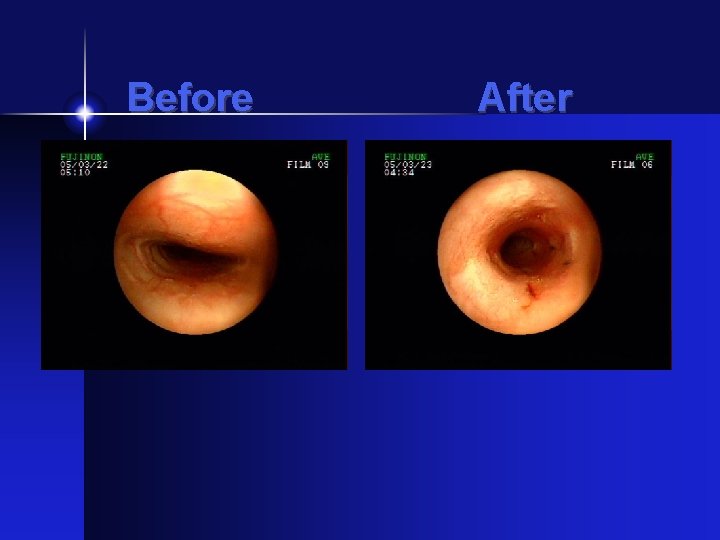
Before After
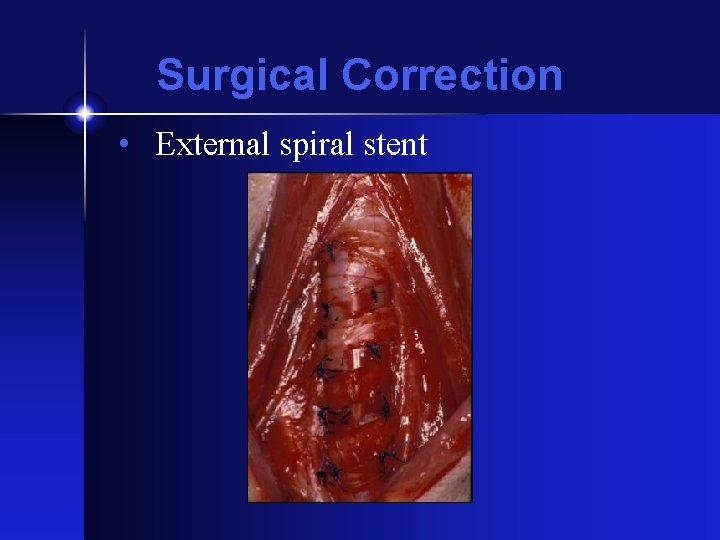
Surgical Correction • External spiral stent
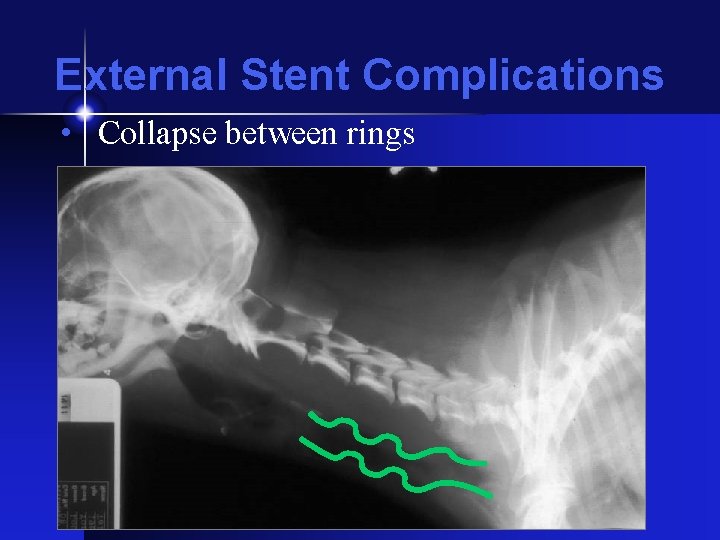
External Stent Complications • Collapse between rings
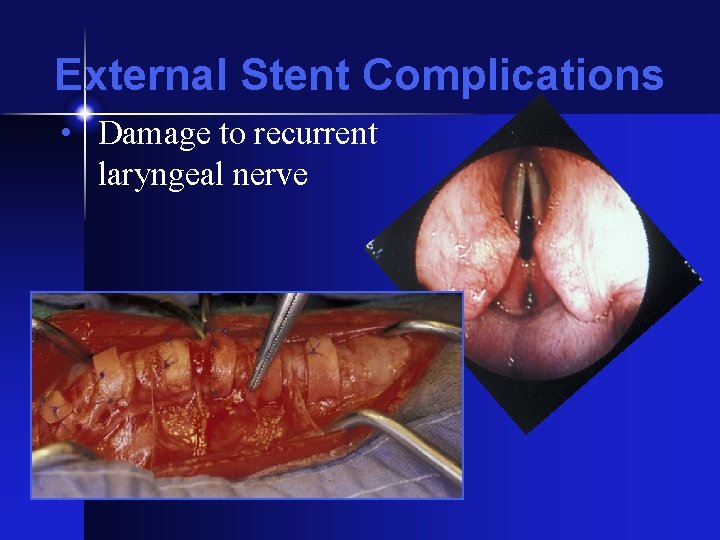
External Stent Complications • Damage to recurrent laryngeal nerve
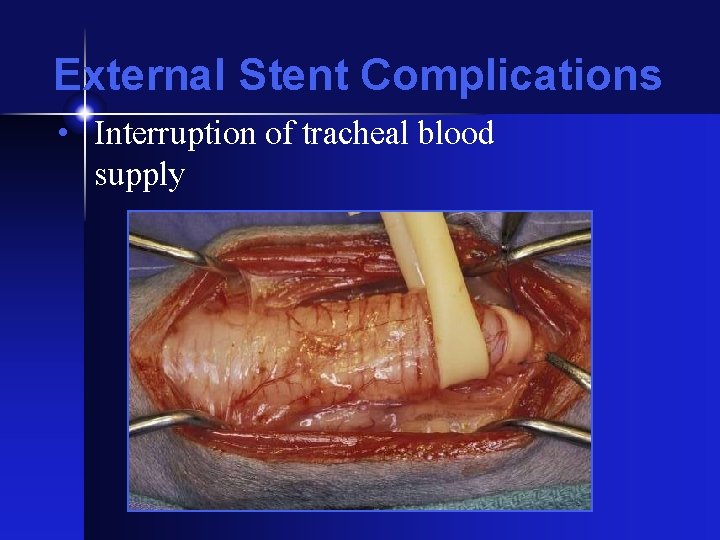
External Stent Complications • Interruption of tracheal blood supply

Internal Stenting • • • What is a stent? History of stenting History of tracheal stenting Modern stents and stent materials Stents in veterinary medicine

® Ultraflex Stent • Radiopaque, self-deployed • 4 - 8 cm length, 10 - 20 mm diameter • Made of nitinol (nickel-titanium alloy) • Proximal or distal deployment • Single strand, open loop knitted design (flexible, contourable) Boston Scientific/ Microvasive.
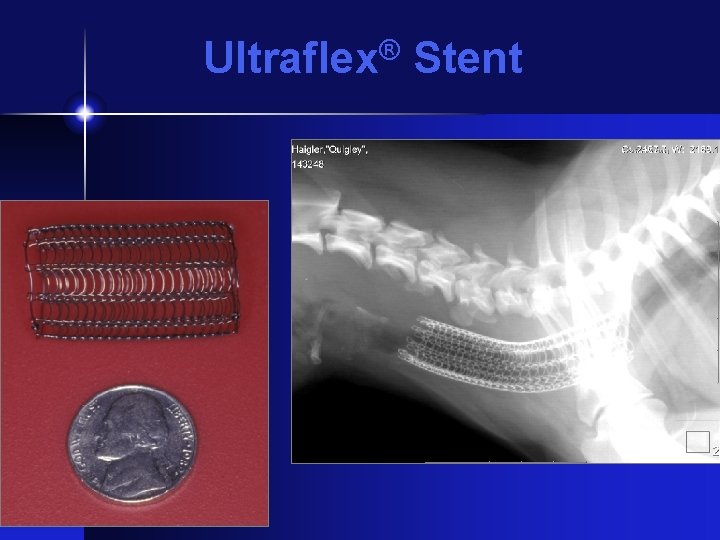
Ultraflex® Stent
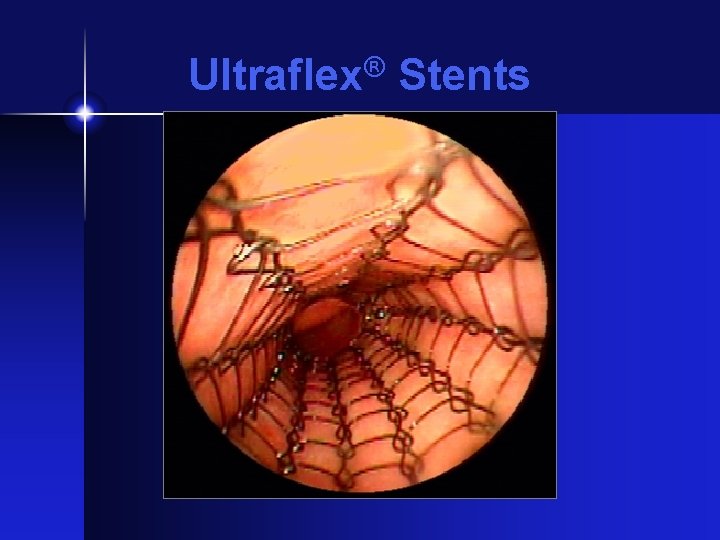
Ultraflex® Stents

Smart. Stent® • • Nitinol tube Laser cut No overlapping wires Less breakage in human vascular applications • Cordis Endovascular®

Infiniti Stent • Also nitinol • Single woven wire • Only stent produced exclusively for vet use • Claims as yet unproven
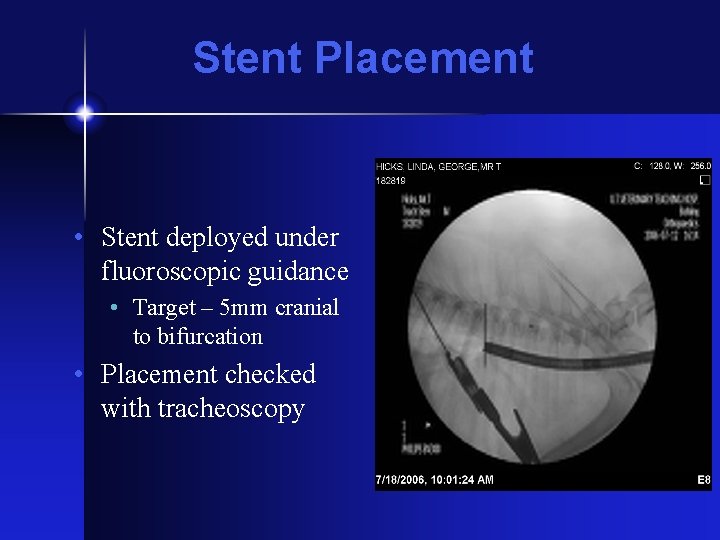
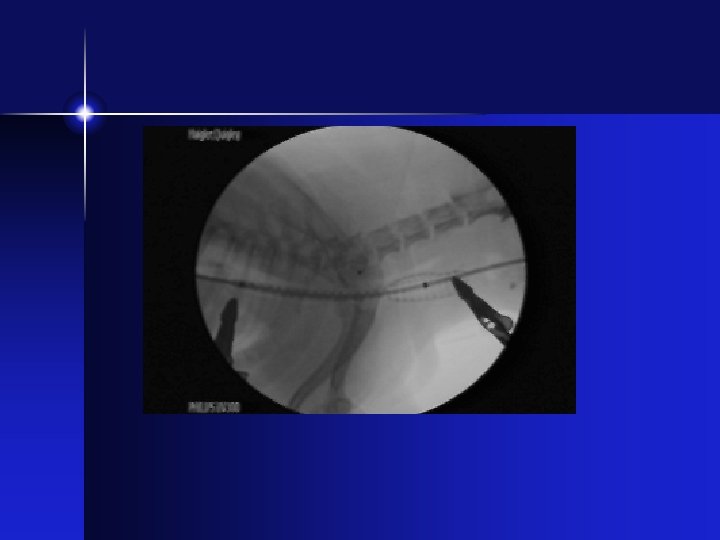
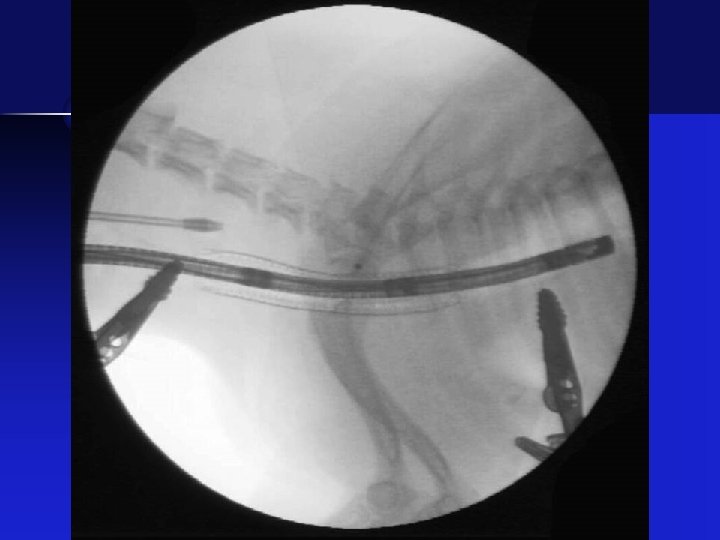
Stent Placement • Stent deployed under fluoroscopic guidance • Target – 5 mm cranial to bifurcation • Placement checked with tracheoscopy
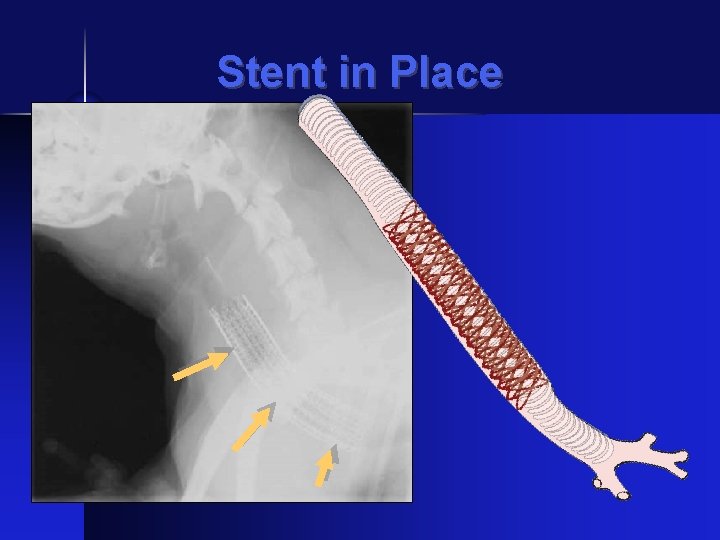
Stent in Place
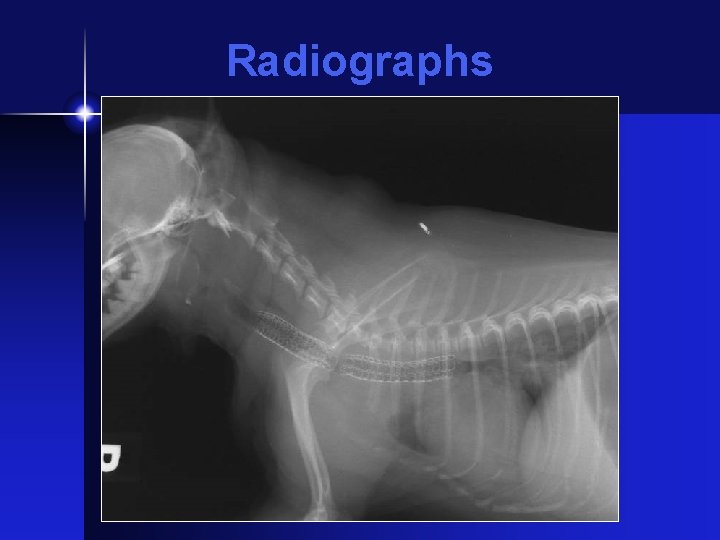
Radiographs

Postoperative Care • • • Perioperative antibiotics Corticosteroids for 7 days Sedation Cough suppression 24 hours oxygen if needed Humidification
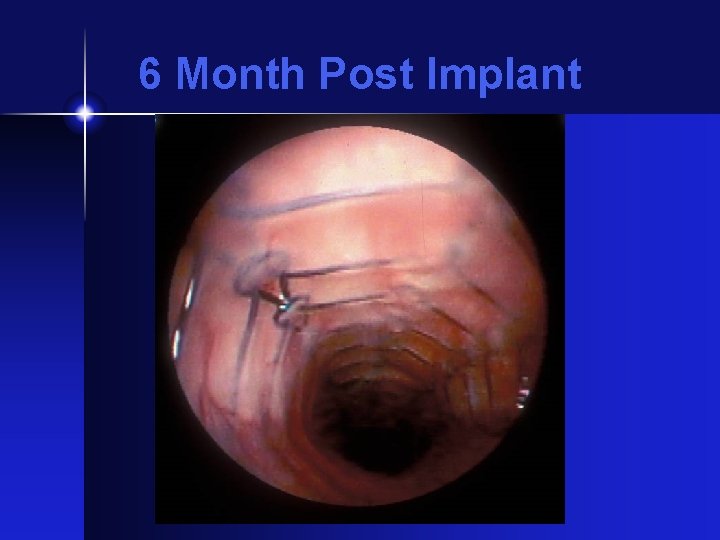
6 Month Post Implant

Stent Results • The little girl with the curl syndrome… • Good outcomes… • Immediate improvement • Breathing near normal • Mild chronic cough • And the not-so-good outcomes…

Stent Complications • Stent fracture • Granulation in stent • Tracheal exudate • Additional collapse at ends of stent
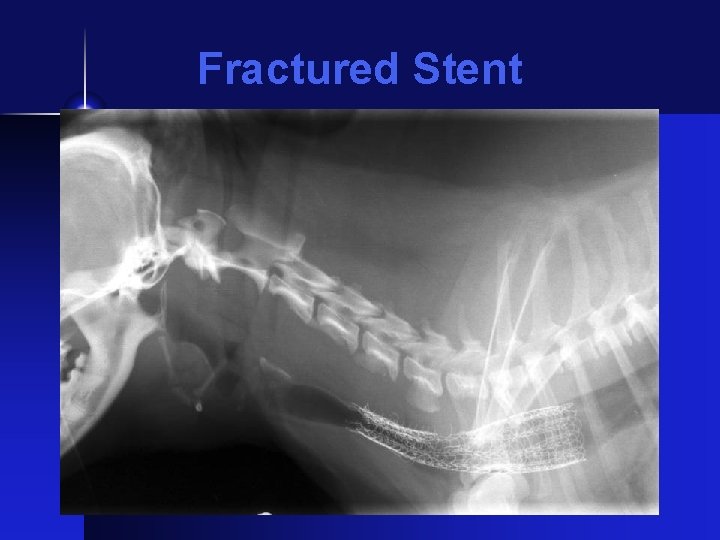
Fractured Stent
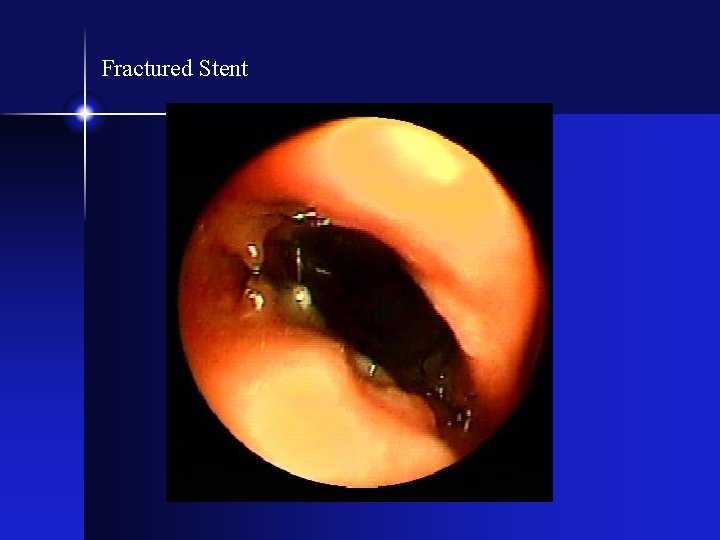
Fractured Stent

Stent Fracture • Originally thought to be due to bending stresses • All brands/types of nitinol stents can fracture - there is NO unbreakable stent • At this time, removal is best option - BUT not for the fainthearted!
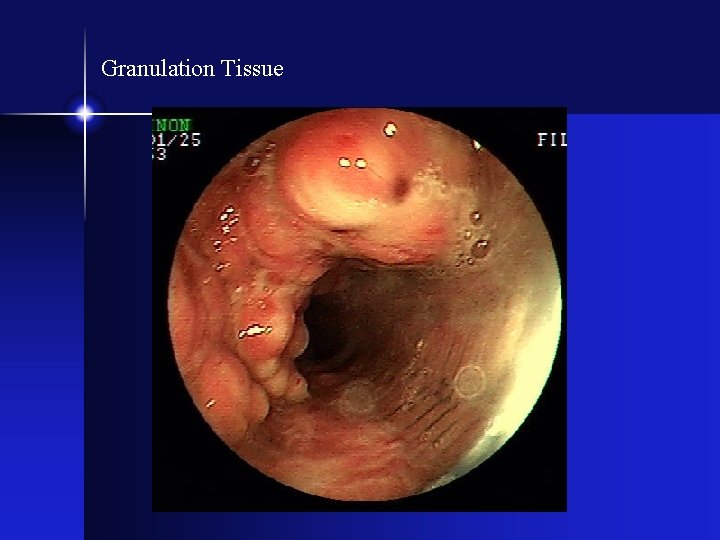
Granulation Tissue
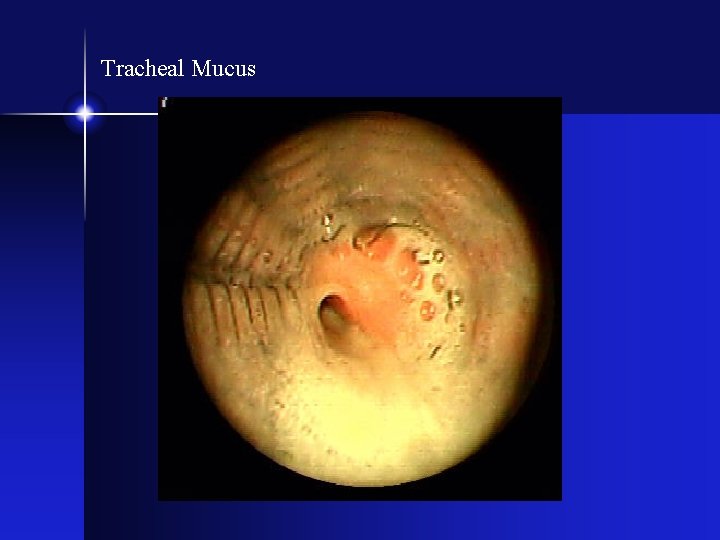
Tracheal Mucus
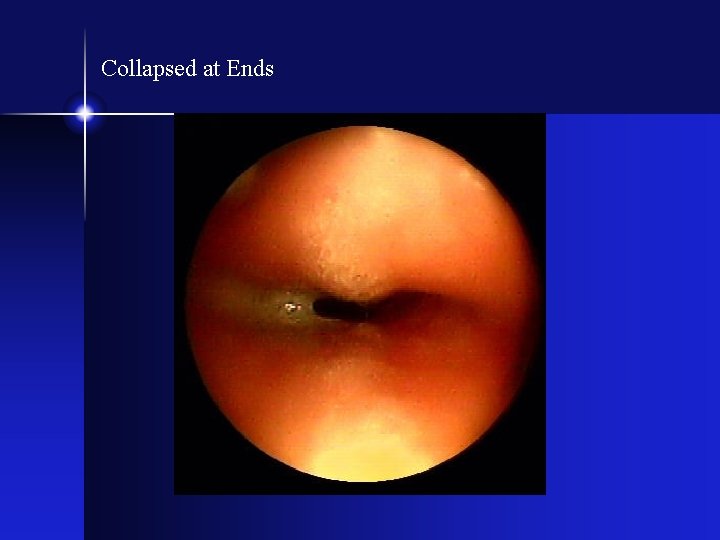
Collapsed at Ends
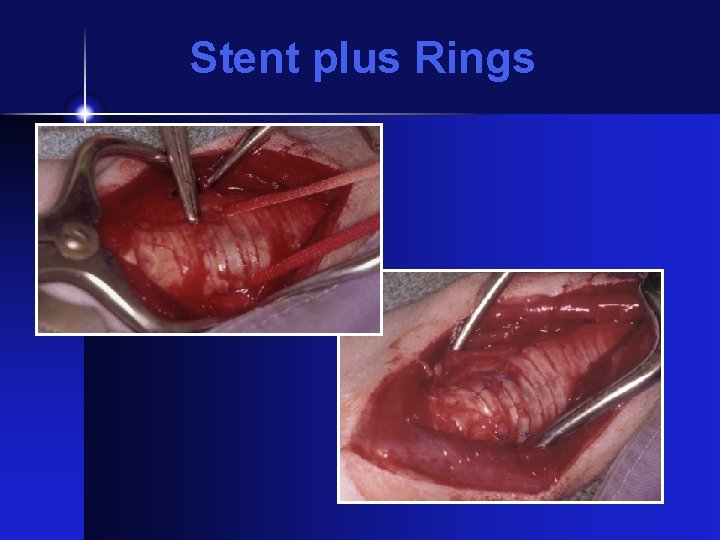
Stent plus Rings

Stent Advantages • Preserves tracheal blood supply • Preserves recurrent laryngeal nerve • Continuous tracheal support • Easy deployment • Multiple, sequential deployment

Rings vs. Stents • • • Cost to client (stent more expensive) Stents are easier and quicker Complication rate similar Neither cure, only control symptoms Stent placement requires expensive equipment • Rings require surgical expertise • Lack of proper size stent

A “typical” case with tracheal rings • Day 1: Preop workup (bloodwork, radiographs, tracheoscopy) • Day 2: Surgery • Postop recovery in ICU • Day 3: Still in ICU • Day 4: Discharged from hospital • Home monitoring – continue medical therapy 2 – 4 weeks • Recheck time variable, depends on outcome • Long term outcome usually good, but…

A “typical” case with tracheal stent • Day 1: Workup as for rings. Order stent from supplier • Day 2: Stent arrives (usually). Stent is placed in a 30 minute procedure and patient recovers in ICU • Day 3 -4: Recovery in ICU • Day 5: Discharge from hospital • Home care for 2 -4 weeks • Re-check tracheoscopy at one month to check if stent is embedded

Miss Piggy - Stent disaster case #1 • Signalment: Miss Piggy • 6 year old spayed female Yorkie • Body weight 13 lbs (BCS 8/9!!) • Grade III/VI heart murmur • History: • Coughing for past 2 years, getting worse past yr • Presented to emergency clinic Saturday night • Unable to breathe, cyanotic • Oxygen dependent

Miss Piggy • Presentation at UT • Still oxygen dependent • Tracheoscopy findings: • Cervical - Grade 3 entire length • Thoracic - Grade 3 -4 entire length • Left main bronchus Grade 2 -3 • Plan: stent entire trachea • Poor anesthetic risk • Guarded prognosis given

Miss Piggy • Stent placement • Thoracic stent 1 cm cranial to carina • 5 mm overlap at thoracic inlet • Cervical stent 1 cm caudal to cricoid

Miss Piggy • Postop first 24 hours • Doing well in oxygen • Next day… • Trial period out of oxygen - - cough and cyanosis • Back to oxygen and medical mgmt • Antitussives • Bronchodilators

Miss Piggy • 3 rd postop day • Brief trial out of oxygen - - same result • Still looks good in oxygen • 4 th postop day • • 4 am “can’t get comfortable” 7 am - 7 pm: awake all day 9 pm: lung sounds getting “harsh” 11 pm: crackles ausculted

Miss Piggy • 5 th day…. • Early am hours - No response to bronchodilators or diuretics • Patient very tired, has not slept in 24 hours • 9 am - respiratory failure

Stent disaster #2 - Tuffy • Signalment: • 4 year old male castrated Yorkie • BW 8 lbs, BCS 6/9 • History: • Started at 2 years old • Now coughs at slightest exertion • Cyanotic with mild exercise
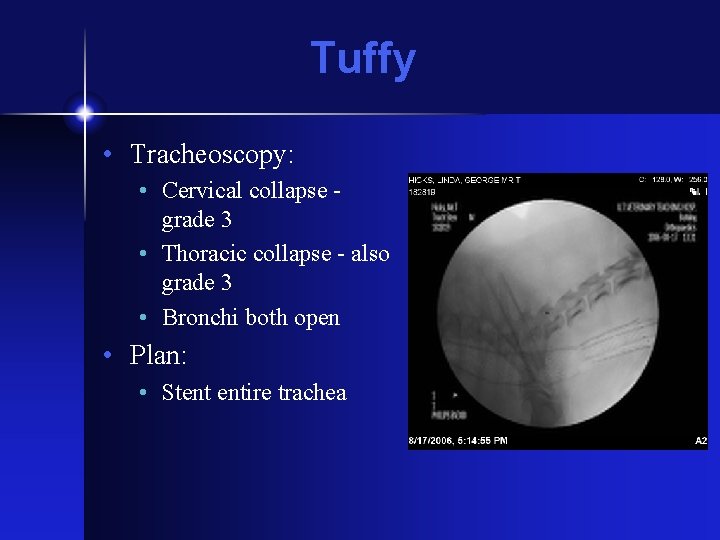
Tuffy • Tracheoscopy: • Cervical collapse grade 3 • Thoracic collapse - also grade 3 • Bronchi both open • Plan: • Stent entire trachea
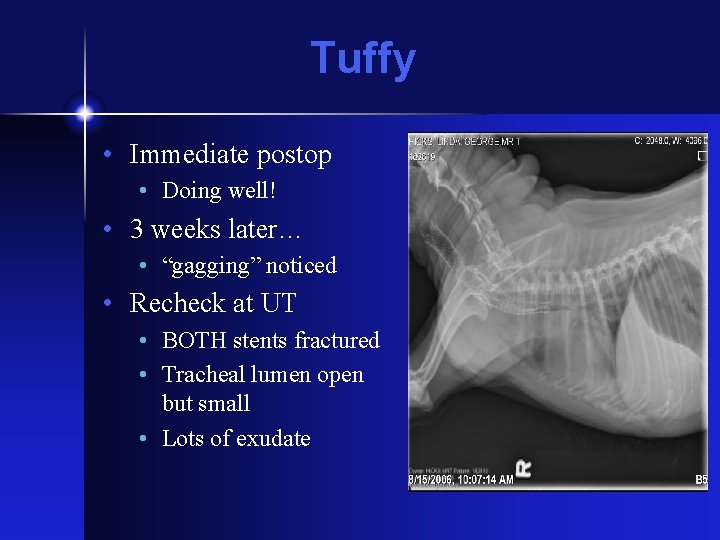
Tuffy • Immediate postop • Doing well! • 3 weeks later… • “gagging” noticed • Recheck at UT • BOTH stents fractured • Tracheal lumen open but small • Lots of exudate

What next? • Immediate plan • Stabilize his condition • Antibiotics • Some antitussives • Definitive plan • Stent removal • Re-stent over the broken ones

Tuffy – the outcome • • Survived the procedure! Immediate improvement in breathing Went home doing well, but some cough Continued to improve • Still coughs some • Overall quality of life – better than before • Cost to owner: $5 K+ total, lots of gray hair!

Future Needs • Immediate needs: • Improved surgical treatment options • Less breakable stents • Improved rings - can we go intrathoracic? • Improved medical management options • Cough suppression with less sedation • Tracheal cartilage - can malacia be arrested?

Future Needs • Long-term needs • Greater understanding of the etiology of this process • What is happening at the cellular and molecular level? • Identification of molecular/genetic marker(s) • Creation of a breed registry for this disease • Apparent genetic cause • Can we “breed it out”?

Special thanks to: • • Dr DJ Krahwinkel Sue Schwarten Danielle Browning UT photo and media services • Linda Hicks and Mr T
Thank you – any questions?
- Slides: 70