Collaboration between Physicians Nurse Practitioners and Physician Assistants

Collaboration between Physicians, Nurse Practitioners, and Physician Assistants X Rachel Korynoski

Medical History • The demand for non-Physician Healthcare Providers such as Nurse Practitioners and Physician’s Assistants came about in similar circumstances the healthcare profession is facing today during the mid 1960 s through the 1980 s. • Healthcare began to change after WWII and began to shift from office based practice to hospital based practice with more professions becoming more specialized. • This specialization of Physicians contributed to the lack of Physicians available to the poor, rural public. • In the 1960 s, healthcare costs were rising after Medicare and Medicade were passed and there was a Physician shortage (like today). • Organizations such as the American Medical Association’s efforts were slow and didn’t make a difference (like today). • Many poor and ill patients were in need of care, and nurses and physicians were willing to help advance themselves to meet their needs. • Loretta Ford and Henry Silver worked together to form the NP profession originally meant to treat children, but which developed into what it is today due to particular circumstances/need, • Future NPs who were nurses at the time, worked with Physicians and patients, “who understood [their] promise and potential” to gain support and federal funding for more education (“Nurse Practitioners : The Evolution and Future of Advanced Practice”). • They received funding from private foundations such as the Robert Wood Johnson, Commonwealth, and Clinical Nurse Scholars foundations as well as the 1964 Nurse Training Act • Lawyers and Physicians worked together to set up a legislative model so that PAs could work under the supervision of Physicians. • “program accreditation, national certification, and state regulation have insured quality educational standards and public accountability. ” • Physicians expanded PA’s roles so that as they gained more knowledge, their roles and autonomy could expand.
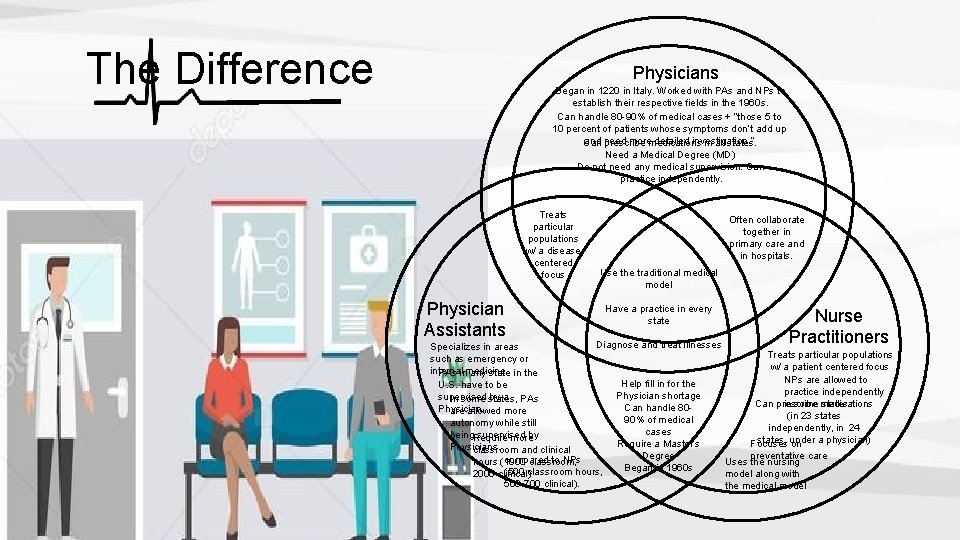
The Difference Physicians Began in 1220 in Italy. Worked with PAs and NPs to establish their respective fields in the 1960 s. Can handle 80 -90% of medical cases + “those 5 to 10 percent of patients whose symptoms don’t add up and need moremedications detailed investigation. ” Can prescribe in all states. Need a Medical Degree (MD) Do not need any medical supervision. Can practice independently. Treats particular populations w/ a disease centered focus Physician Assistants Often collaborate together in primary care and in hospitals. Use the traditional medical model Have a practice in every state Nurse Practitioners Diagnose and treat illnesses Specializes in areas Treats particular populations such as emergency or w/ a patient centered focus internal PAs inmedicine any state in the NPs are allowed to Help fill in for the U. S. have to be practice independently Physician shortage supervised by a PAs In some states, in some medications states. Can prescribe Can handle 80 Physician. are allowed more (in 23 states 90% of medical autonomy while still independently, in 24 cases being. Require supervised by more states, a physician) Require a Master’s Focuses under on Physicians. classroom and clinical Degree preventative care compared to NPs Uses the nursing hours (1000 classroom, Began in 1960 s (500 classroom hours, model along with 2000 clinical) 500 -700 clinical). the medical model

The Issues + Lack of Physicians to provide sufficient healthcare to those in low-income, disease prone areas. + No healthcare funding plans/govt. support + Lack of data/research on NP, PA, and Physician collaboration and combined and individual effectiveness + boundaries and misunderstandings between professions (ex: Physicians feeling threatened by NPs and PAs as they feel they’re acting as substitutes for Physicians) + “competing agendas” (ex: deciding which profession’s education should be funded) + organizational inadaptability to the constant changes in the medical field + Too much division between professions + NP’s and PA’s inability to practice independently in some states.

An Imbalance • “The federal government, as the largest employer of PAs and nurse practitioners, no longer requires direct supervision by physicians and instead has authorized a collaborative relationship among these health care providers” (“Physician Assistants: Collaboration and Care : Introduction. ”). • The Federal Government trusts PAs and NPs enough to practice on their own in branches of the government such as the Department of Veterans Affairs health care facility, Federal Bureau of Prisons, or any branch of the U. S. government. • “Community-based primary care provided outside of formal health facilities will need to be fully developed in low-income settings in order to achieve the United Nation’s sustainable development goal of universal access to health care by 2035” (“Physician Assistants: Collaboration and Care : Introduction. ”). • NPs are allowed to practice independently in some states. • PAs in any state in the U. S. have to be supervised by a Physician. • In some states, PAs are allowed more autonomy while still being supervised by Physicians. To catch up with NP autonomy, some PAs are in a collaboratory state with Physicians. • some argue there is only so much supervision an NP or PA can go other before they can’t grow individually or professionally • Change in these fields is inevitable and has/is already occurring. .

The Tests • In 2009, the Robert Wood Johnson Foundation Initiative on the Future of Nursing Committee was assigned the task of coming up with a plan on how to improve healthcare professions such as nurse practitioning. They decided that there needed to be: • More public and private funding for education • More workers and standards for them • According to The Nursing Profession Development, Challenges, and Opportunities: • “By the year 2020, an estimated 85, 000 additional practitioners will be needed. ” • The Institute of Medicine recommends restrictions against NPs and other non-physician providers be removed to make up for these shortages. • The American Medical Association, however, believes these restrictions should be kept and the public should be informed about the differences between Physician Providers and nonphysician providers.

Quality Care • Despite Physician’s worries that non-physician providers working independently would be a health risk because they could lack the diagnostic education and skills and may take cases less serious/not make referrals to specialists, studies have found … • NPs can provide 90% of the care required by children, and 80% required by adults. • “The research, however, has shown that NPs provide safe and effective care within their scope of practice, which is governed by protocols, and that they seek consultation appropriately. ” • Since the formation of the NP and PA professions in the 1960 s, various research and literature has been published that has supported non-physician’s quality of care. • A study conducted in 2000 and a follow up study by Mundinger ran 21 randomized trials to test the quality of care of NPs and Physicians in Primary Care, and they, “found that the “new professionals” provided primary care that was “indistinguishable from physician care. ”” • Brown and Grimes found that NPs took a more comprehensive medical history, scored higher on diagnostic accuracy than physicians, suggested more health advancing activities than Physicians, ordered more lab tests • Despite Physician’s worries that their jobs are going to be replaced by NPs/PAs: • NPs and Pas are unlikely to be replacing or taking Physician’s jobs because they provide where the need is. • The real issue is not whether non-Physician Providers can provide quality care, but whether they can practice independently to treat more of the patient population in need. • There’s no doubt that MDs have a higher education and more knowledge than NPs and Pas do, but each specializes in a different category than one another. If Nurse Practitioners and Physician Assistants can treat 90% of children’s ailments and 80% of adult’s ailments in primary care which constitutes the majority of patient’s medical needs, then why should their expertise and potentiality be debunked by a medical hierarchy?

Collaboration Benefits • Instead of full independence or supervision, collaboration between Physicians and non-Physician providers is suggested and supported. • A study into the Exploration of the collaborative relationship between physicians and nurse practitioners defined, “collaboration in the healthcare setting [as] a multifaceted process that calls for deliberate knowledge sharing and mutual accountability for patient care. ” Collaboration can be the sharing of knowledge or referring a patient to a fellow colleague. • Collaboration may decrease medical costs and hospital stay times while building professional relationships. • In a study conducted over a 12 month period they found that Nurse Practitioner E&M services cost 29% less than the costs of a Medical Doctor, 18% less for Part B, in-office expenses, and 11 -18% less for office visit costs and that Nurse Practitioners see less Medicare beneficiaries than physicians do. • Although Medicare expenses under NPs are allowed to be 85% of the fees physician’s fees which could account for physician’s services costing more, more NPs practicing would not cost Medicare anything and could actually save them 60 million dollars over 10 years according to a similar study conducted by the CMS Office of the Actuary. • Collaboration doesn’t have to be limited to dependence such as the counterargument suggests. An NP and an MD working together can be independent of one another methodically and in business, but still take a collaborative stance with each other, consulting one another’s medical opinion and support. • Supported by those who see how Physicians and Nurses’ varying focuses, (Physicians focus on science and anatomy, while Nurses focus on the social sciences and have, “more psychosocial concern for the patient, greater attention to the history of the patient, and less reliance on immediate prescribing of medication” ) “complement, ” one another. • Some argue that collaboration between non-Physician providers and Physicians would cause non-Physician providers to be more dependent on the Physicians. They want collaboration to ensure patient safety.

Collaborative Components • • • collaboration could possibly help lower diagnosis or treatment related mishaps that run higher with PAs and NPs because Physicians that have lower malpractice tendencies often work with surgeons and anesthesiologists. A study into collaboration between Physicians and non-physician providers increased as the proportion of patients with at least 1 chronic disease came in. • This collaboration can better care for those with chronic disease, save human resources, prevent professional divides, However, out of all the professions, Physicians and nonphysician providers collaborated the least with each other. • “Current and future challenges in primary care require a more integrated inter-professional collaboration instead of a task shift between general practitioners, ” and other professions and a clear definition of collaboration. The Institute of Medicine worked together to highlight the best methods and catalysts of collaboration which included, “member contributions, effective communication, shared decision making, and shared vision and values. ” • They observed that inter-professional teams who implemented these methods trusted one another and each member had a knowledge of his/her role. They didn’t enforce a medical hierarchy, but kept the focus on the patient. • Having the, “common interest, ” of the patient = more work done (if all team members have come to a consensus on what patient well-being is). • Providers who were happy in their job setting, especially with the people they were working with provided higher quality care which led to = > pay. • They published these findings in an article entitled Working in the Best Interest of Patients.

Nurse Physician Collaboration • Nurse Physicians Workplace Collaboration: A study conducted on the collaborative relationship between nurse and Physician suggests developing emotional maturity (people who are, “persistently positive, humble, and willing to take responsibility for failures and try again, ” accepting differences, taking on different perspectives, and conducting interdisciplinary education (teaching about a different profession than one’s own. • It emphasizes the importance of collaboration instead of a medical hierarchy stating, “Interdisciplinary collaboration among individuals with different skill sets and knowledge bases may result in creative and practical solutions that would not otherwise occur. ” • “team members must define which tasks can be done individually, which must be worked on together, and what the expectations are for joint interactions, ” all while ensuring no one burns out in the process and a healthy level of disagreement is allowed to occur every once in awhile • Similar to Nurse Practitioners, Nurses who took the questionnaire had a more positive attitude toward collaboration than the Physician did. • “the nurses' mean score of 3. 35 (SD = 1. 38) was higher than the physicians (2. 25, SD = 1. 51) on the fourpoint scale. ” • These nurses also rejected the physician being in the more, “dominant, ” role. What can we learn in primary care? reviewed 11 systematic reviews 3 of which found that nurse-physician collaboration lowered blood pressure in patients, decreased the risk of old age people being hospitalized, and increased patient satisfaction.

Verena Schadewaldt et al reviewed 14 qualitative studies, 13 surveys, 2 mixed-method studies, and 1 quantitative study published between 1990 -2012 regarding collaboration efforts and studies between Nurse Practitioners and Physicians and the factors that either inhibited collaboratory efforts or facilitated them. Different Lenses Nurse Practitioners • View collaboration as following instructions and, “advice seeking of NPs, ” with a more, “interdependent, hierarchical relationship. ” • Follow a more autonomous route. Don’t see Physicians as higher up than them. • Follow a more traditional route. Don’t see NPs as autonomous providers who can handle complex cases. See them as assistants. • See NP autonomy as, “full responsibility for patient care, ” while still being able to consult Physicians. • See NP autonomy as having no Physician consults and have a positive view toward supervision of NPs. • Rely on Physicians to support and work with them. Increase in employment by Physicians will influence collaboration relationships due to hierarchy. • 3 survey studies conducted in the UK found that most Physicians would be willing to hire or collaboration with NPs in order to provide more efficient care. • Feel pressure working under a difficult Physician and have a negative view toward supervision of NPs. • “The survey of Hallas et al. [71] revealed that some NPs saw supervision as negative, as being controlled by MPs, others valued supervision as having the MP available on site. “ They published their findings in, “Views and Experiences of Nurse Practitioners and Medical Practitioners with Collaborative Practice in Primary Health Care – an Integrative Review. ” Physicians • View collaboration as assisting and a “reciprocal discussion about patients. ” • Way et al study discovered that, ” only 2% of 173 patient encounters … resulted in a referral to a NP in contrast to 16% of 79 patients who saw a NP and were then referred to a [Physician] for follow-up They pulled these studies from databases such as, “the Cochrane Library, the Joanna Briggs Institute Library, Pub. Med, Medline, CINAHL, Informit and Pro. Quest. ” “Professional turf wars consume enormous resources and are often fueled, or at least supported, by the idiosyncrasies of state politics. Although cause and effect cannot be assumed, the cost of these wars may actually be neglected health care for the most vulnerable and needy people in the state, the very thing the national NP initiative was crafted to alleviate. ” (Nurse Practitioners : The Evolution and Future of Advanced Practice 157). • “[Physicians] with previous experience of working with a NP exhibit a more positive attitude towards collaboration with NPs, ” and believe that they are equipped to prescribe medication and bring in new patients all while providing high quality care (Carr et al study ). • “A survey of 378 primary health care NPs identified that many bi-directional referrals occur between NPs and family [Physicians] or [Physicians] working in community health centers, but only one-way referrals from NPs to specialists were observed. ”

The Barriers Increa bi li ty nce of o f &c ont hierarc rol Physician lack of hy understanding/acceptan ce lia vale pre le NP gal ed mit e w/ i l NP rienc ses e ca exp plex Phcyom sic of fa ian has im ith in NP a lack edu re bala of lity na so er g for d p iafunndin ba y. Nsioc ph NPs se in for Ph workload ysicia n ce in n e d fi n o No c e th r’s e one ano of on abilnitciees roles ora ’s Ign other an Ph thr ysic ea ian ten s ed fee by ling NP s and NPs a r clea ation hipz difference in edu between Physicians l No ers i lead rgan o or ort po pp su Diff e Ide rent olo gie s fe rra nce ls o f

Research Suggestions • “Research will contribute to an understanding of the role of NPs nationally and internationally within a wider context of the players and agenda. ” • Models such as the Nurse Physician Collaboration Scale as used in a study entitled What can organizations do to improve family physician’s inter-professional collaboration? can be created to measure the collaboration between NPs/Pas and Physicians to calculate improvement or barriers. • This model measures the, “sharing of patient information, joint participation in the cure/care decision-making process, and cooperativeness. ” • Its calculation will also emphasize on its definition and importance in the healthcare field. • According to the article, “research in Europe and the USA has focused on self-report measurements of collaboration and related concepts, mainly in relation to nurses and physicians. ” • In order to gather more data and theorize solutions on how to establish collaborator efforts between non-Physician Providers and Physicians, research may have to move towards a more comprehensive, quantitative movement by using measurements similar to the Nurse-Physician Collaboration Scale. • Other model examples include The Professional Practice Environment Assessment Scale (PPEAS) which is a 13 -item scale assessment which tests, “nurse and physician perceptions of the quality of the healthcare environment, ” at a single point in time. “It looks at the presence of positive physician and nurse characteristics, organizational characteristics (beliefs about the importance of nurse-physician respect, communication, and collaboration on patient outcomes), and frequency of joint-patientcare decision making. ” • Studies such as Mundinger and Brown and Grimes can be carried out to continue measuring the quality of care given by nonphysician providers vs. Physicians to continue testing if there really is a risk of having non-physician providers run their own practices, and prescribe medications. • Conducting more research about the quality and efficiency of care provided by non-Physician vs. Physicians, how these professions collaborate, barriers and facilitators, and methods on how to increase collaboration can assist in embettering the quality of care provided to patients.

• Solutions: The Treatments • Implementing more facilitators • Independent or, “expanded practice roles” • education and funding for education for NPs/Pas • Better standards for education • Funding could help, “boost in enrollments, graduations, and practice placements that will be most meaningful in meeting social and health care needs. ” • It can also • acceptance by Physicians • “strong united voices in the policy arena” • Adapting NPs and PAs to healthcare needs • Spreading the word to patients about the quality of care and cost non-Physician providers provide. • more research using various methods and viewpoints into the effectiveness and collaborative efforts between non-Physicians and Physicians • “(1) use consistent and reliable data sources, such as state licensing data, (2) collect basic information about all providers, (3) include PAs and NPs in the calculation of medical practitioner supply estimates, and (4) integrate medical workforce planning for physicians, PAs, and NPs. ”

Works Cited Admin. “Nurse Practitioner Vs. Physician Assistant. ” Nurse. Journal. org, Nurse Journal, nursejournal. org/nurse-practitioner/np-vs-physicianassistants/. Brock, Douglas M. , et al. “Physician Assistant and Nurse Practitioner Malpractice Trends. ”Medical Care Research and Review, vol. 74, no. 5, 2016, pp. 613– 624. , doi: 10. 1177/1077558716659022. Elsous, Aymen, et al. “Nurses and Physicians Attitudes toward Nurse-Physician Collaboration: A Survey from Gaza Strip, Palestine. ” Nursing Research and Practice, Hindawi Publishing Corporation, 23 Feb. 2017, www. ncbi. nlm. nih. gov/pmc/articles/PMC 5343283/. Hooker, Roderick S. “Is Physician Assistant Autonomy Inevitable? ” Semantic. Scholar. org, Semantic Scholar, pdfs. semanticscholar. org/bc 3 f/c 6 d 08 a 39 ff 531 a 6 d 94 ed 127 a 87 b 8870 bf 4 f 6. pdf+ Johnson, Jean E. “Working Together in the Best Interest of Patients. ” The Journal of the American Board of Family Medicine, vol. 26, no. 3, 2013, pp. 241– 243. , www. jabfm. org/content/26/3/241. full. Lindeke, Linda L, and Ann M Sieckert. “Nurse-Physician Workplace Collaboration. ” The Journal of Issues in Nursing, vol. 10, no. 1, Jan. 2005, www. nursingworld. org/Main. Menu. Categories/ANAMarketplace/ANAPeriodicals/OJIN/Tableof. Contents/Volume 102005/No 1 Jan 05/tpc 26_416011. html. Matthys, Evi, et al. “An Overview of Systematic Reviews on the Collaboration between Physicians and Nurses and the Impact on Patient Outcomes: What Can We Learn in Primary Care? ” BMC Family Practice, vol. 18, no. 1, 22 Dec. 2017, doi: 10. 1186/s 12875 -017 -0698 -x. Morgan, Perri, et al. “Physician Assistants and Nurse Practitioners: a Missing Component in State Workforce Assessments. ” Journal of Interprofessional Care, vol. 25, no. 4, Feb. 2010, pp. 2 -5. , doi: 10. 3109/13561820. 2010. 501917. Nurse Practitioners : The Evolution and Future of Advanced Practice, Fifth Edition, edited by Eileen M, Dr. , Ph. D, CRNP, RN, FAAN Sullivan-Marx, et al. , Springer Publishing Company, 2010, pp. 4 -10; 17, 18, 79, 81, 84, 85, 87, 157, 375, 377. , Pro. Quest Ebook Central, .

Works Cited Oregon Health and Science University. Physician Assistants: PArtners in Medicine, Past, Present and Future, www. ohsu. edu/xd/education/library/about/collections/historical-collections-archives/upload/pa-brochure_web. pdf. Perloff, Jennifer, Catherine M. Des. Roches, and Peter Buerhaus. “Comparing the Cost of Care Provided to Medicare Beneficiaries Assigned to Primary Care Nurse Practitioners and Physicians. ” Health Services Research 51. 4 (2016): 1407– 1423. PMC. Web. 7 Jan. 2018. Perreault, Kadija, et al. “What Can Organizations Do to Improve Family Physicians’ Interprofessional Collaboration? ” Canadian Family Physician, 2017, pp. 381– 388. , www. ncbi. nlm. nih. gov/pmc/articles/PMC 5597028/. “Physician Assistants: Collaboration and Care : Introduction. ” U. S. National Library of Medicine, National Institutes of Health, 14 Aug. 2017, www. nlm. nih. gov/exhibition/pa-collaborationandcare/exhibition 0. html. Schadewaldt, Verena, et al. “Views and Experiences of Nurse Practitioners and Medical Practitioners with Collaborative Practice in Primary Health Care – an Integrative Review. ”BMC Family Practice, Bio. Med Central, 5 Sept. 2013, www. ncbi. nlm. nih. gov/pmc/articles/PMC 3846155/. . Siedlecki, Sandra L, and Eric D Hixson. “Relationships Between Nurses and Physicians Matter. ” Journal of Issues in Nursing, vol. 20, 3 Sept. 2015, www. nursingworld. org/Main. Menu. Categories/ANAMarketplace/ANAPeriodicals/OJIN/Tableof. Contents/Vol-202015/No 3 -Sept-2015/Articles-Previous-Topics/Relationships-between-Nurses-and-Physicians-Matter. html. The Nursing Profession : Development, Challenges, and Opportunities, edited by Diane J. Mason, et al. , John Wiley & Sons, Incorporated, 2011. pp. 198 -203, . Pro. Quest Ebook Central, http: //ebookcentral. proquest. com/lib/northgeorgia/detail. action? doc. ID=698095. Ushiro, Rei. “Nurse–Physician Collaboration Scale: Development and Psychometric Testing. ”Journal of Advanced Nursing, vol. 65, www. ncbi. nlm. nih. gov/pmc/articles/PMC 2738564/
- Slides: 16