Cold Weather Injuries Bureau of Workers Comp PA

Cold Weather Injuries Bureau of Workers Comp PA Training for Health & Safety (PATHS) PPT-084 -01 1

Who is at Risk? Anyone who works outside is subject to cold weather injuries! PPT-084 -01 2

Who is at Risk? Whether during their regular shift or during extended shifts due to emergencies. PPT-084 -01 3

Who is at Risk? Others at risk: PPT-084 -01 4

Who is at Risk? Those using extremely cold liquefied gases in industry such as: Liquid Nitrogen and Liquid Helium PPT-084 -01 5

Types of Cold Weather Injuries § § Hypothermia Chilblains Frostbite Trench Foot or Immersion Foot PPT-084 -01 6
Hypothermia is a Medical Emergency • Normal body temperature (98. 6 o. F) drops to or below 95 o. F. • Fatigue or drowsiness; uncontrolled shivering; cool bluish skin; slurred speech; clumsy movements; irritable, irrational or confused behavior. PPT-084 -01 7

Hypothermia Symptoms Mild Shivering Dizziness Hunger Nausea Breathing/heart rate increase Difficulty speaking Slight confusion Fatigue Moderate to Severe Shivering will stop Lack of Coordination Clumsiness Loss of Consciousness Shallow breathing/weak pulse Slurred speech/mumbling Poor decision making Drowsiness, low energy lack of concern PPT-084 -01 8

Causes of Hypothermia • Wearing unsuitable clothing • Working or recreation outdoors too long • Exertion leading to wet clothing • Falls into water PPT-084 -01 9

Causes of Hypothermia Risk Factors: § Elderly or very young § Mental problems interfering with judgment; dementia or mental illness. § Alcohol and drug use causing blood vessels to dilate § Medical conditions; poor nutrition, stroke, severe arthritis, Parkinson’s, diabetes; conditions affecting blood flow. PPT-084 -01 10

Other Conditions § § Freezing body tissues-frostbite Tissue death and decay-gangrene Diagnosis is apparent by physical signs Don’t drink alcohol PPT-084 -01 11

Hypothermia What Should be Done? (land temperatures) o Call for emergency help (e. g. Ambulance or Call 911). o Move the person to a warm dry area. o Don’t leave the person alone. o Remove any wet clothing and replace with warm, dry clothing or wrap the person in blankets. o Have the person drink warm, sweet drinks (sugar water or sports type drinks) if they are alert. Avoid drinks with caffeine (coffee, tea, or hot chocolate) or alcohol. PPT-084 -01 12

Hypothermia What Should be Done? (land temperatures) • Have the person move their arms and legs to create muscle heat. If they are unable to do this, place warm bottles or hot packs in the arm pits, groin, neck and head areas. • Do NOT place them in warm water bath. This may stop their heart. • DO NOT rub the affected area, because rubbing causes damage to the skin and tissue. PPT-084 -01 13

Hypothermia What Should be Done? (water temperatures) Call for emergency help (e. g. Ambulance or Call 911). Body heat is lost up to 25 times faster in water. PPT-084 -01 14

Hypothermia What Should be Done? (water temperatures) o DO NOT remove any clothing. o Button, buckle, zip and tighten any collars, cuffs, shoes and hoods because the layer of trapped water closest to the body provides a layer of insulation that slows the loss of heat. o Keep the head out of water and put on a hat or hood. PPT-084 -01 15

Hypothermia What Should be Done? (Person not breathing) If a person is not breathing or has no pulse: § Call 911 for emergency medical assistance immediately. § Treat the worker as per instructions for hypothermia, but be very careful and do not try to give an unconscious person fluids. § Check him/her for signs of breathing and for a pulse. Check for 60 seconds. § If after 60 seconds the affected worker is not breathing and does not have a pulse, trained workers may start rescue breaths for 3 minutes. PPT-084 -01 16

Hypothermia What Should be Done? (Person not breathing) § § Recheck for breathing and pulse, check for 60 seconds. If the worker is still not breathing and has no pulse, continue rescue breathing. Only start chest compressions per the direction of the 911 operator or emergency medical services* Reassess patient’s physical status periodically. *Chest compression are recommended only if the patient will not receive medical care within 3 hours. PPT-084 -01 17

Hypothermia (water) • Get out of the water quickly or climb on anything floating. • DO NOT attempt to swim unless a floating object or another person can be reached. Swimming or other activity uses the body’s heat and reduces survival time by about 50%. PPT-084 -01 18
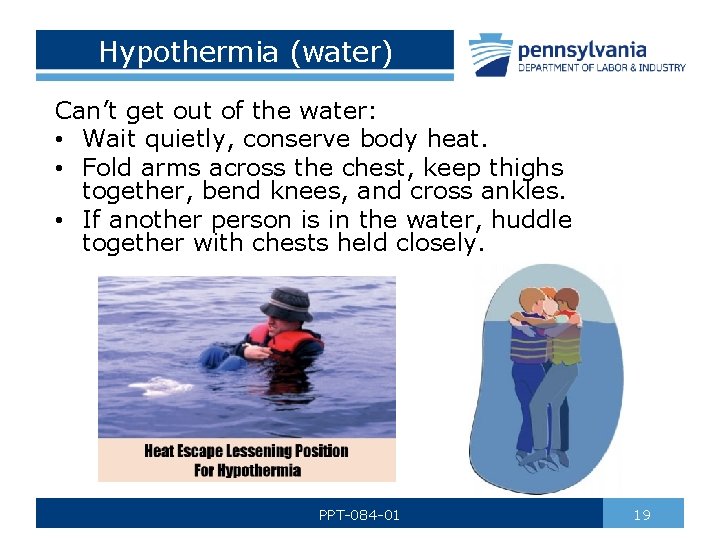
Hypothermia (water) Can’t get out of the water: • Wait quietly, conserve body heat. • Fold arms across the chest, keep thighs together, bend knees, and cross ankles. • If another person is in the water, huddle together with chests held closely. PPT-084 -01 19

Infants and Hypothermia Visual cues: § Skin-bright red and cold § Low energy § Weak cry Precautions: • Dress infants and young in one more layer than adults for same conditions. • If shivering-bring indoors and rewarm. • Babies should not sleep in a cold room. PPT-084 -01 20

Winter Driving Tips Let your destination contact know when you’re leaving and estimated time of arrival. Keep emergency kit in car: q Blankets q Matches q Clean can to melt ice for drinking q First aid kit q Food q Jumper cables q Cellphone PPT-084 -01 21

If Stranded on the Road § Bring everything you’ll need from trunk to car § Stay covered and huddle § Run car for 10 minutes hourly to warm up § Ensure window is down a bit and exhaust pipe is unobstructed. PPT-084 -01 22
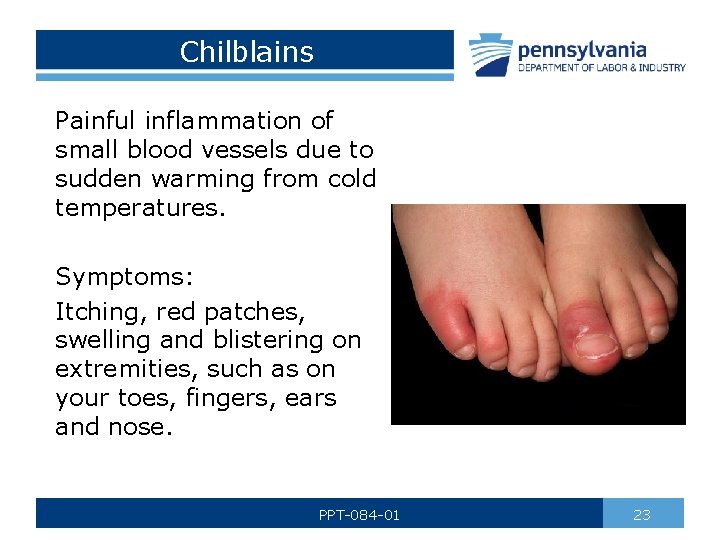
Chilblains Painful inflammation of small blood vessels due to sudden warming from cold temperatures. Symptoms: Itching, red patches, swelling and blistering on extremities, such as on your toes, fingers, ears and nose. PPT-084 -01 23

Chilblains • In one to three weeks, condition may clear as weather warms. • Treatments typically consist of lotions and medication. • Limit your exposure to cold and dress warmly. PPT-084 -01 24

Chilblains Risk Factors • Skin exposed to cold • Being female and underweight • Where Domiciled • Time of year Raynaud’s Phenomenon • Poor circulation • Diagnosed with Raynaud’s Phenomenon PPT-084 -01 25
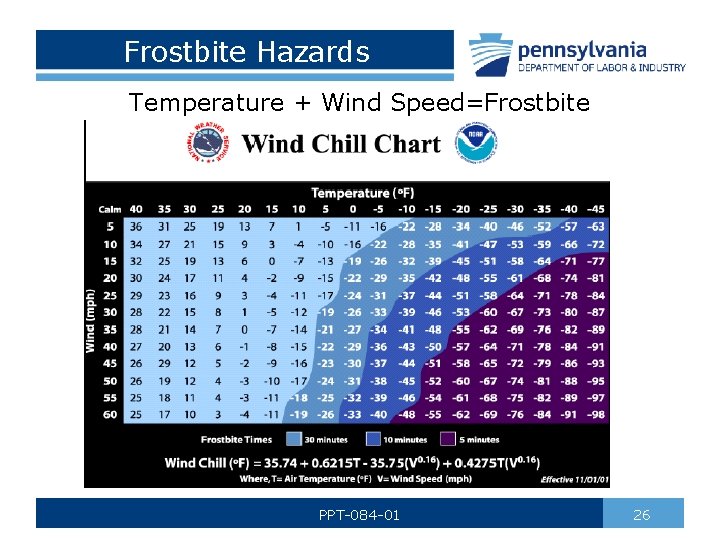
Frostbite Hazards Temperature + Wind Speed=Frostbite PPT-084 -01 26

Frostbite Signs & Symptoms • At first, cold skin and a prickling feeling • Numbness • Red, white, bluish-white or grayish-yellow skin • Hard or waxy-looking skin • Clumsiness due to joint and muscle stiffness • Blistering after rewarming, in severe cases PPT-084 -01 27
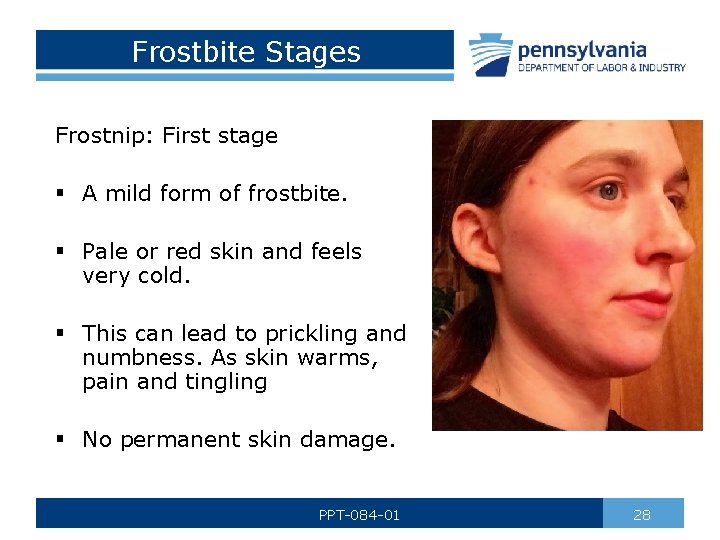
Frostbite Stages Frostnip: First stage § A mild form of frostbite. § Pale or red skin and feels very cold. § This can lead to prickling and numbness. As skin warms, pain and tingling § No permanent skin damage. PPT-084 -01 28
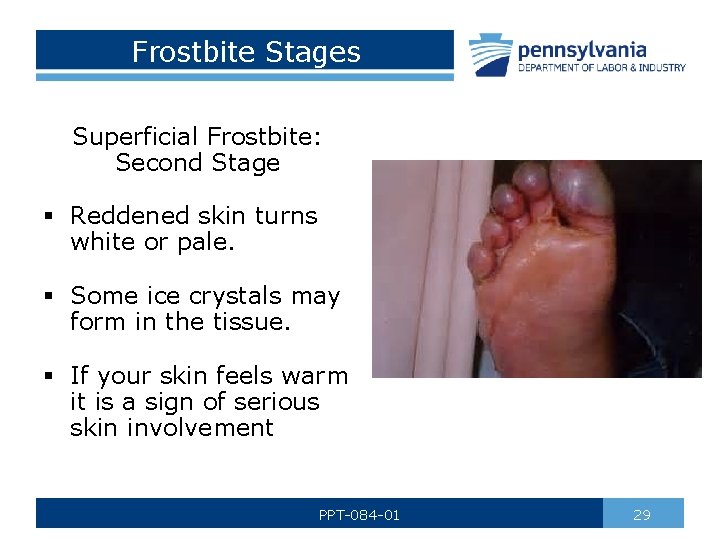
Frostbite Stages Superficial Frostbite: Second Stage § Reddened skin turns white or pale. § Some ice crystals may form in the tissue. § If your skin feels warm it is a sign of serious skin involvement PPT-084 -01 29
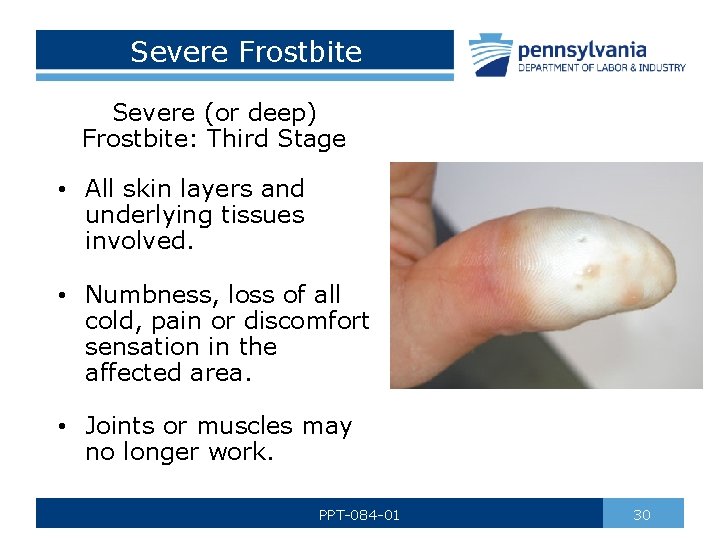
Severe Frostbite Severe (or deep) Frostbite: Third Stage • All skin layers and underlying tissues involved. • Numbness, loss of all cold, pain or discomfort sensation in the affected area. • Joints or muscles may no longer work. PPT-084 -01 30

Frostbite Risk Factors • Medical conditions: dehydration, exhaustion, diabetes and poor blood flow • Alcohol or drug abuse • Smoking • Fear, panic or mental illness, inhibiting your ability to respond to cold • Previous frostbite or cold injury • Infant or older adult: difficulty in producing body heat • High altitudes, reduce oxygen supply to your skin PPT-084 -01 31
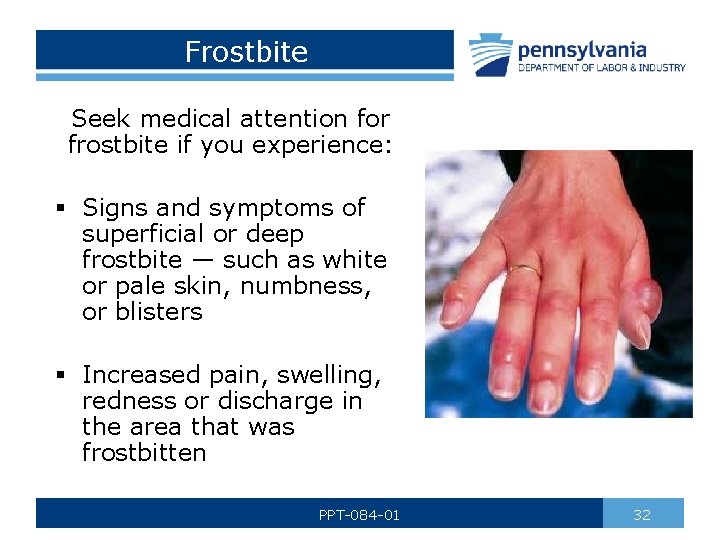
Frostbite Seek medical attention for frostbite if you experience: § Signs and symptoms of superficial or deep frostbite — such as white or pale skin, numbness, or blisters § Increased pain, swelling, redness or discharge in the area that was frostbitten PPT-084 -01 32

Frostbite Seek Medical Attention if: § Fever § New, unexplained symptoms Get emergency medical help if you suspect hypothermia, a condition in which your body loses heat faster than it can be produced. PPT-084 -01 33
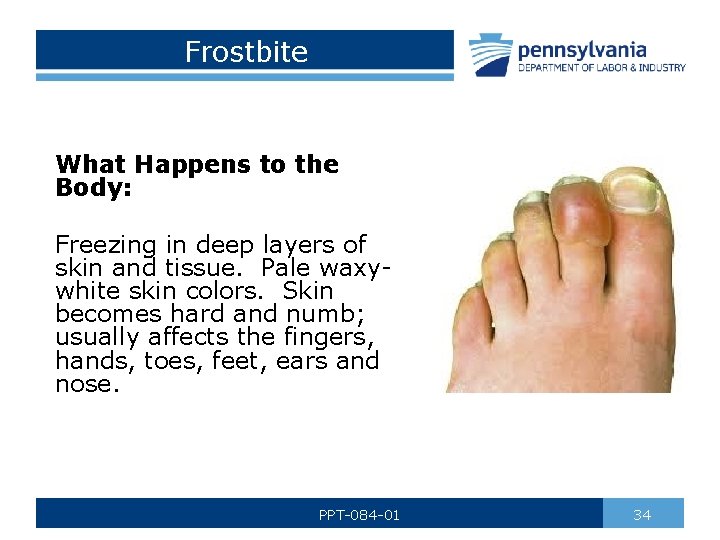
Frostbite What Happens to the Body: Freezing in deep layers of skin and tissue. Pale waxywhite skin colors. Skin becomes hard and numb; usually affects the fingers, hands, toes, feet, ears and nose. PPT-084 -01 34

Frostbite What Should be Done? § Move the person to a warm dry area. Don’t leave the person alone. § Remove any wet or tight clothing that may cut off the blood flow to the affected areas. § DO NOT rub the affected area, because rubbing causes damage to the skin and tissue. PPT-084 -01 35

Frostbite What Should be Done? Gently place the affected area in a warm (105 o. F) water bath and monitor the water temperature to slowly warm the tissue. Don’t pour warm water directly on the affected area because it will warm the tissue too fast causing tissue damage. Warming takes about 25 -40 minutes. PPT-084 -01 36

Frostbite o After the affected area has been warmed, it may become puffy and blister. o The affected area may have a burning feeling or numbness. o When normal feeling, movement and skin color have returned, the affected area should be dried and wrapped to keep it warm. NOTE: If there is a change the area may get cold again, do not warm the skin. If the skin is warmed and then becomes cold again, it will cause severe tissue damage. Seek medical attention as soon as possible. PPT-084 -01 37
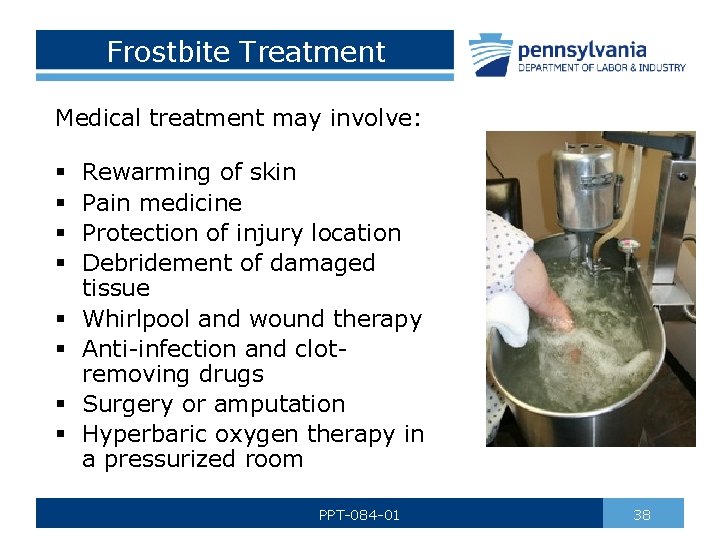
Frostbite Treatment Medical treatment may involve: § § § § Rewarming of skin Pain medicine Protection of injury location Debridement of damaged tissue Whirlpool and wound therapy Anti-infection and clot- removing drugs Surgery or amputation Hyperbaric oxygen therapy in a pressurized room PPT-084 -01 38

Frostbite Complications Increased sensitivity to cold Risk of recurring frostbite Long-term numbness in the affected area Changes in the cartilage between the joints (frostbite arthritis) § Growth defects in children, if frostbite damages a bone's growth plate § § PPT-084 -01 39

Frostbite Complications § Infection § Tetanus § Gangrene — decay and death of tissue resulting from an interruption of blood flow to the affected area — which can result in amputation PPT-084 -01 40

Trench Foot or Immersion Foot First noted in the trench warfare where soldiers suffer from this disease after having their feet exposed to prolonged moisture. This disease is most prevalent during rainy days especially in places where flooding is usual. PPT-084 -01 41
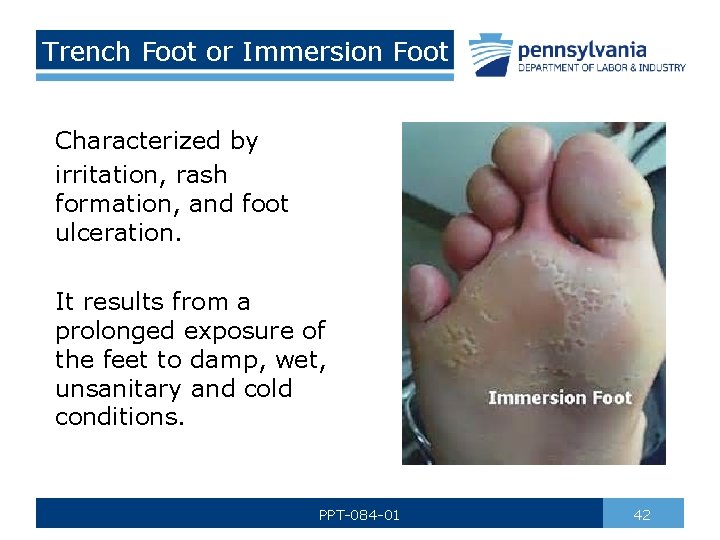
Trench Foot or Immersion Foot Characterized by irritation, rash formation, and foot ulceration. It results from a prolonged exposure of the feet to damp, wet, unsanitary and cold conditions. PPT-084 -01 42
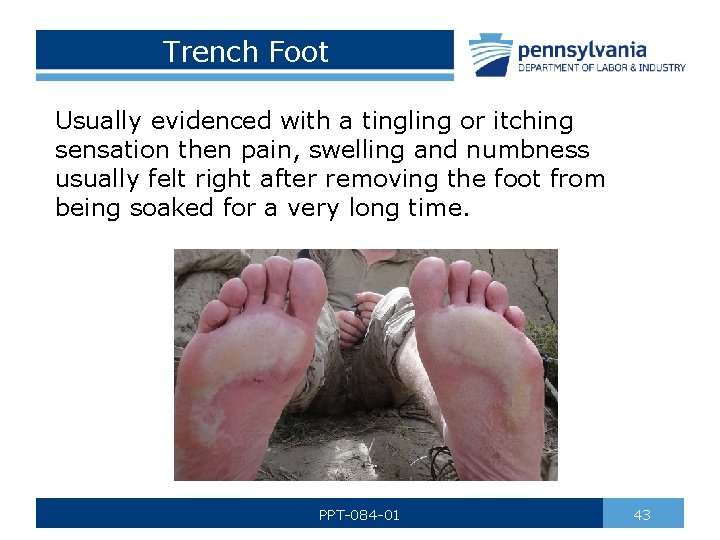
Trench Foot Usually evidenced with a tingling or itching sensation then pain, swelling and numbness usually felt right after removing the foot from being soaked for a very long time. PPT-084 -01 43

Trench Foot Cause While encountered during World War I, this was also an issue during subsequent wars; World War II, Korea and Viet Nam. PPT-084 -01 44

Trench Foot Treatment Prevention first! § Constant change to dry socks. § Keep feet dry and clean. § Do not wear constrictive footwear. § Clean the foot using mild cleansers. § Dry carefully using a clean towel. § After drying the feet, keep them elevated and gently warm them. PPT-084 -01 45
Trench Foot Treatment • Elevating the affected area promotes increased blood circulation which reduces inflammation. • After elevating the feet, carefully warm them by immersing in warm circulating water, about 104 F to 107 F, for 15 to 30 minutes. PPT-084 -01 46

Trench Foot See a physician: o Contact your podiatrist regarding the cure of the disease. o Cover the foot with adequate amounts of clean cloth to prevent the recurring of cold injury. PPT-084 -01 47

Other Conditions Other conditions due to cold environments would also include: § Dehydration § Cold Diuresis § Constipation § Sunburn § Snow Blindness PPT-084 -01 48

Dehydration When you’re wearing multiple layers of clothing, you may not be aware of body moisture loss. You must drink water to replace fluid loss. PPT-084 -01 49

Cold Diuresis & Constipation Cold Diuresis is the increased output of urine during cold weather. Replace fluids. 1. Constipation may result due to putting off relieving yourself in the cold. 2. Eating dehydrated foods. 3. Drinking too little liquid. 4. Irregular eating habits may contribute. 5. Eat fruits and increase fluid intake to at least 2 quarts a day. PPT-084 -01 50

Sunburn This is due to the sun’s reflection off many surfaces and striking sensitive skin: o Snow o Ice o Water The application of sunburn cream and lip salve will help. PPT-084 -01 51

Snow Blindness Sun’s ultraviolet rays are reflected off snow. Symptoms may include: • Feeling of grit in eyes, • Pain in and over eyes which may increase with eyeball movement, • Watering eyes; becoming red • A headache which intensifies PPT-084 -01 52

Snow Blindness Treatment is required since prolonged exposure may result in permanent eye damage. • Bandage eyes until symptoms disappear. • Wear sunglasses. • You can improvise sunglasses by cutting slits in cardboard. • Put soot on cheeks under eyes to reduce glare. PPT-084 -01 53

MSD Risk Factors Cold Temperatures § Cold environments compromise muscle efficiency. § Possible vascular and neurological damage. § Workers with cold-desensitized fingers may grasp loads with more force than necessary: exposes muscles, soft tissues, and joints to increased force. § Alcohol, nicotine, caffeine, and some medication increases MSD risks from cold temperatures. PPT-084 -01 54

Preventive Hygiene Washing areas where moisture develops can help prevent rashes to preclude more severe problems. § Wash where moisture and sweat accumulate: Ø Under arms Ø Between legs § Wipe dry and then periodically wipe in the same areas to remove moisture § Wash feet daily and put on dry socks. PPT-084 -01 55

Protecting Workers § Recognize the environmental and workplace conditions that lead to potential cold-induced illnesses and injuries. § Learn the signs and symptoms of cold-induced illnesses/injuries and what to do to help the worker. § Train the workforce about cold-induced illnesses and injuries. § Select proper clothing for cold, wet and windy conditions. Layer clothing to adjust to changing temperatures. Wear a hat and gloves, in addition to underwear that will keep water away from the skin (polypropylene). PPT-084 -01 56

Protecting Workers o Take frequent short breaks in warm dry shelters to allow the body to warm up. o Perform work during the warmest part of the day. o Avoid exhaustion or fatigue because energy is needed to keep muscles warm. o Use the buddy system (work in pairs). o Drink warm, sweet beverages (sugar water or sports type drinks). Avoid drinks with caffeine (coffee, tea, or hot chocolate) or alcohol. o Eat warm, high-calorie foods like hot pasta dishes. PPT-084 -01 57

Protecting Workers Are at Increased Risk When… • They have predisposing health condition such as cardiovascular disease, diabetes, and hypertension. • They take certain medication (check with your doctor, nurse, or pharmacy and ask if any medicines you are taking affect you while working in cold environments). • They are in poor physical condition, have a poor diet, or are older. PPT-084 -01 58

Protective Measures The National Safety Council recommends: General Controls to promote personal protection: Ø Training Ø Hygiene practices Ø Medical Surveillance Specific Controls advanced: Ø Engineering controls Ø Administrative measures Ø Person Protection (PPE) PPT-084 -01 59

Wear Proper Clothing § Clothing should protect you from cold, wind, and precipitation and should also provide ventilation—be "breathable". § Protect head, feet, hands, and face. Keep dry. § Cover your head. Up to 40 percent of body heat can be lost when the head is exposed. § Footgear should be insulated to protect against cold and dampness. PPT-084 -01 60

Wear Proper Clothing Dress in layers, wearing warm, waterproof/resistant clothing. • An outer layer to break the wind allow some ventilation (like Gore-Tex® or nylon). • A middle layer of wool or synthetic fabric (Qualofil or Pile) to absorb sweat and retain insulation in a damp environment. Down is a useful lightweight insulator; however, it is ineffective once it becomes wet. • An inner layer of synthetic weave to allow ventilation. Synthetic materials such as supplex and coolmax are ideal because they keep you warm and dry. PPT-084 -01 61

Employee’s Responsibilities Dress for conditions Rehydrate Know signs and symptoms of exposure Keep clothing dry Rewarm at station when required Maintain periodic communications with supervisor to apprise of team’s condition § Have an additional set of dry clothing on-hand § § § PPT-084 -01 62

Supervisor’s Responsibility § Brief all teams of their job duties and precautions for cold weather injuries § Check on team’s condition on periodic basis (by radio or field observations) § Inform team of anticipated weather changes and impact § Provide periodic rest breaks in a warm shelter § Provide hot beverages § Know signs and symptoms of exposure § Have provisions for First Aid and Advanced Care if required PPT-084 -01 63

With Cold - Take No Chances PPT-084 -01 64

Bibliography Fundamentals of Industrial Hygiene, Barbara A. Plog, MPH, CIH, CSP, Editor in Chief, National Safety Council, Itasca, IL, 2012 FM 21 -76, US Army Survival Manual, Headquarters, Department of the Army www. mayoclinic. org/diseasesconditions/chilblains/basics/. . . http: //www. safetybok. org/osha_quick_card__cold _stress/ PPT-084 -01 65

Bibliography http: //www. mayoclinic. org/diseasesconditions/hypothermia/basics/prevention/con 20020453 http: //www. mayoclinic. org/diseasesconditions/frostbite/basics/complications/con 20034608 http: //gudhealth. com/trench-foot. html https: //www. osha. gov/SLTC/emergencyprepared ness/guides/cold. html PPT-084 -01 66

Contact Information Health & Safety Training Specialists 1171 South Cameron Street, Room 324 Harrisburg, PA 17104 -2501 (717) 772 -1635 RA-LI-BWC-PATHS@pa. gov Like us on Facebook! - https: //www. facebook. com/BWCPATHS PPT-084 -01 67

Questions PPT-084 -01 68
- Slides: 68