Cognitive Behavioural Therapy for Child Trauma and Abuse

Cognitive Behavioural Therapy for Child Trauma and Abuse Jackie Feather Ph. D Dip. Clin. Psych March 19 2011 NZCCP Auckland

Overview Theoretical frameworks Research and development Clinical use Summary and feedback
Theoretical frameworks informing CBT for child trauma and abuse Contextual/systemic frameworks Cultural considerations Neurobiology Attachment theory Developmental psychology Psychotraumatology CBT Abuse-focus Scientist-practitioner

Contextual/systemic frameworks • An ecological perspective - recognises the many interconnected systems in which a young person exists (Bronfenbrenner, 1979) • Systemic approaches - emphasise the influence of interaction patterns on individuals and relationships within families (Macdonald, Lambie, & Simmonds, 1995) • Cultural world views - shape the conceptualisation and path of an individual and family’s response to abuse and trauma, and have an effect on treatment (Elliott & Urquiza, 2006)

Aotearoa/NZ cultural context Treaty Principles: a guide for policy and practice ◦ Partnership - working together in a spirit of cooperation ◦ Participation – promotes active involvement of all parties ◦ Active protection – includes constant monitoring for safety and improvement Fig 1: My own transition in thinking

Attachment theory • An attachment-based model of intervention focuses on the role of therapist in providing a secure base from which both children and caregivers can explore new ways of relating (Pearce & Pezzot-Pearce, 1994) • Traumatised and abused children may require a longer, more gradual process to develop a trusting relationship with their therapist, particularly if their trauma and attachment histories are early and long-standing (Perry et al. , 1995) • Attachment theory - highlights the importance of the child’s relationships in contributing to and ameliorating the effects of CA trauma

Neurodevelopmental theories • Considerable evidence to suggest that traumatic experiences as a child have a profound effect on the developing brain (Nemeroff, 2004) • Bruce Perry’s model describes how the trauma of abuse can affect the developing brain and shape children’s physiology and related responses. He proposes that CA can result in: ▫ deprivation of sensory stimuli (via neglect, insecure attachment) and/or ▫ overactivation of neural pathways (via the trauma of physical abuse, sexual abuse, and/or witnessing domestic violence), leading to a persistent pattern of hyperarousal or dissociation (Perry et al. , 1995)

Developmental theories Piaget’s theory: ◦ Preoperational (2 -7 years) children learn how to represent the world mentally, but locked into own perspective, and have not yet grasped that there are other “selves” ◦ Concrete operational (7 -11 years) may be able to interrelate their own representations about concrete situations ◦ Formal operational (11 years) begin to develop the cognitive abilities to think abstractly and self-reflect Vygotsky’s theory suggests that a child must be developmentally capable of using thought as a form of “inner speech” for the self-regulation of behaviour

Developmental theories cont. “Meta-cognition” (the ability to reflect about cognition, or “think about one’s thinking”; an inherent feature of CBT) may comprise a range of aspects that develop at different ages and stages (Bolton, 2005) ◦ Recognition that thoughts are under a person’s control and regulating behaviour may appear as early as 6 or 7 years ◦ Concepts such as shame may appear between early and middle childhood ◦ Connection between beliefs (i. e. , the capacity to theorise) may develop in later childhood or adolescence, although even preschoolers may have some aspects of this capacity

Psychotraumatology/PTSD • 1960 s: trauma-specific syndromes recognised with common patterns of psychological distress from diverse traumatic events: ▫ war experiences - “shell shock”, “Vietnam veteran’s syndrome” ▫ interpersonal violence, particularly against women and children - “battered women syndrome” and “abused child syndrome” (van der Kolk et al. , 1996; Weaver & Clum, 1995) • 1980: new diagnosis of PTSD included in the DSM (American Psychiatric Association, 1980) ▫ The PTSD diagnosis was intended to help victims of trauma gain understanding and acceptance and to promote appropriate treatment (Weisaeth, 2002)

PTSD in children Similar to PTSD in adults, including the cardinal symptoms described in the DSM-IV -TR But also differs - children may not meet criteria: Re-experiencing Nightmares Traumatic play Behavioural re-enactments - patterns of behaviour that incorporate aspects of the trauma e. g. sexualised behaviour Psychophysiological re-enactments or ‘body memories’ e. g. physical health problems including headaches, backaches, stomach aches, skin rashes, shortness of breath, tightness in the chest, nausea (Terr, 1990)

PTSD in children cont. Avoidance ◦ Of people, places, events, situations that remind them of the abuse e. g. being alone Hyperarousal ◦ Internalising symptoms e. g. poor concentration and sleep problems ◦ Externalising symptoms e. g. irritability, temper tantrums, exaggerated startle response, ‘freezing’ Associated signs and symptoms ◦ Intensification of normal fears ◦ Magical thinking ◦ Restricted affect/difficulty having tender loving relationships ◦ Depression and sadness/pessimism ◦ Aggressive behaviour

The TRAP acronym* Traumatic event Re-experiencing Avoidance Physiological arousal Terrible thing that happened Remembering even when you don’t want to Avoiding things that remind you Physical reactions in your body *

Exercise: The TRAP activity

Untreated PTSD As children return to safety the initial feelings of helplessness and fear typically turn to anger, rage, shame and guilt The behavioural and emotional changes that accompany PTSD can result in changes in the child’s attitude to life Traumatised children cannot imagine themselves having a normal future e. g. having a job and getting married, or an exciting future becoming an athlete or actor

PTSD and child abuse (CA) • Some abuse-focused clinicians argue the trauma/PTSD conceptualisation does not cover all manifestations of CA e. g. social problems, biological /neurological, other psychological disturbances – anger, shame, guilt (Briere, 1992; Herman, 1992) • CA is often prolonged and repeated - sequelae are more complex than the repetitive symptomatology of simple PTSD, e. g. identity, attachment • But “trauma” and “PTSD” provide useful frameworks for development of theory, research and practice in the field of CA (Briere & Scott, 2006)

Research on child trauma and abuse Limited research in Australasia and internationally on effective psychotherapeutic interventions for child trauma and abuse (James & Mennen, 2001; Mc. Farlane, 2000) Overall prevalence of posttraumatic stress disorder (PTSD) is generally reported for about 1/3 of abused children, depending on the nature of the abuse (Ackerman, Newton, Mc. Pherson, Jones, and Dykman, 1998; Dubner and Motta, 1999; Linning & Kearney, 2004; Mc. Closkey and Walker, 2000) Initial studies suggested that trauma-focused cognitive behavioural therapy (TF-CBT) may be effective and long lasting in the treatment of PTSD in abused traumatised children (Cohen, Deblinger, Mannarino & Steer, 2003; Deblinger, Lippman and Steer, 1999; Kolko, 1996)

Development and evaluation of TF-CBT Aim of the research: To develop and evaluate the effectiveness of a TF-CBT programme for multiplyabused children referred to the Specialist Services of CYF, Puawaitahi, Auckland: ◦ ◦ Locally developed Evidence-based Manualised Clinical setting

Programme elements • Phase 1: Psychosocial strengthening • An essential part of the programme, based on local practice and research – with child and parent/caregivers (Barrett et al. , 2001) • Phase 2: Coping skills • Based on the CBT “Coping Cat” programme for child anxiety • Efficacious, with reduction in anxiety symptoms maintained at 1 - and 3 -year follow-ups (Kazdin & Weiss, 1998; Kendall, Chansky, Kane, Kim, Kortlander, Ronan, Sessa and Siqueland, 1992; Kendall & Southam-Gerow, 1996) • Phase 3: Trauma processing • Imaginal exposure for treating PTSD using creative mediums as recommended in the child trauma literature (Smith, Perrin and Yule, 1998)

Research design Scientist-practitioner clinical research Participants: 16 multiply-abused children with PTSD - 9 girls, 7 boys Design: Single-case multiple-baseline Four studies - 4 children in each: ◦ ◦ Pilot Cultural trial Completed protocol Otherapists

Measures Structured Interview Screen ADIS (Parent/Caregiver and Child) Full Assessment Battery (pre, post and 3, 6 & 12 month follow-up) Child Parent/Caregiver Teacher CDI CBCL-TRF STAIC CPTS-RI TSCC CQ

Measures cont. Short Assessment Battery (weekly during baseline and treatment, and 3, 6, 12 -month follow-up) Children’s Index Posttraumatic Reaction (CPTS-RI, Fredrick, Pynoos & Nader, 1992) Coping Questionnaire (CQ-C ; Kendall et al. , 1992)

Participants - pilot study • Scott (14) – physical and emotional abuse • Jacob (13) - sexual abuse, domestic violence • Kirsty (9) - physical and emotional abuse, domestic violence • Jade (9) - witnessed mother’s suicide attempts, domestic violence

Results PTSD symptoms decreased ◦ Fewer or no bad dreams ◦ Less upset when thinking about the abuse ◦ Less jumpy or nervous Self-reported coping increased ◦ Improved during treatment ◦ Maintained at follow-up
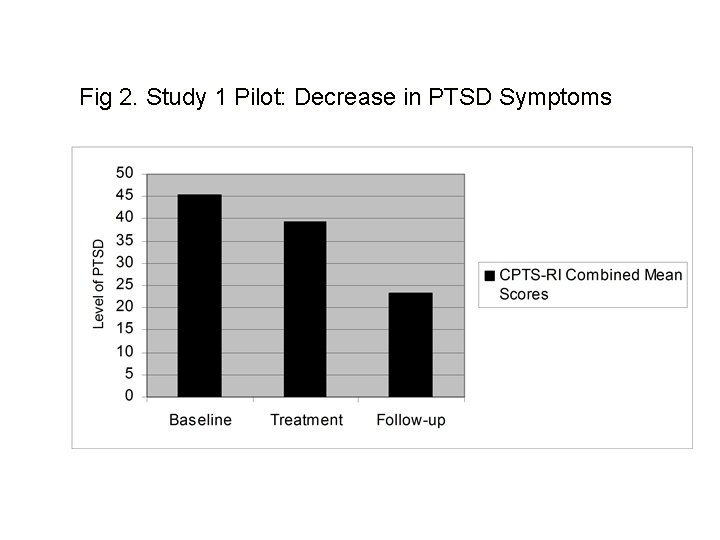
Fig 2. Study 1 Pilot: Decrease in PTSD Symptoms
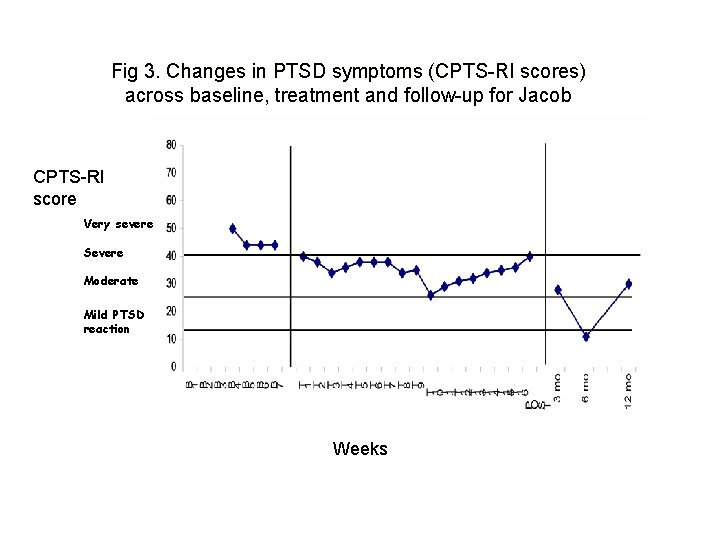
Fig 3. Changes in PTSD symptoms (CPTS-RI scores) across baseline, treatment and follow-up for Jacob CPTS-RI score Very severe Severe Moderate Mild PTSD reaction Weeks
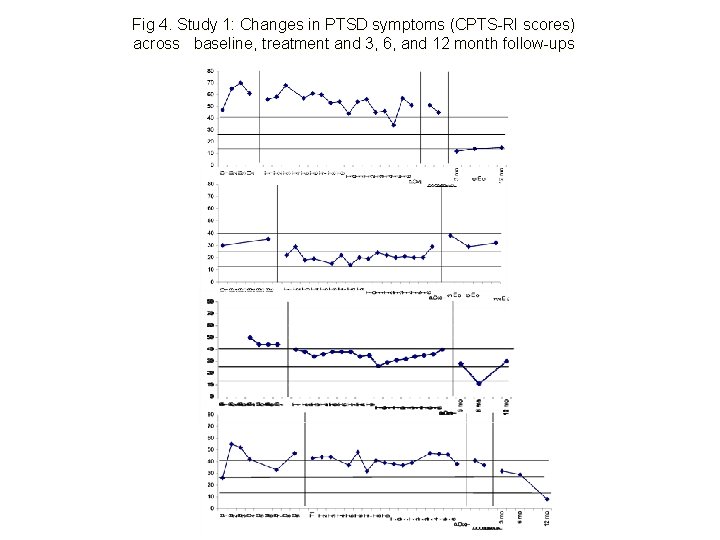
Fig 4. Study 1: Changes in PTSD symptoms (CPTS-RI scores) across baseline, treatment and 3, 6, and 12 month follow-ups
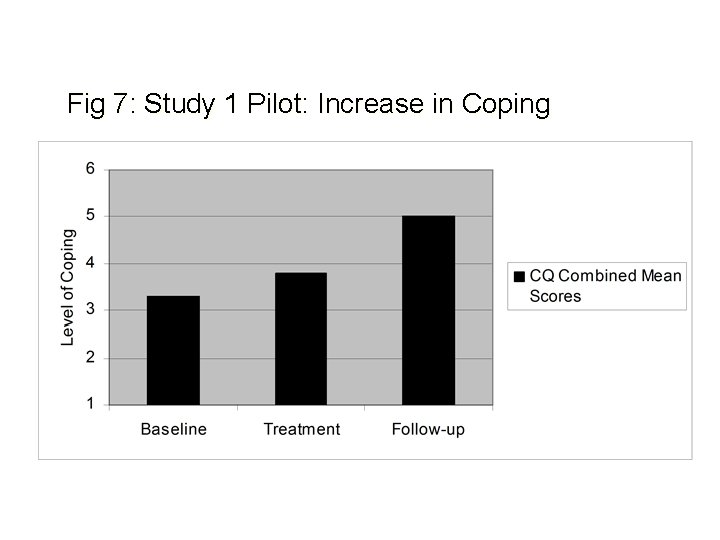
Fig 7: Study 1 Pilot: Increase in Coping
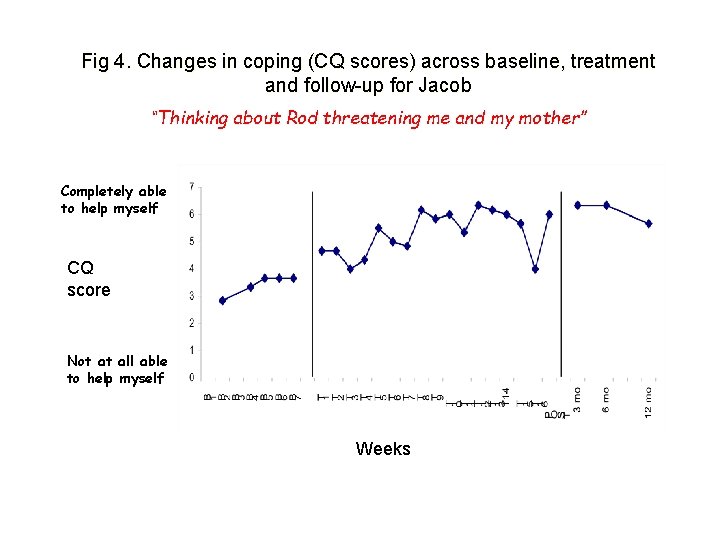
Fig 4. Changes in coping (CQ scores) across baseline, treatment and follow-up for Jacob “Thinking about Rod threatening me and my mother” Completely able to help myself CQ score Not at all able to help myself Weeks
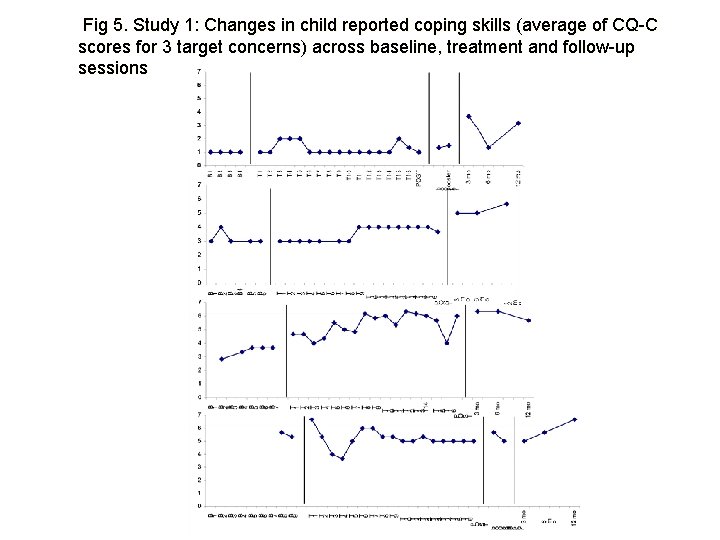
Fig 5. Study 1: Changes in child reported coping skills (average of CQ-C scores for 3 target concerns) across baseline, treatment and follow-up sessions
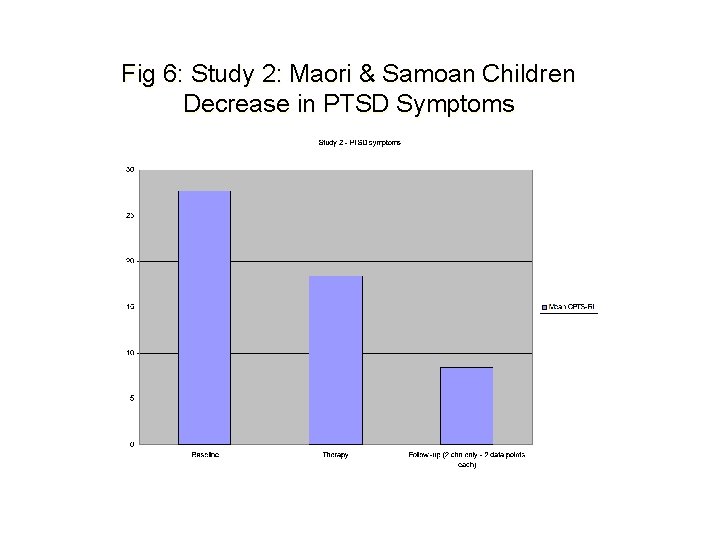
Fig 6: Study 2: Maori & Samoan Children Decrease in PTSD Symptoms
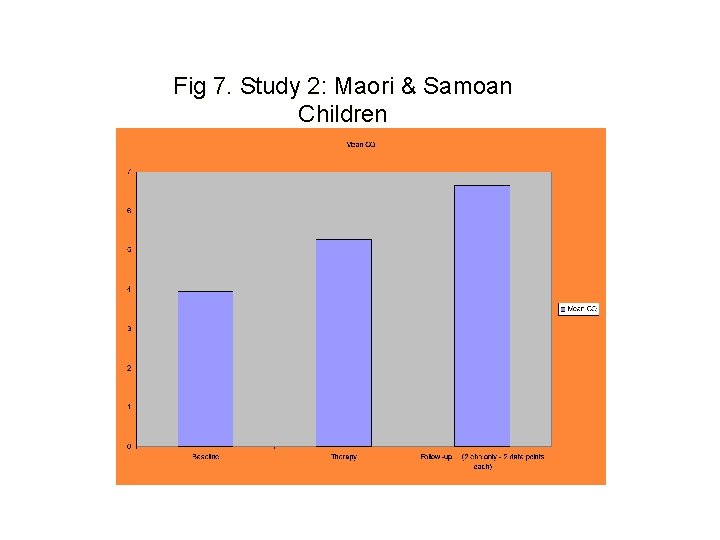
Fig 7. Study 2: Maori & Samoan Children Increase in Coping

Before we move on…a plug for single-case research designs User-friendly in clinical settings Graphed results provide visible evidence of treatment effects on targeted variables, as well as the influence of other documented variables Changes in mean, level, slope, and trend are easily examined, and how a participant is responding to treatment can be interpreted at a glance (Kazdin, 1982) Enables us to be scientist practitioners carrying out research in our own practice settings

Discussion ØThe phase-based manualised TF-CBT programme can be effective in ameliorating the effects of child abuse trauma ØFlexibility required to meet the needs of individual children and families Ø Parent/caregiver involvement Ø Nature of trauma/presenting problems Ø Culture

What contributes to treatment success? Ø Contextual factors Ø Safety Ø Social support Ø Child factors Ø Developmental level (9+) Ø Connection/identity Ø Therapist factors Ø Respect Ø Collaboration Ø Empowerment

TF-CBT: Clinical Use

Assessment Comprehensive assessment § Child § Parent/family § Teachers/other professionals Enables targeted treatment § E. g. , DO NOT re-process historical trauma if no trauma symptoms are present – why?

Therapist focus Effective and sensitive use of TF-CBT for an individual child and family requires an ever-evolving formulation and therapist triple focus: ØDeveloping therapeutic relationship, inspiring hope and participation ØAlleviating symptoms and enhancing coping strategies ØHealing underlying causes of presenting problems

Treatment outline • • Phase 1: Psychosocial Strengthening Phase 2: Coping Skills Phase 3: Trauma Processing Phase 4: Special Issues ØParent/caregiver involvement ØLiaison with other professionals

Therapy session format Review out-of-session activities Set agenda Session activities Homework, summary and feedback

Phase 1: Psychosocial Strengthening Sessions 1 -3 Rapport building, orientation to therapy Relationships/social supports Timeline Orientation for parent/caregivers

Phase 2: Coping Skills Sessions 4 -8 Feelings (recognising and managing emotions) Body reactions (recognising and selfcalming) Thoughts (awareness of self-talk) Actions (active coping and problem solving) Rating and Rewards (self-evaluation and reward) Parent/caregiver session

Coping skills template Te Ara Whetu: The STAR Plan Scary feelings? Thinking bad things? Activities that can help Rating and rewards

Exercise: Self-help task #4

Phase 3: Trauma Processing Sessions 9 -13 • Creation of a trauma narrative to allow emotional processing of traumatic memories using mediums chosen by the child e. g. sandtray, painting, clay, puppets • The child chooses trauma topics to work on from his or her timeline, with gradual exposure from least to most traumatic memories • The 4 -step STAR plan is used to manage trauma symptoms • Parent/caregiver session

Phase 4: Special Issues Sessions 14 – 15 E. g. anger management; separation, grief and loss; guilt and shame; personal safety Session 16 Relapse prevention, celebration, saying goodbye

Summary and feedback Questions? What will you be taking away from this workshop? Feedback

Further reading Feather, J. S. & Ronan, K. R. (2006). Trauma-focused cognitive behavioural therapy for abused children with posttraumatic stress disorder. New Zealand Journal of Psychology, 35, 132 -145. Feather, J. (2004) Becoming a local scientist-practitioner. Social Work Now, 29, 24 -28. Feather, J. S. (2007). Trauma-focused cognitive behavioural therapy for abused children with posttraumatic stress disorder: Development and evaluation of a manualised treatment programme. Ph. D thesis, Massey University, Albany, Auckland. http: //muir. massey. ac. nz/handle/10179/535 Feather, J. S. & Ronan, K. R. (2009). Assessment and interventions for child trauma and abuse. In Taylor, J. & Themessl-Huber, M. (Eds. ) Safeguarding children in the primary care context. UK: Jessica Kingsley Publishers. Feather, J. S. & Ronan, K. R. (2009). Trauma-focused CBT with maltreated children: A clinic-based evaluation of a new treatment manual. Australian Psychologist, 44, 174 -194. Feather, J. S. & Ronan, K. R. (2010). Cognitive behavioural therapy for child trauma and abuse: A step-by-step approach. London, UK: Jessica Kingsley Publishers.
- Slides: 48